Back to Journals » Journal of Blood Medicine » Volume 12
Dynamics of COVID-19 Lockdown on Blood Indices and Its Impact on Individuals’ Immunological Health Status: A Cohort Study in Madinah, Saudi Arabia
Authors Suliman BA
Received 25 March 2021
Accepted for publication 20 May 2021
Published 31 May 2021 Volume 2021:12 Pages 395—402
DOI https://doi.org/10.2147/JBM.S312177
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Martin H Bluth
Bandar A Suliman
College of Applied Medical Sciences, Taibah University, Madinah, Saudi Arabia
Correspondence: Bandar A Suliman
College of Applied Medical Sciences, Taibah University, Madinah, Saudi Arabia
Tel +966-504772422
Email [email protected]
Objective: The complete blood count (CBC) is an essential blood test that has been used for decades to assess individuals’ overall health status. This study aimed to investigate the contributions of lockdown conditions to individuals’ overall health status using blood indices as biological markers. During lockdown, people are limited to confined spaces, have access to limited nutritional supply options, experience increased stress, and are exposed to other environmental factors.
Methods: Our study’s target population included all outpatients who were severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)-negative and requested CBC assessments as part of their routine health checks. A total of 2414 CBC results were included, covering a period from February 2019 to December 2020. The average of different blood indices during the COVID-19 lockdown was compared to the 10-month period preceding the lockdown.
Results: The average counts of RBCs, hemoglobin, and hematocrit showed a significant increase during the lockdown period, which lasted from May 2020 to September 2020. Reductions were observed for the RBC distribution width, total white blood cell count, platelets, and platelet distribution width.
Conclusion: Our findings suggested that the overall health status of individuals improved during the lockdown period in the short term, but health status might be adversely affected under these conditions of a longer period. Both RDW and PDW could be used as indicators for the overall health status when assessed against other blood indices.
Keywords: COVID-19, CBC, lockdown, platelet distribution width, red cell distribution width
Introduction
The complete blood count (CBC) has been used for decades as an essential blood test to assess individuals’ overall health status.1 Specific blood indices, such as the total count of red blood cells (RBCs) which is important to understand the production capacity of the bone marrow, mean corpuscular volume (MCV) which reflects the cell’s size, mean corpuscular hemoglobin (MCH), cell distribution width (RDW) which represent the variation in size between different RBCs, and hemoglobin concentration (HGB) which is used to monitor the blood’s oxygenation capacity, have a significant diagnostic value in reflecting bone marrow’s ability to produce hematopoietic-driven cells.2,3 Other indices related to white blood cells (WBC) and the differential count of each one of them had been used as markers for inflammatory reactions such as bacterial infections, viral infections, parasitic infections, or hematological malignancies.4,5
The immune system is composed of many intertwined cells and organs working in harmony to create the overall protection against pathogens. White blood cell count is very important indicator of how the immune system handles certain clinical and medical situations such as inflammatory reactions or infections by foreign organisms.6–9
SARS-CoV-2 is a single-strand RNA virus belonging to the Coronaviridae family of viruses. It is the primary cause of respiratory symptoms worldwide since the outbreak in Wuhan in January 2020.10 Viral infections are represented in the blood work as a marked increase in total WBC count underlying a significant surge in lymphocytes, which are produced by the immune system as an antiviral response driven by interferons.11–13
The balance in different whole blood indices is essential to maintain the equilibrium of many important blood components such as albumin and plasma proteins. That is why a CBC is ordered and considered an essential blood test in the first line of the diagnostic process in many clinical complications.14
In this study, we aim to investigate the role of COVID-19 and the accompanying lockdown that was enforced between May 2020 and September 2020 on patients’ blood indices in Medina region. We ask if these indices can be used to measure the overall health status of individuals and if a significant difference in blood indices is noticed that may be attributed directly to certain lifestyle changes associated with the lockdown.
Materials and Methods
Ethics Statement
This study was approved by the Internal Review Board of Taibah University in Madinah, Saudi Arabia (No. 2021/90/114/MLT). Written informed consent was obtained from each patient prior to participation in the study.
Study Population
Our study’s target population were all out-patients who were SARS-CoV-2 negative and requested a complete blood count (CBC). Any patient showing respiratory symptoms or was less than 18 years were excluded from the study. A total of 2414 CBC results were obtained from the laboratory information system (Table 1). These results were from 772 males (aged between 18 and 91 years) and 1642 females (aged between 18 and 82 years).
 |
Table 1 Target Population Used for This Study (n = 2414) |
Complete Blood Count
Three milliliters of whole blood samples were collected in Lavender top tubes containing EDTA K3 (Advanced Medical Co., Riyadh) and then placed on a roller (12 RPM) until the analysis. CBC analysis was performed between 10 minutes and 3 hours after sample collection on the XP-300 Automated Hematology Analyzer (Sysmex Corporation, Hyogo).
Statistical Analysis
Blood indices were accumulated for each month to calculate the average, SD, and SEM and then blotted as graphical reorientations. Significance in the difference between monthly averages was calculated using the 2-sample t-test, which is commonly used to compare two independent parametric groups and tests the null hypothesis, assuming that both means are identical.15 Additionally, the Violin plot was used to compare the averages of the entire time periods. The unpaired t-test, and the F-test were performed to calculate the p-value. Statistical analysis and graphical representation of data were performed using Prism 8.2 (GraphPad Software, Inc., San Diego).
Results
Iron-Related CBC Indices are Increased During the Lockdown Period
For the 10 months preceding the lockdown, the average RBC count was 4.32 × 106/µL (Figure 1). This average showed a significant increase to 4.59 × 106/µL, an approximate 7% increase (Figure 2), for the lockdown period, which started in May 2019 and lasted for 5 months. This increase was determined to be significant using both the unpaired t-test and the F-test with a p-value of <0.0001 in both statistical tests. This observation was not limited to only RBCs. We showed that Hemoglobin and Hematocrit (Figure 1) showed very similar results as RBCs (Table 2). Hemoglobin concentration increased significantly from 11.69 g/dL to 12.61 g/dL (t= 7.511; p-value= <0.0001), as well as Hematocrit which increased significantly from 34.33% to 36.91% (t= 7.876; p-value= <0.001; F= 1.223; p-value= <0.01). This clearly indicates that iron-related CBC indices are increased during the lockdown when compared to before that time period (Figure 2). RBC mean corpuscular volumes as well as corpuscular hemoglobin concentrations did not show any significant difference between the two time periods. The MCV average remained steady at 80.3 fL as well as the MCH average at 27.4 pg. The RBC distribution width (RDW-CV), on the other hand, showed a marked decrease from 15.27% to 14.40% in the lockdown period (t= 3.988; p-value= <0.001; F= 1.662; p-value= <0.01).
 |
Table 2 Statistical Analysis for Average Counts of RBC-Related Indices |
White Blood Cell Counts are Decreased During the Lockdown Period
We then compared total WBC counts and the percentage of neutrophil and lymphocyte to the total counts (Figure 3). Total WBC was significantly lower during the lockdown period than in the previous 10 months (Table 3). The average WBC count before the lockdown was 8.423 × 103/µL which dropped to 7.156 × 103/µL during the lockdown. This decrease was determined to be statistically significant (t= 5.581; p-value= <0.001; F= 3.841; p-value= <0.001). However, lymphocyte and neutrophil counts remained on a relatively steady average (Table 3) throughout the year (Figure 4).
 |
Table 3 Statistical Analysis for Average Counts of WBC-Related Indices |
Platelet Counts are Decreased During the Lockdown Period
After that, we looked at Platelet counts, which showed a similar drop during the lockdown (Figure 5). Platelet counts showed an average of 361 × 103/µL before the lockdown (Table 4). This average was significantly lowered to 318 × 103/µL (t= 4.659; p-value= <0.001; F= 2.732; p-value= <0.001). More interestingly, the Platelet distribution width (PDW) was also lowered (Figure 6) from 13.18% to 12.58% (t= 4.439; p-value= <0.001; F= 1.700; p-value= <0.001).
 |
Table 4 Statistical Analysis for Average Counts of Platelet-Related Indices |
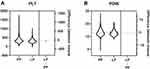 |
Figure 6 Difference between average means of blood indices. (A) PLT: platelets. (B) PDW: platelet distribution width. Abbreviations: PP, period preceding the lockdown; LP, lockdown period. |
Discussion
Many factors are involved in regulating the cellular composition in our blood. These factors come from the environment we share, the food we eat, the atmosphere we breathe, and the pathogens transmitted between individuals in a particular community. The Corona pandemic showed us that many elements are still hidden from our understanding of our bodies’ essential biological functions. One of the immune system’s primary clinical facts is the noticeable increase of cellular and humoral factors upon acquiring an infection. SARS-CoV-2, such as any pathogen, should show similar effects on the parameters of our immune system. However, a question arises about the people who were not infected with the virus or those who have recovered (for more than 30 days or more).
Our study aimed to understand the overall individuals’ immunological status during the lockdown period in Madinah, Saudi Arabia, which lasted for about 5 months, starting from April 2020 until September 2020. People in lockdown practice their daily routines in an entirely different extent than their regular routine which can be clearly observed from our results. Basic daily routines such as physical activity, smoking frequency, type and quantity of food, mental and physiological stress are just a few factors shaping how our body reacts to the external environment.
Here we show that RBC counts along with hemoglobin and hematocrit levels showed a significant increase in our target population during the lockdown period. This increase can be attributed to many factors, most notably smoking. Tobacco smoking is directly linked to an increase in RBC counts and related indices. More importantly, many published studies showed that smoking routine increased considerably among people during the lockdown as a coping mechanism against physical and mental stress.16 Interestingly, the moving average of both MCV and MCH showed no significant deviation throughout the year. This was in agreement with previously published studies showing that smoking had no significant effect on those two hematological parameters.17,18
Moreover, RDW rates were lower during the lockdown period than before the lockdown. RDW represents the uniformity of RBC size, where lower percentages mean that all cells are almost the same size.19 This uniformity in size may indicate that the overall oxygenation requirement levels of those individuals are remarkably similar. Also, many researchers have proposed the use of high RDW as a pathological marker in many disease models.20–25 RDW is an actual representation of volumetric differences between many red blood cell populations including mature red cells, immature red cells and retics. The same technological concept applies to PDW in the context of platelets. Lower RDW might therefore indicate a healthy status, or in other terms, the absence of these pathological conditions. This finding also contradicts the notion of smoking as a detrimental factor of the high levels of RBC, HGB, and HCT.
Immunological status of individuals is very hard to assess. Many biological factors must be considered, such as a healthy diet, physical exercise, proper adherence to medical management, and other factors. The collection of blood specimens from different individuals before and during the lockdown would also generate some statistical bias that needs to be taken into consideration. Recent studies from Saudi Arabia showed that compliance with the medicinal regiment and following a healthy dietary routine were both diminished during the lockdown period.26,27 Our results may shed some light on the impact of reduced physical activity accompanied with high mental stress on individuals’ immune systems by using blood indices as a supporting factor.
Disclosure
The author reported no conflicts of interest for this work.
References
1. Young GP. CBC or not CBC? That is the question. Ann Emerg Med. 1986;15(3):367–371. doi:10.1016/S0196-0644(86)80587-X
2. Barnes P, McFadden S, Machin S, Simson E. The international consensus group for hematology review: suggested criteria for action following automated CBC and WBC differential analysis. Lab Hematol. 2005;11(2):83–90. doi:10.1532/LH96.05019
3. Sandhaus LM, Meyer P. How useful are CBC and reticulocyte reports to clinicians? Am J Clin Pathol. 2002;118(5):787–793. doi:10.1309/CQGG-HY0U-LRKL-GLMP
4. Al-Gwaiz LA, Babay HH. The diagnostic value of absolute neutrophil count, band count and morphologic changes of neutrophils in predicting bacterial infections. Med Princ Pract. 2007;16(5):344–347. doi:10.1159/000104806
5. Todd JK. Childhood infections: diagnostic value of peripheral white blood cell and differential cell counts. Am J Dis Child. 1974;127(6):810–816. doi:10.1001/archpedi.1974.02110250036005
6. Carel RS, Eviatar J. Factors affecting leukocyte count in healthy adults. Prev Med. 1985;14(5):607–619. doi:10.1016/0091-7435(85)90081-7
7. Farhangi MA, Keshavarz S-A, Eshraghian M, Ostadrahimi A, Saboor-Yaraghi -A-A. White blood cell count in women: relation to inflammatory biomarkers, haematological profiles, visceral adiposity, and other cardiovascular risk factors. J Health Popul Nutr. 2013;31(1):58. doi:10.3329/jhpn.v31i1.14749
8. Wang F, Hou M, Wu X, Bao L, Dong P. Impact of enteral nutrition on postoperative immune function and nutritional status. Genet Mol Res. 2015;14(2):6065–6072. doi:10.4238/2015.June.8.4
9. Nishitani N, Sakakibara H. Association of psychological stress response of fatigue with white blood cell count in male daytime workers. Ind Health. 2014;52(6):531–534. doi:10.2486/indhealth.2013-0045
10. Wu D, Wu T, Liu Q, Yang Z. The SARS-CoV-2 outbreak: what we know. Int J Infect Dis. 2020;94:44–48. doi:10.1016/j.ijid.2020.03.004
11. Peltola V, Mertsola J, Ruuskanen O. Comparison of total white blood cell count and serum C-reactive protein levels in confirmed bacterial and viral infections. J Pediatr. 2006;149(5):721–724. doi:10.1016/j.jpeds.2006.08.051
12. Korppi M, Kröger L, Laitinen M. White blood cell and differential counts in acute respiratory viral and bacterial infections in children. Scand J Infect Dis. 1993;25(4):435–440. doi:10.3109/00365549309008524
13. Vieira R, Diniz E, Vaz F. Clinical and laboratory study of newborns with lower respiratory tract infection due to respiratory viruses. J Matern Fetal Neonatal Med. 2003;13(5):341–350. doi:10.1080/jmf.13.5.341.350
14. Park SK. An interpretation on abnormal finding of CBC. Korean J Med. 2010;78(5):531–539.
15. Vetter TR, Mascha EJ. Unadjusted bivariate two-group comparisons: when simpler is better. Anesth Analg. 2018;126(1):338–342. doi:10.1213/ANE.0000000000002636
16. Yach D. Tobacco use patterns in five countries during the COVID-19 Lockdown. Nicotine Tob Res. 2020;22(9):1671–1672. doi:10.1093/ntr/ntaa097
17. Asif M, Karim S, Umar Z, et al. Effect of cigarette smoking based on hematological parameters: comparison between male smokers and non-smokers. Turk J Biochem. 2013;38(1).
18. Nadia M, Shamseldein H, Sara A. Effects of cigarette and Shisha smoking on hematological parameters: an analytic case-control study. Int Multispecialty J Health. 2015;10(1).
19. Evans TC, Jehle D. The red blood cell distribution width. J Emerg Med. 1991;9:71–74. doi:10.1016/0736-4679(91)90592-4
20. Wang C, Zhang H, Cao X, et al. Red cell distribution width (RDW): a prognostic indicator of severe COVID-19. Ann Transl Med. 2020;8(19).
21. Li N, Zhou H, Tang Q. Red blood cell distribution width: a novel predictive indicator for cardiovascular and cerebrovascular diseases. Dis Markers. 2017;2017:1–23. doi:10.1155/2017/7089493
22. Tham T, Bardash Y, Teegala S, Herman WS, Costantino PD. The red cell distribution width as a prognostic indicator in upper aerodigestive tract (UADT) cancer: a systematic review and meta-analysis. Am J Otolaryngol. 2018;39(4):453–458. doi:10.1016/j.amjoto.2018.04.013
23. Pedrazzani C, Tripepi M, Turri G, et al. Prognostic value of red cell distribution width (RDW) in colorectal cancer. Results from a single-center cohort on 591 patients. Sci Rep. 2020;10(1):1–9. doi:10.1038/s41598-020-57721-4
24. Emans ME, van der Putten K, van Rooijen KL, et al. Determinants of red cell distribution width (RDW) in cardiorenal patients: RDW is not related to erythropoietin resistance. J Card Fail. 2011;17(8):626–633. doi:10.1016/j.cardfail.2011.04.009
25. Vayá A, Alis R, Hernández J-L, et al. RDW in patients with systemic lupus erythematosus. Influence of anaemia and inflammatory markers. Clin Hemorheol Microcirc. 2013;54(3):333–339. doi:10.3233/CH-131738
26. Alshareef R, Al Zahrani A, Alzahrani A, Ghandoura L. Impact of the COVID-19 lockdown on diabetes patients in Jeddah, Saudi Arabia. Diabetes Metab Syndr. 2020;14(5):1583–1587. doi:10.1016/j.dsx.2020.07.051
27. Aljohani NE. The effect of the lockdown for the Coronavirus (COVID-19) pandemic on body weight changes and eating habits in Saudi Arabia. J Saudi Soc Food Nutr. 2020;13(1):103–113.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.