Back to Journals » HIV/AIDS - Research and Palliative Care » Volume 13
Dual Contraceptive Use and Associated Factors Among Reproductive Age Group on Antiretroviral Therapy in Borena District, Northeast Ethiopia: A Cross-Sectional Study
Authors Amare G , Cherie N , Mekonen AM
Received 28 October 2020
Accepted for publication 30 December 2020
Published 26 January 2021 Volume 2021:13 Pages 107—114
DOI https://doi.org/10.2147/HIV.S289045
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Bassel Sawaya
Gashaw Amare,1 Niguss Cherie,1 Asnakew Molla Mekonen2
1Department of Reproductive Health and Family Health, School of Public Health, College of Medicine and Health Sciences, Wollo University, Dessie, Amhara, Ethiopia; 2Department of Health Systems Management, School of Public Health, College of Medicine and Health Sciences, Wollo University, Dessie, Amhara, Ethiopia
Correspondence: Asnakew Molla Mekonen
Wollo University, Dessie, Ethiopia
Tel +251921529181
Email [email protected]
Background: Dual contraceptive method use is defined as the use of any modern contraceptive method with a condom for the reduction of mother-to-child transmission of HIV and sexually transmitted infections between sexual partners. The goal of this study was to assess the proportion and factors associated with dual contraceptive use among reproductive age women on antiretroviral therapy in Borena district, Northeast Ethiopia.
Objective: To assess the proportion of dual contraceptive use and associated factors among the reproductive age women on antiretroviral therapy in Borena district, Northeast Ethiopia.
Methods: An institutional-based cross-sectional study was conducted among HIV positive reproductive age group women on antiretroviral therapy in Borena district from February 1 to March 1, 2020. A systematic random sampling technique was used to include 417 study participants. A structured interviewer-administered questionnaire was used to collect the data. A binary logistic regression model was used to identify the factors associated with dual contraceptive use. Odds ratio with 95% confidence interval (CI) and P-value were calculated to assess the strength of association.
Results: The results showed that 19.4% of the HIV positive reproductive age group on antiretroviral therapy were using dual contraceptive method. Urban area (AOR=3.66, 95% CI=1.66– 8.09), educated to secondary education and above (AOR=3.54, 95% CI=1.29– 9.76), those who have no desire to have a child (AOR=4.41, 95% CI=2.66– 7.59), those with partners whose HIV status was negative (AOR=4.96, 95% CI=2.66– 12.02) and those with partners whose HIV status was positive (AOR=2.45, 95% CI=1.25– 4.81) were more likely to use the dual contraception method.
Conclusion: This study showed that the proportion of dual contraceptive use was found to be low in accordance with the WHO recommendation. Therefore increased awareness on the advantages of dual contraception and knowing partner’s HIV status is important.
Keywords: dual contraceptive use, antiretroviral therapy, Borena district, Ethiopia
Introduction
Worldwide, nearly 37.9 million people were living with HIV/AIDS in 2018 and, in 2017, around 1.8 million people were newly infected with HIV.1,2 Obviously, there was declining HIV incidence in many regions of the world and a 33% reduction in AIDS-related deaths between 2010 and 2018. However, a significant global HIV burden still remains, with 38 million people living with HIV and 1.7 million diagnosed with new HIV infections in 2018.3 Besides, HIV/AIDS remains the most common cause of death in sub-Saharan Africa and in 2017, 71% of the world’s HIV-positive population lived there.4,5
Psychosocial, economic, and physical burdens of HIV/AIDS on individual females and countries remain a challenge.6 More than 2 million HIV positive women become pregnant every year due to low dual contraceptive utilization and unsafe sex practices, among them, 600,000 die due to pregnancy-related complications.7 According to 2019 Ethiopian HIV facts, there were 14,843 newly infected people, 669,236 people living with HIV, and 11,546 people died from AIDS related illness.8
Dual contraceptive method is the utilization of any modern contraceptive method along with male or female condoms which can decrease sexually transmitted diseases and unwanted pregnancy.9,10 Dual contraceptive utilization can has a paramount contribution for reducing unwanted pregnancy and sexually transmitted infections for women on ART.11 However, utilization of dual contraceptive is low in many developing countries including Ethiopia.12,13 Studies done in sub-Saharan Africa examined low dual contraceptive utilization among HIV positive women.11,14,15 Moreover, many studies done in Ethiopia investigated that dual contraceptive utilization among reproductive age group women is low. For example, studies have shown that in Tigray (13.8%), Gondar (13.2%), and Oromia, Southwest Ethiopia (19.8%) women on ART used dual contraceptive methods.9,16–19
Different studies revealed that there are enabling and impeding factors for dual contraceptive utilization. Women aged 15–24 years, urban residence, disclosing HIV status to a partner, marital status, higher educational level, employed women, discussion with contraceptive provider, received HIV counseling, and having a higher CD4 cell count were more likely to utilize dual contraceptive methods.9,15–18,20–24
Currently, in Ethiopia, HIV transmission is still high and many HIV positive reproductive age group women are still facing unintended pregnancy.8 This directly related to risk of pregnancy-related complications, mother-to-child transmission of HIV, and transmission of HIV to their sexual partners due to low dual contraceptive utilization. Even though dual contraceptive utilization is useful for the reproductive age group women on ART in Ethiopia, there is limited evidence to describe the current utilization of dual contraceptive methods, especially in our study area of Borena district.
Therefore, the results of this study might be helpful by providing suggestions regarding the proportion of dual contraceptive use and associated factors among the reproductive age group of women on ART in Borena district, Northeast Ethiopia. The finding may also be important to policy makers and planners to develop projects and reforms to reach target groups.
Materials and Methods
An institutional based cross-sectional study was conducted from February 1–May 1, 2020, in Borena district public health facilities with ART clinics. Borena district is located in the South Wollo zone, Amhara regional state, and 469 km away from Addis Ababa the capital city of Ethiopia. The district has a total population of 186,173 and 52% were females. Mekane-Selam health center and Mekane-Selam primary hospital were two government institutions that provided services related to ART for 873 clients.25
The study populations were all HIV positive reproductive age groups (15–49) who had follow-up in the ART clinics of Borena district during the study period. But women who had a history of current pregnancy and hearing difficulties were excluded. The sample size was calculated by using a single population proportion formula by taking the assumptions of proportion of dual contraception use (P=59.5%), 95% confidence interval (CI), 5% margin of error (d), and 10% non-response rate which yielded 417 participants.21
A systematic random sampling technique was applied to select the study population. Study participants were selected based on the proportion to the health facilities ART user women. To allocate the study subjects proportionally, first, the average number of clients who visit the health facilities during the data collection period was estimated and the total number of women on ART determined. Then, the samples were proportionally taken from two health facilities. The sampling interval was determined by dividing the total number of women who were visiting health facilities by calculated sample size. After being determined, first study subject by lottery method; study subjects were selected from, sampling frame.
The dependent variable was dual contraceptive use. The independent variables were socio-demographic and economic variables (age, marital status, religion, occupational status, educational status, residence, ethnicity, partner educational statues, partner occupation, and family income), sexual and reproductive factors (knowledge on contraceptive methods, number of live children, desire to have a child, partner desire to have a child, and HIV status of children), and clinical and HIV related factors (CD4 count, STI history, disclosure statues, number of sexual partners, partner's HIV status, duration on ART, and WHO clinical staging).
Modern contraceptive methods include sterilization, pills, IUD, injectable, implants, and male and female condoms (excluding lactational amenorrhea, rhythm, and withdrawal).10,13 Respondents who had heard of at least one contraceptive method had knowledge of contraceptive methods.13,26 Dual contraceptive method is the utilization of any modern contraceptive method along with male or female condoms for the last months prior to the study.9,10
The pre-tested structured interviewer-administered questionnaire was used. It was prepared in English, then translated to Amharic (the local language), and then back-translated to English to check its consistency. The interview and data extraction was conducted by four female clinical nurses (two from Mekane-Selam primary hospital and two from Mekane-Selam health center). A BSc holder nurse was recruited for supervision. A medical record was used to extract ART history, and clinical data (WHO clinical stage, STI history, CD4 cell count, and duration on ART). The data collectors and supervisors were trained for 2 days regarding the objectives of the study, the technique of the interview, and the ethical concerns of the study. The principal investigators were closely following the day-to-day data collection process and ensured completeness and internal consistency of the collected data. The supervisors were also followed periodically to monitor the process of data collection. A pre-test was done on 50 HIV-positive women at Hidar 11 primary hospitals and the questionnaire was revised accordingly.
Data Processing and Analysis
The data were collected, coded, and entered into Epi-Info 7, then exported to SPSS version 23 for analysis. Summary statistics of variables such as mean, the standard deviation, and median was calculated. Both bi-variable and multivariable binary logistic regression analyses were computed to identify factors associated with dual contraceptive use. The odds ratio with 95% CI was computed to ascertain the association between the independent variables and the dependent variable. Variables that have a P-value<0.25 at bi-variable analysis were included in multivariable logistic regression by a backward stepwise method to control possible confounding factors. A variable P-value<0.05 was considered as having a statistically significant association with the dependent variable.
Ethical Considerations
Ethical clearance was obtained from the Institutional Review Board (IRB), Wollo University, College of medicine and health sciences, and School of public health. A letter of permission was obtained from Mekane-Selam health center and Mekane-Selam primary hospital. After the approval of the ethical issue, the data collectors were trained about how to maintain the ethical aspect of the research process and the data collection procedure. The study subjects were informed about the purpose of the study, their right to refuse, and to withdraw at any time. Informed written consent was obtained from each participant before the data collection. For participants less than 18 years old, consent was taken from their parents/guardian. The confidentiality of the data was kept by avoiding personal identifier and kept in a safe place. The study was conducted in accordance with the Declaration of Helsinki, 2008.
Results
Socio-Demographic and Economic Characteristics of Participants
A total of 417 reproductive age group women on ART participated in this study with a response rate of 98.8%. The majority of the study participants were rural dwellers (72.1%), and married (88.6%), The mean age of the study participants was 32.2 (±7.02). Only 18.4% of women were above secondary education. About less than half, 146 (35.4%) were housewives (Table 1).
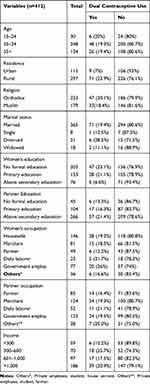 |
Table 1 Socio-Demographic and Economic Characteristics of HIV Positive Reproductive Age Group Women’s are on ART in Borena District, Northeast Ethiopia, 2020 (n=412) |
Sexual and Reproductive Related Characteristics of Study Participants
The majority of the participants (98.8%) had known at least one type of modern contraceptive method. The most known type of contraceptive method was condom, at 383 (94.1%). The majority of the participants (85.4%) had ever used modern contraceptive methods. Out of them, 51.4% had never used dual contraceptive methods (Table 2).
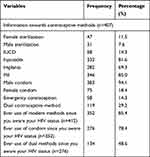 |
Table 2 Sexual and Reproductive Characteristics of HIV Positive Reproductive Age Group Women on ART in Borena District, Northeast Ethiopia, 2020 (n=412) |
Clinical and HIV Related Factors Related Characteristics of Study Participants
The majority of the study participants (404, 98.1%) had single sexual partners and 15 (3.6%) had a history of sexually transmitted infections (STI). Among participants who had a history of STI, seven (46.7%) were not treated. The majority of study participants (351, 85.2%) knew the HIV status of their partner, and 258 (62.6%) study participants had HIV positive partners.
Among study participants, 79 (19.2%) had not disclosed their HIV status to their partners. The reasons for not disclosing were fear of stigma and discrimination, at 27 (34.2%), fear of divorce, at 26 (32.9%), and fear of violence by partner, at 26 (32.9%). From study participants, 362 (87.9%) had awareness of the importance of disclosure. Of the participants, 372 (90.3%) were above 1 years duration on ART, 145 (35.2%) had a CD4 count >350, and 148 (35.9%) were stage four clinical staging.
Current Dual Contraceptive Use
The study revealed that 80 (19.4%) of the study participants had used dual contraceptives in the past 1 month prior to the study. The main reason for dual contraceptive method use was to prevent unintended pregnancy (38, 47.5%). The common method along with condoms (43, 53.8%) was injectables. More than half of the participants (251, 60.9%) were currently using modern contraceptive methods (Table 3).
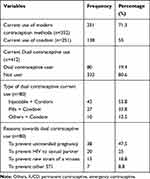 |
Table 3 Current Dual Contraception Use Among HIV Positive Reproductive Age Group Women’s on ART in Borena District, Northeast Ethiopia, 2020 (n=412) |
Factors Associated with Dual Contraceptive Utilization
Educational status, women’s desire of having a child, residence, and HIV status of the partner were significant factors associated with dual contraceptive use.
Participants who were educated to secondary education level and above (AOR=3.54, 95% CI=(1.29–9.76) were 3.54-times more likely to use dual contraception when compared to those who had no formal education. Similarly, women who were urban residents (AOR=3.66, 95% CI=1.66–8.09) were 3.66-times more likely to utilize dual contraceptive methods compared to rural residents. Participants who had a desire of having a child (AOR=4.41, 95% CI=2.66–7.59) were 4.41-times more likely to utilize dual contraceptive methods as compared to those who had no desire of having a child. When compared to participants whose partners HIV status was unknown, participants with a partner known to be HIV status negative (AOR=4.96, 95% CI=(2.66–12.02) and positive (AOR=2.45, 95% CI=1.25–4.81) were 4.96- and 2.45-times more likely to utilize dual contraceptive methods, respectively (Table 4).
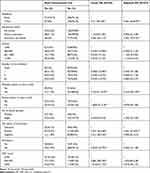 |
Table 4 Factors Associated with Dual Contraceptive Use Among HIV Positive Reproductive Age Group Women’s on the ART in Borena District, Northeast Ethiopia, 2020 (n=412) |
Discussion
The study aimed to assess the proportion of dual contraceptive use and its associated factors among the reproductive age group women on ART in Borena district, Northeast Ethiopia.
The study revealed that 19.4% (95% CI=15.8–23.1) of the reproductive age group women on ART used dual contraceptive methods in the last month prior to the study. The proportion of dual contraceptive utilization in this study was consistent with the studies done in South Ethiopia (19.8%), Gimbie (17%), and in Lusaka Zambia (17.7%).15,18,27 But it is higher compared to the results of studies conducted in Gondar (13.2%) and Tigray (15.7%).17,24 This difference could be the time variation of the studies, study setting, socio-demographic, and cultural characteristics of the study participants. Additionally, it is lower than the studies done in Oromia (59.5%), Fitche (32%), Tanzania (33%), and Thailand (29.6%).9,13,21,26 The inconsistency among study results might be due to socio-demographic differences of the study population and the presence of quality family planning and ART services in Tanzania and Thailand.
The factors identified which were significantly associated with dual contraceptive use were residence, educational status, desire of having a child, and HIV status of the partner. The study revealed that urban resident women more likely use dual contraceptive method. The evidence is supported by a study done in Gondar, Ethiopia.22 This can be explained by urban resident women being more exposed to health information and media outlets. This empowers them to have informed decision-making power and an easy discussion with their partners about contraceptive methods.
Utilization of dual contraceptive was higher among women who were educated to secondary education and above. This was supported by the study done in Adewa, Ethiopian demographic and health survey, and Brazil.12,16,28 This could be explained by highly educated women appreciating the advantage of dual contraceptive utilization, knowledge on HIV, and knowledge on STI, and risk sexual practices.
The study also showed that women who had no future desire of having a child significantly increased dual contraceptive utilization. The finding is supported by studies conducted in Tigray and Fitche.21,24 Since women with HIV/AIDS had low immunity resistance, pregnancy might be complicated and the outcome will be bad. Therefore, women who had this understanding might not be pregnant. This implies not a desire to have a child, which contributes paramount women to utilizing dual contraceptive methods.
The study also revealed knowing partners’ HIV status increased dual contraceptive methods utilization compared with HIV status was unknown. This was supported by the study done in Tigray.24 This might be due to the information women have mutual accepting about the advantage of dual contraceptive utilization. Additionally, knowing HIV status nurtures open discussion with partners about safe sexual practice.
This study was conducted with certain limitations. The first is related to the cross-sectional design which simultaneously evaluates variables of the effect of interest and their associated factors. Second, the study is institutional-based, the results of this study may not generalize to the reproductive age group women attending ART centers outside the study area. In addition, since the questionnaire covers sensitive issues, there might be exposure to social desirability bias.
Conclusion
The proportion of dual contraceptive was found to be low in this study compared with World Health Organization (WHO) recommendation. Educational status, women’s desire of having a child, residence, and HIV status of the partner were significant factors associated with dual contraceptive utilization. Hence, providing health education about the importance of dual contraceptive utilization is helpful. Moreover, strengthening counseling services in health institutions about the importance of disclosing HIV status to sexual partner is helpful for women on ART.
Data Sharing Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Acknowledgement
We deeply express our gratefulness to the Wollo University, the study participants, data collectors and other individuals or organizations that has participated directly or indirectly into the study.
Funding
The authors received no specific funding for this work.
Disclosure
The authors report no conflicts of interest for this work.
References
1. FMOH. National family planning guideline. 2012.
2. Narasimhan M, Yeh PT, Haberlen S, Warren CE, Kennedy CE. Integration of HIV testing services into family planning services: a systematic review. Reprod Health. 2019;16(1):61. doi:10.1186/s12978-019-0714-9
3. Karim SSA, Baxter C. HIV incidence rates in adolescent girls and young women in sub-Saharan Africa. Lancet Global Health. 2019;7(11):e1470–e1. doi:10.1016/S2214-109X(19)30404-8
4. James SL, Abate D, Abate KH, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392(10159):1789–1858.
5. Nweze J, Emmanuel E, Nweze E. HIV/AIDS in sub-Saharan Africa: current status, challenges and prospects. Asian Pac J Trop Dis. 2017;7:239–256. doi:10.12980/apjtd.7.2017D6-366
6. WHO. AIDS epidemic update. 2007.
7. WHO. Preventing HIV and unintended pregnancies: strategic framework 2011–2015. Inter-agency Task Team; 2012.
8. Office FHAPaC. Ethiopian HIV facts. 2020.
9. Gudisa DBDaT. Dual contraceptive use and associated factors among women living with HIV attending art clinics in West Zone Health Facilities Oromia, Ethiopia. EC Gynaecol. 2019;8:4.
10. Chakrapani V, Kershaw T, Shunmugam M, Newman PA, Cornman DH, Dubrow R. Prevalence of and barriers to dual-contraceptive methods use among married men and women living with HIV in India. Infect Dis Obstet Gynecol. 2011;2011:1–8.
11. Mutiso S, Kinuthia J, Qureshi Z. Contraceptive use among HIV infected women attending comprehensive care centre. East Afr Med J. 2008;85(4):171–177. doi:10.4314/eamj.v85i4.9641
12. Tsuyuki K, Barbosa RM, de Araujo Pinho A. Dual protection and dual methods in women living with HIV: the Brazilian context. J Sex Transm Dis. 2013;2013:1–8. doi:10.1155/2013/540789
13. Munsakul W, Lolekha R, Kowadisaiburana B, et al. Dual contraceptive method use and pregnancy intention among people living with HIV receiving HIV care at six hospitals in Thailand. Reprod Health. 2015;13(1):8. doi:10.1186/s12978-016-0123-2
14. Lawani LO, Onyebuchi AK, Iyoke CA. Dual method use for protection of pregnancy and disease prevention among HIV-infected women in South East Nigeria. BMC Women’s Health. 2014;14(1):39. doi:10.1186/1472-6874-14-39
15. Chibwesha CJ, Li MS, Matoba CK, et al. Modern contraceptive and dual method use among HIV-infected women in Lusaka, Zambia. Infect Dis Obstet Gynecol. 2011;2011:2011. doi:10.1155/2011/261453
16. Teklu T, Davey G. Which factors influence North Ethiopian adults’ use of dual protection from unintended pregnancy and HIV/AIDS? Ethiop J Health Dev. 2008;22(3).
17. Reta MM, Tessema GA, Shiferaw G. Prevalence of dual contraceptive use and associated factors among HIV positive women at University of Gondar Hospital, Northwest Ethiopia. BMC Res Notes. 2019;12(1):36. doi:10.1186/s13104-019-4053-2
18. Erashi MW, Tesso FY, Beyene TT. Dual-contraceptive method utilization and associated factors among HIV positive women attending art clinic in Gebretsadik Shawo Hospital, SNNPR, South West Ethiopia. Women’s Health Care. 2015;4:6.
19. Chakrapani V, Kershaw T, Shunmugam M, Newman PA, Cornman DH, Dubrow R. Prevalence of and barriers to dual-contraceptive methods use among married men and women living with HIV in India. Infect Dis Obstet Gynecol. 2011;2011:376432. doi:10.1155/2011/376432
20. Reynolds HW, Janowitz B, Wilcher R, Cates W. Contraception to prevent HIV-positive births: current contribution and potential cost savings in PEPFAR countries. Sex Transm Infect. 2008;84(Suppl2):ii49–ii53. doi:10.1136/sti.2008.030049
21. Demissie DB, Girma T, Abdissa G. Dual contraceptive utilization and associated factors among people living with HIV attending ART clinic in Fitche Hospital, Ethiopia. J Health Med Nurs. 2015;2015:20.
22. Abay F, Yeshita HY, Mekonnen FA, Sisay M. Dual contraception method utilization and associated factors among sexually active women on antiretroviral therapy in Gondar City, northwest, Ethiopia: a cross sectional study. BMC Women’s Health. 2020;20(1):26. doi:10.1186/s12905-020-0890-3
23. Mulongo AM, Lihana RW, Githuku J, Gura Z, Karanja S. Factors associated with uptake of dual contraception among HIV-infected women in Bungoma County, Kenya: a cross-sectional study. Pan Afr Med J. 2017;28(Suppl 1). doi:10.11604/pamj.supp.2017.28.1.9289
24. Gebrehiwot SW, Azeze GA, Robles CC, Adinew YM. Utilization of dual contraception method among reproductive age women on antiretroviral therapy in selected public hospitals of Northern Ethiopia. Reprod Health. 2017;14(1):125. doi:10.1186/s12978-017-0390-6
25. Organization WH. PMTCT strategic vision 2010–2015: preventing mother-to-child transmission of HIV to reach the UNGASS and Millennium Development Goals: moving towards the elimination of paediatric HIV, December 2009. 2010.
26. Damian DJ, George JM, Martin E, Temba B, Msuya SE. Prevalence and factors influencing modern contraceptive use among HIV-positive women in Kilimanjaro region, northern Tanzania. Contracept Reprod Med. 2018;3(1):7. doi:10.1186/s40834-018-0060-2
27. Polisi A, Gebrehanna E, Tesfaye G, Asefa F. Modern contraceptive utilization among female ART attendees in health facilities of Gimbie town, West Ethiopia. Reprod Health. 2014;11(1):30. doi:10.1186/1742-4755-11-30
28. (CSA) CSA. Ethiopian demographic and health survey (EDHS). 2016.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
