Back to Journals » International Journal of General Medicine » Volume 9
Diagnostic errors in older patients: a systematic review of incidence and potential causes in seven prevalent diseases
Authors Skinner T, Scott I , Martin J
Received 20 September 2015
Accepted for publication 15 February 2016
Published 20 May 2016 Volume 2016:9 Pages 137—146
DOI https://doi.org/10.2147/IJGM.S96741
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Thomas R Skinner,1 Ian A Scott,2,3 Jennifer H Martin3,4
1Department of Internal Medicine, Sunshine Coast Health Service District, Nambour Hospital, Nambour, QLD, Australia; 2Internal Medicine and Clinical Epidemiology, Princess Alexandra Hospital, Woolloongabba, QLD, Australia; 3Southern School of Medicine, University of Queensland, Brisbane, QLD, Australia; 4School of Medicine and Public Health, University of Newcastle, Newcastle, NSW, Australia
Background: Misdiagnosis, either over- or underdiagnosis, exposes older patients to increased risk of inappropriate or omitted investigations and treatments, psychological distress, and financial burden.
Objective: To evaluate the frequency and nature of diagnostic errors in 16 conditions prevalent in older patients by undertaking a systematic literature review.
Data sources and study selection: Cohort studies, cross-sectional studies, or systematic reviews of such studies published in Medline between September 1993 and May 2014 were searched using key search terms of “diagnostic error”, “misdiagnosis”, “accuracy”, “validity”, or “diagnosis” and terms relating to each disease.
Data synthesis: A total of 938 articles were retrieved. Diagnostic error rates of >10% for both over- and underdiagnosis were seen in chronic obstructive pulmonary disease, dementia, Parkinson’s disease, heart failure, stroke/transient ischemic attack, and acute myocardial infarction. Diabetes was overdiagnosed in <5% of cases.
Conclusion: Over- and underdiagnosis are common in older patients. Explanations for overdiagnosis include subjective diagnostic criteria and the use of criteria not validated in older patients. Underdiagnosis was associated with long preclinical phases of disease or lack of sensitive diagnostic criteria. Factors that predispose to misdiagnosis in older patients must be emphasized in education and clinical guidelines.
Keywords: older patient, elderly, overdiagnosis, underdiagnosis, misdiagnosis
Background
Accurate diagnosis is critical in older people (defined here as persons aged ≥65 years) to avoid unnecessary investigations and treatments and their associated costs and harm.1 Diagnostic errors are relatively common when compared with other types of errors relating to medications and surgical procedures.2–4 Many older patients have more comorbidities requiring diagnosis, meaning they may be more susceptible to misdiagnosis.5 Misdiagnosis not only endangers the health of older patients but also incurs opportunity costs for health care systems due to misused clinical interventions and care of iatrogenic illness.5–7
Older populations may be more vulnerable to diagnostic error for reasons that relate to both patient and clinician.8 Older persons may attribute symptoms to normal aging, and not report them, and doctors may focus unduly on clinical clues suggesting particular diseases while discounting opposing clues.9 Commonly used diagnostic criteria for specific diseases derived and validated in younger populations may not apply to older individuals.6,10
We undertook a systematic review to determine rates of over- and underdiagnosis of several diseases commonly encountered in older populations and to identify associated predisposing factors.
Data sources and study selection
Sixteen conditions were initially considered for inclusion in this review based on their reported prevalence and level of disease burden in older patients.11,12 These comprised dementia, chronic obstructive pulmonary disease (COPD), heart failure (HF), Parkinson’s disease (PD), stroke/transient ischemic attack (TIA), acute myocardial infarction (AMI), diabetes, osteoarthritis (OA), obstructive sleep apnea, peripheral arterial disease (PAD), gastroesophageal reflux disorder (GERD), epilepsy, hypertension (HTN), major depression, osteoporosis, and renal insufficiency.
Literature searches were undertaken by an author (TS) in July 2011 and repeated in September 2013 and May 2014 to ensure inclusion of newly published articles. The initial search gathered cohort studies, cross-sectional studies, or systematic reviews of studies assessing diagnostic errors, irrespective of disease or age, published in Medline in the last 20 years. The search used key search terms relating to diagnostic error, misdiagnosis, accuracy, or validity of diagnosis as well as MeSH search terms in both English and American formats. This group of articles was then searched for literature relating to the 16 target conditions using keywords and MeSH terms relevant to the conditions (Table 1). Retrieved studies’ reference lists were also examined for further articles addressing misdiagnosis in older patients.
  | Table 1 Search strategy and results (May 2014) |
Selected studies were those published in English, in which ≥50% of study participants were aged ≥65 years and in which quantitative data on diagnostic rates, as measured using reference standards, could be obtained directly from the published study or by contact with study authors. Where articles did not report data specific to older cohorts, authors were contacted with a request for a subset of data including only subjects ≥65 years of age. Study selection and data collection were undertaken by one author (TS) and confirmed independently by the two remaining authors in joint discussion.
Overdiagnosis was measured using 1 − specificity (1−Sp) and 1 − positive predictive value (1−PPV), while underdiagnosis was measured using 1−sensitivity (1−Sn) or 1 − negative predictive value (1−NPV) (Figure 1). Misdiagnosis was considered clinically significant when any of these values was ≥10%. The methodological quality of each study was evaluated for risk of bias and applicability using the quality assessment tool for diagnostic accuracy (QUADAS-2) (Supplementary materials), with those studies displaying higher quality given more emphasis in the qualitative reviews of each condition.
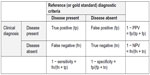  | Figure 1 Explanation of overdiagnosis and underdiagnosis rate calculation. |
Data synthesis
The final search for articles relating to diagnostic error in May 2014 yielded 5,288 titles with abstracts. This pool contained 938 articles pertaining to the 16 target conditions. On reviewing article abstracts, 84 assessed diagnostic validity and were considered relevant to this review. Perusal of bibliographies uncovered a further ten articles, totaling 94 reports for which full-text versions were retrieved. Of these, 22 did not report separate data for older patients, and enquiries were made to corresponding authors, of whom five provided data specific for older patients before expiry of a 2-week deadline.
Sleep disorders, OA, PAD, GERD, epilepsy, HTN, osteoporosis, and renal insufficiency were removed from the list of conditions due to the absence of any studies examining diagnostic accuracy in older patients that met our selection criteria. A meta-analysis from 2010 examining late-life depression was judged by the authors to have adequately addressed our research question for this condition, and it was removed from our condition list as no subsequent studies were found.9 In total, 46 studies pertaining to COPD, dementia, PD, HF, stroke/TIA, AMI, and diabetes involving 112,669 subjects constituted the final analysis (Figure 2). A summary of data abstracted from each included study is provided in the “Supplementary materials” section.
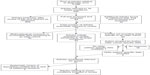  | Figure 2 Article selection flowchart. |
An attempt at meta-analysis of all included studies was considered but subsequently deemed impractical due to the marked heterogeneity in the raw data as a result of widely differing study populations, settings, study designs, choice of reference diagnostic criteria, and analytic methods.
Therefore, meta-analysis was restricted to data pooled from subgroups of five or more similarly designed studies for each condition, which employed the same measures of diagnostic accuracy and comparable clinical diagnostic criteria and reference standards. Although not specified in the original protocol, due to the poor quality of the studies, the decision was made to restrict meta-analysis to those studies where the forest plot of diagnostic accuracy, the funnel plot of the diagnostic accuracy versus the study size, and a plot of diagnostic accuracy versus the confidence interval (CI) range suggested the absence of significant heterogeneity or bias.
Disease-specific results
Chronic obstructive pulmonary disease
Of the 12 articles relating to COPD, ten assessing overdiagnosis using current reference criteria revealed 1−Sp results between 11.7% and 28.7% and 1−PPV results between 8.5% and 52.6%.13–22 Eight studies assessing overdiagnosis met our criteria for attempting meta-analysis. However, on reviewing the forest plot of PPVs with 95% CI and the funnel plots of PPVs against CI range and participant numbers to exclude bias, no consistent relation was found and no further meta-analysis was attempted (Figure 3). Restricting the analysis to the four highest quality studies, 1−PPV varied from 19.6% to 42.2%.14,17,19,20
  | Figure 3 PPV with 95% CIs for COPD subgroup. |
Failure to perform spirometry, improper spirometry technique, incorrect interpretation of the results, and atypical presentations appeared to contribute to overdiagnosis.15,19 Prebronchodilator spirometry use led to COPD misdiagnosis in patients who had asthma in two separate studies (1−PPV of 11% and 20%).13,14 There was also a positive relationship between the number of comorbidities and rates of COPD overdiagnosis.13,20
Three studies assessed the underdiagnosis of COPD with 1−Sn ranging from 35.6% to 71.4% and 1−NPV ranging from 27.8% to 51.8%.16,21,22 These studies assessed populations with risk factors for COPD and likely overestimated the degree of underdiagnosis in the general population. The highest quality study determined that in patients 65 years or older with symptoms of, risk factors for, and treatment consistent with COPD, the disease was undiagnosed in ~35% of cases.21
In defining COPD, the current Global Initiative for Chronic Obstructive Lung Disease (GOLD) guidelines use a fixed postbronchodilator cutoff value of the ratio of forced expiratory volume in 1 second (FEV1) to forced vital capacity (FVC) of <0.70. An alternative definition has been suggested using values below the 95th percentile (or <5% lower limit of normal) of the distribution of FEV1/FVC values within older populations. When compared with the lower limit of normal, the fixed cutoff criteria resulted in 1−PPVs of 27%–29% in a large high-quality study.10 In another study of 71 asymptomatic nonsmoking participants aged >70 years, the GOLD criteria labeled 35% of participants as having COPD, increasing to 50% in those >80 years, results considered clinically implausible.6 These studies suggest that the current reference criteria for COPD diagnosis may be inappropriate in older patients.
The effect of increasing age on diagnostic accuracy was mixed in four high-quality studies.13,15,19,20
Dementia
Ten studies assessed diagnostic validity, including one systematic review. Two studies investigated dementia as a broad category, while six looked at Alzheimer’s disease (AD) and four at dementia with Lewy bodies (DLB). Eight studies used neuropathological reference criteria, with the remaining two using clinical criteria.
Studies assessing overdiagnosis showed 1−Sp ranging from 0% to 50% and 1−PPV from 16% to 40%.23–31 A single study assessed dementia in general and calculated a 1−Sp of 14%, using clinical diagnostic criteria.29 Overdiagnosis of AD was assessed in six studies,23–25,27,28,30 the most rigorous being a neuropathological study, which revealed a 1−Sp of between 29.2% and 40.5% and a 1−PPV between 16.7% and 37.8%.23 All four studies assessing overdiagnosis in DLB had significant bias and applicability concerns.26–28,31 Notwithstanding, overdiagnosis of DLB appeared less prevalent compared to other types of dementia, with three studies showing a 1−Sp of <5%.26–28
Overdiagnosis was more common in patients with milder disease and more comorbidities, with the exception of DLB.28,30
Underdiagnosis of dementia appears more prevalent.23–28,31,32 A systematic review of eight studies of the underdiagnosis of dementia in the primary care setting estimated a 1−Sn of 51% (0%–91%).32 Underdiagnosis of AD was assessed in five further studies. 1−Sn was highly variable from 4% to 75%, with 1−NPV from 6.5% to 30%.23–25,27,28 Four studies examining underdiagnosis in DLB calculated 1−Sn from 71% to 100% and 1−NPV from 10% to 11%.26–28,31 Patients with poor access to health care, lower socioeconomic status, and lower levels of education were more likely to be underdiagnosed.32 Underdiagnosis was also prevalent at the extremes of age, attributed in the older population to the increasing prevalence of HTN, diabetes, and vascular disease.24,32
Parkinson’s disease
Nine studies explored the validity of a diagnosis of PD, all assessing overdiagnosis, with five also investigating underdiagnosis. In relation to overdiagnosis, four studies compared clinical diagnoses with clinicopathological reference criteria, reporting 1−Sp of between 1% and 12%.33–36 The remaining five studies used specialist clinical assessments as reference criteria, against which clinical diagnoses made by nonspecialists demonstrated 1−Sp between 15% and 27%.37–41 Specialist diagnosis was consistently associated with less overdiagnosis in three studies, which demonstrated a 1−PPV of 1.4%–25% for specialists and 27%–47% for nonspecialists.35,37,39 Similar results were found in a more recent study comparing the clinical diagnosis of a specialist with results of FP-CIT SPECT (N-u-fluoro-propyl-2b carbomethoxy-3b-(4-iodophenyl) nortropane single photon emission computed tomography) scanning in 38 patients which reported a 1−Sp of 15%–21% and 1−PPV of 17%–26%.38
Overdiagnosis was more prevalent in patients with no bradykinesia, rigidity, resting tremor, hypomimia, or monotonous speech, as well as less frequent falls, less severe disease, and higher scores on cognitive testing.37 Patients receiving low doses of anti-Parkinson medications, whose dose had not increased in 3 years, who had been on monotherapy for ≥5 years, and who had neither a documented response to medications nor clinical progression were more commonly overdiagnosed.37,39 Patients diagnosed and followed up by a specialist were less susceptible to overdiagnosis.35,37 Early dementia and secondary parkinsonism were the most common etiologies misdiagnosed as PD.34
Five studies assessed underdiagnosis, with two clinicopathological studies reporting 1−Sn between 9% and 50% and 1−NPV between 1% and 10%.35,36 Another study using a validated clinical reference criteria demonstrated a similar 1−Sn of 7% versus 27% for specialists and nonspecialists, respectively.37 The FP-CIT SPECT scanning study reported 1−Sn between 20% and 47%, reflecting the high sensitivity of this imaging technique in early PD.38
Factors associated with underdiagnosis included lower disease severity, shorter disease duration, living in a nursing home, and the absence of typical complications of PD and/or its treatment, such as depression and dyskinesia.37
Increasing age was shown to be associated with higher rates of both over- and underdiagnosis.40
Heart failure
Seven studies explored the validity of a diagnosis of HF. Six studies assessing overdiagnosis of HF reported 1−Sp between 0.7% and 16.5% and 1−PPV between 2% and 64%.8,42–47 While these studies met our criteria for attempted meta-analysis, this was deemed not feasible after reviewing the forest plot of PPVs with 95% CI and the funnel plots of PPVs against CI range and participant numbers to exclude bias (Figure 4).
  | Figure 4 PPV with 95% CIs for heart failure subgroup. |
Those who were diagnosed in a hospital setting showed less overdiagnosis, with 1−PPVs of 1.9%–27.3% compared to 59.1%–63.8% for those diagnosed elsewhere.42–47 Nursing home residents had a 1−PPV of 59% compared to 19% in a similarly designed study of community-dwelling patients.45,47 Comorbidities, particularly atrial fibrillation, COPD, and obesity, were more prevalent among falsely diagnosed cases.42,45
Underdiagnosis was assessed in four studies in which 1−Sn was 17.1% in one autopsy-based study8 and much higher (62.5% and 70.6%) in two high-quality studies45,47 with guideline-endorsed clinical and echocardiographic reference criteria.
Increasing age was associated with poorer diagnostic accuracy, attributed to atypical presentations, higher number of comorbidities, and older patients being less likely to receive echocardiograms.8,43
Stroke and TIA
Three studies assessed misdiagnosis of strokes and TIAs; two were high quality and assessed overdiagnosis.48–50 These studies compared the clinical diagnoses of stroke or TIA recorded in patient registries and emergency department notes with diagnoses made by experts upon review of all available clinical data. 1−PPV of 20%–24% was reported for stroke and 32%–62% for TIA.
Gradual onset, nonspecific symptoms, and past history of unexplained transient neurological syndromes were significantly more common in cases falsely diagnosed as TIA.49 The difficulty in diagnosing these conditions was highlighted by a disagreement rate between experts of 6% and 11% for stroke and TIA, respectively.48
Underdiagnosis was assessed in a single study with significant bias and applicability concerns. The combined 1−Sn for stroke and TIA was 9%, with underdiagnosis occurring more commonly in cases that presented without language or motor deficits.50
The effect of increasing age on the extent of misdiagnosis was mixed.48,49
Acute myocardial infarction
Four studies were included which assessed misdiagnosis of AMI. Two assessed underdiagnosis, with one showing missed diagnosis of AMI in 34% of cases (1−Sn) confirmed at autopsy,8 while a study based on a clinical reference standard reported a much lower rate (2%).51 Underdiagnosis was less prevalent in higher volume emergency departments.51
While no study was found assessing overdiagnosis against current reference standards, two explored the validity of these reference standards.52,53 The validity of the new universal definition for AMI (change in cardiac troponin combined with either clinical symptoms, ischemic electrocardiogram changes, or imaging findings of ischemic or necrotic myocardium) reported a 1−PPV of 0.6% in a healthy group aged 70 years and 7% in a group (median age 67 years) who had suffered a non-ST-elevation AMI 3 months previously.53 A recent high-quality study assessing highly sensitive troponin T testing (HSnTnT) demonstrated a significant relationship between older age and higher HSnTnT.52 This resulted in significant overdiagnosis in those ≥70 years with HSnTnT >14.0 ng/L, a 1−Sp of 49%, and 1−PPV of 58%, compared to 12% and 50%, respectively, for those <70 years old. A higher cutoff in older populations of >53.5 ng/L displayed 1−Sp of 13% and 1−PPV of 29% with a minor increase only in underdiagnosis (1−Sn recorded at only 3% and 5% for the >14.0 ng/L and >53.5 ng/L groups, respectively), suggesting that current reference ranges for HSnTnT may be inaccurate in older patients.52
While these studies suggest increased rates of overdiagnosis in older patients, the effect of age on underdiagnosis was studied in a single autopsy study suggesting less underdiagnosis in older persons.8
Diabetes
A single retrospective study involving 18,000 patients with diabetes from two cohorts revealed 1−PPVs of 2% and 4%.54
Discussion
Overview of results
To our knowledge, this is the first systematic review of the rates of misdiagnosis of common diseases in older populations. While the literature was limited, our results indicate that clinically significant rates of overdiagnosis and underdiagnosis exist for six of the analyzed conditions in older patients. Unfortunately, study heterogeneity precluded meaningful meta-analysis of pooled data in deriving more precise numerical estimates of these rates.
Increasing age is often associated with lower diagnostic accuracy, with increased overdiagnosis of PD, HF, and AMI and underdiagnosis of dementia, PD, and HF. The impact of increasing age on COPD and stroke/TIA was unclear. In the case of COPD data, we hypothesize that this may have resulted from increased disease prevalence in study populations and the use of prevalence-dependent diagnostic measures.
Strengths and limitations
Our review has several strengths in terms of fully scoped and iterative literature searches, attempts to ascertain data specific to older populations (including contact with study authors), assessment of both over- and underdiagnosis rates, study selection criteria that stipulated use of diagnostic reference standards, attempts where appropriate to perform meta-analysis, and efforts to identify factors that predisposed to misdiagnosis.
Limitations included marked heterogeneity in population characteristics, clinical setting, disease severity, prevalence of comorbidities, age distribution, sample size, and analytic methods. Methodological quality of included studies, as assessed using the QUADAS-2 tool, was highly variable, with investigators unblinded to both clinical diagnosis and reference criteria in 40% of studies. In some instances, the reference criteria used had not been validated in older populations, as exemplified by GOLD spirometric cutoff values used to diagnose COPD and HSnTnT reference ranges in AMI. Studies also varied in how they calculated misdiagnosis rates (sensitivity/specificity or predictive values), generating concerns about the impact of disease prevalence on the stated estimates of misdiagnosis.
Research rarely focused on older patients with multiple comorbidities, poor functional reserve and polypharmacy, subgroups at the highest risk of complications from misdiagnosis. Clinician and patient factors predisposing to diagnostic error were infrequently studied.10,55
Implications for practice
Our results emphasize the need for clinicians to be systematic and circumspect in verifying past diagnoses or making a new diagnosis in older patients. In particular, clinicians need to familiarize themselves with clinical features and investigations that best discriminate between the presence and absence of disease in older populations The presence of physical comorbidities was consistently associated with lower accuracy with regard to the diagnoses of COPD, dementia, PD, HF, stroke/TIA, and AMI, possibly because somatic complaints and fatigue arising from concurrent diseases mask features that support or refute the index diagnosis.
Conclusion
Diagnostic errors involving older patients are common and comprise both overdiagnosis and underdiagnosis. Factors that predispose to misdiagnosis in older patients must be given emphasis in training continuing education programs and clinical practice guidelines.
Acknowledgments
The authors thank Justin Scott, biostatistician from the Queensland Facility for Advanced Bioinformatics, and Christine Dalais, University of Queensland Library. The authors also wish to thank Dr Jonathon Belsey, Dr Simon Lusignan, Dr Alfredo J Mansur, Dr Rafael Saad, Assistant Professor Shyam Prabhakaran, Dr Min Joo, and Dr Julia Walters for assisting in this review by providing additional data from their studies.
Author contributions
All authors meet the International Committee of Medical Journal Editors criteria for authorship: substantial contributions to the conception or design of the work or the acquisition, analysis, or interpretation of data for the work; drafting the work or revising it critically for important intellectual content; final approval of the version to be published; and agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Disclosure
The authors report no conflicts of interest in this work.
References
Scott I, Jayathissa S. Quality of drug prescribing in older patients: is there a problem and can we improve it? Intern Med J. 2010;40(1):7–18. | |
Ely JW, Kaldjian LC, D’Alessandro DM. Diagnostic errors in primary care: lessons learned. J Am Board Fam Med. 2012;25(1):87–97. | |
Neale G, Hogan H, Sevdalis N. Misdiagnosis: analysis based on case record review with proposals aimed to improve diagnostic processes. Clin Med. 2011;11(4):317–321. | |
Newman-Toker DE, Pronovost PJ. Diagnostic errors – the next frontier for patient safety. JAMA. 2009;301(10):1060–1062. | |
Alemayehu B, Warner KE. The lifetime distribution of health care costs. Health Serv Res. 2004;39(3):627–642. | |
Hardie JA, Buist AS, Vollmer WM, Ellingsen I, Bakke PS, Morkve O. Risk of over-diagnosis of COPD in asymptomatic elderly never-smokers. Eur Respir J. 2002;20(5):1117–1122. | |
Moynihan R, Doust J, Henry D. Preventing overdiagnosis: how to stop harming the healthy. BMJ. 2012;344:e3502. | |
Saad R, Yamada AT, Pereira da Rosa FH, Gutierrez PS, Mansur AJ. Comparison between clinical and autopsy diagnoses in a cardiology hospital. Heart. 2007;93(11):1414–1419. | |
Mitchell AJ, Rao S, Vaze A. Do primary care physicians have particular difficulty identifying late-life depression? A meta-analysis stratified by age. Psychother Psychosom. 2010;79(5):285–294. | |
Brazzale DJ, Upward AL, Pretto JJ. Effects of changing reference values and definition of the normal range on interpretation of spirometry. Respirology. 2010;15(7):1098–1103. | |
Marengoni A, Angleman S, Melis R, et al. Aging with multimorbidity: a systematic review of the literature. Ageing Res Rev. 2011;10(4):430–439. | |
Naughton C, Bennett K, Feely J. Prevalence of chronic disease in the elderly based on a national pharmacy claims database. Age Ageing. 2006;35(6):633–636. | |
Bellia V, Battaglia S, Catalano F, et al. Aging and disability affect misdiagnosis of COPD in elderly asthmatics: the SARA study. Chest. 2003;123(4):1066–1072. | |
Jones RC, Dickson-Spillmann M, Mather MJ, Marks D, Shackell BS. Accuracy of diagnostic registers and management of chronic obstructive pulmonary disease: the Devon primary care audit. Respir Res. 2008;9:62. | |
Lacasse Y, Daigle JM, Martin S, Maltais F. Validity of chronic obstructive pulmonary disease diagnoses in a large administrative database. Can Respir J. 2012;19(2):e5–e9. | |
Pearson M, Ayres JG, Sarno M, Massey D, Price D. Diagnosis of airway obstruction in primary care in the UK: the CADRE (COPD and Asthma Diagnostic/management REassessment) programme 1997-2001. Int J Chron Obstruct Pulmon Dis. 2006;1(4):435–443. | |
Starren ES, Roberts NJ, Tahir M, et al. A centralised respiratory diagnostic service for primary care: a 4-year audit. Prim Care Respir J. 2012; 21(2):180–186. | |
Thomsen RW, Lange P, Hellquist B, et al. Validity and underrecording of diagnosis of COPD in the Danish National Patient Registry. Respir Med. 2011;105(7):1063–1068. | |
Walters JA, Walters EH, Nelson M, et al. Factors associated with misdiagnosis of COPD in primary care. Prim Care Respir J. 2011;20(4):396–402. | |
Zwar NA, Marks GB, Hermiz O, et al. Predictors of accuracy of diagnosis of chronic obstructive pulmonary disease in general practice. Med J Aust. 2011;195(4):168–171. | |
Joo MJ, Au DH, Fitzgibbon ML, McKell J, Lee TA. Determinants of spirometry use and accuracy of COPD diagnosis in primary care. J Gen Intern Med. 2011;26(11):1272–1277. | |
Queiroz MC, Moreira MA, Rabahi MF. Underdiagnosis of COPD at primary health care clinics in the city of Aparecida de Goiania, Brazil. J Bras Pneumol. 2012;38(6):692–699. | |
Beach TG, Monsell SE, Phillips LE, Kukull W. Accuracy of the clinical diagnosis of Alzheimer disease at National Institute on Aging Alzheimer Disease Centers, 2005-2010. J Neuropathol Exp Neurol. 2012;71(4):266–273. | |
Gay BE, Taylor KI, Hohl U, Tolnay M, Staehelin HB. The validity of clinical diagnoses of dementia in a group of consecutively autopsied memory clinic patients. J Nutr Health Aging. 2008;12(2):132–137. | |
Jobst KA, Barnetson LP, Shepstone BJ. Accurate prediction of histologically confirmed Alzheimer’s disease and the differential diagnosis of dementia: the use of NINCDS-ADRDA and DSM-III-R criteria, SPECT, X-ray CT, and APO E4 medial temporal lobe dementias. The Oxford Project to Investigate Memory and Aging. Int Psychogeriatr. 1997;9(suppl 1):191–222; discussion 247–152. | |
Litvan I, MacIntyre A, Goetz CG, et al. Accuracy of the clinical diagnoses of Lewy body disease, Parkinson disease, and dementia with Lewy bodies: a clinicopathologic study. Arch Neurol. 1998;55(7):969–978. | |
Lopez OL, Litvan I, Catt KE, et al. Accuracy of four clinical diagnostic criteria for the diagnosis of neurodegenerative dementias. Neurology. 1999;53(6):1292–1299. | |
Nelson PT, Jicha GA, Kryscio RJ, et al. Low sensitivity in clinical diagnoses of dementia with Lewy bodies. J Neurol. 2010;257(3):359–366. | |
Phung TK, Andersen BB, Hogh P, Kessing LV, Mortensen PB, Waldemar G. Validity of dementia diagnoses in the Danish hospital registers. Dement Geriatr Cogn Disord. 2007;24(3):220–228. | |
Rasmusson DX, Brandt J, Steele C, Hedreen JC, Troncoso JC, Folstein MF. Accuracy of clinical diagnosis of Alzheimer disease and clinical features of patients with non-Alzheimer disease neuropathology. Alzheimer Dis Assoc Disord. 1996;10(4):180–188. | |
Verghese J, Crystal HA, Dickson DW, Lipton RB. Validity of clinical criteria for the diagnosis of dementia with Lewy bodies. Neurology. 1999;53(9):1974–1982. | |
Bradford A, Kunik ME, Schulz P, Williams SP, Singh H. Missed and delayed diagnosis of dementia in primary care: prevalence and contributing factors. Alzheimer Dis Assoc Disord. 2009;23(4):306–314. | |
Jellinger KA. How valid is the clinical diagnosis of Parkinson’s disease in the community? J Neurol Neurosurg Psychiatry. 2003;74(7):1005–1006. | |
Hughes AJ, Daniel SE, Lees AJ. Improved accuracy of clinical diagnosis of Lewy body Parkinson’s disease. Neurology. 2001; 57(8):1497–1499. | |
Hughes AJ, Daniel SE, Ben-Shlomo Y, Lees AJ. The accuracy of diagnosis of parkinsonian syndromes in a specialist movement disorder service. Brain. 2002;125(pt 4):861–870. | |
Foltynie T, Matthews FE, Ishihara L, Brayne C, MRC CFAS. The frequency and validity of self-reported diagnosis of Parkinson’s disease in the UK elderly: MRC CFAS cohort. BMC Neurol. 2006;6:29. | |
Schrag A, Ben-Shlomo Y, Quinn N. How valid is the clinical diagnosis of Parkinson’s disease in the community? J Neurol Neurosurg Psychiatry. 2002;73(5):529–534. | |
Bajaj NP, Gontu V, Birchall J, Patterson J, Grosset DG, Lees AJ. Accuracy of clinical diagnosis in tremulous parkinsonian patients: a blinded video study. J Neurol Neurosurg Psychiatry. 2010;81(11):1223–1228. | |
Newman EJ, Breen K, Patterson J, Hadley DM, Grosset KA, Grosset DG. Accuracy of Parkinson’s disease diagnosis in 610 general practice patients in the West of Scotland. Mov Disord. 2009;24(16):2379–2385. | |
Feldman AL, Johansson AL, Gatz M, et al. Accuracy and sensitivity of parkinsonian disorder diagnoses in two Swedish national health registers. Neuroepidemiology. 2012;38(3):186–193. | |
Meara J, Bhowmick BK, Hobson P. Accuracy of diagnosis in patients with presumed Parkinson’s disease. Age Ageing. 1999;28(2):99–102. | |
Owen A, Cox S. Diagnosis of heart failure in elderly patients in primary care. Eur J Heart Fail. 2001;3(1):79–81. | |
Lien CT, Gillespie ND, Struthers AD, McMurdo ME. Heart failure in frail elderly patients: diagnostic difficulties, co-morbidities, polypharmacy and treatment dilemmas. Eur J Heart Fail. 2002;4(1):91–98. | |
Ingelsson E, Arnlov J, Sundstrom J, Lind L. The validity of a diagnosis of heart failure in a hospital discharge register. Eur J Heart Fail. 2005;7(5):787–791. | |
Barents M, van der Horst IC, Voors AA, Hillege JL, Muskiet FA, de Jongste MJ. Prevalence and misdiagnosis of chronic heart failure in nursing home residents: the role of B-type natriuretic peptides. Neth Heart J. 2008;16(4):123–128. | |
Fonseca C, Sarmento PM, Marques F, Ceia F. Validity of a discharge diagnosis of heart failure: implications of misdiagnosing. Congest Heart Fail. 2008;14(4):187–191. | |
Kumler T, Gislason GH, Kirk V, et al. Accuracy of a heart failure diagnosis in administrative registers. Eur J Heart Fail. 2008;10(7):658–660. | |
Krarup LH, Boysen G, Janjua H, Prescott E, Truelsen T. Validity of stroke diagnoses in a National Register of Patients. Neuroepidemiology. 2007;28(3):150–154. | |
Prabhakaran S, Silver AJ, Warrior L, McClenathan B, Lee VH. Misdiagnosis of transient ischemic attacks in the emergency room. Cerebrovasc Dis. 2008;26(6):630–635. | |
Morgenstern LB, Lisabeth LD, Mecozzi AC, et al. A population-based study of acute stroke and TIA diagnosis. Neurology. 2004;62(6):895–900. | |
Schull MJ, Vermeulen MJ, Stukel TA. The risk of missed diagnosis of acute myocardial infarction associated with emergency department volume. Ann Emerg Med. 2006;48(6):647–655. | |
Chenevier-Gobeaux C, Meune C, Freund Y, et al. Influence of age and renal function on high-sensitivity cardiac troponin T diagnostic accuracy for the diagnosis of acute myocardial infarction. Am J Cardiol. 2013;111(12):1701–1707. | |
Eggers KM, Lind L, Venge P, Lindahl B. Will the universal definition of myocardial infarction criteria result in an overdiagnosis of myocardial infarction? Am J Cardiol. 2009;103(5):588–591. | |
de Lusignan S, Khunti K, Belsey J, et al. A method of identifying and correcting miscoding, misclassification and misdiagnosis in diabetes: a pilot and validation study of routinely collected data. Diabet Med. 2010;27(2):203–209. | |
Schermer TR, Smeele IJ, Thoonen BP, et al. Current clinical guideline definitions of airflow obstruction and COPD overdiagnosis in primary care. Eur Respir J. 2008;32(4):945–952. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
