Back to Journals » Clinical Optometry » Volume 7
Diagnosis and management of meibomian gland dysfunction: optometrists' perspective
Authors Opitz D , Harthan J , Fromstein S, Hauswirth S
Received 7 April 2015
Accepted for publication 5 June 2015
Published 28 August 2015 Volume 2015:7 Pages 59—69
DOI https://doi.org/10.2147/OPTO.S63484
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 5
Editor who approved publication: Mr Simon Berry
Video abstract presented by Stephanie R Fromstein
Views: 5658
Dominick L Opitz,1 Jennifer S Harthan,1 Stephanie R Fromstein,1 Scott G Hauswirth2
1Department of Clinical Education, Illinois College of Optometry, Chicago, IL, 2Minnesota Eye Consultants, Minneapolis, MN, USA
Abstract: Meibomian gland dysfunction (MGD) is commonly encountered among eye care professionals. Our understanding of the pathophysiology for the development of MGD has greatly expanded in recent years, which helped increase awareness of the disease. Despite increased awareness, it is essential for eye care professionals to make a conscious effort to properly examine the meibomian glands through gland expression even for asymptomatic patients. At minimum, early management should include patient education and supportive therapy such as warm compresses, lid hygiene, and gland expression. As patients become more symptomatic and as the ocular surface becomes more affected, employing additional therapeutic management is recommended and may include oral omega-3 essential fatty acids, topical azithromycin, oral tetracycline, and topical anti-inflammatories to improve clinical signs and patient comfort. In addition to treatment of MGD, clinicians should be mindful of the comorbid conditions of MGD and simultaneously manage them in conjunction of MGD treatment.
Keywords: meibomian gland dysfunction, dry eye, blepharitis, ocular surface disease
Introduction
Ocular surface diseases such as those that occur in dry eye conditions continue to be a leading cause of patient-driven visits to eye care professionals. Generalized inflammation to the eye lid or blepharitis has been implicated as a major contributor to the development of dry eye complaints.1 The two primary distinctions in blepharitis are anterior versus posterior blepharitis. With anterior blepharitis, the inflammation is localized to the lid margin anterior to the gray line, with inflammation concentrated around the base of the lashes in the form of squamous debris (derived from squamous epithelial cells) or collarets, which may spill onto the posterior lid margin.1 Meibomian gland dysfunction (MGD) is often used synonymously with posterior blepharitis; however, posterior blepharitis is an umbrella term describing inflammatory conditions of the posterior lid margin, which includes MGD, as well as a number of other causes, including conjunctivitis and acne rosacea.1 In 2010, the International Workshop on Meibomian Gland Dysfunction developed a recommended definition for MGD in an effort to clarify the differences:
MGD is a chronic, diffuse abnormality of the meibomian glands, commonly characterized by terminal duct obstruction and/or qualitative/quantitative changes in the glandular secretions. This may result in alterations of the tear film, symptoms of eye irritation, clinically apparent inflammation, and ocular surface disease.1
MGD is one of the most common causes for the development of ocular surface disease symptoms, specifically those associated with dry eye conditions. The primary goal in the eye care practitioner’s management of MGD is to reduce or eliminate associated signs and symptoms, to improve patient comfort, and to prevent sight-threatening complications such as corneal scarring, resulting from infection and inflammation. As optometrists, we are on the front lines of this management, and an important first step is proper identification and diagnosis. We must also keep in mind that many patients may have a combination of multiple ocular surface diseases contributing to ocular discomfort. In this review, we will discuss the normal anatomy and functions of the meibomian glands (MGs), the pathophysiology of MGD, comorbidities, as well as diagnostic and therapeutic advancements in the management of MGD.
Normal anatomy and function of the MGs
In an effort to understand the pathophysiology for the development of MGD, it is important to first understand the normal functional anatomy of the MGs and their contributions to a healthy ocular surface and tear layer. The human MGs are holocrine lipid-excreting glands with 20–25 glands along the lower eyelid and 30–40 glands along the upper eyelid.2 Each MG comprises multiple acini connected by a long common duct running through the length of the gland.2 Cells comprising the acini synthesize unique MG lipids that are released into the central duct through a process of acinar cell degeneration. The production of MG lipids by acinar cells is under neuronal, hormonal, and vascular control.2,3 Once produced, these lipids are then excreted as meibum onto the ocular surface through the MGs opening or orifice located at the mucocutaneous junction of the lid margin.2,3 The low melting point of normal, healthy meibum (19–40°C,4–6 with corneal temperature at approximately 32°C)7 is easily excreted through the MG orifice onto the ocular surface by natural blinking and passive migration up and through the MG.
Healthy meibum or lipids excreted by the MGs are fluid and clear, forming the superficial layer of the tear film. These MG lipids provide a smooth optical surface, prevent tear overflow onto the lids, and create a water-tight seal during lid closure during sleep.3,8 The meibomium lipids reduce tear evaporation during waking hours, function as a lubricant for the eyelids during blinking, and may provide a barrier to prevent bacteria from entering the tear film.3,9
Pathophysiology of MGD
The development of a dysfunctional MG can occur as either low delivery or high-delivery of the MG lipids onto the ocular surface.1 High-delivery states – also termed hypersecretory MGD – results in a large volume of MG lipid accumulating at the lid margin. Hypersecretory MGD is usually secondary to systemic conditions such as seborrheic dermatitis, atopic dermatitis, and acne rosacea. Low-delivery states of MG secretions can be further classified into hyposecretion or MG obstruction. Hyposecretion develops when MG atrophy occurs, resulting in a generalized reduction in the number of functioning MGs. MG obstruction is the most common form of MGD.8,10 With obstructive MGD, hyperkeratinization of the epithelium lining the MG duct occurs.11 The exact cause for the development of hyperkeratinization is unknown, but inflammatory mediators are suspected.11 Once the epithelium becomes hyperkeratinized, the orifice of the MG can become obstructed.12–14 This obstruction prevents meibum from exiting the MG, resulting in low delivery of the meibum onto the ocular surface.
During early MG obstruction, the production of meibum continues, but the inability of the meibum to be excreted due to obstruction results in increased pressure within the MG.15 This increased pressure causes dilation of the MG duct and the acini. Acinar degeneration and atrophy can follow ductal dilation, which may ultimately lead to loss of meibocytes. Backup and stagnation of the MG lipids causes alternations to the meibomian secretions. These alterations include thickening and loss of clarity, with increased melting point of the secretions, which can further perpetuate ductal stagnation and pouting of the MG orifices.15 Prolonged MG obstruction leads to bacterial colonization. Eventually, inflammatory mediators are formed and released from lipolytic enzymes that are produced from bacteria such as Staphylococcus epidermidis, S. aureus, Propionibacterium acnes, and Cornebacterium.16 Lipolytic enzymes released by bacteria cause highly irritating free fatty acids to breakdown the lipids in the tear film contributing to the loss of tear film integrity.17 This loss of tear film stability allows for increased aqueous tear evaporation, leading to signs and symptoms of evaporative dry eye.
Diagnosis
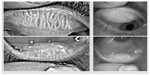
The clinical diagnosis of MGD is often made using a combination of subjective symptoms and clinical signs. During early development of MGD, patients may be asymptomatic. If asymptomatic, the diagnosis of MGD is only detectable by the presence of clinical signs. The most common clinically observable signs of MGD include MG dropout, altered MG excretions, and changes to the lid morphology with plugging or pouting of the MG orifice being the most pathognomonic sign of MGD.18 Other changes to the lid margin that may occur with advancing MGD are listed in Table 1.8,11,18,19 A simple, inexpensive technique to evaluate for MG dropout (partial or complete loss of MGs)20 includes meibography by transillumination of an everted lid at the slit lamp (Figure 1). Infrared meibography has enhanced visualization of the MG, and there are now several commercially available meibographers (Figure 2) for clinical use. MG atrophy is not constant over the entire tarsus, which suggests one potential issue with these methods: the inability to display the entire tarsal plate in focus at the same time.21–24 Furthermore, changes observed may not be exclusively due to MGD, as there can be age-related changes in the MGs in healthy patients as well. The optometrist should keep this in mind when evaluating a patient, as MGD and natural aging changes can act synergistically in causing signs and symptoms on the ocular surface.25 The amount of MG loss and alterations in the quality of expressed meibum have been used to help classify the severity of the disease.1 However, there is no data on the correlation of meibography and gland expression.18,21–24
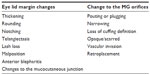  | Table 1 List of the anatomical changes that can occur to both the eyelid margins and the MG orifices in patients with MGD |
  | Figure 1 Infrared image of the meibomian glands of the lower lid. |
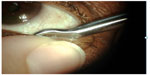
As valuable as MG expression is to the diagnosis of MGD, it is estimated that <10% of comprehensive ophthalmologists and optometrists express the MGs.8 Traditional MG expression techniques to assess alterations of the MG secretions include digital pressure of the examiner’s finger or a cotton swab against the external lid margin. A more advanced technique includes using one or two cotton-tipped applicators (one internal swab moistened with anesthetic and one external swab) or using an instrument such as the Mastrota paddle (Figure 3). The protocol for single cotton-tipped applicator involves instilling two drops of topical anesthetic into the conjunctival sac and then scrubbing the lid margin with a cotton-tipped applicator soaked in the same anesthetic in order to remove lid debris. Simultaneous digital pressure to the external lid and applicator pressure to the palpebral conjunctiva allow the expression of the MG without pressure to the globe.26 The MG evaluator (TearScience Inc., Morrisville, NC, USA) can be used to accomplish the same task using a standardized amount of force applied to the glands, which mimics that force of a deliberate blink.4 The goal of all of these techniques is to express meibum and assess quality and quantity of the meibum expressed. Normal patients will have a clear, easily expressed meibum. Patients with MGD may have varied meibum appearances from clear to cloudy, viscous fluid with particulate matter that is opaque or thickened toothpaste-like material (Table 2).18,19,27 Grading the central third or the central 8 MG of the lower lid is the preferred anatomical location to assess meibum, which helps not only to diagnose MGD, but also to assess response to therapy.
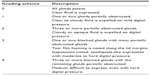  | Table 2 Grading scheme to evaluate the meibum and gland obstruction in patients with MGD |
Symptomatic MGD occurs due to damage to the ocular surface that occurs most often from evaporative dry eye. Symptoms of evaporative dry eye can be similar to that of aqueous-deficient dry eye.28 These symptoms may include ocular itching, burning, redness, irritation, soreness and or edema of the eyelids, foreign body sensation, tearing, fluctuating vision, and contact lens intolerance. The ocular surface damage that occurs from MGD-related evaporative dry eye includes staining to the bulbar conjunctiva and cornea. Lid wiper epitheliopathy may also occur, further contributing to symptoms.29 Lid wiper epitheliopathy is characterized by lissamine green staining of an everted upper lid on the palpebral conjunctiva posteriorly to the superior line of Marx and can occur with evaporative dry eye resulting from MGD. Lid wiper epitheliopathy indicates poor wetting of the cornea and may contribute to irritation of the superior conjunctiva and cornea.29 If inflammation to the posterior lid margin occurs, patient may also experience irritation, itching, and discomfort localizing to the eyelid margins. Although several questionnaires have been reviewed30,31 to assess symptoms of ocular surface disease and dry eye, no single questionnaire is diagnostic for MGD or evaporative dry eye. The Ocular Surface Disease Index (OSDI)30 assesses vision-related function, ocular symptoms, and environmental triggers resulting from dry eye, whereas the Standard Patient Evaluation of Eye Dryness (SPEED)31 assesses the frequency and severity of symptoms. Regardless of their diagnostic sensitivity for MGD versus aqueous-deficient dry eye, standardized questionnaires help assess subjective changes of the patient’s symptoms in response to treatment.
Patients suffering from symptomatic MGD will commonly have changes to the ocular surface, and it is important to assess these changes as this can influence management. Tear break-up time (TBUT) measures tear film abnormalities, and fluorescein staining of the cornea and bulbar conjunctiva helps measure severity of ocular surface disease.18 A low TBUT suggests a compromised lipid layer due to stasis of the meibum. A low TBUT should prompt careful evaluation of the MGs and its secretions. Expressed meibum quality is correlated with TBUT and corneal staining. As MGD progresses, meibum composition continues to be altered, increasing tear film instability and corneal staining.15,18
Bulbar conjunctival staining will often appear prior to corneal staining in patients with ocular surface disease.32 Staining is best visualized using sodium fluorescein with a yellow filter. Lissamine green or rose bengal staining typically occurs later in the disease process and often indicates keratoconjunctivitis sicca.33 Corneal staining is best observed with sodium fluorescein and often appears as areas of superficial punctate epitheliopathy inferiorly due to Staphylococcus exotoxins.34,35 Gram-positive bacteria in general release a huge number of biologically active toxins, which lead to the further release of extracellular enzymes such as staphylokinase, lipase, hyaluronidase, DNAse, coagulase, lysozyme, and others. The sum effect of these enzymes is invasion and compromise of the corneal integrity and the classic inferior superficial punctate keratitis staining.34 The lid margin normally stains at Marx’s line, where the keratinized epithelium of the lid and the non-keratinized epithelium of the conjunctiva meet. The staining pattern may widen with progressive lid margin disease due to increased keratinization. This increase in epithelial keratinization may cover the glands and be an additive factor to MG obstruction.4,13,36 Although not a direct test for the presence or grade of MGD, Schirmer tear test or phenol red thread test may differentiate aqueous-deficient dry eye from evaporative dry eye.18 The diagnostic challenge is that aqueous-deficient dry eye and evaporative dry eye will often coexist suggesting that Schirmer testing should be used in conjunction with other diagnostic measures when evaluating patients with MGD. Schirmer I testing is performed without anesthesia for 5 minutes with the patient’s eyes closed and measures both reflex and basal secretion. Schirmer I testing is often performed on a patient’s initial visit to obtain baseline information. Schirmer II testing is performed with anesthesia and measures basal secretion and is often used at follow up visits.18 MGD may result in more severe ocular surface disease and tear evaporation, thereby reducing Schirmer scores.37 Symptoms may not always correlate with objective signs in patients with MGD. Making a diagnosis of MGD requires close observation of anatomical changes to the lid margins and expression of the MGs. Diagnostic tests such as tear volume, meibometry (non-invasive method to quantify lipids at the lid margin),38 tear film evaporation, ocular surface staining, Schirmer scores, and meibography should be used in conjunction with each other to make the appropriate diagnosis and management plan for patients with MGD (Table 3). These tests should also be used to monitor the progression of the disease and the patient’s response to therapy.
  | Table 3 Normative and abnormal values for the diagnostic testing performed in the evaluation of patients with MGD |
Comorbid conditions
MGD rarely exists in isolation and is closely linked – both in etiology and clinical features – to a host of other ocular and systemic conditions. The challenge when looking at comorbidities in a complex and multifactorial system is to determine whether any given factor is causative, correlated, or coincidental. While the nature of these relationships continues to be elucidated, a number of ophthalmic and systemic conditions have clearly emerged as players in the intricate network of the ocular surface.
Within this network, perhaps the most intertwined relationships exist between dry eye disease, blepharitis, and MGD, each with a tendency to coexist with and exacerbate the next. It has long been established that MGD is elementary in the pathogenesis of evaporative dry eye. Less intuitive, however, is recent research implicating MGD in aqueous-deficient dry eye as well.39,40 Researchers have noted a high prevalence of MGD among patients with Sjogren’s Syndrome40, as well as lipid layer defects in patients with severe aqueous deficiency (not classified as Sjogren’s Syndrome).39 Whether this impact on the MGs is a direct outcome of the disease or instead due to prolonged changes to the ocular surface remains in question. What appears clear, however, is that MGD seems to coexist with aqueous-deficient dry eye.
Both anterior and forms of posterior blepharitis have been shown to play a role in the pathogenesis of MGD. The higher levels of bacterial colonization observed in anterior blepharitis may contribute to inflammation of the posterior lid margin, including MGD.41 Seborrheic blepharitis has additionally been associated with dysfunctional meibum production; given the derivation of MGs from sebaceous glands, however, this association is hardly surprising.41 Overall, patients with chronic blepharitis have MG loss significantly greater than their matched controls,19 further solidifying the correlation between these two conditions.
The role of demodex in blepharitis is well characterized; however, the relationship to MGD remains somewhat equivocal, with some studies showing a high correlation with MGD and others revealing none at all.39 Given the high infestation rate in patients with anterior blepharitis and MGD,42 it appears likely that a role for demodex in the direct or indirect pathogenesis will soon be brought to light.
While the role of demodex in MGD remains indistinct, there has been much research into the relationship of MGD to rosacea, which represents the first of a number of important systemic comorbidities. A number of studies speak to a high percentage of MGD in patients with rosacea, with one citing lid changes in as many as 90% of cases of ocular rosacea.43–45 Similarly, a study of patients with Stevens-Johnson Syndrome revealed an overwhelming percentage of MG involvement (80.4%),46 and patients with graft versus host disease are often documented to display severe MGD.47 Patients with ectodermal dysplasia syndrome showed alterations in their MGs in 95.5% of patients in a study by Kaercher.48 A myriad of other systemic conditions have also been thought to correlate with MGD, including androgen deficiency, atopy, benign prostate hyperplasia, cicatricial pemphigoid, lupus, hypertension, Parkinson’s disease, ocular pemphigoid, polycystic ovary syndrome, psoriasis, and Turner syndrome,39 highlighting the complex connections between systemic disease and ocular complications.
Any discussion of MGD comorbidities would be remiss without discussing the link with contact lens wear and intolerance. While comparing the frequency of MGD in contact lens wearers and non-contact lens wearers, most studies find a greater percentage of MGD in the contact lens group, although it should be noted that not all studies found this difference to be statistically significant.39 Some authors postulate that the relationship may be via mechanical irritation of the glands through the eyelid by the lens and correlate this mechanical stimulus to morphological changes observed.49 Where the story of MGD and contact lens wear becomes clinically relevant is when discussing contact lens intolerance; evidence agrees with clinical experience that discomfort and dryness symptoms in contact lens wearers may be associated with MGD, with asymptomatic contact lens wearers significantly more likely to have normal meibum secretions.10 As such, the prudent eye care practitioner should identify and treat MGD before prescribing lenses in order to improve patient outcomes and decrease patient dropout. Clearly, MGD does not exist in an isolated state and appears connected to a multitude of ocular and systemic conditions. For the eye care professional, this means a multifaceted approach to a decidedly pervasive problem. By recognizing the unique interplay on the ocular surface, we can start to consider therapy that targets not only the MGs but many of the other lid, tear, and systemic issues that are often attendant and provides more comprehensive management to our patients with MGD.
Treatment
Advancements in our understanding of the pathogenesis of MGD and our ability to better diagnose MGD have led to many advancements in the treatment and management of the disease. The MGD Workshop recommended a severity-based approach to treatment.50 In the years since these guidelines were published, many other therapeutic options have become available, and knowledge of each treatment option has deepened. As we begin our discussion of treatment for MGD, it is important to first properly grade the level of MGD severity based on signs, symptoms, and grade of MG secretions. Stage 1–4, with Stage 1 being the mildest, is generally used (Table 2).18,19,27 Further, it is important to note that treatment options are additive – that is, patients with MGD Stage 3 should also receive the treatments in level 2 and level 1.50
The treatment recommendations for MGD Stage 1 in which the patients have no symptoms, no ocular surface staining, and minimally altered expression and secretion quality include patient education on the environmental factors, diet, and systemic medications that can affect the MGs and the tear film.50 Treatment considerations for Stage 1 include lid warming and lid expression. The goal of lid warming, commonly referred to as warm compresses, involves application of heat directly to the lid margins with the ultimate goal of melting the pathologically altered meibomian lipids.50 Patients often report symptomatic improvement from performing warm compresses,51 but patient adherence to warm compresses are often a challenge. Several controlled studies demonstrated that there is therapeutic relief when warm compresses are performed according to a strict protocol, which includes increasing the temperature of the lids to allow the altered meibum to be melted and released from the MG. Studies report a wide range of eye lid temperatures from 89.6°F to 113°F.4,52–55
As part of warm compress therapy, digital massage or gland expression of the eyelids is also recommended. The goal is to express thicker meibum from the gland, usually following warm compresses for several minutes. Therapeutic expression of the gland is considered to be beneficial by expunging all solidified and liquid secretions, allowing the potential for the MG to “reset” and produce more normal secretions. A number of methods are available for performing this, which range from utilizing cotton swabs (protocol reviewed under diagnosis section) to more specific devices created for gland expression including the Mastrota paddle (Figure 3) and Kimura spatula. An important factor in performing manual expression is the amount of pressure required to obtain therapeutic result. The pressure ranges are between 5 psi and 40 psi to obtain the first liquid secretions from a gland and between 10 psi and 40 psi for evacuation of the glandular contents. Unfortunately, only 7% of patients could tolerate the pressure necessary to achieve complete therapeutic expression.56
Lid hygiene commonly referred to as lid scrubs, in conjunction with digital massage of the eyelids and warm compress therapy, has been shown to improve patient symptoms in those who have MGD and anterior blepharitis.57–59 Lid hygiene is used to clean the base of the eyelashes just posterior to the lid margin, which may lessen bacterial load and remove dead skin, potentially reducing inflammation and improving the environment of the lid margin. One study of patients with either mild to moderate anterior blepharitis or MGD showed a significant improvement in subject’s OSDI score, which dropped from 30 to 19 after performing lid hygiene twice daily for 3 weeks and then once per day until day 90. The number of symptomatic patients was reduced by 46% at day 90.60 Both OSDI30 and SPEED31 are validated questionnaires for assessing dry eye disease symptoms, with OSDI also taking into account an assessment of vision-related activities.
In Stage 2 MGD, patients develop minimal to mild symptoms along with clinical signs such as ocular surface staining. Treatment recommendations for Stage 2 include lid hygiene with warm compresses and expression of the MG secretions. The addition of omega-3 fatty acid supplements should also be considered in Stage 2.50 Omega-3 components DHA and EPA are metabolized into anti-inflammatory byproducts, which may provide benefit to the ocular surface, as well as potentially altering the quality of meibum produced in the glands and improving patient signs and symptoms.61–63
Artificial tears, topical azithromycin, topical emollient lubricants, or liposomal sprays should also be considered in Stage 2 MGD.50 Oil-emulsion tears can be used several times per day to supplement the overall volume of the patient’s pre-corneal tear film and to increase the reduced lipid layer thickness. In fact, a single drop of a castor-oil-based tear has been shown to increase lipid layer thickness with the castor oil component persisting for four hours on the tear film.64 Oil-emulsion tears also decrease friction, reduce tear osmolarity, and potentially dilute cytokines and other pro-inflammatory mediators. Studies specifically utilizing oil-emulsion tears in MGD patients show improvements in both subjective symptoms and objective signs. A 4-week, randomized, prospective study using Systane Balance® and saline as control in patients with MGD showed statistically significant increases in the non-invasive TBUT scores in the Systane Balance® (Alcon Pharmaceuticals, Fort Worth, TX, USA) group compared with controls. Additionally, there was reduction in conjunctival and corneal staining, increased goblet cell density, and increased MG expressability.65
The use of topical and oral antibiotics has been found to be beneficial in the treatment of MGD and should be considered for treatment of Stage 2 MGD. Topical azithromycin 1.0% ophthalmic solution is a broad spectrum, macrolide topical antibiotic with presumed anti-inflammatory properties.50 Several studies using topical azithromycin 1.0% ophthalmic solution (AzaSite®) for the treatment of MGD showed a significant improvement in both clinical signs and symptoms of MGD.66–69 Dosing of AzaSite® for this off-label application has been reported to be twice daily for 2 days and then once daily for 14–30 days. Periodic shorter pulse dosing of AzaSite® for 1–2 weeks may be considered after the initial 30-day treatment if symptoms recur.
Oral tetracyclines have a long history of use in dermatologic management of rosacea and have been prescribed for their anti-inflammatory effects as well as the effect on lipid metabolism within the glands. Although the tetracyclines as a whole are noted to reduce levels of MMP and IL-1, it is interesting that doxycycline has not been detectable in the tear film.70 Both minocycline and tetracycline have been found to offer significant improvement of both signs and symptoms associated with MGD.71,72 Interestingly, 20 mg of doxycycline twice daily was found to be just as effective as higher doses of 200 mg twice daily with potentially less systemic side effects.73 The anti-inflammatory effects of low dose doxycycline is likely responsible for the clinical improvement.
Although not originally included in the MGD Workshop, the macrolide antibiotics have also been shown to have anti-inflammatory effects, and their use as oral agents in the treatment of MGD is increasing. Azithromycin tends to be the drug of choice in this category due to good tolerability and potent anti-inflammatory effects. It may also have a direct impact on lipid composition and accumulation in the MGs.74 A study examining the use of oral azithromycin 500 mg per day for 3 days per week over a period of 3 weeks was performed, with a follow up of 1 month. Statistically significant improvements were noted in TBUT.75 In a comparative study of doxycycline and azithromycin, patients were randomized to either 5 days of azithromycin (500 mg on the first day followed by 250 mg/day for 5 days) or 1 month of doxycycline (200 mg/day). Both groups showed improvements from baseline in symptoms; however, the azithromycin group showed more improvement of conjunctival hyperemia and corneal staining.76
As signs and symptoms progress from mild to moderate in Stage 3, the use of oral tetracycline is no longer considered an option but a recommended treatment according to the MGD Workshop.50 Topical anti-inflammatory medications should also be considered in the treatment algorithm in Stage 3. As symptoms and signs become more marked in Stage 4, anti-inflammatories are recommended. Inflammation is a hallmark feature of dry eye, and using anti-inflammatory medications offer therapeutic benefits.28 Similarly, inflammation is often associated with symptomatic MGD. Quelling ocular surface inflammation and eyelid margin inflammation that results from MGD should be beneficial. Topical anti-inflammatory preparations that have shown to be effective in reducing inflammation in patients with MGD include cyclosporine A77,78 and topical steroids, specifically, loteprednol etabonate.79
Other treatment options, which became available after the publication of the MGD Workshop, include lid margin debridement and MG probing. Debridement may be done using a golf club spud, PRK spatula, or any other blunt instrument. The goal is to mechanically debride the lid margin to remove dead skin and debris, which may collect along the line of Marx, which contributes to MG obstruction. This technique improves patient symptoms and reduces the scaling of the lid margin.80
The Maskin probe is a 76 μm diameter probe with probe length ranging from 1 mm to 6 mm, which is inserted into the gland orifice to provide patency to the proximal opening of the gland. The probes may also be inserted much deeper into the gland and are designed to disrupt any fibrovascular membranes, which may exist within inflamed gland structure. These fibrovascular membranes may accelerate gland dysfunction, truncation, and possible dropout. Studies indicate that probing for obstructive MGD offers significant improvement of symptoms,81,82 and one study showed that 90% of patients were able to discontinue oral doxycycline following probing.82
Other new technologies that have emerged in the treatment of MGD include MiBoFlo, LipiFlow Thermal Pulsation, and Intense Pulsed Light (IPL). These commercially available units use heat sources to either assist with warming of the lids and/or expression of the meibum. The MiBoFlo Thermaflo® (Pain Point Medical Systems, Dallas, TX, USA) uses a proprietary thermoelectric heat pump designed to liquefy inspissated secretions and improve MG function.83,84 The unit warms a paddle to 108°F, which is then applied to the lids, melting the meibum to allow for easier expression from the gland. The LipiFlow® unit consists of an eyepiece, which is inserted underneath the upper and lower eyelids and vaults over the cornea.85 The external portion of the shell contains heating elements, which warm to 108°F and provide contact with the inner palpebral conjunctival surface. In addition, the external portion of the eyepiece sits on the external surface of the lids and contains a pneumatically driven pad, providing pulsatile pressure to the external lid causing expression of the MG to take place. The treatment can be done as a bilateral simultaneous procedure, and treatment time runs for 12 minutes. The effect of a single LipiFlow® treatment has shown significant improvements in OSDI scores, lipid layer thickness, and total number of glands producing expressible meibum.86 Even at 9 months after a single LipiFlow® treatment, SPEED and TBUT scores remained significantly improved.87 Symptomatic improvement was more noticeable in milder forms than severe forms of the MGD,86 and significant improvements were maintained after 1 year in MG secretion score, as well as OSDI and SPEED scores in moderate to severe forms of MGD.87
The IPL unit is a non-laser light source utilizing a broad spectrum light, which is emitted between 515 nm and 1200 nm over 0.5–88.5 milliseconds.88 The device takes advantage of two peaks in the oxyhemoglobin absorption spectrum, which allow for increased energy absorption over melanin. Much of the light is converted to heat energy. This heat energy decreases the microvasculature and telangiectasias along the epidermis and anterior dermal boundary, as well as liquefies solidified meibum within the MGs. Following IPL application, manual expression is performed to completely evacuate the liquified contents from the gland. Typically, multiple treatments are scheduled over a period of several months to achieve full treatment. A prospective, double-masked, placebo-controlled study was performed on 28 patients. Significant improvements were noted in lipid layer thickness and NITBUT, as well as patient symptom scores.89 The largest study using IPL for treatment of patients with MGD involved 78 patients with a 30-month follow up. All had been diagnosed with severe dry eye. Treatment consisted of IPL and manual expression. Improvement was noted in TBUT for 68 of 78 patients, with an average of seven treatments and four maintenance visits. A total of 93% of patients reported improved symptoms and satisfaction with the treatment. Postoperative redness and swelling were present in 13% of patients.90
Conclusion
Given the prevalence of MGD, clarifying the pathophysiology, associated conditions, and management options is critical to the eye care professional. Our understanding of the pathophysiology for the development of MGD has greatly expanded in recent years, which has helped to increase awareness of the disease and direct therapies. Along with increased awareness comes a call to action; it is essential for eye care professionals to make a conscious effort to properly examine the MGs through gland expression, even for asymptomatic patients; they represent an undertreated patient base and a wealth of preventative medicine potential. Further nonobvious and asymptomatic MGD is more likely to occur in younger patients. Without early intervention, MGD can and likely progress to obvious and symptomatic MGD. It is possible that if older patients were identified and treated before they became symptomatic, end-stage disease or MG atrophy may not occur. In general, younger patients are more often patients in optometric practices, whereas older patients are patients in ophthalmology practices. In an effort to mitigate the progression and prevent chronic symptoms later in life, optometrists should actively evaluate and treat this condition early. Additionally, the patients wearing contact lens are more likely to be within optometric practices. As previously discussed, symptomatic contact lens wearers have a greater incidence of MGD compared with asymptomatic contact lens wearers. At minimum, early management should include patient education and supportive therapy such as warm compresses, lid hygiene, and gland expression. As clinical signs and symptoms progress, employing additional therapeutic management is recommended and may include oral omega-3 essential fatty acids, topical azithromycin, oral tetracycline, and topical anti-inflammatories to improve ocular surface signs and patient comfort. In addition to treatment of MGD, clinicians should be mindful of the comorbid conditions of MGD and simultaneously manage them in conjunction of MGD treatment. While we continue to elucidate the underlying etiology of the clinical presentation of MGD, new – targeted – treatment options will continue to emerge, and eye care professionals will need to adjust their treatment algorithm based on patients’ needs and severity.
Disclosure
DLO and SH: Allergan, Inc., Bausch + Lomb (Valeant), Shire Pharmaceuticals; SH: BioTissue and Tear Science. The authors report no conflicts of interest in this work.
References
Nelson JD, Shimazaki J, Benitz-de-Castillo JM, et al. The international workshop on meibomian gland dysfunction: report of the definition and classification subcommittee. Invest Ophthalmol Vis Sci. 2011;52:1930–1937. | |
Bron AJ, Tiffany JM. The meibomian gland and tear film lipids: structure, function and control. Adv Exp Med Biol. 1998;438:281–295. | |
McCulley JP, Shine WE. Meibomian gland function and the tear lipid layer. Ocul Surf. 2003;1(3):97–106. | |
Korb DR, Blackie CA. Meibomian gland diagnostic expressiblity: correlation with dry eye symptoms and gland location. Cornea. 2008; 27(10):1142–1147. | |
Terada O, Chiba K, Senoo T, Obara Y. Ocular surface temperature of meibomia gland dysfunction patients and the melting point of meibomian gland secretions (in Japanese). Nippon Ganka Gakkai Zasshi. 2004;108:690–693. | |
Butovich IA, Lu H, McMahon A, et al. Biophysical and morphological evaluation of human normal and dry eye meibum using hot stage polarized light microscopy. Invest Ophthalmol Vis Sci. 2014;55(1):87–101. | |
Shih SR, Li HY, Hasiao YL, Chang TC. The application of temperature measurement of the eyes by digital infrared thermal imaging as a prognostic factor of methylprednisolone pulse therapy for Graves’ ophthalmopathy. Acta Ophthalmol. 2010;88(5):e154–e159. | |
Foulks GN, Bron AJ. Meibomian gland dysfunction: a clinical scheme for description, diagnosis, classification, and grading. Ocul Surf. 2003; 1(3):107–126. | |
Mudgil P. Antimicrobial role of human meibomian lipids at the ocular surface. Invest Ophthalmol Vis Sci. 2014;14(5):7272–7277. | |
Korb DR, Henriquez AS. Meibomian gland dysfunction and contact lens intolerance. J Am Optom Assoc. 1980;51:243–251. | |
Foulks GN, Nichols KK, Bron AJ, Holland EJ, McDonald MB, Nelson JD. Improving awareness, identification, and management of meibomian gland dysfunction. Ophthalmology. 2012;119(10):S1–S11. | |
Jester JV, Nicolaides N, Smith RE. Meibomian gland dysfunction. I. Keratin protein expression in normal human and rabbit meibomian glands. Invest Ophthal Vis Sci. 1989;30:927–935. | |
Jester JV, Nicolaides N, Kiss-Palvolgy I, Smith RE. Meibomian gland dysfunction. II. The role of keratinization in a rabbit model of MGD. Invest Ophthalmol Vis Sci. 1989;30:936–945. | |
Nicolaides N, Santos EC, Smith RE, Jester JV. Meibomian gland dysfunction. III. Meibomian gland lipids. Invest Ophthalmol Vis Sci. 1989;30:946–951. | |
Eom Y, Choi KE, Kang SY, Lee HK, Kim HM, Song JS. Comparison of meibomian gland loss and expressed meibum grade between the upper and lower eyelids in patients with obstructive meibomian gland dysfunction. Cornea. 2014;33:448–452. | |
Dougherty JM, McCulley JP. Comparative bacteriology of chronic blepharitis. Br J Ophthalmol. 1984;68(8):524–528. | |
Bron AJ, Tiffany JM. The contribution of meibomian disease to dry eye. Ocul Surf. 2004;2:149–165. | |
Tomlinson A, Bron AJ, Korb DR, et al. The international workshop on meibomian gland dysfunction: report of the diagnosis subcommittee. Invest Ophthalmol Vis Sci. 2011;52:2006–2049. | |
Mathers WD, Shields WJ, Sachdev MS, Petroll WM, Jester JV. Meibomian gland dysfunction in chronic blepharitis. Cornea. 1991;10:277–285. | |
Feng Y, Gao Z, Feng K, Qu H, Hong J. Meibomian gland dropout in patients with dry eye disease in China. Curr Eye Res. 2104;39(10):965–972. | |
Pult H, Riede-Pult BH. Non-contact meibography: keep it simple but effective. Cont Lens Anterior Eye. 2012;35:77–80. | |
Srinivasan S, Menzies K, Sorbara L, Jones L. Infrared imaging of meibomian gland structure using a novel keratograph. Optom Vis Sci. 2012;89:788–794. | |
Arciniega JC, Wojtowicz JC, Mohamed EM, McCulley JP. Changes in the evaporation rate of tear film after digital expression of meibomian glands in patients with and without dry eye. Cornea. 2011;30:843–847. | |
Finis D, Ackermann P, Pischel N, et al. Evaluation of meibomian gland dysfunction and local distribution of meibomian gland atrophy by non-contact infrared meibography. Curr Eye Res. 2014:1–8. | |
Arita R, Itoh K, Inoue K, Amano S. Noncontact infrared meibography to document age-related changes of the meibomian glands in a normal population. Ophthalmology. 2008;115:911–915. | |
Korb DR, Greiner JV. Increase in tear film lipid layer thickness following treatment of meibomian gland dysfunction. Adv Exp Med Biol. 1994;350:293–298. | |
Nichols KK, Foulks FN, Bron AJ, Glasgow BJ, et al. The international workshop of meibomian gland dysfuction: executive summary. Invest Opthalmol & Vis Sci. 2011;52(4):1922–1993. | |
[No authors listed]. Management and therapy of dry eye disease: report of the Management and Therapy Subcommittee of the International Dry Eye Workshop. Ocul Surf. 2007;5:163–178. | |
Korb DR, Herman JP, Grenier JV, et al. Lid wiper epitheliopathy and dry eye symptoms. Eye Contact Lens. 2005;31:2–8. | |
Schiffman RM, Christianson MD, Jacobsen G, Hirsch JD, Reis BL. Reliability and validity of the ocular surface disease index. Arch Ophthalmol. 2000;118:615–621. | |
Ngo W, Situ P, Keir N, Korb D, Blackie C, Simpson T. Psychometric properties and validation of standard patient evaluation of eye dryness questionnaire. Cornea. 2013;32:1204–1210. | |
Yokoi N, Kinoshita S. Importance of conjunctival epithelial evaluation in the diagnostic differentiation of dry eye from drug-induced epithelial keratopathy. Adv Exp Med Biol. 1998;438:827–830. | |
Kaercher T, Bron AJ. Classification and diagnosis of dry eye. Dev Ophthalmol. 2008;41:36–53. | |
Obrien TP. Management of bacterial keratitis: beyond exorcism toward consideration of organism and host factors. Eye. 2003;17:957–974. | |
Savini G, Prabhawasat P, Kojima T, Grueterich M, Espana E, Goto E. The challenge of dry eye diagnosis. Clin Ophthalmol. 2008;2(1):31–55. | |
Doughty MG, Naase T, Donald C, Hamilton L, Button NF. Visualisation of “Marx’s line” along the marginal eyelid conjunctiva of human subjects with lissamine green dye. Ophthalmic Physiol Opt. 2004;24(1):1–7. | |
Macri A, Pflugfelder S. Correlation of the Schirmer 1 and fluorescein 1 clearance tests with the severity of corneal epithelial and eyelid disease. Arch Ophthalmol. 2000;118(12):1632–1638. | |
Yokoi N, Mossa F, Tiffany JM, Bron AJ. Assessment of meibomian gland function in dry eye using meibometry. Arch Ophthalmol. 1999;117(6):723–729. | |
Schaumberg DA, Nichols JJ, Papas EB, Tong L, Uchino M, Nichols KK. The international workshop on meibomian gland dysfunction: report of the subcommittee on the epidemiology of, and associated risk factors for, MGD. Invest Ophthalmol Vis Sci. 2011;52:1994–2005. | |
Shimazaki J, Goto E, Ono M, Shimmura S, Tsubota K. Meibomian gland dysfunction in patients with sjogren syndrome. Ophthalmology. 1998;105:1485–1488. | |
McCulley JP. Blepharoconjunctivitis. Int Ophthalmol Clin. 1984;24:65–77. | |
Bhandari V, Reddy JK. Blepharitis: always remember demodex. Middle East Afr J Ophthalmol. 2014;21(4):317–320. | |
Zengin N, Tol H, Balevi S, Gunduz K, Okudan S, Endogru H. Tear film and meibomian gland functions in psoriasis. Acta Ophthalmol Scand. 1996;74:358–360. | |
Akpek EK, Merchant A, Pinar V, Foster CS. Ocular rosacea: patient characteristics and follow-up. Ophthalmology. 1997;104:1863–1867. | |
Alvarenga LS, Mannis MJ. Ocular rosacea. Ocul Surf. 2005;3:41–58. | |
Sotozono C, Ang LP, Koizumi N, et al. New grading system for the evaluation of chronic ocular manifestations in patients with Stevens-Johnson Syndrome. Ophthalmology. 2007;114:1249–1302. | |
Ogawa Y, Okamoto S, Wakui M, et al. Dry eye after haematopoietic stem cell transplantation. Br J Ophthalmol. 1999;83:1125–1130. | |
Kaercher T. Ocular symptoms and signs in patients with ectodermal dysplasia syndromes. Graefes Arch Clin Exp Ophthalmol. 2004;242:495–500. | |
Arita R, Itoh K, Inoue K, Kuchiba A, Yamaguchi T, Amano S. Contact lens wear is associated with decrease of meibomian glands. Ophthalmology. 2009;116:379–384. | |
Geerling G, Tauber J, Baudouin C, et al. The international workshop on meibomian gland dysfunction: report of the subcommittee on management and treatment of meibomian gland dysfunction. Invest Ophthalmol Vis Sci. 2011;52:2050–2064. | |
Korb DR, Grenier JV. Increase in tear film lipid layer thickness following treatment with warm compresses in patients with meibomian gland dysfunction. Eye Contact Lens. 2003;29:96–99. | |
Mori A, Oguchi Y, Goto E, et al. Efficacy and safety of infrared warming of the eyelids. Cornea. 1999;18:188–193. | |
Mori A, Shimazaki J, Shimmura S, Fujishima H, Oguchi Y, Tsubota K. Disposable eyelid warming device for the treatment of meibomian gland dysfunction. Jpn J Ophthalmol. 2003;47:578–586. | |
Matsumoto Y, Dogru M, Goto E, et al. Efficacy of a new warm moist air device on tear functions of patients with simple meibomian gland dysfunction. Cornea. 2006;25:644–650. | |
Freedman HL, Preston KL. Heat retention in varieties of warm compresses: a comparison between warm soaks, hard-boiled eggs and the re-heater. Ophthalmic Surg. 1989;20:846–848. | |
Bron AJ, Tiffany JM, Gouveia SM, Yokoi N, Voon LW. Functional aspects of the tear film lipid layer. Exp Eye Res. 2004;78:347–360. | |
Korb DR, Blackie CA. Meibomian gland therapeutic expression: quantifying the applied pressure and the limitation of resulting pain. Eye Contact Lens. 2011;37(5):298–301. | |
Romero JM, Biser SA, Perry HD, et al. Conservative treatment of meibomian gland dysfunction. Eye Contact Lens. 2004;30:14–19. | |
Key JE. A comparative study of eyelid cleaning regimens in chronic blepharitis. CLAO J. 1996;22:209–212. | |
Paugh JR, Knapp LL, Martinson JR, Hom MM. Meibomian therapy in problematic contact lens wear. Optom Vis Sci. 1990;67:803–806. | |
Guillon M, Maissa C, Wong S. Symptomatic relief associated with eyelid hygiene in anterior blepharitis and MGD. Eye Contact Lens. 2012;38(5):306–312. | |
Pinna A, Piccinini P, Carta F. Effect of oral linoleic and gamma-linoleic acid on meibomian gland dysfunction. Cornea. 2007;26(3):260–264. | |
Bhargava R, Kumar P, Kumar M, Mehra N, Mishra A. A randomized controlled trial of omega-3 fatty acids in dry eye syndrome. Int J Ophthalmol. 2013;6(6):811–816. | |
Mascai MS. The role of omega-3 dietary supplementation in blepharitis and meibomian gland dysfunction (an AOS thesis). Trans Am Ophthalmol Soc. 2008;106:336–356. | |
Maissa C, Guillon M, Simmons P, Vehige J. Effect of castor oil emulsion on tear film composition and stability. Cont Lens Anterior Eye. 2010; 33(2):76–82. | |
Aguilar AJ, Marquez MI, Albera PA, Tredicce JL, Berra A. Effects of Systane Balance on noninvasive tear film break-up time in patients with lipid-deficient dry eye. Clin Ophthalmol. 2014;8:2365–2372. | |
Foulks GN, Borchman D, Yappert M, Kakar S. Topical azithromycin and oral doxycycline therapy of meibomian gland dysfunction: a comparative clinical and spectroscopic pilot study. Cornea. 2013;32(1):44–53. | |
Haque RM, Torkildsen GL, Brubaker K, et al. Multicenter open-label study evaluating the efficacy of azithromycin ophthalmic solution 1% on the signs and symptoms of subjects with blepharitis. Cornea. 2010; 29(8):871–877. | |
Opitz DL, Tyler KF. Efficacy of azithromycin 1% ophthalmic solution for treatment of ocular surface disease from posterior blepharitis. Clin Exp Optom. 2011;94(2):200–206. | |
Mantelli F, Di Zazzo A, Sacchetti M, Dianzani C, Lambiase A, Bonini S. Topical azithromycin as a novel treatment for ocular rosacea. Ocul Immunol Inflamm. 2013;21(5):371–377. | |
Smith VA, Khan-Lim D, Anderson L, Cook SD, Dick AD. Does orally administered doxycycline reach the tear film? Br J Ophthalmol. 2008; 92(6):856–859. | |
Lee H, Min K, Kim EK, Kim TI. Minocycline controls clinical outcomes and inflammatory cytokines in moderate and severe meibomian gland dysfunction. Am J Ophthalmol. 2012;154(6):949–957. | |
Souchier M, Joffre C, Grégoire S, et al. Changes in meibomian fatty acids and clinical signs in patients with meibomian gland dysfunction after minocycline treatment. Br J Ophthalmol. 2008;92(6):819–822. | |
Yoo SE, Lee DC, Chang MH. The effect of low-dose doxycycline therapy in chronic meibomian gland dysfunction. Korean J Ophthalmol. 2005;19(4):258–263. | |
Igami TZ, Holzchuh R, Osaki TH, Santo RM, Kara-Jose N, Hida RY. Oral azithromycin for treatment of posterior blepharitis. Cornea. 2011;30(10):1145–1149. | |
Kashkouli MB, Fazel AJ, Kiavash V, Nojomi M, Ghiasian L. Oral azithromycin versus doxycycline in meibomian gland dysfunction: a randomized double-masked open-label clinical trial. Br J Ophthalmol. 2015;99(2):199–204. | |
Prabhasawat P, Tesavibul N, Mahawong W. A randomized double-masked study of 0.05% cyclosporine ophthalmic emulsion in the treatment of meibomian gland dysfunction. Cornea. 2012;31(12):1386–1393. | |
Schechter BA, Katz RS, Friedman LS. Efficacy of topical cyclosporine for the treatment of ocular rosacea. Adv Ther. 2009;26(6):651–659. | |
Lee H, Chung B, Kim KS, Seo KY, Choi BJ, Kim TI. Effects of topical loteprednol etabonate on tear cytokines and clinical outcomes in moderate and severe meibomian gland dysfunction: randomized clinical trial. Am J Ophthalmol. 2014;158(6):1172–1183. | |
Korb DR, Blackie CA. Debridement-scaling: a new procedure that increases meibomian gland function and reduces dry eye symptoms. Cornea. 2013;32(12):1554–1557. | |
Maskin SL. Intraductal meibomian gland probing relieves symptoms of obstructive meibomian gland dysfunction. Cornea. 2010;29(10):1145–1152. | |
Wladis EJ. Intraductal meibomian gland probing in the management of ocular rosacea. Ophthal Plast Reconstr Surg. 2012;28(6):416–418. | |
Lewis JS. Sidebar: therapeutic device for DED treatment uses thermoelectic heat. Adv Ocul Care. 2014; May/June:50. | |
Mibo Medical Group. Available from: http://mibomedicalgroup.com/clinical-research/. Accessed June 1, 2015. | |
Finis D, Hayajneh J, König C, Borrelli M, Schrader S, Geerling G. Evaluation of an automated thermodynamic treatment (LipiFlow) system for meibomian gland dysfunction: a prospective, randomized, observer-masked trial. Ocul Surf. 2014;12(2):146–164. | |
Finis D, König C, Hayajneh J, Borrelli M, Schrader S, Geerling G. Six-month effects of a thermodynamic treatment for MGD and implications of meibomian gland atrophy. Cornea. 2014;33(12):1265–1270. | |
Greiner JV. Long-term (12 month) improvement in meibomian gland function and reduced dry eye symptoms with a single thermal pulsation treatment. Clin Experiment Ophthalmol. 2013;41(6):524–530. | |
Raulin C, Greve B, Grema H. IPL technology: a review. Lasers Surg Med. 2003;32:78–87. | |
Craig JP, Chen YH, Turnbull PR. Prospective trial of intense pulsed light for the treatment of meibomian gland function. Invest Ophthalmol Vis Sci. 2015;56(3):1965–1970. | |
Toyos R, McGill W, Briscoe D. Intense pulsed light treatment for dry eye disease due to meibomian gland dysfunction; a 3-year retrospective study. Photomed Laser Surg. 2015;33(1):41–46. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.