Back to Journals » International Journal of Women's Health » Volume 11
Depressive symptoms during pregnancy and postpartum in women and use of antidepressant treatment – a longitudinal cohort study
Authors Sunnqvist C, Sjöström K , Finnbogadóttir H
Received 31 August 2018
Accepted for publication 19 December 2018
Published 7 February 2019 Volume 2019:11 Pages 109—117
DOI https://doi.org/10.2147/IJWH.S185930
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Elie Al-Chaer
Charlotta Sunnqvist, Karin Sjöström, Hafrún Finnbogadóttir
Faculty of Health and Society, Department of Care Science, Malmö University, Malmö, Sweden
Objective: The aim of this study was to investigate whether women, who reported “symptoms of depression” during pregnancy and up to 1.5 years postpartum, who reported domestic violence or not, were treated with antidepressant medication.
Patients and methods: A prospective longitudinal cohort study recruited primi- and multiparous women (n=1,939). The Edinburgh Postnatal Depression Scale (EPDS), the NorVold Abuse Questionnaire, and a questionnaire about medication during pregnancy were distributed and administered three times, during early pregnancy, late pregnancy, and the postpartum period. Antidepressant medication was compared between women with EPDS scores
Results: EPDS scores ≥13 were detected in 10.1% of the women during the whole pregnancy, of those 6.2% had depressive symptoms already in early pregnancy and 10.0 % during the postpartum period. Women with EPDS scores ≥13 and non-exposure to domestic violence were more often non-medicated (P<0.001). None of the women with EPDS scores ≥13 exposed to domestic violence had received any antidepressant medication, albeit the relationship was statistically nonsignificant.
Conclusion: Pregnant women who experienced themselves as having several depressive symptoms, social vulnerability, and even a history of domestic violence, did not receive any antidepressant treatment during pregnancy nor postpartum. This study shows the importance of detecting depressive symptoms during early pregnancy and a need for standardized screening methods.
Keywords: antidepressant treatment, depression, domestic violence, postpartum, pregnancy, untreated, reproductive age
Introduction
Women have an increased risk of experiencing depressive disorders during pregnancy,1 and the risk is even greater during the postpartum period.2 A review of the literature has revealed that women who are at high risk, eg, those with experience of lifetime abuse, have a significantly increased risk for depression during both the prenatal and the postpartum period.3,4 Postpartum depressive symptom has a prevalence of ~16% in Australian population, and the risk factors for developing postnatal depression include a history of depression before and/or during pregnancy, dysfunctional partner relationship, multiple stressful life events, low social support, low income, and fewer years of education.5 In addition, Finnbogadóttir and Dykes6 showed that symptoms of depression both during pregnancy and up to 1–1.5 years postpartum were associated with domestic violence. Untreated postpartum depression might negatively affect the interaction between mother and child, for example, by reducing sensitivity and availability to the needs of the infant.4 In Sweden, there is no general praxis at the Antenatal Care (ANC) units regarding screening for depression during pregnancy. At the Child Welfare Centers (CWC), however, mothers at 6–8 weeks postpartum are screened for postnatal depression with the Edinburgh Postnatal Depression Scale (EPDS).7
Several studies have found that intimate partner violence (the most frequent type of domestic violence) is significantly associated with both prenatal and postnatal depression.3,4 The presence of severe symptoms of depression detected in early pregnancy,8 late pregnancy,6 and postpartum6 may be a predictive factor for exposure to domestic violence. Thus, not only is untreated depression during pregnancy and postpartum a major risk factor for both mothers’ and infants’ health, but depressive symptoms may also be a result of previous and/or present exposure to domestic violence.6,8 The treatment of pregnant women with depression is complex and requires both evaluation of risks and benefits, and most pregnant women with depression do not get treatment despite devastating effects on women, infants, and families.9 A systematic review from 2015 found that untreated depression could lead to adverse effects on the developing fetus, such as hyperactivity or irregular fetal heart rate and increased rates of premature deaths and neonatal intensive care admissions in newborns.10 Also, women with a history of depression who discontinue antidepressant treatment during pregnancy are at much higher risk of relapse than those who continue their medication. Previous studies have found that antidepressant medical treatment drops from 70% to 27% during pregnancy, and most women do not receive further treatment beyond 6 weeks of gestation.10 There is evidence that pregnant women with major depressive disorder require medical therapy11 and psychotherapy for mild and moderate depressive disorders.12 According to a review by O’Connor et al,12 the absolute risk of antidepressant during pregnancy appear to be small, and cognitive behavioral therapy may be an effective alternative treatment approach for mild and moderate depressive disorders. Results from a previous longitudinal study showed that severe symptoms of depression were associated with domestic violence.6 The distressing situation, being exposed to domestic violence and having a depression weakens the mother’s ability to take care of her newborn child and, therefore, an antidepressant treatment may be helpful for the mother to cope with this vulnerable situation. A woman who is depressed in pregnancy faces the difficult process of weighing the pros and cons of starting antidepressant treatment.13 However, clinicians and patients should carefully and individually weigh maintenance therapy against the small possible risk of neurodevelopmental problems suggested by the currently available literature.14 Therefore, there is a need to explore depressive symptoms and the prevalence of antidepressant medication in the high-risk group of pregnant women who are exposed to domestic violence.
The aim of this study was to investigate whether women, who reported “symptoms of depression” during pregnancy and up to 1.5 years postpartum, with or without exposure to domestic violence, were treated with antidepressant medication.
Patients and methods
The present study is a cohort study with a longitudinal design and a part of a larger project, Pregnant Women and New Mothers’ Health and Life Experience, where the cohort consisted of 1,939 pregnant women, recruited in early pregnancy, in gestational week 13 (mean 12.8, SD ±5.11).8 The inclusion criteria were both primi- and multiparous women ≥18 years of age, registered at ANC when pregnant, and who could understand and write Swedish or English. The recruitment to the study occurred between March 2012 and September 2013 in a multicultural area in the southwest of Sweden, and data collection continued until the end of April 2015. The population comprises of all listed pregnant women at 17 ANCs situated in the multicultural city (n=7), the University City (n=4), and smaller municipalities (n=6). Also, one ANC providing specialized care for complex pregnancies such as women with diabetes and one for women with history of drug abuse in need of extra support were also included. Four of the ANCs were private care facilities. At the time for recruitment, the participants were fully informed about the purpose of the study. They received verbal and written information about the study from their midwife and were invited to respond to the questionnaires in a private place at the ANC facility. The women were promised confidentiality, and they were encouraged to feel free to disclose whether they were living in a violent relationship. Professional help was provided for those respondents who came forward and asked for help. The participants were requested to answer three questionnaires, ie, on two occasions during pregnancy at their ANC (Q-I and Q-II) and once 1–1.5 years postpartum at their CWC (Q-III). The total cohort comprised 1,939 women and they completed the first questionnaire (Q-I) in “early pregnancy”. The second questionnaire II was completed at gestational week 34 or in “late pregnancy” (mean 33.9, SD ±2.20 weeks), with a response rate of 78.8% (N=1,527), and the final questionnaire III (Q-III) was completed at the end of April 2015 by 37.2% (N = 732) women who who visited their CWC 1–1.5 years postpartum (Figure 1).6
  | Figure 1 Flowchart of the distributed and received answers for Q-I–III.6 |
Questionnaires
The questionnaires consisted mainly of four validated instruments. The EPDS is intended to screen risk of depression in the postnatal period but may also be used during pregnancy.15 The EPDS detects common symptoms of depression and consists of ten items. Each item is rated from 0 to 3, with higher scores indicating more perceived symptoms of depression. The participants were requested to rate each statement with regard to how they had felt during the past 7 days (Q-I–III). The cutoff score for depression was originally set at 12/13.15 The EPDS has a 72% sensitivity and 88% specificity for women postpartum but has a lower degree of detection for depression in pregnancy.16 The EPDS was validated on a Swedish community sample against criteria for major depression according to the DSM-III-R.17 We chose the cutoff score to be 13.
The Alcohol Use Disorders Identification Test (AUDIT)18 was used at each time of questionnaire administration (Q-I–III). The first item of the AUDIT concerns the frequency of drinking alcohol. The given answers were “never” or the amount of beverage consumption.
The NorVold Abuse Questionnaire (NorAQ)19 was the main instrument used to investigate emotional, physical, and sexual abuse and level of experienced violence for <18 years of age (during childhood) and ≥18 years of age (adulthood) and is designed for use in and validated in Nordic countries.19 A modified question from the Abuse Assessment Screen20 was used to investigate current partner abuse during pregnancy by answering yes/no, and if yes “by whom”.
One question regarding the pharmacological treatment the women had used during the last year was included in all three questionnaires with the purpose of covering the time period before pregnancy, during pregnancy, and postpartum. The pharmacological treatment alternatives were the following: sleeping pills, pain relievers, antidepressants, sedatives, amphetamine, cocaine, or other psychotropic street drugs. All alternatives were rated as follows: never, occasionally, short period, long period, and all the time. In this study, only the use of antidepressant drugs was analyzed.
Definitions
Domestic violence was defined according to WHO’s definition as physical, sexual, psychological or emotional violence, or threats of physical or sexual violence that are inflicted on a pregnant woman by a family member, ie, an intimate male partner, marital/cohabiting partner, parents, siblings, or a person very well known to the family, or a significant other (ie, former partner), when such violence often takes place in the home.21
A history of violence was defined as a lifetime experience of emotional, physical, or sexual abuse occurring during childhood (<18 years), adulthood (≥18 years), or both, regardless of the level of abuse or the perpetrator’s identity, in accordance with the operationalization of the questions in the NorAQ.21 Also, we used the definitions determined by Swahnberg and Wijma et al19 for severity of abuse, which classifies abuse as mild, moderate, or severe, and the type of abuse used. Any level of any type of violence was regarded as being exposed to violence.
Classification of the sociodemographic variables and medication
The sociodemographic variables used in this study are shown in Table 1.
Three age groups were created: 18–25, 26–34, and ≥35 years, and language was selected as Swedish or a foreign language spoken at home. Cohabiting status was dichotomized as being single/living apart or as cohabitant/married. Educational status was divided into two groups: low educational status, ie, basic education and high school, and high educational status, ie, above high school, including university. Employment status was dichotomized as being employed (including parental leave and studying) or unemployed (sick leave). Financial distress was dichotomized as “no” (no problem) or “yes” (serious financial distress). Smoking/using wet tobacco was dichotomized as “yes” or “no”, ie, yes, if the woman was a daily smoker or wet-tobacco user at some point during pregnancy, and no, if never smoked or used wet-tobacco or stopped before pregnancy. Alcohol consumption was dichotomized as “yes” (at least once a month) or “no” (never). For antidepressant medication, the answers were classified as “no medication”, “medication in periods”, and “constant medication”.
Statistical methods
All data were based on the women’s answers from the questionnaires (Q-I, Q-II, and Q-III). Descriptive statistics were used to show the prevalence and percent of depressive scores during early and late pregnancy, as well as 1–1.5 years postpartum. Chi-square analysis was used to investigate differences in sociodemographic and lifestyle factors in early pregnancy in relation to depressive symptom scores. The variable for depression was computed based on the sum of EPDS scores, ie, symptoms of depression during pregnancy or postpartum, whereby an optimal cutoff of ≥13 was chosen as representing the presence of symptoms of depression. Women who did not report any depressive symptoms at all were analyzed as a separate group (n=130). There were no differences in sociodemographic characteristics between those with a score of zero and those with a score of 1–12 on EPDS, and, therefore, the EPDS variable was dichotomized as EPDS scores <13 or ≥13. Statistical significance was considered at P<0.05 (two-tailed). Statistical analyses were performed using the SPSS version 22.0 for Windows.
Ethics approval and informed consent
The research was conducted according to the principles stated in the World Medical Association Declaration of Helsinki41 and the WHO’s ethical and safety recommendations for research on violence against women.42 Written informed consent was obtained before the participants received their first questionnaire. The participants were informed about the law of Swedish Data Inspection. All questionnaires were collected and coded by the third author and were kept in a locked safe. Approval for the study was obtained from the Regional Ethical Review Board where this study took place (Dnr: 640/2008).
Results
Women with scores of depressive symptoms (EPDS scores ≥13) compared to women with EPDS scores <13, were significantly younger, more often speaking a foreign language at home, single/living apart, less educated, unemployed, financially distressed, and smokers (Table 1).
Prevalence of depressive symptoms
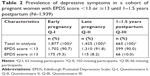
The prevalence of depressive symptoms (EPDS scores ≥13) were in early pregnancy (Q-I) 9.3%, in late pregnancy 8.2% (Q-II), and 10.0% postpartum up to 1.5 years (Q-III) (Table 2).
In early pregnancy (Q-I), 9.3% (n=175) of the women reported scores of depressive symptoms (EPDS score ≥13), and 69.1% (n=121) of them reported it only in the early pregnancy. Almost 34% (n=59) reported scores of depressive symptoms (EPDS score ≥13) only in late pregnancy (Q-II), and 22.7% (n=38) both in early and late pregnancy, but not postpartum. Amply 5% (n=9) reported scores of depressive symptoms (EPDS score ≥13) in late pregnancy as well as postpartum, and additionally 5.1% (n=9) had high scores at all three time points of measures. Total 14.6% (n=284) of the study participants (n=1,939) reported scores of depressive symptoms (EPDS score ≥13) one or more times during pregnancy and/or up to 1.5 years postpartum.
Women exposed and nonexposed to domestic violence
Women with no history of domestic violence and with scores of depressive symptoms were significantly more often non-medicated (P<0.001) compared to women with scores under cutoff of depressive symptoms (EPDS score <13), throughout the study (Q-I–III). Among women exposed to domestic violence with scores of depressive symptoms (EPDS score ≥13) throughout the study (Q-I–III) were more often non-medicated compared to women with under cutoff scores of depressive symptoms (EPDS score <13), but these results did not reach statistical significance (Table 3).
The group of women with scores of depressive symptoms and antidepressant medication
During pregnancy (Q-I and Q-II), 10.1% of women belonged to the group with scores of depressive symptoms (EPDS score ≥13), and of those women, 6.2% had scores of depressive symptoms (EPDS score ≥13) already at the first visit at ANC. The prevalence of women with scores of depressive symptoms (EPDS score ≥13) and no antidepressant medication during pregnancy was 10.8% (n=190) (exclusively presented in the text).
During early pregnancy (Q-I) and late pregnancy (Q-II), the majority of women with scores of depressive symptoms (EPDS score ≥13) who had been exposed to domestic violence did not receive antidepressant medication (80% and 85.7%, respectively). At postpartum (Q-III), none of the women with scores of depressive symptoms (EPDS score ≥13) exposed to domestic violence had received antidepressant medication (100%) (Table 3).
Discussion
We found that all women exposed to domestic violence with scores of depressive symptoms throughout pregnancy and postpartum were untreated with antidepressant medication. We also found that nonexposed women, with scores of depressive symptoms, were barely treated with antidepressant medication. Despite known risk factors for depression, such as, psychosocial vulnerability and ongoing or previous exposure to domestic violence, these risk factors did not lead to clinical identification.
We chose to study maternal depressive symptoms on two occasions during pregnancy and on one occasion during postpartum, ie, 1.5 years after birth. It has been found that perinatal depression occurs during pregnancy or in the first 12 months after birth and is one of the most common medical complications during pregnancy.22 In a review by Goodman,23 postpartum depression occurs within the first couple of weeks after giving birth, but for some women, the symptoms of depression occur later during the first postpartum year. The symptoms of depression may continue for 2 years after giving birth.23
A limitation in the study design was that no clinical assessment of depression could be performed, and, therefore, it is unknown whether the study participants would meet the diagnostic requirements for clinical depression. Thus, the women in the group with symptoms of depression were those with EPDS scores ≥13. Screening with EPDS is valuable but unfortunately not sufficient, because semi-structured interviews would be needed to confirm a diagnosis of depression. Nevertheless, according to Statens Beredning för Medicinsk Utvärdering [Swedish Agency for Health Technology Assessment and Assessment of Social Services],16 EPDS has the advantage of being able to detect several women with depressive symptoms. In addition, the data offer no information if the respondents have been offered or undertaken psychological treatment for depressive symptoms. Furthermore, there was a nonsignificant trend between the report of domestic violence and untreated depression, which may be caused by a lack of power. This in turn may be the result of the well-known difficulties in reporting domestic violence.
The strength of the current study is the large sample size as well as the use of a well-defined cohort. This longitudinal study, based on prospective data, allowed for comparison between those who had more symptoms of depression and those who did not. However, the risk of dropout over time in this type of study is well known and was present in the current study. Another strength was the use of validated instruments included in the questionnaires used.15,19
In this study, women who had symptoms of depression also had less favorable sociodemographic and life-style factors. They were younger, single or living apart from the father, had lower educational level, were unemployed, had more financial distress, were smokers, and spoke a foreign language at home. It has been shown that female gender, living alone, having less education, and with previous childhood traumas were risk factors for depression and suicide attempts.24 A recent systematic review showed that the most significant factors associated with antenatal depression or anxiety were lack of partner or social support and history of abuse or domestic violence.25 In addition, some studies show that the offspring of women who experienced significant psychosocial stress already during pregnancy, have an increased risk of later neuropsychiatric illness,26,27 especially, when untreated.28 Children of these vulnerable mothers also may be extra vulnerable right from birth.29
We also found that women with symptoms of depression, besides being socially vulnerable, also had a risk factor in having been exposed to domestic violence. Previous study has shown a clear association between exposure to domestic violence during early pregnancy as well as in late pregnancy and symptoms of depression.6 Obstacles to early recognition of current or previous exposure to violence may be the lack of local guidelines and lack of available support. Midwives may lack the confidence or knowledge about this matter and furthermore may fear the perpetrator.30 Since 2014, the National Board of Health and Welfare in Sweden has recommended that all women attending ANCs when pregnant should be asked about any experience of violence.31 Nearly 80% of all pregnant women in Sweden were asked about any experience of violence at their ANC during the year 2014.32 However, screening for symptoms of depression is not a routine until 6–8 weeks postpartum at CWCs. It would have been wise to screen for depressive symptoms at the same time as pregnant women were asked about their experience of violence. Another obstacle was the survivors’ fear of authorities and that the social welfare department would take their children from them if they disclosed a violent relationship.30 All in all, to be exposed to domestic violence as well as having symptoms of depression when pregnant is a complex issue, and there is a need of good cooperation between the different health care providers as well as social welfare authorities to ensure the best outcome for the mother-to-be and the unborn infant’s health.
Several studies concerning the general population have shown that only a minority of the depressed patients had received adequate antidepressant therapy before fatal outcome.33 Depression is the most common mental disorder worldwide and is the primary cause of suicide and long-term suffering;2 the lifetime prevalence in women is almost 50%.34 Maternal suicide attempts and suicide are the most serious complications to depression in the perinatal and postnatal time periods.35 Moreover, untreated depression during pregnancy has also been related to lower intellectual and cognitive abilities among offspring,28 and in a recent systematic review and meta-analysis, evidence was found that untreated depression was associated with a significantly increased risk of preterm birth and low birth weight. Furthermore, it has been found that infants born to depressed mothers were admitted to neonatal intensive care twice as often and had a shorter duration of breastfeeding than nondepressed mothers.11 Several studies have reported that depressed mothers are not able to provide the loving and consistent care that the child needs, which has a negative impact for mother and infant attachment.11,36
There is an ongoing debate regarding treatment with antidepressants during pregnancy since antidepressant medication is able to pass through the placental barrier and, therefore, may pose a risk for adverse fetal development.37,38 Nulman et al28 found that there was no deviance in neurodevelopment among offspring to mothers receiving selective serotonin reuptake inhibitors (SSRIs) during pregnancy compared to siblings. However, Brandlistuen et al39 found a relationship among siblings exposed to SSRIs prenatally and anxiety at 36 months, compared to a nonexposed sibling. Anxiety was specific and not related to other behavioral problems in the child. Unfortunately, there are no controlled, randomized trials regarding the use of antidepressants in pregnancy, and according to a review from 2014,40 there is lack of evidence from good quality studies that clinicians and patients should refrain from the initiation of SSRI treatment during pregnancy or that such treatment should be discontinued. However, clinicians and patients should carefully and individually weigh maintenance therapy against the small possible risk of neurodevelopmental problems suggested by the currently available literature.40
Conclusion
This study supports the importance of detecting risks for maternal depression in a standardized manner already during early pregnancy. For pregnant women who reported several depressive symptoms and social vulnerability with a history of domestic violence, these risk factors did not lead to clinical identification nor to any antidepressant treatment during pregnancy or postpartum. The findings show the clinical challenge in detecting this important group of women during an especially vulnerable time in their life. The need for standardized screening methods for depression both during pregnancy and postpartum is emphasized.
Acknowledgments
The authors would like to thank all the midwives who conducted the recruitment as well as all the CWC nurses who helped with the administration of the postpartum questionnaire. Special thanks go to Lars Wahlgren for his excellent statistical support. The Swedish Crime Victim Compensation and Support Authority contributed with funding for this research (Dnr 09082/2014; Dnr 09097/2015).
Author contributions
HF conceived the study and performed the collection of the data, and all authors contributed toward data analysis, drafting and critically revising the paper, gave final approval of the version to be published, and agreed to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Dossett EC. Perinatal depression. Obstet Gynecol Clin North Am. 2008;35(3):419–434. | ||
Kessler RC. Epidemiology of women and depression. J Affect Disord. 2003;74(1):5–13. | ||
Howard LM, Oram S, Galley H, Trevillion K, Feder G. Domestic violence and perinatal mental disorders: a systematic review and meta-analysis. PLoS Med. 2013;10(5):e1001452. | ||
Alvarez-Segura M, Garcia-Esteve L, Torres A, et al. Are women with a history of abuse more vulnerable to perinatal depressive symptoms? A systematic review. Arch Womens Ment Health. 2014;17(5):343–357. | ||
Woolhouse H, Gartland D, Hegarty K, Donath S, Brown SJ. Depressive symptoms and intimate partner violence in the 12 months after childbirth: a prospective pregnancy cohort study. BJOG. 2012;119(3):315–323. | ||
Finnbogadóttir H, Dykes AK. Increasing prevalence and incidence of domestic violence during the pregnancy and one and a half year postpartum, as well as risk factors: a longitudinal cohort study in southern Sweden. BMC Pregnancy Childbirth. 2016;16(1):327. | ||
Wickberg B. Depression hos Nyblivna Mammor och Screening med EPDS [Depression Among new Mothers and Screening With the EPDS]; Revised March 23, 2016. Rikshandboken Barnhälsovården [National manual of Child Health Services]. Available from: https://www.rikshandboken-bhv.se/metoder--riktlinjer/screening-med-epds/. Accessed September 5, 2016. Swedish. | ||
Finnbogadóttir H, Dykes AK, Wann-Hansson C. Prevalence of domestic violence during pregnancy and related risk factors: a cross-sectional study in southern Sweden. BMC Womens Health. 2014;14:63. | ||
Weinreb L, Byatt N, Moore Simas TA, Tenner K, Savageau JA. What happens to mental health treatment during pregnancy? women’s experience with prescribing providers. Psychiatr Q. 2014;85(3):349–355. | ||
Gentile S. Untreated depression during pregnancy: short- and long-term effects in offspring. A systematic review. Neuroscience. 2017;342:154–166. | ||
Bowen A, Bowen R, Butt P, Rahman K, Muhajarine N. Patterns of depression and treatment in pregnant and postpartum women. Can J Psychiatry. 2012;57(3):161–167. | ||
O’Connor E, Rossom RC, Henninger M, Groom HC, Burda BU. Primary care screening for and treatment of depression in pregnant and postpartum women: evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2016;315(4):388–406. | ||
Pariante CM. Depression and antidepressants in pregnancy: molecular and psychosocial mechanisms affecting offspring’s physical and mental health. Neuropsychopharmacology. 2015;40(1):246–247. | ||
Sujan AC, Rickert ME, Öberg AS, et al. Associations of maternal antidepressant use during the first trimester of pregnancy with preterm birth, small for gestational age, autism spectrum disorder, and attention-deficit/hyperactivity disorder in offspring. JAMA. 2017;317(15):1553–1562. | ||
Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression. Development of the 10-item Edinburgh postnatal depression scale. Br J Psychiatry. 1987;150:782c786. | ||
Statens Beredning för Medicinsk Utvärdering (SBU) [Swedish Agency for Health Technology Assessment and Assessment of Social Services]. Diagnostik och uppföljning av förstämningssyndrom – en systematisk litteraturöversikt. Rapport 212 [Diagnosis and monitoring of mood disorders – a systematic literature overview. Report 212]. Available from: https://www.sbu.se/212 Accessed September 5, 2016. Swedish. | ||
Wickberg B, Hwang CP. The Edinburgh postnatal depression scale: validation on a Swedish community sample. Acta Psychiatr Scand. 1996;94(3):181–184. | ||
Saunders JB, Aasland OG, Babor TF, de la Fuente JR, Grant M. Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption – II. Addiction. 1993;88(6):791–804. | ||
Swahnberg IM, Wijma B. The NorVold abuse questionnaire (NorAQ): validation of New measures of emotional, physical, and sexual abuse, and abuse in the health care system among women. Eur J Public Health. 2003;13(4):361–366. | ||
McFarlane J, Parker B, Soeken K, Bullock L. Abuse assessment screen. JAMA. 1992;267:3176–3178. | ||
Krug EG, Ll D, Mercy J, Zwi AB, Lozano R. World Report on Violence and Health. Geneva, world Health organization; 2002. | ||
Committee on Obstetric Practice. The American College of obstetricians and Gynecologists Committee opinion no. 630. Screening for perinatal depression. Obstet Gynecol. 2015;125(5):1268–1271. | ||
Goodman JH. Postpartum depression beyond the early postpartum period. J Obstet Gynecol Neonatal Nurs. 2004;33(4):410–420. | ||
Ten Have M, van Dorsselaer S, de Graaf R. Prevalence and risk factors for first onset of suicidal behaviors in the Netherlands mental health survey and incidence Study-2. J Affect Disord. 2013;147(1–3):205–211. | ||
Biaggi A, Conroy S, Pawlby S, Pariante CM. Identifying the women at risk of antenatal anxiety and depression: a systematic review. J Affect Disord. 2016;191:62–77. | ||
Khashan AS, Abel KM, McNamee R, et al. Higher risk of offspring schizophrenia following antenatal maternal exposure to severe adverse life events. Arch Gen Psychiatry. 2008;65(2):146–152. | ||
Kinney DK, Munir KM, Crowley DJ, Miller AM. Prenatal stress and risk for autism. Neurosci Biobehav Rev. 2008;32(8):1519–1532. | ||
Nulman I, Koren G, Rovet J, Barrera M, Streiner DL, Feldman BM. Neurodevelopment of children prenatally exposed to selective reuptake inhibitor antidepressants: Toronto sibling study. J Clin Psychiatry. 2015;76(7):e842–e847. | ||
Provençal N, Binder EB. The effects of early life stress on the epigenome: from the womb to adulthood and even before. Exp Neurol. 2015;268:10–20. | ||
Finnbogadóttir H, Dykes AK. Midwives’ awareness and experiences regarding domestic violence among pregnant women in southern Sweden. Midwifery. 2012;28(2):181–189. | ||
Socialstyrelsen (The National Board of Health and Welfare). Att vilja se, vilja veta och att våga fråga. Vägledning för att öka förutsättningarna att upptäcka våldsutsatthet (In Swedish). Available from: http://www.socialstyrelsen.se/Lists/Artikelkatalog/Attachments/19568/2014-10-30.pdf (ISBN:978-91-7555-224-8):3–42. Accessed November 15, 2014. | ||
Graviditetsregistret (The Swedish Pregnancy Register). Graviditetsregistret-mödrahälsovård-fosterdiagnostik-förlossning (In Swedish). 2015:2–99. Available from: https://www.medscinet.com/GR/default.aspx. Accessed September 15, 2015. | ||
Isacsson G, Rich CL, Jureidini J, Raven M. The increased use of antidepressants has contributed to the worldwide reduction in suicide rates. Br J Psychiatry. 2010;196(6):429–433. | ||
World Health Organization. Gender and women’s mental health. Gender disparities and mental health: The Facts; 2013. Available from: https://www.who.int/mental_health/prevention/genderwomen/en/ Accessed November 3, 2016. | ||
Orsolini L, Valchera A, Vecchiotti R, et al. Suicide during perinatal period: epidemiology, risk factors, and clinical correlates. Front Psychiatry. 2016;7:138. | ||
Brummelte S, Galea LA. Postpartum depression: etiology, treatment and consequences for maternal care. Horm Behav. 2016;77:153–166. | ||
Loughhead AM, Stowe ZN, Newport DJ, Ritchie JC, Devane CL, Owens MJ. Placental passage of tricyclic antidepressants. Biol Psychiatry. 2006;59(3):287–290. | ||
Rampono J, Simmer K, Ilett KF, et al. Placental transfer of SSRI and SNRI antidepressants and effects on the neonate. Pharmacopsychiatry. 2009;42(3):95–100. | ||
Brandlistuen RE, Ystrom E, Eberhard-Gran M, Nulman I, Koren G, Nordeng H. Behavioural effects of fetal antidepressant exposure in a Norwegian cohort of discordant siblings. Int J Epidemiol. 2015;44(4):1397–1407. | ||
El Marroun H, White T, Verhulst FC, Tiemeier H. Maternal use of antidepressant or anxiolytic medication during pregnancy and childhood neurodevelopmental outcomes: a systematic review. Eur Child Adolesc Psychiatry. 2014;23(10):973–992. | ||
WMA General Assembly: Fortaleza, Brazil 2013. World Medical Association Declaration of Helsinki. Ethical Principles for Medical Research Involving Human Subjects. (2013, 10/30). | ||
World Health Organization. Putting women first: Ethical and safety recommendations for research on domestic violence against women; 2001. Available from: http://www.who.int/mediacentre/factsheets/fs239/en/. Accessed January 14, 2016. |
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.