Back to Journals » Risk Management and Healthcare Policy » Volume 13
COVID-19 in Ethiopia: Assessment of How the Ethiopian Government has Executed Administrative Actions and Managed Risk Communications and Community Engagement
Authors Zikargae MH
Received 27 August 2020
Accepted for publication 17 November 2020
Published 3 December 2020 Volume 2020:13 Pages 2803—2810
DOI https://doi.org/10.2147/RMHP.S278234
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Professor Marco Carotenuto
Mekonnen Hailemariam Zikargae
Department of Journalism and Communications, Bahir Dar University, Faculty of Humanities, Bahir Dar, Ethiopia
Correspondence: Mekonnen Hailemariam Zikargae
Bahir Dar University, Bahir Dar, Ethiopia
Email [email protected]
Introduction: Highly communicable nature of the pandemic attributed the COVID-19 response in Ethiopia harsher and dangerous. It has been causing a huge fatality and death toll reported. Besides, a very swift transmission of viruses distributed within 213 countries, including Ethiopia. Therefore, this empirical study investigates all government and stakeholders’ effects in line with identifying the current status found in Ethiopia.
Methods: Qualitative approach of data collections and thematic analysis were used.
Results: The outcomes indicate that COVID-19 situations gain the highest momentum by increasing alarmingly. It shows significant differences after two months since March 2020 it has reported the first case in Ethiopia. The government took several measures ranging from public health emergency response to the state of emergency. The communication strategy and state of emergency are in place to reduce the prospective risks of COVID-19. The strategy segmented the population by tailoring activities of risk communication and community engagement at all levels. The government has strongly obtained various measures like lockdown and a state of emergency. However, it was not strict and has not been heavy-handed that much.
Conclusion: KAP’s practices are inadequate to fight and minimize the impacts of the pandemic. Such negligence among the public and related factors undermined the preparedness and responses towards COVID-19 in Ethiopia. New cases and deaths are non-stoppable. The government is using several strategies and need to strengthen those efforts to mobilize and upbeat the KAP’s of the public through different communication forms to reinforce the existing efforts and alleviate socio-cultural, political, economic factors to drive out COVID-19 among the people. The efforts are building and strengthening up to the standard level of KAP’s while enhancing and promoting existing strategies and the drawing of new documents by focusing on high-risk parts of the population.
Keywords: COVID-19, Ethiopia, risk communication, community empowerment, emergency preparedness, response
Introduction
Novel Coronaviruses are a family of viruses that cause illness of Severe Acute Respiratory Syndrome. The virus was identified and reported for the first time in December 2019 in the city of Wuhan, China.1 It was named COVID-19 disease by the World Health Organization. The disease has affected 213 countries. The number of infected people and death toll are increasing every day. It is a deadlier than 2002-SARS. In January 2020, the WHO announced the 2019 Novel Coronavirus occurrence as a Public Health Emergency and international concern. The WHO also recommended countries should take standard measures and responses to tackle the effects of the viruses.
Following the fast transmission and risk of the virus, the Director of WHO announced the virus as a global pandemic on the 11th of March. Henceforth, the number of cases reported increased to above 22 million as of 20 Aug 2020. As the virus is new, many things are not clear. However, Russia started a production of the vaccine. Russia has produced the first batch of its Coronavirus vaccine as of 19 Aug 2020. It follows that many countries are looking to Russia for getting the vaccine.
COVID-19, since it has appeared in Wuhan, China, has been spread in different countries (213 countries). Ethiopia is one of the 213 countries that registered COVID-19 cases since 13th of March 2020. In Ethiopia several cases and deaths are identified. Currently, more than 32 thousand cases are reported as of 19 Aug 2020. It is expected to rise since the case is reported from all parts of the country. The knowledge, attitudes and perceptions (KAP’s) are not motivating the response to COVID-19.2 Thus, the objective of the current study is to investigate COVID-19 response status quo in Ethiopia. In this objective different questions were addressed. They are: How Ethiopia has been approaching to tackle COVID-19? What were the Risk Communication and Community Empowerment (RCCE) preparedness and stringent response available to combat COVID-19? What is the current situations of COVID-19 in Ethiopia? What are the major challenges Ethiopia have been facing during the pandemic? How Ethiopia engage the community to tackle COVID-19? In order to address similar questions, I used empirical studies using academic research, COVID-19 guides, protocols, policies, and proclamation documents appeared to preparedness and COVID-19 responses. This paper sheds light on COVID-19 in Ethiopia. Besides, it could contribute to the extent literature review by providing the reasonable arguments and the explanation about investigating all government and stakeholders’ effects. The result indicates that Ethiopian government employed multiple and synergistic approaches from public health preparedness to the highest level of offending state of emergency as of 19 Aug 2020. However, given the different public health efforts and clinical cares, the pandemic has never shown static rather increasing alarmingly.
Methods
A qualitative descriptive approach more specifically qualitative case study was used to examine the Ethiopian local context which allied to the global approaches. Thus, the study employed a qualitative thematic analysis approach used to analyze the data. The study was also dependent on observations and documented knowledge emerged out from the lived experience and practice of the Ethiopian government. In this procedure, I used different terms to mine the data from different web information retrieval systems studies.3 Author marked that “empirical methods are positivistic and typically involve systematic collection and analysis of data”.4 The web-based search terms include “COVID-19 in Ethiopia”; “COVID-19 responses and preparedness in Ethiopia”; “RCCE in Ethiopia”; “early response to COVID-19 in Ethiopia”; “COVID-19 public health measures in Ethiopia”; “ COVID-19 response in Ethiopia”; “COVID-19 epidemiological characteristics”; “worldometer”; “Ethiopia during the pandemic”; “factors affecting COVID-19 response in Ethiopia” etc. Thus, web information retrieval systems studies were used as a framework for this study.
Related Literature Review: KAP’s of the Stakeholders
Research conducted in Ethiopian context showed that low levels of risk and impacts perception, the majority of the people have low perception of taking Coronavirus as a threat. The existence of poor knowledge and poor practice were respectively high.5,6 According to some research,7 findings there are
low educational status, rural residence, and low monthly income were significantly associated with poor knowledge and poor practice. Increasing age was associated with poor knowledge, and poor knowledge itself was associated with poor practice. (p.1958)
The practice of KAP’s even among health workers pharmacy showed only half of them had adequate knowledge about the disease.8 Scholars suggest that understanding of their risk perception could be an effective method to communicate the health policy.9
Results and Discussions
The Situations Since Reported in Ethiopia
The first case of COVID-19 was reported on 13 March 2020 in Ethiopia. Since then the Ethiopian government swiftly responded to minimize the impact of COVID-19 by using different strategies up to the lockdown. However, the situation is becoming unstoppable. Several cases have been reported daily. The cases have reported since escalated to 94,820 COVID-19 cases, with 1451 COVID-19 deaths (1.5% of total cases) and 49,886 COVID-19 recoveries (52.6% of total cases) as of 30 Oct 2020.
COVID-19 Response Coordination
The Government has strengthened its preparedness and response efforts to combat COVID-19 and has set up a well-organized national preparedness and response coordination mechanism through an Emergency Operation Center. Besides, the Ethiopian government has set up four different levels of coordination: (a) National Disaster Risk Management Council led by the deputy prime minister’s office; (b) Public Health Emergency Management (PHEM) incorporated a multi-sectorial national task force led by the Minister of Health; (c) The PHEM technical taskforce that has been managed by the Director-General of Ethiopian Public Health Institute (EPHI); and (d) PHEM Technical Working Group led by the national incident manager. As of 31st March 2020, a synergistic approach COVID-19 humanitarian actions has been coordinated by the established Emergency Coordination Center and national and regional the task forces were established in all regions [Table 1].10
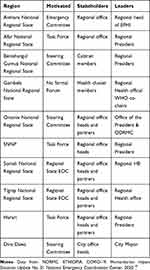 |
Table 1 Regional COVID-19 Coordination Arrangements |
Ethiopia Pass-Through Socio-Economic Impairments: The Impact of COVID-19
Ethiopian socio-economic situations have been drastically changed by COVID-19. The Ethiopian economy, after COVID-19 induced mobility and activity restrictions around the globe, has faced significant challenges.11 COVID-19 impacted by global disruptions have been considerably affected tourism and hotel business, exports and imports, and remittances to the country. Currently, Ethiopia has been passing through remittances declining, household consumption significantly affected, impeded economic growth, increased debt risks, high inflation and high unemployment rate, and lowered business and tourism. Research indicate that the COVID-19 response in Ethiopia is hardly impaired due to contextual factors,12 such as “a weak health system, poor nutritional status, lack of access to proper hygiene and sanitation and densely populated urban areas” (p.4).
COVID-19 Transmission
The case of the COVID-19 occurrence in Ethiopia was reported in Addis Ababa, the capital city of Ethiopia. There are 4.8 million people found in Addis Ababa. The rapid transmission of the diseases in Ethiopia is ascribed to the center of the test and quarantine for its international destinations. Besides, partial lockdown in Addis Ababa also aggravated the situations. It was first appeared in Addis Ababa. This in turn led to an expansion of the outbreak to all parts of the city since Addis Ababa remains the epicenter. The number of cases to the capital city is attributed to over 75% of all confirmed COVID-19 cases within Ethiopia as of August 19, 2020. Following this, efforts such as testing, contact tracing, quarantine, and isolation were not able to effectively to control the outbreaks across the country. Besides, the risk communication and community engagements are the most important aspects of the country’s efforts contributed to minimize the impact and transmission of COVID-19. The specific information is tailored to vulnerable groups (women, children and disabilities) [Table 2].13 Despite the efforts of all parts of the stakeholders, the new cases are alarmingly increasing. Still, some measures have been declining due to the hectic nature of the stakeholders day to day activities. Currently, Ethiopia confirmed that COVID-19 cases are reported in all parts of the country.
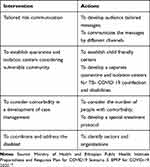 |
Table 2 Vulnerable Population Communication and Engagement Activities |
Epidemiological Characteristics
The COVID-19 causes respiratory infections. It has highly contagious characteristics. It could be considered the most complex global challenge.14 The outbreak has been affected more than 22 million people cases reported around the world as of 18 Aug 2020.15 Whereas more than 15 million (6.75% recovered) people recovered from the pandemic. The most serious case is that more than 700 thousand (3.51% dead) people death reported. Likewise, in the Ethiopian case a total of 94,820 COVID-19 cases out of which 1451 COVID-19 deaths (1.5% of total cases) and 49,886 COVID-19 recoveries (52.6% of total cases) reported as of 30 Oct 2020.
Early Response
The public health preparedness and response during early outbreak used different risk communication and community engagement activities during early outbreak.16 Media messages are powerful to reduce the impacts and risks of the pandemic by posing community and personal sanitation and hygiene activities. Thus, there were tailored messages for five core hygiene habits to respond to COVID-19. As part of the rapid responses, all educational systems, except the virtual learning of postgraduate programs, were closed for several months.
Public awareness creation and public education have been the public health strategic efforts. Some scholars suggest that the role of uncertainties to make effective communications to contain the pandemic,17 The current Ethiopian prime minister has making public announcements concerning the impacts and associated risks of COVID-19. Besides, the Ministry of Ethiopian Health has disseminated a regular briefing. In the media campaign to address all citizens, Ethio-telecom has been using cell-phone ring tones to remind and create awareness about the public health hygiene responses including frequent hand washing, maintaining a social distancing, and wearing of facemasks to fight COVID-19.
Further, the Ethiopian government has been implementing strict and stringent contact tracing after the case report, isolation as well as care, obligatory quarantine, and treatment. The government mobilized the public universities’ dormitories and other buildings to increase the capacity and number of quarantine centers to over 50,000 beds. The government also established additional isolation centers with a total of 15,000 beds. Moreover, the government arranged several treatment centers with a 5000-bed capacity. Further, the government introduced more comprehensive life insurance packages and coverage to protect front-line health workers.
Ethiopia has continued to mobilize national resources to make an effort towards its response to COVID-19. This was aimed to motivate voluntary actions to support the public health emergency and response. These actions allied with the government close coordination among concerned at all levels. Even though the government’s COVID-19 response has been on progress, its success so far illustrates what Ethiopia could achieve despite tight resource constraints.
Ethiopian State of Emergency
Since the news of Ethiopia’s first case of Coronavirus on March 13, various multi-sectorial measures have been taken to counter its spread, including the declaration of a national state of emergency on April 8. The country has banned public gatherings and other social activities of more than four people until September, and rigorous public health responses would be provided at limiting the dissemination of the pandemic could also be introduced,18 The author in his COVID-19 research work mentioned that two major activities must be banned as stated here.
There were different activities banned, restricted, and closed for five months of the state of emergency. All public gatherings: The ban applied to all religious, governmental, non-governmental, commercial, political, and social gatherings. The gathering is of a group of four people where individuals expected to ensure that they are 2 meters apart at all times; different activities: greetings by handshake, land borders movement, passenger loads for all national and local journeys, reducing workforces, students and teachers meetings, and measures on social distancing, sporting activities, and children’s playgrounds were closed.
COVID-19 Guideline and Protocol Development
Since the March Ethiopian government developed standards, guides and protocols documents to respond to COVID-19. The documents have been developed by assessing the situations, impacts and risks of COVID-19 pandemic. I consider for showcase purpose to indicate some of the documents developed by the Ministry of Health and Ethiopian Public Health Institute.13 One of the most important documents is a risk communication and community engagement mechanism in Ethiopia that aimed to have and create a mutual understanding of preparedness and response to minimize the effects of COVID-19. In order to develop such a common understanding is to develop a knowledge base standard guidelines and protocols. Another document is a cleaning and disinfection Protocol for COVID −19 which helps to communicate and inform respected stakeholders in well-designed manner. This is aimed to develop a routine environmental cleaning. The guideline focuses on frequently touched surfaces that consider cleaning and disinfecting of door handles, bedrails, tabletops, light switches, etc. These things should be frequently cleaned. The second category includes minimal touched surfaces such as floors, ceilings, walls, etc. Still some other document on Project Information Document could be developed by the World Bank. The aim of the World Bank Project is to make a holistic approach to the impact posed by COVID-19. Besides, the project expected to strengthen national systems or taskforces for its preparedness in Ethiopia.19 Still some others like a National Implementation Guide for COVID-19 Home-Based Isolation and Care and its objectives of the guide are to outline the steps and the procedures; describe the roles and responses; and provide detailed technical and administrative guidance. In Ethiopia, the epidemiological situations of COVID-19 brought a significant shift in our COVID-19 management response strategy and the overall pandemic response plan. This strategy is developed due to the current and projected trends of the pandemic. Thus, the guide provides clear guidance, recommendation, procedures and practical considerations to manage the case effectively, and efficiently. Moreover, Quarantine and Border Control Implementation Guide considering the increased risk impact of imported cases to the country was developed. Following that, Ethiopia has been implementing border control and applied thermal and clinical screening at the major point of entries. Starting from March 23, 2020, the country has started mandatory 14 days’ quarantine for all incoming passengers. Due to economic and risk impacts, the ongoing strategies are revised by the Ethiopian government. The rest of the documents are summarized as follows [Table 3,].20–28
 |
Table 3 Summary of Documents for COVID-19 Preparedness and Response in Ethiopia |
 |
Table 4 General Audience Communication and Engagement Activities |
Risk Communication and Community Engagement
Now Ethiopia is using an adopted Risk Communication and Community Engagement (RCCE) strategic approach for the pandemic.13 The overall objective of developing RCCE in Ethiopian context is to empower individuals, families, and communities to adopt preventive and health-seeking behaviors contributing to a reduction in the spread of COVID-19 Outbreak in Ethiopia,13 It is strongly believed to improve knowledge, perception, self-efficacy, and health-seeking behaviors; increase community engagement and ownership of the national response; improve evidence generation and knowledge management system; improves all levels coordination of RCCE interventions and enhance multilevel engagement on RCCE interventions. Above all, risk communication imparts confidence among the public during public health emergencies. In order to bring such confidences policies of public communication and instruction in proper use of a medical mask to contain the COVID-19 transmission.13 The strategic objective of the documents emphasized on two interdependent strategic categories in three outbreak phases:
Preparedness Phase: Pre-Outbreak Phase
a. Risk communication: As part of the national RCCE strategic response a risk communication that focuses on the activities of developing a comprehensive RCCE response plan; mapping capacity building RCCE team response to COVID-19; conducting risk perception assessment and engaging the public and institutions; gathering evidence-based information and developing the content; working on rumor and misinformation monitoring and engaging different media channels.
b. Community engagement: the RCCE strategy in the pre-outbreak phase considers community engagement which incorporates the activities of social and community mobilization; training and orientation; psychosocial support and mental health.
Outbreak Phase
a. Risk communication: the strategy of RCCE for the outbreak phase uses different activities such as coordination and monitoring; capacity building; spokesperson system; content development; rumor and misinformation monitoring and media engagement.
b. Community engagement: the strategy of RCCE for the outbreak phase in the community engagement activities includes social and community mobilization; training and orientation; psychosocial support and mental health.
Post-Outbreak Phase
a. Risk communication: the post-outbreak phase RCCE strategy performs different risk communication activities such as risk perception; content development; rumor and misinformation monitoring and media engagement.
b. Community engagement: the post outbreak phase RCCE strategy performs different community engagement activities engagement of the public; social and community mobilization; training and orientation; psychosocial support and mental health.
As a result, the Ethiopian action plan for COVID-19 response developed operation plan. In the operation plan, there are two types of audiences targeted to under risk communication and community engagement. These are the Ministry of Health and Ethiopian Public Health Institute, MoH& EPHI. The primary one is the general public and vulnerable populations.
General audience communication and engagement activities (Table 4).13
The vulnerable population in this regard include children, mental health and women [Table 2].13
Conclusion
The highly communicable nature of the pandemic attributed the COVID-19 response in Ethiopia harsher and dangerous. It has been causing a high fatality and death toll. Besides, a swift transmission of the viruses occurred in 213 world countries, including Ethiopia. The major research outcomes indicate that the COVID-19 situations gain the highest momentum by increasing alarmingly. It shows significant differences after two months since March 20,020 it happened and reported the first case in Ethiopia in March 2020. In response to the pandemic, several measures ranging from public health emergency response to the state of emergency have been underway by the Ethiopian government. The RCCE strategy and state of emergency are in place to reduce the risks and associated impacts of the pandemic. The RRCE strategy to COVID-19 response tried to segment the normal public and vulnerable part of the population by tailoring different activities of both risk communication and community engagement at societal, community and personal levels. Besides, the government has moved swiftly and rolled out a range of measures like lockdown. However, it was not strict and has not been heavy-handed that much. Currently, the status quo of the KAP’s and its practices were not sufficient enough to tackle the rapidly transmitted infectious disease. Such negligence among the public and related factors undermined the preparedness and responses towards COVID-19 in Ethiopia. The results are positive effect 94,820 out of 109 million population as of 30 Oct 2020. It confirmed in slow deaths (1.5%), the highest recoveries (52.6%); unfortunately, the new cases are increasing from day to day. In conclusion, this study searches web documents especially related to the Ethiopian case amid the COVID-19 pandemic to explore how the Ethiopian government has executed administrative actions and managed risk communications and community engagement with its people. The study found out that governmental efforts have not been enough to reduce the spread of the virus. The author also claims that the government should pay attention to high-risk and vulnerable groups to enhance their implementations.
There could be several ways and strategies the government can use. In recommendation, the government needs to revise and strengthen in policy implementation efforts to mobilize and upbeat the KAP’s of the public through different media reporting, films, and edutainment that consolidate the importance of experiential, social, economic, political and cultural factors that drive out the risks and the impacts of COVID-19 among the people. The RCCE efforts should focus on building up to the standard level of knowledge, attitudes and perceptions. In addition, to enhance and promote the implementation of recommended self-care and home-based isolation practices the government should give due attentions to high-risk prone groups and vulnerable parts of the population. There might be ups and downs to end the pandemic. However, it should be supported with strong clinical services and public health research. This could lay a good potential for future research.
Acknowledgment
I would be grateful to say thanks to Mr. Menyichil M. Abebe, University of Gondar, for his proofreading suggestions. My second appreciation also goes to Ms. Yekite Aynalem, Debre Tabor University, for her similar contributions. Thus, both scholars’ contributions were vital to enhancing the quality of this study.
Disclosure
The author reports no conflicts of interest for this work.
References
1. Srivastava N, Baxi P, Ratho RK, Saxena SK. Global trends in epidimology of corona virus disease 2019(COVID-19). In: Saxena S, editor. Coronavirus Disease 2019 (COVID-19). Singapore: Springer Nature; 2020:9–23.
2. Geda NR, Legesse B, Kebede SW, Fikadu B. Perceptions of Risks and Impacts of COVID-19 Among the Public in Ethiopia. Frontier: Insights; 2020.
3. Jansen BJ, Pooch UA. A review of Web searching studies and a framework for future research. J Am Soc Info Sci Tech. 2001;52(3):235–246. doi:10.1002/1097-4571(2000)9999:9999<::AID-ASI1607>3.0.CO;2-F
4. Dan V. Empirical and Non-Empirical Methods. Int Encyclopedia Commun Res Methods. 2017;1–3.
5. Akalu Y, Ayelign B, Molla MD. <p>Knowledge, Attitude and Practice Towards COVID-19 Among Chronic Disease Patients at Addis Zemen Hospital, Northwest Ethiopia. <![CDATA[Infection and Drug Resistance]]>. 2020;Volume 13:1949–1960. doi:10.2147/IDR.S258736
6. Kebede Y, Yitayih Y, Birhanu Z, Mekonen S, Ambelu A. Knowledge, perceptions and preventive practices towards COVID-19 early in the outbreak among Jimma university medical center visitors, Southwest Ethiopia. PLoS One. 2020;15(5):1–15. doi:10.1371/journal.pone.0233744
7. Jemal K, et al. Knowledge, attitude and practice of healthcare workers towards COVID-19 and its prevention in Ethiopia: a multicenter study. Researchsquare. 2020;1–14.
8. Tesfaye ZT, Yismaw MB, Negash Z, Ayele AG. <p>COVID-19-Related Knowledge, Attitude and Practice Among Hospital and Community Pharmacists in Addis Ababa, Ethiopia. <![CDATA[Integrated Pharmacy Research and Practice]]>. 2020;9:105–112. doi:10.2147/IPRP.S261275
9. Huynh TL. The COVID-19 risk perception: A survey on socioeconomics and media attention. Economic Bulletin. 2020;40(1):758–764.
10. NDRMC. ETHIOPIA: COVID-19. Humanitarian Impact Situation Update No. 01 National Emergency Coordination Center; 2020.
11. Beyene S, Makonnen T Research themes. Retrieved from International Growth Center https://www.theigc.org. 2020
12. Shigute Z, Derseh A, Alemu G. Containing the spread of COVID-19 in Ethiopia. J Glob Health. 2020;1–4.
13. Ministry of Health and Ethiopian Public Health Institute. Risk Communication and Community Engagement Strategy for COVID-19 Outbreak Response in Ethiopia. RCCE. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
14. Huynh TLD. (2020). The COVID-19 containment in Vietnam: what are we doing? J Glob Health. 2020;10(1):1–3. doi:10.7189/jogh.10.010338
15. Chekol E, Asmamaw T, Yibeltal M. The newly emerged COVID-19 disease: a systemic review. Virol J. 2020;17(96):1–8.
16. Huynh TLD. “If You Wear a Mask, Then You Must Know How to Use It and Dispose of It Properly!”: A Survey Study in Vietnam. Rev Behav Eco. 2020;7(2):145–158. doi:10.1561/105.00000121
17. Huynh TLD. Does culture matter social distancing under the COVID-19 pandemic? Saf Sci. 2020;130:1–7. doi:10.1016/j.ssci.2020.104872
18. Zikargae M SWOT analysis of a risk communication of COVID-19 preventions in Ethiopian Higher education [unpublished].2020.
19. The World Bank. Ethiopia COVID-19 Emergency Response. COVID-19 Prevention and Control. Addis Ababa, Ethiopia: WB; 2020.
20. Ministry of Health and Ethiopian Public Health Institute. Cleaning and Disinfection Protocol for COVI −19. Protoctol. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
21. Ministry of Health and Ethiopian Public Health Institute. Preparedness and Response Plan for COVID19 Scenario 3. EPRP for COVID-19; 2020.
22. Ministry of Health and Ethiopian Public Health Institute. National Implementation Guide for COVID-19 Home-Based Isolation and Care. Implementation Guide. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
23. Ministry of Health and Ethiopian Public Health Institute. Quarantine and Border Control Implementation Guide. COVID-19 Prevention and Control. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
24. Ministry of Health and Ethiopian Public Health Institute. Home-Based Isolation and Care. National Implementation Guide for COVID-19: Home-Based Isolation and Care. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
25. Ministry of Health and Ethiopian Public Health Institute. Infection Prevention & Control Interim Protocols in Health Caring Centers. COVID-19 Prevention and Control. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
26. Ministry of Health and Ethiopian Public Health Institute. Screening and Quarantine of Cross Country Truck Drivers and Other Crews. COVID-19 Prevention and Control. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
27. Ministry of Health and Ethiopian Public Health Institute. Protocol for Transporting COVID-19 Patients. COVID-19 Prevention and Control. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
28. Ministry of Health and Ethiopian Public Health Institute. Health Care Facility COVID-19 Preparedness and Response. COVID-19 Prevention and Control. Addis Ababa, Ethiopia: MoH & EPHI; 2020.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
