Back to Journals » Clinical, Cosmetic and Investigational Dermatology » Volume 13
Contraception, Sexuality and Pregnancy in Women with Psoriasis: Real-Life Experience of 235 Women
Authors Maccari F , Fougerousse AC , Reguiai Z, Taieb C
Received 8 August 2020
Accepted for publication 7 October 2020
Published 11 November 2020 Volume 2020:13 Pages 817—823
DOI https://doi.org/10.2147/CCID.S275512
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Jeffrey Weinberg
François Maccari,1,2 Anne Claire Fougerousse,2,3 Ziad Reguiai,2,4 Charles Taieb5,6
1Private Practice, La Varenne St Hilaire, Paris, France; 2Reso Pso, Dermatologist Network, Paris, France; 3Military Teaching Hospital Bégin, Saint Mandé, Paris, France; 4Service De Dermatologie, Polyclinique Courlancy, Reims, France; 5FIMARAD, Hôpital Necker Enfants Malades, Paris, France; 6European Market Maintenance Assessment, Vincennes, Paris, France
Correspondence: Charles Taieb Email [email protected]
Background: Little is known about how women of childbearing age with psoriasis experience contraception, sexuality and pregnancies through the lens of their skin condition.
Objective: To evaluate the experiences and expectations in this group of patients.
Materials and Methods: In total, 235 women aged between 18 and 45 years old completed an online survey. We collected the characteristics of psoriasis, contraception and pregnancy history. Psoriasis severity was measured using the Simplified Psoriasis Index. Patient quality of life was assessed using the Dermatology Life Quality Index (DLQI) and the Short Form-12.
Results: Psoriasis was mild in 78% of cases. The mean DLQI score was 8.8, highlighting a moderate impact of psoriasis. In total, 28% of the women had no current follow-ups, while at least two distinct physicians followed 21% of these patients. In total, 31.5% of the women felt that they could discuss sexuality during their consultations. In addition, 63% of respondents had a contraceptive method, but more than half of the women reported that contraception was rarely or never discussed during the consultations. In total, 63% had at least one pregnancy, and 61.5% reported that the doctor managing their psoriasis did not discuss their pregnancy during consultations. Psoriasis worsened during pregnancy for 21% of the respondents but improved in 34%. Among women who were not pregnant, less than 15% reported that the doctor in charge of their psoriasis discussed family planning and pregnancy possibilities.
Conclusion: Our study shows that the management of women of childbearing age with psoriasis must be improved with respect to sexuality, contraception and pregnancy planning.
Keywords: psoriasis, women, childbearing
Introduction
Women between 18 and 45 years old represent more than one-fourth (26.2%) of the French population with psoriasis.1 Based on data from the National Institute of Statistics and Economic Studies (INSEE, Institut national de la statistique et des études économiques, January 2018), we estimated that the prevalence of psoriasis in this group of the general population was 4.7% (726,000 women). The impact of pregnancy on psoriasis is well known, but the impact of psoriasis among pregnant women has not been evaluated. In a previous study, we reported that 26% of women with psoriasis who are seen by a dermatologist are of childbearing age and therefore likely to be pregnant.2 Women are mostly interested in knowing about treatment compatibility with pregnancy, risks to the foetus and the risk of disease transmission.2 In the present study, we sought to investigate the real-life experience of these female psoriasis patients with respect to contraception, sexuality and pregnancy.
Materials and Methods
Study Population
A polling institute (HC Conseil Paris, France) conducted the survey between December 2019 and January 2020 in accordance with local legislation. From a database containing the e-mail addresses of 900,000 Internet users who agreed to participate in different surveys (Megabase-kantar), we first built a representative sample of the French population stratified by age, geographical area of residence and income, and among them, we identified individuals who self-reported suffering from psoriasis. Finally, among those people, we identified women who were of childbearing age between 18 and 45 years old (Figure 1). Each participant agreed to provide answers to a digital questionnaire, including questions regarding their health and skin diseases. Given the prevalence of psoriasis in France (4.42%)1 and the prevalence of psoriasis among women of childbearing age (4.69%),1 it was necessary to interview approximately 200 women (Figure 1).
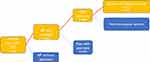 |
Figure 1 Flowchart of the study. |
This study used completely anonymized data and did not involve patient contact, so institutional review board approval was not required.
However, before answering the questionnaire, each respondent was informed of the nature of the survey, that anonymity would be respected and that no collected information that would allow any identification.
The respondent could stop answer at the questionnaire at the time of her choice without any explanation.
By answering the questionnaire, the respondent was confirming his or her agreement, completion of the survey deemed to be informed consent.
Survey
The survey included questions about sociodemographic data (gender, age, occupation/social class, area of residence), psoriasis history and management, contraception methods and past or present pregnancies. The respondents had to answer seven assertions about psoriasis and pregnancy and acknowledge whether they knew the correct answers.
Quality of Life
Quality of life (QoL) was assessed using two self-reported questionnaires: the 12-Item Short-Form Health Survey (SF-12®),3 which is a non-skin-specific questionnaire; and the Dermatology Life Quality Index (DLQI).4 The SF12 is a multipurpose short-form survey with 12 questions, which are selected from the SF-36 Health Survey. The questions are combined, scored, and weighted to create two scales that provide glimpses into mental and physical functioning and overall health-related QoL. This survey provides a generic measure regardless of any specific age or disease group and was developed to provide a shorter but valid alternative to the SF-36, which many health researchers consider to be too long to administer in studies with large samples. The SF-12 is weighted and totalled to provide easily interpretable scales for physical and mental health. Physical and mental health composite scores are computed using the scores of 12 questions and range from 0 to 100, with a score of zero indicating the lowest level of health measured by the scales and 100 indicating the highest level of health.3
Simplified Psoriasis Index patient self-assessment5,6
The Simplified Psoriasis Index (SPI) is a new score for the global assessment of psoriasis severity,5 and a French version of this assessment was recently validated.6 The SPI was derived from the Salford Psoriasis Index, but the Psoriasis Area and Severity Index (PASI) has been replaced with a composite weighted severity score designed to reflect the functional and psychosocial impact of psoriasis affecting important body sites. The SPI specifically assesses the critical locations of psoriasis (scalp, face, hands, feet, and anogenital area) and includes a section on the psychosocial impact and history. It includes 3 distinct domains: current severity of skin disease (SPI-s), psychosocial impact (SPI-p) and past history and interventions (SPI-i). The three domains are presented as three separate scores: SPI-s (0–50), SPI-p (0–10) and SPI-i (0–10). We used here the patient self-assessed version. The patients were also asked to evaluate the extent to which psoriasis bothers their daily lives at the current time using a numeric scale ranging from 0 (for “my psoriasis does not bother me”) to 10 (for “my psoriasis bothers me greatly”).
Knowledge of the Disease
In this project, several assertions were proposed, each of which required patients to express themselves about the truthfulness of the assertion.
These assertions are common (eg, transmission of the disease, treatment during pregnancy, and impact of pregnancy on psoriasis) and were identified on the patient association’s website (www.francepsoriasis.org). Since the current validated questionnaires did not allow us to address all of the questions that we thought were relevant, we created specific questions that did not undergo the validation process.
Statistical Analyses
Statistical analyses were performed using R software, version 3.5.1, which is available on the Internet. Percentages were computed for categorical variables. Given that our objective was to describe the situation to impact future educative programmes and awareness campaigns, we did not perform any comparisons between subgroups.
Results
Overall, 235 women responded to the questionnaires, including two incomplete questionnaires. The following age distribution for 233 patients was observed: 46% (n=108) 35–44 years old, 38.5% (n=88) 25–34 yo and 15.7% (n=37) 18–24 yo. The characteristics of the respondents are summarized in Table 1.
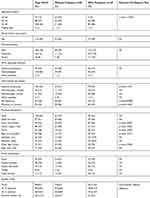 |
Table 1 Characteristics of Patients with Psoriasis Based on Pregnancy Status |
Psoriasis
In total, 46% of women had at least one parent with psoriasis. Seven percent of the significant partners had psoriasis. Psoriasis was severe in 8% (n=18), moderate in 14% (n=34) and mild in 78% (n=183). In addition, 33% of respondents reported having psoriatic arthritis.
Apart from psoriasis, 36% (n=81) reported an additional skin disease, and 14% (n=32) reported two additional skin diseases, including acne (26%, n=59), contact eczema (22%, n=48), atopic dermatitis (15%, n=33), scalp disease (18%, n=41) and vitiligo (4%, n=8).
Diagnosis and Follow-Up
The mean age at diagnosis was 22±9 years old. Psoriasis was diagnosed by a dermatologist in 66% (n=144) of the cases and by a general practitioner (GP) in 32% (n=70). Approximately 55% of the respondents (n=129) consulted a dermatologist within the past 12 months, including 15% (n=35) within the past month. In contrast, 8% (n=19) never consulted a dermatologist. GPs and dermatologists were the referents for psoriasis in 39% (n=106) and 36% (n=97) of the respondents, respectively. One of five women was followed by both. The dermatologists were mostly private based (63% of the cases). Twenty-four percent (n=65) had no current follow-up.
Quality of Life
The mean DLQI score was 8.8±6.5, highlighting a moderate impact of psoriasis. The physical dimension of the SF-12 did not show significant alteration (mean value 50.9±8.3) in contrast to the mental dimension of the SF-12, which showed an alteration with a score far less than 50 (36.7±2.5).
On a scale of 0 (for “my psoriasis does not bother me”) to 10 (for “my psoriasis bothers greatly”), the mean score obtained was 5.8 ± 2.5.
Contraceptive Methods
Sixty-three percent (n = 149) currently used a contraception method, mainly a contraceptive pill (38%, n=90), intrauterine device (17%, n = 26) or implant (6%, n=9). Other methods were rarely used (0% to 3%). Ninety-three percent (n = 138) reported being confident in the effectiveness of their contraceptive method. Thirty-one percent (n = 46/149) stated that contraception use was discussed regularly during consultations, while it was rarely or never discussed in 54% (n=81) of cases. Thirty-two percent acknowledged that sexuality was discussed during consultations. Physician gender was not significantly associated with discussion during consultations. Twelve women (5.1%) were undergoing menopause.
Pregnancy Planning
Thirteen (n=11) and 14% (n=12) of the women without pregnancy reported that the physician treating their psoriasis broached child planning and pregnancy, respectively. Seventy percent (n = 60) did not talk about their psoriasis with their gynaecologist, and 13% (n = 11) did not have a gynaecologist. Eight percent (n = 7) were concerned that psoriasis influenced their pregnancy plans, and 12% (n= 10) were concerned that psoriasis treatment interfered with pregnancy. Fifty-two percent (n = 45) and 44% (n=38) were not concerned “at all” that their psoriasis or psoriasis treatment would affect their future pregnancy, respectively (Table 2).
 |
Table 2 Concerns for Women Psoriasis Regarding Pregnancy |
Pregnancies
One hundred forty-nine women (63%) reported at least one pregnancy, and 18 (7.6%) were currently pregnant. The mean age of the women at birth of the first child was 24.9±4.7 years old. Of the 149 patients who had at least one pregnancy, the pregnancy was full term in 97.3% (n=145). Psoriasis is or was a moderate to enormous concern for 25% of respondents (n=37) during pregnancy, and 61.5% (n=91) reported that the physician managing their psoriasis did not talk about the pregnancy during consultations. In addition, 36% (n=20) discussed their concerns with their gynaecologist.
In total, only one out of every two women [52% (n=77)] discussed this subject with at least one physician (including dermatologists and gynaecologists), and 37% (n=56) of patients stopped their treatment for psoriasis during pregnancy. The most frequently withdrawn treatment was UVB and UVA phototherapy (20% of respondents), methotrexate (18%), retinoids and cyclosporine (7% both), and biologics (3.6%). Local treatments were also stopped in 37.5% of cases.
Twenty-one percent of the respondents felt that psoriasis worsened during pregnancy, 34% felt that psoriasis improved during pregnancy, and 45% felt that psoriasis did not change during pregnancy. After pregnancy, 19% felt that psoriasis worsened after giving birth, 30% felt that psoriasis improved, and 51% felt that the psoriasis remained similar.
Knowledge of the Disease
The correct response rates to each of the questions are described in Table 3. None of the assertions had more than 60% correct answers.
 |
Table 3 Response Rate of Women Who Answered Correctly to the Following Statements About Psoriasis |
Discussion
We report on the real-life experience of 235 women of childbearing age with psoriasis. Psoriasis had an overall mild impact on QoL in our cohort. Contraception and the sexuality of the patients were discussed in approximately one-third of cases. We previously reported on the difficulties of opening up and discussing sexuality with physicians.2 In a study of 183 couples, we found that psoriasis severity and/or a significant impact on QoL were factors associated with sexual dysfunction in male partners of women with psoriasis, but the opposite scenario was not observed.7 Contraception in childbearing women with psoriasis is important, and therapeutic options must be considered for all women with psoriasis who are sexually active irrespective of intentions of starting a family.8 For example, acitretin, methotrexate, and oral psoralen/ultraviolet A are all contraindicated in pregnancy.7 Conversely, cyclosporine and anti-TNF alpha can be considered.9–11 Notably, a recent Italian study showed that women were less likely to receive biologics than men.12
Two-thirds of the patients already had at least one child. The majority of those without children were rather confident about the outcome of pregnancy. It is important to remind us that psoriasis is usually improved during pregnancy because of high oestrogen levels. Oestrogen might improve psoriasis by suppressing the T-cell immune response, reducing keratinocyte cytokine and chemokine production, restoring the balance of redox and enhancing the skin barrier.13 The greatest concern was about foetal risk under psoriasis therapy, with 17.5% of the women expressing concerns (much to enormous concern). However, up to 25% of pregnant patients reported concerns. This finding illustrates the difference in the state of mind between planning a pregnancy and being pregnant. In our previous study, dermatologists reported, that upon diagnosing women of childbearing age with psoriasis, they approached short-term desires of pregnancy (83.5%), contraception (68%), long-term desires of pregnancy (41%) and drug therapies during pregnancy (35%).2 Conversely, according to dermatologists, the main topics discussed by women included compatibility of therapy with pregnancy (64%), disease transmission (54%), foetal risks of therapy (49%), and contraception (32%).2 However, in the present study, 13–14% of non-pregnant women reported that the physician managing their psoriasis discussed child planning and pregnancy. In addition, 61.5% of pregnant patients reported that the physician managing their psoriasis did not talk about the pregnancy during consultations. This strong discrepancy can be explained by the managing physician being either a dermatologist or a GP. In addition, the patients in this study were more often followed by a dermatologist in private practice (26%) than one from a hospital (15%). However, in our previous study,2 the respondents were mainly hospital based (49%). We did not inquire here about short-term or long-term wishes.
Finally, we observed that the level of knowledge about psoriasis and pregnancy was rather low. For six of the seven statements, less than half of the women could provide the correct answer. For two statements, less than one-third of the women provided correct answers. The dearth of knowledge was more important among non-pregnant women. This finding seems logical because interest about the topic might be lower when a pregnancy is not planned.
Limitations of our survey include the small sample size of our cohort, a convenience sample that was not fully representative of the population, a lack of validated questionnaires, recollection bias given the self-reported nature of the study and the lack of a control group.
Conclusion
Patient associations have been calling for support for parental projects for many years. It is essential to ensure the health safety of both the woman and the child. With our study, we wish to raise awareness among dermatologists to systematically address questions about sexuality and contraception with their patients during follow-ups. The development of therapeutic educative programmes is also warranted. Studies such as ours and future studies will help to improve the situation.
Our study showed that the management of women of childbearing age must be improved with regard to sexuality, contraception and pregnancy planning. It is important that the dermatologists managing these patients with psoriasis address these issues during consultations.
Funding
UCB Pharma.
Disclosure
The authors report no conflicts of interest for this work.
References
1. Richard MA, Corgibet F, Beylot-Barry M, et al. Sex- and age-adjusted prevalence estimates of five chronic inflammatory skin diseases in France: results of the OBJECTIFS PEAU study. J Eur Acad Dermatol Venereol. 2018;32(11):1967–1971. doi:10.1111/jdv.14959
2. Maccari F, Fougerousse AC, Esteve E, et al. Gem resopso and the AJDerm. Crossed looks on the dermatologist’s position and the patient’s preoccupations as to psoriasis and pregnancy: preliminary results of the PREGNAN-PSO study. J Eur Acad Dermatol Venereol. 2019;33(5):880–885. doi:10.1111/jdv.15423
3. Ware J, Kosinski M, Keller SD. A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med Care. 1996;34(3):220–233. doi:10.1097/00005650-199603000-00003
4. Finlay AY. Quality of life assessments in dermatology. Semin Cutan Med Surg. 1998;17:291–296. doi:10.1016/S1085-5629(98)80026-6
5. Chularojanamontri L, Griffiths CE, Chalmers RJ. The Simplified Psoriasis Index (SPI): a practical tool for assessing psoriasis. J Invest Dermatol. 2013;133(8):1956–1962. doi:10.1038/jid.2013.138
6. Richard MA, Aractingi S, Joly P, et al. [French adaptation of a new score for global assessment of psoriasis severity: the Simplified Psoriasis Index (SPI)]. Ann Dermatol Venereol. 2019;146(12):783–792. doi:10.1016/j.annder.2019.08.004. original article was published in french.
7. Halioua B, Maccari F, Fougerousse AC, et al. Impact of patient psoriasis on partner quality of life, sexuality and empathy feelings: a study in 183 couples. J Eur Acad Dermatol Venereol. 2020;34(9):2044–2050. doi:10.1111/jdv.16270
8. Gottlieb AB, Ryan C, Murase JE. Clinical considerations for the management of psoriasis in women. Int J Womens Dermatol. 2019;5(3):141–150. doi:10.1016/j.ijwd.2019.04.021
9. Bangsgaard N, Rørbye C, Skov L. Treating psoriasis during pregnancy: safety and efficacy of treatments. Am J Clin Dermatol. 2015;16(5):389–398. doi:10.1007/s40257-015-0137-5
10. Götestam Skorpen C, Hoeltzenbein M, Tincani A, et al. The EULAR points to consider for use of antirheumatic drugs before pregnancy, and during pregnancy and lactation. Ann Rheum Dis. 2016;75(5):795–810. doi:10.1136/annrheumdis-2015-208840
11. Cacciapuoti S, Scala E, Megna M, et al. Impact of current anti-psoriatic systemic treatments on male and female fertility: what the endocrinologist needs to know. Minerva Endocrinol. 2020. doi:10.23736/S0391-1977.20.03236-8
12. Scala E, Megna M, Amerio P, et al. Patients’ demographic and socioeconomic characteristics influence the therapeutic decision-making process in psoriasis. PLoS One. 2020;15(8):e0237267. doi:10.1371/journal.pone.0237267
13. Lin X, Huang T. Impact of pregnancy and oestrogen on psoriasis and potential therapeutic use of selective oestrogen receptor modulators for psoriasis. J Eur Acad Dermatol Venereol. 2016;30(7):1085–1091. doi:10.1111/jdv.13661
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
