Back to Journals » Journal of Multidisciplinary Healthcare » Volume 12
Compliance, adherence, concordance, empowerment, and self-management: five words to manifest a relational maladjustment in diabetes
Authors Settineri S , Frisone F , Merlo EM, Geraci D , Martino G
Received 8 November 2018
Accepted for publication 23 January 2019
Published 29 April 2019 Volume 2019:12 Pages 299—314
DOI https://doi.org/10.2147/JMDH.S193752
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Salvatore Settineri,1 Fabio Frisone,2 Emanuele Maria Merlo,2 Daniele Geraci,3 Gabriella Martino3
1Department of Biomedical and Dental Sciences and Morphofunctional Imaging, University of Messina, Messina, Italy; 2Department of Cognitive Sciences, Psychology, Educational and Cultural Studies (COSPECS), University of Messina, Messina, Italy; 3Department of Clinical and Experimental Medicine, University of Messina, Italy
Background: The pathological reality of diabetes and the incidents in following the prescribed therapies have been considered and are still a serious and relevant problem in the health sector.
Objective: This review aims at highlighting the importance of clinical psychological phenomena that underlie the notion of therapies.
Methods: The review was conducted through search engines such as PubMed, Medline, Web of Science and Google Scholar. The articles related to compliance, adherence, concordance, empowerment and the self-management of diabetes were included, in order to highlight the possible similarities and differences that these terms bring with them in them management of diabetes.
Results: Starting from 252 initial publications, 101 articles were selected that highlighted the practical implications that each term has compared to the others.
Conclusion: The review can represent a bridge between the medical approach and clinical psychology, in which integration can suggest paths aiming at improving patients’ existential conditions and adaptation.
Keywords: compliance, adherence, concordance, empowerment, self-management, diabetes
Introduction
The lack of phenomenological knowledge of the health professional of diabetes, both under the aspect of pharmacology and of physical health, often causes health professionals themselves to forget that the drug has aspects that exceed its biochemical efficacy. We cannot ignore the emotional significance that the patient gives to the drug, and the surplus value that the health professional gives to the therapeutic medium. In this review we will deal with the aspects of collaboration between health professionals and patients that can be seen as effective, or the various proposals by many other authors.1–7
The educational approach is not sufficient enough, since therapy has a stronger meaning than prescriptions, as suggested by literature.8 This concept is limited to what the patient views as having an active role in their own self-management9,10 or “adherence”.11–13 These terms derive from the Latin “adhaerentia”, derivative of adhaerēre “to adhere”, is to be attached, supported, and closed. The use of etymologies and metaphors express only a part of the adjustment processes of the subject. There is in fact a lack between clear instructions given to patients and unknown variables not sufficiently understood, together with low empathy.
It is probably better to use the term “self-care”14 to underline a sort of emotional relationship that is something more than an empathic act. The last cited author suggests an approach to this type of relationship, while suggesting seven behaviors. The same psychoanalyst Jung uses this metaphor: «the meeting of two personalities is like the contact between two chemical substances; if there is a reaction, both are transformed».15
The concept of transference and counter-transference has been emphasized by psychoanalysis. Several other orientations have foreseen further concepts, like Winnicott, who specialized in the field of play and Gestalt in the encounter between patient and therapist. All those theoretical fields, impose on phenomenology as a method of describing the dimension of the phenomenon and the attempt to reach therapeutic protocols that must be adopted to every singular patient. The intent of this research is to highlight the need to get in touch with the subjective experience, in order to improve the outcomes of treatment. The clinical approach ensures a greater likelihood of glycemic control, as proven by the fact that many changes in glycemic metabolism are dictated by the same efforts and styles of health care as Hayes et al16 have taken into account. A frequent mistake made by clinicians is to confuse the prescription and general theoretical orientations of psychology with the subjectivity of a lifestyle. Therefore, there is a necessity to distinguish a prescription from the value that the individual patient attributes to it.
The analysis, although apparently complex and long, arises from the need to highlight the trend of past and current clinical approaches in scientific literature.
Methods
Search strategy
A review of the scientific literature was conducted in order to analyze the behaviors of adherence to the pharmacological treatments of diabetes. Research strategies have been used through the computer database of PubMed, Medline, Web of Science and Google Scholar; the searched keywords refer to the concepts of Compliance, Adherence, Empowerment, Concordance, and Self-Management.
During this phase, the various domains on which the article is focused on have been identified:
- Definitions of the phenomena related to the adherence of pharmacological treatments for diabetes;
- Intervention strategies and results obtained;
- Analysis of current knowledge referring to the origin of non-adherence.
Eligibility
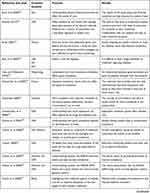
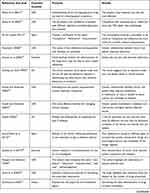
Based on the keywords searched, 252 articles were found, of which 101 selected on the basis of title and abstract. The 101 articles in the table allow us to observe the similarities and differences that characterize the studies that conceptually prefer a term like compliance rather than empowerment or the others to investigate the therapeutic adherence.
Results
 |
 |
 |
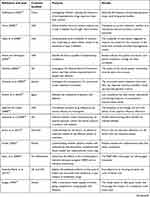 |
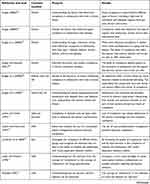 | Table 1 Summary table of classification of articles |


Compliance
The meaning of compliance in medicine refers to the ability of an organ to distend in response to applied pressure. In physics, compliance refers to the property of a material undergoing elastic deformation or (of a gas) changing in volume when subjected to an applied force. In therapy, it means to agree with rules or standards. More specifically, the patient and the family’s response to the prescription given.103
In 1997 it was hypothesized that it would be sufficient to reduce the frequency of the doses of the drug to achieve an improvement in compliance; but this practice included risks, as it depended on the therapeutic range of the drug itself.77 Of course, that does not divert from the fact that a better compliance can be achieved by using simpler and less frequent dosage regimens to facilitate the correct intake of drugs.19,30,33,35,39,40,48,51,52,59,61,92,99,102 It is also true that some studies5,10,25,71,72,100,101 have shown that the patient’s motivation to be more compliant with treatment also increases according to the efforts and confidence that the health care provider can transmit in reference to the guidelines to be followed by the patient. The high number of the authors cited underlines the strength of the “trust” element in adhesion to the treatment. Referring to childhood, it has been noted that the complexity related to the treatment of chronic diseases greatly complicates adherence to treatment.44 In order to be able to effectively manage a chronic disease such as diabetes, it seems essential not only to establish a relationship of trust between the health professional and the patient, but also a “friendship”.73 There seems to be a correlation between the quality of an established cooperation and the quality of diabetic treatment. When we talk about the factor of friendship we enter into subjectivity closely linked to the personality of the health professional. The studies on compliance in adolescence64–70,88 highlighted that the crucial factor for achieving the best possible treatment depends mainly on the type of relationship that the patient is able to establish with health-care workers, family members and friends. It can be seen from other studies that the importance of the patient-health professional relationship seems to play a decisive role at any age.21,26,38,45,54,57 In light of the above, it seems that in order to achieve an improvement in the patient’s compliance with diabetic care the main solutions are traceable in the possibility of using less painful procedures in taking the required drugs. This is a way of increasing the patient’s knowledge of the chronic disease,29,89,93 while also improving the relationship between the health professional and the patient. Perhaps, the health professional should favor those essential self-care components that Shrivastava summarizes in the seven essential behaviors: healthy eating, being physically active, monitoring blood sugar along with medications, good problem-solving skills, healthy coping skills and risk-reduction behaviors.
 | Figure 1 The arrow shows the remarkable reduction of HbA1c % in the favourable condition of full compliance, where the patient maintains a passive role. |
Adherence
This term refers to the health professional prescriptions regarding timing, doses, frequency and periods of drugs-consumed.103
From this it is possible to notice how adherence to therapy is defined as the extent to which a person’s behavior in taking medication, following a diet and/or performing changes in lifestyle, corresponds to the recommendations agreed upon by a health professional. Research suggests that adherence to therapeutic recommendations for diabetes treatment is low.96 Producing an effective improvement, could either reduce the risk of complications caused by ineffective treatment or decrease the frustrations of the said health professionals.42
The reasons for non-adherence are multifactorial and difficult to identify. They include age, information, perception and duration of the disease, complexity of the dosage regimen, poly-therapy, cognitive factors, tolerability, clinical inertia, socioeconomic problems, culture, patient education and beliefs, social support and polypharmacy.18,32,43,47,50,82,85,87,97 Those studies also indicate how adherence is implemented through a combination of fixed-dose tablets and less frequent administration regimens, through educational initiatives - with particular attention to the quality of communication between patient and health professional - and through reminders and support systems to help reduce costs. Overall, some results suggest that fixed dose combined tablets and individual dose packaging may improve adherence in a number of settings, but the limitations of available evidence indicate that uncertainty remains about the extent of these benefits.34 Electronic monitoring systems have been useful to improve adherence to individual patients, and could help health professionals to identify patients who need additional support;35 however, even in this case it can be seen how the results obtained cannot completely overcome the problem of adherence.
 | Figure 2 The arrow shows how adherence improves treatment. Also in this case the patient maintains a passive role. |
Concordance
The term refers to the deep knowledge of the relationship and to the achievability of examining crucial questions regarding the patient’s lifestyle.104
It is important to clarify the dynamics that differentiate the various aspects of the approach to pharmacological therapies in diabetes,20 since the interactive level between clinicians and patients should not be experienced exclusively as an instructive end,21 but as a space for the grouping of skills and support in the decision-making process related to the drug therapy.41 Regarding the terminological transition from compliance to concordance,8 there is a need to overcome the emotion related to rigid orders, to a relationship based on cooperation. It would make the process of taking medicine more stress-free, considering the subject as a decision-maker. The patient’s consideration avoids undergoing orders that place the agents on different levels, and considers both figures of equal breadth.31
 | Figure 3 Patient active role with cooperation. |
Empowerment
This term refers to the strengthening and improvement of power.103
103Empowerment can be considered as a process, in which the contact between an authority and another figure generate improvements in the state of health. There are some studies that suggest setting up structured objectives,56 adapted through problem-solving practices and coping strategies.24,62 The term includes several associated meanings, such as patient-centered and collaborative care but a collaborative approach to clinical reality remains transversal.23 Several scientific contributions tend to emphasize the importance of education in empowerment groups.6,55 However, we cannot help but consider the fact that processes of the over-evaluation of empowerment can produce negligence on other important issues related to the treatment of chronic diseases, as suggested in a review by Paterson.78
 | Figure 4 Patient active role with acquisition of competences. |
Self-management
This term refers to a system of participative management.103
From a review by Norris et al,2 it emerges that educational self-management and cooperation with patients can be more effective than the exclusive intervention of the health professional, for example glycemic, weight and lipid control. The author reports important scientific contributions that clarify the role of major and minor life events related to self-reported compliance, clarifying that educational intervention can be considered as an indicator of improvement in health status,9 even though it is still unclear how to achieve certain clinical results. It is therefore evident that self-management education produces positive effects, as it is also known that the benefit begins to decline from one to three months after the intervention, suggesting the need to implement practices aimed at promoting them.76 Multi-faceted and organizational interventions that would facilitate structured patient reviews are effective in care pathways.10,80,81
 | Figure 5 Active role of patient with responsibility. |
Discussions
The results related to the adherence in the treatment of diabetes highlight a critical fact, because over time the treatment has had different meanings. The Table 1 contains a large number of articles related to the theme; the various articles have posed the problem. Can these terms be used as synonyms or do they need a distinction? In the first analysis the Figures 1–5 show how the words (compliance, adherence, concordance, empowerment, self-management) empathize the passive or active role of the patient, the exclusive role of the health worker and the synergy of more professionals. The current research involves the collaboration of various figures related to the clinical field; they agree on the need to implement the knowledge of the phenomena related to the failure of adherence. The review of the literature has highlighted how difficult it is to understand the implications of a clinical fact that interfere with the assumption of therapy. Among the elements that lead to these results it would be useful to consider the unconscious aspects of patients. It is noticed that these aspects are dictated by emotions such as desire expressed differently if the patient has a passive role, as shown in Figures 3–5. It seems interesting to note how all five terms can currently be used according to: a) health education; b) knowledge of the patient; c) level of emotional maturity of the subject; d) personality type; e) value given by the health professional to cognitive and emotional processes; f) life planning; g) availability to knowledge; h) resilience.
However, it is not possible to respond hastily to some issues. Is it certain that among the terms “compliance”, “adherence”, “concordance”, “empowerment”, “self-management” a term can bring us closer to the patient’s experience? Is it evident that we can confide with the patient’s experience following the guidelines of one approach instead of another? Is it not true that a chronic pathology like diabetes could, in the long run, provoke a deviation in the subjective perception of the Self?
These questions, rather than discouraging health care, should shift attention from the objective processes of care to the comprehension of each patient. This is close to the phenomenological approach introduced by the German phenomenological tradition.105 In this case, one could easily notice how the quality of the therapeutic proposal, which in self-management would seem to be the best because it activates the conscience in terms of responsibility, in a chronic disease that is so widespread like diabetes it would be effective only in terms of ideals. Since therapy is a path rather than a goal, the idea is to propose a symbolic integration inherent in the very word of self-management. The word Self implies the overcoming of the Ego emphasized in compliance and in adherence, the intellectual overcoming of concordance, the mechanical cognitivism of empowerment.
Conclusions
The vast amount of literature, rather than emphasizing the successes and failures of the treatments, should offer a synthesis based on the complexity that every chronic disease poses. We suggest that the undoubted advantages of multi-disciplinary studies have contributed to a lengthening and improvement in the quality of life. We are faced with a complex phenomenology, which is foreseen by a continuum of damage that goes from the biological lesion to the maladjustment of the subject. The concept of care must be preceded by the promotion of quality of life and prevention policies. Based on the research carried out, a comprehensive need is outlined. We must take into account the resistance and the difficulties of including some aspects within patient care pathways. The valorization and the comprehension of the subjective modalities106 of conducting lifestyle would produce knowledge useful to bring the patient closer to clear indications of the medical prescriptions. The unknown aspects of physical and existential damage107 increase the weight of the phenomenon. The possibility of basing future treatments even on existential knowledge in the scientific field is certainly advantageous. The practical implications of this article refer to the inclusion of existential models of knowledge. The figures involved in this article have helped to suggest that the various points of view can be integrated into the field of care for diabetic patients, in order to turn the research experience into a practical support for patients and their subjective differences. This research aims to suggest an open point of view to the consideration of functional models that provide comprehension.
The peculiarity of the clinical psychology contribution suggests that even for chronic diseases such as diabetes, the mere possibility of listening to the patient could be a valid measure to alleviate the loneliness that aggravates every condition of suffering.108
Disclosure
The authors report no conflicts of interest in this research.
References
1. Boccuzzi SJ, Wogen J, Fox J, Sung JC, Shah AB, Kim J. Utilization of oral hypoglycemic agents in a drug-insured US population. Diabetes Care. 2001;24(8):1411–1415.
2. Norris SL, Engelgau MM, Narayan KV. Effectiveness of self-management training in type 2 diabetes: a systematic review of randomized controlled trials. Diabetes Care. 2001;24(3):561–587.
3. Gadsby R. Epidemiology of diabetes. Adv Drug Deliv Rev. 2002;54(9):1165–1172.
4. Michie S, Miles J, Weinman J. Patient-centredness in chronic illness: what is it and does it matter? Patient Educ Couns. 2003;51(3):197–206.
5. Pugh MJ, Anderson J, Pogach LM, Berlowitz DR. Differential adoption of pharmacotherapy recommendations for type 2 diabetes by generalists and specialists. Med Care Res Rev. 2003;60(2):178–200. doi:10.1177/1077558703060002003
6. Adolfsson ET, Smide B, Gregeby E, Fernström L, Wikblad K. Implementing empowerment group education in diabetes. Patient Educ Couns. 2004;53(3):319–324. doi:10.1016/j.pec.2003.07.009
7. Odegard PS, Capoccia K. Medication taking and diabetes. Diabetes Educ. 2007;33(6):1014–1029. doi:10.1177/0145721707308407
8. Mullen PD. Compliance becomes concordance. BMJ. 1997;314(7082):691. doi:10.1136/bmj.314.7082.691
9. Brown SA. Interventions to promote diabetes self-management: state of the science. Diabetes Educ. 1999;25(6_suppl):52–61. doi:10.1177/014572179902500623
10. Sugiharto S, Stephenson M, Hsu YY, Fajriyah NN. Diabetes self-management education training for community health center nurses in Indonesia: a best practice implementation project. BI Database System Rev Implement Rep. 2017;15(9):2390–2397. doi:10.11124/JBISRIR-2016-003329
11. Lutfey KE, Wishner WJ. Beyond” compliance” is” adherence”. Improving the prospect of diabetes care. Diabetes Care. 1999;22(4):635–639.
12. McNabb WL. Adherence in diabetes: can we define it and can we measure it? Diabetes Care. 1997;20(2):215. doi:10.2337/diacare.20.2.215
13. Tilson HH. Adherence or compliance? Changes in terminology. Ann Pharmacother. 2004;38(1):161–162. doi:10.1345/aph.1D207
14. Shrivastava SR, Shrivastava PS, Ramasamy J. Role of self-care in management of diabetes mellitus. J Diabetes Metab Disord. 2013;12(1):14. doi:10.1186/2251-6581-12-14
15. Jung CG. The Collected Works of CG Jung: Complete Digital Edition. Princeton: Princeton University Press; 2014.
16. Hayes E, McCahon C, Panahi MR, Hamre T, Pohlman K. Alliance not compliance: coaching strategies to improve type 2 diabetes outcomes. J Am Acad Nurse Pract. 2008;20(3):155–162. doi:10.1111/j.1745-7599.2007.00297.x
17. Aronson JK. Compliance, concordance, adherence. Br J Clin Pharmacol. 2007;63(4):383–384. doi:10.1111/j.1365-2125.2007.02893.x
18. Bailey CJ, Kodack M. Patient adherence to medication requirements for therapy of type 2 diabetes. Int J Clin Pract. 2011;65(3):314–322. doi:10.1111/j.1742-1241.2010.02544.x
19. Bangalore S, Kamalakkannan G, Parkar S, Messerli FH. Fixed-dose combinations improve medication compliance: a meta-analysis. Am J Med. 2007;120(8):713–719. doi:10.1016/j.amjmed.2006.08.033
20. Bell JS, Airaksinen MS, Lyles A, Chen TF, Aslani P. Concordance is not synonymous with compliance or adherence. Br J Clin Pharmacol. 2007;64(5):710–711. doi:10.1111/j.1365-2125.2007.02971_1.x
21. Bissell P, May CR, Noyce PR. From compliance to concordance: barriers to accomplishing a re-framed model of health care interactions. Soc Sci Med. 2004;58(4):851–862.
22. Bissonnette JM. Adherence: a concept analysis. J Adv Nurs. 2008;63(6):634–643. doi:10.1111/j.1365-2648.2008.04745.x
23. Bodenheimer T, Lorig K, Holman H, Grumbach K. Patient self-management of chronic disease in primary care. JAMA. 2002;288(19):2469–2475.
24. Bott U, Bott S, Hemmann D, Berger M. Evaluation of a holistic treatment and teaching programme for patients with Type 1 diabetes who failed to achieve their therapeutic goals under intensified insulin therapy. Diabet Med. 2000;17(9):635–643.
25. Bruni ML, Nobilio L, Ugolini C. Economic incentives in general practice: the impact of pay-for-participation and pay-for-compliance programs on diabetes care. Health Policy. 2009;90(2–3):140–148. doi:10.1016/j.healthpol.2008.09.008
26. Brunton S. I have never liked the term “compliance”. Clin Diabetes. 2017;35(2):76–77. doi:10.2337/cd17-0010
27. Burge MR. Lack of compliance with home blood glucose monitoring predicts hospitalization in diabetes. Diabetes Care. 2001;24(8):1502–1503.
28. Buse JB, Caprio S, Cefalu WT, et al. How do we define cure of diabetes? Diabetes Care. 2009;32(11):2133–2135. doi:10.2337/dc09-9036
29. Chan YM, Molassiotis A. The relationship between diabetes knowledge and compliance among Chinese with non-insulin dependent diabetes mellitus in Hong Kong. J Adv Nurs. 1999;30(2):431–438.
30. Charpentier G, Fleury F, Dubroca I, Vaur L, Clerson P. Electronic pill-boxes in the evaluation of oral hypoglycemic agent compliance. Diabetes Metab. 2005;31(2):189–195.
31. Chatterjee JS. From compliance to concordance in diabetes. J Med Ethics. 2006;32(9):507–510. doi:10.1136/jme.2005.012138
32. Ciechanowski PS, Katon WJ, Russo JE. Depression and diabetes: impact of depressive symptoms on adherence, function, and costs. Arch Intern Med. 2000;160(21):3278–3285.
33. Claxton AJ, Cramer J, Pierce C. A systematic review of the associations between dose regimens and medication compliance. Clin Ther. 2001;23(8):1296–1310.
34. Connor J, Rafter N, Rodgers A. Do fixed-dose combination pills or unit-of-use packaging improve adherence? A systematic review. Bull World Health Organ. 2004;82:935–939.
35. Cramer JA. A systematic review of adherence with medications for diabetes. Diabetes Care. 2004;27(5):1218–1224.
36. Cramer JA, Okikawa J, Bellaire S, Clauson P. Compliance with inhaled insulin treatment using the AERx® iDMS insulin diabetes management system. Diabetes Technol Ther. 2004;6(6):800–807. doi:10.1089/dia.2004.6.800
37. Cramer J, Okikawa J, Clauson P. Compliance with inhaled insulin treatment using AERx® iDMS insulin diabetes management system. Diabetes. 2003;52:A103.
38. Cyrino AP, Schraiber LB, Teixeira RR. Education for type 2 diabetes mellitus self-care: from compliance to empowerment. Interface (Botucatu). 2009;13(30):93–106. doi:10.1590/S1414-32832009000300009
39. Dailey G, Kim MS, Lian JF. Patient compliance and persistence with antihyperglycemic drug regimens: evaluation of a medicaid patient population with type 2 diabetes mellitus. Clin Ther. 2001;23(8):1311–1320.
40. Dailey G, Kim MS, Lian JF. Patient compliance and persistence with anti-hyperglycemic therapy: evaluation of a population of type 2 diabetic patients. J Int Med Res. 2002;30(1):71–79. doi:10.1177/147323000203000111
41. De las Cuevas C. Towards a clarification of terminology in medicine taking behavior: compliance, adherence and concordance are related although different terms with different uses. Curr Clin Pharmacol. 2011;6(2):74–77.
42. Delamater AM. Improving patient adherence. Clin Diabetes. 2006;24(2):71–77. doi:10.2337/diaclin.24.2.71
43. Donnan PT, MacDonald TM, Morris AD. Adherence to prescribed oral hypoglycaemic medication in a population of patients with type 2 diabetes: a retrospective cohort study. Diabet Med. 2002;19(4):279–284.
44. Fielding D, Duff A. Compliance with treatment protocols: interventions for children with chronic illness. Arch Dis Child. 1999;80(2):196–200.
45. Funnell MM, Anderson RM. The problem with compliance in diabetes. JAMA. 2000;284(13):1709. doi:10.1001/jama.284.13.1709-JMS1004-6-1
46. Funnell MM, Anderson RM. Empowerment and self-management of diabetes. Clin Diabetes. 2004;22(3):123–127. doi:10.2337/diaclin.22.3.123
47. García-Pérez LE, Álvarez M, Dilla T, Gil-Guillén V, Orozco-Beltrán D. Adherence to therapies in patients with type 2 diabetes. Diabetes Ther. 2013;4(2):175–194. doi:10.1007/s13300-013-0034-y
48. Gedawy A, Martinez J, Al-Salami H, Dass CR. Oral insulin delivery: existing barriers and current counter-strategies. J Pharm Pharmacol. 2018;70(2):197–213. doi:10.1111/jphp.12852
49. Glasgow RE, Anderson RM. In diabetes care, moving from compliance to adherence is not enough. Diabetes Care. 1999;22(12):2090. doi:10.2337/diacare.22.12.2090
50. Grant RW, Devita NG, Singer DE, Meigs JB. Polypharmacy and medication adherence in patients with type 2 diabetes. Diabetes Care. 2003;26(5):1408–1412.
51. Guillausseau PJ. Influence of oral antidiabetic drugs compliance on metabolic control in type 2 diabetes. A survey in general practice. Diabetes & Metab. 2003;29(1):79–81. doi:10.1016/S1262-3636(07)70011-3
52. Guillausseau PJ. Impact of compliance with oral antihyperglycemic agents on health outcomes in type 2 diabetes mellitus. Treat Endocrinol. 2005;4(3):167–175.
53. Harris MI. Health care and health status and outcomes for patients with type 2 diabetes. Diabetes Care. 2000;23(6):754–758.
54. Helme DW, Harrington NG. Patient accounts for noncompliance with diabetes self-care regimens and physician compliance-gaining response. Patient Educ Couns. 2004;55(2):281–292. doi:10.1016/j.pec.2003.10.004
55. Henshaw L. Empowerment, diabetes and the national service framework: a systematic review. J Diabetes Nurs. 2006;10(4):128.
56. Howorka K, Pumprla J, Wagner-Nosiska D, Grillmayr H, Schlusche C, Schabmann A. Empowering diabetes out-patients with structured education:: short-term and long-term effects of functional insulin treatment on perceived control over diabetes. J Psychosom Res. 2000;48(1):37–44.
57. Ibrahim NK, Attia SG, Sallam SA, Fetohy EM, El-Sewi F. Physicians’ therapeutic practice and compliance of diabetic patients attending rural primary health care units in Alexandria. J Family Community Med. 2010;17(3):121. doi:10.4103/1319-1683.74325
58. Ingersoll KS, Cohen J. The impact of medication regimen factors on adherence to chronic treatment: a review of literature. J Behav Med. 2008;31(3):213–224. doi:10.1007/s10865-007-9147-y
59. Istepanian RS, Sungoor A, Earle KA. Technical and compliance considerations for mobile health self-monitoring of glucose and blood pressure for patients with diabetes. Conf Proc IEEE Eng Med Biol Soc. 2009;2009:5130–5133.
60. Jensen ML, Jørgensen ME, Hansen EH, Aagaard L, Carstensen B. Long-term patterns of adherence to medication therapy among patients with type 2 diabetes mellitus in Denmark: the importance of initiation. PLoS One. 2017;12(6):e0179546. doi:10.1371/journal.pone.0179546
61. Kardas P. The DIACOM study (effect of DosIng frequency of oral Antidiabetic agents on the COMpliance and biochemical control of type 2 diabetes). Diabetes Obes Metab. 2005;7(6):722–728. doi:10.1111/j.1463-1326.2004.00462.x
62. Keers JC, Blaauwwiekel EE, Hania M, et al. Diabetes rehabilitation: development and first results of a Multidisciplinary Intensive Education Program for patients with prolonged self-management difficulties. Patient Educ Couns. 2004;52(2):151–157.
63. Kennedy-Martin T, Boye KS, Peng X. Cost of medication adherence and persistence in type 2 diabetes mellitus: a literature review. Patient Prefer Adherence. 2017;11:1103. doi:10.2147/PPA.S134792
64. Kyngäs H. A theoretical model of compliance in young diabetics. J Clin Nurs. 1999;8(1):73–80.
65. Kyngäs H. Compliance of adolescents with chronic disease. J Clin Nurs. 2000;9(4):549–556.
66. Kyngäs H. Compliance of adolescents with diabetes. J Pediatr Nurs. 2000;15(4):260–267. doi:10.1053/jpdn.2000.6169
67. Kyng As HA, Kroll T, Duffy ME. Compliance in adolescents with chronic diseases: a review. J Adolesc Health. 2000;6(26):379–388.
68. Kyngäs H, Rissanen M. Support as a crucial predictor of good compliance of adolescents with a chronic disease. J Clin Nurs. 2001;10(6):767–774.
69. Kyngäs H, Duffy ME, Kroll T. Conceptual analysis of compliance. J Clin Nurs. 2000;9(1):5–12.
70. Kyngäs H, Hentinen M, Barlow JH. Adolescents’ perceptions of physicians, nurses, parents and friends: help or hindrance in compliance with diabetes self-care? J Adv Nurs. 1998;27(4):760–769.
71. Lawler FH, Viviani N. Patient and physician perspectives regarding treatment of diabetes: compliance with practice guidelines. J Fam Pract. 1997;44(4):369–374.
72. Lobach DF, Hammond WE. Computerized decision support based on a clinical practice guideline improves compliance with care standards. Am J Med. 1997;102(1):89–98.
73. Lombardo F, Salzano G, Messina MF, De Luca F. Compliance and administration methods in management of type 1 diabetes. Acta Biomed. 2005;76(Suppl 3):66–69.
74. Moström P, Ahlén E, Imberg H, Hansson PO, Lind M. Adherence of self-monitoring of blood glucose in persons with type 1 diabetes in Sweden. BMJ Open Diabetes Res Care. 2017;5(1):e000342. doi:10.1136/bmjdrc-2016-000342
75. Nazir R, Ur S, Azmi Hassali M, Saleem F, Bashir S, Aljadhey H. Does adherence to the therapeutic regimen associate with health related quality of life: findings from an observational study of type 2 diabetes mellitus patients in Pakistan. Pak J Pharm Sci. 2017;30(6):2159–2165.
76. Norris SL, Lau J, Smith SJ, Schmid CH, Engelgau MM. Self-management education for adults with type 2 diabetes: a meta-analysis of the effect on glycemic control. Diabetes Care. 2002;25(7):1159–1171.
77. Paes AH, Bakker A, Soe-Agnie CJ. Impact of dosage frequency on patient compliance. Diabetes Care. 1997;20(10):1512–1517.
78. Paterson B. Myth of empowerment in chronic illness. J Adv Nurs. 2001;34(5):574–581.
79. Pladevall M, Williams LK, Potts LA, Divine G, Xi H, Lafata JE. Clinical outcomes and adherence to medications measured by claims data in patients with diabetes. Diabetes Care. 2004;27(12):2800–2805.
80. Renders CM, Valk GD, Griffin SJ, Wagner EH, Assendelft WJ. Interventions to improve the management of diabetes in primary care, outpatient, and community settings: a systematic review. Diabetes Care. 2001;24(10):1821–1833.
81. Renders CM, Valk GD, Griffin SJ, Wagner E, van Eijk JT, Assendelft WJ. Interventions to improve the management of diabetes mellitus in primary care, outpatient and community settings. Cochrane Database Syst Rev. 2000;(4). doi:10.1002/14651858.CD001481.
82. Rosen MI, Beauvais JE, Rigsby MO, Salahi JT, Ryan CE, Cramer JA. Neuropsychological correlates of suboptimal adherence to metformin. J Behav Med. 2003;26(4):349–360.
83. Roter DL, Hall JA, Merisca R, Nordstrom B, Cretin D, Svarstad B. Effectiveness of interventions to improve patient compliance: a meta-analysis. Med Care. 1998;1138–1161. doi:10.1097/00005650-199808000-00004
84. Schaper NC, Nikolajsen A, Sandberg A, Buchs S, Bøgelund M. Timing of insulin injections, adherence, and glycemic control in a multinational sample of people with type 2 diabetes: a cross-sectional analysis. Diabetes Ther. 2017;8(6):1319–1329. doi:10.1007/s13300-017-0317-9
85. Schectman JM, Nadkarni MM, Voss JD. The association between diabetes metabolic control and drug adherence in an indigent population. Diabetes Care. 2002;25(6):1015–1021.
86. Schilling LS, Grey M, Knafl KA. The concept of self-management of type 1 diabetes in children and adolescents: an evolutionary concept analysis. J Adv Nurs. 2002;37(1):87–99.
87. Shenolikar RA, Balkrishnan R, Camacho FT, Whitmire JT, Anderson RT. Race and medication adherence in Medicaid enrollees with type-2 diabetes. J Natl Med Assoc. 2006;98(7):1071.
88. Shoemaker A, Cheng P, Gal RL, et al. Predictors of loss to follow-up among children with type 2 diabetes. Horm Res Paediatr. 2017;87(6):377–384. doi:10.1159/000475595
89. Srinivasan NK, John D, Rebekah G, Kujur ES, Paul P, John SS. Diabetes and diabetic retinopathy: knowledge, attitude, practice (KAP) among diabetic patients in a tertiary eye care centre. J Clin Diagn Res. 2017;11(7):NC01. doi:10.7860/JCDR/2017/24731.9963
90. Steinhardt MA, Brown SA, Dubois SK, Jr L H, Lehrer HM, Jaggars SS. A resilience intervention in African-American adults with type 2 diabetes. Am J Health Behav. 2015;39(4):507–518. doi:10.5993/AJHB.39.4.7
91. Steinhardt MA, Mamerow MM, Brown SA, Jolly CA. A resilience intervention in African American adults with type 2 diabetes. Diabetes Educ. 2009;35(2):274–284. doi:10.1177/0145721708329698
92. Subramanian K, Midha I, Chelapilla V. Overcoming the challenges in implementing type 2 diabetes mellitus prevention programs can decrease the burden on healthcare costs in the United States. J Diabetes Res. 2017;2017:2615681.
93. Sweileh W, Aker O, Hamooz S. Rate of compliance among patients with diabetes mellitus and hypertension. An-Najah Univ J Res (N Sci). 2005;19:1.
94. Timms N, Lowes L. Autonomy or non-compliance in adolescent diabetes? Br J Nurs. 1999;8(12):794–800. doi:10.12968/bjon.1999.8.12.6574
95. Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care activities measure: results from 7 studies and a revised scale. Diabetes Care. 2000;23(7):943–950.
96. Vermeire EI, Wens J, Van Royen P, Biot Y, Hearnshaw H, Lindenmeyer A. Interventions for improving adherence to treatment recommendations in people with type 2 diabetes mellitus. Cochrane Database Syst Rev. 2005;(2). doi:10.1002/14651858.CD003638.pub2.
97. Walker EA, Usher JA. Understanding and enhancing adherence in adults with diabetes. Curr Diab Rep. 2003;3(2):141–148.
98. Wens J, Vermeire E, Van Royen P, Hearnshaw H. A systematic review of adherence with medications for diabetes (Letter). Diabetes Care. 2004;27:2284. doi:10.2337/diacare.27.9.2284
99. Winer N, Folker A, Murphy JA, et al. Effect of fixed-dose ACE-inhibitor/calcium channel blocker combination therapy vs. ACE-inhibitor monotherapy on arterial compliance in hypertensive patients with type 2 diabetes. Prev Cardiol. 2005;8(2):87–92.
100. Worrall G, Freake D, Kelland J, Pickle A, Kennan T. Care of patients with type II diabetes: a study of family physicians’ compliance with clinical practice guidelines. J Fam Pract. 1997;44(4):374–382.
101. Zhao G, Ford ES, Li C, Mokdad AH. Compliance with physical activity recommendations in US adults with diabetes. Diabet Med. 2008;25(2):221–227. doi:10.1111/j.1464-5491.2007.02332.x
102. Zhu J, Xu J, Chen Y, et al. Cross-cultural adaption and psychometric properties of the Chinese version of the Diabetes Behavior Rating Scale: a pilot study. Sci China Life Sci. 2018;61(3):310–317. doi:10.1007/s11427-016-9070-7
103. Oxford English Dictionary; 2008. Available from:
104. Manfredi P. La concordanza nel rapporto medico-paziente e la formazione medica [Concordance in the doctor-patient relationship and medical training]. MEDIC. 2016;24(2):58–63. Italian.
105. Jaspers K. Allgemeine Psychopathologie. Berlin: Springer; 1959 [1913] (trad. it. di R. Priori, Psicopatologia generale, Il pensiero Scientifico Editore, Roma 1964).
106. Langher V, Caputo A, Martino G. What happened to the clinical approach to case study in psychological research? A clinical psychological analysis of scientific articles in high impact-factor journals. Mediterr J Clin Psychol. 2017;5(3).
107. Marchini F, Caputo A, Napoli A, Balonan JT, Martino G, Nannini V, Langher V. Chronic illness as loss of good self: underlying mechanisms affecting diabetes adaptation. Mediterr J Clin Psychol. 2018
108. Borgna E, ed. Malinconia [Melancholy]. Milan: Universale Economica Feltrinelli/Saggi; 2001. Italian.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
