Back to Journals » Clinical Ophthalmology » Volume 14
Comparison of the iLUX and the LipiFlow for the Treatment of Meibomian Gland Dysfunction and Symptoms: A Randomized Clinical Trial
Authors Tauber J , Owen J , Bloomenstein M, Hovanesian J , Bullimore MA
Received 10 October 2019
Accepted for publication 10 January 2020
Published 12 February 2020 Volume 2020:14 Pages 405—418
DOI https://doi.org/10.2147/OPTH.S234008
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Joseph Tauber,1 James Owen,2 Marc Bloomenstein,3 John Hovanesian,4 Mark A Bullimore5
1Tauber Eye Center, Kansas City, MO 64111, USA; 2TLC Laser Eye Centers-La Jolla, La Jolla, CA 92122, USA; 3Schwartz Laser Eye Center, Scottsdale, AZ 85260, USA; 4Harvard Eye Associates, Laguna Hills, CA 92653, USA; 5University of Houston, College of Optometry, Houston, TX 77204, USA
Correspondence: Joseph Tauber
Tauber Eye Center, 4400 Broadway, Suite 202, Kansas City, MO 64111, USA
Tel +1 816 531 9100
Fax +1 816 531 9105
Email [email protected]
Purpose: To compare the effects of eyelid treatment with the iLUX MGD Treatment System and the LipiFlow Thermal Pulsation System on objective and subjective parameters of meibomian gland function and symptoms.
Patients and Methods: In this randomized, open-label, controlled, multicenter clinical trial, both eyes of 142 patients aged ≥ 18 years with Ocular Surface Disease Index (OSDI) scores ≥ 23, total meibomian gland scores (MGS) ≤ 12 in the lower eyelid of each eye, and tear break-up time (TBUT) < 10 s were randomized 1:1 to iLUX or LipiFlow treatment, with stratification by test center. The primary effectiveness endpoints were changes in total MGS (masked) and TBUT from baseline to 4 weeks. The secondary effectiveness endpoint was changed in OSDI score from baseline to 4 weeks.
Results: Both devices significantly improved effectiveness outcomes, with no differences between the two devices. At the 4-week visit, mean MGS, TBUT, and OSDI scores improved at least 16.9 ± 11.5, 2.6 ± 3.2 s, and 28.0 ± 22.8, respectively, across treatment groups and treated eyes. Four device/procedure-related events occurred in the iLUX group, compared with none in the LipiFlow group, but there were no device-related adverse events that involved changes in lid margins, eyelids, or lash integrity. Corneal staining, intraocular pressure, and visual acuity did not differ in the two groups.
Conclusion: Both treatments produced significant improvements in meibomian gland function and symptoms. For all effectiveness measures, there were no statistically significant differences between the two treatments.
Keywords: meibomian gland dysfunction, meibomian gland score, tear break-up time, ocular surface disease index
Introduction
Meibomian gland dysfunction (MGD) is one of the most commonly encountered ocular conditions in ophthalmic practice, with an estimated prevalence of 3.5% to almost 70%.1 Although previously thought to primarily affect older individuals, one study reported a prevalence of 42% in a pediatric population, as evidenced by meibomian gland atrophy (MGA).2 MGD is also thought to contribute to contact lens discomfort.3 Because MGD is frequently not obvious,4 it can be underdiagnosed or diagnosed too late once it becomes clinically obvious, with eyelid margin changes, MGA and ocular surface inflammation. Its chronic and progressive nature warrants regular and comprehensive care of the approximately 60 meibomian glands in each eye.4
Treatment of MGD often involves the application of heat to the eyelids, using warm compresses, with or without lid massage to melt the abnormal meibum and facilitate its re-entry into the tear film.5 Lipid-based artificial tears can restore thin or irregular lipid layers, temporarily relieving symptoms and improving quality of vision.6,7 Pharmaceutical options include essential fatty acid supplementation, systemic tetracycline and azithromycin, topical antibiotics and corticosteroids, and topical tacrolimus ointment for refractory cases.5,8 Mechanical management involves debridement of eyelid margins9 and various methods to forcibly express abnormal meibum, with or without prior heating. In patients with severe terminal duct obstruction, conductive thermal pulsation treatment of the eyelids has been shown to improve signs and symptoms over 12 months.10 Moreover, patients with inflammatory ocular rosacea related to MGD may benefit from intense pulsed light therapy.11
Sustained heat from the level of the meibomian glands to the posterior portion of the eyelid is highly important. The melting point of meibomian gland secretions ranges from 32°C to 40°C,12 with melting points elevated in patients with meibomian gland dysfunction, allowing secretions to stagnate.12,13 Warm compresses rapidly lose heat and fall below the therapeutic temperature of 40°C within the first minute of application.14 Even commercially available eyelid masks microwaved for 10–20 s do not remain consistently above 38°C for the entire 10-min treatment.14 An evaluation of eight methods of eyelid warming found that the method that most effectively maintained internal eyelid temperature, the bundle method, was also the most cumbersome.15 Eyelid thermal pulsation devices apply heat at the appropriate temperature closer to the meibomian glands, while simultaneously compressing the glands to evacuate their contents.15
The iLUX MGD Treatment System (Alcon, Fort Worth, TX, USA) is a device that simultaneously applies localized heat and compression to safely and effectively treat MGD. This study compared objective and subjective changes in meibomian gland function and symptoms after treatment of upper and lower eyelids with the iLUX and the LipiFlow Thermal Pulsation System (Johnson & Johnson Vision, Jacksonville, FL, USA).
Materials and Methods
Study Design
This randomized, open-label, controlled, multicenter clinical trial compared the iLUX MGD Treatment System with the LipiFlow Thermal Pulsation System for the treatment of MGD. The goal of this study was to verify that technological differences between the two systems did not adversely affect safety and efficacy. Eligible subjects at eight clinical sites in the United States were randomized 1:1 to one session each of bilateral treatment with the iLUX or Lipiflow device. This study conformed to the principles of the Declaration of Helsinki. The protocol was approved by the Aspire IRB and all subjects provided written informed consent prior to any study-related procedures. The trial was registered at www.clinicaltrials.gov as NCT03055832.
Inclusion and Exclusion Criteria
The inclusion criteria were age ≥18 years; any gender or race; a history of self-reported dry eye symptoms for 3 months prior to study enrollment, as shown by baseline scores on the Ocular Surface Disease Index (OSDI) questionnaire ≥23, indicative of moderate or severe ocular surface disease;16 evidence of meibomian gland obstruction, as shown by total meibomian gland scores (MGS) ≤12 in the lower eyelid of each eye;17,18 tear break-up time (TBUT) <10 s; and agreement/ability to abstain from dry eye/MGD medications for the study duration. Ocular lubricants were allowed if no changes to the regimen were made during the study.
Exclusion criteria were conditions that could potentially increase the risk of procedure-related injury or confound study results, including a history of ocular surgery, giant papillary conjunctivitis, punctal plugs or previous punctal cautery, ocular injury or trauma, chemical burns, limbal stem cell deficiency, aphakia, cicatricial lid margin disease, active ocular infection or non-dry eye inflammation, irregular cornea, lid abnormalities, anterior or Demodex blepharitis, and systemic disease conditions that cause dry eye. Subjects were also excluded if they had a history of use of isotretinoin within 1 year, cyclosporine-A 0.05% or lifitegrast 5% within 3 months or any other pharmaceutical treatments for dry eye/MGD within 2 weeks; contact lens wear during the prior 3 months; LipiFlow treatment within 2 years; eyelid tattoos including permanent eyeliner makeup; or use of other ophthalmic investigational devices or agents within 30 days of study participation.
Randomization
Eligible subjects at each site were randomized 1:1 to the iLUX or LipiFlow group. Sequentially numbered envelopes containing the assigned treatment procedure were provided to each site. Before treatment, the personnel assigned to perform the treatment opened the lowest numbered envelope. The envelope number was documented on the study source documents and in the database.
Treatment
Both eyes were treated on the same day (Day 0). Eye makeup was removed, and anesthetic eye drops were instilled into both eyes. The selected device was prepared and treatment was delivered as described in the user manual for that device. In the iLUX group at all study sites, right eyes were treated prior to left eyes. The upper lid, central-nasal region was treated first; followed by the lower lid, central-nasal region; and the lower lid, central-temporal region. Adverse events were monitored throughout treatment and for 1 hr afterward.
Effectiveness Endpoints
The primary effectiveness endpoints were changes from baseline to 4 weeks in total MGS and TBUT. MGS was assessed by slit-lamp microscopy and involved grading the meibum quality of five glands in each of three lower eyelid regions (nasal, central, temporal) with the Meibomian Gland Evaluator (Johnson & Johnson Vision). Each of these 15 glands was graded from 0 to 3 (0 = no secretion, 1 = inspissated, 2 = cloudy, 3 = clear liquid).19,20 The clinicians evaluating MGS were not involved in any other study procedure and were masked to subject treatment assignment.
TBUT was evaluated using fluorescein strips as described previously.21 Briefly, one or two drops of non-preserved saline were applied to the impregnated tip of 0.12-mg fluorescein strips (Amcon Laboratories, Saint Louis, MO, USA). The patient was asked to look down and in, and the strip was gently applied to the superior temporal bulbar conjunctiva. The patient was asked to blink naturally three times and open their eyes. The time between the last blink and the first appearance of a dark spot on the cornea was recorded in seconds. Three consecutive measurements were averaged and the procedure repeated with a new strip for the second eye.
The secondary effectiveness endpoint was the change from baseline to 4 weeks in patient symptoms, as assessed using the OSDI, a validated, 12-item questionnaire using a 5-point scale to evaluate the frequency of dry eye symptoms in three categories. Total OSDI was calculated as the sum of scores × 25/number of questions answered.22,23
All efficacy measures were assessed at baseline and 2 and 4 weeks after treatment.
Safety Endpoints
The primary safety endpoint was the incidence of device-related adverse events, including changes in lid margins; development of floppy eyelids, entropion or ectropion; and lash integrity, with the latter defined as subjective impression of any lash irregularity or loss. Secondary safety endpoints included discomfort and pain during treatment, and changes from baseline in ocular surface staining, intraocular pressure (IOP), and best spectacle-corrected visual acuity (BSCVA).
Pain was assessed using a 100-point visual analog scale with anchored descriptions. Subjects rated pain in or around the eyelids or face during the procedure immediately after the procedure and pain during the previous week at all time points. For reference, a rating of 20 corresponds to “hurts a little bit.” Questionnaires were self-administered by the subject prior to any clinical assessment.
Slit-lamp examination was used to grade the adnexa, lids/lashes, conjunctiva, sclera, corneal clarity and surface integrity, anterior chamber, and iris and to record significant positive findings, including pterygium, pinguecula, corneal scar, conjunctival pigment, and corneal arcus. Any observed lid margin abnormalities were graded on a 0–4 scale, based on the number of the following present in each eye: irregular lid margin, vascular engorgement, plugged meibomian gland orifices, and anterior or posterior displacement of the mucocutaneous junction.24 The development of entropion or ectropion, floppy eyelids, and loss of lash integrity was also recorded.
Corneal fluorescein staining was evaluated by slit-lamp examination of five corneal regions: superior, inferior, central, temporal, and nasal, using the National Eye Institute corneal grading scale.25 On this scale, 0 = normal-no staining, 1 = mild-superficial stippling/micropunctate staining, 2 = moderate-macropunctate staining with some coalescent areas, and 3 = severe-numerous coalescent macropunctate areas and/or patches.
BSCVA was measured using by-letter scoring with ETDRS high contrast charts with manifest refraction results. IOP was measured by Goldmann tonometry.
All safety measures were assessed at baseline and 2 and 4 weeks after treatment. In addition, BSCVA and IOP were measured and corneal staining was graded immediately after treatment and the following day. Pain and discomfort were also assessed the day after treatment.
The iLUX MGD Treatment System
The iLUX MGD Treatment System is an eyelid thermal pulsation system comprised of a single-use patient interface device and a handheld battery-powered instrument (Figure 1). The patient interface device is made of biocompatible medical grade silicone, with the inner and outer pads in contact with the palpebral conjunctiva and the external eyelid, respectively. Temperature sensors measure the inner and outer eyelid temperatures, to maintain a meibum melt temperature of 38–42°C. These sensors automatically turn off the LEDs when the temperatures on the inner and outer eyelids exceed 44°C and 45°C, respectively.
 |
Figure 1 The iLUX MGD Treatment System. Reproduced with permission of Alcon. |
Data Analysis
Continuous variables are reported as number, mean, standard deviation, and, for change, 95% confidence intervals, and categorical and binary variables as number and percentage. Analysis of covariance (ANCOVA) was used to assess the effects of iLUX and LipiFlow treatment on the primary and secondary effectiveness endpoints assessed at baseline and at 4 weeks, with the baseline measurement considered a covariate for each endpoint analyzed.
If non-inferiority was demonstrated for the primary endpoints, success was claimed only if the mean change from baseline in the test arm was clinically significant (see definitions below) and significantly different from zero. If these conditions were met, a test for superiority was performed.
All enrolled subjects were included in the safety analysis. Subjects who were randomized but not treated for any reason were included in the intent-to-treat analysis but excluded from the per-protocol analysis.
Clinically Significant Effects
Criteria for clinical relevance were used to establish the non-inferiority margins for change from baseline and comparisons of study arms. For example, a 5-point difference in MGS, indicating a change in MGD severity, was the criterion for clinical relevance.21 Because criteria for clinically relevant improvements in TBUT have not been determined, clinical relevance was based on the labeling of the DET test strip. The difference between dry and normal tear stability was 5 s; thus, a moderate change of 50% defines a TBUT difference of 2.5 s as clinically relevant. A change in OSDI score of ≥7 points was defined as clinically relevant, based on a study of patients with moderate and severe dry eye.16
Sample Size Justification
This study design provides a combined power of 88% to demonstrate non-inferiority, based on a) an MGS non-inferiority delta of 5 points and standard deviation (SD) of 8 points, providing a MGS primary endpoint power of 93.9%; and b) a TBUT non-inferiority delta of 2.5 s and SD of 4 s, providing a TBUT primary endpoint power of 93.9%. Based on both primary endpoints being independent and assessed 4 weeks after treatment, the probability that both endpoints are significant was 0.93922 = 0.882, or 88.2%.
For the secondary endpoint (OSDI), a SD of 14 was assumed based on pilot data, and the non-inferiority delta was set at 7. The chosen sample size and ɑ = 0.025 provide 80% power for this endpoint.
The minimum sample size required to demonstrate non-inferiority for treatment with iLUX compared with LipiFlow for the primary effectiveness endpoint was 256 eyes (128 subjects). Based on a 10% dropout rate, 142 subjects with MGD and a history of dry eye symptoms were enrolled.
Results
This study enrolled and randomized 142 subjects, consisting of 101 women and 41 men aged 19–86 years (mean age, 54.9 ± 15.3 years); the sex ratio is typical of patients with dry eye, with a ratio of women to men ranging from 2:1 to 3:1.16,19,26 Most subjects (90.8%) were white. Seventy-one subjects were treated with the iLUX and 70 with the LipiFlow. One subject in the LipiFlow treatment arm had one eye that could not be treated because the device’s activator was too large to fit the subject’s eye. One subject in the iLUX treatment arm withdrew from the study 1 week after treatment due to resumption of contact lens wear during the study period (Figure 2).
 |
Figure 2 CONSORT flow diagram presenting patient enrollment at each phase of the study for both the Lipiflow and iLUX treatment groups. |
Effectiveness of Treatment
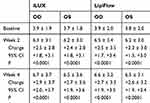
Table 1 shows mean MGS for right and left eyes of the two treatment groups at weeks 2 and 4, as well as changes from baseline. Figure 3 shows that the mean MGS for both eyes improved significantly from baseline in both treatment groups, at both follow-up visits (p<0.0001 each). MGS improvements, however, were similar in the two treatment groups at weeks 2 and 4 (p≥0.63).
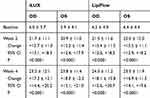 |
Table 1 Mean Meibomian Gland Scores (±SD) at Each Study Visit for Patients Treated with iLUX and LipiFlow. Change from Baseline at Weeks 2 and 4 are Also Shown Along with 95% Confidence Intervals |
 |
Figure 3 Mean ± SD Meibomian Gland Scores in the right eyes of subjects in the iLUX and LipiFlow groups at baseline and 2 and 4 weeks after treatment. |
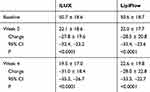
Table 2 shows mean TBUT for right and left eyes of the two treatment group at weeks 2 and 4, as well as changes from baseline. Figure 4 shows that the mean TBUT for both eyes improved significantly from baseline in both groups at both follow-up visits (all p<0.0001). TBUT improvements were similar in the two groups at both follow-up visits (p≥0.76).
 |
Figure 4 Mean ± SD tear break-up times in the right eyes of subjects in the iLUX and LipiFlow groups at baseline and 2 and 4 weeks after treatment. |
Table 3 shows mean OSDI scores for each treatment group at weeks 2 and week 4, as well as changes from baseline, and Figure 5 shows that mean OSDI scores improved significantly from baseline in both treatment groups at both follow-up visits (all p<0.0001). OSDI improvements were similar in the two groups, both overall (p=0.37) and after 4 weeks (p=0.29).
 |
Figure 5 Mean ± SD Ocular Surface Disease Index scores of subjects in the iLUX and LipiFlow groups at baseline and 2 and 4 weeks after treatment. |
Because of the lack of significant differences between the two instruments for any of the primary and secondary effectiveness endpoints, we performed post hoc sample size calculations to determine the differences that could have been detected with a given statistical power. With 140 eyes (70 per arm) and based on a two-tailed hypothesis and an alpha of 0.05, the study would have had 80% power to detect a six-point difference in MGS, a 12 point difference on the OSDI, and a 2-second difference in TBUT between the instruments.
Safety of Treatment
There were no device-related adverse events in either arm of the study that involved changes in the lid margin; development of floppy eyelids, entropion or ectropion; or changes in lash integrity. Four device/procedure-related adverse events were observed in the iLUX group. All four were self-limited, transient, and resolved without sequelae. The incidence of procedure-related adverse events did not differ significantly in the iLUX and Lipiflow groups (Fisher’s exact test, p=0.12).
Four device/procedure-related events occurred in the iLUX group. One subject pulled away during the first application of the iLUX, feeling that the device was too hot despite the use of topical ocular anesthetic. The device temperature was verified to be under 42ºC throughout the treatment. No eyelid findings consistent with burn or injury were observed, although the subject experienced bilateral epiphora, which resolved after 10 mins. This subject did not experience increases in post-treatment pain and discomfort scores. A second subject reported a burning sensation during treatment, which resolved after 1 day. This subject had permanent eye makeup (eyelid margin tattoo) and should not have been enrolled in the trial per the protocol. A third subject experienced bilateral mild petechial hemorrhaging on the lower palpebral conjunctiva. This event, which was reported to be mild in severity, required no treatment and resolved within 2 weeks. All three of these subjects were able to complete treatment, with no significant findings or changes in visual acuity, BSCVA, slit-lamp examination, IOP, or corneal fluorescein staining. At the 1-day follow-up visit, the fourth subject presented with a 10-letter decrease in BSCVA. During the procedure on the previous day, the outer pad of the device reached the maximum safe temperature, resulting in device shut off (a safety feature). The patient resumed treatment at the same visit and completed the procedure. This subject’s corneal fluorescein staining score increased to 3 (from a baseline of 1) in the inferior region of both eyes immediately after treatment but returned to baseline 1 day later. Because both eyes presented with inferior corneal staining, this was unlikely due to device shut-off resulting from the elevated temperature on the outer pad, which does not interface with the corneal surface, and only occurred on the left eye. The cause of corneal staining is unclear, but this type of superficial punctate keratitis has been observed in patients administered topical anesthetic drops for other procedures, such as LASIK and cataract surgery, or for exposure keratitis. In these patients, the condition resolved without treatment, as in this subject. This subject’s BSCVA returned to baseline at 2 weeks.
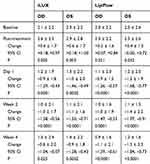
Tables 4 and 5 show the mean pain and discomfort ratings, respectively, for right and left eyes of each group, as well as their changes from baseline. Mean pain and discomfort scores were significantly lower than baseline in the two treatment groups at follow-up (p<0.0001). Pain rating improvement did not differ significantly in the iLUX and Lipiflow groups at 4 weeks (p≥0.13), whereas discomfort improvement in right (p=0.025) and left (p=0.052) eyes favored the iLUX group.
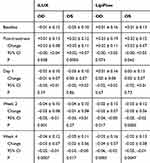
Table 6 shows the mean corneal staining scores for right and left eyes in each group at each study visit, as well as changes from baseline. Staining scores for both eyes increased immediately after treatment in both groups, but only about 0.5 points on a 15-point scale. At all follow-up visits through week 4, corneal staining was significantly reduced relative to baseline in both groups, but was similar in the two groups (p>0.09).
Table 7 shows the mean BSCVA for right and left eyes in each group at each study visit, as well as changes from baseline. BSCVA in both groups was reduced 0.02–0.05 logMAR (1 or 2 letters) immediately after treatment, likely due to contact of the eye and adnexa with both instruments. BSCVA improved subsequently and, relative to baseline, was significantly improved by 0.02–0.04 logMAR at week 4 in both groups, with no significant between-group differences (p≥0.68).
IOP in both groups did not change significantly immediately after treatment. At week 4, IOP was reduced significantly in the iLUX group but this reduction of 1 mmHg was not clinically meaningful.
Discussion
Overall, both the iLUX and LipiFlow treatments significantly improved the signs and symptoms of MGD. For all effectiveness measures, there were no clinically meaningful or statistically significant differences between the two treatments. Furthermore, the difference between treatment groups was not influenced by gender or clinical site. Both primary effectiveness endpoints, MGS and TBUT, improved significantly from baseline in both groups, at both follow-up visits and in both eyes. The 4-week improvement of 17–18 of 45 points on the MGS was substantially greater than the 5-point threshold for clinical relevance.21 Similarly, the 4-week improvement in TBUT was greater than the clinically meaningful level of 2.5 s. In addition, OSDI scores improved significantly from baseline in both groups at both follow-up visits. The 30-point change observed in both groups at 4 weeks should be compared with previous determinations of clinically meaningful changes. For example, a study of 310 patients ranging in dry eye severity found that changes in OSDI scores of 4.5–7.3 points were meaningful for subjects with mild or moderate symptoms and changes of 7.3–13.4 points were meaningful for subjects with severe symptoms.16 The 30-point improvement observed in the present study was therefore likely to be clinically important.
The observed improvements in OSDI scores compare favorably with those of FDA-approved topical medications for the management of dry eye. A randomized, multicenter, double-masked clinical trial of various concentrations of cyclosporine (0.05–0.4%) found that mean improvements in OSDI scores ranged from 3 to 15 points at the end of the 12-week treatment and from 7 to 13 points 4 weeks later.27 That study, however, included patients with less severe disease (baseline OSDI 33–42) than those in the present study (baseline OSDI >50).
A multicenter, prospective, double-masked, placebo-controlled trial found that lifitegrast (0.1%, 1.0%, 5.0%) improved mean OSDI scores 5–6 points on days 14 and 84, with no change in the placebo group.28 Again, baseline OSDI scores ranged from 29 to 33, indicating that these subjects had less severe disease than those in the present study. These improvements were not replicated in a larger randomized, double-masked, multicenter clinical trial of 5.0% lifitegrast ophthalmic solution in 588 subjects with dry eye disease.29 Mean OSDI scores were 27 and 26 in the placebo and lifitegrast groups, respectively, but no statistically significant differences were observed at baseline or at any follow-up visit. The primary efficacy outcome, change in the visual-related function subscale of the OSDI, also did not differ in the lifitegrast and placebo groups.
The Dry Eye Assessment and Management (DREAM) Study Research Group randomized 535 patients to a daily oral dose of 3000 mg of fish-derived n-3 fatty acids or an olive oil placebo.26 OSDI scores at 12 months improved significantly in both groups, by 13.9 and 12.5 points, respectively, but did not differ significantly in these two groups. Patients in the DREAM study were required to have OSDI scores of 25–80 at screening and 21–80 at eligibility confirmation. The mean OSDI scores in the DREAM study at baseline were 44 points in both groups, indicating that these subjects had similar disease severity as subjects in the present study.
No subject in either group of the present study experienced any device-related adverse events that involved changes in the lid margin; development of floppy eyelids, entropion or ectropion; or changes in lash integrity. Four subjects in the iLUX group experienced device/procedure-related adverse events not specified as key events within the primary safety endpoint. Two patients experienced burning sensations without skin findings and one had petechial hemorrhaging in the lower lids. One patient experienced a transient decrease in BSCVA with findings consistent with exposure keratitis. All of these events were self-limited, transient, and resolved without sequelae. Similar results were reported in a previous Lipiflow study, in which 3 of 138 eyes experienced moderate eyelid pain, one eye had a moderate conjunctival vascular injection, and two eyes experienced a 10-letter decrease in BSCVA.20 In the same study, the most common slit-lamp findings were trace to mild conjunctival injection, hyperemia, or redness; and trace to mild petechial hemorrhages on the eyelid or conjunctiva immediately after treatment or 1-day later, with all of these being fully resolved without treatment 2 weeks later.
In general, there were no between-group differences in pain, surface staining, IOP, and BSCVA, confirming that the two eyelid thermal pulsation devices were equally safe. Corneal staining was significantly increased immediately after treatment in both groups, likely due to the contact of both instruments with the eye and adnexa. Importantly, however, no epithelial abrasions were reported following the use of either device.
Both corneal staining and BSCVA, defined as secondary safety outcomes, improved significantly following treatment. These improvements are further evidence of the effectiveness of these procedures and reflect improvements to the ocular surface. One possible explanation for these improvements is that patients with hyposecretory MGD likely have gland blockage or, in some cases, altered meibum composition, preventing the ease of meibum secretion from the meibomian gland ducts.30 These patients can experience tear hyperosmolarity due to a poor protective lipid layer and can present with corneal staining due to ocular surface desiccation and inflammation and epithelial cell damage.31 Eyelid heat therapy is designed to melt the meibum, thereby increasing availability on the lid margin. The lipids are likely re-incorporated into the tear film, reducing the rate of aqueous evaporation, thereby decreasing tear osmolarity and restoring homeostasis to the tear film. Enhanced lubrication from improved aqueous retention leads to epithelial cell regeneration, reducing or eliminating corneal epithelial staining and improving optical quality.
In summary, this clinical evaluation demonstrated that the iLUX MGD Treatment System is substantially equivalent to the LipiFlow Thermal Pulsation System in both efficacy and safety.
Pain and Discomfort
Post-treatment pain and discomfort scores were significantly lower than baseline in both groups but did not differ between groups. In contrast, pain and discomfort scores assessed immediately after treatment were lower in the LipiFlow group, but the differences were not statistically significant. At week 4, the iLUX group showed significantly greater improvements in discomfort score and greater improvements in pain score, although the latter was not significant. The transiently higher pain and discomfort scores in the iLUX group during the procedure may have been due to the ability of clinicians to apply greater manual compression force for gland evacuation with the iLUX than with the Lipiflow. The LipiFlow system applies pressure through an inflatable air bladder resting atop the closed eyelids, accounting for the slightly greater comfort, as well as the smaller treatment-related improvements in discomfort at week 4.
Several previous studies have assessed the effects of LipiFlow treatment on MGD signs and symptoms.18,20,32–35 Figure 6 shows that improvement in MGS, TBUT and OSDI in the present study was in broad agreement with the results of six previous studies of the LipiFlow device.18,20,32–35 Differences in pre-treatment values across studies reflect differences in eligibility criteria and patient populations. It should be noted that the plots are presented to demonstrate baseline variations and reported changes with treatment; however, the relationship between baseline and 4 weeks for all measurements cannot be assumed to be linear.
Study Limitations
One limitation of the present study was that meibography was not performed to assess the baseline severity of meibomian gland atrophy and changes at any time point over 4 weeks. Another clinical test that may have been beneficial is measurement of non-invasive tear breakup time. Although fluorescein tear breakup time was measured, its results can vary widely, as fluorescence dimming observed at both high and low fluorescein concentrations can lead to clinical misinterpretation.36 The frequency of use of artificial tears, warm compresses, and eyelid hygiene at home were not monitored. Although ocular lubricants are not likely to alter meibomian gland score, the primary study outcome, the regular use of warm compresses and lid hygiene can affect meibomian gland score. Randomization, however, likely resulted in random distribution of frequent users of either or both therapies between the two study groups, and the finding of a lack of difference between study arms should still be valid. Another limitation was the lack of masking for endpoints other than MGS; this was especially important when assessing OSDI. However, the OSDI is a subjective outcome evaluated by each participant and should therefore be unaffected by examiner bias. An additional limitation was the relatively short follow-up period. Follow-up periods in previous studies of Lipiflow have ranged from 2 months10,17,35 to 3 years.37 The two devices showed equivalent outcomes at 4 weeks, but longer-term studies are required to understand the optimal treatment frequency with the iLUX and how it compares with the Lipiflow. Although patient condition is assumed to be constant over time, day-to-day exacerbations and seasonal differences occur.38 Measures and symptoms of dry eye disease, however, do not change much over a short period of time, as supported by our findings at 2 and 4 weeks.
Summary and Conclusions
The iLUX MGD Treatment System is a novel eyelid thermal pulsation device that effectively treats MGD. It can safely reach the appropriate melting temperature of meibum while simultaneously compressing and evacuating the meibomian glands. The iLUX System allows direct visualization of any cloudy or inspissated meibum while also permitting greater compression and/or longer heating time, if needed, depending on the level of obstruction or atrophy encountered in each region of the eyelid. The clinical utility and design of the iLUX system may lead to positive patient-reported outcomes, as demonstrated by the large effect size of symptomatic improvement at 4 weeks.
In conclusion, the present study showed that the iLUX MGD Treatment System provides outcomes clinically equivalent to those of the LipiFlow Thermal Pulsation System over 4 weeks in the treatment of dry eye associated with meibomian gland dysfunction.
Data Sharing Statement
Additional information can be obtained by contacting the research staff of this study; individual patient data, however, will not be shared.
Acknowledgments
The following investigators and clinical sites participated in the clinical trial: Marc Bloomenstein, Schwartz Laser Eye Center, Scottsdale, AZ; Jon Dishler, Dishler Laser Institute, Greenwood Village, CO; John Hovanesian, Harvard Eye Associates, Laguna Hills, CA; Jay Pepose, Pepose Vision Institute, Chesterfield, MO; John Schachet, Eyecare Consultants – Vision Source, Englewood, CO; David Schanzlin, Gordon Schanzlin New Vision Institute, San Diego, CA; William Schiff, Barnet-Dulany-Perkins Eye Center, Phoenix, AZ; Joseph Tauber, Tauber Eye Center, Kansas City, MO. Justin Kwan, OD, provided input on an earlier draft of the manuscript. Editorial support was provided by BelMed Professional Resources, with funding from Alcon.
Funding
The study was funded by Alcon Research, LLC.
Disclosure
J.O. has received honoraria or consulting fees from Science Based Health, AMO, Alcon. AcuFocus, and Tear Film Innovations. M.B. is on the speakers’ panel and is a consultant for Alcon, Allergan, Bausch+Lomb, Eyevance, Johnson & Johnson, Novartis, Reichert, OcuSoft, and Bruder. J.H. is an equity holder in Tear Film Innovations. He also reports personal fees from Alcon and JNJ, during the conduct of the study. M.A.B. is a consultant for and received personal fees from Alcon, CooperVision, Essilor, Genentech, jCyte, Johnson & Johnson Vision, and Novartis. The authors report no other conflicts of interest in this work.
References
1. Schaumberg DA, Nichols JJ, Papas EB, Tong L, Uchino M, Nichols KK. The international workshop on meibomian gland dysfunction: report of the subcommittee on the epidemiology of, and associated risk factors for, MGD. Invest Ophthalmol Vis Sci. 2011;52:1994–2005. doi:10.1167/iovs.10-6997e
2. Gupta PK, Stevens MN, Kashyap N, Priestley Y. Prevalence of meibomian gland atrophy in a pediatric population. Cornea. 2018;37:426–430. doi:10.1097/ICO.0000000000001476
3. Arita R, Fukuoka S, Morishige N. Meibomian gland dysfunction and contact lens discomfort. Eye Contact Lens. 2017;43:17–22. doi:10.1097/ICL.0000000000000351
4. Blackie CA, Korb DR, Knop E, Bedi R, Knop N, Holland EJ. Nonobvious obstructive meibomian gland dysfunction. Cornea. 2010;29:1333–1345. doi:10.1097/ICO.0b013e3181d4f366
5. Geerling G, Tauber J, Baudouin C, et al. The international workshop on meibomian gland dysfunction: report of the subcommittee on management and treatment of meibomian gland dysfunction. Invest Ophthalmol Vis Sci. 2011;52:2050–2064. doi:10.1167/iovs.10-6997g
6. Fogt JS, Kowalski MJ, King-Smith PE, et al. Tear lipid layer thickness with eye drops in meibomian gland dysfunction. Clin Ophthalmol. 2016;10:2237–2243. doi:10.2147/OPTH
7. Korb DR, Scaffidi RC, Greiner JV, et al. The effect of two novel lubricant eye drops on tear film lipid layer thickness in subjects with dry eye symptoms. Optom Vis Sci. 2005;82:594–601. doi:10.1097/01.opx.0000171818.01353.8c
8. Sakassegawa-Naves FE, Ricci HMM, Moscovici BK, et al. Tacrolimus ointment for refractory posterior blepharitis. Curr Eye Res. 2017;42:1440–1444. doi:10.1080/02713683.2017.1339805
9. Korb DR, Blackie CA. Debridement-scaling: a new procedure that increases meibomian gland function and reduces dry eye symptoms. Cornea. 2013;32:1554–1557. doi:10.1097/ICO.0b013e3182a73843
10. Blackie CA, Coleman CA, Holland EJ. The sustained effect (12 months) of a single-dose vectored thermal pulsation procedure for meibomian gland dysfunction and evaporative dry eye. Clin Ophthalmol. 2016;10:1385–1396. doi:10.2147/OPTH
11. Seo KY, Kang SM, Ha DY, Chin HS, Jung JW. Long-term effects of intense pulsed light treatment on the ocular surface in patients with rosacea-associated meibomian gland dysfunction. Cont Lens Anterior Eye. 2018;41:430–435. doi:10.1016/j.clae.2018.06.002
12. Ong BL, Larke JR. Meibomian gland dysfunction: some clinical, biochemical and physical observations. Ophthalmic Physiol Opt. 1990;10:144–148. doi:10.1111/opo.1990.10.issue-2
13. Terada O, Chiba K, Senoo T, Obara Y. [Ocular surface temperature of meibomia gland dysfunction patients and the melting point of meibomian gland secretions]. Nihon Ganka Gakkai Zasshi. 2004;108:690–693.
14. Bitton E, Lacroix Z, Leger S. In-vivo heat retention comparison of eyelid warming masks. Cont Lens Anterior Eye. 2016;39:311–315. doi:10.1016/j.clae.2016.04.002
15. Murakami DK, Blackie CA, Korb DR. All warm compresses are not equally efficacious. Optom Vis Sci. 2015;92:e327–e333. doi:10.1097/OPX.0000000000000675
16. Miller KL, Walt JG, Mink DR, et al. Minimal clinically important difference for the ocular surface disease index. Arch Ophthalmol. 2010;128:94–101. doi:10.1001/archophthalmol.2009.356
17. Greiner JV. Long-term (12-month) improvement in meibomian gland function and reduced dry eye symptoms with a single thermal pulsation treatment. Clin Exp Ophthalmol. 2013;41:524–530. doi:10.1111/ceo.2013.41.issue-6
18. Greiner JV. A single LipiFlow(R) thermal pulsation system treatment improves meibomian gland function and reduces dry eye symptoms for 9 months. Curr Eye Res. 2012;37:272–278. doi:10.3109/02713683.2011.631721
19. Blackie CA, Carlson AN, Korb DR. Treatment for meibomian gland dysfunction and dry eye symptoms with a single-dose vectored thermal pulsation: a review. Curr Opin Ophthalmol. 2015;26:306–313. doi:10.1097/ICU.0000000000000165
20. Lane SS, DuBiner HB, Epstein RJ, et al. A new system, the LipiFlow, for the treatment of meibomian gland dysfunction. Cornea. 2012;31:396–404. doi:10.1097/ICO.0b013e318239aaea
21. Tomlinson A, Bron AJ, Korb DR, et al. The international workshop on meibomian gland dysfunction: report of the diagnosis subcommittee. Invest Ophthalmol Vis Sci. 2011;52:2006–2049. doi:10.1167/iovs.10-6997f
22. Walt JG, Rowe MM, Stern KL. Evaluating the functional impact of dry eye: the ocular surface disease index. Drug Inf J. 1997; 31(1436): [abstract].
23. Schiffman RM, Christianson MD, Jacobsen G, Hirsch JD, Reis BL. Reliability and validity of the ocular surface disease index. Arch Ophthalmol. 2000;118:615–621. doi:10.1001/archopht.118.5.615
24. Arita R, Itoh K, Inoue K, Amano S. Noncontact infrared meibography to document age-related changes of the meibomian glands in a normal population. Ophthalmology. 2008;115:911–915. doi:10.1016/j.ophtha.2007.06.031
25. Lemp MA. Report of the National Eye Institute/industry workshop on clinical trials in dry eyes. CLAO J. 1995;21:221–232.
26. Asbell PA, Maguire MG, Pistilli M, et al.; Dry Eye Assessment and Management Study Research Group. n-3 fatty acid supplementation for the treatment of dry eye disease. N Engl J Med. 2018;378:1681–1690. doi: 10.1056/NEJMoa1709691.
27. Stevenson D, Tauber J, Reis BL. Efficacy and safety of cyclosporin A ophthalmic emulsion in the treatment of moderate-to-severe dry eye disease: a dose-ranging, randomized trial. The Cyclosporin A Phase 2 Study Group. Ophthalmology. 2000;107:967–974. doi:10.1016/S0161-6420(00)00035-X
28. Semba CP, Torkildsen GL, Lonsdale JD, et al. A phase 2 randomized, double-masked, placebo-controlled study of a novel integrin antagonist (SAR 1118) for the treatment of dry eye. Am J Ophthalmol. 2012;153:1050–1060. doi:10.1016/j.ajo.2011.11.003
29. Sheppard JD, Torkildsen GL, Lonsdale JD, et al. OPUS-1 Study Group. Lifitegrast ophthalmic solution 5.0% for treatment of dry eye disease: results of the OPUS-1 Phase 3 study. Ophthalmology. 2014;121:475–483. doi:10.1016/j.ophtha.2013.09.015
30. Nelson JD, Shimazaki J, Benitez-del-Castillo JM, et al. The international workshop on meibomian gland dysfunction: report of the definition and classification subcommittee. Invest Ophthalmol Vis Sci. 2011;52:1930–1937. doi:10.1167/iovs.10-6997b
31. Bron AJ, de Paiva CS, Chauhan SK, et al. TFOS DEWS II pathophysiology report. Ocul Surf. 2017;15:438–510. doi:10.1016/j.jtos.2017.05.011
32. Finis D, Hayajneh J, Konig C, Borrelli M, Schrader S, Geerling G. Evaluation of an automated thermodynamic treatment (LipiFlow(R)) system for meibomian gland dysfunction: a prospective, randomized, observer-masked trial. Ocul Surf. 2014;12:146–154. doi:10.1016/j.jtos.2013.12.001
33. Finis D, Konig C, Hayajneh J, Borrelli M, Schrader S, Geerling G. Six-month effects of a thermodynamic treatment for MGD and implications of meibomian gland atrophy. Cornea. 2014;33:1265–1270. doi:10.1097/ICO.0000000000000273
34. Friedland BR, Fleming CP, Blackie CA, Korb DR. A novel thermodynamic treatment for meibomian gland dysfunction. Curr Eye Res. 2011;36:79–87. doi:10.3109/02713683.2010.509529
35. Satjawatcharaphong P, Ge S, Lin MC. Clinical outcomes associated with thermal pulsation system treatment. Optom Vis Sci. 2015;92:e334–e341. doi:10.1097/OPX.0000000000000670
36. King-Smith PE, Ramamoorthy P, Braun RJ, Nichols JJ. Tear film images and breakup analyzed using fluorescent quenching. Invest Ophthalmol Vis Sci. 2013;54:6003–6011. doi:10.1167/iovs.13-12628
37. Greiner JV. Long-term (3 year) effects of a single thermal pulsation system treatment on meibomian gland function and dry eye symptoms. Eye Contact Lens. 2016;42:99–107. doi:10.1097/ICL.0000000000000166
38. Ayaki M, Kawashima M, Uchino M, Tsubota K, Negishi K. Possible association between subtypes of dry eye disease and seasonal variation. Clin Ophthalmol. 2017;11:1769–1775. doi:10.2147/OPTH
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.