Back to Journals » Clinical Interventions in Aging » Volume 15
Comparison of a Novel Muscle Training Device with Conventional Rehabilitation Training in Motor Dysfunction of Lower Limb Patients: A Pilot Study
Authors Cai XY, Lin D, Xiao Z, Zhang D, Lin Y, Chen H, Xu Y, Zhou Y
Received 14 August 2020
Accepted for publication 2 November 2020
Published 18 November 2020 Volume 2020:15 Pages 2209—2218
DOI https://doi.org/10.2147/CIA.S277118
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Zhi-Ying Wu
Xin-ying Cai,1 Dong-qi Lin,2 Zhi-zhen Xiao,3 Dan-dan Zhang,3 Ying Lin,3 Han-yu Chen,4 Yan-xing Xu,3 Yu-hua Zhou3
1Clinical Medical Research Center, Shantou Central Hospital, Affiliated Shantou Hospital of Sun Yat-Sen University, Shantou, Guangdong, People’s Republic of China; 2Department of Cardiothoracic Surgery, The Second Affiliated Hospital of Shantou University Medical College, Shantou, Guangdong, People’s Republic of China; 3Nursing Department, Shantou Central Hospital, Affiliated Shantou Hospital of Sun Yat-Sen University, Shantou, Guangdong, People’s Republic of China; 4Rehabilitation Department, Shantou Central Hospital, Affiliated Shantou Hospital of Sun Yat-Sen University, Shantou, Guangdong, People’s Republic of China
Correspondence: Yu-hua Zhou
Nursing Department, Shantou Central Hospital, Wai-ma Road 114, Shantou City, Guangdong Province, People’s Republic of China
Tel +86 0754-88903584
Fax +86 0754-88548117
Email [email protected]
Dong-qi Lin
Department of Cardiothoracic Surgery, The Second Affiliated Hospital of Shantou University Medical College, Shantou, Guangdong, People’s Republic of China
Tel +86 0754-88915647
Email [email protected]
Background: Postoperative functional training for fracture or osteoarthritis is mainly focused on functional self-exercise, which aims to recover the function of the lower limbs.
Purpose: To compare the function and life quality recovery in patients with fracture or arthritis treated with novel muscle training device (NMT) or conventional rehabilitation training (CRT) following surgery.
Patients and Methods: A total of 32 fracture patients were randomly divided into the NMT or the CRT groups. The evaluation was performed on the first and 7th day after surgery. The outcome measurements included the incidence of foot drop, Deep Vein Thrombosis and pressure ulcers, Hospital for Special Surgery knee score (HSS scores), pain scores for the Visual Analogue Scale (Pain scores for VAS), Zung self-rating anxiety scale (SAS), Pittsburgh sleep quality index (PSQI) and the Barthel Index score.
Results: The comparison of the change scores between the two groups indicated significant differences on day 7 following surgery in the Barthel Index score (P< 0.01). The Pain scores for VAS between the two groups indicated a significant difference (P< 0.05, U=20.0). The HSS scores between the two groups indicated a significant difference (P< 0.05, U=19.0). The HSS scores exhibited a highly significant difference in the NMT group (P< 0.01). The Mann–Whitney test was used to analyze the various components of the HSS scores. The comparison of the change scores on the function between the two groups indicated a significant difference (P< 0.05). The Range of Motion difference between groups exhibited highly significant differences (P< 0.01).
Conclusion: The novel muscle training device positively influenced the decrease in pain score, which resulted in a range increase of knee joint movement and a significant overall improvement in motion.
Keywords: orthopedics, fracture, middle-aged and elderly, function exercise
Introduction
The aging population is a high-risk group that is prone to develop several health conditions and disorders.1 According to a recent survey, the aging population is at high risk of developing fractures notably at the lower limbs. The fractures are usually caused by osteoporosis and poor ADL (activities of daily living).2 The hip and knee surgery, lower limb fracture, arthroscopic surgery, lower limb arthritis and prolonged stay in bed may lead to a variety of nursing problems, such as foot drop and venous thrombosis. Therefore, it is of great significance to provide early rehabilitation training for patients with lower limb dyspraxia.3,4
Several studies have reported a limited number of factors, such as pain, anxiety and low life quality that are caused by surgery associated with functional recovery.5,6 Elderly patients are often accompanied by hypertension, osteoporosis and other health problems, which lead to slow wound healing following surgery. A prolonged period of staying in bed and keeping motionless following surgery will cause loss of muscle tone, limited range of movement, pressure sores, constipation and other skin and urinary disorders.7,8 Ceroni et al reported significant differences in teenagers with low limb fracture on the average muscle stone on both sides of the lower limbs.9 A descriptive cohort study examined the need of physical therapy in patients who had undergone fracture surgery. The results indicated significant differences in the independence of patients undergoing individualized physical therapy compared with patients who had not been treated at the time of discharge evaluation.10 Therefore, it is essential for the patients with lower limb fracture and motor dysfunction to exercise early for rehabilitation. Host et al performed a study on rehabilitation exercise training following hip joint surgery in the elderly. Rehabilitation training in a supervised environment with appropriate time and strength following hip joint surgery can promote the physical recovery and muscle strength.11
Modern clinical nurses increasingly rely on innovative technologies to evaluate and treat patients.12,13 The development of nursing patents has significantly promoted the process of nursing treatment. Moreover, the nursing patent technology has played a vital role in the clinic. Until now, a limited number of studies have been conducted regarding the evaluation of patents used in clinical applications. A patent for a novel muscle training device was applied in 2014, which aimed at promoting the strength of lower limbs and preventing the weakness of lower limbs and the foot drop (Figure 1). Therefore, we conducted a pilot study to compare the short-term rehabilitation of the novel muscle training device (NMT) group and the conventional rehabilitation training (CRT) group. The present study aimed to provide a reference for subsequent randomized clinical trials.
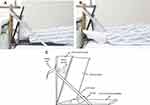 |
Figure 1 Novel muscle training device. |
Patients and Methods
Study Design
A pilot study with two study groups was performed in an orthopaedic ward in one college affiliated hospital. The present study was approved by the Ethics Committee of Shantou Central Hospital (2019-Ke-Yan (137)). This study has complied with the Declaration of Helsinki. In addition, this study was a pilot study and not a formal clinical study. Additional trials can be extracted from the Chinese Clinical Trial Registry (ChiCTR2000029979).
Participants
The following inclusion criteria were used: hospitalized patients aged 50–85, presence of hip knee gonarthrosis or knee injury or femoral neck, intertrochanteric surgery or surgery caused by subtrochanteric fracture and necrosis of the femoral head or unilateral and bilateral motor dysfunction of lower limbs following surgery. The enrolled patients were hospitalized to regain normal function with regard to flexion, extension and varus of the ankle joint. The exclusion criteria were as follows: patients with ankle arthropathy or ankle surgery. In addition, patients with consciousness disorders including coma and dementia, pregnant and lactating women and those who refused to participate in the study were also excluded.14 The patients were assigned to either NMT or CRT groups following the principles of normalization, fairness and randomization.
The demographic and clinical characteristics of these two groups were similar (Table 1).
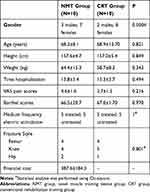 |
Table 1 Personal Characteristics of the Study Participants |
Allocation
(1) Following completion of baseline evaluation, the random sequence was generated by the statistician. The premier designer decided the type of random number allocation for the NMT or CRT groups. (2) The premier designer would compile a list of distribution sequences, which was divided into 3 columns. The first column included the sequence number. The second column was the random number. The third column was the group identification. (3) The random number was obtained by the random number generator. The sequence number corresponding to each object was strictly matched with the random number generated by the sequence. (4) The group was determined according to the random number. The large number group was defined as group A, while the small number group was defined as group B. The same sample size was used by both groups. The trial was supervised and guided by the premier designer and statistician.
The open study design was adopted rather than the blind method. It was impractical to blind the clinical nurses and rehabilitation physicians conducting the intervention study considering the operation of the device. It was notable that the blind method could not be adopted after the patients were allocated.
The clinical nurses who did not participate in the trial were responsible for recruiting patients according to the inclusion criteria. The sequence numbers were assigned on the basis of the time of attendance. The sequence numbers were recorded and kept by the clinical nurses. The measurement outcomes were assessed by the clinical nurses and the rehabilitation physicians who did not participate in the allocation.
Intervention
Each patient read and signed an informed consent form at the pretrial period. Moreover, the patients received the standardized rehabilitation treatment provided in our rehabilitation department and were closely supervised by the physician of the corresponding rehabilitation department. The content of standardized rehabilitation treatment was not different between the groups. The patients in the NMT and CRT groups required postoperative rehabilitative exercise, such as quadriceps femoris isometric contraction exercise and ankle joint flexion and extension exercise with the help of doctors and nurses in the orthopedics department. In addition, the NMT group applied for a new patent, which was approved by the Intellectual Property Office of the People’s Republic of China on May 23, 2014. The following certificate was obtained for this method: Certificate No. 3,953,389. The present study was conducted from February 2020 to August 2020. All patients of the NMT group received treatment for at least 20 min per day twice in the morning and in the afternoon by the device in addition to the conventional rehabilitation treatment. The patients in the CRT received only 20 min of conventional rehabilitation treatment from the physical therapist every day. This device included a vertical and a horizontal base plate that was connected to form an included angle. A training pedal hinged to the vertical base plate was provided in the included angle and a return spring was provided between the training pedal and the vertical base plate. A fixing rope was arranged on the back of the vertical base plate and a bump for limiting the rear heel was arranged on the horizontal base plate. The bumps were made of sponge to improve comfort and prevent friction (Figure 1). The training device was installed by the nurse in the bed. The patients underwent muscle strength training under the guidance of rehabilitation physicians and orthopaedic nurses. All the training was conducted under optimal conditions and the patient wellbeing was ensured. In case the patient was tired or unwell, he could pause for a while to recover and continue to complete the strength training exercise. The whole training process was supervised and guided by the physicians and nurses. The lower extremity condition was evaluated and the results were recorded following completion of the training. The patient could train the muscle strength of the lower extremities and promote the recovery of the muscle tone of the thigh femoris, calf gastrocnemius and soleus muscles through the device without getting out of bed. Postoperative patients were allowed to start muscle training on a novel muscle training device following evaluation on the first day postoperatively. The rehabilitation physicians and orthopedic nurses guided and supervised the patients to carry out rehabilitative exercises.
The patients were free to use the device without assistance during rehabilitation training. The device was not only used for training under supervision, but was also provided to patients in the NMT group in the ward during the day.
Outcome Measurement
On admission, the demographic and clinical data were collected, which included age, gender, weight, height, fracture location, type of surgery, and underlying disease. The outcome measurements were assessed on admission (prior to intervention) and on the day after one week of intervention.
1.The Hospital for Special Surgery (HSS) knee score15 was proposed by the American Hospital for Special Surgery in 1976 with a total score of 100 points. It was used to evaluate the movements of patella joint and femoral tibial joint following surgery.
2.The Visual Analogue Scale (VAS) comprised a straight line with a length of 100 mm and the scale used was as follows: a segment labelled 0 denoted “painless,” and 10 denoted “unbearable pain”.16 The leftmost and rightmost number represented “painless” and the strongest pain, respectively;17
3.The SAS anxiety scale (Zung self-rating anxiety scale (SAS))18 is a fairly simple clinical tool for analyzing the symptoms of the patients. It is suitable for adults with anxiety symptoms and it is applied widely for this purpose. In the present study, it was used to assess the psychological and emotional situation during hospitalization.
4. Pittsburgh sleep quality index (PSQI) is a scale proposed by Buysse et al in 1989 and aims to evaluate individual sleep quality.19 The present study evaluated the sleep quality of the patients using the PSQI scale during hospitalization.
5.The Barthel index (the Barthel index of ADL) was designed and formulated by the American doctor Barthel and Florence Mahoney in 1965.20,21 It is commonly used in American rehabilitation institutions. The Barthel index was used to assess the patient activities of daily living following surgery.
Conventional Rehabilitation Training After Lower Limb Fractures
The pelvic and acetabular fractures were assessed as follows: After the operation, the patients were instructed to perform quadricep isometric contraction and ankle joint training. The patients underwent early passive knee flexion and extension activities that could gradually change to initiative activities according to optimal conditions. The patients who exhibited successful recovery received hip joint activity training.
The knee, femoral intertrochanter, or femoral neck fracture were assessed as follows: After the surgery, the patient was instructed to carry out gradually early passive knee flexion and extension activities that would eventually change to active activities. Ankle joint activities mainly included dorsiflexion activities. Isometric contraction exercises of quadriceps were instructed for patients step by step in order to promote muscle strength recovery.
All evaluations and tests were performed with the patient’s consciousness and informed consent.
Statistical Analysis
All statistical analyses were conducted using the SPSS 21 software. Descriptive statistics were used to describe the study population and measured parameters. Since the muscle training device of this study was under intellectual protection of a patent, no relevant reports could be found on this method. The differences in the continuous variables were compared between the groups using the Mann-U Whitney test. The differences in the categorical variables were assessed with the Fisher’s exact test. The within-group measured outcomes were compared prior to and following the intervention using the Wilcoxon signed rank test. The statistical significance was denoted at P<0.05 and P<0.01.
Results
A total of 37 patients who underwent lower limb fracture or motor dysfunction were screened for the study, of which 32 were eligible. A total of 16 out of the 32 patients were assigned to the NMT group, whereas 16 were assigned to the CRT group. A total of 6 patients in the NMT group and 6 patients in the CRT group dropped out during the study. One person in the CRT group was excluded from the study due to discharge from the hospital within 7 days following surgery. One person withdrew from the study due to his condition, whereas one person was forced to withdraw from the study. The other three patients were excluded for personal reasons. Three patients from the NMT group were discharged from the hospital within 7 days following surgery and the other three persons chose to quit from the study due to financial reasons. The flow of the pilot study is shown in Figure 2. Following evaluation by the rehabilitation physician and the orthopaedic nurses on the first day after surgery, the NMT group was treated with the muscle training device and the conventional rehabilitation training, while the CRT group received only conventional rehabilitation training.
 |
Figure 2 Flow of the pilot study. |
A total of 20 patients were divided into the NMT (3 males, 7 females) and CRT groups (2 males, 8 females). Both groups included more females than males, which was similar to previously reported findings.22 The two groups were similar in terms of gender, age, height, weight, time of hospitalization, pain scores by VAS and Barthel scores (Table 1). It was worth noting that during the postoperative recovery period, 5 persons (50%) of the two groups received intermediate frequency electrical stimulation treatment by the rehabilitation physicians. No significant differences were noted in the demographic or baseline measures between groups. In addition, one patient in the CRT group was diagnosed with DVT (Deep Vein Thrombosis) on admission. No additional DVT cases were found in the two groups during the study. Foot drop and pressure ulcers did not occur in both groups during the study period (Table 2).
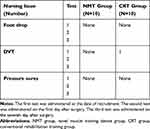 |
Table 2 The Incidence of Postoperative Complications |
The HSS and VAS pain scores of the two groups were significantly improved on day 7 following surgery compared to those noted in the CRT group. No significant differences were noted in the SAS, PSQI and Barthel scores between the NMT and the CRT groups (Table 3).
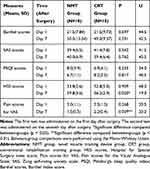 |
Table 3 Mean and Standard Deviation Between-Groups in the CRT Group and NMT Group |
The NMT group indicated significant improvement in the HSS scores of the 7-day evaluations compared with the evaluation of the first day following surgery (Table 2). Both Barthel and pain scores were improved in each group following the intervention. The difference in the Barthel scores of both groups was statistically significant. Although the results of the pain scores showed improvement following VAS assessment, the NMT group exhibited significant differences compared with the CRT group (Table 4).
 |
Table 4 Mean and Quartile Within-Groups in the CRT Group and NMT Group |
The improvement in the HSS scores was presented as box plots for each of the 7-day evaluations corresponding to each group (Figure 3). The evaluation on the function and ROM (Range of Motion) of the NMT group indicated significant improvement compared with that of the CRT group.
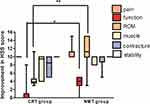 |
Figure 3 The improvement of components presented as box plots at each of the evaluations for the NMT group and CRT group. |
Discussion
The present study compared the occurrence of the CRT and the NMT groups on postoperative complications, such as foot drop and venous thrombosis. In addition, psychological anxiety, sleep quality, activities of daily living, pain perception and knee joint movement were assessed in patients with two different interventions. We found that pain perception and knee joint movement were improved in the NMT group compared with the CRT group. Although several studies have been conducted on rehabilitation training with lower limb fracture, the present study exhibited novel information, specifically, with regard to the clinical trial report of the product patent application. The present study provided important information for the evaluation of the clinical application of the patent. In addition, as a pilot study of clinical trials, the present study followed the requirements of clinical trial implementation including patient recruitment, allocation, intervention and evaluation of parameters to ensure its feasibility. Therefore, the present data are unique in terms of assessing objective quantifications, as well as with regard to the novelty of the patent. Both groups indicated an improvement in the outcomes of the Barthel and pain scores as demonstrated by VAS, with significant differences noted on HSS scores in the NMT group. The results suggested that rehabilitation therapy treated with the novel muscle training device combined with conventional rehabilitation training for patients with lower limb fracture or motor dysfunction was better than single conventional rehabilitation training. No foot drop, pressure sores or DVT were noted in both groups within 7 days following surgery. Only one patient was admitted to hospital with native DVT. The muscle training device used in the NMT group aimed to prevent the occurrence of foot drop, DVT and pressure ulcers caused by long-term bed rest and lack of physical exercise following surgery. According to previous studies, age is an important risk factor for lower limb DVT in patients with fracture.23 The blood in the venous sinuses of the leg muscles requires the action of the muscle pump to effectively achieve centripetal return. Venous insufficiency of the lower limbs or partial loss of the function of the venous pump requires effective lower limb exercise to improve venous return.24 A previous study has found that early ankle activity can reduce the risk of postoperative thromboembolism.25 The muscle training device used in the present study was similar to the ankle pump, which aimed to promote venous return of the lower limbs, reduce blood stasis and improve blood circulation and edema. However, no significant differences were noted in the incidence of DVT between the different groups. This may be attributed to the small sample size and short research process, which may also explain why the foot drop and pressure sores were not noted in the two groups. It is necessary to increase the sample size and extend the time period of the study to confirm these results in the next trial.
No significant differences were noted in the SAS, PSQI and Barthel scores at the 7-day period following surgery, which was different from previously reported findings19 (Table 3). Sleep is a cyclical process, which effectively improves the termination of the physiological awakening and the fatigue state of various tissues and organs.26 Disease has a negative effect on human physiological function, which leads to the decrease in the sleep quality of patients. The decrease in the sleep quality will cause the patient’s physical health to deteriorate further. In addition, it will also have a negative impact on the patient’s psychology, which makes patients prone to fatigue, anxiety and depression. As a result, it affects the treatment effect of the disease to reduce the quality of life and satisfaction.27 However, due to the short time of intervention, the improvement of the sleep quality and mental state is limited. Therefore, it is necessary to further extend the time of experimental intervention.
The changes in the HSS and pain scores were compared by VAS assessment between the different groups. Their scores indicated a significant difference in both groups. The HSS score of the NMT group was increased from 33.8±2.6 to 39.8±3.6 compared with that noted in the CRT group (increase of 32.8±5.0 to 36.23±2.9). The difference was statistically significant (Table 3). In addition, the pain following surgery was significantly relieved in the rehabilitation activities. Compared with the CRT group, the NMT group exhibited a significant difference in pain perception seven days following surgery. This finding supports our hypothesis, which suggests that the muscle training device combined with conventional rehabilitation training is more effective than rehabilitation training alone.
We conducted statistical analysis of within-group differences and found that the Barthel scores were significantly improved in both groups seven days after surgery (Table 4). The pain scores assessed by VAS in the NMT group were significantly improved than those in the CRT group (Table 4). The Barthel score in the NMT group did not improve compared with that in the CRT group, which indicated that this muscle training device did not exhibit advantages in daily living activities in a short time compared with the conventional rehabilitation training method. Pain is the most obvious stressor following fracture surgery. According to Vilmarsson, the sympathetic reflex caused by the painful stimulation after surgery leads to constriction of blood vessels and muscles, which results in insufficient blood supply to the incision and ultimately delays wound healing and increases the chance of infection.28 Johal et al demonstrated that 10–50% of patients with root bone fractures exhibited incision infections, nonunion of marginal flaps and necrosis.29 Therefore, pain relief for patients with lower limb fracture is of great significance for promoting wound healing and preventing infection. In addition, early postoperative rehabilitation exercises can aid the improvement of the blood and lymph circulation and reduce limb swelling and pain perception.30,31 Previously, Kronborg et al32 reported that it was feasible to initiate progressive knee straighter strength training for fractured limbs in acute wards, which could reduce force asymmetry between limbs without increasing hip pain. In the present study, the muscle training device was used to achieve muscle relaxation mainly through repeated contractions and relaxation. Concomitantly, it diverted the patient’s attention so that the body and mind were relaxed. Certain rehabilitation physicians and orthopedic nurses were present to provide fixed supervision and guidance exercise, which aimed to improve the mood of the patients with a sense of trust. This resulted in their willingness to carry out rehabilitation training. The regular guidance of the rehabilitation team could aid the patients understand the importance of rehabilitation exercise and assist them in learning additional rehabilitation knowledge so that they could participate in the early training more autonomously. A previous study has shown that the patient understanding of the importance of rehabilitation training may increase his/her compliance rate even when the medical staff is absent.33 In the present study, the patients in the NMT group used the remaining of the time to exercise autonomously in addition to the fixed time of supervised exercise time. This aided the reduction of the postoperative pain, which could in turn improve compliance with rehabilitation exercises. The two processes can interact with each other.
The results demonstrated that the HSS score in the NMT group was improved, while that of the CRT group indicated no significant differences compared with that noted at baseline (Table 4). The analysis on the components of the HSS scores indicated significant differences in function and ROM. Notably, ROM indicated significant improvement (P<0.01). Significant differences were not found in the parameters knee joint pain, muscle, contracture and stability between the two groups (Figure 3). It is believed that intense functional exercises require two weeks following hip and knee replacement, which results in skeletal muscle weakness.34 Recent studies have shown that early postoperative hip and knee joint exercises should be carried out with proper intensity. The muscle training device used in this study forced the muscles to move around the ankle joint by means of equipment exercise and gradually restored the muscle strength through the ankle flexion and dorsiflexion exercises. Moreover, it enhanced the lower limb circulation and lymph reflux. The active foot flexion and dorsiflexion exercises performed by the ankle joint strengthened the stability and coordination of the muscles and ligaments. Thereby, they increased the range of the knee joint and the recovery function of the lower limbs.35 The range of the knee joint and the strength of the surrounding muscles are increased through progressive resistance exercises and long-term continuous stretching of the joint muscle. These exercises can prevent contracture adhesion, maintain the range of joint motion, gradually improve the stability and prevent the formation of DVT in the lower limbs.
The limitations of the present study are the small sample size and short assessment period. In addition, the natural recovery process of each individual is independent of rehabilitation training. All patients were not followed up in this pilot study and the assessment of their effects can be further investigated in future clinical trials. There may be intra-day and inter-day deviations in the measurement of the parameters evaluated, which limits the consistency of the results. Finally, it was unsuitable to blind the participants due to the nature of the intervention.
Conclusion
The results of the present study indicated no significant statistical differences on multiple indices between the two groups examined. However, the data demonstrated that the novel muscle training device positively influenced the decrease of pain, reaching a range increase of knee joint movement, which could be further improved from the analysis of the differences noted in the HSS and VAS pain scores between the different groups.
Acknowledgments
The study was funded by the Nursing Department, Shantou Central Hospital, Affiliated Shantou Hospital of Sun Yat-sen University, Shantou.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Javaheri B, Carriero A, Wood M, et al. Transient peak-strain matching partially recovers the age-impaired mechanoadaptive cortical bone response. Sci Rep. 2018;8(1):6636. doi:10.1038/s41598-018-25084-6
2. Young KH, Yong-Chan H, Tae-Young K, et al. Healthcare costs of osteoporotic fracture in Korea: information from the national health insurance claims database, 2008–2011. J Bone Metabol. 2017;24(2):125–133. doi:10.11005/jbm.2017.24.2.125
3. Hofman M, Kolejewska A, Greven J, et al. Gait analysis and muscle weight analysis after lower extremity fractures in a small animal model. Gait Posture. 2020;77:207–213.
4. Selakovic I, Dubljanin-Raspopovic E, Markovic-Denic L, Marusic V, Tulic G. Can early assessment of hand grip strength in older hip fracture patients predict functional outcome? PLoS One. 2019;14(8):e0213223. doi:10.1371/journal.pone.0213223
5. A?Court J, Lees D, Harrison W, Ankers T, Reed MR. Pain and analgesia requirements with hip fracture surgery. Orthop Nurs. 2017;36(3):224–228. doi:10.1097/NOR.0000000000000347
6. Van Grootven B, Detroyer E, Devriendt E. Is preoperative state anxiety a risk factor for postoperative delirium among elderly hip fracture patients? Geriatr Gerontol Int. 2016;16(8):948–955. doi:10.1111/ggi.12581
7. Damiani C, Mangone M, Paoloni M, et al. Trade-offs with rehabilitation effectiveness (REs) and efficiency (REy) in a sample of Italian disabled persons in a in post-acuity rehabilitation unit. Ann Ig. 2020;32(4):327–335.
8. Seccia R, Boresta M, Fusco F, et al. Data of patients undergoing rehabilitation programs. Data Brief. 2020;30:105419. doi:10.1016/j.dib.2020.105419
9. Ceroni D, Martin XE, Farpour-Lambert NJ, Delhumeau C, Kaelin A. Assessment of muscular performance in teenagers after a lower extremity fracture. J Pediatr Orthop. 2010;30(8):807–812. doi:10.1097/BPO.0b013e3181fa7969
10. Gohy B, Ali E, Van den Bergh R, et al. Early physical and functional rehabilitation of trauma patients in the Médecins Sans Frontières trauma centre in Kunduz, Afghanistan: luxury or necessity? Int Health. 2016;8(6):381–389. doi:10.1093/inthealth/ihw039
11. Host H, Sinacore D, Bohnert K, Steger-May K, Brown M, Binder E. Training-induced strength and functional adaptations after hip fracture. Physical Therapy. 2007;87(3):292–303.
12. Masiero S, Litwocenko S, Agostini F. Rehabilitation in an Italian thermal setting: a new therapeutic strategy for patients with musculoskeletal disability-the results of an Italian survey. Int J Biometeorol. 2020;64(6):951–954. doi:10.1007/s00484-019-01765-3
13. Bernetti A, Mangone M, Alviti F, et al. Spa therapy and rehabilitation of musculoskeletal pathologies: a proposal for best practice in Italy. Int J Biometeorol. 2020;64(6):905–914. doi:10.1007/s00484-019-01731-z
14. Lo Torto F, Kaciulyte J, Marcasciano M, et al. Peroneus Brevis flap in Achilles tendon reconstruction. Clinical, radiological and functional analysis. Foot Ankle Surg. 2020;26(2):218–223. doi:10.1016/j.fas.2019.02.004
15. Harris WH. Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am. 1969;51(4):737–755. doi:10.2106/00004623-196951040-00012
16. Sheth T, Miranda OM, Johnson B. Assessment of patient satisfaction, functionality, and quality of life after ultrasound-guided knee intervention: a prospective study. Clin Rheumatol. 2020;101:1–6.
17. Santilli V, Mangone M, Paoloni M, Agostini F, Alviti F, Bernetti A. Comment on early efficacy of intra-articular HYADD® 4 (Hymovis®) injections for symptomatic knee osteoarthritis. Joints. 2018;6(2):131–132. doi:10.1055/s-0038-1660791
18. William WKZMD. A rating instrument for anxiety disorders. Psychosom. 1971;12(6):371–379. doi:10.1016/S0033-3182(71)71479-0
19. Buysse D, Reynolds C, Monk T, Berman S, Kupfer D. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213. doi:10.1016/0165-1781(89)90047-4
20. Bouwstra H, Smit E, Wattel E, et al. Measurement properties of the Barthel index in geriatric rehabilitation. J Am Med Dir Assoc. 2019;20(4):420–425.e421. doi:10.1016/j.jamda.2018.09.033
21. Marijke H-R, Helmi VH, Paul DV, Ellen F. Activities of daily living in older community-dwelling persons: a systematic review of psychometric properties of instruments. 2018.
22. Lowe G. Epidemiology of venous thromboembolism: the need for large (including prospective) studies and meta-analyses. J Thromb Haemost. 2012;10(10):2186–2188. doi:10.1111/j.1538-7836.2012.04882.x
23. Elsner A, Schiffer G, Jubel A, Koebke J, Andermahr J. The venous pump of the first metatarsophalangeal joint: clinical implications. Foot Ankle Int. 2007;28(8):902–909. doi:10.3113/FAI.2007.0902
24. Keene D, Williamson E, Bruce J, Willett K, Lamb S. Early ankle movement versus immobilization in the postoperative management of ankle fracture in adults: a systematic review and meta-analysis. J Orthop Sports Phys Ther. 2014;44(9):690–697. doi:10.2519/jospt.2014.5294
25. Paulsen MG, Dowsey MM, Castle D, Choong PFM. Preoperative psychological distress and functional outcome after knee replacement. ANZ J Surg. 2011;81(10):681–687. doi:10.1111/j.1445-2197.2010.05634.x
26. Baek Y, Jung K, Lee S. Effects of sleep restriction on subjective and physiological variables in middle-aged Korean adults: an intervention study. Sleep Med. 2020;70:60–65. doi:10.1016/j.sleep.2020.02.006
27. Park I, Oh SM, Lee KH, Kim S, Lee YJ. The moderating effect of sleep disturbance on the association of stress with impulsivity and depressed mood. Psychiatry Investig. 2020;17(3):243–248. doi:10.30773/pi.2019.0181
28. Minns Lowe C, Barker K, Dewey M, Sackley C. Effectiveness of physiotherapy exercise following hip arthroplasty for osteoarthritis: a systematic review of clinical trials. BMC Musculoskelet Disord. 2009;10:98. doi:10.1186/1471-2474-10-98
29. Johal K, Boulton C, Moran C. Hip fractures after falls in hospital: a retrospective observational cohort study. Injury. 2009;40(2):201–204.
30. Perez-Cruz P, Nguyen L, Rhondali W, et al. Attitudes and perceptions of patients, caregivers, and health care providers toward background music in patient care areas: an exploratory study. J Palliat Med. 2012;15(10):1130. doi:10.1089/jpm.2012.0152
31. Yang SD, Ning SH, Zhang LH, Zhang YZ, Ding WY, Yang DL. The effect of lower limb rehabilitation gymnastics on postoperative rehabilitation in elderly patients with femoral shaft fracture: a retrospective case-control study. Medicine. 2016.
32. Lise K, Thomas B, Henrik P, et al. Feasibility of progressive strength training implemented in the acute ward after hip fracture surgery. PLoS One. 2014;9(4):e93332. doi:10.1371/journal.pone.0093332
33. Walcott-Mcquigg JA, Zerwic JJ, Dan A, Kelley MA. An ecological approach to physical activity in African American women. Medscape Womens Health. 2001;6(6):3.
34. Fatoye F, Wright J, Yeowell G, Gebrye T. Clinical and cost-effectiveness of physiotherapy interventions following total hip replacement: a systematic review and meta-analysis. Rheumatol Int. 2020;40(9):1385–1398. doi:10.1007/s00296-020-04597-2
35. Inhuber S, Sollmann N, Schlaeger S, et al. Associations of thigh muscle fat infiltration with isometric strength measurements based on chemical shift encoding-based water-fat magnetic resonance imaging. Eur Radiol Exp. 2019;3(1):45. doi:10.1186/s41747-019-0123-4
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
