Back to Journals » Clinical Ophthalmology » Volume 13
Clinical Pattern And Visual Impairment Associated With Herpes Simplex Keratitis
Authors Shah A , Joshi P , Bhusal B , Subedi P
Received 12 June 2019
Accepted for publication 17 October 2019
Published 12 November 2019 Volume 2019:13 Pages 2211—2215
DOI https://doi.org/10.2147/OPTH.S219184
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Anica Shah, Purushottam Joshi, Bijaya Bhusal, Prabha Subedi
Department of Cornea, Mechi Eye Hospital, Birtamode, Nepal
Correspondence: Anica Shah
Department of Cornea, Mechi Eye Hospital, 9 Sainikmode, Nepal
Tel +97 798 0331 9327
Email [email protected]
Purpose: Herpes simplex keratitis (HSK) has varied presenting patterns, and is one of the leading causes of corneal scarring and subsequent visual disability. This study was carried out to determine the incidence and patterns of HSK presenting at a tertiary eye center in eastern Nepal and to assess the associated visual impairment.
Methods: This was a descriptive, cross-sectional study at a tertiary eye-care center that included 302 cases of clinically diagnosed HSK over a period of 1 year. Detailed ocular examination was done in all patients. Clinical manifestations and visual acuity at presentation and on subsequent visits in cases that followed up were recorded. Findings were noted in structured format and later assessed.
Results: Of 302 cases of HSK, 53 presented with epithelial keratitis, 156 with stromal keratitis without ulceration, 22 with stromal keratitis with ulceration, 66 with endothelitis, and five with neurotrophic ulcers. Presenting visual acuity in 108 patients (35.7%) was <3/60. Of 175 patients who followed up, 36 patients continued to have vision <3/60.
Conclusion: This study shows that HSK has diverse presentation and can cause significant vision impairment. Stromal keratitis without ulceration was the most common presentation in our study. In developing nations, due to higher incidence of fungal and bacterial keratitis, HSK is not studied much. Few epidemiological data are available on the subject, and since the disease is notorious for recurrence, long-term study is paramount to estimate the burden of visual morbidity caused by the disease.
Keywords: herpes simplex keratitis, viral keratitis, herpes simplex
Introduction
Herpes simplex virus (HSV) is known to be ubiquitous in humans. HSV is endemic worldwide.1 HSV latency is widely present, and it is estimated that at least 33% of the world's population has clinically evident recurrent HSV infections.2 HS keratitis (HSK) is primarily caused by HSV1 in >95% of the cases, and is a common ocular infection that can affect all the layers of cornea.3,4 Owing to its recurrent nature, it is capable of causing significant corneal scarring, and it happens to be one of the most important causes of corneal opacity leading to corneal blindness. Global incidence of HSK is roughly 1.5 million, including 40,000 new cases of severe monocular visual impairment or blindness each year.5 Though established as the most common infective cause of blindness in developed nations, due to the comparatively high prevalence of bacterial and fungal keratitis not much emphasis has been placed on studying HSK in developing countries. In the Indian subcontinent, studies available on HSK are few in number. The aim of this study was to document the epidemiology, clinical manifestations, and visual morbidity caused by HSK in eastern areas of Nepal and India. We also aimed to add information to the small pool of data available on the subject in the Indian subcontinent.
Methods
This was a hospital-based cross-sectional study carried out over 12 months — from January to December 2017 — at Mechi Eye Hospital (MEH), Birtamode, Nepal targeting all patients presenting with HSK to the hospital. Written informed consent was obtained from each patient or their guardian for pediatric cases. Ethical approval was obtained from the institutional review board, and the study was conducted adhering to the principles of the Declaration of Helsinki.
A total of 302 cases of clinically diagnosed HSK were included. Only cases presenting to the cornea clinic at MEH for the first time during January to December 2017) were included. MEH is one of the largest eye-care centers in eastern Nepal and provides services to populations from Nepal, eastern and northern India, Bangladesh, and Bhutan.
All patients underwent detailed ocular examination — visual acuity with Snellen chart, intraocular pressure measurement, and slit-lamp examination — by a cornea specialist. Forms with full demographic (age, sex, location) profiles of patient were filled. Visual acuity on presentation, other clinical findings in detail, and diagnosis were noted after clinical examination. Diagnosis of epithelial keratitis was made if the lesion comprised either dendritic ulcers (lesions with a branching, linear pattern with terminal bulbs), or geographic ulcers (broad ulcers with swollen, scalloped, or geographic epithelial borders). Stromal lesions were classified into two categories; stromal keratitis without ulceration, and stromal keratitis with epithelial involvement and ulceration (necrotizing keratitis). Stromal keratitis without ulceration included cases of immunostromal keratitis, which can manifest as focal, multiple, or diffuse stromal opacities often accompanied by edema, and cases of interstitial keratitis, which have accompanying blood vessels with stromal opacity. Endothelitis included cases of disciform keratitis, which comprises stromal edema in a disc shape with underlying keratic precipitates, and cases of keratouveitis, in which uveitis predominates with mutton-fat keratic precipitates.
Patients were treated according to disease entity. Cases of epithelial keratitis were treated with topical antivirals, whereas topical steroids and oral antivirals were used in cases of stromal keratitis. Topical steroids as mainstay, and oral antivirals as needed were used for cases of endothelitis. Each case was followed up to the last visit. Patients with any other form of keratitis were excluded from the study. Data were collected and analyzed with SPSS 15.
Results
The total number of cases presenting with HSK was 302. Patients’ mean age of presentation was 41.13±17.14 (5–81) years. The maximum number of patients belonged to the age-group 21–50 years, comprised 174 cases (56.6%, Table 1). Among the total number of cases, 230 were male and 72 were female. The male:female ratio was 3:1.
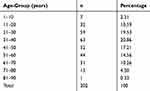 |
Table 1 Age Distribution Of Patients |
A majority of cases presented with chief complaints of diminution of vision, foreign-body sensation, redness, and watering, while 64% of epithelial keratitis cases presented with a chief complaint of foreign-body sensation. A majority — 70% with stromal keratitis with ulceration — presented with a chief complaint of diminution of vision. Pain/foreign-body sensation was the primary complaint in 72% of patients with stromal keratitis without ulceration. Cases with endothelitis had blurring of vision as their main complaint: 65%.
Patients presented with all possible manifestations of HSK. In sum, 53 (17.5%) patients presented with epithelial keratitis, which included 39 cases of dendritic ulcers and 14 cases of geographical ulcers. Most cases presented with stromal keratitis without ulceration (156 patients [51.6%]), while 22 (7.2%) presented with stromal keratitis with ulceration, and 66 (21.8%) had endothelitis, which comprised 48 cases of disciform keratitis and 18 cases of keratouveitis. Five cases (1.6%) presented with neurotrophic ulceration (Table 2).
 |
Table 2 Clinical Presentation Of Cases |
Presenting visual acuity of all cases was recorded: 85 cases (28.14%) had visual acuity of 6/6–6/18, 80 (26.49%) 6/24–6/60, 29 (9.5%) <6/60–3/60, and 108 (35.76%) <3/60 (Figure 1). Presenting visual acuity was also categorized for each type of presentation of HSK (Figure 2).
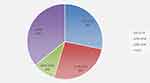 |
Figure 1 Presenting visual acuity. |
 |
Figure 2 Presenting visual acuity in different types of keratitis. |
Of 175 cases that followed to 6 weeks since the first visit, 86 (49.1%) had visual acuity of 6/6–6/18, 41 (23.4%) 6/24–6/60, 12 cases (6.8%) <6/60–3/60, and 36 (20.5%) <3/60 (Figure 3).
 |
Figure 3 Presenting visual acuity in follow-up cases. |
Discussion
Twenty-five centuries ago, Hippocrates used the word “herpes” to describe spreading cutaneous lesions.6 Herpetic infection is ubiquitous in humans, and nearly 100% of those older than 60 years harbor HSV in their trigeminal ganglia at autopsy.1 HSV is the most common infective cause of blindness in developed countries, with reported incidence of 5.9–20.7 episodes per 100,000 persons each year.7,8 A Rochester study reported a possible increase in the incidence of herpetic keratitis from 1950 to 1982 in the general population.7 However, according to Kabra et al, estimation of the true incidence of HSK and ocular morbidity may be difficult, as some episodes of infection may go unnoticed by the patient.9 Our descriptive cross-sectional study included a good number of cases over a duration of 1 year, which can lead to many insights into the epidemiology of HSK among a group of patients from the Indian subcontinent. However, like any other studies, it has its limitations too.
Our study included 302 patients. Patient’s mean age at presentation was 41.13±17.14 years, which is higher than any other similar study done on HSK. In the subcontinent, a study in India reported a mean age of 29.9±16.69 years for females and 32.09±15.79 years for males, and a similar study in Nepal reported a mean age of 36.63±16.94 years in a sample of 130 patients.9,10 Long-term studies of ocular HSV1 in the US and UK found the mean age for first occurrence to be 37.4 and 25 years, respectively.11–13 In our study, those aged 20–50 years comprised 57.6% of the total, which is similar to findings of various other studies.9,10,14,15 This signifies that HSK affects largely the productive age-group, and hence any significant scarring can have an adverse effect on this particular population. Kabra et al reported that 61.11% of patients with HSK were 20–50 years old.9 Similarly, Chaudhary et al reported that 46.91% of their cases were 16–45 years old.10 A study done in south India also reported 46.6% of those presenting with HSK belonging were aged 20–50 years.14 In our study, the male:female ratio was 3:1. Most similar studies done in the Indian subcontinent have shown a clear male preponderance for HSK.9,10,16 However, in a multicentric study done in France, Labetoulle et al reported a sex ratio of 1:1, and Darougar et al reported a ratio of 1.1:1.12,15 The reason for the male:female ratio being a little higher in our study might that the society from which these patients come is highly patriarchal, so much so that often health issues of females are neglected and their hospital visits are fewer in comparison to males. These findings from various studies suggest that HSK mostly presents in adult age-groups, with the majority of the cases presenting in the adult productive age-group with clear male preponderance.
In our study, 17.5% patients presented with epithelial keratitis, 51.6% with stromal keratitis without ulceration, 7.2% with stromal keratitis with ulceration, 21.8% with endothelitis, and 1.6% of with neurotrophic ulceration. This finding is very similar to Kabra et al, who reported 20% of cases presenting with dendritic and geographic ulcers and 53.64% with stromal keratitis.9 In both studies, stromal keratitis without ulceration was found to be the most common presenting pattern of HSK. However, other studies have reported epithelial keratitis to be the commonest presentation of HSK. Labetoulle et al mentioned that epithelial dendritic lesions represented the most frequent type of recurrent keratitis (56.3%), followed by herpes stromal keratitis (29.5%).15 A study comprising 238 patients reported 65% with epithelial keratitis, whereas 35% of cases had stromal keratitis.16 Chaudhary reported disciform keratitis to be the commonest presentation of HSK.10 However, studies done earlier showed a very low rate of stromal involvement. A 1989 study of 122 patients reported that 63% of cases had superficial corneal disease, only 6% stromal disease, and only 4% uveitis.11 In 1985, Darougar et al reported dendritic keratitis in 15% of cases and disciform keratitis in only 2%.12 This increase in incidence of stromal herpetic keratitis and keratouveitis points toward a shift in the natural history of the disease. Stromal keratitis and uveitis are immunomediated disorders, rather than just being infective entities, which indicates that there has been a rise in immunomediated diseases over time. The fewer cases of epithelial keratitis in our study might also have been because of the self-limiting nature of the disease, which prevents patients from seeking any medical attention for same.
The major presenting complaints in our study were diminution of vision, pain/foreign-body sensation, and redness. This finding is similar to almost all similar aforementioned studies;9,10,14 however, Darougar et al described blurring of vision as a less frequent symptom.12 This may have been due to the fact that that study reported a very lower number of stromal diseases and visual disturbance mostly being attributed to stromal involvement.
In our study, the visual acuity of all cases presenting was recorded: 54.63% had visual acuity >6/60 and 35.76% had visual acuity <3/60. Though of 175 cases that followed-up, only 36 had visual acuity <3/60, this made up 11.9% of the total. This indicates the serious visual impairment that HSK can cause in a significant proportion of the population. There have been few studies to concentrate on visual impairment associated with herpetic keratitis. In the Rochester study, only four eyes had visual acuity <20/100. This again may have been due to the fact that that study reported only 6% cases having stromal disease.11 In another study done in Nepal by Chaudhary et al, 8.4% of the patients had visual acuity <3/60.10 These data indicate how significant the visual morbidity caused by HSK is.
With its varied presentation and recurrent nature, HSK is capable of causing significant visual morbidity. From a review of various literature available on the subject, it can be concluded that the incidence of different presentations have been changing over the years. Unfortunately, in the Indian subcontinent, not many long-term studies have been done on the subject to help estimate the frequency and the impact of the condition. This study and its findings will help to add to the data pool available on the subject. Furthermore, the authors stress the need for long-term studies on the subject so that incidence and impact of the disease can be estimated accurately.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Liesegang TJ. Herpes simplex virus epidemiology and ocular importance. Cornea. 2001;20(1):1–3. doi:10.1097/00003226-200101000-00001
2. Umene K, Sakaoka H. Evolution of herpes simplex virus type 1 under herpesviral evolutionary processes. Arch Virol. 1999;144:637–656. doi:10.1007/s007050050533
3. Pavan-Langston D. Herpes simplex of the ocular anterior segment. Curr Clin Top Infect Dis. 2000;20:298–324.
4. Dutt S, Acharya M, Gour A, Sapra N, Chauhan L, Mathur U. Clinical efficacy of oral and topical acyclovir in herpes simplex virus stromal necrotizing keratitis. Indian J Ophthalmol. 2016;64(4):292. doi:10.4103/0301-4738.182940
5. Whitcher JP, Srinivasan M, Upadhayay MP. Corneal blindness; a global perspective. Bull Whorl Health Org. 2001;79:214–221.
6. Pepose JS, Leib DA, Stuart PM, Easty DL. Herpes simplex virus diseases anterior segment of the eye. In: Pepose JS, Holland GR, Wilhelmus KR, editors. Ocular Infection and Immunity. St Louis: Mosby-Year Book; 1996:905–932.
7. Liesegang TJ, Melton LJ, Daly PJ, Ilstrup DM. Epidemiology of ocular herpes simplex. Incidence in Rochester, Minn., 1950 through 1982. Arch Ophthalmol. 1989;107:1155–1159. doi:10.1001/archopht.1989.01070020221029
8. Norn MS. Dendritic (herpetic) keratitis, I: incidence-seasonal variations-recurrence rate-visual impairment-therapy. Acta Ophthalmol. 1970;48:91–107. doi:10.1111/j.1755-3768.1970.tb06577.x
9. Kabra A, Lalitha P, Mahadevan K, Prajna NV, Srinivasan M. Herpes simplex keratitis and visual impairment: a case series. Indian J Ophthalmol. 2006;54(1):23. doi:10.4103/0301-4738.21610
10. Chaudhary M. Clinical and epidemiological profile of herpetic eye disease in a tertiary eye care center. J Inst Med. 2017;40(2).
11. Liesegang TJ. Epidemiology of ocular herpes simplex: natural history in Rochester, Minn, 1950 through 1982. Arch Ophthalmol. 1989;107(8):1160–1165. doi:10.1001/archopht.1989.01070020226030
12. Darougar S, Wishart MS, Viswalingam ND. Epidemiological and clinical features of primary herpes simplex virus ocular infection. Br J Ophthalmol. 1985;69(1):2–6. doi:10.1136/bjo.69.1.2
13. Rowe AM, Leger AS, Jeon S, Dhaliwal DK, Knickelbein JE, Hendricks RL. Herpes keratitis. Prog Retin Eye Res. 2013;32:88–101. doi:10.1016/j.preteyeres.2012.08.002
14. Raju KV, Jyothi PT, SIM M. Clinical profile of herpes simplex keratitis. KSOS J. 2011;23(1):33–36.
15. Labetoulle M, Auquier P, Conrad H, et al. Incidence of herpes simplex virus keratitis in France. Ophthalmology. 2005;112(5):888–895. doi:10.1016/j.ophtha.2004.11.052
16. Pramod NP, Rajendran P, Kannan KA, Thyagarajan SP. Herpes simplex keratitis in South India: clinico-virological correlation. Jpn J Ophthalmol. 1999;43(4):303–307. doi:10.1016/S0021-5155(99)00026-X
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
