Back to Journals » Clinical Ophthalmology » Volume 8
Clinical application of optical coherence tomography in combination with functional diagnostics: advantages and limitations for diagnosis and assessment of therapy outcome in central serous chorioretinopathy
Authors Schliesser J, Gallimore G, Kunjukunju N, Sabates N, Koulen P, Sabates F
Received 23 August 2014
Accepted for publication 16 September 2014
Published 21 November 2014 Volume 2014:8 Pages 2337—2345
DOI https://doi.org/10.2147/OPTH.S73119
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Joshua A Schliesser, Gary Gallimore, Nancy Kunjukunju, Nelson R Sabates, Peter Koulen, Felix N Sabates
Vision Research Center, Department of Ophthalmology, University of Missouri – Kansas City, School of Medicine, Kansas City, MO, USA
Purpose: While identifying functional and structural parameters of the retina in central serous chorioretinopathy (CSCR) patients, this study investigated how an optical coherence tomography (OCT)-based diagnosis can be significantly supplemented with functional diagnostic tools and to what degree the determination of disease severity and therapy outcome can benefit from diagnostics complementary to OCT.
Methods: CSCR patients were evaluated prospectively with microperimetry (MP) and spectral domain optical coherence tomography (SD-OCT) to determine retinal sensitivity function and retinal thickness as outcome measures along with measures of visual acuity (VA). Patients received clinical care that involved focal laser photocoagulation or pharmacotherapy targeting inflammation and neovascularization.
Results: Correlation of clinical parameters with a focus on functional parameters, VA, and mean retinal sensitivity, as well as on the structural parameter mean retinal thickness, showed that functional measures were similar in diagnostic power. A moderate correlation was found between OCT data and the standard functional assessment of VA; however, a strong correlation between OCT and MP data showed that diagnostic measures cannot always be used interchangeably, but that complementary use is of higher clinical value.
Conclusion: The study indicates that integrating SD-OCT with MP provides a more complete diagnosis with high clinical relevance for complex, difficult to quantify diseases such as CSCR.
Keywords: spectral domain optical coherence tomography, retina, ophthalmology, microperimetry, visual acuity, structure-function
Introduction
Central serous chorioretinopathy (CSCR), an acute disease affecting the blood-retina barrier of the eye, is characterized by a combination of structural damage to the retina and retinal pigment epithelium as well as symptoms ranging from blurred vision to scotomas.1–3 Both diagnosis and treatment of this poorly understood disorder are difficult, as the complexity of CSCR, characterized by a combination of transient and permanent signs and symptoms, has prevented the development of effective guidelines in both areas. Clinical care of CSCR involves pharmacotherapy targeting inflammation and neovascularization, including novel approaches such as intravitreal administration of antivascular endothelial growth factor biologicals, focal laser photocoagulation, and photodynamic therapy (PDT).1 At the same time, the diagnosis of the disease typically relies on identification of a range of clinical parameters. These include causative aspects of the disease, such as a compromised blood-retina barrier that requires identification with fluorescein angiography to identify sites of retinal pigment epithelium detachment and of serous fluid leakage in the retina. Indocyanine green angiography can be beneficial for some patients when the diagnosis is uncertain and when PDT is being considered for treatment.4 The main diagnostic tools target functional and structural changes. Assessment of visual acuity (VA) is the primary method of evaluating function; however, its usefulness is limited, as even 20/20 vision can be accompanied by visual disturbances, and the Amsler grid has its own limitations, creating a need for more accurate functional analyses.5 Optical coherence tomography (OCT) is the diagnostic tool of choice to identify structural changes that underlie such disturbances, including areas of disease origination that require targeting with focal laser photocoagulation and PDT strategies.5 This more objective form of structural analysis and testing can also be complemented with objective forms of diagnosis that test visual function by measuring retinal sensitivity to defined visual stimuli such as microperimetry (MP).6 The need for such integrated complementary diagnostic strategies is particularly great in complex diseases such as CSCR, because different functional and structural parameters used to determine disease severity and therapy outcome can have distinct temporospatial patterns, with some parameters lagging behind others. For example, VA can improve while retinal thickness measured with OCT does not change, or retinal sensitivity assessed by MP can improve while VA remains unchanged or worsens. These confounding clinical observations are partially driven by the quality of the diagnostic tools employed and also by the different sensitivities of both functional and structural diagnostics; the documentation of VA is often operator dependent and changes in best corrected vision may not be achievable. This emphasizes the need for a comprehensive integration and evaluation of such subjective measures with more objective measures of testing such as OCT and MP. Using these functional and structural parameters, the study investigated how an OCT-based diagnosis of CSCR can be significantly supplemented with functional diagnostic tools, and to what degree the determination of disease severity and therapy outcome can benefit from diagnostics complementary to OCT. To this end, the present study tested if the correlation of VA, mean retinal sensitivity (as assessed by MP), mean retinal thickness (measured using OCT), and other clinical parameters facilitated the differential assessment of disease severity and of therapy outcome at defined time points of clinical care.
While spectral domain optical coherence tomography (SD-OCT) generates a detailed three-dimensional image of the retina, advanced modalities allow also an assessment of the choroid,7 which is critical for both diagnosis and treatment of eye diseases, including CSCR. Similarly, technical advancements have been made in the area of MP, where the sensitivity of specific regions of the retina and macula is registered with an image of the retina that is typically generated with a scanning laser ophthalmoscope. The integration of functional MP data with advanced OCT data is gaining greater clinical utilization.6 Previous studies have identified CSCR as an ideal target disease for such differential integration of diagnostics complementary to OCT, as both functional and structural abnormalities often persist in resolved CSCR8 and led us to investigate the potential use of a differential assessment of disease severity and of therapy outcome.
Methods
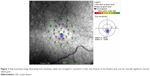
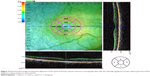
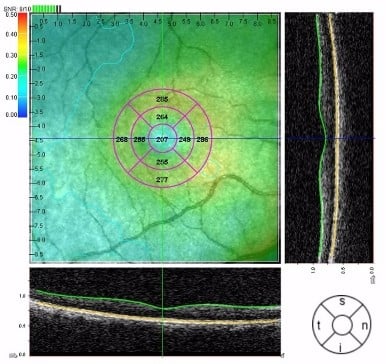
Using a prospective study design, the present Institutional Review Board-approved study involved 15 patients with clinically validated CSCR history (serous detachment determined by OCT, serous fluid leakage determined by fluorescein angiography) in one eye at presentation and measured their best corrected VA, macular sensitivity using MP, and retinal thickness using SD-OCT as primary outcome measures. Patients received clinical care that involved pharmacotherapy targeting inflammation and neovascularization or focal laser photocoagulation. Patients also had resolution of serous detachment (Figure 1) at time of final MP testing, ie, the study visit. Study patients were excluded if they had previous history of glaucoma, ocular hypertension with an intraocular pressure greater than 21 mmHg, or if they had a media opacity such as a cataract or corneal pathology that would affect testing of retinal sensitivity. The average time from presentation to study visit was 188 weeks. Clinical parameters recorded and evaluated age, sex, VA under standard conditions using the Snellen acuity chart, presenting symptoms, treatments administered, fluorescein angiography leakage pattern, retinal thickness assessed by SD-OCT, retinal sensitivity measured with MP, the existence of detached retinal pigment epithelium at the time of presentation, and the time until the serous detachment was resolved. All patients underwent a detailed ophthalmic exam that included applanation tonometry, slit-lamp microscopy, and binocular fundus examination using indirect ophthalmoscopy. Patient demographics are listed in Table 1. During the study visit, eyes were dilated (1% tropicamide, 2.5% phenylephrine hydrochloride eye drops) and a OPKO SLO/SD-OCT microperimeter (OPKO Health, Inc., Miami, FL, USA) was used to measure retinal sensitivity and thickness as described previously.6 Figure 2 illustrates how threshold MP employed a specific stimulus and testing pattern using a clinically significant macular edema (CSME) grid. MP data included the average sensitivity, stability of fixation, and identified macular scotomas as shown previously6 (relative scotoma: sensitivity ≤10 dB; absolute scotoma: sensitivity of 0 dB). Stability of fixation was determined using the classification scheme established by Fujii et al,9 and a three-dimensional map of the retina was generated after MP testing using SD-OCT determining retinal thickness as the distance between the retinal nerve fiber and retinal pigment epithelial layers and using the CSME grid (Figure 3). Statistical analysis was performed by summarizing measured variables of primary outcome measures, VA, retinal sensitivity, and thickness, and the use of descriptive statistics (Microsoft® Office Excel® 2010). Excluded outliers were qualified as values deviating from the mean by more than three standard deviations and represented one case in the studied population characterized by extreme retina damage that did not resolve. Statistically significant differences among covariates were determined with analysis of variance (ANOVA) with P-values <0.05 termed significant and P-values <0.01 and <0.001 identified separately. Correlation between measured parameter variables was calculated using the Pearson product-moment correlation coefficient and linear regression analyses along with goodness of fit measurements were performed.
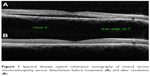  | Figure 1 Spectral domain optical coherence tomography of central serous chorioretinopathy serous detachment before treatment (A) and after resolution (B). |
  | Table 1 Patient demographics |
Results and discussion
The patient demographics are listed in Table 1. Fifteen eyes of fifteen patients with resolved CSCR were evaluated. There were eleven men and four women whose ages ranged from 30 to 67 years old (mean age, 49 years). Best corrected visual acuity at initial presentation was 0.22 logarithm of the minimum angle of resolution (logMAR) (±0.21) in eyes with CSCR and 0.02 logMAR (±0.08) in unaffected eyes. In four eyes, no treatment was administered and the patients were observed. Intravitreal injection of bevacizumab, an antivascular endothelial growth factor biological, was used in three eyes as initial treatment. Focal laser photocoagulation and PDT was used in four eyes. In patients unresponsive to all other treatment options, topical nonsteroidal anti-inflammatory eye drops were used in three cases and sub-Tenon’s injection of triamcinolone was used in one eye. These patients who received nonsteroidal anti-inflammatory eye drops and sub-Tenon’s injection of triamcinolone were grouped into an anti-inflammatory treatment group. All patients were followed for resolution of CSCR. Table 2 lists average ± standard deviation for VA, macular sensitivity, and retinal thickness for the eyes with CSCR and unaffected eyes at presentation and at the study visit. Statistically significant differences between the affected eye and the unaffected control eye at presentation and lack thereof at the study visit after resolution of CSCR indicate improvement of clinically relevant parameters following therapy. The average time to resolution for all eyes with CSCR was 19 weeks, with serous detachment taking approximately twice as long to resolve in the observation group compared to the treated groups (P<0.01). This finding confirms previous studies identifying that treatment considerably decreases the time necessary for resolution of serous detachment resolution and for improvement in VA.10–12 An evaluation of the stability of fixation during MP data acquisition was performed at the time of the study visit. All but one of the CSCR eyes had stable fixation (more than 75% of all fixation points were located within the two-degree circle). The one eye without stable fixation was classified as relatively stable (fewer than 75% of fixation points were located within the two-degree circle, but more than 75% of the same fixation points were located within a defined four-degree circle), had been treated with focal laser photocoagulation and PDT, and had significant improvement in average macular sensitivity from presentation despite moderate fixation losses. The patients in the bevacizumab group had minimal improvement in VA, but no improvement in macular sensitivity despite resolution of the serous detachment. Similarly, patients in the observation group had only minimally improved VA and macular sensitivity, but lacked an improvement in retinal thickness. Only patients in the focal laser photocoagulation and PDT group showed improvement in VA and retinal thickness. These findings show that despite resolution of subretinal fluid, with or without treatment, functional abnormality of the retina potentially persists over time.8,13–15
This composition of patient demographics and variable disease phenotypes and therapy outcomes in CSCR patients provided an ideal scenario to test the overall goal of the present study, to identify how an OCT-based diagnosis of CSCR can be significantly supplemented with functional diagnostic tools, and to what degree the determination of disease severity and therapy outcome can benefit from diagnostics complementary to OCT. Three different data sets were evaluated statistically using data normalization strategies with relevance to either disease diagnostics or evaluation of therapy outcome:
(1) | Parameters were normalized as data for the affected eye over data from the contralateral control eye for VA and MP and the inverse ratio for OCT at the time of presentation. This normalization allowed us to identify disease-mediated damage as ratios smaller than one at the beginning of the study. |
(2) | A second set of normalized parameters were generated by dividing the value for the affected eye by the respective value for the healthy, contralateral control eye obtained at the end of the study after treatment of the study participants had taken place for VA and MP, while the inverse ratios were calculated for OCT identifying disease-mediated damage in parameters assessing visual function and retina structure as ratios smaller than one at the end of the study. |
(3) | The third set of normalized data was obtained by dividing values for the affected eye at the end of the study by values for the same eye acquired at the time of presentation (VA and MP) or the inverse ratio for OCT. This allowed us to identify therapy-related improvement in parameters assessing visual function and retina structure as values greater than one. |
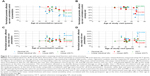
Statistical analysis with analysis of variance showed that there were no statistical differences among the three clinical outcome measures: VA, mean retinal sensitivity as assessed by MP, and mean retinal thickness measured using OCT for normalization strategies 1–3 (P-values: 0.24, 0.07, and 0.14, respectively). This finding that the three main diagnostic strategies were not statistically different in their capability to evaluate and qualify disease severity and therapy outcome allowed us to further assess how well the diagnostic modalities were correlated. We initially correlated these parameters assessing visual function and retina structure with patient age. In Figure 4, normalized values for decimal VA, mean retinal sensitivity as assessed by MP, and mean retinal thickness measured using OCT were plotted over the age of the study participants for each individual data set. Linear regression analyses and analysis of the degree of correlation show that when parameters were normalized as ratios of data from the affected and the contralateral control eye, moderate correlations with age exist for VA, mean retinal thickness and mean retinal sensitivity, though weaker for mean retinal thickness (Figure 4A). When correlating the same parameters acquired at the end of the study over the age, comparable correlations with age were found for all three parameters (Figure 4B). However, when data sets were normalized only for the affected eye by forming ratios from values acquired at the time of presentation and at the end of the study, the moderate correlations found for VA measurement with age were only paralleled by weak correlations for mean retinal thickness and mean retinal sensitivity when correlated with the study participants’ age at the time of presentation (Figure 4C) or their age at the final study visit (Figure 4D). In sum, correlation of VA, mean retinal sensitivity, and mean retinal thickness with the age of the study participants showed a moderate positive correlation of disease-mediated damage with age, but also a weak positive correlation of therapy-related improvement with age. While the functional measures were similar in diagnostic power, a reduced strength in the correlation of retina structure by OCT with functional measures shows that the diagnostic measures cannot always be used interchangeably, but that a complementary use is of higher clinical value.
We subsequently correlated the parameters assessing visual function and retina structure at defined time points of clinical care and with data normalization, allowing the comparison of disease severity and of therapy outcome. Normalized values for the decimal conversion of VA, for mean retinal sensitivity as assessed by MP, and for mean retinal thickness were plotted using the above-mentioned three different methods of normalization corresponding to time points of clinical care and evaluating disease severity and therapy outcome (Figure 5). At presentation, functional parameters (MP and VA) are strongly correlated (Figure 5A), while structural assessment of the retina with OCT is moderately correlated with the standard measure of visual function, VA (Figure 5B). This implies that OCT can function as an adjuvant diagnostic tool identifying disease aspects that are not accessible with measures of VA alone.
The parameters assessing visual function through MP and retinal structure through OCT are highly correlated for time points assessing the extents of initial disease-related damage (Figure 5C) and of therapy outcome (Figure 5F, I). While the strength of the moderate correlation between OCT and VA is similar during initial disease assessment (Figure 5B) and at the end of the treatment (Figure 5E, H), the strongest correlation between VA and MP was seen during initial disease assessment (Figure 5A) and was lower at the final study visit (Figure 5D, G). This finding indicates that combining OCT with MP provides a more complete diagnosis with high clinical relevance for complex and difficult to quantify diseases such as CSCR.
Conclusion
In sum, the correlation of parameters assessing visual function and retina structure at defined time points of clinical care will facilitate the differential assessment of disease severity and of therapy outcome. This is particularly relevant, because CSCR is an example of diseases with a broad clinical spectrum of signs and symptoms that can be analyzed with structural and functional parameters and where quantitative OCT is routinely employed. MP can be a valuable adjunct to this quantitative measure as well as of more qualitative measures, such as VA, in the evaluation and management of disease.
Acknowledgments
Research reported in this publication was supported by the Felix and Carmen Sabates Missouri Endowed Chair in Vision Research, a Challenge Grant from Research to Prevent Blindness, and the Vision Research Foundation of Kansas City. We thank Margaret, Richard, and Sara Koulen for generous support and encouragement.
Disclosure
The authors report no conflicts of interest in this work.
References
Nicholson B, Noble J, Forooghian F, Meyerle C. Central serous chorioretinopathy: update on pathophysiology and treatment. Surv Ophthalmol. 2013;58(2):103–126. | ||
Gass JD. Pathogenesis of disciform detachment of the neuroepithelium. Am J Ophthalmol. 1967;63(3):Suppll–139. | ||
Jalali S, Gupta A, Jain IS, Ram J. Visual prognosis in central serous choroidopathy: residual Amsler grid changes. Can J Ophthalmol. 1991;26(5):270–272. | ||
Yannuzzi LA, Slakter JS, Gross NE, et al. Indocyanine green angiography-guided photodynamic therapy for treatment of chronic central serous chorioretinopathy: a pilot study. Retina. 2003;23(3):288–298. | ||
Roisman L, Lavinsky D, Magalhaes F, et al. Fundus autofluorescence and spectral domain OCT in central serous chorioretinopathy. J Ophthalmol. 2011;2011:706849. | ||
Sabates FN, Vincent RD, Koulen P, Sabates NR. Gallimore G. Normative data set identifying properties of the macula across age groups: integration of visual function and retinal structure with microperimetry and spectral-domain optical coherence tomography, Retina, 2011;31(7):1294–1302. | ||
Adhi M, Duker JS. Optical coherence tomography – current and future applications. Curr Opin Ophthalmol. 2013;24(3):213–221. | ||
Ozdemir H, Karacorlu SA, Senturk F, Karacorlu M, Uysal O. Assessment of macular function by microperimetry in unilateral resolved central serous chorioretinopathy. Eye (Lond). 2008;22(2):204–208. | ||
Fujii GY, De Juan E, Humayun MS, Sunness JS, Chang TS, Rossi JV. Characteristics of visual loss by scanning laser ophthalmoscope microperimetry in eyes with subfoveal choroidal neovascularization secondary to age-related macular degeneration. Am J Ophthalmol. 2003;136(6):1067–1078. | ||
Kim M, Lee SC, Lee SJ. Intravitreal ranibizumab for acute central serous chorioretinopathy. Ophthalmologica. 2013;229(3):152–157. | ||
Seong HK, Bae JH, Kim ES, Han JR, Nam WH, Kim HK. Intravitreal bevacizumab to treat acute central serous chorioretinopathy: short-term effect. Ophthalmologica. 2009;223(5):343–347. | ||
Chong CF, Yang D, Pham TQ, Liu H. A novel treatment of central serous chorioretinopathy with topical anti-inflammatory therapy. BMJ Case Rep. 2012;2012. pii: bcr2012006970. | ||
Toonen F, Remky A, Janssen V, Wolf S, Reim M. Microperimetry in patients with central serous retinopathy. Ger J Ophthalmol. 1995;4(5):311–314. | ||
Ehrlich R, Mawer NP, Mody CH, Brand CS, Squirrell D. Visual function following photodynamic therapy for central serous chorioretinopathy: a comparison of automated macular microperimetry versus best-corrected visual acuity. Clin Experiment Ophthalmol. 2012;40(1):e32–e39. | ||
Vasconcelos H, Marques I, Santos AR, et al. Long-term chorioretinal changes after photodynamic therapy for chronic central serous chorioretinopathy. Graefes Arch Clin Exp Ophthalmol. 2013;251(7):1697–1705. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.