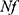Back to Journals » International Journal of General Medicine » Volume 13
Blood Pressure Control, Left Ventricular Hypertrophy and Treatment Practice Among Hypertensive Patients in Ethiopia
Authors Kinfe DG ![]() , Berhe G
, Berhe G ![]() , Gidey K
, Gidey K ![]() , Demoz GT
, Demoz GT ![]()
Received 29 July 2020
Accepted for publication 1 October 2020
Published 20 October 2020 Volume 2020:13 Pages 903—916
DOI https://doi.org/10.2147/IJGM.S273668
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Daniel Gebrehawaria Kinfe,1 Gebretsadik Berhe,2 Kibreab Gidey,3 Gebre Teklemariam Demoz4
1Department of Internal Medicine, School of Medicine, Aksum University, Aksum, Ethiopia; 2Department of Epidemiology, School of Public Health, Mekelle University, Mekelle, Ethiopia; 3Department of Internal Medicine, School of Medicine, Mekelle University, Mekelle, Ethiopia; 4Department of Clinical Pharmacy, School of Pharmacy, Aksum University, Aksum, Ethiopia
Correspondence: Gebre Teklemariam Demoz
Department of Clinical Pharmacy, School of Pharmacy, Aksum University, Aksum 298, Ethiopia
Tel +251914031986
Email [email protected]
Background: Globally, hypertension is the most important public health issue and is a increasing health problem in Ethiopia. Blood pressure (BP) control is an ultimate therapeutic goal of hypertensive patients in reducing early complications of hypertension. Hence, this study was sought to examine the magnitude of uncontrolled BP, left ventricular hypertrophy (LVH), and treatment practice. Predictors of uncontrolled BP and LVH were also investigated.
Methods: A hospital-based cross-sectional study was conducted among 223 outpatients with hypertension on follow-up at Ayder Comprehensive Specialized Hospital (ACSH). Hypertensive patients with ≥ 18 years old who had been on follow-up care for at least 3 months were included in the study. Severely ill patients requiring urgent medical care and wheelchair-bound individuals or persons who had difficulty standing steady and pregnant women were excluded. Data were collected using a structured questionnaire and patients’ chart review. Data were entered and analyzed using SPSS version 22.0. To identify predictors, binary logistic regression model analysis was performed. Statistical significance was set at P-value of < 0.05.
Results: The magnitude of uncontrolled BP (> 140/90mmgH) and LVH was found to be 31.4% and 39.5%, respectively. More than half (53%) of participants were on at least two antihypertensive drug combinations of different classes. Uncontrolled BP was significantly associated with poor adherence to salt reduction in meal (Adjusted Odds Ratio (AOR) =8.552, 95% CI: 2.853, 15.638, P< 0.001), non-adherence to medications (AOR =2.886, 95% CI: 1.710, 3.935, P< 0.001), and taking triple-drug therapy (AOR=7.228, 95% CI: 1.110, 10.57, P=0.039). Presence of LVH was significantly associated with abdominal obesity (AOR= 2.2, 95% CI: 1.399, 4.69, P=0.003), age of ≥ 60 years (AOR= 2.421, 95% CI: 1.263, 4.639, P=0.008), and uncontrolled BP (AOR= 3.16, 95% CI: 1.208, 5.232, P=0.021).
Conclusion: In this study, a significant proportion of patients with uncontrolled BP and LVH were found. Abdominal obesity, older age and uncontrolled blood pressure were predictors of LVH. Therefore, tailored interventions targeting BP control to reduce the magnitude of LVH and other early complications of hypertension deemed to be compulsory.
Keywords: blood pressure, hypertension, left ventricular hypertrophy, predictors, Ethiopia
Background
Hypertension is an important public health issue and globally, an estimated 26% of populations are living with hypertension. This figure is projected to rise to 29% in 2025.1 Thus, hypertension is a major attributor to other cardiovascular diseases that becomes the world first leading cause of death and demands a significant public health burden.2
In 2014, the prevalence of hypertension in Africa is as high as 30%. In Sub-Saharan Africa, hypertension has shown a rapid increase in prevalence affecting significant numbers of people.1 Though one-fourth (25%) of Ethiopians are living with hypertension, the prevalence of hypertension in various regions are varied widely.3 One study conducted in Northern Ethiopia reported that the prevalence of hypertension is 18.1%.4
Blood pressure (BP) control is an ultimate therapeutic goal of hypertensive patients in reducing early complications of hypertension. Thus, the primary goal of antihypertensive treatment is to prohibit cardiovascular and renal morbidity and mortality. A reduction in cardiovascular problems is a vital that patients with hypertension get proper treatment for optimal control of BP.5 This will help reduce the risk of congestive heart failure by 50%, cerebrovascular diseases by 25–30%, and myocardial infarction by 20–25%.6
Complications commonly found are left ventricular hypertrophy (LVH) and microalbuminuria, with rates of 33% and 6–40%, respectively.2
Generally, these complications are observed at an early stage of hypertension followed by other complications. According to the survey conducted in the United State, 35% of patients with hypertension had their BP under control.7 The association between elevated BP and cardiovascular incident risk is ongoing, persistent and independent from other risk factors. The higher the BP, the greater will be the chance of heart attack, heart failure, stroke, and kidney diseases. Thus, risk of hypertension is increased by existence of each additional risk factors.8
In Ethiopia, a study done at Jimma Specialized Hospital9 and Adama10 showed that rate hypertension control was 50.3% and 43.6%, respectively.
A further marker of early hypertension complications is LVH. In hypertensive patients, premature ventricular contractions, ventricular arrhythmias and sudden heart death are observed more frequently with LVH than in those without LVH.11,12 Studies have shown a direct relationship between the level and duration of elevated BP and LVH.12
The success of treating hypertension has been limited, and despite well-established approaches for diagnosis and treatment, in many communities, fewer than a half of all hypertensive patients have controlled blood pressure.13 Hypertension is becoming a major public health challenge in our country.8 However, there is little national and regional data regarding the level of blood pressure control and factors associated with hypertension control as well as early complications of hypertension, such as LVH and microalbuminuria which are thought to be early markers of renal and cardiac complications of uncontrolled hypertension, respectively.
Therefore, this study sought to investigate the level of hypertension control, early complications and to identify possible predictors for uncontrolled BP and LVH among patients with hypertension on follow-up care at Ayder Comprehensive Specialized Hospital, Ethiopia.
Methods
Study Setting
This study was conducted at Ayder Comprehensive Specialized Hospital (ACSH). ACSH is found at Mekelle city, Tigray region, northern Ethiopia, located at 783 km away from Addis Ababa, the capital city of Ethiopia. This hospital the first largest referral and teaching hospital in the region affiliated with Mekelle University. ACSH is one of the university hospitals in the country with regard to the type and quality of services provision intended to serve for more than 8 million people and render referral and non-referral services to catchment areas of Tigray, neighbouring regions of Afar and Amhara population. This hospital has more than 500 beds and comprised many departments. Internal medicine department is one of the departments consists of cardiology, gastroenterology, pulmonology, neurology, haematology, nephrology and endocrinology units. This study was particularly conducted at ACSH medical referral clinic unit for hypertension follow-up care.
Study Design and Participants
A hospital-based cross-sectional study was carried out from September 2019 to December 2019. All adult hypertensive outpatients who visited the clinic during the study period were included in this study.
Eligibility Criteria
Patients 18 years old age and above who had been on follow-up care for at least 3 months in the clinic were included in the study. Severely ill patients requiring urgent medical care and wheelchair-bound individuals or persons who had difficulty standing steady and pregnant women were excluded.
Variables
Level of BP control and magnitude of Left Ventricular Hypertrophy (LVH) were our dependent variables. Age, gender, residence, duration of illness, medication adherence, smoking, salt intake, physical inactivity were our independent variables.
Data Collection Instruments and Procedures
A data abstraction format was used to record the necessary information from the patient’s chart and a structured questionnaire was used to interview the participants. The questionnaire was adopted from the literature review with modifications to fit the current study. Weight, height, and waist circumferences of patients were taken on the day of the interview.
Data were collected using interviewer-administered structured questionnaire which was prepared in English and designed to meet the study objective. The questionnaire had different parts including the socio-demographic data, comorbidities, BP recordings, questions on adherences and relevant laboratory investigations for the study attempting to extract possible factors that lead to poor hypertension control. Chart reviews and Smart care (patient information on computers) were also used to extract relevant data. Electrocardiography was interpreted by cardiologists.
The standard mercury sphygmomanometer and auscultatory methods with a stethoscope were used to measure the BP after allowing the patient a rest for at least 5 minutes. There are a well-experienced nurses assigned at the unit who takes the BP of each patient. When there is very low or very high BP measurement, it’s repeated after 10–15 minutes rest either by the nurse or the resident and the final measurement is recorded on the chart. Three consecutive measures were taken to determined the level of BP control. In each follow up when there is uncontrolled BP (≥140/90) tight control (<120/70) the BP is measure again to minimize measurement errors. Weight was measured using a balance beam scale and participants were asked to remove heavy outer garments and shoes and if they refused to remove their garments or shoes, it was reported in the data collection form. Height was measured using a measuring rod attached to the balanced beam scale.
Waist circumference was measured at a level midway between the lower rib margin and iliac crest with a flexible but non-stretchable tape meter. Self-reported measurements were not accepted. The expense for investigations was covered by the study participants as part of base line workup for all hypertensive patients. There was no interference with the hospital protocol during data collections. Medication adherence for antihypertensive was assessed using Brief Medication Questionnaire (BMQ).14 Reported drug side effect data were extracted from patient charts as well as self-reported by patients and interpreted as a drug side effect by attending physicians.
Sample Size Determination and Sampling Technique
Every adult hypertensive patient who fulfilled the inclusion criteria was included in this study. The sample size was determined from the estimated populations who had follow up at ACSH hypertension follow-up clinic and who had been on antihypertensive medications for at least 3 months prior to enrolment. An assumption was taken that each month about 110 hypertensive patients could be seen at the medical referral clinic (MRC) and a patient could be appointed after a maximum follow-up period of 3 months for the next visit which means about 330 hypertensive patients could be seen at the MRC.
The sample size was calculated using the formula: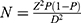
Where (P) is the proportion of people with controlled BP. The value of P was taken from a similar study conducted in Ethiopia previously where the level of BP control was found to be 52.5%.15
D is margin of error and Z is the standard normal value at 95% confidence level which is substituted with 1.96.
In the present study, (D) is chosen to be 5% giving a power of (1-D) =95%.
Therefore, the sample size 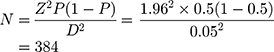
Since source population is small (330 people) correction of the sample size using correction formula is needed.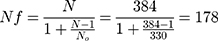
Adding 10% for non-response rate, the final sample size would be 196.
N= initially estimated sample size
No = study population.
Therefore, we decided to include all adult hypertensive outpatients who were on follow-up care during the study period and met the inclusion criteria were enrolled using consecutive sampling technique (Figure 1).
 |
Figure 1 Schematic flow chart of recruiting participants for analysis. |
Data Quality Assurance
Content validity of the questionnaire was assessed using two experts (cardiologists) and implications of all variables were checked accordingly. Items understandability by the study participants were evaluated by pre-testing the questionnaire on 5% of the sample population prior to data collection and the necessary correction was taken accordingly. The questionnaire was also provided in the original language namely English, avoiding the need for translation and maintaining consistency of the questions and responses.
The principal investigator trained data collectors and supervisors for two days. The training included detail explanation on the objectives of the study, meanings of the lists of questions on the questionnaire, approach to study participants; and a clear explanation on the ethical procedure. The data collectors were three clinical nurses working at ACSH who were supervised by two cardiologists working at the medical referral clinic and the principal investigator. The principal investigator and supervisors reviewed participants’ charts followed and checked the way how data collectors conducted the interviews. Then the collected data was immediately put in a safe place. Double data entry was used and saved in different computers.
Data quality was also assured by checking the data collection sheet daily for completeness and errors by supervisors, and when necessary corrections were made immediately. Data cleaning, coding and entering were done carefully using the standard instruments and operating procedures listed above.
Data Processing and Analysis
Data were cleaned and entered into Statistical Package for Social Sciences (SPSS) version 22.0 for analysis. Descriptive and analytical statistics including bivariate and multivariate analysis was employed to confirm the association between variables, and measures of frequency and proportions were utilized for socio-demographic variables. Whether the multivariate logistic regression model is adequate or not, Hosmer-Lemeshow goodness- of- fit test was done and found to be insignificant at 5% (P-value=0.461). This indicates that the model is adequate. The level of BP control was assessed using the average of three consecutive BP records obtained from three different visits measurement values. Bivariate logistic regression was performed and P-value of <0.25 was used for further multivariate logistic regression analysis to predictors that affect BP control and LVH. This was done using odds ratio and significance of statistical association was tested using a 95% confidence interval and statistical significance was set at a P-value of < 0.05. The results were narrated and summarized using texts and presented using tables and graphs.
Operational Definitions
Hypertension: sustained high blood pressure (SBP≥ 140mmHg and/or DBP≥ 90 mmHg) and/or taking antihypertensive medications controlled BP: BP<140/90 mmHg for all hypertensive patients and Uncontrolled BP: BP≥140/90 mmHg for all hypertensive patients.16 Overweight: BMI between 25 and 29.9 kg/m2, Obesity: BMI ≥ 30kg/m2, Over weight: 25–29.9kg/m2, Underweight: BMI < 18kg/m2, Normal weight: 18–24kg/m2 17 and Central obesity: waist circumference >94 cm for males and >80 cm for females.6 Physically active: an individual who performs physical exercise for at least 30 minutes/day for at least 05 days/week and Physically inactive: an individual who performs physical exercise for less than 30 minutes/day and/or for less than 05 days/week.18 Salt Restriction: 1TSP salt≈6g NaCl≈2.4g Na that a participant was said to be on salt restriction if he/she reported the use of separate dish without adding salt or adding not more than half TSP salt over 24 hours; otherwise he/she was said to be on no salt restriction.6 Smoking, Khat chewing and alcohol intake: if a patient reports using any of these for recreational or similar purposes it was taken as a positive answer regardless of the dose or amount. Left Ventricular Hypertrophy (LVH): The following criteria have been developed to diagnose LVH on ECG. Cornell Criteria: If the sum of the R wave in aVL and the S wave in V3 is > 28mm and 20mm in males and females, respectively; LVH is present. Modified Cornell Criteria: If the R wave in aVL is > 12mm in amplitude; LVH is present. Sokolow-Lyon Criteria: If the sum of the S wave in V1 and the R wave in V5 or V6 is >35mm; LVH is present.19 Micro-albuminuria: An abnormally increased excretion rate of albumin in the urine in the range of 30–299mg/g creatinine. Urine protein lab values for micro-albuminuria of >30mg/day correspond to a detection level within the “trace” to “1+” range of a urine dipstick protein assay.20
Results
Socio-Demographic Characteristics
A total of 228 hypertensive patients were interviewed and 223 of them were eligible and included in the study with a response rate of 97.8%. The majority of study participants were females 143 (64.1%). The mean age of respondents was 56.21 (SD=11.80) and more than half (54.7%) of the participants were under the age of 60. Most of the respondents 196 (87.9%) were urban residents. More than half (66.4%) of the participants were married, 107 (48%) housewives, and 103 (46.2%) had no formal education. The most common religion 203 (91%) was Orthodox Christianity. Nearly two-thirds (62.3%) of the participants were in the low-income category (Table 1).
 |
Table 1 Socio-Demographic Characteristics of Hypertensive Patients on Follow Up at ACSH, Ethiopia, 2019 |
Lifestyle Related Factors
Among the participants, 165 (74.0%) reported that they reduced salt in their meal while 3 (1.3%) were smokers. Forty-seven (21.1%) of the respondents were physically inactive. Fifty-nine (26.5%) of participants were overweight while 12 (5.4%) were obese. Majority of 107 (74.8%) of women had a waist circumference of >80cm while sixteen (20%) of men had a waist circumference of >94cm. Most of the participants 160 (71.7%) have been drinking coffee while 12 (5.4%) of them were alcohol drinkers (Table 2).
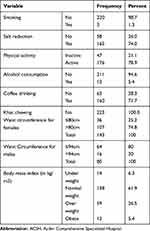 |
Table 2 Life Style and Anthropometric Related Characteristics of Hypertensive Patients on Follow Up at ACSH, Ethiopia, 2019 |
Clinical Characteristics
Among the study participants, 29 (13.0%) had a family history of hypertension. The mean duration of hypertension was 5.70 (SD=4.87) years and 116 (52.0%) of the participants had hypertension for less than 5 years. The mean treatment duration was 4.35 (SD=4.15) years. Most participants 163 (73.1%) got their BP measured every 2–4 weeks while thirty (13.4%) of them got measurements with an interval of >4 weeks. Nearly one-third (34.1%) of participants had comorbidities. Stroke was the most common comorbidity accounting for 9.4% (Table 3).
 |
Table 3 Clinical Characteristics of Hypertensive Patients on Follow Up at ACSH, Ethiopia, 2019 |
Prescribing Pattern of Antihypertensive Drugs and Their Side Effects
The majority (59.64%) of the participants received more than one antihypertensive medication. More than half (51.12%) of the participants were on two medications and 40.36% were on single-drug therapy. Forty (18%) of the participants on dual therapy had uncontrolled BP while 68 (30.5%) of participants had controlled BP. Fifteen (7%) of participants were on triple antihypertensive medications. Thiazide diuretics and angiotensin-converting enzyme (ACE) inhibitors were the most common combination of antihypertensive medications (43.8%), followed by calcium channel blockers and thiazide diuretics (26.3%). Overall, the most commonly prescribed drug was hydrochlorothiazide (68.2%) followed by enalapril (45.7%) and nifedipine (28.7%).
Among all the respondents 17.5% of participants experienced at least one side effect of the medications. Peripheral oedema (8.1%) was the most common side effect which occurred in 17% of patients taking CCBs followed by headache (4.9%). Dry cough was the next common (3.6%) side effect occurring in 8% of patients taking ACEIs while 82.5% of participants reported no side effects. Furthermore, 160 (71.7%) participants were adherent to their antihypertensive medications while 28.3% were non-adherent (Table 4).
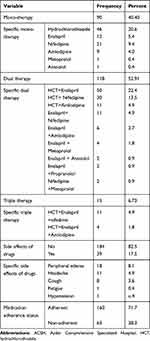 |
Table 4 Prescribing Pattern of Antihypertensive Drugs and Common Side Effects Among Hypertensive Patients on Follow Up at ACSH, Ethiopia, 2019 |
Blood Pressure Control
The mean SBP was found to be 132.74 (SD=16.40) while the mean DBP was 79.68 (SD=7.70). Majority (69.1%) of participants had a controlled SBP while 88.3% had controlled DBP. The cumulative control of BP was achieved in more than two-third of the study participants (68.6%). Patients taking CCB had uncontrolled BP compared to patients taking thiazides or ACEIs (COR=2.143, 95% CI: 1.204, 3.814 P=0 0.010). This has an implication on prescribing practice of antihypertensive treatment that ACEIs or thiazides are more preferable compared to CCB to control BP. Therefore, prescribers give attention when selecting drugs for hypertensive patients with LVH. But there was no difference in BP control between urban and rural dwellers (Figure 2).
 |
Figure 2 Level of BP control among hypertensive patients on follow-up care at ACSH, Ethiopia, 2019. |
Predictors of Uncontrolled Blood Pressure
The association of independent variables with the dependent variable was assessed using both bivariate and multivariate logistic regression. Overall, 31.4% of participants had uncontrolled blood pressure. In bivariate logistic regression; age, frequency of BP measurement, family history of hypertension, number of drugs taken, taking calcium channel blockers (CCB), adding salt to meal, medication non-adherence, and physical inactivity were found to be associated with uncontrolled BP; therefore they were used in multivariate analysis.
The result of multivariate analysis showed that patients who were poor adherence to salt reduction in their meal were 8.5 times (AOR=8.552, 95% CI: 2.853, 15.638) more likely to have uncontrolled hypertension as compared to those who reduced salt in their meal. Patients who were non-adherent to their antihypertensive medications were 3 times more likely to have uncontrolled hypertension than adherents (AOR=2.886, 95% CI: 1.710, 3.935). Patients who were on three-drug combinations were 7 times more likely to have uncontrolled hypertension compared to those who were on single drug or two-drug therapy (AOR=7.228, 95% CI: 1.110, 10.57). Hence, non-adherence to anti-hypertension medications and salt reduction and being on three-drug combinations were found to be predictors of uncontrolled hypertension (Table 5).
 |
Table 5 Bivariate and Multivariate Logistic Regression Analyses of Predictors of Uncontrolled BP Among Hypertensive Patients on Follow Up at ACSH, Ethiopia, 2019 |
Left Ventricular Hypertrophy (LVH)
More than one-third (39.5%) of participants had LVH on ECG while 17% of them had proteinuria (Figure 3).
 |
Figure 3 Magnitude of LVH and Proteinuria among hypertensive patients on follow up at ACSH, Ethiopia, 2019. |
Predictors of Left Ventricular Hypertrophy
In this study, 223 hypertensive participants had ECG investigation and of these, 39.50% had LVH. From the bivariate analysis, patients with the age of ≥60 years old, non-adherence to medications, abdominal obesity, physical inactivity, adding salt to diet and uncontrolled hypertension were found to be associated with the presence of LVH (Table 6). However, the result from the multivariate analysis showed that abdominal obesity, age≥60 years, and uncontrolled hypertensions were found to be predictors of LVH. The participants with abdominal obesity were 2.2 times more likely to have LVH when compared to participants who had no abdominal obesity (AOR= 2.2, 95% CI: 1.399, 4.69). Participants with the age of 60 years old and above were more than 2 times more likely to have LVH than participants with the age of <60 years (AOR= 2.421, 95% CI: 1.263, 4.639). Uncontrolled hypertension was found to have significant association with LVH in that participants with uncontrolled hypertension were more than 3 times more likely to develop LVH as compared to those with controlled hypertension (AOR= 3.16, 95% CI: 1.208,5.232) (Table 6).
 |
Table 6 Predictors of LVH Among Hypertensive Patients on Follow Up at ACSH, Ethiopia, 2019 |
Discussion
This study was sought to examine the BP control, left ventricular hypertrophy, treatment practice and possible predictors among hypertensive patients. Findings of this study showed that two-thirds (68.6%) of participants had controlled BP. More than one-third (39.5%) of participants had LVH on ECG. Poor adherence to anti-hypertension medications and salt reduction, and being on triple anti-hypertensive drug therapy were found to be predictors of uncontrolled hypertension. Age≥60 years, abdominal obesity, and uncontrolled hypertension were found to be predictors of LVH.
In this study, the success of treating hypertension and achieving optimal BP regulation was limited and, given well-established diagnostic and treatment strategies in many communities, less than half of all hypertensive patients controlled BP adequately.13 The level of BP control in this study (68.6%) was higher than most hospital-based reports of hypertension control across the world including; United State 60%,21 Spain 58%,22 Zimbabwe 32.8%,23 South Africa 42%,24 Nigeria 35%,25 Kenya 33.4%,26 and Ethiopia (Adama) 43.6%,10 and (Jimma) 50.3%.9 The possible explanation for the better BP control in our study may be due to differences in baseline characteristics of study participants. Besides the majority of participants in this study were relatively of young age, non-obese, non-smokers and with less comorbidity.
Adherence to antihypertensive drugs is a predictor of treatment success. Poor adherence to antihypertensive drugs amplifies optimal clinical outcomes and thus reduces overall health-care performance.6 In this study, the adherence rate of participants to antihypertensive medications was found to be 72%. This level of adherence is higher than what was reported from Jimma, Ethiopia (60.5%),9 Adama, Ethiopia (59.5%)10 and Nigeria (42.9%).25 According to a report from the systemic analysis for the global burden of disease study, estimates of the extent to which patients adhere to antihypertensive pharmacotherapy medications range between 44% and 90%.1
In this study the findings of adherence to antihypertensive medications are low; therefore further efforts are encouraged to optimize adherence to antihypertensive medications in order to reduce uncontrolled BP and associated cardiovascular diseases among hypertensive individuals. Adherence to antihypertensive medications is a key for achieving an optimal BP control; the findings of this study showed that non-adherent participants were 3 times more likely to have uncontrolled hypertension compared to adherent participants (P<0.001). This finding is consistent with the results reported from studies in the USA,27 South Africa,28 Zimbabwe,23 and Nigeria.25 Therefore, health professionals should focus on the importance of adherence to medications and encourage and counsel to their hypertensive patients.
In the current study, the rate of adherence of salt reduction was found to be 74% which is much lower than the recommendation.16 Adoption of healthy lifestyles by all people is critical for the prevention of high BP and is an indispensable part of the management of those with hypertension.17 JNC-8 recommends a moderately low intake of dietary sodium (<2.4g of sodium per day) for all individuals,16 and suggests that an even lower level may result in a greater reduction in BP. Hence hypertensive patients should be advised to decrease dietary salt intake to at least less than 1 tablespoon salt per 24 hours which is equivalent to 6 gram of sodium chloride.
The findings of the current study showed that participants with poor adherence to salt reduction in their meal were more than 8 times more likely to have uncontrolled blood pressure than those who reduced salt (P<0.001). This finding is consistent with the results from Jimma, Ethiopia,9 Zimbabwe,23 and South Africa.24 According to the TONE Collaborative Research Group; reduction of dietary sodium intake leads to in an additional 4.3 mmHg decrease in systolic BP among patients with hypertension.29
Drug therapy is the cornerstone of hypertension management. Currently, many options of drugs are available. More than two-thirds of patients with hypertension was not controlled with a single antihypertensive agent and eventually may require two or more antihypertensive agents from different drug classes.30 The findings of the current study revealed that more than a half (53%) of participants were on two drug combinations from different classes while more than one-third (40%) were on monotherapy; the remaining (7%) were on three drug combinations. The protocol of combining antihypertensive medications from different classes to achieve target blood pressure was consistent with the recommendations.6
The number of antihypertensive drugs used in the treatment of hypertension plays a big role in hypertension control. The results of this study showed that the participants who were on three-drug combinations were seven times more likely to have uncontrolled hypertension than those on monotherapy while two drug combinations were a referent. This finding is consistent with a hospital-based study done in Kenya26 and a cohort study from the United State of America.27 This difference can be due to the high likelihood that participants on triple combinations were those whose BP was difficult to control on single or two antihypertensive medications and would be difficult to control with three medications as well.
According to JNC 8; thiazide diuretics, ACEIs, ARBs, and CCBs are the initial therapy of choice while thiazide diuretics and CCBs are preferable in blacks.16 In this study the most commonly prescribed antihypertensive medications were thiazide diuretics 152 (68.2%), calcium channel blockers 105 (47.1%) and angiotensin-converting enzyme inhibitors 102 (45.7%). The most common combination therapies used were thiazides + ACEI 65 (29.1%), thiazides + CCB 56 (25.1%), and ACEI + CCB 34 (14.3%). Two participants were on B-blockers. The types of antihypertensive medications both monotherapy, as well as combination drugs, were not found to have significant association with BP control which is consistent with a meta-analysis of randomized controlled trials that showed comparable outcome benefits of all first-line drug classes.31
The prevalence of LVH based on ECG findings is variable.12 Studies have shown a direct relationship between the level and duration of elevated BP and LVH.12 In the present study, 88 (39.5%) of hypertensive participants had signs of LVH on ECG using the Cornell and Sokolow-Lyon criteria. Uncontrolled hypertension was found to have significant association with LVH. Participants with uncontrolled hypertension were more likely to develop LVH as compared to those with controlled hypertension. These findings were consistent to the cross-sectional study in Spanish hypertensive patients with LVH diagnosed according to Cornell criteria;32 whereas a study was done in hypertensive Nigerians revealed no significant difference in LVH prevalence between those with controlled and uncontrolled BP.33 The difference with the current study may be explained by differences in the methods of evaluation and type of study-base.
Premature ventricular contractions, ventricular arrhythmias, and sudden cardiac deaths are observed more often in hypertensive patients with LVH than in those without LVH.11,12 Therefore, early detection of LVH and aggressive lowering of BP can help to decrease these complications. The risk of LVH is increased twofold by associated obesity.12 In the current study, 74% of females had abdominal obesity while 20% of males had abdominal obesity. This finding is similar with studies done in Jimma, Ethiopia,9 Nigeria25 and Kenya26 but it’s more exaggerated in females in the current study. This difference might be due to differences in the life-style between females and males. The other explanation for this discrepancy could be due to differences in the operational definition of abdominal obesity. Since increased abdominal obesity is a risk factor for LVH emphasis should be given to the implementation of lifestyle modifications.
The result of this study has shown that abdominal obesity was significantly associated with LVH Participants with abdominal obesity increase their odds to have LVH compared to participants who had no abdominal obesity. Studies have shown that sustained weight loss of 4.4kg or more can reduce systolic and diastolic blood pressure by 7.0 and 5.0 mmHg, respectively.34 So all hypertensive patients should be counselled to be engaged in a moderate exercise in order to prevent obesity and control their BP. The mean age of participants in this study was 56.21 (SD=11.80), and more than half (54.7%) of them were younger than 60 years old. The odds of participants with 60 years or older were higher to develop LVH than those who were younger than 60 years. Similar reports were obtained from a study in Spain.32 This difference can be due to higher risk of arterial vascular disease and associated with uncontrolled BP in the elderly; hence particular attention should be given to elderly hypertensive individuals in controlling their BP.
The presence of a decreased glomerular filtration rate or albuminuria has prognostic implications for hypertensive patients. Studies reveal strong relationships between decrease in glomerular filtration rate and increase in cardiovascular morbidity and mortality.11,35 In the current study, 70% of participants had micro-albuminuria on two out of two or three urine collections using anti-body based dipstick tests. There was no statistically significant difference in the rate of micro-albuminuria between participants with controlled and uncontrolled hypertension group which is not in line with previous studies that suggest micro-albuminuria was associated with the early detection of renal damage from hypertension.35 This difference may be due to the occurrence of false-negative results since antibody-based dipstick was employed in the detection of micro-albuminuria. To conclude if micro-albuminuria can predict early kidney damage in the hypertensive population, it needs further study using more sensitive urine assays.
Limitations of the Study
The current study makes a unique contribution to the existing literature on assessing the magnitude of LVH and identifying its determinants for patients with uncontrolled hypertension by exclusively focusing on patients who had no prior identified hypertension complications seeking healthcare. Also, it assesses the association between LVH and uncontrolled BP, medication adherence, lifestyle modifications, number of antihypertensive drugs and other demographic and clinical characteristics. However, certain limitations should be considered. Since cross-sectional study design was employed temporal relationship between the outcome and explanatory variables could not be established. It was also difficult to standardize local drinks and the amount of salt added to meals that subjectivity may affect the result. BP measures could be underestimated or overestimated, given that the BP monitoring parameter used was more of the values from their BP records on charts. However, in this study re-measuring, BP by experienced nurses and taking an average of three consecutive follow-up BP measurements could offset this limitation.
Conclusions
In the current study, it was found that nearly two-thirds of hypertensive patients uncontrolled BP and more than one-third of participants had developed LVH. Patients with poor adherence to salt restriction and medications and those who were on triple antihypertensive drugs were found to be predictors of uncontrolled BP. Moreover, abdominal obesity, age of 60 years or older and uncontrolled BP were predictors of LVH. More than half (53%) of participants were on at least two antihypertensive drug combinations of different classes. Therefore, tailored interventions targeting BP control to reduce the magnitude of LVH and other early complications of hypertension deemed to be compulsory.
Abbreviations
ACEIs, angiotensin converting enzyme inhibitors; AOR, adjusted odds ration; ARBs, angiotensin receptor blockers; ACSH, Ayder Comprehensive Specialized Hospital; BMI, body mass index; BMQ, Brief Medication Questionnaire; BP, blood pressure; CCBs, calcium channel blockers; DM, diabetes mellitus; DASH, Dietary Approach to Stop Hypertension; ECG, electrocardiograph; ERB, Ethics Review Board; HF, heart failure; HHD, hypertensive heart disease; JNC 8, Joint National Committee 8; LVH, left ventricular hypertrophy; MI, myocardial infarction; NHANES, National Health and Nutrition Examination Survey; NCD, non-communicable diseases; PAD, peripheral arterial diseases; SPSS, Statistical Package for Social Sciences.
Data Sharing Statement
All data used in this study supplied with the manuscript and supplementary data can be obtained from the corresponding author upon request when needed.
Ethics Approval
Ethical clearance and approval were obtained from the Institutional Review Board (IRB) of Mekelle University prior to data collection. Subsequently, support letter was secured to the medical director of Mekelle University Comprehensive Specialized Hospital (MU-CSH). The methods were carried out in accordance with the relevant guidelines and regulations of the IRB of the University. Our study was conducted in accordance with the Declaration of Helsinki. Written informed consent was obtained from each participant before conducting this study. Participants’ information obtained was kept confidential. The right of patients to withdraw or not to participate was respected. Before commencing the study, the aim of the study was explained for each participant. Privacy and confidentiality were kept by eliminating identifiers and curbing data access, respectively.
Acknowledgments
We would like to thank the Office of the Postgraduate Programs of Mekelle University for giving the educational opportunity and Aksum University for granting study leave. Our appreciation also goes to all data collectors and study participants.
Author Contributions
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Funding
There is no funding to report.
Disclosure
The authors declare that they have no competing interests.
References
1. Christopher J L Murray, Mohammad H Forouzanfar, Lily Alexander, H Ross Anderson, Victoria F Bachman, Stan Biryukov, et al. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks in 188 countries, 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;386(10010):2287–323.
2. Benjamin EJ, Blaha MJ, Chiuve SE, et al. Heart disease and stroke statistics-2017 update: a report from the American Heart Association. circulation. 2017;135(10):e146e603.
3. Abdissa SG, Feleke Y, Awol M. Prevalence of hypertension and pre-hypertension in Addis Ababa, Ethiopia: A survey done in recognition of World Hypertension Day, 2014. EJHD. 2015;29.
4. Mengistu MD. Pattern of blood pressure distribution and prevalence of hypertension and prehypertension among adults in Northern Ethiopia: disclosing the hidden burden. BMC Cardiovasc Disord. 2014;14(1):33. doi:10.1186/1471-2261-14-33
5. Hansson L, Zanchetti A, Carruthers SG, et al. Effects of intensive blood-pressure lowering and low-dose aspirin in patients with hypertension: principal results of the Hypertension Optimal Treatment (HOT) randomised trial. Lancet. 1998;351(9118):1755–1762. doi:10.1016/S0140-6736(98)04311-6
6. Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL
7. Mancia G, De Backer G, Dominiczak A, et al. ESH-ESC practice guidelines for the management of arterial hypertension: ESH-ESC task force on the management of arterial hypertension. J Hypertens. 2007;25(9):1751–1762. doi:10.1097/HJH.0b013e3282f0580f
8. Xin X, He J, Frontini MG, Ogden LG, Motsamai OI, Whelton PK. Effects of alcohol reduction on blood pressure: a meta-analysis of randomized controlled trials. Hypertension. 2001;38(5):1112–1117. doi:10.1161/hy1101.093424
9. Asgedom SW, Gudina EK, Desse TA. Assessment of blood pressure control among hypertensive patients in Southwest Ethiopia. PLoS One. 2016;11(11):e0166432. doi:10.1371/journal.pone.0166432
10. Lichisa G, Tegegne G, Gelaw B, Defersha A, Woldu M, Linjesa J. Blood pressure control and its contributing factor among ambulatory hypertensive patients in Adama Hospital medical college, East Shoa, Adama, Ethiopia. Int J Pharm Biol Sci Res Development. 2014;2:7.
11. Elmehdawi RR, Albarsha A. Pattern of antibiotic prescription to hospitalized patients in a teaching hospital in Benghazi-Libya. Libyan J Infect Dis. 2008;2:29–34.
12. Shimbo D, Muntner P, Mann D, et al. Association of left ventricular hypertrophy with incident hypertension: the multi-ethnic study of atherosclerosis. Am J Epidemiol. 2011;173(8):898–905. doi:10.1093/aje/kwq509
13. Weber MA, Schiffrin EL, White WB, et al. Clinical practice guidelines for the management of hypertension in the community: a statement by the American Society of Hypertension and the International Society of Hypertension. j Clin Hypertension. 2014;16(1):14–26. doi:10.1111/jch.12237
14. Svarstad BL, Chewning BA, Sleath BL, Claesson C. The brief medication questionnaire: a tool for screening patient adherence and barriers to adherence. Patient Educ Couns. 1999;37(2):113–124. doi:10.1016/S0738-3991(98)00107-4
15. Gebremichael GB, Berhe KK, Zemichael TM. Uncontrolled hypertension and associated factors among adult hypertensive patients in Ayder comprehensive specialized hospital, Tigray, Ethiopia, 2018. BMC Cardiovasc Disord. 2019;19(1):121. doi:10.1186/s12872-019-1091-6
16. James PA, Oparil S, Carter BL, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA. 2014;311(5):507–520. doi:10.1001/jama.2013.284427
17. He J, Whelton PK, Appel LJ, Charleston J, Klag MJ. Long-term effects of weight loss and dietary sodium reduction on incidence of hypertension. Hypertension. 2000;35(2):544–549. doi:10.1161/01.HYP.35.2.544
18. Whelton SP, Chin A, Xin X, He J. Effect of aerobic exercise on blood pressure: a meta-analysis of randomized, controlled trials. In: Database of Abstracts of Reviews of Effects (DARE): Quality-Assessed Reviews. The University of York, Centre for Reviews and Dissemination, United Kingdom; 2002. Accessed from: https://www.ncbi.nlm.nih.gov/books/NBK69571/
19. Alfakih K, Walters K, Jones T, Ridgway J, Hall AS, Sivananthan M. New gender-specific partition values for ECG criteria of left ventricular hypertrophy: recalibration against cardiac MRI. Hypertension. 2004;44(2):175–179. doi:10.1161/01.HYP.0000135249.66192.30
20. Toto RD. Microalbuminuria: definition, detection, and clinical significance. j Clin Hypertension. 2004;6:2–7. doi:10.1111/j.1524-6175.2004.4064.x
21. Gu Q, Burt VL, Dillon CF, Yoon S. Trends in antihypertensive medication use and blood pressure control among United States adults with hypertension: the national health and nutrition examination survey, 2001 to 2010. Circulation. 2012;126(17):2105–2114. doi:10.1161/CIRCULATIONAHA.112.096156
22. Banegas JR, Segura J, Ruilope LM, et al. Blood pressure control and physician management of hypertension in hospital hypertension units in Spain. Hypertension. 2004;43(6):1338–1344. doi:10.1161/01.HYP.0000127424.59774.84
23. Goverwa TP, Masuka N, Tshimanga M, et al. Uncontrolled hypertension among hypertensive patients on treatment in Lupane District, Zimbabwe, 2012. BMC Res Notes. 2014;7(1):703. doi:10.1186/1756-0500-7-703
24. Adebolu FA, Naidoo M. Blood pressure control amongst patients living with hypertension presenting to an urban district hospital outpatient clinic in Kwazulu-Natal. African j Primary Health Care Family Med. 2014;6(1):1–6. doi:10.4102/phcfm.v6i1.572
25. Iloh GU, Ofoedu JN, Njoku PU, Amadi AN, Godswill-Uko EU. Medication adherence and blood pressure control amongst adults with primary hypertension attending a tertiary hospital primary care clinic in Eastern Nigeria. African j Primary Health Care Family Med. 2013;5:1. doi:10.4102/phcfm.v5i1.446
26. Mutua EM, Gitonga MM, Mbuthia B, Muiruri N, Cheptum JJ, Maingi T. Level of blood pressure control among hypertensive patients on follow-up in a regional referral hospital in Central Kenya. Pan Afr Med J. 2014;18.
27. Elperin DT, Pelter MA, Deamer RL, Burchette RJ. A large cohort study evaluating risk factors associated with uncontrolled hypertension. J Clin Hypertension. 2014;16(2):149–154. doi:10.1111/jch.12259
28. Onwukwe SC, Omole OB. Drug therapy, lifestyle modification and blood pressure control in a primary care facility, south of Johannesburg, South Africa: an audit of hypertension management. South African Family Practice. 2012;54(2):156–161. doi:10.1080/20786204.2012.10874196
29. Whelton PK, Appel LJ, Espeland MA, Applegate WB, Ettinger, Jr WH
30. Cushman WC, Ford CE, Cutler JA, et al. Original papers. Success and predictors of blood pressure control in diverse north american settings: the antihypertensive and lipid‐lowering treatment to prevent heart attack trial (ALLHAT). J Clin Hypertension. 2002;4(6):393–404. doi:10.1111/j.1524-6175.2002.02045.x
31. Fretheim A, Odgaard-Jensen J, Brørs O, et al. Comparative effectiveness of antihypertensive medication for primary prevention of cardiovascular disease: systematic review and multiple treatments meta-analysis. BMC Med. 2012;10(1):33. doi:10.1186/1741-7015-10-33
32. Lozano JV, Redön J, Cea-Calvo L, et al. Left ventricular hypertrophy in the Spanish hypertensive population. The ERIC-HTA study.Spanish Journal of Cardiology. 2006;59(2):136–142.
33. Salako BL, Ogah OS, Adebiyi AA, et al. Blood pressure control and left ventricular hypertrophy in hypertensive Nigerians. Ann Afr Med. 2009;8:3.
34. Heart N, Lung; Institute B, Diabetes NIO, Digestive; Diseases K. Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults: the evidence report. National Heart Lung Blood Inst. 1998.
35. Jensen JS, Feldt-Rasmussen B, Strandgaard S, Schroll M, Borch-Johnsen K. Arterial hypertension, microalbuminuria, and risk of ischemic heart disease. Hypertension. 2000;35(4):898–903. doi:10.1161/01.HYP.35.4.898
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.