Back to Journals » International Journal of Nanomedicine » Volume 10 » Supplement 1 Challenges in biomaterials research
Biodegradation and cytotoxicity of ciprofloxacin-loaded hydroxyapatite-polycaprolactone nanocomposite film for sustainable bone implants
Authors Nithya R, Sundaram NM
Received 19 January 2015
Accepted for publication 18 March 2015
Published 1 October 2015 Volume 2015:10(Supplement 1 Challenges in biomaterials research) Pages 119—127
DOI https://doi.org/10.2147/IJN.S79995
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Thomas Webster
Rajendran Nithya, Nachiappan Meenakshi Sundaram
Department of Biomedical Engineering, PSG College of Technology, Coimbatore, India
Introduction: In recent years there has been a steep increase in the number of orthopedic patients for many reasons. One major reason is osteomyelitis, caused by pyrogenic bacteria, with progressive infection of the bone or bone marrow and surrounding tissues. So antibiotics must be introduced during bone implantation to avoid prolonged infection.
Aim: The objective of the study reported here was to prepare a composite film of nanocrystalline hydroxyapatite (HAp) and polycaprolactone (PCL) polymer loaded with ciprofloxacin, a frequently used antibiotic agent for bone infections.
Methods: Nanocrystalline HAp was synthesized by precipitation method using the precursor obtained from eggshell. The nanocomposite film (HAp-PCL-ciprofloxacin) was prepared by solvent evaporation. Drug-release and biodegradation studies were undertaken by immersing the composite film in phosphate-buffered saline solution, while a cytotoxicity test was performed using the fibroblast cell line NIH-3T3 and osteoblast cell line MG-63.
Results: The pure PCL film had quite a low dissolution rate after an initial sharp weight loss, whereas the ciprofloxacin-loaded HAp-PCL nanocomposite film had a large weight loss due to its fast drug release. The composite film had higher water absorption than the pure PCL, and increasing the concentration of the HAp increased the water absorption. The in vitro cell-line study showed a good biocompatibility and bioactivity of the developed nanocomposite film.
Conclusion: The prepared film will act as a sustainable bone implant in addition to controlled drug delivery.
Keywords: osteomyelitis, antibiotics, nanocrystalline, cytotoxicity, fibroblast, in vitro
Introduction
Osteomyelitis refers to a bone infection, almost always caused by bacteria. Over time, the result can be destruction of the bone itself.1 Ciprofloxacin is a broad-spectrum fluoroquinolone antibacterial agent used in the treatment of osteomyelitis caused by pathogens like Staphylococcus aureus and Pseudomonas aeruginosa.2 A high concentration of the drug is required for 5 weeks to several months to cure the bone infection. Thus, local drug delivery would be advantageous and reduce the side effects that occur due to high dosage of the drug.3
Compared with metal, metal alloy, and ceramic bone-substitute materials, organic/inorganic composite structures are best suited to orthopedic biomaterials as their properties closely mimic those of natural bone.4 A novel method for the preparation of ceramic/polymer composites is required to combine the advantages of the bioactive, biodegradable, and biological properties of scaffolds for bone regeneration. The development of organic/inorganic composites as orthopedic materials has attracted much attention during the last few years.
Natural bone is composed of inorganic compound (hydroxyapatite [HAp] 65% on the nanoscale) and organic compounds (collagen matrix 35%). Hence, to mimic natural bone and to maintain biocompatibility, a polymer/ceramic material would be ideal for bone drug delivery. The inorganic HAp is an important component of natural bone tissue. It is attractive for use in synthetic bone-tissue scaffolds as a means of more closely mimicking natural tissue composition.3 The polymer chosen for drug delivery should be biodegradable and biocompatible. Polycaprolactone (PCL) is a biodegradable, bio-resorbable polymer used for drug formulations and medical purposes. It is an ideal polymer for the application of drug or biomolecule delivery, as it has a relatively low degradation rate that extends over 1 year. The US Food and Drug Administration has approved PCL as it is ideal for a number of medical and drug-delivery devices.5
Ahola et al investigated in vitro bone filling composite materials that release ciprofloxacin to kill any remaining bacteria and that contain bio-ceramic to help the bone to heal.6 Kim et al developed an HAp porous scaffold coated with HAp and PCL composite and entrapped the antibiotic drug tetracycline hydrochloride within the coating layer.5 They found that the release rate of the drug was sustained for prolonged periods and was highly dependent on the degree of coating dissolution, suggesting the possibility of controlled drug release from the porous scaffold with HAp-PCL coating.5
In the work presented here, a composite film of nanoscale HAp, prepared from eggshell, and PCL was prepared and loaded with ciprofloxacin for drug delivery to bones. The phase composition and morphology of the developed nanocomposite were studied by X-ray diffraction (XRD), transmission electron microscopy (TEM), and Fourier-transform infrared (FTIR) spectroscopy. The drug-release study was done in vitro and its absorbance value was measured using a UV-visible spectrophotometer. The degradation of the composite film was studied by immersing it in phosphate-buffered saline (PBS) for 7 days. Cytotoxicity studies were performed in a fibroblast cell line, and cell proliferation was examined in an osteoblast cell line.
Methods
Synthesis of HAp from eggshell
Apart from standard calcium salts, HAp can also be produced from some natural sources of calcium like sea corals,7 eggshell,8 sea shells,9 and also from body fluids.10 The utilization of calcium from a natural source minimizes the chances of impurities like silica being present in the finished product. Moreover, the cost of production can be reduced, as there will be no need to purify.
An important aspect in the development of methods for the synthesis of HAp is the use of raw materials from unconventional sources. The world’s egg production was estimated to be approximately 6.37×107 tons in 2010.11 Taking into account that the shell comprises about 11% of the weight of each egg, the amount of eggshell produced in the world in the last year ascends to about 7×106 tons.12 Though eggshells are occasionally used as a fertilizer due to their high calcium and nitrogen content, most are discarded as waste. By utilizing this organic waste, the cost of a high-quality calcium source for preparation of HAp is reduced, and, at the same time, the recycling of a waste product of human daily activity can also be taken care of, underscoring the importance of using eggshell as a calcium source.13,14
Eggshell is composed of calcium carbonate, which acco-unts for around 94% of the total weight; calcium phosphate (1%); organic matter (4%); and magnesium carbonate (1%).15
HAp from eggshell was synthesized via a precipitation and low-combustion method that was lengthy, complicated, and required pH control and adjustment. The eggshells were cleaned manually with de-ionized water then boiled in water for 30 minutes. The uncrushed and washed eggshells were placed in a porcelain crucible and calcined in a Kanthal™ wire heating furnace for 2 hours to decompose organic matter and to convert the calcium carbonate to calcium oxide. The product was then finely ground with a pestle in an agate mortar.
The eggshells are transformed into calcium oxide and carbon dioxide evolves above 900°C . The expected reaction is presented in Equation 1.
CaCO3 | (1) |
A stoichiometry amount of calcined eggshell (1 M) was dispersed in 50 mL of distilled water. After dispersing in distilled water, the CaO converted into Ca(OH)2, as shown in Equation 2.
CaO + H2O | (2) |
Under rigorous stirring, reagent-grade orthophosphoric acid solution (0.6 M) was added in drops at a controlled rate to the suspension at room temperature. Initially, the pH of the solution was found to be 12, but at the end of the addition of orthophosphoric acid, it had decreased to 8.5 and a precipitate had formed. The precipitate was subjected to aging treatment for 24 hours. The solution was then stirred for another 30 minutes without heating and then left for another 10 hours for complete precipitation occur. The precipitate was filtered and thoroughly washed with distilled water before being filtered again. Finally, after drying at 80°C for 3 hours, the precipitate was calcined at 900°C for 2 hours.
Preparation of ciprofloxacin-loaded HAp-PCL nanocomposite film
The ciprofloxacin loading of the HAp-PCL nanocomposite film was undertaken as follows. Initially, ciprofloxacin was dissolved in dichloromethane for 1 hour, then HAp powder, prepared from eggshell, was added to the solution and the mixture stirred for 6 hours at room temperature. During this process, the drug concentration was adjusted to 75% w/w with respect to HAp-PCL.16 Lastly, PCL pellets were added and the suspension was stirred for 12 hours to prepare the drug-loaded HAp-PCL solution (Figure 1). The PCL film is prepared by dissolving 1.5 % w/v PCL pellets into dichloromethane. Then the mixture is poured into a glass petri dish and dried under ambient conditions.
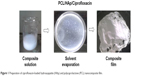  | Figure 1 Preparation of ciprofloxacin-loaded hydroxyapatite (HAp) and polycaprolactone (PCL) nanocomposite film. |
PCL of 1.5% w/v was dissolved in dichloromethane. The HAp and PCL were maintained at the ratio of 1:1. The mixture was poured into a glass petri dish and dried under ambient conditions for 24 hours to obtain the composite film.17,18
In vitro degradation tests
As a medium for in vitro degradation tests, PBS (pH 7.4) was used. The PCL film and drug-loaded film were weighed and incubated in 30 mL of PBS at 37°C for a period of 7 days. The medium was refreshed every 1 hour for the first 5 hours, and then every 24 hours thereafter. At predetermined periods of time, the samples were taken out, blotted on a filter paper, and weighed using a balance.
The water uptake was obtained by determining the weight difference between the sample initially and the wet sample (Wwet/Winitial).
The material degradation was obtained by determining the weight difference between the sample initially and the sample after drying; [1− (Wdry/Winitial)].19
In vitro drug-release studies
In vitro drug-release studies were conducted to estimate the rate of drug release from the drug-loaded film and to find the concentration of the drug released at particular times. PBS (pH 7.4) was used as the medium for the in vitro drug-release tests. The drug-loaded film was immersed in a glass vessel containing medium and incubated at 37°C and pH 7.4 for periods of up to 7 days. The drug-release studies were performed by directly immersing the films into the beaker containing distilled water. At frequent time intervals, 3 mL of sample was extracted and analyzed with a UV-visible spectrophotometer.20
Diffusion studies were carried out using dialysis membrane. The film was placed to one end of the dialysis tube, then the dialysis tube was placed in a beaker containing 100 mL distilled water/PBS so that the film was dipped in the water/PBS. The beaker was then placed on a magnetic stirrer. 5 mL of sample is withdrawn from the beaker and the concentration of drug in each sample is estimated using UV-Visible spectrophotometer at 271 nm. An equal volume of fresh distilled water/PBS is replaced after withdrawal of each sample.
Cytotoxicity testing
Although biologically acceptable ingredients were present in the final form of the composite, the problem of non-biocompatibility could have arisen due to the presence of trace amounts of solvents and/or monomers released from the polymer, or due to processing factors. Thus, the biocompatibilities of the nanocomposite scaffolds were studied by in vitro cell culture by employing the fibroblast cell line NIH-3T3 and osteoblast cell line MG-63.21,22
Cell growth on the surface, and cell migration into the pores, of the composite, if any, and cell morphology and attachment all indicated the biocompatibility and suitability of the material for in vivo use. Cellular responses (eg, cell proliferation) of the nanoscale HAp filled PCL composites were assessed by means of 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay using the fibroblast cell line NIH-3T3 and osteoblast cell line MG-63 obtained from the National Center for Cell Science, Pune, India. Three samples per group are evaluated for all experiments. Cells were cultured in Dulbecco’s Modified Eagle’s Medium supplemented with 10% fetal bovine serum, containing L-glutamine, penicillin, and streptomycin. Cells were trypsinized and resuspended in fresh media before being seeded onto the sample surfaces in a 24-well plate at a density of 1×104 well. Then 1 mL of McCoy’s 5A medium (with L-glutamine, without phenol red or sodium bicarbonate) supplemented with 5% fetal calf serum and 5% bovine calf serum was added to each well. The cells were maintained at 37°C in an atmosphere of 5% CO2 and 95% air, and the culture medium was changed every day without disturbing the cell monolayer.
MTT assay (Sigma-Aldrich Co, St Louis, MO, USA) was performed to assess cell proliferation on the sample surface. An MTT solution was prepared by adding 5 mg of MTT in 1 mL PBS (5 mg/mL) then filter-sterilized. The MTT was diluted (50 μL into 450 μL) in serum-free, phenol red-free Dulbecco’s Modified Eagle’s Medium. The diluted MTT solution (500 μL) was then added to each sample in 24-well plates. After 2 hours of incubation, 500 μL of solubilization solution, containing 10% Triton™ X-100, 0.1 N HCl, and isopropanol, was added to dissolve the formed purple formazan crystals from the MTT that had been reduced by the active mitochondria of viable cells. A volume of 100 μL of the resulting supernatant was transferred into a 96-well plate and read at 570 nm at a bench-top microplate reader (MAKE). Cell densities on samples were measured after 1, 3, and 7 days. Data are presented as mean ± standard deviation.23 Cells were cultured (100,000 cells/disc) in a 6.3 cm2 petri dish, as shown in Figure 2.
  | Figure 2 Phase contrast microscopy of morphology of cultured NIH-3T3 cells. |
Results and discussion
XRD
Figure 3 shows the XRD pattern of HAp recorded using a Siemens D5000 diffractometer (Siemens AG, Berlin and Munich, Germany) with CuKα radiation (λ=0.154 nm). The diffractometer was operated at 40 kV and 30 mA at a 2 theta range of 4°–90° employing a step size of 0.1° and a 0.60-second exposure. The peaks of HAp appearing at 26.2°, 32.2°, 49.6°, and 64.0° (2θ) correspond to the 002, 211, 123, and 304 reflection planes.
  | Figure 3 X-ray diffraction pattern of nano hydroxyapatite. |
The XRD pattern of the HAp powder obtained is in good in agreement with the XRD pattern of a HAp standard available from the Joint Committee on Powder Diffraction Standards (JCPDS; standard number 84-1998). The XRD pattern possesses a strong peak at around 32.2° corresponding to the 211 plane of HAp’s crystalline structure.
No other characteristic peaks corresponding to other calcium phosphate phases or impurities were observed. From the peaks of the XRD diffraction pattern, the prepared HAp samples are in hexagonal space group. (JCPDS 84-1998).
FTIR
The structure of the ciprofloxacin loaded HAp-PCL nanocomposite film was analyzed using FTIR spectroscopy, as shown in Figure 4. The spectrum is recorded in the range of 4,000–400 cm−1 for all the samples. Figure 5 shows the FTIR spectrum of synthesized HAp. The representative FTIR spectrum shows all characteristic absorption peaks of HAp. The first indication of the formation of HAp is the strong, complex, broad FTIR band centered around 1,000–1,100 cm−1 due to the asymmetric stretching mode of vibration of the PO4 group. As a major peak of the phosphate group, the n3 vibration peak could be identified in the region between 1,100 and 960 cm−1 for both powders, which was due to the asymmetric stretching of P-O in PO43−. The presence of the peak in the region 1,400–1,450 cm−1 is due to absorbed carbon dioxide. The crystalline powder generated two characteristic stretching modes of O-H bands at about 3,497 cm−1 which are noticed in all FTIR spectra of HAp.
  | Figure 4 Fourier-transform infrared spectrum of ciprofloxacin loaded hydroxyapatite (HAp)-polycaprolactone (PCL) nanocomposite film. |
  | Figure 5 Fourier-transform infrared spectrum of hydroxyapatite. |
For ciprofloxacin, one prominent characteristic peak was found between 3,500 and 3,450 cm−1, which was attributed to the stretching vibration of the OH group and intermolecular hydrogen bonding (Figure 4).
Another band at 3,000–2,950 cm−1 represents the alkenes and aromatic C-H stretching, mainly υ = C-H. The peak at 2,900 cm−1 was assigned to the C-H stretching vibration of the cyclopropyl group. The 1,950–1,450 cm−1 region exhibited FTIR absorption from a wide variety of double-bonded functional groups. The band at 1,750–1,700 cm−1 represented carbonyl C=O stretching. The peak at 1,650–1,600 cm−1 was assigned to quinolones. The band at the 1,450–1,400 cm−1 represents C-O and that at 1,300–1,250 cm−1 suggests the bending vibration of the O-H group, proving the presence of carboxylic acid.
The FTIR spectrum of the nanocomposite film shows all the characteristic peaks of HAp and ciprofloxacin along with those of PCL – 2,972, 2,868, and 1,723 cm−1, which were assigned to the vibration of the –CH2 and –C=O bonds, respectively.
TEM
A JEM2100 microscope operating at 100 kV is employed to study the morphologies of the prepared samples. The sample for TEM was prepared by dispersing a small amount of the sample in ethanol and sonication for 30 minutes. A few drops of the resultant suspension are dropped on to a copper grid. The results from energy-dispersive X-ray spectroscopy (EDAX)-coupled TEM show that the obtained samples had stoichiometric HAp and exhibited characteristic nanorods and spherical nanoparticles.
The TEM image in Figure 6A demonstrates that the HAp was in the submicron to nanosize range, with all particles in the longest dimensions of 50–100 nm. The larger crystals may have been formed due to the lower number of crystal nucleation sites because of the rapid addition of Ca+ in PO4−.
  | Figure 6 Transmission electron microscopy image (A), and energy-dispersive X-ray spectroscopy and SAD (B) of hydroxyapatite. |
The EDAX results (Figure 6B) confirm the existence of the elements such as Ca, P, and O. The atomic ratio was in agreement with that of calcium-rich HAp.
In vitro degradation studies
In vitro degradation study was carried out for pure PCL film and the ciprofloxacin-loaded HAp-PCL film for 7 days. Data are presented as mean ± standard deviation.
Figure 7A shows the weight loss (in grams) versus immersion time (hours) of both films. The pure PCL film had quite a low dissolution rate after an initial sharp weight loss. The ciprofloxacin-loaded HAp-PCL nanocomposite film had a large weight loss due to its fast drug release. In the beginning, the dry film absorbed more water and this could not be removed completely. So, due to the absorbed water, we had negative weight loss in the beginning.
Figure 7B shows the water absorption capacity of the films with and without the addition of HAp and ciprofloxacin. For the drug-loaded HAp-PCL nanocomposite film, the water absorption showed an initial sharp increase within a short period (12 hours), then a maximum and subsequent drop, and further slowing of the rate. For pure PCL, after a initial sharp increase, a steady and gradual increase with time was observed. The composite film had higher water absorption than the pure PCL, and increasing the HAp content increased the water absorption for all periods.
In vitro drug release from ciprofloxacin-loaded composite film
The absorbance values of the drug-loaded composite film placed in the dialysis membrane was measured from filtrate dilutions of PBS. The maximum wavelength (λmax), obtained by scanning all samples from 200 to 400 nm, was found to be 272 nm. The drug release was studied for a prolonged period and the absorbance value was found to be constant. Figure 8 shows the drug-release kinetics, which were burst in the initial period and sustained later. The same procedure was repeated at 37°C and the results showed a large amount of drug was released compared with the amount of drug released at room temperature.
  | Figure 8 Drug-release profile of ciprofloxacin in phosphate-buffered saline (PBS) for prolonged periods at room temperature (RT) and at 37°C. |
Fibroblast attachment and proliferation
The control cells (Figure 9) grew on the surface of a cultivation dish, and during 24 hours of incubating, a monolayer was formed. Figure 10 shows the significant morphology and cell number changes that occurred within 96 hours of the extracts influence.
  | Figure 9 Phase contrast microscopy of cells attached onto composite film at 24 hours. |
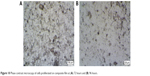  | Figure 10 Phase contrast microscopy of cells proliferated on composite film at (A) 72 hours and (B) 96 hours. |
The effects of the composite on NIH-3T3 cell viability measured by MTT assay is shown in Figure 11. MTT is a yellow, water-soluble tetrazolium dye, which is reduced by live cells to a purple formazan product insoluble in aqueous solutions. The amount of formazan generated is directly proportional to the number of viable cells.
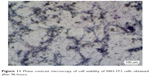  | Figure 11 Phase contrast microscopy of cell viability of NIH-3T3 cells obtained after 96 hours. |
The cell viability of the prepared ciprofloxacin-loaded HAp-PCL nanocomposite film was measured with the help of fibroblast cells. NIH-3T3 cells were found to be present in large numbers around the sample. This implies that the test materials did not show any detectable toxic zone around or under the specimen.
The cell proliferation rate depends on various chemical and physical aspects of a material, such as composition, roughness, porosity, morphology, and surface energy. The maximum cell density (1×104 cells in an area of 6.3 cm2) was observed after 24 hours of culture. Thus, from the cytotoxicity results it can be said that the HAp-PCL composite film is less cytotoxic than pure PCL film. This implies that the presence of a more bioactive/resorbable phase lowers the cytotoxicity.
From Figure 12, it can be seen that the differentiation rate of MG-63 cells on the composite film was much higher than on pure PCL film, indicating that the composite film could accelerate the differentiation of MG-63 cells.
Conclusion
A key issue is that it is very complex replacing damaged bone, as fast as possible, with a new mature bone. In this work, an organic–inorganic composite material suitable for bone-tissue engineering based on HAp and PCL was studied. The nanoscale HAp obtained from eggshell had good agreement with natural HAp. The nanoscale HAp and PCL were blended together in an organic solvent to form a composite film. The obtained scaffold presented suitable forms for filling bone defects. Furthermore, the in vitro tests revealed that the processed scaffold has the potential for use in drug-delivery systems. The biodegradation and cytotoxicity studies prove that the prepared ciprofloxacin-loaded HAp-PCL nanocomposite film would be suitable for sustainable bone implants, as it had good interaction with the natural tissue and cells and degradation of the polymer helps with drug release and in avoiding a second surgery.
Acknowledgment
The authors are thankful to the principal and management of PSG College of Technology, Coimbatore, Tamil Nadu, India, for providing facilities to carry out this research. This work was partially supported by the University Grants Commission (Major) [file number 42-907/2013(SR)] and Department of Science and Technology - Science and Engineering Research Board (number SB/S2/CMP-106/2013), New Delhi, India.
Disclosure
The authors declare no conflicts of interest in this work.
References
Schlickewei CW, Yarar S, Rueger JM. Eluting antibiotic bone graft substitutes for the treatment of osteomyelitis in long bones. A review: evidence for their use? Orthop Res Rev. 2014;6:71–79. | ||
Liu H, Webster TJ. Mechanical properties of dispersed ceramic nanoparticles in polymer composites for orthopedic applications. Int J Nanomedicine. 2010;5:299–313. | ||
Devanand Venkatasubbu G, Ramasamy S, Ramakrishnan V, Kumar J. Nanocrystalline hydroxyapatite and zinc-doped hydroxyapatite as carrier material for controlled delivery of ciprofloxacin. 3 Biotech. 2011;1(3):173–186. | ||
Hutmacher DW. Scaffolds in tissue engineering bone and cartilage. Biomaterials. 2000;21(24):2529–2543. | ||
Kim HW, Knowles JC, Kim HE. Hydroxyapatite/poly(epsilon-caprolactone) composite coatings on hydroxyapatite porous bone scaffold for drug delivery. Biomaterials. 2004;25(7–8):1279–1287. | ||
Ahola N, Männistö N, Veiranto M, et al. An in vitro study of composites of poly(L-lactide-co-ε-caprolactone), β-tricalcium phosphate and ciprofloxacin intended for local treatment of osteomyelitis. Biomatter. 2013;3(2):e23162. | ||
Samur R, Ozyegin L, Agaogullari D, et al. Calcium phosphate formation from sea urchin- (Brissus latecarinatus) via modified mechano-chemical (ultrasonic) conversion method. Metalurgija. 2013;52(3):375–378. | ||
Gergely G, Wéber F, Lukács I, et al. Preparation and characterization of hydroxyapatite from eggshell. Ceram Int. 2010;36(2):803–806. | ||
Eddy G, Poinern J, Fawcett D. The manufacture of a novel 3D hydroxyapatite microstructure derived from cuttlefish bones for potential tissue engineering applications. American Journal of Materials Science. 2013;3(5):130–135. | ||
Chavan PN, Bahir MM, Mene RU, Mahabole MP, Khairnar RS. Study of nanobiomaterial hydroxyapatite in simulated body fluid: formation and growth of apatite. Mater Sci Eng B Solid State Mater Adv Technol. 2010;168(2010):224–230. | ||
The Poultry Site [webpage on the Internet]. Global poultry trends. 2010. Available from http://www.thepoultrysite.com/reports/?id=1025. Accessed 21 April 2015. | ||
Hui P, Meena SL, Singh G, Agarawal RD, Prakesh S. Synthesis of hydroxyapatite bio-ceramic powder by hydrothermal method. Journal of Minerals and Materials Characterization and Engineering. 2010;9(8):683–692. | ||
Prabakaran K, Balamurugan A, Rajeswari S. Development of calcium phosphate based apatite from hen’s eggshell. Bulletin of Materials Science. 2005;28(2):115–119. | ||
Sanosh KP, Chu MC, Balakrishnan A, Kim TN, Cho SJ. Utilization of biowaste eggshells to synthesize Nanocrystalline hydroxyapatite powders. Mater Lett. 2009;63(24–25):2100–2102. | ||
Siva Rama Krishna D, Siddharthan A, Seshadri SK, Sampath Kumar TS. A novel route for synthesis of nanocrystalline hydroxyapatite from eggshell waste. J Mater Sci Mater Med. 2007;18(9):1735–1743. | ||
Elliot JC. Structure and Chemistry of the Apatites and Other Calcium Orthophosphates. Amsterdam: Elsevier; 1994. | ||
Chuenjitkuntaworn B, Inrung W, Damrongsri D, Mekaapiruk K, Supaphol P, Pavasant P. Polycaprolactone/hydroxyapatite composite scaffolds: preparation, characterization, and in vitro and in vivo biological responses of human primary bone cells. J Biomed Mater Res A. 2010;94(1):241–251. | ||
Chen J, Luo Y, Hong L, et al. Synthesis, characterization and osteoconductivity properties of bone fillers based on alendronate-loaded poly(ε-caprolactone)/hydroxyapatite microspheres. J Mater Sci Mater Med. 2011;22(3):547–555. | ||
Macedo FA, Nunes EH, Vasconcelos WL, Santos RA, Sinisterra RD, Cortes ME. A biodegradable porous composite scaffold of PCL/BCP containing Ang-(1–7) for bone tissue engineering. Cerâmica. 2012;58(348):481–488. English and Portuguese. | ||
Kumar NA, Kumar SK. Hydroxyapatite–ciprofloxacin minipellets for bone-implant delivery: preparation, characterization, in-vitro drug adsorption and dissolution studies. International Journal of Drug Delivery and Research. 2009;1(1):47–59. | ||
Chatterjee K, Sun L, Chow LC, Young MF, Simon CG Jr. Combinatorial screening of osteoblast response to 3D calcium phosphate/poly(ε-caprolactone) scaffolds using gradients and arrays. Biomaterials. 2011;32(5):1361–1369. | ||
Kumar G, Tison CK, Chatterjee K. The determination of stem cell fate by 3D scaffold structures through the control of cell shape. Biomaterials. 2011;32(35):9188–9196. | ||
Selvakumar M, Jaganathan SJ, Nando GB, Chattopadhyay S. Synthesis and characterization of novel polycarbonate based polyurethane/polymer wrapped hydroxyapatite nanocomposites: mechanical properties, osteoconductivity and biocompatibility. J Biomed Nanotechnol. 2011;10:1–15. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

 CaO + CO2
CaO + CO2

