Back to Journals » Local and Regional Anesthesia » Volume 13
Benefits and Barriers to Increasing Regional Anesthesia in Resource-Limited Settings
Authors Dohlman LE , Kwikiriza A, Ehie O
Received 18 June 2020
Accepted for publication 29 September 2020
Published 22 October 2020 Volume 2020:13 Pages 147—158
DOI https://doi.org/10.2147/LRA.S236550
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Nurten Inan
Lena Ebba Dohlman,1 Andrew Kwikiriza,2 Odinakachukwu Ehie3
1Department of Anesthesiology, Critical Care and Pain Medicine, Massachusetts General Hospital, Boston, MA, USA; 2Department of Anaesthesia and Critical Care, Mbarara Regional Referral Hospital, Mbarara University of Science and Technology, Mbarara, Uganda; 3Department of Anesthesiology and Perioperative Services, University of California San Francisco, San Francisco, CA, USA
Correspondence: Odinakachukwu Ehie
Department of Anesthesiology and Perioperative Services, University of California San Francisco, 1975 4th Street, Suite C2823, San Francisco, CA 94158-3217, USA
Tel +1 415-476-4392
Fax +1 415 476 4926
Email [email protected]
Abstract: Safe and accessible surgical and anesthetic care is critically limited for over half of the world’s population, particularly in Sub-Saharan African and Southeast Asian countries. Increasing the use of regional anesthesia in these areas has potential benefits regarding access, safety, and cost-effectiveness. Perioperative anesthesia-related mortality is significantly higher in resource-limited countries and every effort should be made to encourage the use of anesthetic techniques in these countries that are safest under the present conditions. Studies from Sub-Saharan Africa, although limited in number, have shown a lower risk of death with regional compared to general anesthesia. Regional anesthesia has the further benefit of decreasing the risk of COVID-19 spread to healthcare providers by avoiding the aerosol-generating procedures that occur during general anesthesia. Neuraxial regional anesthesia is relatively easy to teach and perform and is considered the anesthetic of choice for surgeries below the umbilicus in resource-limited settings due to its safety, efficacy, and low cost. Although regional anesthesia has multiple potential advantages, education and training of anesthetic providers in low-and-middle-income countries (LMIC) are a significant barrier to growth. Anesthesia professionals, especially in Sub-Saharan Africa, are often poorly supported and undervalued, and recruitment and retention of adequate numbers of trained practitioners are a continuing problem. Greater use of regional anesthesia could be one way to safely increase anesthesia access and simultaneously create value and enthusiasm for the field. Deficits in anesthesia infrastructure, equipment, and drugs also limit anesthesia capacity in low-and middle-income countries. Ultrasound-guided regional anesthesia may be helpful in improving access to safe and reliable anesthesia in low-resource countries as it continues to become more user-friendly, durable, and affordable.
Keywords: low-resource countries, developing countries, regional anesthesia, ultrasound-guided nerve blocks, anesthesia safety
Introduction
There is a critical lack of access to safe and affordable surgical and anesthetic care for an estimated 4.8 billion people worldwide that is found predominately in low-resource countries (LRCs).1,2 Safe anesthesia care has been particularly slow to develop in many countries in Sub-Saharan Africa and Southeast Asia and is unavailable in most rural district hospitals.3–5 A lack of resources, including trained providers, equipment, and drugs, are largely to blame, but poor adaptive leadership and support also play a role.6 Expanding the use of regional anesthesia in these countries has potential benefits in safety, access, and cost.7–9 In high-resource countries (HRCs), the value of regional anesthesia has been recognized with growing enthusiasm for the past 15 years, but training and adoption of regional techniques have lagged in developing countries despite the many potential benefits that make it particularly suitable for conditions in these countries.10,11 Regional (including neuraxial) anesthesia has been shown to be especially advantageous in obstetric, trauma, and orthopedic patients. These are the very cases that most commonly present for surgery in low-and-middle-income countries (LMICs).12–14 Benefits of using regional rather than general anesthesia include fewer life-threatening perioperative airway and respiratory complications, especially in obstetrical patients and patients with pre-existing lung disease. The use of neuraxial anesthesia has been found to decrease blood loss during orthopedic hip surgery and to lower the incidence of post-operative blood clots after lower limb surgery. Other potential benefits include improved analgesia, a shortened length of stay in post-anesthesia care units (PACU), and increased operating room (OR) efficiency.15–19 These advantages can contribute to a decrease in intensity and cost of care which could help in countries where financial and personnel resources for surgical and anesthetic care are severely restricted. Regional anesthesia is also considered an essential component of multimodal general anesthesia (MGA) by decreasing the stress response to surgery and minimizing the need for opioids and their undesirable side effects through better analgesia.20 Decreasing the need for analgesics should be useful in LMICs where access to opioids is often severely limited for surgical and terminally ill pain patients. According to data from 2016, only 14% of the world’s morphine for pain management is available to 80% of the world’s population. The remaining 86% of morphine is used by a small number of HRCs located mainly in North America, Europe, and Australia. The lowest amount of morphine available to treat patient pain is in the Sub-Saharan region of Africa.21,22 The poor or non-existing access to opioids for pain in LRCs is blamed on overly stringent legal and regulatory restrictions, cultural biases, inflated costs, and misinformation among prescribers and patients.21,23,24 Regional anesthesia can provide an excellent alternative to opioids for pain control whenever the surgical site can be blocked with local anesthetics. With the onset of the COVID-19 pandemic, regional anesthesia has been recommended as preferable to general anesthesia in infected patients. Avoiding general anesthesia decreases the risk of aerosol generation from airway manipulation and the potential for COVID-19 spread, especially among personnel handling the airway.25 This is relevant in LRCs where the supply of healthcare workers is already critically low. The World Health Organization (WHO) recently reported that 10% of all COVID-19 cases globally occur among health workers. As of July 2020, more than 10,000 health workers in Africa have been infected with COVID-19.26 This review will further explore the potential advantages of using neuraxial, peripheral, and other nerve blocks in developing countries and discuss existing barriers that are slowing the implementation of these techniques.
Can Regional Anesthesia Improve Perioperative Safety and Access in Developing Countries?
Perioperative anesthesia-related mortality has been reported in multiple studies to be significantly higher in developing countries than in HRCs. This increased mortality related to anesthesia is considered avoidable, especially in low-risk surgical patients.7,27–31 The reported deaths that are linked to anesthetic care are believed to largely be a result of airway and respiratory problems, and inadequate volume resuscitation during general anesthesia or in the postoperative period.7,12,32,33 An increase in anesthetic mortality in LMICs is not surprising considering the deficiencies of anesthetic equipment, drugs, basic monitors, safety protocols, and well-trained anesthesiologists and anesthetists.4,34 Although resources are slowly improving, it seems reasonable that every effort should be made in these countries to use the anesthetic techniques that are safest under the present conditions. The few studies from developing countries that exist show a lower risk of death in patients receiving regional instead of general anesthesia. The international medical humanitarian organization, Medicins Sans Frontieres (MSF), which provides health care to areas in crisis, published a report in 2016 supporting this statement. Mortality rates from 6 years of anesthetic care at MSF-resourced sites between 2008 and 2014 were analyzed. The all-cause perioperative mortality was 0.25% among 75,536 anesthetics. When compared to general anesthesia with intubation, the perioperative mortality rates were significantly lower with neuraxial (0.04%) and regional (0.06%) anesthesia.35 A review and meta-analysis of maternal complications associated with caesarean sections by Sohby found maternal deaths to be 100 times higher in LMICs than deaths reported in high-income countries.36 The risk of intraoperative complications during caesarean sections (including those attributed to anesthesia) was 17 times as high as in HRCs. Sohby also found high numbers of maternal death in countries with low frequencies of caesarean sections, suggesting lack of access as a contributing cause of increased maternal mortality. A 2016 review and meta-analysis on anesthesia-related maternal mortality in LMICs found a higher risk of death from general anesthesia compared to neuraxial anesthesia.7 Anesthesia was considered responsible for one in seven maternal deaths during or after caesarean sections. General anesthesia compared to neuraxial anesthesia tripled the odds of maternal death and doubled the odds of perinatal death. General anesthesia was also associated with low Apgar scores at 1 and 5 minutes and with an increase in post-partum hemorrhage. In addition, perioperative hemorrhage was responsible for a majority of maternal deaths. Among the anesthetic-attributed deaths in which the underlying cause was reported, 45% were due to airway complications and 31% were from pulmonary aspiration. High spinals accounted for only 6% of deaths.7 This is not surprising as regional anesthetics can provide a surgical field without compromising the airway. In HRCs difficult airway management in operating room settings has improved with better training, equipment, and monitoring.37,38 Unfortunately, the incidence of difficult and failed intubation in the obstetric population has not changed even in HRCs over the past 40 years despite the advances in airway techniques.39 Airway management under general anesthesia in obstetric patients remains riskier than in non-obstetric patients, even when resources and training are available. This is one of the reasons why regional neuraxial techniques continue to be the recommended anesthetic of choice for obstetric surgical procedures. In LRCs where anesthesia practitioners have less training on average, little backup, and limited access to advanced equipment, it seems reasonable that neuraxial regional anesthesia should also be the anesthetic of choice for obstetrical patients.12 In addition to being considered safe and effective, neuraxial anesthesia is relatively easy to teach and perform. It is felt by many to be the anesthetic of choice in LRCs for surgeries at and below the umbilicus. In some areas, such as parts of India and Sri Lanka, the percentage of surgery done under spinal anesthesia is reportedly greater than in some HRCs, but there are still many areas of Sub-Saharan Africa and Southeast Asia where neuraxial anesthesia would be appropriate but is not performed.8,13 This is especially surprising since the basic equipment required is simple and less expensive than what is required for most general anesthetics (Figure 1). The frequent lack of access to functioning anesthetic machines, basic airway equipment, capnography, neuromuscular function monitors, and even oxygen in LRCs has been well documented.4,40,41 The safety and access to general anesthesia are particularly affected by these resource gaps. When there are emergent surgical cases to be done and not enough anesthetic machines available, regional anesthesia can provide a less resource-intense option in many cases. The level of staffing, amount of time required to monitor the patient, and concerns about airway safety especially postoperatively can also be expected to be less with regional anesthesia.42 The patients benefit from the analgesia provided by the local anesthetics which is advantageous in countries where there is poor access to opioids.21,24,40 Regional anesthesia, especially neuraxial, has the potential to make surgery safer and more comfortable for patients in LMICs (Box 1). Although there are additional barriers to increasing the use of peripheral nerve blocks in LMICs, many of the benefits of improved safety and patient comfort are the same as with neuraxial anesthesia. Making regional anesthetics more available should amplify the safety benefit in hospitals that have an inadequate supply of oxygen, anesthetic machines, monitoring equipment, and trained staff to keep patients safe in the operating room and postoperatively.
 |
Box 1 Key Points on the Safety Benefits of Regional Anesthesia |
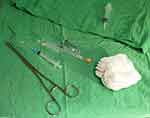 |
Figure 1 Equipment for neuraxial anesthesia typically seen in LRCs. |
Education, Training, and Mentorship Barriers and Solutions
There are multiple potential benefits to regional anesthesia use that may be amplified in low-resource countries. Why then are regional techniques not more widespread in LMICs? The low numbers of anesthesia practitioners available to learn and practice any type of anesthesia is an obvious obstacle. In one report, 30.4% of the 344 medical facilities surveyed had no anesthesia providers at any level (physicians, nurses, or technicians) accessible for patient care.43 The crisis in human resources for anesthesia care in many LRCs is contributed to by the low standing that the profession has, especially in Sub-Saharan Africa, and the resulting problems with recruitment and retention of practitioners at all levels.13 Encouraging a change of attitude towards the anesthesia profession is a complex problem that will take a multipronged approach and time. Collaborative assistance by international organizations and universities can help develop the educational infrastructure in LMICs to fill the provider pipeline and build capacity.13,44 In the meantime, small steps can be made by the current workforce to make anesthesia more accessible, more rewarding, and therefore more attractive to new recruits. Greater use of regional anesthesia can be one way to safely increase anesthesia access and create enthusiasm for the field at the same time. A lack of awareness of what is possible is sometimes an explanation for not adopting new techniques.45 Successful introduction of anesthetic techniques in a hospital requires well-trained practitioners who are knowledgeable in the indications and management of possible complications. The practitioner must have enough experience to be confident in their ability to successfully demonstrate the value of the techniques to patients, surgeons, nurses, and administrators. This is illustrated by the following example as told by a trainee anesthetic officer who returned to his rural home district after being trained in the use of spinal anesthesia. He described being on “night duty” when a woman presented with obstructed labor requiring a caesarean section. After determining there were no contraindications, he obtained permission from his supervising senior anesthetic officer and the patient and placed a spinal anesthetic. It was only after the surgery was successfully completed that he discovered he was the first to perform spinal anesthesia at that hospital.
The surgeon was particularly excited and the news about that spinal anaesthesia spread all over the hospital and the nearby village especially when the patient was taken back to the ward fully conscious and talking, which most people referred to as a “miracle”.
The anesthetic officer was invited the next day to work with the medical superintendent of the hospital and to use spinal anesthesia for his cases.
The theatre was full of staff from the wards and the theatre staff who wanted to observe how spinal anaesthesia was performed and how it works. The medical superintendent was so impressed, to the extent that he ordered the purchase of spinal drugs and needles which was effected the following week.
In two days this anesthetic officer, despite being low in the hierarchy at the hospital, demonstrated adaptive leadership by introducing a new, useful, and safe technique to the hospital using cooperative teamwork and good communication. He sustainably changed the practice, and neuraxial regional anesthesia continues to be used in the hospital with strong support from the surgeons, the hospital administration, and the community.
Patients now know about spinal anaesthesia and request it, especially mothers who are due [for] Caesarean section.
He credited the good training he received from his tutors and the head of anesthesia department at his educational institution for his success and clearly took great personal satisfaction from his experience, calling it: “My best anaesthetic experience.”46
Progress in the use of regional anesthesia can also be spurred by collaboration with outside academic or non-governmental organizations who assist in education, training, and mentoring. Kybele, Inc. is an example of an organization working in LMICs to improve obstetric anesthesia services. One of their projects began a 5-year collaboration in 2007 with the Ridge Regional Hospital in Accra, Ghana to teach spinal anesthesia for cesarean delivery. The use of spinal anesthesia at the hospital in 2006 prior to the collaboration was 6%. By 2009 the use had increased to 89%, and by 2012 greater than 90% of cesarean deliveries were performed under spinal anesthesia. Because of a lack of personnel and other resources, Kybele’s attempt to increase the use of labor analgesia was not equally successful.47 The reported increased use of spinal anesthesia in most district hospitals, from Sub-Saharan Africa during the past 10 years, is likely due to training of mid-level anesthesia providers and a demonstrated success under the limitations of resources available. Improving the use of the more sophisticated regional anesthesia techniques will also require trained personnel and institutional support for equipment and medications. This type of regional anesthesia expertise also requires students who are interested, educators who are willing and able to teach, and a stable and supportive venue to learn and practice. Most peripheral nerve, fascial plane, and paravertebral blocks will require extensive training that can best be achieved by anesthesiologists. These physicians have the significantly longer in-depth training necessary compared to non-physician anesthetists. Physician anesthesiologists should be expected to take the lead in the practice and education of the more challenging forms of regional anesthesia. The lack of subspecialty training available in many low-resource countries is a significant barrier to building an adequate number of anesthesiologists who can rapidly develop the specialty. There are currently no full-length regional anesthesia and acute pain management (RAAPM) fellowships in any country in Africa, although Rwanda is in the process of opening the first such program at the University Central Hospital of Kigali.48 In comparison, the United States has 83 RAAPM fellowships according to the American Society of Regional Anesthesia (ASRA).49 One underlying reason for the lack of regional anesthesia subspecialty training is the overall shortage of anesthesiologists in LRCs. This is particularly true in the African and the Southeast Asian regions where one survey found that more than 77 countries had less than 5 physician anesthesiologists per 100,000 population, which is the recommended minimum number for safe surgery and anesthesia.50 In sub-Saharan Africa, a majority of countries have less than 1 anesthesiologist per 100,000 population.51 Anesthesia training has had a very low priority for many decades in LMICs, and there is a severe shortage of both medical students interested in anesthesia and trained anesthesiologists available to teach.13 The number of medical schools and anesthesia residency programs is slowly increasing, but it will take many years to graduate enough anesthesiologists for quality subspecialty training to be possible. Task shifting with non-physician anesthetists helps with the clinical burden. However, there are too few physician anesthesiologists to successfully teach medical students, nurses, and residents as well as to supervise quality clinical anesthetic care in the operating rooms, ICUs, and maternity wards. Anesthesiologists from LMICs, who are trained in regional anesthetic techniques, have often been educated in programs outside their country or by visiting educators through academic partnerships or non-governmental organizations (NGOs). The support offered by the European Society of Regional Anaesthesia and Pain Therapy (ESRA), the World Federation of Societies of Anaesthesiologists (WFSA), academic programs in HRCs, and NGOs, have enabled a growing number of young doctors to study regional anesthesia techniques abroad or through in-country mentoring.52,53 One of our authors (AK) describes how he became involved in regional anesthesia practice at the Mbarara Regional Referral Hospital in Mbarara, Uganda.
We started by using nerve stimulators to perform nerve blocks and even using blind techniques for some of the blocks like transabdominal plane block (TAP). Ultrasound guided nerve blocks are a newer practice and not many anaesthesia providers are comfortable with these techniques. Ultrasound guided nerve blocks are currently practiced a lot in our hospital, especially the TAP block, however this type of regional anaesthesia is not common in our country except Mbarara Regional Referral Hospital and the Mulago National Referral Hospital in Kampala, Uganda. The introduction to ultrasound guided regional anaesthesia to our hospital was from a group of regional anaesthesiologists from the Massachusetts General Hospital (MGH) in Boston. They came for a week which was inadequate to really start something unsupervised, however repeat visits from the team from MGH largely contributed to the gradual improvement in our practice. In addition, I was lucky to do a 1-month rotation at MGH to observe. This rotation greatly opened my eyes to the practice of regional anaesthesia. I now have extensive practice with the TAP block which helped me to get confident with the needle technique. Initially the surgical team did not welcome these procedures because they told us we were wasting time and they would not work. With continued practice, we became more familiar with the procedures. We took less time and the success rate increased. We noticed a progressive appreciation by the surgical team, especially the orthopedic team.
The collaborative work between MGH and the anesthesia department at Mbarara Hospital also resulted in a study demonstrating that TAP block and intrathecal morphine after caesarean section are equivalent for postoperative pain control.54 Providing up-to-date regional anesthesia training and mentoring can give anesthesiologists confidence and professional satisfaction in their ability to safely and successfully perform blocks.45 This is increasingly important in LMICs for quality of patient care and as an incentive to retain both surgeons and anesthesiologists in the country and avoid “brain drain,” the migration of healthcare workers to higher-income countries. Lack of professional advancement opportunities is a primary driver of physicians to leave their country of training.55 In-country training programs that include sub-specialty training at the level found in HRCs is still a luxury but should be encouraged to help recruit and retain anesthesiologists in LRCs. Small programs of subspecialty training in pediatric anesthesia have already started in several countries, but subspecialty training in regional anesthesia should also be a priority.31 Building a core of anesthesiologists who are skilled in regional anesthesia and motivated to train others contribute to the hope of a sustainable growth of quality anesthesia care in developing countries. Recommended basic regional anesthetic blocks which should be included in the curriculum of anesthesiology residents are listed in Boxes 2 and 3. Box 2 lists regional blocks that can be done relatively safely using anatomic landmarks only although many would benefit from ultrasound visualization. Box 3 lists regional blocks which are safer and more efficiently performed when using ultrasound guidance as seen in any major book on regional anesthesia.
 |
Box 2 Recommended Anatomic Landmark-Based Regional Blocks |
 |
Box 3 Recommended Basic Ultrasound-Guided Regional Blocks |
Barriers in Infrastructure, Equipment, and Drugs
The deficits in anesthesia infrastructure, equipment, and drugs that severely limit anesthesia capacity in most low-resource countries have been well documented in multiple studies.1–4,43,56,57 Few hospitals in LMICs can reliably satisfy even the minimum monitoring, medication, and equipment for safe anesthetic practice recommended by the WHO and WFSA in their international guidelines.58 This is especially a problem in Sub-Saharan African district-level hospitals where essential surgical services are meant to be provided for the predominantly rural population. A recent example is provided in the SURG-Africa (Scaling up Safe Surgery for District and Rural Populations in Africa) study conducted in Zambia, Malawi, and Tanzania in 2017.3 One-third of the 76 hospitals surveyed were found to lack reliable access to a functioning anesthesia machine and compressed oxygen. Most hospitals also reported that available anesthetic machines were inadequate in number and often old and poorly functioning, particularly in Tanzania. In Malawi, almost 70% of hospitals surveyed had no reliable access to running water and 77% had unreliable access to electricity. Other supplies required for safe general anesthesia were also found to be deficient, and practitioners frequently resorted to using ketamine as the sole anesthetic. The lack of resources in these district hospitals is compounded by an inadequate number of qualified anesthesia providers. No hospital had a physician anesthesiologist, and most relied on mid-level anesthetists some of whom were not formally trained. In Zambia, 7 out of 24 surveyed hospitals relied on recruitment of untrained operating room staff to give anesthetics because no one else was available.3 One can imagine that under these circumstances general anesthesia is not very safe and often patients, even in time-sensitive emergent cases, must be transferred to larger more resource-rich hospitals for care. Spinal anesthesia was not always available in the hospitals. Some regional anesthesia was performed, but it was unclear what type.3 Ketamine was readily available at all the hospitals and remains a valuable, and safer anesthetic choice as a substitute to general anesthesia in LRCs. Ketamine like regional anesthesia usually preserves airway and respiratory functions, provides opioid-sparing analgesia, and is inexpensive to use. In HRCs ketamine is used as an adjunct to sedation, general anesthesia, and for postoperative analgesia. It is only rarely used as the sole agent to replace general anesthesia. Ketamine does not provide muscle relaxation, but regional anesthesia does. This is one reason regional is preferable for most limb and lower abdominal surgeries. Ketamine is not recommended for patients with poorly controlled hypertension and ischemic heart disease because it increases cardiac output, blood pressure, and heart rate when used as an anesthetic. In contrast, regional anesthesia, especially peripheral nerve blocks, can be helpful in these patients by providing analgesia and decreasing stress hormones with minimal cardiovascular effects. Ketamine is a dissociative anesthetic agent and can frequently cause what many people would consider unpleasant psychological effects on emergence.59,60 Unfortunately, ketamine can also be abused as a recreational drug which has threatened its continued presence on the WHO list of essential drugs.61 Regional anesthesia preserves patient consciousness which is appreciated by mothers undergoing caesarean sections who can be awake and aware when their babies are delivered under spinal anesthesia instead of ketamine or general anesthesia. Given the choice, most anesthesiologists would choose a well-performed regional anesthetic over a ketamine-only anesthetic for cases that are amenable to either because of the above reasons. Spinal anesthesia is especially advantageous as a ketamine or general anesthesia substitute since the supplies required are relatively inexpensive and do not require technical support (Figure 1). Techniques are easily taught to mid-level providers but certainly require anesthesia training to understand the contraindications and how to handle the rare life-threatening and disabling complications. It deserves saying that having a surgeon or other non-anesthesia-trained physician in the room will not be adequate backup to monitor and deal with any major anesthetic complications as is sometimes suggested. A surgeon cannot and should not have to deal with ongoing surgery and an anesthetic problem at the same time. Fortunately in the larger national or regional referral hospitals, such as Mbarara Regional Referral Hospital (MRRH) in Uganda, spinal anesthesia for obstetrics and gynecological procedures and caudal epidural anesthesia for pediatric procedures have become increasingly well-established techniques over the past 15 years and are mostly performed by experienced mid-level providers. Problems remain with access to post-dural puncture headache-reducing pencil-point spinal needles which are more expensive than quincke needles and to the anesthetic medications needed for regional anesthesia. Intermittent drug supply chain problems have been an increasing problem in HRCs, but in many LMICs the absence of a reliable supply of anesthetic medications is so widespread and persistent that it remains an obstacle to choosing the safest anesthetic care.3,40 The limited supply of basic medications and the reported poor quality or counterfeit medications causing complications in patients is of great concern and deserves investigation and new initiatives.3,62,63 According to the WHO Global Surveillance and Monitoring System, 42% of substandard and falsified product reports from 2013 to 2017 came from the WHO Africa Region and 8.5% of the products reported were anesthetics and painkillers.63 For regional anesthesia techniques to expand, ensuring reliable access to quality medications is vital so that its safety and efficiency can be realized. Overcoming the equipment and medication barriers to regional anesthesia in LRCs is surmountable and important in order to increase surgical access when anesthesia capacity and cost are the limiting factors (Box 4).
 |
Box 4 Key Points on Barriers to Use of Regional Anesthesia in LMICs |
Next Steps: The Argument for Greater Use of Ultrasound in Low-Resource Countries
The use of ultrasound to guide regional anesthesia for peripheral and fascial plane blocks has become the preferred method in most HRCs because of advantages in safety, efficacy, and efficiency. Peripheral nerve blocks performed under ultrasound guidance have a higher success rate with fewer needle passes, reduced dosage of local anesthetics, and lower incidence of local anesthetic toxicity.64 The lack of trained anesthesiologists and the cost of ultrasound equipment have been cited as major barriers to greater use of ultrasound techniques in LMICs. Several recent developments support the increased feasibility of using ultrasound for anesthesia even in low-resource countries. Evolving technology is producing ultrasound equipment that is more durable, portable, and with longer battery lives. These improvements are valuable in harsh environments where electricity and access to equipment maintenance is inconsistent.65,66 Machine design has been streamlined with fewer knobs and user-friendly controls which improves the learning curve for new users.67 In the last few years, increasingly affordable handheld devices that can be connected to cell phones or laptops have become available for one-tenth or less of the price of traditional ultrasound machines. Anesthesiologists have also expanded the use of ultrasound techniques beyond peripheral nerve block and vascular access procedures. Point-of-care ultrasound (POCUS) can be valuable for quickly diagnosing multiple perioperative clinical conditions that can impact the anesthetic management. Some examples include recognition of pneumothorax, hemoperitoneum, or hemopericardium in trauma patients. Knowing that a patient has underlying cardiac valvular disease can be extremely helpful in determining what type of anesthesia will be best tolerated. Ultrasound of the inferior vena cava (IVC) can be used to estimate blood loss and dehydration which should influence anesthetic choice, management, urgency of surgery, and need for transfusion. In developing countries, ultrasound has also been used to help diagnose cerebral malaria in children and abdominal tuberculosis, either of which would be important conditions to recognize prior to any anesthetic. Ultrasound tools are especially valuable in remote hospitals where access to imaging is scarce, and safe transport of acutely ill patients is difficult.65 A rapid ultrasound scan can aid in a risk-benefit decision about the urgency of performing anesthesia and surgery in a low-resource hospital or delaying surgery to allow for transport to a better-resourced hospital. When considering the initial cost outlay for an ultrasound machine, it is important to include all possible benefits of access to this multipurpose tool. The initial and maintenance costs of having multiple anesthesia machines that require reliable electricity, oxygen, airway equipment, and anesthetic gases and drugs must also be considered when choosing where to spend hospital funds. Fortunately, the value of ultrasound access in LMICs has been increasingly recognized by the WHO, ministries of health, and non-governmental organizations.67 Ultrasound related research and the application of ultrasound technology in LMICs for screening and diagnostic clinical decision-making has increased in the past decade. This increased use has occurred mostly in tertiary care facilities and in middle-income countries, although Sub-Saharan African countries were found to be the most innovative in the use of ultrasound for diagnostic purposes.65 Educational training programs, improved portability, and decreasing cost of equipment were deemed contributing factors to improved use. Ultrasound is recognized as a valuable tool in LRCs because it compares favorably in cost and portability to other imaging techniques.66 However, there are very few studies and reports on the use of ultrasound for regional anesthesia in LRCs. The recent development of a handheld, whole-body ultrasound probe that uses a chip technology and smartphone as a screen and costs $2000 USD has the potential to improve access to safe regional anesthesia in LMICs.68 There remains a cost barrier to peripheral nerve blocks as reported by our author AK. The pharmacies in Uganda do not sell ultrasound nerve block needles or insulated stimulating needles. This would require a special order thus making it more expensive. In our hospital, we usually get these needles from friends that come from the United States. We are currently using spinal needles which cost about $1–2 USD. It is of course more difficult to use spinal needles for ultrasound-guided blocks but the easiest option in our setting. Despite barriers, there is evidence of enthusiasm for learning ultrasound regional anesthesia techniques in LRCs.69 However, a lack of teachers competent in the use of ultrasound and low numbers of available anesthesia trainees will be a challenge for growing the subspecialty. Developing skilled anesthesia personnel in the use of basic ultrasound anesthesia techniques requires at a minimum a strong background in medical studies and a short but intensive training period that includes lectures and practical experience followed by repeat review sessions and outcome supervision. Anesthesia specialist programs in LMICs should be encouraged to include basic ultrasound training for residents and medical students. National and international anesthesia societies can help support and advocate for improved subspecialty training in ultrasound-guided regional anesthesia. Physician anesthesiologists who are trained in all aspects of regional anesthesia, including ultrasound use, are particularly needed as educators for the medical students and early career anesthesiologists who are looking for professional challenges and satisfaction beyond the routine anesthesia cases. Providing opportunities for professional education and growth is thought to be one of the motivators for improved recruitment and retention of anesthesia residents.55 The typical training period for non-physician anesthetists in LMICs may be too short to include more than an introduction to basic ultrasound use. However, seasoned anesthetists can reasonably be trained in low-risk regional techniques using ultrasound in training modules followed by the supervision of an anesthesiologist. It will take time to build the capacity of trained anesthesiologists, anesthetists, and equipment before ultrasound-guided regional anesthesia can be reliably and widely offered in LMICs. The growth has started tentatively in several countries including Ghana, Uganda, Rwanda, Ethiopia, Nepal, and Vietnam to mention a few.13,44,69 The rate at which ultrasound-guided regional anesthesia grows will depend on the support of hospital administrations, ministries of health, domestic and international medical universities, anesthesia societies, non-governmental organizations, and surgical and pharmacy departments. Going forward, it will be important to measure outcomes to determine whether the potential benefits of regional anesthesia can be realized as a guide to distribution of resources and future directions (Box 5).
 |
Box 5 Solutions for Increased Regional Anesthesia Capacity in LMICs |
Summary
Expanding the use of regional anesthesia in low-resource countries has potential safety, access, and cost benefits. Regional including neuraxial anesthesia has been shown to be particularly advantageous in the obstetric, trauma, and orthopedic patients who often present for surgery in LMICs. Benefits of using regional rather than general anesthesia include fewer life-threatening perioperative airway and respiratory complications, especially in obstetrical patients and patients with pre-existing lung disease. Greater access to regional anesthesia should amplify the safety benefit in hospitals that have an inadequate supply of oxygen, anesthetic machines, monitoring equipment, and trained staff to care for patients in the operating room and postoperatively. More outcomes research is needed to strengthen the evidence for improved access and safety specifically with regional anesthesia in resource-limited settings since most research on this topic has occurred in HRCs. Ultrasound-guided peripheral nerve blocks and neuraxial anesthesia share many of the same benefits in improved safety and patient comfort. The cost of ultrasound equipment has been cited as a barrier to increased use of ultrasound techniques for peripheral nerve blocks. In the last few years, handheld devices that can be connected to cell phones or laptops have become available for one-tenth or less the price of traditional ultrasound machines. Newer ultrasound equipment has also been designed to be more durable, portable, and with longer battery lives. These improvements are valuable in harsh environments where electricity and access to equipment maintenance is inconsistent.65,66 In addition to its use for regional anesthesia techniques, an ultrasound machine benefits patient care as an aid to perioperative diagnosis and decision-making, as well as vascular access. This should be taken into consideration when making decisions on where to spend institutional funds. An additional barrier to developing regional anesthesia and especially ultrasound-guided techniques are the lack of adequate numbers of physician anesthesiologists and well-trained anesthetists. The lack of support for the profession and the resulting low morale contributes to the difficulty in recruiting and retaining anesthesia practitioners. Attracting medical students and talented mid-level practitioners to the anesthesia profession in LRCs will take a multipronged approach and time. One method should be to provide up-to-date regional anesthesia training and mentoring to build the confidence of anesthesiologists and anesthetists to improve professional satisfaction. Developing a core of anesthesiologists who are skilled in regional anesthesia and motivated to train others should contribute to a sustainable growth of quality anesthesia care in developing countries. Collaboration between international organizations and universities can also help develop the educational infrastructure in LMICs to fill the provider pipeline and build capacity. Increasing training opportunities in ultrasound-guided nerve blocks combined with the recent availability of more robust and affordable ultrasound equipment would improve the options for providing safe and accessible anesthesia and surgery in low-resource countries.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Drake G, LeBrun BA, Chackungal S, et al. Prioritizing essential surgery and safe anesthesia for the post-2015 development agenda: operative capacities of 78 district hospitals in 7 low-and middle-income countries. Surgery. 2014;155:365–373. doi:10.1016/j.surg.2013.10.008
2. Alkire BC, Raykar NP, Shrine MG, et al. Global access to surgical care: a modelling study. Lancet Glob Health. 2015;3:e316–e323. doi:10.1016/S2214-109X(15)70115-4
3. Gajewski J, Pittalis C, Lavy C, et al. Anesthesia capacity of district-level hospitals in Malawi, Tanzania, and Zambia: A mixed-methods study. Anesth Analg. 2020;130(4):845–853. doi:10.1213/ANE.0000000000004363
4. Handler RA, Chawla S, Stewart BT, et al. Anesthesia care capacity at health facilities in 22 low- and middle-income countries. World J Surg. 2016;40:1025–1033. doi:10.1007/s00268-016-3430-4
5. Kasole-Zulu T, Ndebea A, Chikumbanje SS, Bould MD. Anesthesia capacity in rural Zambia, Malawi, and Tanzania: the anesthesiologist’s perspective. Anesth Analg. 2020;130(4):841–844. doi:10.1213/ANE.0000000000004638
6. Gajeelee A, Chaumont C, Glenn J. New leadership for global health. Stanford Social Innovation Review. 2020;18(3):1–5.
7. Sobhy S, Zamora J, Dharmarajah K, et al. Anaesthesia-related maternal mortality in low-income and middle-income countries: a systematic review and meta-analysis. Lancet Glob Health. 2016;4:e320–27. doi:10.1016/S2214-109X(16)30003-1
8. Mgbakor AC, Adou BE. Plea for greater use of spinal anaesthesia in developing countries. Trop Doct. 2012;42:49–51. doi:10.1258/td.2011.100305
9. Khan FA, Merry AF. Improving anesthesia safety in low-resource settings. Anesth Analg. 2018;126(4):1312–1320. doi:10.1213/ANE.0000000000002728
10. Kettner SC, Willschke H, Marhofer P. Does regional anaesthesia really improve outcome? Br J Anaesth. 2011;107:i90–i5. doi:10.1093/bja/aer340
11. Walker JW, Long JB, Sathyamoorthy M, et al. Complications in pediatric regional anesthesia: an analysis of more than 100,000 blocks from the pediatric regional anesthesia network. Anesthesiology. 2018;129(4):721–732.
12. Lonnee HA, Madzimbamuto F, Erlandsen ORM, et al. Anesthesia for Cesarean delivery: a cross-sectional survey of provincial, district, and mission hospitals in Zimbabwe. Anesth Analg. 2018;126(6):2056–2064. doi:10.1213/ANE.0000000000002733
13. Brouillette MA, Aidoo AJ, Hondras MA, et al. Anesthesia capacity in Ghana: a teaching hospital’s resources, and the national workforce and education. Anesth Analg. 2017;125(6):2063–2071. doi:10.1213/ANE.0000000000002487
14. Rukewe A, Fatiregun A, Alonge TO. Orthopaedic anaesthesia for upper extremity procedures in a Nigerian hospital. Malawi Med J. 2014;26(3):90–92.
15. American Society of Anesthesiology. Practice guidelines for obstetric anesthesia: an updated report by the American Society of Anesthesiologists Task Force on obstetric anesthesia and the society for obstetric anesthesia and perinatology. Anesthesiology. 2016;124(2):1–31.
16. Gadsden J, Warlick A. Regional anesthesia for the trauma patient: improving patient outcomes. Local Reg Aesth. 2015;8:45–55. doi:10.2147/LRA.S55322
17. Warren J, Sundaram K, Anis H, et al. Spinal anesthesia is associated with decreased complications after total knee and hip arthroplasty. J Am Acad Orthop Surg. 2020;28:e213–e221. doi:10.5435/JAAOS-D-19-00156
18. Rodgers A, Walker N, Schug S, et al. Reduction of postoperative mortality and morbidity with epidural or spinal anaesthesia: results from overview of randomised trials. BMJ. 2000;321:1493.
19. Brown EN, Pavone KJ, Naranjo M. Multimodal general anesthesia: theory and practice. Anesth Analg. 2018;127(5):1246–1258. doi:10.1213/ANE.0000000000003668
20. Uppal V, Sondekoppam RV, Lobo CA, et al. Practice Recommendations on Neuraxial Anesthesia and Peripheral Blocks during the COVID-19 Pandemic: a joint statement by the American Society of Regional Anesthesia and Pain Medicine (ASRA) and European Society of Regional Anesthesia and Pain Therapy (ESRA). Available from: www.asra.com/covid-19/raguidance.
21. International Narcotics Control Board. Narcotic drugs. Technical reports. Estimated world requirements for 2020—statistics for 2018. Available from: https://www.incb.org/incb/en/narcotic-drugs/Technical_Reports/narcotic_drugs_reports.html.
22. Cherrny NI The international collaborative project to evaluate the availability and accessibility of opioids for the management of cancer pain in Africa, Asia, Latin America, & the Caribbean, and the Middle East. ESMO Palliative Care Working Group. Available from: http://www.esmo.org/Policy/International-Access-to-Opioids-Survey.
23. Knaul FM, Farmer PE, Krakauer EL, et al. Alleviating the access abyss in palliative care and pain relief-an imperative of universal health coverage: the Lancet Commission report. Lancet. 2018;391(10128):1391–1454. doi:10.1016/S0140-6736(17)32513-8
24. Bhadelia A, De Lima L, Arreola-Ornelas H, et al. Solving the global crisis in access to pain relief: lessons from country actions. Am J Public Health. 2019;109:58–60. doi:10.2105/AJPH.2018.304769
25. Biccard BM, Madiba TE, Kluyts HL, et al. Perioperative patient outcomes in the African Surgical Outcomes Study: a 7-day prospective observational cohort study. Lancet. 2018;391:1589–1598.
26. World Health Organization Regional Office for Africa. Over 10,000 health workers in Africa infected with COVID-19. Available from: http://whotogo-whoafroccmaster.newsweaver.com/JournalEnglishNewsletter.
27. Newton MW, Hurt SE, McEvoy MD, et al. Pediatric perioperative mortality in Kenya: a prospective cohort study from 24 hospitals. Anesthesiology. 2020;132:452–460. doi:10.1097/ALN.0000000000003070
28. Bainbridge DB, Martin J, Arango M, Cheng D. Perioperative and anaesthetic-related mortality in developed and developing countries: a systematic review and meta-analysis. Lancet. 2012;380:1075–1081. doi:10.1016/S0140-6736(12)60990-8
29. Koga FA, El Dib R, Wakasugui W, et al. Anesthesia-related and perioperative cardiac arrest in low- and high-income countries: a systematic review with meta-regression and proportional meta-analysis. Medicine. 2015;94:e1465. doi:10.1097/MD.0000000000001465
30. Cooper MG. Global safe pediatric anesthesia care. Anesthesiology. 2020;132:413–415. doi:10.1097/ALN.0000000000003028
31. Ouro-Bang’na Maman AF, Tomta K, Ahouangbevi S, Chobli M. Deaths associated with anesthesia in Togo, West Africa. Trop Doct. 2015;35(4):220–222. doi:10.1258/004947505774938666
32. Manyumwa P, Chimhundu-Sithole T, Marange-Chikuni D, Evans FM. Adaptations in pediatric anesthesia care and airway management in the resource-poor setting. Paediatr Anaesth. 2020;30(3):241–247. doi:10.1111/pan.13824
33. Rajbhandari R, McMahon DE, Rhatigan JJ, Farmer PE. The neglected hospital- the district hospital’s central role in global health care delivery. NEJM. 2020;382(5):397–399. doi:10.1056/NEJMp1911298
34. Ariyo P, Trelles M, Helmand R, et al. Providing anesthesia care in resource-limited settings: a 6-year analysis of anesthesia services provided at Medicines Sans Frontieres facilities. Anesthesiology. 2016;124:561–569. doi:10.1097/ALN.0000000000000985
35. Sobhy S, Arroyo-Manzano D, Murugesu N, et al. Maternal and perinatal mortality and complications associated with Caesarean section in low-income and middle-income countries: A systematic review and meta-analysis. Lancet. 2019;393(10184):1973–1982. doi:10.1016/S0140-6736(18)32386-9
36. Nickerson JW, Pettus K, Wheeler KE, et al. Access to controlled medicines for anesthesia and surgical care in low-income countries: a narrative review of international drug control systems and policies. Can J Anesth. 2017;64:296–307. doi:10.1007/s12630-016-0805-9
37. Cook TM, Woodall N, Frerk C; on behalf of the Fourth National Audit Project. Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 1: anaesthesia. Br J Anaesth. 2011;106(5):617–631. doi:10.1093/bja/aer058
38. Norris AM, Hardman JG, Asai T. A firm foundation for progress in airway management. Br J Anaesth. 2011;106(5):613–616. doi:10.1093/bja/aer088
39. Kinsella SM, Winton AL, Mushambi MC, et al. Failed tracheal intubation during obstetric general anesthesia: a literature review. Int J Obstet Anesth. 2015;24:356–374. doi:10.1016/j.ijoa.2015.06.008
40. Hendel S, Coonan T, Thomas S, et al. The rate-limiting step: the provision of safe anesthesia in low-income countries. World J Surg. 2015;39:833–841. doi:10.1007/s00268-014-2775-9
41. Duke T, Graham SM, Cherian MN, et al. Oxygen is an essential medicine: a call for international action. Int J Tuberc Lung Dis. 2010;14(11):1362–1368.
42. Tao K, Sokha S, Yuan H. The challenge of safe anesthesia in developing countries: defining the problems in a medical center in Cambodia. BMC Health Serv Res. 2020;20(204):1. doi:10.1186/s12913-020-5068-z
43. Ho M, Livingston P, Bould MD, et al. Barriers and facilitators to implementing a regional anesthesia service in a low-income country: a qualitative study. Pan Afr Med J. 2019;32:152. doi:10.11604/pamj.2019.32.152.17246
44. Rukewe A, Fatiregun A. The use of regional anesthesia by anesthesiologists in Nigeria. Anesth Analg. 2010;110(1):243–244. doi:10.1213/ANE.0b013e3181c0f00e
45. Schnittger T. Regional anaesthesia in developing countries. Anaesthesia. 2007;62(Suppl. 1):44–47. doi:10.1111/j.1365-2044.2007.05297.x
46. Olufolabi AJ, Atito-Narh E, Eshun M, et al. Teaching neuraxial anesthesia techniques for obstetric care in a Ghanaian referral hospital: achievements and obstacles. Anesth Analg. 2016;120:1317–1322. doi:10.1213/ANE.0000000000000464
47. Swisher M, Uwamahoro E, Banguti P, Uwineza JB Development of the East African Regional Anesthesia and Acute Pain Medicine Fellowship Program. ASRA News; August 2019. Available from: www.asra.com/asra-news/.
48. Fellowship directory-American Society of Regional Anesthesia. Available from: https://www.ASRA.com/fellowship-dir.
49. Kempthorne P, Morriss WW, Mellin-Olsen J, Gore-Booth J. The WFSA global anesthesia workforce survey. Anesth Analg. 2017;125(3):981–990. doi:10.1213/ANE.0000000000002258
50. Davies JI, Vreede E, Onajin-Obembe B, Morriss WW. What is the minimum number of specialist anaesthestists needed in low-income and middle-income countries? BMJ Glob Health. 2018;3(6):e001005. doi:10.1136/bmjgh-2018-001005
51. ESRA Educational Grant. Available from: https://esraeurope.org/grants-award.
52. WFSA Fellowship Programs. Available from: https://www.wfsa-fellowship.
53. Kwikiriza A, Kiwanuka JK, Firth PG, et al. The analgesic effects of intrathecal morphine in comparison with ultrasound-guided transversus abdominis plane block after caesarean section: a randomized controlled trial at a Ugandan regional referral hospital. Anaesthesia. 2019;74:167–173.
54. Epiu I, Tindimwebwa JVB, Mijumbi C, et al. Challenges of anesthesia in low-and middle-income countries: a cross-sectional survey of access to safe obstetric anesthesia in East Africa. Anesth Analg. 2017;124(1):290–299. doi:10.1213/ANE.0000000000001690
55. Dohlman L, DiMeglio M, Hajj J, et al. Global brain drain: how can the Maslow theory of motivation improve our understanding of physician migration? Int J Env Res Public Health. 2019;16:1182. doi:10.3390/ijerph16071182
56. Epiu I, Wabule A, Kambugu A, et al. Key bottlenecks to the provision of safe obstetric anaesthesia in low-income countries: a cross-sectional survey of 64 hospitals in Uganda. BMC Pregnancy Childbirth. 2017;17(1):387. doi:10.1186/s12884-017-1566-3
57. Gelb AW, Morriss WW, Johnson W, Merry A; for International Standards for a Safe Practice of Anesthesia Workgroup. World Health Organization-World Federation of Societies of Anaesthesiologists (WHO-WFSA) international standards for a safe practice of anesthesia. Anesth Analg. 2018;126:2047–2055. doi:10.1213/ANE.0000000000002927
58. Adepoju P. African nations to criminalise falsified medicine trafficking. World Report. Lancet. 2020;395(10221):324. doi:10.1016/S0140-6736(20)30244-0
59. Kurdi MS, Theerth KA, Deva RS. Ketamine: Current applications in anesthesia, pain, and critical care. Anesth Essays Res. 2014;8(3):283–290. doi:10.4103/0259-1162.143110
60. Gales A, Maxwell S. Ketamine: recent evidence and current uses. ATOTW Tutorial. 2018;381:1–7.
61. Domino EF. Taming the ketamine tiger. Anesthesiology. 2010;113:678–684.
62. Neal JM, Brull R, Horn JL, et al. The second American society of regional anesthesia and pain medicine evidence-based medicine assessment of ultrasound-guided regional anesthesia: executive summary. Reg Anesth Pain Med. 2016;41(2):181–194. doi:10.1097/AAP.0000000000000331
63. Pisani E WHO Global Surveillance and Monitoring System for substandard and falsified medical products. Geneva: World Health Organization; 2017. Licence: CC BY-NC-SA 3.0 IGO. Available from: www.who/EMP/RHT/2017.01.
64. Sippel S, Muruganandan K, Levine A, Shah S. Review article: use of ultrasound in the developing world. Int J Emerg Med. 2011;4:72. doi:10.1186/1865-1380-4-72
65. Stewart KA, Navarro SM, Kambala S, et al. Trends in ultrasound use in low-and-middle income countries: A systematic review. IJMA. 2020;9(1):103–120.
66. Becker DM, Tafoya CA, Becker SL, et al. The use of portable ultrasound devices in low-and middle-income countries: a systematic review of literature. Trop Med Int Health. 2016;21(3):294–311. doi:10.1111/tmi.12657
67. Paniker J, Graham SM, Harrison JW. Global trauma: the great divide. SICOT J. 2015;1(19):1–6. doi:10.1051/sicotj/2015019
68. McNeil DG In African villages, these phones become ultrasound scanners. The New York Times. Available from: https://www.nytimes.com/2019/04/15/health/medical-scans-butterfly-iq.html.
69. Hamal PK, Rayamajhi AJ, Pokhrel N, et al. Can ultrasound guided anesthesia improve rural anesthesia services and address safety issues in low income country? Perspective from Nepal. J Nepal Health Res Counc. 2020;18(46):144–146. doi:10.33314/jnhrc.v18i1.2614
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
