Back to Journals » Neuropsychiatric Disease and Treatment » Volume 12
Associations between the mismatch-negativity component and symptom severity in children and adolescents with attention deficit/hyperactivity disorder
Authors Yamamuro K, Ota T , Iida J, Nakanishi Y, Kishimoto N, Kishimoto T
Received 24 August 2016
Accepted for publication 14 November 2016
Published 12 December 2016 Volume 2016:12 Pages 3183—3190
DOI https://doi.org/10.2147/NDT.S120540
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Taro Kishi
Kazuhiko Yamamuro,1 Toyosaku Ota,1 Junzo Iida,2 Yoko Nakanishi,1 Naoko Kishimoto,1 Toshifumi Kishimoto1
1Department of Psychiatry, 2Faculty of Nursing, Nara Medical University School of Medicine, Kashihara, Japan
Aim: Cognitive impairment is an important predictor of functional outcome in patients with attention deficit/hyperactivity disorder (ADHD). However, the neurophysiology of ADHD-related cognitive impairments remains unclear. Event-related potentials (ERPs) represent the noninvasive measurement of neural correlates of cognitive function. Mismatch negativity (MMN) is an ERP component that is presumed to index the preattentive monitoring of changes in the auditory environment.
Materials and methods: Previous studies have shown altered MMN amplitude and latency in patients with ADHD. However, little is known about the relationship between MMN and ADHD-symptom severity. To address this, we measured the amplitude and latency of MMN in ERPs and assessed correlations with the clinical severity of ADHD, as measured by the ADHD Rating Scale IV – Japanese version. Participants were 51 treatment-naïve children and adolescents with ADHD (mean age 10.42±3.35 years) and 15 normally developing age- and sex-matched children (mean age 11.8±3.36 years).
Results: In the ADHD group, MMN amplitudes were attenuated at the central electrode and MMN latencies prolonged at the parietal electrode (Pz) relative to those in the control group. Furthermore, MMN amplitudes at Pz were negatively correlated with ADHD full-scale and hyperactivity–impulsivity and inattention subscale scores, and MMN latency at Pz was positively correlated with ADHD hyperactivity–impulsivity subscale scores.
Conclusion: Our data suggest that MMN reflects the severity of ADHD symptoms in children and adolescents, and provides support for the use of ERPs in evaluating ADHD symptoms in patients.
Keywords: attention deficit/hyperactivity disorder, event-related potentials, mismatch negativity, symptom severity, relationship
Introduction
Attention deficit/hyperactivity disorder (ADHD) is a highly prevalent condition in children and adolescents that is characterized by inattention, hyperactivity, impulsivity, and abnormalities in one or more cognitive processes. With regard to cognitive abnormalities, children with ADHD have difficulties inhibiting responses, and consequently tend to make more errors. These deficits are similar to those reported for patients with frontal lobe lesions.1,2 Indeed, several neuroimaging studies have reported that deficits in inhibitory control are associated with structural and functional disorganization with respect to the connectivity between the basal ganglia and the prefrontal cortex (PFC) in individuals with ADHD.3,4
Event related potentials (ERPs) represent a sensitive, noninvasive reflection of covert brain activity. ERPs are obtained by measuring voltage fluctuations in electroencephalography (EEG) data, time-locked to an event of interest. The P300 is a well-characterized late-ERP component that has been implicated in various psychiatric disorders. It is thought to reflect executive and attentional function, including the updating of working memory, event categorization, and attentional reorientation.5 Previous studies have reported that the P300 amplitude is lower in children with ADHD compared with control participants.6–9 In addition, several studies have reported that the latency of the P300 is longer in children with ADHD compared with controls.9,10 Previously, our group examined the P300 component in treatment-naïve children and adolescents with ADHD during an auditory oddball task, and found a positive correlation between ADHD-subscale rating and P300 amplitude at the central electrode (Cz), as well as P300 latency at the frontal electrode (Fz), Cz, and the parietal electrode (Pz).11 These data suggest that the characteristics of P300 can be correlated with the severity of ADHD symptoms in patients. However, the P300 may reflect a late stage of the inhibitory process,12 and is thus likely to be affected by preceding cognitive factors. For this reason, mismatch negativity (MMN), which is a pre-P300 component that provides an index of preattentive auditory sensory memory function, has become the focus of recent research. MMN is thought to reflect information processing more accurately than the P300, and is closely related to attention deficits. MMN is generated in response to occasional variations (eg, duration, frequency, intensity) in acoustic stimuli, and occurs about 100–200 ms after the onset of deviant stimulation, with peak amplitudes observed at the frontocentral leads.13,14 Additionally, MMN reflects an automatic cerebral discrimination process that is not under attentional control.15 Several studies have demonstrated that methylphenidate, an ADHD medication, normalizes decreased MMN amplitudes in children with ADHD.16 Correspondingly, Sawada et al reported a correlation between ADHD severity and MMN components in children with pervasive developmental disorder with ADHD-like symptoms.17 However, no studies have directly examined whether MMN amplitude and latency vary according to the severity of ADHD symptoms in ADHD-only patients.
To address this, we evaluated the relationship between changes in MMN and the severity of ADHD symptoms in treatment-naïve children and adolescent patients with ADHD. We hypothesized that more severe ADHD symptoms would be associated with lower MMN amplitude and longer MMN latency. To our knowledge, our study is the first to investigate direct correlations among MMN amplitude, latency, and symptom severity in children and adolescents with ADHD.
Materials and methods
Participants
We recruited 51 patients with ADHD (41 boys, mean age 9.74±3.08 years, and ten girls, mean age 13.2±3.5 years) from the outpatient clinic at the Department of Psychiatry at Nara Medical University, Japan (Table 1). We recruited 15 healthy individuals (eleven boys, mean age 11.8±2.77 years, and four girls, mean age 11.8±3.77 years) as controls. We confirmed the absence of psychiatric illness in the control group using a standard clinical assessment that included a psychiatric evaluation and a structured diagnostic interview (Structured Clinical Interview for Diagnostic and Statistical Manual of Mental Disorders, 4th edition (DSM-IV) Axis Disorders Nonpatient Edition). This study was approved by the Institutional Review Board at Nara Medical University and carried out in accordance with the Declaration of Helsinki. All study participants or their legal guardians provided written informed consent for participation prior to initiation of the study.
Patients were deemed eligible for inclusion if they had a diagnosis of ADHD according to the DSM-IV-Text Revision (DSM-IV-TR) as described in the Kiddie Schedule for Affective Disorders and Schizophrenia for School-Age Children – Present and Lifetime Version,18 as evaluated by one or more experienced psychiatrists. Exclusion criteria were as follows: presence of a neurological disorder, head injury, serious medical condition, or history of substance abuse/dependence. A trained psychologist assessed intelligence using the Wechsler Intelligence Scale for Children, fourth edition, and participants with a full-scale intelligence quotient (FIQ) score below 70 were also excluded. None of the included participants had comorbid obsessive–compulsive disorder, major depressive disorder, schizophrenia, or epilepsy. Five patients had comorbid autism-spectrum disorder, one patient had comorbid tic disorder, and one patient had comorbid conduct disorder. All patients included were naïve to medical treatment.
Assessment of ADHD symptoms
We evaluated ADHD symptoms and symptom severity in all patients using the ADHD Rating Scale IV – Japanese version (ADHD-RS-IV-J) of the ADHD-RS-IV – home version.19 The ADHD-RS-IV-J is an 18-item scale based on the DSM-IV-TR, and is reliable and easy to administer for the assessment of ADHD symptoms. Each statement on the ADHD-RS-IV-J is rated on a 4-point Likert scale (never or rarely, sometimes, often, or very often), and the scale yields an ADHD-RS-IV-J full (ARF) score, an ADHD-RS-IV-J inattention subscale (ARI) score, and an ADHD-RS-IV-J hyperactivity–impulsivity subscale (ARH) score, where higher scores represent more severe ADHD symptoms.
Measurement of ERPs
Based on guidelines for the measurement of evoked potentials, we elicited MMN components using an auditory oddball task.20 We used a Multi Stim II auditory stimulus system (NEC, Tokyo, Japan) to present stimuli to both ears of the participants through headphones. Standard stimuli were 1,000 Hz tone bursts (P=0.9), and deviant stimuli were 1,100 Hz bursts (P=0.1). Stimuli were presented for 50 ms at 500 ms intervals and at 80 dB intensities. Frequent and infrequent stimuli were presented in a randomized fashion. MMN components were measured while participants read books or magazines of their choice. The participants were asked not to pay attention to the auditory stimuli.
Recording and analyses
ERPs were recorded with an MEB 2200 evoked potential-measuring system (Nihon Kohden, Tokyo, Japan). EEG readings were recorded at the Fz, Cz, Pz, C3, and C4 positions on the scalp using disk electrodes. All electrodes were re-referenced off-line to the average of two mastoid electrodes. Electrode impedance was set to ≤5 kΩ. MMN was analyzed between the 50 ms prestimulus and the 360 ms poststimulus. Artifact-free responses to stimuli were summated and averaged for EEG-amplitude data ≥100 μV. To reduce high-frequency content irrelevant to the components of interest, a digital 0.5–70 Hz band-pass filter (attenuation by 12 dB/octave) was applied to all data prior to analysis. Finally, data were corrected for eye-movement artifacts.21
The duration of each auditory oddball task was 250 seconds, and infrequent and frequent stimuli were presented 50 and 450 times, respectively. The sample rate was 5,000 Hz. The 450 responses to frequent standard stimuli and the 50 responses to infrequent deviant stimuli were averaged separately, and a waveform was calculated as the difference between the averaged waveforms (frequent minus infrequent). The MMN was identified from the difference waveform as a negative wave with a peak latency between 100 ms and 250 ms, and its latency and amplitude were recorded. To prevent participants from habituating to the stimuli, each trial was conducted only once.
Statistical analyses
Statistical calculations were conducted with the assistance of PASW Statistics 18.0 J for Windows (SPSS, Chicago, IL, USA). Data are expressed as means ± standard deviation (SD). We calculated Spearman’s correlation coefficient (ρ) for the relationships between ADHD-RS-IV-J scores (including ARF, ARI, and ARH subscale scores) and electrophysiological variables. Bonferroni-adjusted P-values are reported. P-values <0.05 were considered to be statistically significant.
Results
Demographic data
Age, sex, FIQ, and ADHD-RS-IV-J scores, including ARF, ARI, and ARH subscale scores, are shown in Table 1. The participant groups did not differ in terms of mean age (t=−0.63, df=64; P=0.26), sex (χ2=0.01, df=1; P=0.97), or FIQ (t=−0.68, df=64; P=0.25). The mean ARF, ARH, and ARI subscale scores of patients with ADHD were 27.37 (SD 14.35, range 6–51), 11.57 (SD 8.13, range 0–26), and 15.8 (SD 7.59, range 2–27), respectively.
Comparison of MMN-component characteristics between patients with ADHD and control participants
Consistent with previous reports,10,22,23 we found that the grand average of the MMN amplitude in the ADHD group was significantly smaller than that in the control group at Cz (t=−1.97, df=64; P<0.05). Also, we found that the grand average of the MMN latency in the ADHD group was significantly longer than that in the control group at Pz (t=−2.33, df=64; P<0.05) (Table 2 and Figure 1).
Correlation between MMN-component characteristics and ADHD-RS-IV-J subscale scores
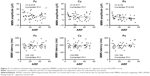
We calculated Spearman correlation coefficients (with Bonferroni-adjusted P-values) for MMN amplitude and latency, as well as ADHD-RS-IV-J subscale scores (Table 3 and Figures 2–4). We identified negative correlations between the amplitude of MMN at Pz and ARF (ρ=−0.32, Bonferroni-corrected P<0.05), ARH (ρ=−0.322, Bonferroni-corrected P<0.05), and ARI (ρ=−0.295, Bonferroni-corrected P<0.05) scores. Furthermore, we found positive correlations between ARH scores and MMN latency at Pz (ρ=0.33, Bonferroni-corrected P<0.05).
Discussion
To the best of our knowledge, this is the first study to investigate the relationship between MMN characteristics and the clinical severity of ADHD in treatment-naïve children and adolescents. As mentioned, MMN is produced in the frontal cortex in association with shifts in attention following the automatic detection of changes in stimuli by the auditory cortex.24,25 Accordingly, MMN is a preattentive ERP component. Indeed, MMN amplitudes have been suggested to reflect preattentive cognitive operations.26 Previous studies have indicated that MMN has reduced amplitude and prolonged latency in children with ADHD relative to control participants.10,22,23 MMN abnormalities have also been reported in several psychiatric disorders, including schizophrenia,27 bipolar affective disorder,28 and major depression.29 Furthermore, MMN has been posited as an index of general cognitive decline in a broad spectrum of clinical disorders.13 Our data are in agreement with these findings: in the present study, we observed that reductions in the MNN amplitude at Pz correlated with ADHD-symptom severity, as measured by the scores for all subscales of the ADHD-RS-IV-J. Additionally, the MMN latency at Pz was positively correlated with the severity of hyperactivity–impulsivity symptoms, suggesting that MMN latency may be a specific indicator of cognitive abnormality in children and adolescents with ADHD.
Neuropsychological theories of ADHD highlight the role of impaired frontal lobe function, especially in the PFC. Functional magnetic resonance imaging studies of patients with ADHD have indicated abnormal activity in the dorsolateral and ventrolateral PFC.30,31 These findings are consistent with the observation that working memory, which is thought to primarily involve the PFC, is a core cognitive function that is affected in individuals with ADHD.32 On the other hand, patients with ADHD have been found to have increased activity in the parietal lobe,33,34 an area that plays a role in attention.35 Our findings of significant correlations among MMN-component characteristics over the PFC and the clinical severity of ADHD symptoms emphasize the relevance of the PFC in ADHD.
In patients with schizophrenia, reports about a negative correlation between MMN amplitude and symptom severity have been inconsistent. However, MMN has been consistently associated with scores on the Global Assessment of Functioning scale25,36,37 and other measurements of social and occupational status.38,39 Sawada et al examined MMN components during an auditory oddball task in ten individuals with pervasive developmental disorder with ADHD symptoms.17 They found that scores on the ADHD-RS-IV-J tended to be positively associated with MMN latency and were significantly and strongly negatively correlated with MMN amplitude. We found that lower MMN amplitude and prolonged MMN latency were correlated with the severity of subdomains of the ADHD-RS-IV-J (ie, the ARH). These findings indicate that MMN may be a common index of preattentive auditory sensory memory function in several psychiatric disorders, including ADHD.
There are some limitations that should be taken into consideration when interpreting our findings. First, our sample size was relatively small, and six patients with ADHD had comorbid psychiatric illnesses, including autism-spectrum disorder (n=4), tic disorder (n=1), and conduct disorder (n=1). Future studies using a larger cohort are needed to validate our findings and to determine whether MMN-component characteristics can distinguish patients with ADHD from those with other neurodevelopmental disorders. Second, since our study evaluated ADHD symptoms using only the ADHD-RS-IV-J, future studies employing other neuropsychological tests would be helpful in increasing the strength of our hypothesis. Third, the methods employed in our study did not allow a focus on altered patterns of connectivity. Recently, functional magnetic resonance imaging studies have produced evidence supporting the necessity of network integration during response inhibition, and have confirmed altered functional connectivity in individuals with ADHD.40–42 Fourth, the MMN baseline interval used in our study was short, which might have reduced the reliability of the signal. However, our group has taken ERP measurements using this method during several investigations of psychiatric disorders,17,43,44 and these findings were consistent with those of our previous studies. Given these limitations, future studies should be conducted to determine whether abnormalities in the frontal lobe are resultant from or causative of altered functional connectivity.
Conclusion
The present study demonstrates that changes in MMN amplitude and latency can predict the severity of ADHD symptoms, and thus indicates that these may be important signals for the neurophysiological mechanisms underlying ADHD. Furthermore, our findings support the notion that ERPs represent a clinically useful and noninvasive method for estimating disease severity in children and adolescents with ADHD.
Acknowledgments
We wish to thank the study participants for their valuable contribution. The authors would also like to thank NEC for the NEC Multi Stim II equipment and their skilled technical and methodological support.
Author contributions
KY, TO, JI, YN, NK, and TK were involved in data collection and wrote the first draft of the manuscript. JI and TK supervised the entire project, were critically involved in study design, and contributed to the editing of the final manuscript. All authors contributed toward data analysis, drafting and revising the paper and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Iaboni F, Douglas VI, Baker AG. Effects of reward and response costs on inhibition in ADHD children. J Abnorm Psychol. 1995;104(1):232–240. | ||
Trommer BL, Hoeppner JA, Lorber R, Armstrong KJ. The go-no-go paradigm in attention deficit disorder. Ann Neurol. 1988;24(5):610–614. | ||
Casey BJ, Castellanos FX, Giedd JN, et al. Implication of right frontostriatal circuitry in response inhibition and attention-deficit/hyperactivity disorder. J Am Acad Child Adolesc Psychiatry. 1997;36(3):374–383. | ||
Castellanos FX. Toward a pathophysiology of attention-deficit/hyperactivity disorder. Clin Pediatr (Phila). 1997;36(7):381–393. | ||
Polich J. Updating P300: an integrative theory of P3a and P3b. Clin Neurophysiol. 2007;118(10):2128–2148. | ||
Frank Y, Seiden JA, Napolitano B. Event-related potentials to an “oddball” auditory paradigm in children with learning disabilities with or without attention deficit hyperactivity disorder. Clin Electroencephalogr. 1994;25(4):136–141. | ||
Kutas M, McCarthy G, Donchin E. Augmenting mental chronometry: the P300 as a measure of stimulus evaluation time. Science. 1977;197(4305):792–795. | ||
Magliero A, Bashore TR, Coles MG, Donchin E. On the dependence of P300 latency on stimulus evaluation processes. Psychophysiology. 1984;21(2):171–186. | ||
Ozdag MF, Yorbik O, Ulas UH, Hamamcioglu K, Vural O. Effect of methylphenidate on auditory event related potential in boys with attention deficit hyperactivity disorder. Int J Pediatr Otorhinolaryngol. 2004;68(10):1267–1272. | ||
Winsberg BG, Javitt DC, Silipo GS, Doneshka P. Mismatch negativity in hyperactive children: effects of methylphenidate. Psychopharmacol Bull. 1993;29(2):229–233. | ||
Yamamuro K, Toyosaku O, Iida J, et al. Event related potentials correlate with the severity of child and adolescent patients with attention deficit/hyperactivity disorder. Neuropsychobiology. 2016;73(3):131–138. | ||
Nieuwenhuis S, Yeung N, van den Wildenberg W, Ridderinkhof KR. Electrophysiological correlates of anterior cingulate function in a go/no-go task: effects of response conflict and trial type frequency. Cogn Affect Behav Neurosci. 2003;3(1):17–26. | ||
Naatanen R, Kujala T, Escera C, et al. The mismatch negativity (MMN): a unique window to disturbed central auditory processing in ageing and different clinical conditions. Clin Neurophysiol. 2012;123(3):424–458. | ||
Näätänen R, Paavilainen P, Rinne T, Alho K. The mismatch negativity (MMN) in basic research of central auditory processing: a review. Clin Neurophysiol. 2007;118(12):2544–2590. | ||
Jonkman LM, Kemner C, Verbaten MN, et al. Event-related potentials and performance of attention-deficit hyperactivity disorder: children and normal controls in auditory and visual selective attention tasks. Biol Psychiatry. 1997;41(5):595–611. | ||
Sawada M, Iida J, Ota T, et al. Effects of osmotic-release methylphenidate in attention-deficit/hyperactivity disorder as measured by event-related potentials. Psychiatry Clin Neurosci. 2010;64(5):491–498. | ||
Sawada M, Negoro H, Iida J, Kishimoto T. Pervasive developmental disorder with attention deficit hyperactivity disorder-like symptoms and mismatch negativity. Psychiatry Clin Neurosci. 2008;62(4):479–481. | ||
Kaufman J, Birmaher B, Brent D, et al. Schedule for Affective Disorders and Schizophrenia for School-Age Children – Present and Lifetime Version (K-SADS-PL): initial reliability and validity data. J Am Acad Child Adolesc Psychiatry. 1997;36(7):980–988. | ||
DuPaul GJ, Power TG, Anastopoulos AD, Reid R. ADHD Rating Scale-IV: Checklists, Norms, and Clinical Interpretation. New York: Guilford Press; 1998. | ||
Picton TW, Bentin S, Berg P, et al. Guidelines for using human event-related potentials to study cognition: recording standards and publication criteria. Psychophysiology. 2000;37(2):127–152. | ||
Gratton G, Coles MG, Donchin E. A new method for off-line removal of ocular artifact. Electroencephalogr Clin Neurophysiol. 1983;55(4):468–484. | ||
Kemner C, Verbaten MN, Koelega HS, et al. Event-related brain potentials in children with attention-deficit and hyperactivity disorder: effects of stimulus deviancy and task relevance in the visual and auditory modality. Biol Psychiatry. 1996;40(6):522–534. | ||
Kilpelaäinen R, Partanen J, Karhu J. Reduced mismatch negativity (MMN) suggests deficits in pre-attentive auditory processing in distractible children. Neuroreport. 1999;10(16):3341–3345. | ||
Jahshan C, Wynn JK, Breitmeyer BG, Green MF. Nonconscious and conscious color priming in schizophrenia. J Psychiatr Res. 2012;46(10):1312–1317. | ||
Jahshan C, Cadenhead KS, Rissling AJ, Kirihara K, Braff DL, Light GA. Automatic sensory information processing abnormalities across the illness course of schizophrenia. Psychol Med. 2012;42(1):85–97. | ||
Umbricht D, Krljes S. Mismatch negativity in schizophrenia: a meta-analysis. Schizophr Res. 2005;76(1):1–23. | ||
Perez VB, Woods SW, Roach BJ, et al. Automatic auditory processing deficits in schizophrenia and clinical high-risk patients: forecasting psychosis risk with mismatch negativity. Biol Psychiatry. 2014;75(6):459–469. | ||
Catts SV, Shelley AM, Ward PB, et al. Brain potential evidence for an auditory sensory memory deficit in schizophrenia. Am J Psychiatry. 1995;152(2):213–219. | ||
Umbricht D, Koller R, Schmid L, et al. How specific are deficits in mismatch negativity generation to schizophrenia? Biol Psychiatry. 2003;53(12):1120–1131. | ||
Rubia K, Overmeyer S, Taylor E, et al. Hypofrontality in attention deficit hyperactivity disorder during higher-order motor control: a study with functional MRI. Am J Psychiatry. 1999;156(6):891–896. | ||
Vaidya CJ, Austin G, Kirkorian G, et al. Selective effects of methylphenidate in attention deficit hyperactivity disorder: a functional magnetic resonance study. Proc Natl Acad Sci U S A. 1998;95(24):14494–14499. | ||
Kofler MJ, Rapport MD, Bolden J, Sarver DE, Raiker JS. ADHD and working memory: the impact of central executive deficits and exceeding storage/rehearsal capacity on observed inattentive behavior. J Abnorm Child Psychol. 2010;38(2):149–161. | ||
Schweitzer JB, Faber TL, Grafton ST, Tune LE, Hoffman JM, Kilts CD. Alterations in the functional anatomy of working memory in adult attention deficit hyperactivity disorder. Am J Psychiatry. 2000;157(2):278–280. | ||
Durston S, Tottenham NT, Thomas KM, et al. Differential patterns of striatal activation in young children with and without ADHD. Biol Psychiatry. 2003;53(10):871–878. | ||
Petersen SE, Posner MI. The attention system of the human brain: 20 years after. Annu Rev Neurosci. 2012;35:73–89. | ||
Kiang M, Light GA, Prugh J, Coulson S, Braff DL, Kutas M. Cognitive, neurophysiological, and functional correlates of proverb interpretation abnormalities in schizophrenia. J Int Neuropsychol Soc. 2007;13(4):653–663. | ||
Kawakubo Y, Kasai K. Support for an association between mismatch negativity and social functioning in schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry. 2006;30(7):1367–1368. | ||
Rasser PE, Schall U, Todd J, et al. Gray matter deficits, mismatch negativity, and outcomes in schizophrenia. Schizophr Bull. 2011;37(1):131–140. | ||
Wynn JK, Sugar C, Horan WP, Kern R, Green MF. Mismatch negativity, social cognition, and functioning in schizophrenia patients. Biol Psychiatry. 2010;67(10):940–947. | ||
Fair DA, Posner J, Nagel BJ, et al. Atypical default network connectivity in youth with attention-deficit/hyperactivity disorder. Biol Psychiatry. 2010;68(12):1084–1091. | ||
Mennes M, Potler NV, Kelly C, Di Martino A, Castellanos FX, Milham MP. Resting state functional connectivity correlates of inhibitory control in children with attention-deficit/hyperactivity disorder. Front Psychiatry. 2011;2:83. | ||
van Rooij D, Hartman CA, Mennes M, et al. Altered neural connectivity during response inhibition in adolescents with attention-deficit/hyperactivity disorder and their unaffected siblings. Neuroimage Clin. 2015;7:325–335. | ||
Yamamuro K, Ota T, Nakanishi Y, et al. Event-related potentials in drug-naive pediatric patients with obsessive-compulsive disorder. Psychiatry Res. 2015;230(2):394–399. | ||
Yamamuro K, Ota T, Iida J, et al. Event-related potentials reflect the efficacy of pharmaceutical treatments in children and adolescents with attention deficit/hyperactivity disorder. Psychiatry Res. 2016;242:288–294. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.