Back to Journals » International Journal of Women's Health » Volume 14
Association of Higher Educational Attainment on Antenatal Care Utilization Among Pregnant Women in East Africa Using Demographic and Health Surveys (DHS) from 2010 to 2018: A Multilevel Analysis
Authors Raru TB , Ayana GM , Zakaria HF , Merga BT
Received 21 November 2021
Accepted for publication 19 January 2022
Published 1 February 2022 Volume 2022:14 Pages 67—77
DOI https://doi.org/10.2147/IJWH.S350510
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Marleen van Gelder
Temam Beshir Raru,1 Galana Mamo Ayana,1 Hamdi Fekredin Zakaria,1 Bedasa Taye Merga2
1Department of Epidemiology and Biostatistics, School of Public Health, Haramaya University, Harar, Ethiopia; 2Department of Public Health and Health Policy, School of Public Health, Haramaya University, Harar, Ethiopia
Correspondence: Temam Beshir Raru, Tel +251 922693210
, Email [email protected]
Introduction: The use of antenatal care (ANC) plays a major role in minimizing maternal and child mortality through effective and appropriate screening, preventive, or treatment intervention. Even though almost all pregnancy-related mortalities are largely preventable through adequate use of ANC, sub-Saharan Africa (SSA), particularly East African Countries, continues to share the largest share of global maternal, and newborn mortality. Therefore, this study assesses if educational attainment is associated with optimal ANC utilization in East Africa.
Methods: A secondary data analysis was done based on Demographic and Health Surveys (DHS) from 2010 to 2018 in the 11 East African Countries. A total weighted sample of 84,660 women who gave birth in the 5 years preceding each country’s DHS survey and had ANC visits were included in this study. Data processing and analysis were performed using STATA 15 software. A multilevel mixed-effect logistic regression model was fitted to examine the association of educational attainment and ANC utilization. Variables with a p-value < 0.05 were declared as significant factors associated with ANC utilization. Model comparison was done based on Akaike and Bayesian Information Criteria (AIC and BIC).
Results: The magnitude of optimal ANC utilization in East African Countries was 56.37% with 95% CI (56.03, 56.69) with the highest optimal ANC utilization in Zimbabwe (80.96%) and the lowest optimal ANC utilization in Rwanda (44.31%). Women who had higher education levels were more likely to have optimal ANC utilization, compared to those with no education (AOR = 2.34; 95 and CI; 2.11– 2.59). Women who had media exposure were more likely to have optimal ANC utilization than those who have no media exposure (AOR = 1.07; 95% CI; 1.03, 1.10).
Conclusion: Antenatal care utilization was low in East African countries. Educational attainment, maternal age, wealth index, birth order, media exposure, and living countries were factors associated with ANC utilization. Efforts to improve antenatal care and other maternal health service utilization in East Africa must take into account these factors. Specifically, working on the access to mass media by women may also improve antenatal care utilization.
Keywords: antenatal care, utilization, education, East Africa, DHS
Introduction
Globally, about 303,000 women died in 2015 because of pregnancy and childbirth complications. Most of these deaths come from poor countries, and there is a huge disparity as compared to the developed countries. For a woman living in sub-Saharan Africa, the lifetime risk of maternal mortality is over 47 times greater than for a woman living in the United States (US).1 In 2013, the World Health Organization (WHO) and US Agency for International Development (USAID) representatives proposed an energetic but accomplished target in the Lancet Global Health to decrease the global mean maternal mortality ratio (MMR) to less than 50 per 100,000 live births by 2035.1
The use of antenatal care (ANC) plays a major role in minimizing maternal and child mortality through effective and appropriate screening, preventive, or treatment interventions.2 In low and middle-income countries, ANC services make a significant improvement in birth outcomes and long-term reductions of child mortality and malnutrition.3 Even if many African countries are still struggling to achieve high coverage of four ANC visits, eight ANC contacts are suggested by WHO.4
By reducing stillbirths and neonatal deaths, ANC had a direct improvement on the survival and health of babies and had indirect improvement by providing an entry point for health encounters with the woman at a critical point in the continuum of care.5 The goal of the ANC package is to prepare for birth and to avoid, identify, mitigate, or treat health issues that affect mothers and babies during pregnancy.5 However, sub-Saharan Africa (SSA) countries account for 19 of the 20 countries with the highest maternal mortality rates.6 Even though almost all pregnancy-related mortalities are largely preventable through adequate use of ANC, SSA, particularly in East African countries, continues to share the largest share of global maternal and newborn mortality.
There is strong evidence suggesting that religion, level of education, occupation, distance from the health facility, residence, country, mass media, maternal age, and wealth index were associated with ANC utilization.7–14 From the previous, many sociocultural factors were associated with late ANC booking.15,16 Among the factors likely to be critical in health promotional activities and health services uptake is educational attainment.17–19
Understanding the factors associated with the utilization of ANC services among pregnant women is needed to design strategies, policies, and interventions to reduce maternal mortality. Previous studies on the utilization of ANC have mainly focused on sub-Saharan Africa20 and specific countries within the region.21–25 Moreover, the association of higher educational attainment with ANC utilization and its mechanisms are not well studied in the region. Therefore, this study aimed to find out if educational attainment is associated with ANC utilization in the 11 East African Countries from 2010 to 2018 using recent Demographic and Health Surveys (DHS).
Methods
Study Setting and Data Source
The United Nations (UN) Statistics Division has subdivided the African continent into five regions. Among these countries, East Africa is the largest region that includes 19 countries (Burundi, Comoros, Djibouti, Ethiopia, Eritrea, Kenya, Madagascar, Malawi, Mauritius, Mozambique, Reunion, Rwanda, Seychelles, Somalia, Somaliland, Tanzania, Uganda, Zambia, and Zimbabwe). This study was a secondary data analysis based on Demographic and Health Surveys (DHS). Of these 19 East African countries, 13 countries have DHS data, whereas 6 (Djibouti, Somalia, Somaliland, Seychelles and Mauritius, Reunion). Among these 13 countries that have DHS data, 2 countries have DHS data that was conducted before 2010 (Eritrea-2002 and Madagascar-2008). In this study, we included 11 countries’ DHS data that was conducted after 2010.
The data of these 11 East African countries were accessed from the demographic health survey (DHS) program official database www.measuredhs.com after authorization was granted through an online request by explaining the goal of our study. We used the individual Record (IR file) data set and extracted the dependent and independent variables. To collect knowledge that is comparable across countries in the world, the DHS program adopts standardized methods involving uniform questionnaires, manuals, and field procedures. DHS is a nationally representative household survey that offers data from a wide variety of population, health, and nutrition tracking and effect assessment measures with face-to-face interviews of women aged 15 to 49. Stratified, multi-stage, random sampling is used in the surveys. In each country, information was obtained from qualified women aged 15 to 49 years. Detailed survey techniques and methods of sampling used to collect data have been recorded elsewhere.26 There are a total of 89,991 women who gave birth in the 5 years preceding each country’s DHS survey. Of these, 84,660 women were reported using ANC service 5 years before the survey, and they are being eligible for our study in which this implies that around 5% of the women in East Africa did not attend ANC at all.
Variables
Outcome Variable
The response (outcome) variable of this study was ANC utilization. The response variable is binary, and it is coded as 1 if women received ANC from skilled healthcare providers (doctors, midwives, nurses, and health officers) at least four times and 0 otherwise.
Independent variables
Independent variables are classified as community and individual-level factors.
Community-level variables: Country (11 countries in East Africa) and residence (urban and rural).
The individual-level variables: Age (maternal age was categorized by 5 years interval as follows: 15–19, 20–24, 25–29, 30–34, 35–39, 40–44, and 45–49 years), level of education (no education, primary education, secondary, and higher education), distance from a health facility (big problem and not a big problem), birth order (1st, 2nd–4th, and ≥5th), mass media exposure was recorded as the frequency of reading newspaper, listening to radio and watching TV (categorized as Has exposure or Has no exposure), and wealth index.
Household wealth is represented by the wealth index (in five categories: poorest, poorer, middle, richer, and richest). Wealth index was constructed using data on a households’ ownership of selected assets, such as television and bicycles, materials used for housing construction, and types of water access and sanitation facilities. The index placed individual households on a continuous scale relative to their wealth status.27
Data Processing and Management
Data processing and analysis were performed using STATA 15 software. The data were weighted using sampling weight, primary sampling unit, and strata before any statistical analysis to restore the representativeness of the survey and to tell the STATA to take into account the sampling design when calculating standard errors to get reliable statistical estimates.
Statistical Analysis
Cross tabulations and summary statistics were conducted to describe the study population. In the first step, bi-variable analysis and cross-tabulations by Pearson’s chi-squared test were used to examine if educational attainment was associated with ANC utilization. Later, since the DHS data have a hierarchical nature, women within a cluster may be more similar to each other than women in the other cluster. Due to this, the assumption of independent observations and equal variance across clusters might be violated. Therefore, an advanced statistical model is required to take into account the between cluster variability to get a reliable standard error and unbiased estimate.
Furthermore, by taking into account the dichotomous nature of the outcome variable, multilevel mixed-effect logistic regression was fitted. Model comparison was done based on Akaike and Bayesian Information Criteria (AIC and BIC). A mixed-effect model with the lowest Information Criteria (AIC and BIC) was selected.
The individual and community-level variables associated with ANC utilization were checked independently in the bi-variable multilevel mixed-effect logistic regression model, and variables that were statistically significant at p-value 0.20 in the bi-variable multilevel mixed-effects logistic regression analysis were considered for the final individual and community-level model adjustments. In the multivariable multilevel mixed-effect analysis, variables with a p-value≤0.05 were declared as significant determinants of ANC utilization. Intra-class correlation coefficients (ICC) were used to check whether or not the multilevel model is appropriate and how much of the overall variation in the response is explained by clustering.
Four models were fitted. The first was the null model that did not include exposure variables, which were used to verify community variance and provide evidence to assess random effects at the community level. Then, Model-I was the multivariable model adjustment for individual-level variables, and Model-II was adjusted for community-level factors. In Model-III, the outcome variable was equipped with potential candidate variables from both individual and community-level variables.
The fixed effects (a measure of association) were used to estimate the association between the optimal ANC utilization and explanatory variables and expressed as an odds ratio with a 95% confidence interval. Regarding the measures of variation (random-effects), community-level variance with standard deviation and intra-cluster correlation coefficient (ICC) was used.
Results
Participation and Women’s Characteristics
A total of 84,660 women who gave birth in the 5 years preceding each country’s DHS survey and having ANC visits were included for the final analysis. The majority of women 21,775 (25.72%) lie in the age group of 25–29. Almost three-fourths of the women were from rural residents 62,945 (74.35%). More than two-thirds of the women had a media exposure 57,951 (68.45%). Most of the women included were from Kenya 13,850 (16.36%) and the smallest number of women included from Comoros 1921 (2.27%) (Table 1).
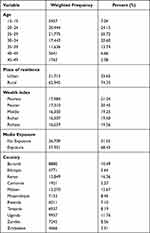 |
Table 1 Basic Characteristic of Women’s Attending Antenatal Clinics in the 11 East African Countries from 2010 to 2018 (n = 84,660) |
Educational Attainment
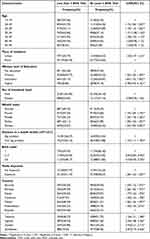
The proportion of women who attended at least four ANC visits was 56.37% with 95% CI (56.03, 56.69). The highest and lowest optimal ANC utilization was reported in Zimbabwe 80.96% with 95% CI (79.81, 82.06) and Rwanda 44.31% with 95% CI (43.06, 45.56), respectively. Educational attainment of the women was varied significantly between rural and urban residents, in which the urban residents had higher educated participants. There is a significant association between optimal ANC utilization and the wealth index of the mothers. The majority 53.76% of the participants were reported to have primary education as their highest educational attainment, while 19.61% had no education. Educational attainment was significantly associated with optimal ANC utilization. The odds of optimal ANC utilization were 3.78 (Crude odds ratio (COR) = 3.78; 95% CI; 3.44–4.16) times higher among the women who have higher education level, 1.81 (COR = 1.81; 95% CI; 1.72–1.90) times higher among the women who have secondary education, and 1.25 (COR = 1.25; 95% CI; 1.21–1.30) times higher among the women who have primary education, compared to those who had no education (Table 2).
Determinants of ANC Utilization
Result of the Random Effects
The results of the null model revealed that there was statistically significant variability in the odds of optimal ANC utilization with community variance of 48.90% and the ICC in the null model suggested that 12.94% of the total variability in the optimal ANC utilization was ascribed to the differences between communities. In the full model (model adjusted for both individual and community-level factors) community variance = 0.30; SE 0.01 remained significant but reduced and 8.38% of the total variance of optimal ANC utilization can be ascribed to the community (Table 3).
 |  |  |
Table 3 Multivariable Multilevel Mixed-Effect Logistic Regression Analysis of Factors Associated with ANC Utilization in East African Countries from 2010 to 2018 |
Result of the Fixed Effects
The model with smaller AIC and BIC was best to fit the data, and the interpretation of the fixed effects was based on this model. Model-III was adjusted for both individual and community-level factors that have small AIC and BIC, compared to other models, and this model fits the data well. In the multivariable analysis respondent’s age group, respondent’s education, wealth index, birth intervals, media exposure, and living country were significantly associated with the ANC utilization in East Africa at a 5% level of significance.
The odds of optimal ANC utilization were 1.72 (AOR = 1.71; 95% CI; 1.51–1.95) times higher among the women in the age group of 45–49, compared to the women in the age group of 15–19. This suggests that the higher the age of the woman, the more likely the woman would have optimal ANC utilization. The women who have higher education levels were 2.34 times more likely to have optimal ANC utilization, compared to those with no education (AOR = 2.34; 95 and CI; 2.11–2.59). Richest women were 1.46 times more likely to have optimal ANC utilization than women who are poorest (AOR = 1.46; 95% CI; 1.37–1.1.56). Women who have media exposure are 1.07 times more likely to have optimal ANC utilization than their counterparts (AOR = 1.07; 95% CI; 1.03, 1.10). Pregnant women living in Zimbabwe, Zambia, and Uganda are 5.3, 2.6, and 2.2 times more likely to have optimal ANC utilizations, respectively, than the women living in Rwanda; Zimbabwe (AOR = 5.34; 95% CI; 4.72–6.03), Zambia (AOR = 2.60; 95% CI; 2.34–2.87), Uganda (AOR = 2.19; 95% CI; 1.99–2.40) (Table 3).
Discussion
The overall aim of this study was to investigate the association between ANC utilization and educational attainments in the 11 East African Countries from 2010 to 2018 using the last Demographic and Health Surveys dataset of each country. The pooled magnitude of ANC utilization in East African Countries was 56.37% with 95% CI (56.03, 56.69) with the highest optimal ANC utilization in Zimbabwe (80.96%) and the lowest optimal ANC utilization in Rwanda (44.31%). This finding is comparable with the study conducted in Nepal,28 and the study conducted in seven countdown countries,29 but lower than finding reported at Nigeria National Hospital,30 Northern Nigeria,31 Uganda,12 and Ethiopia.32 This might be attributed to differences in sample size, socioeconomic and sociocultural aspects of the society. Even if majorities (99%) of pregnant women in Rwanda attend ANC at least once, only 44% of them complete all four visits.33,34 This low optimum ANC utilization is due to unintended pregnancy, of which nearly 47% of all pregnancies are estimated to be.33,35
The odds of optimal ANC utilization were higher among women of older age groups (45–49) compared to women of younger age groups (15–19). This finding is supported by a systematic review conducted in sub-Saharan Africa,20 Ethiopia,14 and Uganda.12 This might be explained by, as the age of the mother increases; they might have better knowledge, understanding, and experience of pregnancy and pregnancy-related complications.13
We found evidence suggesting that the higher education level of the woman was a significant factor in determining optimal ANC utilization. This was supported by similar findings.13,17–19 This might be because the educated women most likely have adequate knowledge on ANC services and understand the importance of early booking for ANC as well as attending the recommended four visits. Thus, they tend to value ANC services and will take advantage of this compared to women with lower education. In addition, women with better educational status are capable of identifying danger signs and easily understand the adverse outcome of avoiding the recommended ANC service. Moreover, education may be useful for some women to overcome gender-specific discrimination and barriers such as domestic violence, female genital mutilation, and others, all of which are significant predictors of ANC utilization.36,37 Besides being a major determinant of socioeconomic status, education has the potential to empower women and increase their health literacy.38,39 Thus, long-term public health strategies should reach beyond health and take a comprehensive view, for example, including the enhancement of women’s education.
Women who were the richest were more likely to utilize ANC than the poorest women. This finding is consistent with a study conducted in Ethiopia,14 and elsewhere28,29 This is because women in better socioeconomic status have more ability to pay for both direct and indirect healthcare costs. Simkhada et al identified the cost of travel and services as the main barriers to accessing ANC in most low- and middle-income countries.17 In addition, poorer women cannot afford to spend when they have family and household duties and to attend to, even if ANC services and transport are free.40
Women exposed to media were more likely to have ANC utilization than their counterparts. This finding is in line with a population-based study conducted in Nepal using the DHS data,28 in a systematic review conducted in developing countries17 and a systematic review and meta-analysis study conducted in Ethiopia.7 Media such as TV and radio can promote healthy behavioral changes by frequently broadcasting programs and public service announcements supported by the government or non-state actors that describe the benefits of timely initiation, and utilization of ANC and other maternal healthcare services.41 They also disseminate health information sponsored by the government such as announcements of locations and working hours of health facilities with free maternal healthcare services, which encourage women and their partners to take practical action towards healthy behavioral changes.41
Higher birth order was negatively associated with ANC utilization. Women with higher birth order had lower odds of ANC utilization. This finding is supported by a study conducted in Ethiopia,14,18,19 and seven countdown countries.29 This might be because women with higher birth order may perceive themselves as being capable of handling their pregnancy during the early stages and will not see the need to seek ANC, thus endangering their lives and that of their unborn babies.42
Strengths and Limitations of the Study
The study had certain limitations. The cross-sectional nature of the data limited the possibility of drawing any conclusion from the analyses about causation. This study only allowed the detection of associations between women’s education, other independent factors, and antenatal care utilization, not causality. As the study depended on women’s reports, there may be a potential for recall bias. Despite these limitations, the study findings have important implications for research and programmes/interventions aimed at improving antenatal care utilization in East Africa.
Conclusions
Antenatal care utilization was relatively low in East African countries. This study depicts that a higher level of maternal formal education significantly increases the utilization of antenatal care services, even after controlling for other socioeconomic factors. Maternal age, wealth index, birth order, media exposure, and living countries were identified as factors associated with ANC utilization. The strong association of women’s education and household wealth with the utilization of antenatal care services highlights the need for efforts to improve households’ livelihoods and increase girls’ schooling to correct perceptions of the importance of skilled maternal health care. Ensuring adequate ANC regardless of maternal age, birth order of the child, and country of residence of pregnant women could guarantee universal maternal healthcare coverage as devoted to sustainable development goals. Furthermore, working on the access to mass media by women may also improve antenatal care utilization.
Abbreviations
AIC, Akaike Information Criteria; ANC, Antenatal Care; AOR, Adjusted Odds Ratio; BIC, Bayesian Information Criteria; DHS, Demographic and Health Survey; ICC, Intra-class Correlation Coefficient; SSA, sub-Saharan Africa; WHO, World Health Organization.
Data Sharing Statement
The EDHS data sets are open and can be accessed from the Measure DHS website www.measuredhs.com through an online request by explaining the objective of the study. The datasets analyzed during the current study are available from the corresponding author upon reasonable request.
Ethics Approval
Ethical clearance for the current study was obtained from the International Review Board (IRB) of the Demographic and Health Surveys (DHS) Program. Data are available to the general public by request in different formats from the Measure DHS website [www.measuredhsprogram.com]. We applied the Measure DHS by briefly stating the objectives of the study and got permission to download the dataset in STATA format. A permission letter for access to the database was received from the Measure DHS program. The DHS research protocol complies with the Helsinki declaration.
Acknowledgment
We greatly acknowledge the Measure DHS program for granting access to the East African DHS data sets.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis, and interpretation, or in all these areas; took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
No funding was obtained for this study.
Disclosure
The authors have declared that they have no conflicts of interest related to this work.
References
1. Jolivet RR, Moran AC, O’Connor M, et al. Ending preventable maternal mortality: phase II of a multi-step process to develop a monitoring framework, 2016–2030. BMC Pregnancy Childbirth. 2018;18(1):1–13. doi:10.1186/s12884-018-1763-8
2. Jokhio A, Winter H, Cheng K, Khan K, MacArthur C. Strategies for reducing maternal mortality. Lancet. 2006;368(9553):2122. doi:10.1016/S0140-6736(06)69854-1
3. Kuhnt J, Vollmer S. Antenatal care services and its implications for vital and health outcomes of children: evidence from 193 surveys in 69 low-income and middle-income countries. BMJ Open. 2017;7(11):e017122. doi:10.1136/bmjopen-2017-017122
4. World Health Organization. WHO Recommendations on Antenatal Care for a Positive Pregnancy Experience. World Health Organization; 2016.
5. Lincetto O, Mothebesoane-Anoh S, Gomez P, Munjanja S. Antenatal care. Opportunities for Africa’s newborns: practical data, policy and programmatic support for newborn care in Africa; 2006:55–62.
6. Alvarez JL, Gil R, Hernández V, Gil A. Factors associated with maternal mortality in Sub-Saharan Africa: an ecological study. BMC Public Health. 2009;9(1):1–8. doi:10.1186/1471-2458-9-462
7. Adewuyi EO, Auta A, Khanal V, et al. Prevalence and factors associated with underutilization of antenatal care services in Nigeria: a comparative study of rural and urban residences based on the 2013 Nigeria demographic and health survey. PLoS One. 2018;13(5):e0197324. doi:10.1371/journal.pone.0197324
8. Kawungezi P, Akiibua D, Aleni C, et al. Attendance and utilization of antenatal care (ANC) services: multi-center study in upcountry areas of Uganda. Open J Prev Med. 2015;5(3):132–142.
9. Gupta S, Yamada G, Mpembeni R, et al. Factors associated with four or more antenatal care visits and its decline among pregnant women in Tanzania between 1999 and 2010. PLoS One. 2014;9(7):e101893. doi:10.1371/journal.pone.0101893
10. Ali N, Sultana M, Sheikh N, et al. Predictors of optimal antenatal care service utilization among adolescents and adult women in Bangladesh. Health Serv Res Managerial Epidemiol. 2018;5:2333392818781729. doi:10.1177/2333392818781729
11. Tessema ZT, Animut Y. Spatial distribution, and determinants of an optimal ANC visit among pregnant women in Ethiopia: further analysis of 2016 Ethiopia demographic health survey. BMC Pregnancy Childbirth. 2020;20(1):1–13. doi:10.1186/s12884-020-2795-4
12. Atuhaire S, Mugisha J. Determinants of antenatal care visits and their impact on the choice of birthplace among mothers in Uganda: a systematic review. Obstet Gynecol Int J. 2020;11(1):77–81. doi:10.15406/ogij.2020.11.00492
13. Ayalew TW, Nigatu AM. Focused antenatal care utilization and associated factors in Debre Tabor Town, Northwest Ethiopia, 2017. BMC Res Notes. 2018;11(1):1–6. doi:10.1186/s13104-018-3928-y
14. Ousman SK, Mdala I, Thorsen VC, Sundby J, Magnus JH. Social determinants of antenatal care service use in Ethiopia: changes over a 15-year span. Front Public Health. 2019;7:161. doi:10.3389/fpubh.2019.00161
15. Nwosu BO, Ugboaja J, Obi-Nwosu A, Nnebue C, Ifeadike C. Proximate determinants of antenatal care utilization among women in southeastern Nigeria. Niger J Med. 2012;21(2):196–204.
16. Cresswell JA, Yu G, Hatherall B, et al. Predictors of the timing of initiation of antenatal care in an ethnically diverse urban cohort in the UK. BMC Pregnancy Childbirth. 2013;13(1):1–8. doi:10.1186/1471-2393-13-103
17. Simkhada B, Teijlingen ERV, Porter M, Simkhada P. Factors affecting the utilization of antenatal care in developing countries: a systematic review of the literature. J Adv Nurs. 2008;61(3):244–260. doi:10.1111/j.1365-2648.2007.04532.x
18. Tsegaye B, Ayalew M. Prevalence and factors associated with antenatal care utilization in Ethiopia: an evidence from demographic health survey 2016. BMC Pregnancy Childbirth. 2020;20(1):1–9. doi:10.1186/s12884-020-03236-9
19. Yeneneh A, Alemu K, Dadi AF, Alamirrew A. Spatial distribution of antenatal care utilization and associated factors in Ethiopia: evidence from Ethiopian demographic health surveys. BMC Pregnancy Childbirth. 2018;18(1):1–12. doi:10.1186/s12884-018-1874-2
20. Okedo-Alex IN, Akamike IC, Ezeanosike OB, Uneke CJ. Determinants of antenatal care utilization in sub-Saharan Africa: a systematic review. BMJ Open. 2019;9(10):e031890. doi:10.1136/bmjopen-2019-031890
21. Yaya S, Bishwajit G, Ekholuenetale M, Shah V, Kadio B, Udenigwe O. Timing and adequate attendance of antenatal care visits among women in Ethiopia. PLoS One. 2017;12(9):e0184934. doi:10.1371/journal.pone.0184934
22. Tiruaynet K, Muchie KF. Determinants of utilization of antenatal care services in Benishangul Gumuz Region, Western Ethiopia: a study based on demographic and health survey. BMC Pregnancy Childbirth. 2019;19(1):1–5. doi:10.1186/s12884-019-2259-x
23. Shibre G, Zegeye B, Idriss-Wheeler D, Ahinkorah BO, Oladimeji O, Yaya S. Socioeconomic and geographic variations in antenatal care coverage in Angola: further analysis of the 2015 demographic and health survey. BMC Public Health. 2020;20(1):1–10. doi:10.1186/s12889-020-09320-1
24. Bonono R, Ongolo-Zogo P. Optimizing the use of antenatal care services in Cameroon. Centre for Development of Best Practices in Health–Central Hospital Yaoundé, Cameroon SURE–Supporting the Use of Research Evidence (SURE) for Policy in African Health Systems–is a collaborative project that builds on and supports the Evidence-Informed Policy Network (EVIPNet) in Africa and the Regional East African Community Health (REACH) Policy Initiative. SURE is funded by the European Commission’s 7th Framework Programme; 2012.
25. Halle-Ekane GE, Obinchemti TE, Nzang JLN, et al. Assessment of the content and utilization of antenatal care services in a rural community in Cameroon: a cross-sectional study. Open J Obstet Gynecol. 2014;4(14):846. doi:10.4236/ojog.2014.414119
26. Rutstein SO, Rojas G. Guide to DHS Statistics. Calverton, MD: ORC Macro; 2006:38.
27. Central Statistical Agency Ethiopia. Ethiopia demographic and health survey 2016. Addis Ababa, Ethiopia, and Rockville, Maryland, USA: CSA and ICF; 2016.
28. Joshi C, Torvaldsen S, Hodgson R, Hayen A. Factors associated with the use and quality of antenatal care in Nepal: a population-based study using the demographic and health survey data. BMC Pregnancy Childbirth. 2014;14(1):1–11. doi:10.1186/1471-2393-14-94
29. Saad–Haddad G, DeJong J, Terreri N, et al. Patterns and determinants of antenatal care utilization: analysis of national survey data in seven countdown countries. J Glob Health. 2016;6(1). doi:10.7189/jogh.06.010404
30. Onasoga OA, Afolayan JA, Oladimeij BD. Factor’s influencing utilization of antenatal care services among pregnant women in Ife Central LGA, Osun State Nigeria. Adv Appl Sci Res. 2012;3(3):1309–1315.
31. Kabir M, Iliyasu Z, Abubakar I, Sani A. Determinants of the utilization of antenatal care services in Kumbotso village, Northern Nigeria. Trop Doct. 2005;35(2):110. doi:10.1258/0049475054036814
32. Tekelab T, Chojenta C, Smith R, Loxton D. Factors affecting utilization of antenatal care in Ethiopia: a systematic review and meta-analysis. PLoS One. 2019;14(4):e0214848. doi:10.1371/journal.pone.0214848
33. Manzi A, Munyaneza F, Mujawase F, et al. Assessing predictors of delayed antenatal care visits in Rwanda: a secondary analysis of Rwanda demographic and health survey 2010. BMC Pregnancy Childbirth. 2014;14(1):1–8. doi:10.1186/1471-2393-14-290
34. Påfs J, Musafili A, Binder-Finnema P, Klingberg-Allvin M, Rulisa S, Essén B. ‘They would never receive you without a husband’: paradoxical barriers to antenatal care scale-up in Rwanda. Midwifery. 2015;31(12):1149–1156. doi:10.1016/j.midw.2015.09.010
35. Basinga P, Moore AM, Singh SD, Carlin EE, Birungi F, Ngabo F. Abortion incidence and postabortion care in Rwanda. Stud Fam Plann. 2012;43(1):11–20. doi:10.1111/j.1728-4465.2012.00298.x
36. Banda PC, Odimegwu CO, Ntoimo LF, Muchiri E. Women at risk: gender inequality and maternal health. Women Health. 2017;57(4):405–429. doi:10.1080/03630242.2016.1170092
37. Ragetlie R, Sano Y, Antabe R, Luginaah I. Married women’s experiences of intimate partner violence and utilization of antenatal health care in Togo. Sex Reprod Healthc. 2020;23:100482. doi:10.1016/j.srhc.2019.100482
38. Corroon M, Speizer IS, Fotso J-C, et al. The role of gender empowerment on reproductive health outcomes in urban Nigeria. Matern Child Health J. 2014;18(1):307–315. doi:10.1007/s10995-013-1266-1
39. Dankwah E, Zeng W, Feng C, Kirychuk S, Farag M. The social determinants of health facility delivery in Ghana. Reprod Health. 2019;16(1):1–10. doi:10.1186/s12978-019-0753-2
40. Finlayson K, Downe S. Why do women not use antenatal services in low-and middle-income countries? A meta-synthesis of qualitative studies. PLoS Med. 2013;10(1):e1001373. doi:10.1371/journal.pmed.1001373
41. Fatema K, Lariscy JT. Mass media exposure and maternal healthcare utilization in South Asia. SSM Popul Health. 2020;11:100614. doi:10.1016/j.ssmph.2020.100614
42. Aliyu AA, Dahiru T. Predictors of delayed Antenatal Care (ANC) visits in Nigeria: secondary analysis of 2013 Nigeria Demographic and Health Survey (NDHS). Pan Afr Med J. 2017;26:124.
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

