Back to Journals » Psychology Research and Behavior Management » Volume 13
Anxiety, Depression, Stress, and Decision-Making Among Orphans and Non-Orphans in Pakistan
Authors Shafiq F , Haider SI, Ijaz S
Received 7 January 2020
Accepted for publication 9 March 2020
Published 30 March 2020 Volume 2020:13 Pages 313—318
DOI https://doi.org/10.2147/PRBM.S245154
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Igor Elman
Farah Shafiq,1 Sonia Ijaz Haider,2 Shamaila Ijaz1
1Lahore Institute of Special Care and Attention (LISCA-Private Clinic), Lahore, Punjab, Pakistan; 2Department for Educational Development, The Aga Khan University, Karachi, Sindh, Pakistan
Correspondence: Sonia Ijaz Haider
Department for Educational Development, The Aga Khan University, Karachi, Sindh, Pakistan
Tel +92 213 4864502
Email [email protected]
Purpose: Orphanhood is a time which involves many psychological and emotional problems. Lack of self-determination and inability to take decision puts orphans at risk of anxiety. In Pakistan, there is minimal evidence which explores the relationship between anxiety, depression, stress, and decision-making among orphans. The aim of the study is to explore the relationship between anxiety, depression, stress, and decision-making among orphans and non-orphans adolescents.
Methods: The sample size consisted of 150 orphans and 150 non-orphans adolescents (n=300). The data were collected from different orphanages and schools located in the city of Lahore, Pakistan. The instruments used were Depression, Anxiety & Stress Scales (DASS) and the Adolescent Decision Making Questionnaire (ADMQ). Descriptive statistics was used to determine the mean, standard deviations, and range. Pearson product moment was used to determine the correlation. The independent t test was performed to determine gender differences, and simple regression analysis was used to predict the effect of social interaction anxiety.
Results: The correlation matrix for decision making, stress, anxiety, depression and DASS indicated that decision making has significant correlation with stress (r= 0.30, **p< 0.01), anxiety (r=0.27**, p< 0.01) and depression (r= 0.15*, p< 0.05). Independent t test revealed significant gender differences between orphan and non-orphans (M=9.45, SD=5.06) (M=8.03, SD=3.61) t(217)=2.48 p=0.01 < 0.05. Simple regression analysis indicated that anxiety is a significant predictor of decision making β = 0.276, F= 17.90, p< 0.001.
Conclusion: The study has implications. First, there is a need to raise awareness at governmental and non-governmental institutions towards finding therapeutic programs for orphans. Second, screening for depression and mental and psychological care should be integrated into routine health care provided to orphans. Third, there should be furnishing of life skills training for orphans such as stress management, coping skills, problem-solving, and decision-making skills.
Keywords: orphans, non-orphans, anxiety, depression, stress, decision making
Introduction
The loss of parents during childhood also termed as orphanhood is considered stressful and deemed as a risk factor for poor mental health of children.1 According to a census, there are approximately 153 million adolescents who have lost a mother or a father and 17.8 million of them have lost both parents.2 An orphanhood is a time period which involves many psychological and emotional problems.3 Lack of self-determination and inability to take decisions put them at risk of anxiety.4
Anxiety is defined as a fearful situation in which a person feels hesitant to talk or interact with the feared object,5 and might paralyze intimate relationships,2 and exhibit high anxiety, phobia, emotional and behavioral problems.6 Decision-making is the process of choosing among alternatives, implement a decision and using the subsequent outcome to shape any further decisions associated with the earlier one.7 World Health Organization (WHO) defines depression as a common mental disorder in which symptoms include depressed mood, loss of interest or pleasure, decreased energy, feelings of guilt or low self-worth, disturbed sleep or appetite, and poor concentration.8 Depression prevalence among the orphan adolescents was found to be 36.4%,9 with physical ailments such as digestive problems, sleep disorders, feelings of boredom and helplessness, and social isolation.
Stressful experiences damage their personalities and affect all interpersonal relationships.10 Deficiency in communication causes high negative emotions, poor self-image, low confidence,11 increased level of daily stress,12 poor management of internal and external stressors,13 psychosocial troubles and issues,14 and deficits in creative activities and cognitive motivation. It was further reported that the type of care and gender plays an important role in social interaction anxiety.15,16 It was found that orphans had low mental prosperity, while non-orphans had high mental prosperity.17 School support for orphans may help to buffer against the onset or worsening of depression symptoms over time.18 A study identified 7.5% hyperactivity disorder, 37.5% peer problems, and 12.5% severe peer problems. Regarding pro-social behavior, 22.5% were at risk, while 5% had abnormal pro-social behavior.19 It can be concluded that there is a need for cultivating positive emotions to optimize health and well-being of orphans.
In Pakistan, there is minimal evidence which explores relationships between anxiety, depression, stress, and decision-making among the orphanages' adolescents. Adolescents living in foster homes of Pakistan had less psychological problems, that those living in orphanage homes,20 who demonstrated less positive emotions,21 and had low self-confidence.22 High rate of behavioral problems was found among adolescents living in orphanages of Karachi, Pakistan.23
The aim of the research is to explore the relationship between anxiety, depression, stress, and decision making among orphans and non-orphans. The objectives of the study are
- To determine the relationship between anxiety, stress, depression, and decision-making between orphans and non-orphans.
- To investigate the predictor of anxiety in adolescent decision-making.
Methods
Correlational research design was used in this study to investigate the relationship between decision-making and anxiety, depression, and stress among orphans and non-orphans. The sample of the study was adolescents between 12 to18 years of age; therefore, purposive sampling technique was used. Data were collected from different orphanages and schools located in the city of Lahore, Pakistan. The inclusion criteria included the following: single, double orphans, and non-orphans between age range 12 and 18 years. Both boys and girls were included in this research. Participants living in orphan homes were included in this research. Orphans with any physical disability, and diagnosed with psychological disorders were excluded. Partially filled questionnaires were also excluded.
The instruments used were Depression, Anxiety, Stress Scales (DASS)24 and the Adolescent Decision Making Questionnaire (ADMQ).25,26
The ADMQ evaluates the concept of decision-making. The self-report instrument has 30-item using 4 point ratings (0= not at all to 3= almost always true). It has 5 sub-scales (decision self-esteem, vigilance, panic, cope out and complacency) and each sub-scale consists of 6 items. It is a valid and reliable questionnaire.25,26
The DASS27 is a set of three self-report scales designed to measure the emotional states of depression, anxiety, and stress. Each of the three scales (depression, stress, and anxiety) contains 7 items, divided into subscales with similar content. The depression scale assesses dysphoria, hopelessness, devaluation of life, self-deprecation, lack of interest/involvement, anhedonia, and inertia. The anxiety scale assesses autonomic arousal, skeletal muscle effects, situational anxiety, and subjective experience of anxious affect. The stress scale is sensitive to levels of chronic nonspecific arousal. It assesses difficulty relaxing, nervous arousal, and being easily upset/agitated, irritable/over-reactive and impatient. Scores for depression, anxiety, and stress are calculated by summing the scores for the relevant items. The recommended cut off scores for conventional severity for depression is: normal (0–9); mild (10–13) moderate (14–20); severe (21–27); extremely severe (28+). For anxiety the range is normal (0–7); mild (8–9); moderate (10–14); severe (15–19); extremely severe (20+). For stress the range is normal (0–14); mild (15–18); moderate (19–25); severe (26–33); extremely severe (34+). According to the instructions given in the manual scores on the DASS were multiplied by 2 to calculate the final score.27 The reliability and validity of DASS have been confirmed in previous studies.27,28
Procedure
Ethical review committee of the Ripah University approved the study. Permission to conduct the study was also taken from the official authority of 3 orphanages and 2 schools. A parent or legal guardian of all participants under the age of 18 years provided written informed consent. Confidentiality and anonymity were ensured. Instructions were given in both verbal and written form. Participants were given the right to withdraw from the study at any time and their responses would not be included in the study.
Data were analyzed according to the hypothesis, using SPSS 21. Descriptive statistics was used to determine the mean, standard deviations, and range, and further reliability analysis was performed to check the reliability of standardized scales. Pearson product moment was used to determine the correlation, T-Test matrix was carried out for gender differences, and Simple Regression analysis predicted the effect of social interaction anxiety.
Results
The study examined the relationship among anxiety, depression, stress and adolescent decision-making among orphans and non-orphans.
Table 1 shows the demographic information of the participants. For the present study, 150 orphans from different orphanages and 150 non-orphans were taken from different schools, respectively. Total number of sample was N=300.
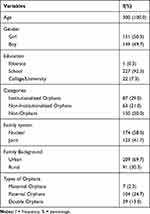 |
Table 1 Demographic Information of Participants |
Table 2 shows the psychometric properties of the standardized scales. The alpha reliability of the Depression Anxiety Stress Scale is Cronbach α.87. This scale has 42 items and the mean score is M=50.0 (SD=21.04). The Alpha reliability of its sub-scale Stress is Cronbach α 0.58, sub-scale Anxiety is Cronbach α.51, and sub-scale Depression is Cronbach α.63. The alpha reliability of Adolescent Decision-Making Scale is Cronbach α.53. This scale has 30 items and the mean score is M=44.3 (SD=8.13). The alpha reliability of its sub-scale Vigilance is Cronbach α 0.58, sub-scale Complacency is Cronbach α.47, sub-scale Panic is Cronbach α.50, sub-scale Self-Esteem is Cronbach α.42, and the sub-scale Cope out Defensive Avoidance is Cronbach α.37.
 |
Table 2 Psychometrics Properties of the Standardized Scales |
Table 3 shows the T-test matrix to find out gender difference. An independent t test reveals significant gender differences between orphans and non-orphans (M=9.45, SD=5.06) (M=8.03, SD=3.61) t (217) =2.48 p=0.01 @<0.05.
 |
Table 3 T-Test Matrix to Find Out Gender Difference on Study Variables |
Table 4 shows the correlation matrix for decision making, stress, anxiety, depression and DASS. The matrix indicates that decision making has significant correlation with stress (r= 0.30**, p<0.01), anxiety (r=0.27**, p<0.01), depression (r= 0.15*, p<0.05) and DASS (r= 0.29*, p<0.05). Stress has significant correlation with anxiety (r= 0.48**, p<0.01) and depression (r=0.47*, p<0.05). Decision Making has significant correlation with DASS (r= 0.67**, p<0.05). Anxiety has significant correlation with Depression (r= 0.61**, p<0.01). Anxiety has significant correlation with DASS (r= 0.76**, p<0.05). Depression has significant correlation with DASS (r= 0.81**, p<0.05)
 |
Table 4 Correlation Matrix for Decision- Making, Stress, Anxiety, Depression, and DASS |
Table 5 shows the predictor of adolescent decision-making. It indicates that anxiety is a significant predictor of adolescent decision-making (β =0.276, F=17.90, p<0.001). The value of R2 (0.076) explained 7% variance for anxiety in the adolescent decision-making.
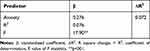 |
Table 5 Predictor of Adolescent Decision- Making |
Discussion
In the present study, anxiety is more prevalent in orphans as compared to non-orphans. Existing literature supports that orphans suffer from social anxiety and have poor social interaction.11,15 Higher levels of social and general anxiety level have been reported, with orphans striving for attention and approval of adults and afraid of receiving negative evaluation.29,30
In the present study, the anxiety was low in both groups, but gender difference was significant with females having high level of social anxiety. Existing evidence supports that orphan girls have higher levels of depression and low self-esteem as compared to orphan boys.34,35 Negative image of the world was more clearly found more in girls as compared to orphan boys.31–33
Findings from the present study indicate that adolescent’s decision-making is a significant predictor of depression, anxiety, and stress. In the present study, decision-making is negatively associated with awareness of self, perceived choice, vigilance, and self-esteem. Noam (2018)36 studied that self-awareness results in decision-making, but in this study, the orphans had to abide by social rules and thus decision-making was significant. Orphans and non-orphans decision-making skills are hindered by feelings of anxiety, depression, and low self-esteem while interacting with others in social settings.18,37-39
In the present study, there is significant correlation of stress and depression with decision-making. Similarly, orphan children as compared to non-orphans are more vulnerable to severe depression and are at risk of what appears to be clinical depression.9,40 These findings are corroborated in existing literature in which orphaned children living in the Gaza strip had considerable posttraumatic stress disorder, anxiety, and depression.31 Likewise, another study confirmed high prevalence of depression among orphans and identified low level of social support, higher length of stay, community discrimination, the presence of visitors, and younger age of entrance were statistically significant variables to develop depression.4
The study had a few limitations. One of the limitations of the study was that the mental status of the samples while completing the questionnaire may have influenced their response. The other limitation is that the study cross-sectional design did not allow studying the causal links and specific risk factors associated with symptoms of stress, depression, and anxiety.
Future studies should be based on longitudinal designs, as this would potentially be more beneficial in understanding the life experience of these orphaned children. By studying the variables of depression, anxiety, stress, coping, and the overall quality of life in different time-points would help to draw inferences about how orphanage placement impacts on psychological well-being of orphans.
Existing evidence has explored prevalence of anxiety, depression, and stress among orphans; however, this study further adds that anxiety, stress, and depression can influence their decision-making which can have major implications for their personal and professional life. The study has implications; first, there is a need to raise more awareness and attention from governmental and non-governmental institutions towards finding therapeutic programs for the orphans to enable them to live effectively and be functional and productive. Second, screening for depression and mental and psychological care should be integrated into routine health care provided to orphans. Third, there should be furnishing of life skills training such as stress management and coping skills, the formation and sustenance of healthy peer relationship, problem-solving and decision-making skills, as well as conflict management skills.
Conclusion
The present study concluded that anxiety, depression, and stress are positively associated with decision-making. In gender, girls had high anxiety as compared to boys. All girls and boys had high decision-making. Orphans and non-orphans had low social anxiety. The decision-making was high in both orphans and non-orphans. The implications of the study are that first there is a need to raise more awareness at governmental and non-governmental institutions towards finding therapeutic programs for orphans. Second, screening for depression and mental and psychological care should be integrated into routine health care provided to orphans. Third, there should be furnishing of life skills training such as stress management and coping skills, problem-solving and decision-making skills.
Acknowledgments
The authors thank all the respondents for participating in the study.
Disclosure
The author reports no conflicts of interest in this work.
References
1. Morantz M, Cole D, Vreeman R, Ayaya S, Ayuku D, Braitstein P. Child abuse and neglect among orphaned children and youth living in extended families in Sub-Saharan Africa: what have we learned from qualitative inquiry? Vulnerable Child Youth Stud. 2013;8(4):338–352.
2. Brunello N, den Boer JA. Social phobia: diagnosis and epidemiology, neurobiology and pharmacology, comorbidity and treatment. J Affect Disord. 2000;60(1):61–74. doi:10.1016/S0165-0327(99)00140-8
3. Kaur R, Vinnakota A, Panigrahi S, et al. A descriptive study on behavioral and emotional problems in orphans and other vulnerable children staying in institutional homes. Indian J Psychol Med. 2018;40:161–168.
4. Shiferaw G, Bacha L, Tsegaye D. Prevalence of depression and its associated factors among orphan children in orphanages in Ilu Abba Bor Zone, South West Ethiopia. Psychiatry J. 2018;1–7. doi:10.1155/2018/6865085
5. Hofmann SG, Anu Asnaani MA, Hinton DE. Cultural aspects in social anxiety and social anxiety disorder. Depress Anxiety. 2010;27(12):117–127. doi:10.1002/da.20759
6. Musisi S, Kinyanda E, Nakasujja N, et al. Personality differences between orphans and non-orphans. Afr Health Sci. 2007;7(4):202–213.
7. Lawson RB, Shen Z, Lawson R. Organizational Psychology: Foundations and Applications. New York: Oxford University Press.; 1998.
8. World Health Organization. Depression: let’s talk. Secondary Depression: let’s talk; 2019. Available from: https://www.who.int/mental_health/management/depression/en/.
9. Demoze MB, Angaw DA, Mulat H. Prevalence and associated factors of depression among Orphan Adolescents in Addis Ababa, Ethiopia. Psychiatry J. 2018;2018:1–7. doi:10.1155/2018/5025143
10. Dorsey S, Lucid L, Murray L, et al. A qualitative study of mental health problems among orphaned children and adolescents in Tanzania. J Nerv Ment Dis. 2015;203(11):864–870. doi:10.1097/NMD.0000000000000388
11. Akshita S, Suvidha. Well being of orphan: a review on their mental health status. Sci Technol. 2016;2(5):2395–6011.
12. Mohammadzadeh M, Awang H, Ismail S, et al. Stress and coping mechanisms among adolescents living in orphanages: an experience from Klang Valley, Malaysia. Asia Pac Psychiatry. 2018;10(1).
13. Gaviţa OA, David D, Bujoreanu S, et al. The efficacy of a short cognitive-behavioral parent program in the treatment of externalizing behavior disorders in Romanian foster care Children: building parental emotion-regulation through Unconditional self-and child-acceptance strategies. Child Youth Serv Rev. 2012;34(7):1290–1297. doi:10.1016/j.childyouth.2012.03.001
14. Zhou G. Understanding the Psychological Well-Being of Orphans and Vulnerable Children (OVC): The Intersection of Research and Policy. Duke University-Durham, Sanford Institute of Public Policy Studies; 2012.
15. Sushma B, Padmaja G, Agarwal S. Well-being, psychosocial problems and social interaction anxiety in children. Int J Indian Psychol. 2016;3(4):30–43.
16. Zhao J, Li X, Barnett D, et al. Parental loss, trusting relationship with current caregivers, and psychosocial adjustment among children affected by AIDS in China. Psychol Health Med. 2011;16(4):437–449. doi:10.1080/13548506.2011.554569
17. Tsegaye A. A Comparative Study of Psychological Wellbeing Between Orphan and Non-Orphan Children in Addis Ababa: The Case of Three Selected Schools in Yeka Sub-City. Addis Ababa University; 2013.
18. Green EP, Cho H, Gallis J, et al. The impact of school support on depression among adolescent orphans: a cluster-randomized trial in Kenya. J Child Psychol Psychiatry. 2019;60(1):54–62. doi:10.1111/jcpp.2019.60.issue-1
19. Sujatha R, Jacob SM. Study on emotional and behavioural problems among adolescent children in selected orphanages at mangalore. Zenith Int J Multi Res. 2014;4(7):253–259.
20. Ahmed A, Qamar J, Siddiq A, et al. A 2-years follow up of orphans’ competence, social emotional problems and post-traumatic stress disorder symptoms in traditional foster care and orphanages in Iraqi Kurdistan. Care Health Dev. 2005;31(2):203–215. doi:10.1111/j.1365-2214.2004.00477.x
21. Mostafaei A, Aminpoor H, Mohammadkhani M. The comparison of happiness in Orphanage and non-orphanage children. Ann Biol Res. 2012;3(8):4065–4069.
22. Farooqi YN, Intezar M. Differences in self-esteem of orphan children and children living with their parents. J Res Soc Pak. 2009;46(2):115–130.
23. Lassi ZS, Mahmud S, Syed EU, et al. Behavioral problems among children living in orphanage facilities of Karachi, Pakistan: comparison of children in an SOS Village with those in conventional orphanages. Soc Psychiatry Psychiatr Epidemiol. 2011;46(8):787–796. doi:10.1007/s00127-010-0248-5
24. Mann L. Decision Making Questionaire Manual. The Flinders University of South Australia; 1982.
25. Burnett PC, Mann L, Beswick G. Validation of the flinders decision making questionnaire on course decision making by students. Aust Psychol. 1989;24(2):285–292. doi:10.1080/00050068908259567
26. Lane SH. Psychometric analysis of the Adolescent Decision-Making Questionnaire. South Online J Nurs Res. 2010;10(4):1–12.
27. Lovibond PF, Lovibond SH. The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the beck depressions and anxiety inventories. Behav Res Ther. 1995;33:335–343. doi:10.1016/0005-7967(94)00075-U
28. Crawford JR, Henry JD. The Depression Anxiety Stress Scales (DASS): normative data and latent structure in a large non-clinical sample. Br J Clin Psychol. 2003;42(Pt 2):111–131. doi:10.1348/014466503321903544
29. Avakyan TV, Volikova SV. Social anxiety in children. Psychol Russ. 2014;1:74–82.
30. Tamara VA, Svetlana VV. Social anxiety in adolescents. Psychol Russ. 2014;7(1).
31. Thabet AA, Panos V. Effect of Trauma on mental health of parents and children in the middle area of the Gaza strip. JOJ Nurs Health Care. 2017;3(5):555–621.
32. Nyamukapa CA, Gregson S, Wambe M, et al. Causes and consequences of psychological distress among orphans in eastern Zimbabwe. AIDS Care. 2010;22(8):988–996. doi:10.1080/09540121003615061
33. Majeed R, Khan MA, Khan MNS. Gender differences in personality of orphans and non-orphans of Lahore. J Global Res Educ Soc Sci. 2015;2(1).
34. Ibrahim A, El-Bilsha MA, El-Gilany AH, et al. Prevalence and predictors of depression among orphans in Dakahlia orphanages, Egypt. Int J Collab Res Internal Med Public Health. 2012;4(12):2036–2043.
35. Safdar S. Comparative analysis of childhood depression and self-esteem among orphan girls and boys. J Psychol Clin Psychiatry. 2018;9(1):00498. doi:10.15406/jpcpy.2018.09.00498
36. Dishon N, Oldmeadow JA, Kaufman J. Trait self-awareness predicts perceptions of choice meaningfulness in a decision-making task. BMC Res Notes. 2018;11(1):75. doi:10.1186/s13104-018-3191-2
37. Demoze MB, Angaw DA, Prevalence MH. Associated factors of depression among Orphan Adolescents in Addis Ababa, Ethiopia. Psychiatry J. 2018;2018:5025143.
38. Thabet AA, Elhelou MW, Vostanis P. Prevalence of PTSD, depression, and anxiety among orphaned children in the Gaza Strip. EC Paediatr. 2017;5(6):159–169.
39. Robinson OJ, Vytal K, Cornwell BR, et al. The impact of anxiety upon cognition: perspectives from human threat of shock studies. Front Hum Neurosci. 2013;7(203). doi:10.3389/fnhum.2013.00203.
40. Yendork JS, Somhlaba NZ. Stress, coping and quality of life: an exploratory study of the psychological well-being of Ghanaian orphans placed in orphanages. Child Youth Serv Rev. 2014;46:28–37. doi:10.1016/j.childyouth.2014.07.025
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
