Back to Journals » Pediatric Health, Medicine and Therapeutics » Volume 7
Adopted youth and sleep difficulties
Authors Radcliff Z, Baylor A, Rybarczyk B
Received 17 August 2016
Accepted for publication 10 October 2016
Published 7 December 2016 Volume 2016:7 Pages 165—175
DOI https://doi.org/10.2147/PHMT.S119958
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Roosy Aulakh
Zach Radcliff, Allison Baylor, Bruce Rybarczyk
Department of Psychology, Virginia Commonwealth University, Richmond, VA, USA
Abstract: Sleep is a critical component of healthy development for youth, with cascading effects on youth’s biological growth, psychological well-being, and overall functioning. Increased sleep difficulties are one of many disruptions that adopted youth may face throughout the adoption process. Sleep difficulties have been frequently cited as a major concern by adoptive parents and hypothesized in the literature as a problem that may affect multiple areas of development and functioning in adopted youth. However, there is limited research exploring this relationship. Using a biopsychosocial framework, this paper reviews the extant literature to explore the development, maintenance, and impact of sleep difficulties in adopted youth. Finally, implications for future research and clinical interventions are outlined.
Keywords: adoption, sleep, youth
Introduction
During childhood and adolescence, quality sleep is critical for the development of good physical and mental health, particularly for vulnerable populations.1,2 Sleep is regulated through two biological processes, the circadian rhythm and homeostatic system, both of which are influenced by environmental factors.3 Psychosocial stressors may disturb sleep and the biological regulation processes which, in turn, may disrupt daily functioning, impair physical and mental health, and negatively influence development.1,4,5 This cycle of disruption may result in long-term changes in the biological processes that regulate sleep as well as chronic sleep difficulties and physical and mental health consequences.6,7 Further, research indicates that sleep difficulties often persist into adulthood, and are accompanied by cascading negative outcomes.8 Improving sleep in youth has been targeted as a critical area for intervention due to the potential for a wide range of positive outcomes.9,10
In 2012, nearly 400,000 children were in the foster system in the US, of which greater than 50,000 were adopted while another 100,000 waited to be adopted.11 Including international adoptions in 2008, more than 130,000 children were adopted into homes in the US.12 Further, the pre-adoption experiences and adoption pathways are heterogeneous, influencing their development in a number of ways.13 Overall, adopted youth are at increased risk for developing sleep difficulties and associated negative biopsychosocial outcomes.14,15 The process from pre-adoption through post-adoption is replete with biopsychosocial risk factors for sleep difficulties including stress, abuse, neglect, psychopathology, other environmental or parental dysfunction, inconsistency, or disruption.16,17 These factors can influence neurobiological functioning and increase adopted youth’s risk for sleep difficulties, which may further complicate the many challenges adopted youth already experience throughout the adoption process.16,18 Further, adoptive parents cite sleep difficulties as a primary concern and as an opportunity for targeted treatment.19,20 However, despite the wealth of research on environmental risk factors in adopted youth, there is limited research on how these factors influence sleep in adopted youth. Finally, post-adoption, there are often protective factors that begin to stabilize risk factors, improving sleep and psychosocial outcomes for adopted youth.21
The present paper reviews the literature on sleep in adopted youth, focusing particularly on adoption-related psychosocial stressors that may exacerbate and maintain sleep difficulties. First, common familial psychosocial stressors (ie, family, mental health, physical environment) experienced by adopted youth are outlined. Of note, psychosocial stressors that extend beyond the home environment (eg, peer, school, cultural), as well as genetic components, are outside the scope of this review. Further, the existing literature primarily focuses on American families adopting internationally, which excludes children who have been through domestic foster care in the US. Because of the limited literature on sleep in domestic adoptees, papers on international adoption are included with the goal of identifying pre- and post-adoption risk factors that may be generalizable to domestic studies. Subsequently, emphasis is placed on how these psychosocial stressors influence key biological systems that contribute to sleep difficulties, as well as how these sleep difficulties may contribute to detriments in mental health. Figure 1 provides an overview of the factors being considered and Figure 2 shows the common trajectories for children who are adopted superimposed on a timeline illustrating the key normal developmental changes in sleep which take place. Finally, future directions and implications are explored.
  | Figure 1 Common biopsychosocial risk factors for sleep difficulties in adopted youth. Abbreviation: PTSD, post-traumatic stress disorder. |
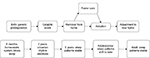  | Figure 2 The overlap of sleep development on typical adoption processes. |
Limited literature on sleep in adoption
Currently, there is limited research available that specifically examines sleep in adopted youth. Literature searches were conducted using PubMed and PsycINFO which included combinations of the following key terms: sleep, sleep difficulties, sleep disturbances, and insomnia; adoption, adopted, foster, and foster care; and child, children, youth, adolescents, and teens. Studies were included for review if they examined any aspect of routine or abnormal sleep in youth who had been adopted. Youth were defined as children between birth and 17 years old. The resulting seven studies are described in Table 1.
  | Table 1 Studies found that examine sleep in adopted youth Abbreviation: CBCL, Child Behavior Checklist. |
All seven studies show that sleep difficulties are common in adopted youth.15,20,22–26 Maltreatment and institutionalization prior to adoption predicted poorer sleep post-adoption.22,23,26 In the only study of post-adoption risk factors, marital discord at baseline was found to predict sleep problems at follow-up.24 These findings highlight that both pre- and post-adoption factors play important roles in youth sleep. Further, to manage post-adoption sleep difficulties, parents reported high levels of co-sleeping with distressed infants and an increased need to provide physical and verbal soothing.15,20 In the only study to examine school-aged children, maltreatment prior to adoption related to sleep difficulties, and independently, sleep difficulties were related to disruptive behavior.22 Finally, a study on institutionalized adopted Chinese girls demonstrated that adverse environments may have a biological impact on sleep issues, as children experienced higher asymmetry tympanic membrane temperatures (an indicator of physical well-being, cerebral temperature, and hemispheric lateralization) coupled with sleep difficulties prior to adoption.23 However, these results were not maintained at 9-month follow-up, possibly indicating that biological aspects of sleep difficulties reduce as sleep difficulties decrease post-adoption. Taken collectively, these findings suggest that it is not just pre-adoptive experiences that influence psychosocial outcomes post-adoption.
The current body of literature has several notable limitations. First, most studies examine internationally adopted Asian female infants,15,20,23,25,26 and only two studies have used a short-term longitudinal design.23,24 This is important because domestic adoptions and older children make up a significant number of adoptions,11,12 which limits our ability to understand the influence of pre-adoption events and adoption on sleep during later childhood and adolescence. Further, only two studies measured sleep with validated sleep questionnaires,22,24 while the remaining used select questions off of behavior measures or developed their own.15,20,23,25,26 The use of these instruments often results in less descriptive data on the nature of these sleep difficulties and reduces generalizability or replication. Most of these studies are based on qualitative research.15,20,23,25,26 As a result, it has been difficult to formulate or test an inclusive biopsychosocial model that can explain the findings in these studies. Given the paucity of literature specifically on foster/adopted children and sleep, the following sections review related sleep literature (eg, trauma, chaotic environments) in order to frame the discussion of the adoption literature.
Psychosocial factors
Psychosocial risk factors during adoption process
The majority of risk factors experienced by adopted youth occur prior to adoption, during their time with their biological parents, transitioning care, or foster/temporary care. These factors place them at risk for a variety of mental and physical health outcomes, including sleep difficulties.27 The reason for removal from their biological home may be a traumatic experience for each child. The most common reasons for removal include child abuse, child neglect, parental substance use, parental incarceration, parental death, or child behavioral problems.28,29 Further, children who are abused or neglected are more likely to live in a community with increased violence levels, which can compound trauma exposure. Even when children are removed from harmful home environments for their safety and well-being, losing their parents can be in and of itself a traumatic experience.28
As a result of these stressors, greater than 30% of children entering the foster system have serious mental health issues (eg, depression, anxiety, or disruptive behavior disorders) or developmental problems (eg, delayed/stunted growth or speech and language difficulties).28 Notably, the median age at entry to foster care is 6.4 years old, with the mean age of children in foster care being 8.9 years old.11 Children who are placed in the foster system stay in the system for an average of 33 months and typically experience one or more changes in caregivers.11,28 This is a period in development where sleep patterns normally become stabilized, though this is likely to be contingent on establishment of a consistent sleep routine and stable sleep environment.
In the past, the predominant wisdom was that it was best to remove children from harmful living situations; however, recent research is showing that removal is a far more complex issue.30 Compared to children who remain in their biological home (even in the case of similar risk factors with maltreatment), children who have experienced foster care were more likely to have serious behavior and internalizing problems.30 This may be the result of children placed in foster care undergoing a traumatic (though temporary) loss of their parents coupled with adapting to a new home environment and forging attachments with new caregivers. It may also be attributable to the success of family-based interventions that were administered to families flagged for maltreating their children but whose children stayed in the home.30 This issue is further complicated for older children, and children who have behavioral problems are more likely to experience multiple foster homes and remain in the foster system longer.29 As a result, during this important developmental window, these children are forging new attachments and rebuilding their social support on top of navigating typical developmental milestones. These disruptions may increase child stress, directly influencing sleep and its neurobiological regulation system.14,31 Despite the potential for negative outcomes associated with foster care, many children who are adopted experience improvements across physical and mental health domains,13,17,21,32,33 and adoption is viewed as significantly more favorable than remaining in foster care.
Psychosocial influences of sleep
Youth experience a wide variety of psychosocial stressors that may influence their ability to obtain quality sleep. This section focuses on psychosocial risk factors influencing sleep which are related to family, mental health, and physical environment. Risk factors associated with these areas have been linked to negative sleep outcomes and may be present in the pre- and post-adoption lives of adopted youth.1,34 These factors may result in the biological disruptions of sleep regulation, which in turn may maintain sleep difficulties (Figures 1 and 2).4,35
Family factors
Family-related stressors can greatly influence a child’s ability to achieve quality sleep. Violence in the home, parent substance abuse, parent mental health, parenting style and supervision, family structure, and family beliefs about sleep all contribute to the development of sleep patterns in youth.36,37
Children may be exposed to a variety of behaviors by their parents, including domestic violence, substance abuse, and a parent’s own mental health struggles.37 A recent study in the Netherlands found that children exposed to intimate partner violence were more likely to have difficulty sleeping, slept less, had more nightmares, and more frequent nocturnal enuresis, some of which may persist into adulthood.8,38 Further, electroencephalograms of sleeping children whose parents have a history of substance abuse showed decreased activity in thalamus regions that protect sleep, making them more vulnerable to sleep difficulties.39 Finally, higher levels of parental depression and other psychopathology are related to children having difficulty initiating sleep, particularly when mothers are emotionally unavailable.40,41 Thus due to parental psychopathology, children may not have structured bedtime, may not have their emotional needs met, or may experience detrimental parenting behaviors, in turn influencing their ability to get enough quality sleep.
Additionally, children who are abused, neglected, or experience family conflict are more likely to experience sleep difficulties.42 There is evidence that youth who are abused/neglected experience sleep difficulties during childhood, adolescence, and into adulthood, demonstrating both the immediate and lasting effects of abuse/neglect on youth sleep.37,42 Youth who were placed in state custody due to parental neglect or physical abuse from parents have higher rates of sleep difficulties and decreased sleep efficiency than youth in state custody who had not experienced abuse or neglect.43,44 Further, family conflict during childhood and early adolescence predict sleep difficulties during late adolescence.37
In addition to conflict, parent–child attachment and parenting style may both play an important role in children’s sleep. Toddlers who are more securely attached to their primary caregiver(s) are more likely to have higher sleep quality and quantity,45 while infants and toddlers who have a disorganized or insecure attachment sleep less, have poorer sleep quality, and have more awakenings.46 Vaughn et al47 found that these trends remain stable as children grow older. In addition to attachment, parenting styles play a role in bedtime structure, which is linked to a child’s ability to fall and stay asleep.48 Higher levels of parent warmth relate to increased quantity of sleep in youth under age 11, while adolescents obtain more sleep when their parents practice higher parental monitoring and control.49 These studies show the importance of parent–child interaction and bonding as a means to establish an effective bedtime routine and ensure that the child feels safe and relaxed in bed.
Mental health
Mental health concerns have been discussed extensively in relation to sleep difficulties50–52 and also adopted youth.53–55 In this section, mental health concerns that are most prominent in adopted youth are focused on particularly as they pertain to initiation and maintenance of sleep difficulties. Adopted youth access mental health services at higher rates and are more likely to have more severe presentations.54,55 They are more likely to have experienced abuse or neglect and engage in disruptive behaviors.54 They present with internalizing disorder rates comparable to their non-adoptive peers.53,54 While this relation is well established, it remains difficult to determine the causal direction, and likely, it is bidirectional in nature.50,56 The relationship between mental health and sleep issues is so intertwined that sleep difficulties can be viewed as a risk factor for mental health concerns and a symptom of others. According to the Diagnostic and Statistical Manual of Mental Disorders (fifth edition),57 a number of anxiety disorders, mood disorders, and trauma-related disorders have some form of sleep dysregulation as a symptom.
Both internalizing and externalizing disorders have been implicated in the disruption of sleep.51,56 Armstrong et al51 followed a cohort of children throughout childhood and adolescence, and found that at age 4, hostile/aggressive and hyperactive behaviors were associated with sleep difficulties. At age nine, children with sleep difficulties were more likely to have depressive symptoms, attention deficit hyperactivity disorder, or externalizing behaviors. For adolescents at age 18, anxiety and externalizing behaviors were associated with difficulty sleeping. Further, in a review of sleep difficulties in mood disorders, Lofthouse et al56 found that from early childhood to late adolescence, mood disorders were associated with an increase in sleep difficulties. Similar research has found that anxiety during childhood and adolescence is associated with an increase of sleep difficulties including quality and quantity of sleep.58 As noted, children who have experienced or witnessed traumatic events are more likely to have difficulty sleeping.42
There are a number of proposed mechanisms behind the relationship between youth psychopathology and sleep difficulties. Youth who experience affective disturbances (ie, difficulty regulating emotions, negative self-perceptions, and dysphoric mood) are more likely to have both sleep difficulties and psychopathology such as depression and anxiety.42 These disturbances may increase arousal in youth impairing their ability to get the required quantity and quality of sleep. As a part of increased arousal, engaging in cognitive rumination about past events, worries, or depressive thoughts may further decrease the ability to fall asleep.59 Further, youth with anxiety and heightened fear expression may not view their home or bedroom as safe place and thus have a harder time relaxing and feeling comfortable while they sleep.52 These fears may be greater in youth who have experienced abuse or trauma in their bedroom or at home, particularly at night. Lower cognitive flexibility may also play a role in these fears as these youth cannot engage in effective coping strategies.42 As a result of this complex relation, it is easy to see how mental health concerns may be both a catalytic and a maintaining factor for sleep difficulties for some children.
Physical environment
Children’s physical environment influences their ability to obtain sufficient and good-quality sleep. Adopted youth typically see an improvement in their physical environment34 but may experience any number of stressors that could impair sleep.60–63 For example, preadolescent youth who are exposed to unsafe or hostile home environments are more likely to experience difficulty sleeping.60 More broadly, living in a community with elevated crime rates is associated with increased sleep difficulties in adolescents.61 Further, if impoverished adolescents witness violent crimes, they are also more likely to have insomnia, nightmares, and daytime sleepiness in addition to greater autonomic nervous system (ANS) activation and reactivity.62,63
In addition to needing a safe overall environment, children benefit from a comfortable bedroom environment that is conducive to sleep. Sleep duration was even shorter among minority and older youth64 and has been further related to disruptive night time noises.50 Sharing a bed or room is also related to shorter sleep duration across youth ages and is more common in Eastern cultures, single-parent households, and low socioeconomic status homes.50,65,66 If co-sleeping continues for more than a year, disrupted sleep behaviors may become habitual in children.67
The biology of sleep and adoption
Biological regulation of sleep
Sleep regulation occurs through two biological processes: the circadian rhythm and the homeostatic system.68 These two systems work together to regulate the sleep/wake cycle in the body. The circadian rhythm is the 24-hour “wake drive” which determines alertness and works like a clock. Its rhythm refreshes daily based on cues such as light exposure and temperature.69 The homeostatic system, “sleep drive”, is a sleep-dependent process driven by the gradually increasing need for sleep (sleep pressure), which builds throughout the day and releases at night, like a spring.69 Both processes rely on neurochemicals for regulation. The parabolic increase and decrease of melatonin drive the sleep/wake cycle of the circadian rhythm,69,70 while sleep pressure is regulated by adenosine increasing linearly throughout the day.71
A number of neural structures have been implicated in regulation of sleep.72 The circadian rhythm is driven primarily by the hypothalamus but is also regulated in part by the pituitary gland and melatonin-producing pineal gland.70 The homeostatic system is regulated in part by the basal forebrain, a group of acetylcholine-producing structures in the cortex.73 In this way, the homeostatic system is related to the cortico-limbic system, which includes regions of the basal forebrain and regulates cognitive arousal through acetylcholine.73 Regions of the cortico-limbic system implicated in sleep include the amygdala, hippocampus, thalamus, and hypothalamus. Further, the cortico-limbic regions work with the sympathetic nervous system to help to regulate the body during sleep.74 Finally, the ANS, regulated primarily by the hypothalamus, helps to maintain homeostasis in the body including sleep and the threat response.75 Thus, the hypothalamus and basal forebrain participate in multiple modes of regulation; a redundancy that may make sleep disruption difficult.
At birth, these biological mechanisms do not fully regulate sleep, but as children develop, regulation of sleep begins to stabilize. Prior to 6 months, children’s circadian rhythm is not yet developed, so sleep is primarily driven by their homeostatic rhythm.70 By age two, the circadian rhythm and homeostatic system are working together to facilitate nocturnal sleep, while the homeostatic rhythm will often drive napping.76 Circadian and homeostatic rhythms begin to stabilize around age two, and by age five become set patterns that are difficult to change.76,77 From age five until adolescence, these rhythms continue to work together to regulate sleep, and gradually, the homeostatic need for naps declines. During adolescence, sleep/wake times shift later, due to the biological changes associated with puberty as well as psychosocial factors.78 During their twenties, young adults fall into a stable sleep cycle, requiring 6–8 hours of sleep that relies on both circadian and homeostatic rhythms to regulate. However, at any stage during development, these sleep patterns may be derailed by a number of psychosocial factors.
Biological disruption of sleep
Neurobiological disruption has been independently associated with both sleep difficulties and the psychosocial stressors seen in adopted youth.4,35 These biological consequences are varied and range in severity and length of their influence. Both temporary and long-term sleep difficulties may have concurrent influences on next-day functioning, while the long-term presence of sleep difficulties may also have lasting neurobiological implications.79 Psychosocial stressors, like those experienced pre-adoption, may have similar lasting effects on neurobiology.80,81 This section focuses on the lasting neurobiological implications which tend to relate to longer-term sleep difficulties and long-term exposure to psychosocial stressors.79,82
The psychosocial stressors that impact adopted youth discussed are associated with dysregulation in the regions and pathways that regulate sleep. As the cortico-limbic system is associated with affect and mood, mood disorders (ie, depression and bipolar) have been associated with dysfunction in this system – particularly the hypothalamus, amygdala, and hippocampus.80,81,83 During adolescence, decreases in cortico-limbic gray matter are associated with childhood maltreatment.84 Further, hypothalamus–pituitary dysregulation has been associated with increases in anxiety, post-traumatic stress disorder, and physical or emotional abuse directed at the child.35,80,85
As sleep is disrupted by these stressors, the endogenous systems and brain regions associated with sleep change.86 Connectivity decreases between regions in the cortico-limbic pathway and its associated sleep regulation locations.87,88 Greater reactivity of the ANS, which is primarily regulated by the hypothalamus, is associated with decreased sleep quantity through increased activation of the neural pathways linked to homeostasis.89 Further, hypothalamic and pituitary hyperactivity and dysfunction are associated with decreased sleep quantity in children and adolescents.4,86 As these changes occur, the ability to regulate sleep decreases, and sleep difficulties become stabilized neural pathways.90 Further, these neurobiological changes may increase physiological arousal at bedtime.91 As a result, the brain is increasing wakefulness instead of inducing relaxation and rest.
Neurobiological effects of adoption process
As noted, the brain regions responsible for sleep regulation are also responsible for a number of other functions. As such, they can be influenced by a variety of external stressors. For adopted youth, the adoption process represents an external stressor that can influence the neurobiology of these regions.92,93 Both the limbic system and hypothalamus–pituitary–adrenal (HPA) axis may undergo changes during the adoption process.92,94,95 These changes may result in the dysregulation of regions also responsible for sleep regulation.
The HPA axis is the primary region indicated in neurobiological change during the adoption process. The HPA axis is responsible for the biological stress response in addition to other homeostatic and autonomic processes in the body.96 As a result, increased stress from time spent in a stressful home environment, foster care, or transitioning care can lead to dysregulation of the HPA stress response and of other HPA-controlled homeostatic systems such as sleep.14,97 Children who experienced emotional abuse prior to adoption were more likely to experience decreased HPA axis activity, while children experiencing physical neglect had increased HPA axis activity with both resulting in pervasive HPA dysregulation.97 Further, children in the foster care system exhibit continued elevated HPA activity, impairing normative HPA functioning.92 Finally, adopted children with internalizing problems experience decreased HPA axis activity, while adopted children with externalizing problems experience increased HPA axis activity.98 Adopted children may experience HPA axis dysregulation at all these stages, and the cumulative effects may result in stabilization of the dysfunction of the HPA axis.98
To date, the disruption of the ANS processes and limbic pathways has only been studied in international youth with a history of institutionalization.95,99 Children who have been in an institution prior to adoption have increased sympathetic nervous system activity. The sympathetic nervous system is the activating branch of the ANS, which is responsible for the stress/threat response and overriding the parasympathetic relaxation response.99 Neuroimaging indicates a significant decrease in limbic white matter volume and connectivity in adopted children who experience significant neglect or deprivation.95 Both studies implicated increased stress experienced by neglected and deprived children as the likely cause for these results. Thus, it may be hypothesized that adopted youth in the US who experienced significant neglect prior to adoption may show similar ANS and limbic disruptions.
Outcomes
Psychosocial outcomes of sleep difficulties
With the disruption of biological systems, a youth’s ability to navigate psychosocial stressors is hindered, and many mental health and psychosocial outcomes have been linked to sleep difficulties.
Sleep difficulties have particularly salient effects on neurocognitive and social functioning. Children who sleep poorly may have difficulty paying attention in school, process information slower, or struggle to regulate their emotions.6,100 School-aged children with poor sleep were more likely to be aggressive and have social–relational difficulties, behaviors which can persist into adolescence.101,102 Further, sleep difficulties were associated with poor school performance and behavioral problems.10,102 Youth with sleep difficulties experience greater difficulty paying attention, concentrating on work, and forming and retaining memories.10,103 Youth of all ages who reported shortened sleep duration also reported poorer quality of life and perceived less social support than their peers.10
Effects of adoption
The effects of adoption are generally viewed as positive in nature, and youth experience many gains as their lives begin to stabilize in their new family.21 Benefits of adoption may be most significant for children adopted prior to the age of two.99 However, across ages, youth quickly “catch up” to their community-matched peers physically, while psychological difficulties may take more time.33 These psychological delays are supported by research indicating that there is limited change to the HPA axis dysregulation post-adoption and a slow increase in limbic white matter.14,95,98 Lloyd and Barth32 found that adopted youth continued to have externalizing behavior problems and exhibitive maladaptive behavior patterns. There is no literature exploring whether there are improvements in sleep post-adoption; instead, research has focused on the sleep difficulties that children have at the time of adoption.15,19,25 However, based on that many risk factors disappear post-adoption and that some individuals improve without intervention, it can be hypothesized that some children will see improvement in sleep post-adoption if their neurobiology has not stabilized in a dysfunctional pattern.14,24,99
Discussion
Interest in enhanced sleep as a universal intervention for youth with complex issues is growing. Sleep difficulties can cause impairment in multiple domains, and resolution may improve a child’s functioning. Children of all ages and backgrounds are susceptible to the development of sleep difficulties. However, certain psychosocial stressors increase the likelihood that a child will experience sleep difficulties. Parenting styles, parent psychopathology, abuse, neglect, dangerous neighborhoods, transitioning living situations, and child psychopathology may all increase the likelihood that children will develop sleep difficulties through similar mechanisms seen in populations of youth with psychopathology or trauma exposure.29,30,42 These experiences are more prevalent in adopted youth than their non-adopted counterparts.18,28 Thus, in keeping with adoptive parent report, it is likely that sleep difficulties are a significant complication facing newly formed families post-adoption.
These psychosocial stressors may create concurrent and lasting sleep difficulties for adopted children. While the neurobiology behind sleep regulation is designed to prevent disruption, many of these stressors influence multiple regions of the brain (ie, HPA axis, limbic system).99,104 Thus, the regions responsible for sleep regulation may be disrupted, potentially perpetuating sleep difficulties. The disruptions from psychosocial stressors may become stabilized in the brain through new neural pathways.90 Thus, sleep difficulties stemming from the psychosocial experience prior to and throughout the adoption process may result in long-term sleep difficulties. Further, adopted children are at an increased risk for the development of psychopathology, which may also maintain sleep difficulties and create a vicious cycle of reinforcement.
Future directions and implications
Adoptive parents frequently cite sleep difficulties as areas of concern, and report wanting assistance in helping their children cope with sleep difficulties.20,31 As noted, there is limited research exploring this critical area in adoption. However, there is a growing body of literature on sleep in related populations such as youth with psychopathology, youth experiencing maltreatment, and attachment and parenting styles.42,48,91 This paper describes and integrates aspects of this literature that applies to adopted youth and allows for a theoretical framework to be applied.
As in many areas with a paucity of research, more research needs to be conducted before the model proposed in this paper can be empirically evaluated. First, further research effort is needed to describe the problem more thoroughly. The types of sleep difficulties, how disruptive they are, and the methods families use to address them will provide critical information to researchers and clinicians. Further, it would be useful to explore whether there are factors that moderate or mediate the relation between the adoption process and sleep including adoption process experiences (ie, foster care, family adoption), trauma history, and types of trauma experienced. School performance, social functioning, psychopathology, and family adjustment will all be important outcomes to measure.
After this information has been collected, it will be possible to test sleep interventions targeted at the subpopulations that most need intervention and tailor interventions to their needs. Sleep restriction as a part of cognitive behavioral therapy for insomnia has been shown to be effective in many populations of children as it works to reset the circadian rhythm and homeostatic system.105 It would be beneficial to test sleep restriction across the unique populations seen in the adoption community (ie, international, intra-family, and inter-family). Additionally, it may be important to examine how to implement sleep restriction across cultures in adoption, which may be particularly important for international adoptions. Other areas for intervention may include sleep hygiene and bedtime routines. As noted, children may experience ineffective parenting around bedtime which increases sleep disturbances.
Finally, there are immediate clinical implications of this model. Adoptive parents regularly request assistance improving their children’s sleep habits and correcting sleep issues.20 Sleep may be an ideal area for clinicians working with adopted children to target. Often treated as a symptom of psychosocial stressors, addressing it more directly may allow for improved functioning and a greater ability to manage other psychosocial stressors. While sleep restriction is a difficult process for both children and parents, it may be an effective way to interrupt the cycle of biopsychosocial disruption and maintenance proposed in this model.
Whether addressed first or as a part of a multifaceted treatment, it is likely that many adopted children would benefit from a more direct approach to treating their sleep difficulties. By using this model as a framework for research and treatment, researchers and clinicians may be able to more effectively conceptualize and treat adopted children’s sleep difficulties and ease the transition into their new family. With a growing number of adoptions in the US every year, it is important to address this concern to improve sleep for millions of children.
Disclosure
The authors declare that they have no relevant financial or nonfinancial relationships to disclose in this work. The authors report no other conflicts of interest in this work.
References
El-Sheikh M, Sadeh A. I. Sleep and development: introduction to the monograph. Monogr Soc Res Child Dev. 2015;80(1):1–14. | ||
Poe GR, Walsh CM, Bjorness TE. Cognitive neuroscience of sleep. Prog Brain Res. 2010;185:1–19. | ||
Carskadon MA, Tarokh L. Developmental changes in sleep biology and potential effects on adolescent behavior and caffeine use. Nutr Rev. 2014;72(Suppl 1):60–64. | ||
Fernandez-Mendoza J, Vgontzas AN, Calhoun SL, et al. Insomnia symptoms, objective sleep duration and hypothalamic-pituitary-adrenal activity in children. Eur J Clin Invest. 2014;44(5):493–500. | ||
Gerber L. Sleep deprivation in children: a growing public health concern. Nursing. 2014;44(4):50–54. | ||
Gregory AM, Caspi A, Moffitt TE, Poulton R. Sleep problems in childhood predict neuropsychological functioning in adolescence. Pediatrics. 2009;123(4):1171–1176. | ||
Goel N, Rao H, Durmer JS, Dinges DF. Neurocognitive consequences of sleep deprivation. Semin Neurol. 2009;29(4):320–339. | ||
Chapman DP, Liu Y, Presley-Cantrell LR, et al. Adverse childhood experiences and frequent insufficient sleep in 5 U.S. states, 2009: a retrospective cohort study. BMC Public Health. 2013;13:3. | ||
Lukowski AF, Bell MA. On sleep and development: recent advances and future directions. Monogr Soc Res Child Dev. 2015;80(1):182–195. | ||
Shochat T, Cohen-Zion M, Tzischinsky O. Functional consequences of inadequate sleep in adolescents: a systematic review. Sleep Med Rev. 2014;18(1):75–87. | ||
United States Children’s Bureau. The adoption and foster care analysis and reporting system report for 2012. 2013. Available from: https://www.acf.hhs.gov/sites/default/files/cb/afcarsreport20.pdf. Accessed May 15, 2016. | ||
Child Welfare Information Gateway. How many children were adopted in 2007 and 2008? 2011. Available from: https://www.childwelfare.gov/pubs/adopted0708/. Accessed May 15, 2016. | ||
Grotevant HD, McDermott JM. Adoption: biological and social processes linked to adaptation. Annu Rev Psychol. 2014;65:235–265. | ||
Koss KJ, Hostinar CE, Donzella B, Gunnar MR. Social deprivation and the HPA axis in early development. Psychoneuroendocrinology. 2014;50:1–13. | ||
Tan TX, Marfo K, Dedrick RF. Preschool-age adopted Chinese children’s sleep problems and family sleep arrangements. Infant Child Dev. 2009;18(5):422–440. | ||
Hussey DL, Falletta L, Eng A. Risk factors for mental health diagnoses among children adopted from the public child welfare system. Child Youth Serv Rev. 2012;34(10):2072–2080. | ||
Simmel C, Barth RP, Brooks D. Adopted foster youths’ psychosocial functioning: a longitudinal perspective. Child Fam Soc Work. 2007;12(4):336–348. | ||
Child Welfare Information Gateway. Finding and using postadoption services. 2012. Available from: http://www.childwelfare.gov/pubs/f_postadoption.cfm. Accessed May 16, 2016. | ||
Tan TX. Preschool-age adopted Chinese girls’ behaviors that were most concerning to their mothers. Adopt Q. 2010;13(1):34–49. | ||
Tirella LG, Tickle-Degnen L, Miller LC, Bedell G. Parent strategies for addressing the needs of their newly adopted child. Phys Occup Ther Pediatr. 2012;32(1):97–110. | ||
Simmel C. Risk and protective factors contributing to the longitudinal psychosocial well-being of adopted foster children. J Emot Behav Disord. 2007;15(4):237–249. | ||
Cuddihy C, Dorris L, Minnis H, Kocovska E. Sleep disturbance in adopted children with a history of maltreatment. Adopt Foster. 2013;37(4):404–411. | ||
Damsteegt RC, van IJzendoorn MH, Out D, Bakermans-Kranenburg MJ. Tympanic membrane temperature in adopted children associated with sleep problems and pre-adoption living arrangements: an exploratory study. BMC Psychol. 2014;2(1):51. | ||
Mannering AM, Harold GT, Leve LD, et al. Longitudinal associations between marital instability and child sleep problems across infancy and toddlerhood in adoptive families. Child Dev. 2011;82(4):1252–1266. | ||
Rettig MA, McCarthy-Rettig K. A survey of the health, sleep, and development of children adopted from China. Health Soc Work. 2006;31(3):201–207. | ||
Tirella LG, Miller LC. Self-regulation in newly arrived international adoptees. Phys Occup Ther Pediatr. 2011;31(3):301–314. | ||
Baldwin S. Growth, development, and behavior: confronting the issues of international adoption. J Ark Med Soc. 2011;107(9):183–185. | ||
American Academy of Child and Adolescent Psychiatry. Facts for families: foster care. 2012. Available from: http://www.aacap.org/AACAP/Families_and_Youth/Facts_for_Families/FFF-Guide/Foster-Care-064.aspx. Accessed May 16, 2016. | ||
Connell CM, Vanderploeg JJ, Flaspohler P, Katz KH, Saunders L, Tebes JK. Changes in placement among children in foster care: a longitudinal study of child and case influences. Soc Serv Rev. 2006;80(3):398–418. | ||
Lawrence CR, Carlson EA, Egeland B. The impact of foster care on development. Dev Psychopathol. 2006;18(1):57–76. | ||
Tininenko JR, Fisher PA, Bruce J, Pears KC. Sleep disruption in young foster children. Child Psychiatry Hum Dev. 2010;41(4):409–424. | ||
Lloyd EC, Barth RP. Developmental outcomes after five years for foster children returned home, remaining in care, or adopted. Child Youth Serv Rev. 2011;33(8):1383–1391. | ||
Palacios J, Román M, Camacho C. Growth and development in internationally adopted children: extent and timing of recovery after early adversity. Child Care Health Dev. 2011;37(2):282–288. | ||
Christoffersen MN. A study of adopted children, their environment, and development: a systematic review. Adopt Q. 2012;15(3):220–237. | ||
Dieleman GC, Huizink AC, Tulen JH, et al. Alterations in HPA-axis and autonomic nervous system functioning in childhood anxiety disorders point to a chronic stress hypothesis. Psychoneuroendocrinology. 2015;51:135–150. | ||
Giannotti F, Cortesi F. Family and cultural influences on sleep development. Child Adolesc Psychiatr Clin N Am. 2009;18(4):849–861. | ||
Gregory AM, Caspi A, Moffitt TE, Poulton R. Family conflict in childhood: a predictor of later insomnia. Sleep. 2006;29(8):1063–1067. | ||
Lamers-Winkelman F, De Schipper JC, Oosterman M. Children’s physical health complaints after exposure to intimate partner violence. Br J Health Psychol. 2012;17(4):771–784. | ||
Tarokh L, Carskadon MA. Sleep electroencephalogram in children with a parental history of alcohol abuse/dependence. J Sleep Res. 2010;19(1 Pt 2):165–174. | ||
Benhamou I. Sleep disorders of early childhood: a review. Isr J Psychiatry Relat Sci. 2000;37(3):190–196. | ||
Lee S, Rhie S, Chae KY. Depression and marital intimacy level in parents of infants with sleep onset association disorder: a preliminary study on the effect of sleep education. Korean J Pediatr. 2013;56(5):211–217. | ||
Cecil CA, Viding E, McCrory EJ, Gregory AM. Distinct mechanisms underlie associations between forms of childhood maltreatment and disruptive nocturnal behaviors. Dev Neuropsychol. 2015;40(3):181–199. | ||
Epstein RA, Bobo WV, Cull MJ, Gatlin D. Sleep and school problems among children and adolescents in state custody. J Nerv Ment Dis. 2011;199(4):251–256. | ||
Kelly RJ, Marks BT, El-Sheikh M. Longitudinal relations between parent-child conflict and children’s adjustment: the role of children’s sleep. J Abnorm Child Psychol. 2014;42(7):1175–1185. | ||
Bélanger MÈ, Bernier A, Simard V, Bordeleau S, Carrier J. Viii. Attachment and sleep among toddlers: disentangling attachment security and dependency. Monogr Soc Res Child Dev. 2015;80(1):125–140. | ||
Charuvastra A, Cloitre M. Safe enough to sleep: sleep disruptions associated with trauma, posttraumatic stress, and anxiety in children and adolescents. Child Adolesc Psychiatr Clin N Am. 2009;18(4):877–891. | ||
Vaughn BE, El-Sheikh M, Shin N, Elmore-Staton L, Krzysik L, Monteiro L. Attachment representations, sleep quality and adaptive functioning in preschool age children. Attach Hum Dev. 2011;13(6):525–540. | ||
Gregory AM, Sadeh A. Sleep, emotional and behavioral difficulties in children and adolescents. Sleep Med Rev. 2012;16(2):129–136. | ||
Adam EK, Snell EK, Pendry P. Sleep timing and quantity in ecological and family context: a nationally representative time-diary study. J Family Psychol. 2007;21(1):4–19. | ||
Chen T, Wu Z, Shen Z, Zhang J, Shen X, Li S. Sleep duration in Chinese adolescents: biological, environmental, and behavioral predictors. Sleep Med. 2014;15(11):1345–1353. | ||
Armstrong JM, Ruttle PL, Klein MH, Essex MJ, Benca RM. Associations of child insomnia, sleep movement, and their persistence with mental health symptoms in childhood and adolescence. Sleep. 2014;37(5):901–909. | ||
Noll JG, Trickett PK, Susman EJ, Putnam FW. Sleep disturbances and childhood sexual abuse. J Pediatr Psychol. 2006;31(5):469–480. | ||
Keyes MA, Sharma A, Elkins IJ, Iacono WG, McGue M. The mental health of US adolescents adopted in infancy. Arch Pediatr Adolesc Med. 2008;162(5):419–425. | ||
Kotsopoulos S, Côté A, Joseph L, et al. Psychiatric disorders in adopted children: a controlled study. Am J Orthopsychiatry. 1988;58(4):608–612. | ||
Juffer F, van Ijzendoorn MH. Behavior problems and mental health referrals of international adoptees: a meta-analysis. JAMA. 2005;293(20):2501–2515. | ||
Lofthouse N, Gilchrist R, Splaingard M. Mood-related sleep problems in children and adolescents. Child Adolesc Psychiatr Clin N Am. 2009;18(4):893–916. | ||
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Arlington, VA: American Psychiatric Association; 2013. | ||
Sarchiapone M, Mandelli L, Carli V, et al. Hours of sleep in adolescents and its association with anxiety, emotional concerns, and suicidal ideation. Sleep Med. 2014;15(2):248–254. | ||
Zoccola PM, Dickerson SS, Lam S. Rumination predicts longer sleep onset latency after an acute psychosocial stressor. Psychosom Med. 2009;71(7):771–775. | ||
Lepore SJ, Kliewer W. Violence exposure, sleep disturbance, and poor academic performance in middle school. J Abnorm Child Psychol. 2013;41(8):1179–1189. | ||
Kliewer W, Lepore SJ. Exposure to violence, social cognitive processing, and sleep problems in urban adolescents. J Youth Adolesc. 2015;44(2):507–517. | ||
Spilsbury JC, Babineau DC, Frame J, Juhas K, Rork K. Association between children’s exposure to a violent event and objectively and subjectively measured sleep characteristics: a pilot longitudinal study. J Sleep Res. 2014;23(5):585–594. | ||
Umlauf MG, Bolland AC, Bolland KA, Tomek S, Bolland JM. The effects of age, gender, hopelessness, and exposure to violence on sleep disorder symptoms and daytime sleepiness among adolescents in impoverished neighborhoods. J Youth Adolesc. 2015;44(2):518–542. | ||
Falbe J, Davison KK, Franckle RL, et al. Sleep duration, restfulness, and screens in the sleep environment. Pediatrics. 2015;135(2):e367–e375. | ||
Madansky D, Edelbrock C. Cosleeping in a community sample of 2- and 3-year-old children. Pediatrics. 1990;86(2):197–203. | ||
Weimer SM, Dise TL, Evers PB, Ortiz MA, Welldaregay W, Steinmann WC. Prevalence, predictors, and attitudes toward cosleeping in an urban pediatric center. Clin Pediatr (Phila). 2002;41(6):433–438. | ||
Latz S, Wolf AW, Lozoff B. Cosleeping in context: sleep practices and problems in young children in Japan and the United States. Arch Pediatr Adolesc Med. 1999;153(4):339–346. | ||
Borbély AA. A two process model of sleep regulation. Hum Neurobiol. 1982;1(3):195–204. | ||
Borbély AA. Processes underlying sleep regulation. Horm Res Paediatr. 1998;49(3–4):114–117. | ||
Mirmiran M, Maas YG, Ariagno RL. Development of fetal and neonatal sleep and circadian rhythms. Sleep Med Rev. 2003;7(4):321–334. | ||
Basheer R, Strecker RE, Thakkar MM, McCarley RW. Adenosine and sleep–wake regulation. Prog Neurobiol. 2004;73(6):379–396. | ||
Zeitzer JM. Control of sleep and wakefulness in health and disease. Prog Mol Biol Transl Sci. 2013;119:137–154. | ||
Buysse DJ, Germain A, Hall M, Monk TH, Nofzinger EA. A neurobiological model of insomnia. Drug Discov Today Dis Models. 2011;8(4):129–137. | ||
Perry JC, Bergamaschi CT, Campos RR, Silva AM, Tufik S. Interconnectivity of sympathetic and sleep networks is mediated through reduction of gamma aminobutyric acidergic inhibition in the paraventricular nucleus. J Sleep Res. 2014;23(2):168–175. | ||
Maes J, Verbraecken J, Willemen M, et al. Sleep misperception, EEG characteristics and autonomic nervous system activity in primary insomnia: a retrospective study on polysomnographic data. Int J Psychophysiol. 2014;91(3):163–171. | ||
Barclay NL, Gregory AM. Sleep in childhood and adolescence: age-specific sleep characteristics, common sleep disturbances and associated difficulties. Curr Top Behav Neurosci. 2014;16:337–365. | ||
Waterhouse J, Fukuda Y, Morita T. Daily rhythms of the sleep-wake cycle. J Physiol Anthropol. 2012;31(1):5. | ||
Giannotti F, Cortesi F, Sebastiani T, Ottaviano S. Circadian preference, sleep and daytime behaviour in adolescence. J Sleep Res. 2002;11(3):191–199. | ||
Roth T, Roehrs T. Insomnia: epidemiology, characteristics, and consequences. Clin Cornerstone. 2003;5(3):5–15. | ||
Shea A, Walsh C, Macmillan H, Steiner M. Child maltreatment and HPA axis dysregulation: relationship to major depressive disorder and post traumatic stress disorder in females. Psychoneuroendocrinology. 2005;30(2):162–178. | ||
Teicher MH, Andersen SL, Polcari A, Anderson CM, Navalta CP, Kim DM. The neurobiological consequences of early stress and childhood maltreatment. Neurosci Biobehav Rev. 2003;27(1–2):33–44. | ||
Lian Y, Xiao J, Liu Y, et al. Associations between insomnia, sleep duration and poor work ability. J Psychosom Res. 2015;78(1):45–51. | ||
Suzuki H, Belden AC, Spitznagel E, Dietrich R, Luby JL. Blunted stress cortisol reactivity and failure to acclimate to familiar stress in depressed and sub-syndromal children. Psychiatry Res. 2013;210(2):575–583. | ||
Edmiston EE, Wang F, Mazure CM, et al. Corticostriatal-limbic gray matter morphology in adolescents with self-reported exposure to childhood maltreatment. Arch Pediatr Adolesc Med. 2011;165(12):1069–1077. | ||
Kuhlman KR, Geiss EG, Vargas I, Lopez-Duran NL. Differential associations between childhood trauma subtypes and adolescent HPA-axis functioning. Psychoneuroendocrinology. 2015;54:103–114. | ||
Zhang J, Lam SP, Li SX, et al. A community-based study on the association between insomnia and hypothalamic-pituitary-adrenal axis: sex and pubertal influences. J Clin Endocrinol Metab. 2014;99(6):2277–2287. | ||
Huang Z, Liang P, Jia X, et al. Abnormal amygdala connectivity in patients with primary insomnia: evidence from resting state fMRI. Eur J Radiol. 2012;81(6):1288–1295. | ||
O’Byrne JN, Berman Rosa M, Gouin JP, Dang-Vu TT. Neuroimaging findings in primary insomnia. Pathol Biol (Paris). 2014;62(5):262–269. | ||
El-Sheikh M, Erath SA, Bagley EJ. Parasympathetic nervous system activity and children’s sleep. J Sleep Res. 2013;22(3):282–288. | ||
Salas RE, Galea JM, Gamaldo AA, et al. Increased use-dependent plasticity in chronic insomnia. Sleep. 2014;37(3):535–544. | ||
Steine IM, Harvey AG, Krystal JH, et al. Sleep disturbances in sexual abuse victims: a systematic review. Sleep Med Rev. 2012;16(1):15–25. | ||
Laurent HK, Gilliam KS, Bruce J, Fisher PA. HPA stability for children in foster care: mental health implications and moderation by early intervention. Dev Psychobiol. 2014;56(6):1406–1415. | ||
Sheridan M, Drury S, McLaughlin K, Almas A. Early institutionalization: neurobiological consequences and genetic modifiers. Neuropsychol Rev. 2010;20(4):414–429. | ||
Fisher PA, Mannering AM, Van Scoyoc A, Graham AM. A translational neuroscience perspective on the importance of reducing placement instability among foster children. Child Welfare. 2013;92(5):9–36. | ||
Kumar A, Behen ME, Singsoonsud P, et al. Microstructural abnormalities in language and limbic pathways in orphanage-reared children: a diffusion tensor imaging study. J Child Neurol. 2014;29(3):318–325. | ||
Peng H, Long Y, Li J, et al. Hypothalamic-pituitary-adrenal axis functioning and dysfunctional attitude in depressed patients with and without childhood neglect. BMC Psychiatry. 2014;14:45. | ||
Bruce J, Fisher PA, Pears KC, Levine S. Morning cortisol levels in preschool-aged foster children: differential effects of maltreatment type. Dev Psychobiol. 2009;51(1):14–23. | ||
Laurent HK, Neiderhiser JM, Natsuaki MN, et al. Stress system development from age 4.5 to 6: family environment predictors and adjustment implications of HPA activity stability versus change. Dev Psychobiol. 2014;56(3):340–354. | ||
McLaughlin KA, Sheridan MA, Tibu F, Fox NA, Zeanah CH, Nelson CA 3rd. Causal effects of the early caregiving environment on development of stress response systems in children. Proc Natl Acad Sci U S A. 2015;112(18):5637–5642. | ||
Moore M, Kirchner HL, Drotar D, et al. Relationships among sleepiness, sleep time, and psychological functioning in adolescents. J Pediatr Psychol. 2009;34(10):1175–1183. | ||
Lin WH, Yi CC. Unhealthy sleep practices, conduct problems, and daytime functioning during adolescence. J Youth Adolesc. 2015;44(2):431–446. | ||
Simola P, Liukkonen K, Pitkaranta A, Pirinen T, Aronen ET. Psychosocial and somatic outcomes of sleep problems in children: a 4-year follow-up study. Child Care Health Dev. 2014;40(1):60–67. | ||
Chee MW, Chuah LY. Functional neuroimaging insights into how sleep and sleep deprivation affect memory and cognition. Curr Opin Neurol. 2008;21(4):417–423. | ||
Fisher PA, Van Ryzin MJ, Gunnar MR. Mitigating HPA axis dysregulation associated with placement changes in foster care. Psychoneuroendocrinology. 2011;36(4):531–539. | ||
Paine S, Gradisar M. A randomised controlled trial of cognitive-behaviour therapy for behavioural insomnia of childhood in school-aged children. Behav Res Ther. 2011;49(6–7):379–388. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
