Back to Journals » Journal of Pain Research » Volume 13
Acupotomy versus Manual Acupuncture for the Treatment of Back and/or Leg Pain in Patients with Lumbar Disc Herniation: A Multicenter, Randomized, Controlled, Assessor-Blinded Clinical Trial
Authors Jeong JK , Kim E , Yoon KS, Jeon JH, Kim YI , Lee H, Kwon O , Jung SY, Lee JH , Yang C , Kang JH , Han CH
Received 15 October 2019
Accepted for publication 7 March 2020
Published 1 April 2020 Volume 2020:13 Pages 677—687
DOI https://doi.org/10.2147/JPR.S234761
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor E Alfonso Romero-Sandoval
Jeong Kyo Jeong,1,* Eunseok Kim,1,* Kwang Sik Yoon,2 Ju Hyun Jeon,1 Young Il Kim,1 Hyun Lee,2 Ojin Kwon,3 So-Young Jung,3 Jun-Hwan Lee,3,4 Changsop Yang,3 Jae Hui Kang,2 Chang-Hyun Han3,4
1Department of Acupuncture and Moxibustion Medicine, Daejeon University Dunsan Korean Medicine Hospital, Daejeon, Republic of Korea; 2Department of Acupuncture and Moxibustion Medicine, Daejeon University Cheonan Korean Medicine Hospital, Cheonan, Republic of Korea; 3Clinical Medicine Division, Korea Institute of Oriental Medicine, Daejeon 34054, Republic of Korea; 4Korean Medicine Life Science, University of Science and Technology (UST), Campus of Korea Institute of Oriental Medicine, Daejeon 34054, Republic of Korea
*These authors contributed equally to this work
Correspondence: Chang-Hyun Han
Clinical Medicine Division, Korea Institute of Oriental Medicine, 1672, Yuseongdaero, Daejeon 34054, Republic of Korea
Tel +82 42 868 9498
Fax +82 42 869 2775
Email [email protected]
Jae Hui Kang
Department of Acupuncture and Moxibustion Medicine, Daejeon University Cheonan Korean Medicine Hospital, 4, Notaesan-ro, Cheonan 31099, Republic of Korea
Tel +82 41 521 7579
Fax +82 41 521 7007
Email [email protected]
Background: Acupotomy, which involves the addition of a scalpel function to the conventional acupuncture treatment, has recently been applied as a conservative treatment method for lumbar disc herniation (LDH). This study investigated the effectiveness and safety of acupotomy, compared to manual acupuncture, for the treatment of patients with LDH.
Methods: A total of 146 patients diagnosed with LDH were randomly assigned to either the acupotomy group or the manual acupuncture group at a 1:1 ratio. Participants in both groups received four sessions of each intervention over 2 weeks. Outcome assessments based on the visual analog scale (VAS), Roland Morris Disability Questionnaire (RMDQ), Modified-Modified Schober Test (MMST), EuroQol Five Dimensions (EQ-5D), clinically important difference (CID), and patient global impression of change (PGIC) were conducted at baseline and at 2, 4, and 6 weeks post-randomization.
Results: The acupotomy group showed significant improvement in VAS and MMST at 2, 4, and 6 weeks than did the manual acupuncture group. RMDQ was significantly different between the two groups at 2 and 6 weeks. In EQ-5D, there was no significant difference between the two groups. The proportion of patients with ≥ 15 mm decrease on the VAS (minimal CID) was significantly higher in the acupotomy group at weeks 2 and 4. Better improvement in the PGIC at week 4 was also observed in the acupotomy group. Post-intervention muscle pain was reported, but there was no serious adverse event related to interventions.
Conclusion: In this study, four sessions of acupotomy treatment were found to be effective in improving the pain intensity and range of motion of the lumbar region in patients with LDH. Despite post-treatment muscle pain, acupotomy treatment can be considered a preferred treatment method over manual acupuncture.
Trial Registration: This trial has been registered 24 April 2018 in Clinical Research Information Service of South Korea (CRIS-KCT0002824).
Keywords: acupotomy, manual acupuncture, lumbar disc herniation, pain intensity, range of motion
Background
Lumbar disc herniation (LDH) is caused by the protrusion or extrusion of the lumbar disc from its normal position for various reasons. As the herniated disc irritates the nerve roots, it causes back and/or leg pain, radiating pain, and paresthesia or weakness in the lower extremities.1–3 Typically, surgery is considered when symptoms of cauda equina syndrome or progressive neurological deficit are observed or when there is no improvement despite conservative treatment. However, surgical treatment places a burden of concerns on these patients with LDH, which may include fears of post-operative failure syndrome.
Among the various conservative treatments that have been applied to treat LDH,4–9 acupuncture has recently gained traction.10,11 Acupotomy is a special type of acupuncture, which involves the addition of a scalpel function to the existing acupuncture needle. Since the tip of the acupotomy needle is a flat blade that can also function for synechotomy, the effects of both acupuncture and surgical treatment are expected from the procedure.12,13 Consequently, acupotomy treatment has been applied for various musculoskeletal diseases14–19 and some metabolic diseases such as lymphatic edema.20
Although the effectiveness of acupotomy on LDH was suggested by several case reports and a pilot study,13,21–23 a more extensive confirmatory study was needed to confirm the effectiveness and safety of acupotomy on LDH. Therefore, we performed a multicenter, randomized, controlled, assessor-blinded, clinical trial to evaluate the effectiveness and safety of acupotomy treatment compared with manual acupuncture treatment.
Methods
Study Design and Participants
A total of 146 patients diagnosed with LDH were recruited in this study. They included: 96 patients visited Daejeon University’s Dunsan Korean Medicine Hospital (DUDKMH) from April 09, 2018 to December 08, 2018, and 50 patients visited Daejeon University’s Cheonan Korean Medicine Hospital (DUCKMH) from March 23, 2018 to October 8, 2018. This study was approved by both Institutional Review Boards of DUDKMH (DJDSKH-18-BM-02) and DUCKMH (DJUMC-2018-BM-01), and registered by the Clinical Research Information Service (CRIS-KCT0002824) in Republic of Korea. This trial was conducted in accordance with the Declaration of Helsinki.
Based on the results of the pilot study4 and its clinical significance, we assumed that the mean difference (δ) between the changes in the visual analog scale (VAS) before and after treatment in each group was 15, and the standard deviation (σ) was 24.71 for confirming the effectiveness of acupotomy. After considering the significance level of 5% and the power of 90%, 58 subjects were included in each group in the 1:1 assignment of group allocation ratios. Considering the dropout rate of 20%, a total of 146 patients (73 per group) were eventually recruited. The complete process of sample size calculation is described in detail in the protocol paper.24 Before data collection, in addition, all participants received a full explanation of this study’s protocol and were provided a written explanation and informed consent form.
The inclusion criteria were: 1) patients aged between 19 and 70 years who were diagnosed with LDH and showed symptoms such as low back pain, radiating pain, and paresthesia or weakness in the lower extremities and 2) scored more than 30 mm on the VAS at the time of screening. The LDH diagnosis was based on both physical examination and medical imaging findings such as CT (Computed Tomography) or MRI (Magnetic Resonance Imaging). We excluded the participants who: 1) major spinal pathology such as spondylolisthesis, spondylolysis, compression fracture, neoplasm, and congenital abnormality; 2) had a hypersensitive reaction to previous acupuncture treatment; 3) had previous spinal surgery due to neurological deficits or cauda equine syndrome; 4) were suffering from pain in another region greater than that in the low back and/or lower extremities; 5) were using drugs to relieve the pain; 6) had participated in another clinical trial with interventions within the past 3 months; 7) had hemorrhagic or cardiovascular diseases or other factors, such as the use of anticoagulant or antiplatelet drugs, that could affect hemostasis; and 8) were considered unsuitable by the researchers.
Randomization and Blinding
Participants were randomly assigned to either the acupotomy group (n = 73; 48 in DUDKMH and 25 in DUCKMH) or the manual acupuncture group (n = 73; 48 in DUDKMH and 25 in DUCKMH). The random number table was generated by a statistician independent from this study. Based on the results of previous studies that suggested that women preferred Korean Medicine treatment to men and that they were better improved at pain and quality of life than men, stratified block randomization with gender as a strata factor was performed in order to reduce bias.25 All subjects were given a detailed explanation of the study procedure.
Additionally, all researchers were divided into groups and placed in charge of the intervention procedure, outcome assessment, data management, and statistical analysis. As the intervention procedure was different between the two groups, it was impossible to blind the participants and intervention practitioners; however, outcome assessors and data managers were blinded to the allocation status of all the participants. Each intervention practitioner performed only one of the two interventions (either acupotomy or manual acupuncture) and was not involved in the outcome measurements.
Interventions
In the acupotomy group, a total of four acupotomy treatments were administered for 2 weeks using flat-head-screw-driver-shaped, stainless steel, disposable and sterilized acupotomy needles (0.75 mm in diameter and 80 mm in length; DONGBANG Medical Co., Ltd., Chungcheongnam-do, Republic of Korea) (Figure 1). The insertion points were set at the corresponding disc level based on the imaging findings; this was 20–30 mm away from the spinous process and to a depth of 50–60 mm. They could be inserted on one or both sides, according to the symptoms and appearances of the herniated lumbar disc on the image findings. After local sterilization with 10% betadine solution and skin anesthetization with Emla Cream 5% (AstraZeneca Korea, lidocaine and prilocaine, each 25mg/g), the needle was inserted, manipulated, and removed immediately.
 |
Figure 1 Acupotomy needle. |
In the manual acupuncture group, four manual acupuncture treatments were administered for 2 weeks using 0.25 mm × 40 mm, single-use, sterile, stainless steel needles (DONGBANG Medical Co., Ltd., Chungcheongnam-do, Republic of Korea). The manual acupuncture treatment was performed at GV3 and bilateral BL23, BL24, BL25, BL26, GB3, BL40, and BL60.24 The depth of insertion was 20 mm for BL40 and BL60 and 30 mm for the other acupuncture points. The needles were removed after 15 mins.
Acetaminophen (SAMNAM Pharm. Co. Ltd., acetaminophen Tab. 500 mg) was administered to both groups as rescue medication. The details of the intervention and co-interventions have also been described in the protocol paper.24
Outcome Measures
The primary outcome was the mean changes in the VAS scores for low back and/or leg pain between the baseline and a follow-up visit at the 4th week (4 weeks post-randomization). The secondary outcome measures included the Korean version of the Roland Morris Disability Questionnaire (RMDQ),26,27 Modified-Modified Schöber Test (MMST),28 EuroQol Five Dimensions questionnaire (EQ-5D),29 minimal clinically important difference (CID),30–33 and patient global impression of change (PGIC).34 All the above outcomes were measured at the baseline and at 2, 4, and 6 weeks post-randomization.
The adverse events based on the vital signs, medical examinations, and other blood test results were assessed at every visit. The causal relationships between adverse events and intervention, and the severity of the intervention-related adverse events, such as pain, bleeding, hematoma, or bruise, were evaluated. All the outcome values were registered on the electronic case report form (eCRF), which was designed by the Korea Institute of Oriental Medicine (KIOM) and only accessible to the blinded researchers.
Statistical Analysis
Statistical analyses were performed using SAS® version 9.4 (SAS Institute. Inc., Cary, NC) by a statistician who was blinded to the participant’s allocation. The data corresponding to the full analysis set (FAS), which includes participants who were treated with the assigned intervention and were subjected to outcome measurement once or more, were analyzed. The independent t-test or Wilcoxon signed-rank test for continuous variables and the chi-squared or Fisher’s exact test for categorical variables were used to examine the potential differences in the baseline demographics and medical history variables between the two groups. The analysis of covariance (ANCOVA) was used to compare the mean changes in the VAS, RMDQ, MMST, and EQ-5D from the baseline to the 4th week. The paired t-test or Wilcoxon signed-rank test was used to compare the outcomes before and after treatment within each group. The repeated measures analysis of variance (RM ANOVA) was used to assess the differences between the two groups over time. A value of p < 0.05 was considered statistically significant.
Results
Between March 2018 and December 2018, a total of 158 participants were screened for eligibility. In total, 12 of them were considered ineligible to participate in the study and dropped out because they did not meet the eligibility criteria. Of the 146 eligible patients, 140 completed the study while the remaining 6 (4.11%), comprising 3 in each group, dropped out (Figure 2). No significant differences between the groups were found in the demographic characteristics, clinical features, or outcome variables at baseline (Table 1).
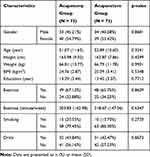 |
Table 1 Baseline Demographics and Clinical Characteristics |
 |
Figure 2 Study flowchart. Abbreviations: FAS, full analysis set; PP, per protocol. |
The observed mean VAS scores showed a 4-week reduction from the baseline value of 18.67 points for the acupotomy group compared with 8.13 points for the manual acupuncture group. The adjusted mean difference in the VAS scores between the two groups at week 4 was −11.13 (95% confidence interval [CI]: −17.49 to −4.77), and the acupotomy group was confirmed to show significantly improved VAS scores compared with the manual acupuncture group (p < 0.001) (Table 2). The mean difference between the two groups at week 6 was −8.45 (95% confidence interval [CI]: −14.94 to −1.95; p<0.05), which was slightly lower than the value at week 4. In the repeated measures ANOVA, the VAS scores that did not meet the assumptions of the sphericity test were then analyzed using a Greenhouse-Geisser epsilon analysis and showed a significant group × time interaction effect (p < 0.05) (Figure 3). In this study, rescue medication was given for back and/or leg pain is so severe that it is unbearable. There was no significant difference between the two groups in the dose and frequency of rescue medication (Table 3). In a post hoc analysis with adjustments for the baseline score and the rescue medication use, significant differences in the VAS scores between the groups were noted at every visit.
 |
Table 2 Observed Outcomes and Adjusted Group Differences |
 |
Table 3 Dosage and Frequency of Rescue Medication |
In RMDQ, the acupotomy group showed significant improvement compared with the manual acupuncture group at weeks 2 and 6. In MMST, the acupotomy group also showed significant improvement compared with the manual acupuncture group at weeks 2, 4, and 6. However, no significant differences between the two groups were found in the EQ-5D (Table 2). Significant group × time interaction effects were also found for the following outcome: RMDQ (p = 0.0031) and MMST (p = 0.0128) (Figure 3). At week 4, in the within-group analyses before and after the intervention, the acupotomy group showed significant improvement in VAS, RMDQ, MMST, and EQ-5D, while the manual acupuncture group showed significant improvement in VAS, RMDQ, and EQ-5D.
The proportions of patients with decreased VAS scores of more than 15 mm (minimal CID), were significantly higher in the acupotomy group than in the manual acupuncture group at weeks 2 and 4; additionally, the moderate CID/substantial improvements were higher in the acupotomy group than in the manual acupuncture group at weeks 2, 4, and 6 (Figure 4). In PGIC, a statistically significant higher number of patients in the acupotomy group than in the manual acupuncture group reported their global impressions of change as: “very much improved”, “much improved”, or “minimally improved” at week 4 (Figure 5).
 |
Figure 4 Clinical relevance. Note: a p < 0.05.Abbreviation: CID, clinically important difference. |
 |
Figure 5 Patient global impression of change. Note: All patients below the dashed line reported improvement. |
Among 429 visitations of the acupotomy group, 14 mild adverse events were reported, and there was no severe adverse event (SAE). Furthermore, among 426 visitations of the manual acupuncture group, 13 mild adverse events were reported, and 1 SAE which was not related to the intervention of this study, was reported. Post-intervention muscle pain was the most common discomfort. However, other adverse events not related to the intervention included: abnormal findings on the blood test, common cold, other musculoskeletal pain, itching, ophthalmitis, and hematoma. Additionally, there was one case of SAE; but, the subject sustained a contusion on the Rt. Lisfranc joint during regular daily activity. The patient was subsequently hospitalized for surgery and stopped participating in the study. Hence, no SAEs related to the intervention were observed (Table 4).
 |
Table 4 Summary of Adverse Events |
Discussion
The adjusted mean differences in VAS and MMST scores between the two groups were significantly different at weeks 2, 4, and 6. Acupotomy treatment particularly showed the greatest improvement in pain relief and lumbar range of motion (ROM) at week 4 compared with manual acupuncture treatment. Additionally, the proportion of subjects with pain reductions of ≥30% and ≥50% was significantly higher in the acupotomy group. At weeks 2 and 6, the degree of functional disability due to LDH significantly improved in the acupotomy group than in the manual acupuncture group. The quality of life (QOL) was also significantly improved in each group; however, there was no significant difference between the two groups. Although mild adverse events were reported in both groups, all of them were temporary; with regard to the interventions, no SAEs occurred.
Acupotomy is one of the ancient types of acupuncture that has been developed as modern acupotomy by professor Hanzhang Zhu in China.35 This new type of acupuncture combines the use of a flat blade with conventional acupuncture and can be applied to anatomical structural defects as well as existing acupoints. Since acupotomy treatment involves the process of adhesiolysis by the sharp blade, it could also promote blood circulation and healing responses at the site. Thus, treating the affected region of LDH with acupotomy is considered to reduce the physical pressure on the nerve roots and activate the microcirculation, consequently improving low back pain and/or leg pain.36
Inoue et al implemented a clinical trial to evaluate the effectiveness of electroacupuncture treatment on low back pain and lower limb symptoms.37 They carried out electroacupuncture stimulation of the nerve root under an X-ray fluoroscope; this resulted in immediate relief, which was sustained until follow-up at the 3 months time point in two of the three patients diagnosed with LDH. This electroacupuncture stimulation and the acupotomy treatment used in our study have a common feature, that is, they stimulate the tissues around the affected nerve root despite using a different stimulation method. However, it is difficult to compare the two treatment methods because the study carried out by Inoue et al involved very few cases.
In the pilot study21 that was previously conducted by our study group, the participants were followed-up to week 4 after a 2-week intervention. Significant differences in the improvement of functional disability and pain relief between the acupotomy group and the manual acupuncture group were observed. However, in this confirmatory study, follow-up was performed up to week 6, and pain reduction and ROM improvement were most noticeable at week 4. At week 6, the mean difference between the two groups decreased slightly compared to week 4, but there was still a significant difference. Therefore, it was confirmed that the better improvement in the acupotomy group was maintained until week 6. Additionally, the degree of functional disability showed a significant difference between the groups at week 2 and week 6; the significant group × time interaction effects were also noteworthy. In addition, rescue medication was provided for back and/or leg pain that is so severe that it is unbearable. The dose and frequency of rescue medication in both groups gradually decreased after the intervention period, and there was no significant difference in dose and frequency of rescue medication between the two groups. From the results of this study, we can conclude that despite some post-treatment discomforts, acupotomy treatment can be considered as a preferential treatment method over manual acupuncture.
Nevertheless, this study has several limitations. First, the follow-up period of 4 weeks post-intervention was not enough to confirm the long-term effects of acupotomy. Second, neither the participants nor practitioners were blinded, which could act as a potential bias, such as the expectation by the subject and the reliability of the assigned intervention. However, despite these methodological limitations, this study provides an objective and clinically beneficial outcome for comparing the effects of the two different acupuncture treatments. In the future, it is necessary to perform large-scale, long-term follow-up clinical trials comparing other conservative interventions with acupotomy; furthermore, studies evaluating the synergistic effects of other treatments with acupotomy treatment are also required.
Conclusions
The improvement in the pain intensity and ROM of the lumbar region observed in patients with LDH after four sessions of acupotomy treatment was higher than that observed after manual acupuncture. Based on the CID and PGIC, the differences in pain intensity between the two groups were clinically relevant. Acupotomy treatment was also confirmed to be as safe as conventional acupuncture. Therefore, acupotomy treatment can be considered as a valuable treatment option for the patients with LDH.
Abbreviations
ANCOVA, Analysis of Covariance; CID, Clinically Important Difference; CT, Computed Tomography; DUCKMH, Daejeon University’s Cheonan Korean Medicine Hospital; DUDKMH, Daejeon University’s Dunsan Korean Medicine Hospital; eCRF, electronic Case Report Form; EQ-5D, EuroQol Five Dimensions questionnaire; FAS, Full Analysis Set; KIOM, Korea Institute of Oriental Medicine; LDH, Lumbar disc herniation; MMST, Modified-Modified Schöber Test; MRI, Magnetic Resonance Imaging; PGIC, Patient Global Impression of Change; QOL, Quality of Life; RMANOVA, Repeated Measures Analysis of Variance; RMDQ, Roland Morris Disability Questionnaire; ROM, Range of Motion; SAE, Severe Adverse Event; VAS, Visual Analog Scale.
Data Sharing Statement
The datasets generated during the current study are available from the corresponding author on reasonable request.
Ethics and Consent Statement
This study was approved by both Institutional Review Boards of DUDKMH (DJDSKH-18-BM-02) and DUCKMH (DJUMC-2018-BM-01), and registered by the Clinical Research Information Service (CRIS-KCT0002824) in Republic of Korea. Before data collection, all participants received a full explanation of this study’s protocol and were provided a written explanation and informed consent form.
Author Contributions
All authors contributed to the study design, conception, data analysis, drafting and revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Funding
This study was supported by grants from the project KSN2013210 of Korea Institute of Oriental Medicine, Republic of Korea. The funding sources had no role in the experimental design, procedures, writing, and decision to submit the work for publication.
Disclosure
The authors have no conflicts of interest to declare in this work.
References
1. Yang H, Liu H, Li Z, et al. Low back pain associated with lumbar disc herniation: role of moderately degenerative disc and annulus fibrous tears. Int J Clin Exp Med. 2015;8(2):1634–1644.
2. Fardon DF, Williams AL, Dohring EJ, Murtagh FR, Gabriel Rothman SL, Sze GK. Lumbar disc nomenclature: version 2.0: recommendations of the combined task forces of the North American Spine Society, the American Society of Spine Radiology and the American Society of Neuroradiology. Spine J. 2014;14(11):2525–2545. doi:10.1016/j.spinee.2014.04.022
3. McCall IW. Lumbar herniated disks. Radiol Clin. 2000;38(6):1293–1309. doi:10.1016/S0033-8389(08)70007-1
4. Zhang B, Xu H, Wang J, Liu B, Sun G. A narrative review of non-operative treatment, especially traditional Chinese medicine therapy, for lumbar intervertebral disc herniation. Biosci Trends. 2017;11(4):406–417. doi:10.5582/bst.2017.01199
5. Ter Meulen BC, Maas ET, Vyas A, et al. Treatment of acute sciatica with transforaminal epidural corticosteroids and local anesthetic: design of a randomized controlled trial. BMC Musculoskelet Disord. 2017;18(1):215. doi:10.1186/s12891-017-1571-8
6. Knezevic NN, Mandalia S, Raasch J, Knezevic I, Candido KD. Treatment of chronic low back pain - new approaches on the horizon. J Pain Res. 2017;10:1111–1123. doi:10.2147/JPR.S132769
7. Karimi N, Akbarov P, Rahnama L. Effects of segmental traction therapy on lumbar disc herniation in patients with acute low back pain measured by magnetic resonance imaging: a single arm clinical trial. J Back Musculoskelet Rehabil. 2017;30(2):247–253. doi:10.3233/BMR-160741
8. Lee DG, Ahn S-H, Lee J. Comparative effectivenesses of pulsed radiofrequency and transforaminal steroid injection for radicular pain due to disc herniation: a prospective randomized trial. J Korean Med Sci. 2016;31(8):1324–1330. doi:10.3346/jkms.2016.31.8.1324
9. Kreiner DS, Hwang SW, Easa JE, et al. An evidence-based clinical guideline for the diagnosis and treatment of lumbar disc herniation with radiculopathy. Spine J. 2014;14(1):180–191. doi:10.1016/j.spinee.2013.08.003
10. Liang YD, Li Y, Zhao J, Wang XY, Zhu HZ, Chen XH. Study of acupuncture for low back pain in recent 20 years: a bibliometric analysis via CiteSpace. J Pain Res. 2017;10:951–964. doi:10.2147/JPR.S132808
11. Hutchinson AJ, Ball S, Andrews JC, Jones GG. The effectiveness of acupuncture in treating chronic non-specific low back pain: a systematic review of the literature. J Orthop Surg Res. 2012;7(1):36. doi:10.1186/1749-799X-7-36
12. Guo C, Liu N, Li X, et al. Effect of acupotomy on nitric oxide synthase and beta-endorphin in third lumbar vertebrae transverse process syndrome model rats. J Tradit Chin Med. 2014;34(2):194–198. doi:10.1016/s0254-6272(14)60078-9
13. Kim H-J, Jeon J-H, Kim Y-I. Clinical effect of acupotomy combined with Korean medicine: a case series of a herniated intervertebral disc. J Acupunct Meridian Stud. 2016;9(1):31–41. doi:10.1016/j.jams.2015.09.001
14. Ou G, Yin F, Do B, et al. Based on mechanical stimulation of muscle and ligament growth mechanics balance and adaptation: a clinical study on acupotomy preventing and treating degenerative joint disease. Osteoarthritis Cartilage. 2018;26:S311–S312. doi:10.1016/j.joca.2018.02.626
15. Kim JI, Kim HS, Park GN, Jeon JH, Kim JH, Kim YI. Miniscalpel needle therapy with integrative Korean medical treatment for carpal tunnel or tarsal tunnel syndrome: case series of three patients. The Acupuncture. 2017;34(3):139–152. doi:10.13045/acupunct.2017100
16. Dong B, Yao J, Yuan P, et al. Symptom scores and gait analyses on knee osteoarthritis by acupotomy. Osteoarthritis Cartilage. 2017;25:S378–S379. doi:10.1016/j.joca.2017.02.647
17. Jia L. The effect of acupotomy treatment of knee osteoarthritis, a systematic review and meta-analysis. Osteoarthritis Cartilage. 2017;25:
18. Li S, Shen T, Liang Y, Zhang Y, Bai B. Effects of miniscalpel-needle release on chronic neck pain: a retrospective analysis with 12-month follow-up. PLoS One. 2015;10(8):e0137033. doi:10.1371/journal.pone.0137033
19. Lim N-R, Jang E-H, Park M-Y, Kim S-C. Case study of oriental medicine treatment with acupotomy therapy of the tarsal tunnel syndrome. J Pharmacopuncture. 2009;12(1):109–117. doi:10.3831/KPI.2009.12.1.109
20. Jang E-H, Kim S-Y, Kim H-S, Kim S-C. Acupotomy and venesection in upper limb lymphedema and peripheral neuropathy following breast cancer surgery. J Pharmacopuncture. 2009;12(4):119–126. doi:10.3831/KPI.2009.12.4.119
21. Kim SY, Kim E, Kwon O, Han C-H, Kim Y-I. Effectiveness and safety of acupotomy for lumbar disc herniation: a randomized, assessor-blinded, controlled pilot study. Evid Based Complement Alter Med. 2018;2018.
22. Kim HS, Kim SY, Kim HJ, Kim ES, Kim YI. The effect of acupotomy on lumbar herniated intervertebral disc: report of a case series. J Acupunct Res. 2015;32(3):185–195. doi:10.13045/acupunct.2015050
23. Kim SY, Kim HJ, Ji YS, Lee SM, Kim YI. The effect of acupotomy on lumbar and cervical spine combined with oriental medical treatment: report of five cases. J Acupunct Res. 2014;31(2):183–193. doi:10.13045/acupunct.2014036
24. Jeong JK, Kim YI, Kim E, et al. Effectiveness and safety of acupotomy for treating back and/or leg pain in patients with lumbar disc herniation: a study protocol for a multicenter, randomized, controlled, clinical trial. Medicine. 2018;97(34):e11951. doi:10.1097/MD.0000000000011951
25. Jeon G-S, Choi E-S, Lee H-Y. Gender-related difference in the utilization of health care services by Korean adults. J Korean Acad Public Health Nurs. 2010;24(2):182–196.
26. Stratford PW, Binkley JM. Applying the results of self-report measures to individual patients: an example using the Roland-Morris Questionnaire. J Orthop Sports Phys Ther. 1999;29(4):232–239. doi:10.2519/jospt.1999.29.4.232
27. Roland M, Morris R. A study of the natural history of back pain. Part I: development of a reliable and sensitive measure of disability in low-back pain. Spine. 1983;8(2):141–144. doi:10.1097/00007632-198303000-00004
28. Tousignant M, Poulin L, Marchand S, Viau A, Place C. The modified-modified Schober test for range of motion assessment of lumbar flexion in patients with low back pain: a study of criterion validity, intra- and inter-rater reliability and minimum metrically detectable change. Disabil Rehabil. 2005;27(10):553–559. doi:10.1080/09638280400018411
29. Lee YK, Nam HS, Chuang LH, et al. South Korean time trade-off values for EQ-5D health states: modeling with observed values for 101 health states. Value Health. 2009;12(8):1187–1193. doi:10.1111/j.1524-4733.2009.00579.x
30. Ostelo RW, de Vet HC. Clinically important outcomes in low back pain. Best Pract Res Clin Rheumatol. 2005;19(4):593–607. doi:10.1016/j.berh.2005.03.003
31. Jaeschke R, Singer J, Guyatt GH. Measurement of health status. Ascertaining the minimal clinically important difference. Control Clin Trials. 1989;10(4):407–415. doi:10.1016/0197-2456(89)90005-6
32. Dworkin RH, Turk DC, Wyrwich KW, et al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J Pain. 2008;9(2):105–121. doi:10.1016/j.jpain.2007.09.005
33. Beurskens AJ, de Vet HC, Koke AJ. Responsiveness of functional status in low back pain: a comparison of different instruments. Pain. 1996;65(1):71–76. doi:10.1016/0304-3959(95)00149-2
34. Farrar JT, Young JP
35. LX H. Acupuncture Treatment Categorized Collection of Literature on Chinese Acupuncture and Moxibustion Technique.
36. Lee GM, Lee EY, Han JH, Cho KH, Kang SR, Yoon SH. Effects of wonli acupuncture procedure in patients with LSS: a clinical, retrospective study. Evid Based Complement Alternat Med. 2014;2014:212098. doi:10.1155/2014/212098
37. Inoue M, Kitakoji H, Yano T, Ishizaki N, Itoi M, Katsumi Y. Acupuncture treatment for low back pain and lower limb symptoms-the relation between acupuncture or electroacupuncture stimulation and sciatic nerve blood flow. Evid Based Complement Alternat Med. 2008;5(2):133–143. doi:10.1093/ecam/nem050
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

