Back to Journals » Adolescent Health, Medicine and Therapeutics » Volume 14
A Scoping Review Exploring Access to Survivorship Care for Childhood, Adolescent, and Young Adult Cancer Survivors: How Can We Optimize Care Pathways?
Authors McLoone JK, Sansom-Daly UM, Paglia A, Chia J, Larsen HB, Fern LA, Cohn RJ, Signorelli C
Received 20 July 2023
Accepted for publication 11 September 2023
Published 21 September 2023 Volume 2023:14 Pages 153—174
DOI https://doi.org/10.2147/AHMT.S428215
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor M Constantine Samaan
Jordana K McLoone,1,2 Ursula M Sansom-Daly,1,2 Alexia Paglia,1,2 Jessica Chia,1,2 Hanne Bækgaard Larsen,3 Lorna A Fern,4 Richard J Cohn,1,2 Christina Signorelli1,2
1Behavioural Sciences Unit, Discipline of Paediatrics & Child Health, School of Clinical Medicine, UNSW Medicine & Health, Randwick Clinical Campus, UNSW Sydney, Sydney, NSW, Australia; 2Kids Cancer Centre, Sydney Children’s Hospital, Randwick, NSW, Australia; 3Department for Pediatric and Adolescent Medicine, The Juliane Marie Center, Copenhagen University Hospital–Rigshospitalet, Copenhagen, Denmark & Faculty of Health and Medical Sciences, University of Copenhagen, Copenhagen, Denmark; 4Cancer Clinical Trials Unit, University College London Hospitals NHS Foundation Trust, London, NW1 2PG, UK
Correspondence: Jordana K McLoone, Discipline of Paediatrics & Child Health, UNSW Medicine & Health, Randwick Clinical Campus, UNSW, Sydney, NSW, Australia, Email [email protected]
Abstract: Childhood, adolescent, and young adult (CAYA) cancer survivors are at risk of developing late effects associated with their cancer and its treatment. Survivors’ engagement with recommended follow-up care to minimize these risks is suboptimal, with many barriers commonly reported. This scoping review aims to summarize the barriers to accessing follow-up care, using the dimensions of Levesque’s framework for accessing healthcare. We retrieved quantitative studies addressing barriers and facilitators to accessing survivorship care in CAYA survivors from PubMed, EMBASE and CINAHL. Data was categorized into the five healthcare access dimensions outlined in Levesque’s framework: i) approachability, ii) acceptability, iii) availability and accommodation, iv) affordability, and v) appropriateness. We identified 27 quantitative studies in our review. Commonly reported barriers to accessing care included a lack of survivor and provider knowledge of cancer survivorship, poor health beliefs, low personal salience to engage in follow-up care, high out-of-pocket costs and survivors living long distances from clinical services. Many studies reported increased barriers to care during the transition from paediatric to adult-oriented healthcare services, including a lack of developmentally appropriate services, lack of appointment reminders, and a poorly defined transition process. Healthcare-related self-efficacy was identified as an important facilitator to accessing follow-up care. The transition from pediatric to adult-oriented healthcare services is a challenging time for childhood, adolescent, and young adult cancer survivors. Optimizing CAYAs’ ability to access high-quality survivorship care thus requires careful consideration of the quality and acceptability of services, alongside financial and physical/practical barriers (eg distance from available services, appointment-booking mechanisms). Levesque’s model highlighted several areas where evidence is well established (eg financial barriers) or lacking (eg factors associated with engagement in follow-up care) which are useful to understand barriers and facilitators that impact access to survivorship for CAYA cancer survivors, as well as guiding areas for further evaluation.
Keywords: pediatric, adolescent and young adult, cancer, survivorship care, barriers, access to care
Introduction
Long-term survival rates for most childhood, adolescent, and young adult (CAYA) cancers have increased significantly over the last few decades owing to rapid advancements in diagnostic and treatment methods.1,2 The five-year survival rate for most CAYAs diagnosed with cancer is now above 80–90% in western countries, with the survivorship period extending decades into adulthood.1,2 Despite increased survival, CAYA survivors face a significant risk of developing late effects from their cancer and/or its treatment, which may develop years or decades later. Up to 96% of survivors are likely to develop an average of five severe, disabling or life-threatening chronic health conditions as a result of their cancer and its related interventions.3 Common late effects include, but are not limited to, endocrine, cardiovascular, neurocognitive, pulmonary, reproductive disorders and premature aging.4–6
Late effects are typically associated with unique treatment regimens and cancer diagnoses.7,8 For example, head and neck radiotherapy increases a patient’s risk of developing pituitary and thyroid associated hormone dysregulation, while chemotherapies such as alkylating agents can cause gonadal dysfunction, leading to subsequent late effects including osteoporosis and infertility, as well as secondary cancers. Use of corticosteroid treatments – widely used across a range of cancer diagnoses and treatment regimens, including bone-marrow transplants – can similarly increase the risk of diabetes and metabolic syndrome.9
In addition to physical late effects, survivors may experience significant psychological, social, and functional late effects, as well as stress from their ongoing medical conditions, which is associated with poorer health outcomes across multiple psychosocial domains.10 While most long-term CAYA survivors do not report significant mental health conditions, they remain at a higher risk of developing psychological symptoms in comparison to the general population, impacting their quality of life.11,12 This includes being at a 20% higher risk of suicidality compared to age-matched peers from the general population.13,14 A subset of CAYA survivors are susceptible to developing symptoms of depression and anxiety, with elevated levels of distress still reported decades into the follow-up period.12,15,16 The psychosocial impacts of cancer survivorship are especially salient for adolescent and young adult patients, as they navigate multiple challenges in achieving developmental milestones such as gaining independence and the formation of self-identity.17 Diagnosis and cancer treatment as an adolescent can cause significant disruptions in family and social relations, educational and vocational aspirations and achievements as well as physical and psychosocial health challenges.17–19 Interruptions to education, work, financial independence, and changing personal relations may in themselves become barriers to receiving follow-up care, particularly for CAYA survivors for whom finances and/or family/carer support are critical enablers to follow-up attendance.17 Overall, the challenges associated with cancer diagnosis during adolescence can have far-reaching effects on survivors, affecting physical, emotional, and social well-being in the long term.
Engagement with Survivorship Care
The goal of survivorship care is to screen for treatment-related toxicities including recurrent and secondary cancers, and to reduce the burden of late effects experienced by CAYA cancer survivors. A comprehensive and multidisciplinary approach to follow-up care focuses on preventing or managing late effects through education, surveillance and by discouraging risky healthy behaviors which may further heighten survivors’ risk of late effects.20,21 Despite the documented benefits of follow-up care,20 these services tend to be underutilized by survivors, particularly by childhood and adolescent survivors who often become disengaged from follow-up care following the transition from pediatric to adult healthcare. A study from the United States (US) involving 11,000 childhood cancer survivors showed that less than half of high-risk survivors engaged in follow-up surveillance for subsequent or secondary cancers (12.6%) and cardiac disorders (41.4%).22 An Australian and New Zealand bi-national study found that up to 68.5% of long-term childhood cancer survivors reported not engaging in any cancer-related follow-up care and highlighted several system, provider and patient-related barriers to care.23 Even in Westernized countries with comprehensive healthcare systems, follow-up care rates are suboptimal with survivors’ engagement diminishing as they age.23,24 It is plausible that these patterns of sub-optimal engagement in long-term follow-up care may be driven, at least in part, by a lack of consistent frameworks for follow-up care.
Barriers to Accessing Care
Barriers at the patient, provider, and healthcare system levels may contribute to sub-optimal engagement in survivorship care. At the patient level, childhood and adolescent survivors may have poor knowledge of their past cancer diagnosis and the treatment they received as well as their need for long-term follow-up care.25 At the provider level, primary care providers (PCPs) may lack awareness of the complexities of survivorship care, including survivorship guidelines, surveillance and treatment needs, and consequently, may not refer survivors to recommend screening and management protocols.26–28 The presence of system-level barriers in the delivery of survivorship care reflects the abrupt transition of pediatric cancer patients to adult healthcare services and the lack of comprehensive guidelines governing the provision of survivorship care.24,29 Addressing these obstacles is critical to improving the quality of survivorship care for patients, as they can significantly impact the continuity and effectiveness of care across the cancer survivorship trajectory.
Multidimensional Nature of Accessing Healthcare
Efforts to improve access to survivorship care need to address an overarching conceptualization of healthcare access, acknowledging the various patient, provider and healthcare system factors that can limit access. The term “access to care” has varying definitions but is broadly used to describe the ability or opportunity to obtain appropriate healthcare resources.30,31 Levesque et al’s 2013 model defines access as the opportunity to receive healthcare, along the entire process from the moment patients identify the need for care, seek out and reach care, to the moment they utilize care that is appropriate for their needs.32 This model conceptualizes healthcare access as consisting of five dimensions: i) approachability, ii) acceptability, iii) availability and accommodation, iv) affordability, and v) appropriateness. The framework’s dimensions are further organized into supply- and demand-side factors. Supply-side factors relate to the healthcare provider (eg, location of services, quality of services provided), while demand-side factors involve the patients, families and communities who require care (eg, health literacy, income, social support; see Figure 1). This framework offers a clear structure that conceptualizes the obstacles that impede access to healthcare, so that they can be optimized. It is one of the most comprehensive frameworks for healthcare access, as it considers factors across all stakeholder perspectives and across the full trajectory of obtaining care.
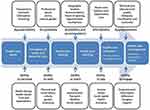 |
Figure 1 Levesque framework. Notes: Reproduced from Levesque JF, Harris MF, Russell G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. International Journal for Equity in Health. 2013;12(1):18. Creative Commons.32 |
Despite research studies reporting barriers or facilitators to accessing care, access to long-term follow-up care within CAYA cancer survivors remains complex and poorly understood. To advance research and clinical survivorship care, barriers and facilitators need to be conceptualized in terms of the level to which they impact on CAYA survivors’ ability to access and engage with survivorship care. The next clear step to achieve this aim is to cohesively map existing data on barriers/facilitators to inform a clear overarching conceptual model to identify opportunities for meaningful changes that can be made to optimize successful healthcare access.24,33–35 Our review aimed to synthesize existing data and map this onto the conceptual dimensions of Levesque et al model of healthcare access.32
Methods
Search Strategy
The literature search was performed in August 2022 for literature from the past 20 years (2002–2022) to maximize relevance to the current delivery of healthcare. We searched three databases (PubMed, Embase and CINAHL) and limited to papers published in the English language. Search terms were used to restrict the search to the CAYA cancer survivor population including (child OR paediatric OR adolescent OR young adult) AND (cancer OR oncology). These were combined with terms relating to survivorship care including (“long term follow-up care” OR “follow-up care” OR “survivorship care”). These were combined with the terms (access OR barriers OR facilitators). We prioritized manuscripts with original data and excluded non-original works such as conference abstracts or reviews.
We downloaded papers to Endnote and removed duplicates. We then uploaded the remaining papers to Rayyan where the titles and abstracts of each of the paper were screened by two authors (JC, CS) to identify papers that focused on barriers/facilitators to care among survivors of child, adolescent, or young adult cancers. We then performed full text-reviews to screen for papers that provided a quantitative assessment of barriers or facilitators to long-term follow-up care. Figure 2 summarizes the screening process.
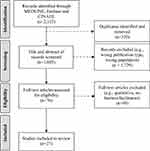 |
Figure 2 PRISMA flow diagram of studies identified for inclusion. |
Inclusion and Exclusion Criteria
Research papers were deemed eligible for inclusion within the scoping review if the paper:
- Assessed barriers or facilitators to long-term follow-up care in the CAYA survivor population (ie diagnosed before age 39 years). We considered all aspects of cancer-related follow-up care were included, eg, physical, functional and/or mental care needs.
- Included original quantitative data identifying barriers or facilitators to long-term follow-up care.
- Included self-reported data drawn from either patient and/or provider perspectives.
While there is agreement in the unique needs of the CAYA cohort,36 the definition of childhood, adolescents, and young adults often varies. Children are generally considered those diagnosed under the age 14, 16 or 18 years, with the start of adolescence beginning around the age of 14/15, therefore there can be overlap between “children and adolescents” within countries depending on age restrictions on access to children’s services. Globally the definition of young adulthood varies for example the upper age limit in the United Kindgom is 24/25 years, compared to 29 years in Australia or 39 years in the United States. For the purposes of this review, we defined children as those who are diagnosed <16 years, adolescents those diagnosed between 14 and 21 years, and young adults as those diagnosed 21–39 years consistent with the broadest global definition.
Data Extraction
Quantitative data on barriers and facilitators were extracted from the eligible papers. Barriers and facilitators were categorized into Levesque’s five dimensions of healthcare access:32 approachability, acceptability, availability and accommodation, affordability, and appropriateness, as defined below:
- Approachability: refers to the capacity of individuals with health requirements to effectively recognize the availability of services, access them, and experience positive effects on their well-being.
- Acceptability: reflects cultural and social factors that influence an individual’s ability to accept aspects of care as well as how they judge the appropriateness of seeking care.
- Availability and accommodation: involve the physical existence of health resources with sufficient capacity to produce health services. Further, the ability of health services to be reached in a timely manner.
- Affordability: reflects the economic capacity for people to spend resources in terms of time and money to use appropriate resources.
- Appropriateness: denotes the fit between services and patients’ needs, its timeliness and the amount of care taken to assess health problems and determine the correct treatment, and the technical and interpersonal quality of the services provided.
We further categorized these according to the PRISMA flow diagram as shown in Figure 2 and noted any factors that could not be incorporated into Levesque’s model of healthcare access. According to the model, barriers and facilitators were then organized into demand-side factors (relating to patient and parent/carer factors), and supply-side factors (relating to provider and health-system barriers).
To maximize coding validity, we employed a dual-coding method. The data was first coded by author JC and then blind-coded a second time by author AP. Any discrepancies were discussed by the wider authorship team until consensus was reached. Given the subjective nature of interpretation, and the way barriers expressed themselves in the studies, some barriers could have been categorized into several dimensions of the model. Where barriers appeared to relate to more than one dimension of the model, we categorized the barrier in the dimension it primarily related to.
Results
Study Characteristics
Twenty-seven studies were included in this review, representing 8255 CAYA survivors, 104 parents of CAYA survivors and 434 healthcare professionals, with data having been collected from across 574 institutions. Access to survivorship care was analyzed based on Levesque et al framework.32 The majority of papers reported on survivors from the US (18/29, 62%), followed by Australia (4/29, 14%), Switzerland (4/29, 14%), Germany (1/29, 3%) and Japan (1/29, 3%). Around two-thirds of participants represented in these studies were childhood or adolescent cancer survivors (diagnosed <18 years), and the remaining one-third were young adults (diagnosed 18–29 years). Other participant groups included parents, pediatric oncologists, medical institutions, primary care practitioners (PCPs), pediatric medical directors and clinical nurses. Most studies reported barriers from survivors’ perspectives (48%), with other studies reporting barriers from institution (19%), oncologist/PCP (11%) and parent-reported perspectives (7%). Most studies assessed overall follow-up care (67%), and transition from adolescent to adult-based care (19%). The remaining care types (15%) primarily included PCP-led care and survivorship clinics. The study findings are summarized in Table 1.
 |
Table 1 Key Findings Summarized According to Levesque’s Five Dimensions of Accessing Healthcare32 |
Dimension 1: Approachability and the Ability to Perceive
Approachability was reported in fifteen of the twenty-seven studies. Of these studies, thirteen evaluated the perspectives of AYA survivors with the remaining two including that of parents and PCPs.
Supply-Side Factors: Transparency, Outreach, Information and Screening
Patients reported several barriers associated with the approachability of survivorship and screening services, including a lack of transparency, outreach, and information provision. Patients reported being unaware that survivorship clinics and/or appropriate follow-up services existed. Most survivors reported feeling disconnected from their cancer treatment centers and lacked information about their need for medical follow-up, with many survivors unable to discern the purpose of accessing survivorship care.23,42,50,58
Demand-Side Factors: Ability to Seek, Health Beliefs, Health Literacy, Trust and Expectations
The primary reasons survivors reported for not attending specialist follow-up care included a lack of information about follow-up care, the belief that follow-up care was unnecessary and a low perceived need to attend a survivorship clinic due to current good health.23,42,47,48,50,51,58 Some survivors lacked knowledge about their diagnosis, disease, the treatment they were given, and the late effects and risks associated with childhood cancer.61 The belief that follow-up care is unnecessary was associated with significantly decreased levels of attendance at follow-up care.23,47 Conversely, increased attendance was associated with survivors perceiving value in attending long-term follow-up care because it facilitated necessary yearly check-ups and cancer screening.60 Knowledge about the need for follow-up care was also significantly associated with follow-up care attendance in the past two years.50 Survivors in two studies reported, however, that they did not attend follow-up care on the advice of their healthcare providers who had reportedly indicated there was “no need”.42,48
In terms of seeking survivorship care in the primary sector, patients in one study questioned whether PCPs had adequate knowledge about childhood cancer survivorship and lacked confidence in the PCPs’ ability to provide satisfactory survivorship care.57 Survivors reported perceiving that PCPs lacked appropriate knowledge regarding primary diagnosis, treatment and the potential risks of long-term complications, as well as recommended follow-up care. This was perceived as a barrier to seeking PCP-based follow-up care, in favor of oncologist-led care.23 Two studies reported that competent providers and “being taking taken seriously” were most important to patients during appointments, with the latter creating trust in the PCP and strengthening rapport between doctor and patient.51,57
Dimension 2: Acceptability and the Ability to Seek
Fifteen studies assessed aspects of healthcare acceptability, and the ability to seek care. Most barriers related to the acceptability of care were reported by healthcare providers, while barriers related to the ability to seek care were reported by survivors and parents of survivors.
Supply-Side Factors: Professional Values and Norms
Healthcare professionals including oncologists, healthcare policy experts and representatives from Children’s Oncology Group institutions identified a general lack of interest and support from healthcare organizations to provide long-term follow-up care for childhood cancer survivors.41,49,61 Survivorship issues were reported to be underappreciated in the healthcare system with organizational values prioritizing treatment first and providing the care of chronic illnesses within the remit of other non-oncology specialists. However, primary care providers (PCPs) reported numerous barriers to providing childhood cancer survivorship care, including a lack of confidence and understanding about the potential risks associated with treatments, the long-term effects they may have, inadequate funding, and time constraints.57 Providers in three studies also noted the culture of some oncologists not wanting to “let go” of patients as they transitioned from pediatric to adult care, which was perceived as a barrier to providing ongoing survivorship care outside of the pediatric and/or tertiary setting.43,45,55
Demand-Side Factors: Personal and Social Values, Autonomy and Survivor Demographics
Some adolescent cancer survivors reported negative emotions, and having developed aversions to clinical settings, which impacted their ability to engage with survivorship care.24,42,57 Some survivors reported fear of discovering late effects, being diagnosed with a secondary or recurring cancer, and painful memories of cancer treatment as barriers to seeking care.44,61 Survivors also reported that returning to the hospital where they received painful and traumatic cancer treatments triggered distress, which they felt inhibited them from “moving on” from their cancer.23,58 By contrast, one study found that having health concerns was associated with an increased likelihood of having a cancer-related health visit.44
Health-related self-efficacy – or the confidence to manage one’s own healthcare – was also positively associated with follow-up care attendance.50,53 Patients also reported that feelings of “readiness” eased their transition from pediatric to adult-based care.40,56 Conversely, feelings of reluctance or hesitancy were associated with greater disengagement from survivorship care.60
Seven studies assessed the correlation between survivor characteristics and survivorship care attendance. There was mixed evidence on the correlation between age and attendance. While most studies suggested that younger survivors were more likely to seek and attend follow-up care, Ernst et al’s study reported a positive association between older age and follow-up care attendance.42 The influence of sex on attendance was found to be negligible, except for two studies that reported a lower likelihood of follow-up care attendance among male survivors. Two studies that analyzed patient data from the United States showed that non-Caucasian survivors were less likely to attend follow-up care than Caucasian survivors.
Dimension 3: Availability, Accommodation and the Ability to Reach
Fifteen studies identified barriers and facilitators associated with the availability of survivorship services. Ten provided the perspectives of the childhood cancer survivors, four on the perspectives of healthcare providers (eg, oncologists), and one of the perspectives of parents of survivors.
Supply-Side Factors: Availability of Resources and Providers, Geographic Location, Opening
Hours and Appointment Mechanisms
The four studies involving healthcare providers highlighted that limited availability of healthcare resources and providers were significant barriers to the delivery of survivorship care. All four studies reported a lack of long-term follow-up programs, adult providers with childhood cancer and survivorship expertise, and subspecialty providers (eg, oncologists), which limited the availability of healthcare services.49,55,59,61 Many survivors reported that the limited availability of services and the fact that they are concentrated within urban, metropolitan centers was an obstacle to accessing follow-up care, particularly when they had relocated back to their home communities and services became too far away.24,48,58 Centers that limited appointments to within business hours only also restricted access, as there was no availability at times most preferred by survivors who worked full time, had schooling commitments or whose parents (who provided support and transportation) worked full time.23,56
Demand-Side Factors: Living Environments, Social Support, Transportation and Mobility
Survivors reported logistical reasons as barriers to attending follow-up visits. An inability to reach follow-up services was primarily related to transportation problems or the inability to travel without the assistance of a parent/caregiver due to age and/or a patient’s mobility needs.46 Some young adult survivors reported that they disengaged from follow-up care because their parents did not prompt or remind them.24 Other logistical barriers included the poor health of other family members, finding childcare, the inconvenience of attending appointments, and the inability or unwillingness to take leave from their workplace.
Dimension 4: Affordability and the Ability to Pay
Twenty studies assessed financial factors that affected the provision of survivorship care or access to these services. Out-of-pocket costs and funding challenges were commonly reported by survivors and providers, respectively.
Supply-Side Factors: Direct, Indirect and Opportunity Costs
Healthcare providers in four studies listed a lack of funding as a significant barrier to providing follow-up services. Providers reported that insufficient funding was linked to staff shortages in clinics,23 with some also reporting limited physical space and other resources as impacting service provision. Survivors also reported that direct healthcare expenses and medical costs were also barriers to care.23
Demand-Side Factors: Insurance, Out of Pocket Expenses and Lack of Financial Support
Insufficient insurance coverage was a significant barrier to obtaining survivorship care, as reported by several studies from the US. Additionally, four studies listed insurance acceptability and opportunity for insurance counselling as facilitators of follow-up care and transition from pediatric to adult care.38,40,56 Survivors expressed concerns that being diagnosed with late effects during follow-up care might cause them to lose their existing health insurance, which would impact their ability to pay for healthcare.61 Mertens et al noted that in some healthcare systems, insurance did not adequately cover preventative healthcare, negatively affecting a survivor’s ability to afford and access care.49 Any change in survivor health insurance was associated with a decreased likelihood of follow-up care attendance.54 Survivors also identified opportunity costs from lost wages, lack of financial support, and high perceived cost of medical expenses such as screening examinations as obstacles to obtaining survivorship care.
Dimension 5: Appropriateness and Ability to Engage
Fifteen studies assessed the appropriateness of existing services and survivors’ ability to engage with survivorship care. Many factors were associated with the quality of services and the challenges of transitioning survivors from pediatric to adult care.
Supply Side Factors: Technical and Interpersonal Quality, Adequacy, Coordination and Continuity
Healthcare providers and survivors in several studies reported that existing primary care providers and non-oncology specialists did not appear to have sufficient knowledge about survivors of childhood and adolescent cancers.43,49,55,57 This included knowledge about late effects, recommended surveillance schedules and general survivorship information as well as an inability to differentiate if health problems were related to a previous cancer or cancer treatment or not. For example, Sadak et al found that the lack of knowledge in childhood cancer survivorship among available adult providers was the second most common barrier (55%) to providing survivorship care to adult childhood cancer survivors.56 Access to comprehensive care, including other sub-specialists (eg, fertility and endocrinology), mental health professionals (eg, social workers and psychologists), and vocational training was considered a crucial aspect of survivorship care by the majority of childhood cancer survivors and parents of survivors in two studies.40,56
Healthcare providers noted that poor coordination of care between pediatric and adult providers resulted in inadequate services for older survivors remaining in pediatric settings.23 Coordination and continuity was reported to be an important factor in the ability to engage with follow-up care, particularly in the context of transitioning from pediatric to adult care.52 Poor communication was reported between providers in most of the studies, with one study reporting administrative pressure to transition or discharge patients from pediatric services over the age of 18.59 Oncologists also wanted to receive more feedback from primary care providers about their patients, while primary care providers expressed a preference for specific management plans to be prepared for them.57 Providers in one study reported difficulties in identifying/reaching survivors, while providers and patients in three studies reported difficulties locating medical records across pediatrics and adult clinics.37,49,61
Survivors expressed that they preferred to continue receiving care from the same doctor, rather than changing doctors with every visit. Patients in two studies identified that having a single identified contact person was an important facilitator during the transition to adult care.40,56 Providers in three studies also suggested that the undefined transition process and insufficient or conflicting follow-up guidelines were barriers to care engagement.23,43,49,59
Demand-Side Factors: Empowerment, Information, Adherence and Caregiver Support
Few studies examined survivors’ ability to engage in survivorship care. Survivors and parents in two studies perceived that it was important for adult-based services to promote independence and personal responsibility in survivors who were transitioning out of pediatric services.40,56
Discussion
This scoping review used Levesque et al's conceptual framework of access to care, including dimensions of approachability, acceptability, availability and accommodation, affordability, and appropriateness to conceptualize factors affecting access to long-term follow-up care in CAYA survivors. We identified barriers across all dimensions of healthcare access, which we further organized into the Framework’s demand side factors (relating to patient and parent factors) and supply side factors (relating to provider and health system barriers). Commonly reported barriers included practical concerns such as distance from available services, transportation issues, appointment reminders, out-of-pocket costs and lack of financial support. However, our review also revealed several barriers specific to adolescent and young adult survivors. These included, but were not limited to, a lack of CAYA cancer survivorship services and changes to living arrangements and social support as survivors transitioned from pediatric to adult care. Although several studies in our review acknowledged the significance of patient–provider relationships and survivors’ self-efficacy in healthcare management, only a limited number of them addressed the facilitators that contribute to their development.
The distance survivors must travel to access survivorship services has consistently been reported within the literature as being too far, too expensive, and too inconvenient for survivors to manage on a regular basis.24,48,58 Greater involvement of PCPs may alleviate some of the challenges associated with accessing survivorship care by necessitating less patient travel, shorter wait times and by capitalizing on a patient’s familiarity with their local doctor to facilitate regular care. However, the literature suggests that primary care physicians report insufficient education and training about childhood cancer survivorship, including the potential late effects of cancer and its treatment, leading to difficulties managing these patients.57 Facilitating better communication between PCPs and oncologists may enable patients to fully benefit from community-based survivorship services while also ensuring that PCPs received the specialized education and training needed to deliver high-quality care.62
Our review identified several demand-side factors that impeded CAYA survivors’ attendance at a survivorship clinic. These factors included moving away from home to pursue higher education and reduced parental involvement in their care, leading to a lack of appointment scheduling and attendance reminders. This reflects challenges explained in the literature, which shows how young survivors are increasingly expected to manage their own care while navigating personal and social challenges as well as challenges within their living environments.24,25,28 These survivors have also expressed the necessity for developmentally appropriate care that recognizes their need for autonomy while also recognizing the potential need for parental involvement.35
Some novel survivorship care delivery models have emerged in recent years to address the dual challenges of the AYA developmental period, and the complexity of continuing to engage AYA survivors of child and adolescent cancer in the critical importance of ongoing surveillance for cancer-related late-effects, years after this seems most salient. For example, in Australia, the Engage program – a nurse-led e-health intervention involving a personalized follow-up care plan for survivors, has shown success in increasing survivor self-efficacy and engagement in follow-up care.58 The program ensures multidisciplinary communication, seeking review from medical specialists such as pediatric oncologists, clinical psychologists, endocrinologists, neurologists, and allied health. This may be particularly useful given how prevalent distance was as an identified barrier in this review. Additional research is necessary to identify potential enhancements to current care models and explore other viable methods of care delivery that can offer high-quality services to cancer survivors.
Despite the recognized need for childhood and adolescent specific services, there is an inadequate provision of services like Engage within Australia and overseas.63,64 Greater funding and support are needed to ensure survivors receive developmentally appropriate care. Considering the gaps in these services, promoting healthcare self-efficacy is necessary to ensure survivors have the confidence and abilities to engage with existing adult-oriented services.50,65 Interestingly, in our review, only seven of the 27 studies looked at CAYA survivor characteristics associated with engagement in survivorship care. This may suggest a gap in the literature in terms of understanding factors that may contribute to survivors’ engagement in care – and individuals for whom survivorship care services currently work better, and less well, for. Understanding survivors’ individual characteristics and related healthcare needs will also inform how multidisciplinary survivorship care can best address the unique physical and psychosocial needs of childhood and adolescent survivors. Depending on the needs of individual survivors, services that are likely to augment the impact and relevance of survivorship care are likely to include well-integrated mental health services, fertility preservation, education and vocational support.16,18
Limitations and Future Directions
A key limitation of our review is the inclusion of only studies published in English, as it may exclude the additional challenges faced in different cultural and healthcare contexts and populations. Within the constraints of literature published in Englishto date, studies have only reported on barriers to survivorship care in high-income countries, where advances in survivorship have led to the need for, and empirical focus on, how survivorship care is delivered (and accessed); unfortunately, in the low-to-medium income setting, the burden of childhood cancer is greatest, yet survival rates also remain the poorest.66 Indeed, two-thirds of our included papers were from the US, which has unique and specific financial considerations with regard to healthcare insurance. Another limitation could be whether the framework adequately captures all reported barriers. While no barriers were unable to fit within the model, future research can be guided by the lack of research published in certain dimensions. A strength of our review is its ability to provide a comprehensive summary and synthesis of the literature, across a myriad of countries and contexts. However, it should be acknowledged that the inherent complexity and uniqueness of healthcare settings may also limit how much each finding can be related to an individual country or clinical setting. To further build understanding of CAYA survivorship healthcare access in the literature, future work could build on the present analysis with qualitative data, which may add further insights as to how barriers to survivorship care are experienced from multiple perspectives.
Conclusion
This review provides a comprehensive overview of the barriers that survivors must overcome to receive adequate and appropriate survivorship care. To optimize survivorship healthcare services, each of the barriers within the Levesque framework needs to be overcome, with emphasis on the importance of patient-related factors such as personal values and perceptions of care. When developing future guidelines and survivorship programs, it is important to consider the intricate interplay between barriers and facilitators through the entire process from seeking to obtaining care. This includes addressing obstacles that may arise at various stages of a patient’s healthcare journey, as well as identifying strategies to promote access and offer support to childhood cancer survivors.
Data Sharing Statement
Data are available on request from the authors.
Funding
Dr Jordana McLoone is supported by an MRFF Brain Cancer Survivorship grant (MRFBC000002). Dr Ursula-Sansom Daly (2020/ECF1163) and Dr Christina Signorelli (2020/ECF1144) are supported by Cancer Institute NSW Early Career Fellowships. Dr Lorna Fern is funded by Teenage Cancer Trust. These funding bodies did not have any role in the study, writing of the manuscript, or decision to submit for publication.
Disclosure
The authors have no conflicts of interest to declare in this work.
References
1. Society AC. Key Statistics for Childhood Cancers; 2023. Available from: https://www.cancer.org/cancer/types/cancer-in-children/key-statistics.html.
2. Welfare AIoHa. Cancer in adolescents and young adults in Australia 2023. 2023.
3. Signorelli C, Fardell JE, Wakefield CE, Webber K, Cohn RJ. The cost of cure: chronic conditions in survivors of child, adolescent, and young adult cancers. In: Cancer and Chronic Conditions: Addressing the Problem of Multimorbidity in Cancer Patients and Survivors. Springer; 2016:371–420.
4. Williams AM, Mandelblatt J, Wang M, et al. Premature aging as an accumulation of deficits in young adult survivors of pediatric cancer. JNCI. 2023;115(2):200–207. doi:10.1093/jnci/djac209
5. Bright CJ, Hawkins MM, Guha J, et al. Risk of cerebrovascular events in 178 962 five-year survivors of cancer diagnosed at 15 to 39 years of age: the TYACSS (Teenage and Young Adult Cancer Survivor Study). Circulation. 2017;135(13):1194–1210. doi:10.1161/CIRCULATIONAHA.116.025778
6. Van Dorp W, Haupt R, Anderson RA, et al. Reproductive function and outcomes in female survivors of childhood, adolescent, and young adult cancer: a review. J Clin Oncol. 2018;36(21):2169. doi:10.1200/JCO.2017.76.3441
7. Signorelli C, Wakefield CE, McLoone JK, et al. Childhood cancer survivors’ reported late effects, motivations for seeking survivorship care, and patterns of attendance. Oncologist. 2023;28(5):e276–e86. doi:10.1093/oncolo/oyad004
8. Hudson MM, Bhatia S, Casillas J, et al. Long-term follow-up care for childhood, adolescent, and young adult cancer survivors. Pediatrics. 2021;148(3). doi:10.1542/peds.2021-053127
9. Rose SR, Horne VE, Howell J, et al. Late endocrine effects of childhood cancer. Nat Rev Endocrinol. 2016;12(6):319–336. doi:10.1038/nrendo.2016.45
10. Zhang A, Wang K, Zebrack B, Tan CY, Walling E, Chugh R. Psychosocial, behavioral, and supportive interventions for pediatric, adolescent, and young adult cancer survivors: a systematic review and meta-analysis. Crit Rev Oncol Hematol. 2021;160:103291. doi:10.1016/j.critrevonc.2021.103291
11. Michel G, Brinkman TM, Wakefield CE, Grootenhuis M. Psychological outcomes, health-related quality of life, and neurocognitive functioning in survivors of childhood cancer and their parents. Pediatr Clin. 2020;67(6):1103–1134. doi:10.1016/j.pcl.2020.07.005
12. Fardell JE, Wakefield CE, De Abreu Lourenco R, et al. Long‐term health‐related quality of life in young childhood cancer survivors and their parents. Pediatr Blood Cancer. 2021;68(12):e29398. doi:10.1002/pbc.29398
13. Yang P, Zhang L, Hou X. Incidence of suicide among adolescent and young adult cancer patients: a population-based study. Cancer Cell Int. 2021;21(1):1–11. doi:10.1186/s12935-021-02225-y
14. Brinkman TM, Zhang N, Recklitis CJ, et al. Suicide ideation and associated mortality in adult survivors of childhood cancer. Cancer. 2014;120(2):271–277. doi:10.1002/cncr.28385
15. Brinkman TM, Zhu L, Zeltzer L, et al. Longitudinal patterns of psychological distress in adult survivors of childhood cancer. Br J Cancer. 2013;109(5):1373–1381. doi:10.1038/bjc.2013.428
16. Sansom-Daly UM, Wakefield CE. Distress and adjustment among adolescents and young adults with cancer: an empirical and conceptual review. Transl Pediatr. 2013;2(4):167. doi:10.3978/j.issn.2224-4336.2013.10.06
17. Hydeman JA, Uwazurike OC, Adeyemi EI, Beaupin LK. Survivorship needs of adolescent and young adult cancer survivors: a concept mapping analysis. J Cancer Surviv. 2019;13(1):34–42. doi:10.1007/s11764-018-0725-5
18. Fardell JE, Wakefield CE, Patterson P, et al. Narrative review of the educational, vocational, and financial needs of adolescents and young adults with cancer: recommendations for support and research. J Adolesc Young Adult Oncol. 2018;7(2):143–147. doi:10.1089/jayao.2017.0086
19. Sisk BA, Fasciano K, Block SD, Mack JW. Impact of cancer on school, work, and financial Independence among adolescents and young adults. Cancer. 2020;126(19):4400–4406. doi:10.1002/cncr.33081
20. Signorelli C, Wakefield CE, Fardell JE, et al. The impact of long-term follow-up care for childhood cancer survivors: a systematic review. Crit Rev Oncol Hematol. 2017;114:131–138. doi:10.1016/j.critrevonc.2017.04.007
21. Sansom‐Daly UM, Wilson CL, Ashton LJ, Wakefield CE, Johnston K, Cohn RJ. Further evidence for the co‐occurrence of adverse health behaviors among childhood cancer survivors. Pediatr Blood Cancer. 2013;60(1):167–168. doi:10.1002/pbc.24305
22. Yan AP, Chen Y, Henderson TO, et al. Adherence to surveillance for second malignant neoplasms and cardiac dysfunction in childhood cancer survivors: a childhood cancer survivor study. J Clin Oncol. 2020;38(15):1711. doi:10.1200/JCO.19.01825
23. Signorelli C, Wakefield C, McLoone JK, et al. Childhood cancer survivorship: barriers and preferences. BMJ Support Palliat Care. 2019;12(e5):e687–e695. doi:10.1136/bmjspcare-2019-002001
24. Berg C, Stratton E, Esiashvili N, Mertens A, Berg CJ. Young adult cancer survivors’ experience with cancer treatment and follow-up care and perceptions of barriers to engaging in recommended care. J Cancer Educ. 2016;31(3):430–442. doi:10.1007/s13187-015-0853-9
25. Janssen SHM, van der Graaf WTA, van der Meer DJ, Manten-Horst E, Husson O. Adolescent and Young Adult (AYA) cancer survivorship practices: an overview. Cancers. 2021;13(19):4847. doi:10.3390/cancers13194847
26. Howard AF, Kazanjian A, Pritchard S, et al. Healthcare system barriers to long-term follow-up for adult survivors of childhood cancer in British Columbia, Canada: a qualitative study. J Cancer Surviv. 2018;12(3):277–290. doi:10.1007/s11764-017-0667-3
27. Suh E, Daugherty CK, Wroblewski K, et al. General internists’ preferences and knowledge about the care of adult survivors of childhood cancer: a cross-sectional survey. Ann Intern Med. 2014;160(1):11–17. doi:10.7326/M13-1941
28. Psihogios AM, Pauly-Hubbard H, Schwartz L, Ginsberg JP, Hobbie W, Szalda D. Understanding and improving knowledge of cancer survivorship care among college providers. J Cancer Educ. 2018;33(5):1075–1081. doi:10.1007/s13187-017-1208-5
29. Ryan D, Chafe R, Moorehead P. Transition from pediatric to adult aftercare for survivors of pediatric cancer in Newfoundland and Labrador: a qualitative study. Can Med Assoc Open Access J. 2021;9(2):E309–E16.
30. Oliver A, Mossialos E. Equity of access to health care: outlining the foundations for action. J Epidemiol Community Health. 2004;58(8):655–658. doi:10.1136/jech.2003.017731
31. Gold M. Beyond coverage and supply: measuring access to healthcare in today’s market. Health Serv Res. 1998;33(3 Pt 2):625–684.
32. Levesque J-F, Harris MF, Russell G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. Int J Equity Health. 2013;12(1):18. doi:10.1186/1475-9276-12-18
33. Hendriks MJ, Harju E, Michel G. The unmet needs of childhood cancer survivors in long-term follow-up care: a qualitative study. Psycho Oncol. 2021;30(4):485–492. doi:10.1002/pon.5593
34. Keegan THM, Tao L, DeRouen MC, et al. Medical care in adolescents and young adult cancer survivors: what are the biggest access-related barriers? J Cancer Surviv. 2014;8(2):282–292. doi:10.1007/s11764-013-0332-4
35. Psihogios AM, Schwartz LA, Deatrick JA, et al. Preferences for cancer survivorship care among adolescents and young adults who experienced healthcare transitions and their parents. J Cancer Surviv. 2019;13(4):620–631. doi:10.1007/s11764-019-00781-x
36. Ferrari A, Stark D, Peccatori F, et al. Adolescents and young adults (AYA) with cancer: a position paper from the AYA Working Group of the European Society for Medical Oncology (ESMO) and the European Society for Paediatric Oncology (SIOPE). ESMO open. 2021;6(2):100096. doi:10.1016/j.esmoop.2021.100096
37. Bowers DC, Adhikari S, El-Khashab YM, Gargan L, Oeffinger KC. Survey of long-term follow-up programs in the United States for survivors of childhood brain tumors. Pediatr Blood Cancer. 2009;53(7):1295–1301. doi:10.1002/pbc.22240
38. Christen S, Vetsch J, Mader L, et al. Preferences for the organization of long-term follow-up in adolescent and young adult cancer survivors. Support Care Cancer. 2016;24(8):3425–3436. doi:10.1007/s00520-016-3157-7
39. Cousineau MR, Kim SE, Hamilton AS, Miller KA, Milam J. Insurance Coverage, and having a regular provider, and utilization of cancer follow-up and noncancer health care among childhood cancer survivors. INQUIRY. 2019;56:0046958018817996. doi:10.1177/0046958018817996
40. DiNofia A, Shafer K, Steacy K, Sadak KT. Parent-perceived facilitators in the transition of care for young adult survivors of childhood cancer. J Pediatr Hematol Oncol. 2017;39(7):e377–e80. doi:10.1097/MPH.0000000000000765
41. Effinger KE, Haardörfer R, Marchak JG, et al. Current pediatric cancer survivorship practices: a report from the Children’s Oncology Group. J Cancer Surviv. 2022;17(4):1–10.
42. Ernst M, Brähler E, Faber J, Wild PS, Merzenich H, Beutel ME. A mixed-methods investigation of medical follow-up in long-term childhood cancer survivors: what are the reasons for non-attendance? Front Psychol. 2022;13:846671. doi:10.3389/fpsyg.2022.846671
43. Eshelman-Kent D, Kinahan KE, Hobbie W, et al. Cancer survivorship practices, services, and delivery: a report from the Children’s Oncology Group (COG) nursing discipline, adolescent/young adult, and late effects committees. J Cancer Surviv. 2011;5(4):345–357. doi:10.1007/s11764-011-0192-8
44. Ford JS, Tonorezos ES, Mertens AC, et al. Barriers and facilitators of risk-based health care for adult survivors of childhood cancer: a report from the Childhood Cancer Survivor Study. Cancer. 2020;126(3):619–627. doi:10.1002/cncr.32568
45. Kenney LB, Melvin P, Fishman LN, et al. Transition and transfer of childhood cancer survivors to adult care: a national survey of pediatric oncologists. Pediatr Blood Cancer. 2017;64(2):346–352. doi:10.1002/pbc.26156
46. Klosky JL, Cash DK, Buscemi J, et al. Factors influencing long-term follow-up clinic attendance among survivors of childhood cancer. J Cancer Surviv. 2008;2(4):225–232. doi:10.1007/s11764-008-0063-0
47. Lupatsch JE, Wengenroth L, Rueegg CS, et al. Follow-up care of adolescent survivors of childhood cancer: the role of health beliefs. Pediatr Blood Cancer. 2016;63(2):318–325. doi:10.1002/pbc.25755
48. Maeda N, Horibe K, Kato K, Kojima S, Tsurusawa M. Survey of childhood cancer survivors who stopped follow-up physician visits. Pediatr Int. 2010;52(5):806–812. doi:10.1111/j.1442-200X.2010.03158.x
49. Mertens AC, Cotter KL, Foster BM, et al. Improving health care for adult survivors of childhood cancer: recommendations from a delphi panel of health policy experts. Health Policy. 2004;69(2):169–178. doi:10.1016/j.healthpol.2003.12.008
50. Milam J, Freyer DR, Miller KA, et al. Project Forward: a Population-Based Cohort Among Young Adult Survivors of Childhood Cancers. JNCI Cancer Spectr. 2021;5(5). doi:10.1093/jncics/pkab068
51. Michel G, Kuehni CE, Rebholz CE, et al. Can health beliefs help in explaining attendance to follow-up care? The Swiss Childhood Cancer Survivor Study. Psycho Oncol. 2011;20(10):1034–1043. doi:10.1002/pon.1823
52. Michel G, Gianinazzi ME, Eiser C, et al. Preferences for long-term follow-up care in childhood cancer survivors. Eur J Cancer Care. 2016;25(6):1024–1033. doi:10.1111/ecc.12560
53. Miller KA, Wojcik KY, Ramirez CN, et al. Supporting long-term follow-up of young adult survivors of childhood cancer: correlates of healthcare self-efficacy. Pediatr Blood Cancer. 2017;64(2):358–363. doi:10.1002/pbc.26209
54. Mobley EM, Kim SE, Cousineau M, et al. Insurance coverage change and survivorship care among young adult survivors of childhood cancer. Health Serv Res. 2022;57(1):159–171. doi:10.1111/1475-6773.13868
55. Sadak KT, Szalda D, Lindgren BR, et al. Transitional care practices, services, and delivery in childhood cancer survivor programs: a survey study of U.S. survivorship providers. Pediatr Blood Cancer. 2019;66(8):e27793. doi:10.1002/pbc.27793
56. Sadak KT, Dinofia A, Reaman G. Patient-perceived facilitators in the transition of care for young adult survivors of childhood cancer. Pediatr Blood Cancer. 2013;60(8):1365–1368. doi:10.1002/pbc.24494
57. Thornton-Benko E, Lie HC, Alvaro F, et al. The role of primary care physicians in childhood cancer survivorship care: multiperspective interviews. Oncologist. 2019;24(5):710–719. doi:10.1634/theoncologist.2018-0103
58. Signorelli C, Wakefield CE, Johnston KA, et al. Re-engage: a novel nurse-led program for survivors of childhood cancer who are disengaged from cancer-related care. J Natl Compr Canc Netw. 2020;18(8):1067–1074. doi:10.6004/jnccn.2020.7552
59. Signorelli C, Wakefield CE, McLoone JK, et al. Models of childhood cancer survivorship care in Australia and New Zealand: strengths and challenges. Asia Pac J Clin Oncol. 2017;13(6):407–415. doi:10.1111/ajco.12700
60. Quillen J, Bradley H, Calamaro C. Identifying barriers among childhood cancer survivors transitioning to adult health care. J Pediatr Oncol Nurs. 2017;34(1):20–27. doi:10.1177/1043454216631953
61. Zebrack BJ, Eshelman DA, Hudson MM, et al. Health care for childhood cancer survivors: insights and perspectives from a Delphi panel of young adult survivors of childhood cancer. Cancer. 2004;100(4):843–850. doi:10.1002/cncr.20033
62. Wadhwa A, Chen Y, Bhatia S, Landier W. Providing health care for patients with childhood cancer and survivors: a survey of pediatric primary care providers. Cancer. 2019;125(21):3864–3872. doi:10.1002/cncr.32391
63. Baird H, Patterson P, Medlow S, Allison KR. Understanding and improving survivorship care for adolescents and young adults with cancer. J Adolesc Young Adult Oncol. 2019;8(5):581–586. doi:10.1089/jayao.2019.0031
64. Cheung CK, Zebrack B. What do adolescents and young adults want from cancer resources? Insights from a Delphi panel of AYA patients. Support Care Cancer. 2017;25(1):119–126. doi:10.1007/s00520-016-3396-7
65. Szalda D, Piece L, Brumley L, et al. Associates of engagement in adult-oriented follow-up care for childhood cancer survivors. J Adolesc Health. 2017;60(2):147–153. doi:10.1016/j.jadohealth.2016.08.018
66. Force LM, Abdollahpour I, Advani SM, et al. The global burden of childhood and adolescent cancer in 2017: an analysis of the Global Burden of Disease Study 2017. Lancet Oncol. 2019;20(9):1211–1225. doi:10.1016/S1470-2045(19)30339-0
 © 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
