Back to Journals » OncoTargets and Therapy » Volume 13
A Rare Case of Moderately Differentiated Adenocarcinoma With PD-L1 Overexpression and a Heterogeneous LELC Component in the Ascending Colon
Authors Nagano H, Watanabe T, Togawa T , Ohnishi K, Kimura T, Iida A , Sato Y, Goi T
Received 17 October 2019
Accepted for publication 31 December 2019
Published 28 January 2020 Volume 2020:13 Pages 791—801
DOI https://doi.org/10.2147/OTT.S234945
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Sanjeev K. Srivastava
Hideki Nagano,1 Takeshi Watanabe,1 Tamotsu Togawa,1 Kenji Ohnishi,1 Toshihisa Kimura,1 Atsushi Iida,1 Yasunori Sato,2 Takanori Goi3
1Department of Surgery, National Hospital Organization Tsuruga Medical Center, Fukui 914-0195, Japan; 2Department of Human Pathology, Kanazawa University, Graduate School of Medicine, Kanazawa 920-8640, Japan; 3First Department of Surgery, Faculty of Medicine, University of Fukui, Fukui 910-1193, Japan
Correspondence: Hideki Nagano Tel +81-776-25-1660
Fax +81-770-25-7409
Email [email protected]
Background: Lymphoepithelioma-like carcinomas (LELCs), especially colorectal cancers (CRCs), are uncommon pathological phenotypes generally associated with poor aggressiveness and a preferable prognosis. However, PD-L1 overexpression in CRCs is associated with poor outcomes. We report a case of moderately differentiated adenocarcinoma with PD-L1 overexpression, an LELC component, and Crohn’s-like lymphoid reaction (CLR) presenting with extreme locoregional aggression and complete remission with chemotherapy after noncurative excision.
Case presentation: A 69-year-old man was referred to our hospital for abdominal fullness and pain. Computed tomography (CT) showed a circumferential tumor in the ascending colon, accompanied by bulky swollen lymph nodes. Under the preoperative diagnosis of T4N2M1 (lymph nodes) ascending colon cancer, we performed a right hemicolectomy; however, paracaval and parailiac vein lymph nodes were abandoned. Pathological findings showed moderate to poorly differentiated adenocarcinoma invading the subserosa accompanied by an LELC component invading the superficial muscularis propria. Lymph node metastases were found in a neighboring tumor and in retroperitoneal lymph nodes with glandular differentiation. No relation to microsatellite instability (MSI) or Epstein-Barr virus (EBV) was observed. In the component with glandular differentiation, PD-L1 overexpression was revealed. CLR findings were also observed. The tumor was diagnosed as T3N2M1 cancer that was moderately to poorly differentiated and had an LELC component. The patient was treated with chemotherapy, and the metastasized lymph nodes ultimately disappeared. He was alive without tumor recurrence 5-years post-operation.
Conclusion: This is a very rare case of moderately differentiated adenocarcinoma with PD-L1 overexpression and a heterogeneous LELC component that developed in the ascending colon. Unlike the previously reported weak aggressive properties of LELCs, the present case showed an extremely aggressive locoregional extent, but complete remission was finally achieved with chemotherapy. This type of LELC with CLR could be associated with a good response to chemotherapy and a good prognosis in CRC patients.
Keywords: lymphoepithelioma-like carcinoma, lymphoid stroma, adenocarcinoma, PD-L1, Crohn’s-like lymphoid reaction, colon
Background
Lymphoepithelioma-like carcinoma (LELC) is defined as a tumor with histological similarity to that of nasopharyngeal carcinoma, characterized histologically by a syncytial growth pattern of undifferentiated malignant epithelial cells with ill-defined borders, prominent nucleoli, numerous mitoses, and prominent stromal and intratumoral lymphoid infiltrates.1 LELCs have been described in several organs, including the thymus, salivary glands, lungs, vagina, tonsils, oral cavity, larynx, skin, cervix, stomach, biliary tract, and urinary bladder.1 However, reports of LELCs derived from the colorectum are extremely rare, and we found only eight reports to date, all of which were consistent with LELC findings for the whole lesion.1–8 LELCs are also known to be relatively weakly aggressive in the clinic and have a high survival rate despite their poorly differentiated features,9,10 and similar characteristics have also been reported in previous colorectal cancers (CRCs) with LELC. The interaction between programmed death 1 (PD-1) and programmed death ligand-1 (PD-L1) is one of the most important costimulatory signals; its mediated immunosuppression is an important part of the dynamic immune system balance because it limits the immune response and prevents autoimmune disease.11 A recent meta-analysis revealed that PD-L1 overexpression in CRC was related to short overall survival (OS) and short recurrence-free survival (RFS)/disease-free survival (DFS).11 Crohn’s-like lymphoid reaction (CLR), characterized by peritumoral lymphoid aggregates and discrete lymphoid aggregates, is associated with a low incidence of locoregional recurrence, few distant metastases and prolonged cancer-specific survival and OS.12–15
Herein, we report a case of ascending colon cancer consisting of heterogeneous components of a moderately differentiated adenocarcinoma with PD-L1 overexpression and LELC, and the finding of CLR suggested extremely aggressive locoregional spreading compared with that of ordinary CRC. After noncurative excision, complete remission of residual node metastases with chemotherapy was demonstrated.
This study was approved by the Ethics Committee of the National Hospital Organization Tsuruga Medical Center (registration number: 31-15), and written informed consent was obtained according to the Declaration of Helsinki.
Case Report
A 69-year-old Japanese man experienced a sensation of abdominal fullness and whole abdominal pain for 2 weeks. His body weight decreased by 3 kg over 3 months. He visited his family physician in September 2014 and was referred to our hospital the same day. He had received a colonoscopy and polypectomy 3 years prior. His past medical and family histories were noncontributory. A physical examination revealed a palpable fist-sized, right-lower-quadrant mass accompanied by tenderness. Laboratory tests, including a blood cell count (white blood cells (WBCs): 6300/µL; neutrophils: 70.6%; lymphocytes: 20.6%), electrolytes, liver and renal function and nutritional values, showed no abnormalities. The serum levels of epithelial tumor markers, such as carcinoembryonic antigen (CEA; 1.7 ng/mL) and carbohydrate antigen 19-9 (CA19-9; 0.1 U/mL), and the lymphoma-specific marker soluble interleukin-2 receptor (sIL-2R; 435 U/mL) were within normal limits.
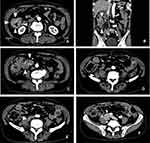
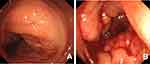
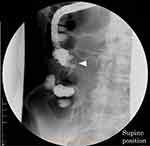
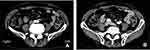
The patient underwent a computed tomography (CT) examination with contrast medium injection, and an extreme circumferential wall thickness in the ascending colon with a contrast effect, measuring 50 × 50 mm in size, was detected in the right abdomen [Figure 1A]. According to the frontal plane of the reconstructed view, the large mass was measured to be 68 × 46 mm [Figure 1B]. Bulky swollen lymph nodes involving ileocolic vessels were detected [Figure 1C]. Swollen lymph nodes were also observed in the retroperitoneal space on the right side of the psoas muscle [Figure 1D], attached to the right side of the inferior vena cava [Figure 1E], and on the right-to-posterior side of the right iliac vein, compressing it [Figure 1F]. Distant metastases (ie, to the liver, lungs or peritoneum) were not found. Colonoscopy did not reveal anything beyond a constriction of the tumor at the ascending colon [Figure 2B]. The observable tumor border was covered by a normal mucous membrane [Figure 2A], and the diagnosis of carcinoma was not made by the biopsy specimens. We conducted fluoroscopy using gastrografin simultaneously, revealing that the stenosis was irregular, measuring 62 mm in length and accompanied by a niche reflecting an ulceration, which strongly suggested that the tumor consisted of an epithelial neoplasm [Figure 3]. Considering these imaging findings, we made a preoperative diagnosis of stage IV T4N2M1 (lymph nodes) ascending colon cancer.
During the surgery, which was performed in October 2014, liver or peritoneal metastasis was not revealed. The tumor of the ascending colon was fixed to the neighboring swollen lymph nodes. A right hemicolectomy accompanied by lymph node dissection along the superior mesenteric vein was conducted. After excision of the ascending colon tumor, the swollen lymph nodes located at the neighboring psoas muscle were resected; however, the paracaval and parailiac lymph nodes were abandoned.
Pathological Findings
Gross Pathology
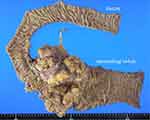
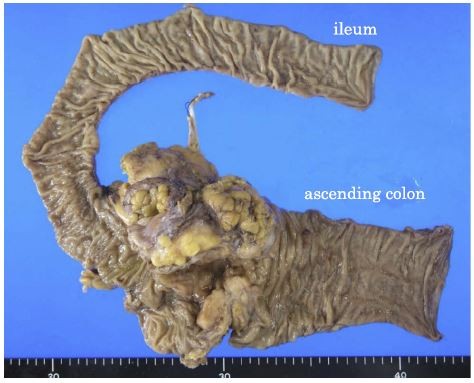
The circumferential ascending colon tumor was cut and opened [Figure 4]. The resected specimen consisted of a polypoid tumor accompanied by ulcer formation, measuring 60 × 40 mm, located at the circumferential wall of the ascending colon.
Microscopy
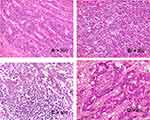
The tumor was comprised of a moderately to poorly (solid type) differentiated adenocarcinoma component [Figure 5A, ×200]. In a portion of the tumor, a poorly differentiated carcinoma component accompanied by remarkable lymphocyte permeation was found [Figure 5B, ×200]. In the component, glandular formation was not observed, and the component was arranged in cords or clusters. The individual tumor cells were large and pleomorphic with abundant eosinophilic cytoplasms, large vesicular nuclei, irregular nuclear profiles and prominent nucleoli; however, the findings of a syncytial growth pattern of undifferentiated malignant epithelial cells and ill-defined borders were obscure [Figure 5C, ×400]. The lymphocytes appeared small, round and mature. There were more infiltrating lymphocytes than tumor cells. The glandular component was accompanied by a fibrous stroma; on the other hand, the stroma was modest in the abundant lymphocyte permeation component. Lymph node metastases were noted in the nodes neighboring the tumor and retroperitoneal lymph nodes; however, metastasis was not observed in the nodes located in the root of the ileocolic artery or along the superior mesenteric vein. Intermediate degrees of lymphatic, venous, and perineural infiltration were also noted. In the metastasized lymph nodes, tumor cells exhibited both poorly and moderately differentiated histologies with gland formation, suggesting that the metastasis originated from the nonlymphocyte-rich component [Figure 5D, ×400].
Microsatellite Instability (MSI) Assay
We performed a MSI assay (BML, Inc., Japan) after obtaining the patient’s consent, and the result was negative.
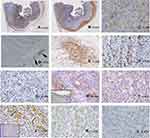
Immunohistochemical staining (details of the antibodies are shown in Table 1): Immunohistochemical staining using an antibody for leukocyte common antigen (LCA; CD45, catalog number: M 0701; Dako, Japan) clearly showed a lymphocyte permeation department with an apparent demarcation line [Figure 6A, loupe]. Additional staining with an α-smooth muscle actin (αSMA, catalog number: M 851, Dako, Japan) antibody clearly showed the muscularis propria. Interestingly, while the glandular component invaded the subserosa, the lymphocyte permeation-rich component invaded the superficial part of the muscularis propria [Figure 6B, loupe]. The tumor-infiltrating lymphocytes were revealed to have CD3-positive T lymphocyte predominance (CD3, catalog number: 413241, Nichirei, Japan) [Figure 6C, ×400]. In addition, mild CLR consisting of CD20-positive lymphocytes was observed in the slightly remote colon wall from a tumor accompanied by lymphoid follicles (CD20, catalog number: NCL-L-CD20-L26, LicaBiosystems, UK) [Figure 6D, ×40 and E, ×100]. The Ki67 labeling index showed a higher value in the nonlymphocyte-rich component (42%) [Figure 6F, ×400] than in the lymphocyte-rich component (22%) [Figure 6G, ×400]. We conducted immunohistochemical staining for PD-L1 (PD-L1, catalog number: ab205921, Abcam Japan), and overexpression was observed in the tumor cells of the nonlymphocyte-rich component, whereas very weak expression was observed in the lymphocyte-rich component [Figure 6H, ×400 and I, ×400; the lower left of Figure 6H shows the positive control using tonsil tissue samples according to the manufacturer’s instructions, ×400]. We also assayed single-stranded DNA (ssDNA, catalog number: 18731, IBL, Japan) to determine the levels of apoptosis, and overexpression was observed in the lymphocyte-rich component [Figure 6J, ×400; the arrows indicate the apoptotic cells; the lower left of Figure 6J is the positive control using tissue from the germinal center of the lymph follicle according to the manufacturer’s instructions, ×400], whereas very weak expression was observed in the nonlymphocyte-rich component [Figure 6K, ×400]. The opposite immunohistochemical results were observed for Ki67.
 |
Table 1 Details of Used Antibodies |
In situ Hybridization
Epstein-Barr virus (EBV)-encoded small RNAs (EBERs) were negative in the tumor cells and positive in a small portion of interstitial lymphocytes (EBER RNA PNA Probe/Fluorescein, catalog number: Y5200, Dako, Japan) [Figure 6L, ×400].
Considering these results, the tumor was diagnosed as T3N2M1 cancer, not medullary carcinoma, with moderately to poorly differentiated carcinoma, PD-L1 overexpression and an LELC histology component inside the tumor.
The patient showed an uneventful recovery, and chemotherapy consisting of mFOLFOX6 was initiated 3 weeks after the operation. Bevacizumab was added to the mFOLFOX6 regimen beginning at the fourth course. After six courses of chemotherapy (three courses with the addition of bevacizumab), the patient underwent follow-up CT, which revealed significantly reduced sizes of the residual lymph nodes. Chemotherapy was continued, and after the patient had an allergic reaction to oxaliplatin in May 2015 (after 14 courses of mFOLFOX6), oxaliplatin was removed from the regimen. In April 2016, after 31 courses of chemotherapy, chemotherapy was discontinued due to prolonged thrombopenia. During this period, increased sizes of the residual lymph nodes were not observed with CT, and the residual lymph nodes ultimately completely disappeared [Figure 7A and B]. The patient was alive without tumor recurrence 5 years after the operation. The changes in the clinical parameters are shown in Figure 8.
 |
Figure 8 Changes in various clinical parameters, including the timing of the operation, the therapeutic chemotherapy agent doses, the lymph node sizes and the platelet count values. |
Discussion
Most carcinomas of the digestive tract are adenocarcinomas, while a small subset shows a solid growth pattern of malignant cells with the appearance of sheets or nests. Such tumors are characterized by abundant tumor-infiltrating lymphocytes and are divided into medullary carcinomas and LELCs. Medullary carcinomas are arranged in syncytial sheets and have well-defined peripheral margins; the preponderance of inflammation is peritumoral and associated with MSI. LELCs do not tend to have continuous sheets of tumors that are broken up by large numbers of intratumoral lymphocytes and are associated with EBV.16
LELC was independently described in 1921 by Regaud and Reverchon17 and Schminke18 as an undifferentiated nasopharyngeal carcinoma (UNPC) characterized by large, polygonal tumor cells with vesicular nuclei and prominent nucleoli. The cytoplasmic borders are often indistinct and result in a syncytial pattern of growth. LELCs in the gastrointestinal tract are mainly seen in the stomach, and gastric carcinomas with a lymphoid stroma constitute approximately 4% of all gastric carcinomas.7 Invariably, there are more infiltrating lymphocytes than tumor cells.19 However, to our knowledge, regarding CRC, only eight cases of LELC have been sporadically reported in the English literature.1–8 Colorectal LELCs as well as LELCs of other organs have been reported to be clinically less aggressive. To date, all colorectal LELCs have been reported to have homogenous histological features. However, it is histologically common that a mixture of different patterns composes a tumor. In gastric cancer cases, the histology has some overlap with gastric carcinoma with lymphoid stroma, and the absence of massive lymphoid infiltrates is sometimes observed either in whole or in part.20 The present case showed a poorly differentiated carcinoma component with remarkable lymphocyte permeation in a portion of the tumor, and the moderately to poorly differentiated adenocarcinoma component was seen on the background of glandular differentiation and sharp demarcation between these components. The lymphocytic component was mainly intratumoral, with a small peritumoral presence. Although the ascending colon cancer was circumferentially large, regarding the lymphocytic component, the tumor invasion remained in the superficial layer of the muscularis propria, while the component with glandular differentiation without lymphocyte permeation reached the subserosal layer. The lymph node metastases exhibited glandular differentiation, suggesting that the metastasis originated from the nonlymphocytic component. Regarding the components with a lymphoid stroma, relatively shallow tumor permeation was maintained and showed relatively weakly aggressive features, as reported for colorectal LELCs. However, lymphocytic permeation was restricted to the poorly differentiated component demarcated from the glandular component. The infiltrated abundant lymphocytes did not show an inhibitory influence on the portion of the cancer without lymphocyte infiltration.
PD-L1 overexpression was observed in the nonlymphocyte permeate component, whereas PD-L1 expression was very weak in the lymphocyte-rich component. A recent systemic review and meta-analysis of colorectal cancer11 revealed that PD-L1 overexpression was related to short OS, short RFS/DFS, a poor tumor stage and the absence of vascular invasion. PD-L1 overexpression in the nonlymphocyte component might play an important role in aggressive locoregional spreading without hematogenous metastasis by avoiding tumor immunity. We also conducted immunohistochemical staining for ssDNA21 in addition to Ki67 to clarify whether PD-L1 was involved in apoptosis or cell proliferation during tumor growth. PD-L1 overexpression in the nonlymphocyte-rich component showed more Ki67 labeling and very weak ssDNA expression. These results suggest that PD-L1 overexpression is more extensively involved in cell proliferation than apoptosis. Immunohistochemistry revealed that infiltrative lymphocytes had a CD3-positive T lymphocyte predominance. The lymphoid reaction in gastric LELCs is reported to be comprised predominantly of T-cells, including numerous T-cell intracytoplasmic antigen (TIA-1)-positive activated cytotoxic lymphocytes and/or natural killer cells in close contact with tumor cells.22 Of nine cases of reported colorectal LELCs, including ours, a lymphocyte surface antigen assay was carried out in five cases; three cases showed T lymphocyte predominance, one case showed the equivalent expression of B and T lymphocytes; and the other case showed B-cell predominance.
The individual tumor cells of the poorly differentiated carcinoma with abundant lymphocyte permeation were large and pleomorphic with abundant eosinophilic cytoplasms, large vesicular nuclei, irregular nuclear profiles and prominent nucleoli; however, the findings of a syncytial growth pattern of undifferentiated malignant epithelial cells and ill-defined borders were obscure and suggested that the tumor was strictly but slightly different from typical UNPC findings. However, some cases of LELC being reported for CRC have shown findings similar to those observed in our case,2,8 and diagnostic criteria regarding CRC may broaden.
Chetty16 reported that gastric medullary carcinoma demonstrates a syncytial growth pattern, bears robust peritumoral inflammation, and has a well-defined border, while lymphoepithelioma-like carcinoma is formed by small clusters of cells that “do not correspond to the syncytial growth patterns seen in medullary carcinoma” and has more prominent intratumoral inflammation and an infiltrative border. Although we diagnosed the LELC of CRC based on pathological findings similar to those of nasopharyngeal LELCs, the diagnostic criteria for LELCs of CRC are not yet clear, and the disease entity has not been established.
In the present case, mild CLR was also observed. The term CLR was coined by Graham and Appelman in 199023 and described as discrete lymphoid aggregates, some with germinal centers, mostly located in the muscularis propria and pericolonic adipose tissue beyond the advancing tumor edge.24 Several cancers of Lynch syndrome were noted to be associated with dense Crohn’s-like lymphoid aggregates; however, our case did not show MSI. In the present case, CLR consisted of CD20-positive B lymphocytes. In the early stages of CLR development, CD4+ T-cells cluster predominantly with mature antigen-presenting dendritic cells. As CLR matures, increasing numbers of B-cells, as well as follicular dendritic cells, are recruited to create lymphoid follicles.24 Our CLR consisted of B-cells and had a mature lymphoid structure with lymphoid follicle development.
CLR has been associated with a low incidence of locoregional recurrence, few distant metastases and prolonged cancer-specific survival and OS.12–15 Although locoregional lymph node metastases were aggressive in our case, no hematogenous metastases or lymph node metastases developed along the root of the main trunk of the feeding vessels, consistent with the reported CLR cases. Regarding immunological features, CLR has been consistently associated with increased tumor intraepithelial and stromal lymphocytic infiltrates, which appears to be independent of the MSI status.14,24 CLR density is also correlated with peripheral immune markers, such as the absolute peripheral lymphocyte count and the lymphocyte to neutrophil ratio, which also carry prognostic significance.15,24,25 In addition, CLR-promoting chemokines are inversely associated with the intratumoral expression of immune checkpoint molecules, including PD-1, PD-L1 and cytotoxic T-lymphocyte-associated protein 4 (CTLA-4).24,26 CLR is reported to be predictive of the chemotherapy response in the context of metastatic CRC, suggesting a potential synergistic effect of cytotoxic chemotherapy with the adaptive immune response to metastatic disease.24,27,28 Prominent CLR can be found in over 30% of CRC cases.16,29 Although our case presented a relatively mild appearance of CLR, it might have influenced complete remission with chemotherapy after noncurative excision. It did not show an elevation in the absolute peripheral lymphocyte count (1300/µL) or the lymphocyte to neutrophil ratio (29.2%); however, these immunologic indexes are thought to be independent of CLR. CRC with a lymphoid stroma can be divided into cases associated with EBV, MSI, or neither, as well as gastric cancer with a lymphoid stroma. Among the eight reported cases of colorectal LELC, the MSI status was investigated in only one case,7 and the result was high MSI. Our case presented no association with EBV infection or MSI. Generally, poorly differentiated carcinomas that are not related to EBV or MSI have a worse prognosis than related cases. This case interestingly presented both the advantages of the LELC phenotype and CLR and the disadvantages of PD-L1 overexpression and no relation between LELC and EBV or MSI for prognosis. It remains unclear what decisively contributed to the preferable outcome. It seems that these characteristics contribute to a conflicting aggressive locoregional extent and a complicated complete response to chemotherapy. Even if the LELC of CRC is not related to EBV or MSI, it is thought to be capable of a good response to chemotherapy and to have a good prognosis in cases of CLR. The accumulation and analyses of further cases are necessary.
Conclusion
We reported a very rare and interesting case of moderately differentiated, PD-L1-overexpressing ascending colon cancer with an LELC component accompanied by CLR presenting with extremely aggressive locoregional spreading and complete remission with chemotherapy after noncurative excision. Even if the LELC of CRC is not related to EBV or MSI and PD-L1 overexpression is found, a good response to chemotherapy and a good prognosis is achievable in cases of CLR. Further accumulation and analyses of cases of colorectal LELCs are necessary.
Abbreviations
PD-L1, programmed death ligand-1; LELC, lymphoepithelioma-like carcinoma; CRC, colorectal cancer; PD-1, programmed death 1; OS, overall survival; RFS, recurrence-free survival; DFS, disease-free survival; CLR, Crohn’s-like lymphoid reaction; WBC, white blood cell; CEA, carcinoembryonic antigen; CA19-9, carbohydrate antigen 19-9; sIL-2R, soluble interleukin-2 receptor; CT, computed tomography; LCA, leukocyte common antigen; CD45, cluster of differentiation 45; αSMA, α-smooth muscle actin; CD3, cluster of differentiation 3; CD20, cluster of differentiation 20; ssDNA, single-stranded deoxyribonucleic acid; EBV, Epstein-Barr virus; EBER, EBV-encoded small RNAs; MSI, microsatellite instability; UNPC, undifferentiated nasopharyngeal carcinoma; TIA-1, T-cell intracytoplasmic antigen; CTLA-4, cytotoxic T-lymphocyte-associated protein 4.
Ethics Approval and Consent to Participate
All procedures used in this research were approved by the Ethical Committee of the National Hospital Organization Tsuruga Medical Center.
Consent for Publication
Written informed consent was obtained from the patient for the publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Data Sharing Statement
All data generated or analyzed during this study are included in this published article.
Acknowledgment
The authors would like to sincerely thank Sarah Conte, Thomas Barbour and Kimberly Yasutis from American Journal Experts (AJE) for their English-language proofreading of the manuscript.
Author Contributions
All authors made substantial contributions to the conception and design of the study; the acquisition, analysis or interpretation of the data; and drafting or critical revision of the article for important intellectual content. All authors approved of the final version to be published and agreed to be accountable for all aspects of the work.
Disclosure
The authors have no competing interests to declare for this work.
References
1. Giovanni DP, Robert L, Daniel MQ, Paul RF, Janet UB, Kojo EJ. Lymphoepithelioma-like carcinoma of the colon in a patient with hereditary nonpolyposis colorectal cancer. Arch Pathol Lab Med. 1999;123:720–724.
2. Vilor M, Tsutsumi Y. Localization of Epstein-Barr virus genome in lymphoid cells in poorly differentiated adenocarcinoma with lymphoid stroma. Pathol Int. 1995;45:695–697. doi:10.1111/j.1440-1827.1995.tb03524.x
3. Palazzo JP, Mittal KR. Lymphoepithelioma-like carcinoma of the rectum in a patient with ulcerative colitis. Am J Gastroenterol. 1996;91:398–399.
4. Samaha S, Tawfik O, Horvat R, Bhatia P. Lymphoepithelioma-like carcinoma of the colon: report of a case with histologic, immunohistochemical, and molecular studies for Epstein-Barr virus. Dis Colon Rectum. 1998;41:925–928. doi:10.1007/BF02235379
5. Kon S, Kasai K, Tsuzuki N, et al. Lymphoepithelioma-like carcinoma of rectum: possible relation with EBV. Pathol Res Pract. 2001;197:577–582. doi:10.1078/0344-0338-00130
6. Kojima Y, Mogaki M, Takagawa R, et al. A case of lymphoepithelioma-like carcinoma of the colon with ulcerative colitis. J Gastroenterol. 2007;42:181–185. doi:10.1007/s00535-006-1981-0
7. Delaney D, Chetty R. Lymphoepithelioma-like carcinoma of the colon. Int J Clin Exp Pathol. 2012;5:105–109.
8. Mori Y, Akagi K, Yano M, et al. Lymphoepithelioma-like carcinoma of the colon. Case Rep Gastroenterol. 2013;7:127–133. doi:10.1159/000348765
9. Watanabe H, Enjoji M, Imai T. Gastric carcinoma with lymphoid stroma. Its morphologic characteristics and prognostic correlations. Cancer. 1976;38:232–243. doi:10.1002/(ISSN)1097-0142
10. Nacopoulou L, Aaris P, Papacharalampous N, et al. Prognostic significance of histologic host response in cancer of the large intestine. Cancer. 1981;47:930–936. doi:10.1002/1097-0142(19810301)47:5<930::AID-CNCR2820470519>3.0.CO;2-1
11. Yang L, Xue R, Pan C. Prognostic and clinicopathological value of PD-L1 in colorectal cancer: a systematic review and meta-analysis. Onco Targets Ther. 2019;12:3671–3682. doi:10.2147/OTT.S190168
12. Buckowitz A, Knaebel HP, Benner A, et al. Microsatellite instability in colorectal cancer is associated with local lymphocyte infiltration and low frequency of distant metastases. Br J Cancer. 2005;92:1746–1753. doi:10.1038/sj.bjc.6602534
13. Ueno H, Hashiguchi Y, Shimazaki H, et al. Objective criteria for Crohn-like lymphoid reaction in colorectal cancer. Am J Clin Pathol. 2013;139:434–441. doi:10.1309/AJCPWHUEFTGBWKE4
14. Rozek LS, Schmit SL, Greenson JK, et al. Tumor-infiltrating lymphocytes, Crohn’s-like lymphoid reaction, and survival from colorectal cancer. J Natl Cancer Inst. 2016;12:108.
15. Posch F, Silina K, Leibl S, et al. Maturation of tertiary lymphoid structures and recurrence of stage II and III colorectal cancer. Oncoimmunology. 2018;7:e1378844. doi:10.1080/2162402X.2017.1378844
16. Chetty R. Gastrointestinal cancers accompanied by a dense lymphoid component: an overview with special reference to gastric and colonic medullary and lymphoepithelioma-like carcinomas. J Clin Pathol. 2012;65:1062–1065. doi:10.1136/jclinpath-2012-201067
17. Regaud C, Reverchon L. Sur un cas d’epitheliome epidermoide developpe dams les massif maxillaire superieur. Rev Laryngol Otol Rhinol. 1921;42:369–378.
18. Schminke A. Uber lympho-epitheliale Geschwulste. Beitr Pathol Anat Allg Pathol. 1921;68:161–170.
19. Cho HJ, Kim JY, Yoo J, Lee SS. Gastric carcinoma with lymphoid stroma: incidence of EBV and Helicobacter pylori infection. Appl Immunohistochem Mol Morphol. 2003;11:149–152. doi:10.1097/00129039-200306000-00010
20. Matsuda I, Kan K, Doi S, Motoki Y, Onodera M, Hirota S. A case of gastric cancer with heterogenous components of EB virus (+)/TP53 (+) and EB virus (-)/TP53 (-). Int J Clin Exp Pathol. 2015;8:11766–11771.
21. Watanabe I, Toyoda M, Okuda J, et al. Detection of apoptotic cells in human colorectal cancer by two different in situ methods: antibody against single-stranded DNA and terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end-labeling (TUNEL) methods. Jpn J Cancer Res. 1999;90:188–193. doi:10.1111/cas.1999.90.issue-2
22. Chapel F, Fabiani B, Davi F, et al. Epstein-Barr virus and gastric carcinoma in Western patients: comparison of pathological parameters and p53 expression in EBV-positive and negative tumours. Histopathology. 2000;36:252–261. doi:10.1046/j.1365-2559.2000.00843.x
23. Graham DM, Appelman HD. Crohn’s-like lymphoid reaction and colorectal carcinoma: a potential histologic prognosticator. Mod Pathol. 1990;3:332–335.
24. Maoz A, Dennis M, Greenson JK. The Crohn’s-like lymphoid reaction to colorectal cancer-tertiary lymphoid structures with immunologic and potentially therapeutic relevance in colorectal cancer. Front Immunol. 2019;10:1884. doi:10.3389/fimmu.2019.01884
25. Sjoquist KM, Renfro LA, Simes RJ, et al. Personalizing survival predictions in advanced colorectal cancer: the ARCAD nomogram project. J Natl Cancer Inst. 2018;110:638–648. doi:10.1093/jnci/djx253
26. Weinstein AM, Giraldo NA, Petitprez F, et al. Association of IL-36 gamma with tertiary lymphoid structures and inflammatory immune infiltrates in human colorectal cancer. Cancer Immunol Immunother. 2019;68:109–120. doi:10.1007/s00262-018-2259-0
27. Halama N, Michel S, Kloor M, et al. The localization and density of immune cells in primary tumors of human metastatic colorectal cancer shows an association with response to chemotherapy. Cancer Immun. 2009;9:1.
28. Halama N, Michel S, Kloor M, et al. Localization and density of immune cells in the invasive margin of human colorectal cancer liver metastases are prognostic for response to chemotherapy. Cancer Res. 2011;71:5670–5677. doi:10.1158/0008-5472.CAN-11-0268
29. Alexander J, Watanabe T, Wu TT, Rashid A, Li S, Hamilton SR. Histopathological identification of colon cancer with microsatellite instability. Am J Pathol. 2001;158:527–535. doi:10.1016/S0002-9440(10)63994-6
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.