Back to Journals » International Medical Case Reports Journal » Volume 9
A rare case of anastomosis between the external and internal jugular veins
Authors Karapantzos I, Zarogoulidis P, Charalampidis C, Karapantzou C, kioumis I, Tsakiridis K, Mpakas A, Sachpekidis N, organtzis J, Porpodis K, Zarogoulidis K, pitsiou G, Zissimopoulos A, Kosmidis C, Fouka E, Demetriou T
Received 21 October 2015
Accepted for publication 7 January 2016
Published 21 March 2016 Volume 2016:9 Pages 73—75
DOI https://doi.org/10.2147/IMCRJ.S98801
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Ronald Prineas

Ilias Karapantzos,1 Paul Zarogoulidis,2 Charalampos Charalampidis,3 Chrysanthi Karapantzou,1 Ioannis Kioumis,2 Kosmas Tsakiridis,4 Andrew Mpakas,4 Nikolaos Sachpekidis,4 John Organtzis,2 Konstantinos Porpodis,2 Konstantinos Zarogoulidis,2 Georgia Pitsiou,2 Athanasios Zissimopoulos,5 Christoforos Kosmidis,6 Evagelia Fouka,2 Theodoros Demetriou3
1Ear, Nose and Throat Department, “Saint Luke” Private Hospital, Panorama, 2Pulmonary Department, “G. Papanikolaou” General Hospital, Aristotle University of Thessaloniki, Thessaloniki, 3Department of Anatomy, Democritus University of Thrace, Alexandroupolis, 4Cardiothoracic Surgery Department, “Saint Luke” Private Hospital, Panorama, Thessaloniki, 5Nuclear Medicine Department, University General Hospital of Alexandroupolis, Democritus University of Thrace, Alexandroupolis, 6Surgery Department, “Interbalkan” European Medical Center, Thessaloniki, Greece
Abstract: Jugular veins bring deoxygenated blood from the head back to the heart. There are two sets of external and internal veins. The external jugular vein receives the greater part of the blood from the cranium and the deep parts of the face. It commences from the substance of the parotid gland and runs down the neck at the posterior border of sternocleidomastoideus and ends in the subclavian vein in front of the scalenus anterior. The external jugular vein is covered by the platysma and its upper half runs parallel with the great auricular nerve. There is also another minor jugular vein, the anterior, draining the submaxillary region. In our patient, we recognized a shunt between the external and internal jugular veins. It appeared in the middle of the veins, between the pair of valves, which are placed ~2.5 cm above the termination of the vessel. The anastomosis was fully functional, and there was no problem in the blood pressure of the patient. Moreover, the shunt was not associated with any systemic disease.
Keywords: jugular veins, anastomosis, parotid gland
Introduction
Jugular veins bring deoxygenated blood from the head back to the heart. There are two sets of external and internal veins. The external jugular vein (EJV) receives the greater part of the blood from the exterior of the cranium and the deep parts of the face. It commences in the substance of the parotid gland and runs down the neck at the posterior border of sternocleidomastoideus. It ends in the subclavian vein in front of the scalenus anterior. It is covered by the platysma and its upper half runs parallel with the great auricular nerve. There is also another minor jugular vein, the anterior, draining the submaxillary region. The internal jugular vein (IJV) is a paired vein collecting the blood from the brain, neck, and the superficial parts of the face. At the base of the brain, the inferior petrosal sinus and the sigmoid sinus join to form the IJV. It begins in the posterior compartment of the jugular foramen. It runs down the side of the neck in a vertical direction and is united with the subclavian vein to form the brachiocephalic vein. It is a little distance from the common carotid artery. The left vein is smaller than the right and each contains a pair of valves, which are placed ~2.5 cm above the termination of the vessel. Parts of the right sternocleidomastoid and platysma have been excised to expose the trunk of the IJV. The EJV is visible through the lower part of the platysma. Near its end, a large branch often descends along the anterior border of sternocleidomastoid to the anterior jugular vein. Its uppermost segment, above its junction with the superior labial vein (vide infra) is often termed as angular vein. Near its beginning, the facial vein connects with the superior ophthalmic vein both directly and via the supraorbital vein; it is thus connected to the cavernous sinus. It receives veins of the ala nasi and, lower, a large deep facial vein from the pterygoid venous plexus. Below the omohyoid, it is covered by the infrahyoid muscles and the sternocleidomastoid muscles and it is crossed by the anterior jugular vein. Deep cervical lymph nodes lie along the vein, mainly on its superficial aspect. At the root of the neck the right IJV is separated from the common carotid, but the left usually overlaps its artery. At the base of the skull the internal carotid artery is anterior, separated from the vein by the ninth to 12th cranial nerves.1–4
Surface anatomy
The IJV is represented in surface projection by a broad band from the ear lobule to the medial end of the clavicle; its inferior bulb is in the interval (depression) between the sternal and clavicular heads of the sternocleidomastoid (ie, the bulb bulges into the lesser supraclavicular fossa; a needle may be inserted here with precision).
Tirbutaries are the inferior petrosal sinus, facial, lingual, pharyngeal, superior, and middle thyroid veins, and sometimes the occipital. They may communicate with the EJV. The thoracic duct opens near the union of the left subclavian and IJVs; the right lymphatic duct is at the same site on the right.
Case report
During root cervical cleaning of a 54-year-old male suffering from supraglottic cancer, we observed a combination of the right EJV with the IJV at the level of the thyroid cartilage. The merger took place through a medium-sized vein, which passes above the thyroid cartilage without folds or other processes. The vein has a length of ~1.5 m. It starts moving from the right EJV, approximately in the middle thereof, and passing through the sternocleidomastoid muscle leads downwardly via the jugular vein. The vein was operated as an extra EJV and drained the blood normally to the IJV. This whole complex is approximately 7.5 million to 1 (Figures 1 and 2).1–4 This case report presentation was approved by the investigational review board of “G. Papanikolaou” General Hospital. Written informed consent was obtained from the patient, in order to proceed with the publication.
  | Figure 1 Anatomic findings during surgery. |
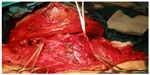  | Figure 2 The ligation of the vessel. |
Discussion
The rarity of this incident was confirmed by the literature. Similar incidents are poorly recorded. This study has clinical value, not only for anatomists and clinicians performing invasive procedures in the region but also for radiologists applying invasive techniques. In addition, a proper study of the head–neck area will help future anatomists to better understand the topography and any variants. Yadav et al reported a case where EJV crossed sternocleidomastoid superficially and ended in IJV.1 Choudhry et al reported a case of anterior facial vein ending as EJV.2 This vein develops from the cephalic vein and anastomoses secondarily with the anterior facial vein. In our case, we recognized a shunt between the EJV and IJV. It appeared in the middle of the veins, between the pair of valves, which are placed ~2.5 cm above the termination of the vessel. The anastomosis was fully functional, with no problem in the blood pressure of the patient, and was not associated with any systemic disease.3,4
Disclosure
The authors report no conflicts of interest in this work.
References
Yadav S, Ghosh SK, Anand C. Variations of superficial veins of head and neck. J Anat Soc India. 2000;49:61–62. | |
Choudhry R, Tuli A, Choudhry S. Facial vein terminating in the external jugular vein. An embryologic interpretation. Surg Radiol Anat. 1997;19:73–77. | |
Hollinshead WH. Anatomy for Surgeons. The Head and Neck. Harper and Row, New York, NY, USA;1998:530. | |
Siegel EL, Caresio J, Eckard DA. Use of the external jugular vein approach for tranasvenous liver biopsy. J Vasc Interv Radiol. 1992;3:371–374. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
