Back to Journals » Clinical Ophthalmology » Volume 10
A novel color-LED corneal topographer to assess astigmatism in pseudophakic eyes
Authors Ferreira T , Ribeiro F
Received 18 May 2016
Accepted for publication 5 July 2016
Published 13 August 2016 Volume 2016:10 Pages 1521—1529
DOI https://doi.org/10.2147/OPTH.S113027
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Tiago B Ferreira, Filomena J Ribeiro
Department of Ophthalmology, Hospital da Luz, Lisbon, Portugal
Purpose: To assess the accuracy of corneal astigmatism evaluation measured by four techniques, Orbscan IIz®, Lenstar LS900®, Cassini®, and Total Cassini (anterior + posterior surface), in pseudophakic eyes.
Patients and methods: A total of 30 patients (46 eyes) who had undergone cataract surgery with the implantation of a monofocal intraocular lens (AcrySof IQ) were assessed after surgery. For each eye, subjective assessment of astigmatism and its axis was performed. Minimum, maximum, and mean keratometry and astigmatism and its axis were evaluated using the four measurement techniques. All measurements were compared with the subjective measurements. Agreement between each measurement technique and subjective assessment was evaluated using Bland–Altman plots. Linear regressions were performed and compared.
Results: Linear regression analysis of astigmatism axis showed very high R2 for all models, with Total Cassini showing the least difference to the unit slope (0.052) and the least difference to a null constant (3.790), although not statistically different from the other models. Regarding astigmatism value, the Cassini and Total Cassini models were similar and statistically better than the Lenstar model. Cassini and Total Cassini showed better J0 compared with Orbscan.
Conclusion: On linear regression models, Cassini and Total Cassini showed the best performance regarding astigmatism value. Cassini and Total Cassini also showed the least J0 deviation from the Cartesian origin compared with Orbscan, which had the lowest performance. Total corneal measurement with the color LED topographer seems to be a better technique for astigmatism assessment.
Keywords: astigmatism, keratometry, topography
Introduction
Cataract surgery is increasingly more demanding and currently aims at emmetropia, with the best uncorrected visual acuity possible. For this goal to be achieved, lower order aberrations (LOAs) must be corrected at the time of surgery, either with a separate surgical procedure or with the use of adequate intraocular lenses (IOLs). In the absence of properly corrected LOAs, any attempt to correct higher order aberrations will be irrelevant.
Astigmatism is a highly prevalent LOA in cataract patients and its prevalence varies only slightly between studies: 64.4% of corneal astigmatism prevalence between 0.25 D and 1.25 D and 22.2% of 1.50 D or higher1 or 63.96% <1.00 D and 27.95% between 1.00 D and 2.00 D.2 In general, it is estimated that up to 40% of patients undergoing cataract surgery have a corneal astigmatism of 1.00 D or more,1,3 and it has been suggested that correction of astigmatism of >0.5 D can improve visual outcomes, whereas correction of astigmatism <0.5 D would have limited visual benefit.4 Therefore, without surgical correction1 of this astigmatic component, it is unlikely that spectacle independence will be achieved, with the consequent personal, social, and economic burden.5
Correct measurements of the cornea are of utmost importance to accurately calculate astigmatism and decide whether to correct it, which may be challenging for small values, and if so, to determine which toric IOL to use for each patient. Although astigmatism does not stem from the cornea alone, as it may also be influenced by the pupil and retinal curvature, corneal measurements are the only preoperative parameters used to calculate IOL cylindrical power.
Cassini® (i-Optics, Den Haag, the Netherlands) is a new technology specifically developed to assess eyes before cataract surgery, which uses LED reflection to evaluate the anterior surface, covering a larger corneal surface and not assuming corneal rotational symmetry. It also evaluates corneal posterior surface using 2nd Purkinje Imaging Technology, a video register with less points than devices based on Scheimpflug imaging, such as the Pentacam (OCULUS Optikgeräte GmbH, Wetzlar, Germany), but with rapid acquisition (20 seconds).
The aim of this work was to assess the accuracy of corneal astigmatism evaluation measured by four techniques, using subjective refraction of pseudophakic eyes as a comparator, and evaluate if total corneal measurement is different from anterior corneal measurement alone.
Patients and methods
Population sample
A total of 30 patients (46 eyes), with an average age of 67.3±7.3 years, 16 women and 14 men, who had undergone cataract surgery with the implantation of a monofocal nontoric IOL (AcrySof IQ; Alcon Laboratories, Inc., Fort Worth, TX, USA), were assessed at least 3 months after surgery. This population sample was chosen in order to assure that the cornea was the only source of astigmatism. All eyes showed a well-centered IOL with no tilt, stable capsular bag, no posterior capsule opacification, and no retinal or corneal pathologies. All corrected distance visual acuities were ≥20/30. Inclusion and exclusion criteria were recommended for cataract surgery. The study protocol was approved by Hospital da Luz Institutional Review Board. All participants provided written informed consent.
Subjective assessment of astigmatism
Subjective assessment of astigmatism and its axis was performed using trial frames at a nominal vertex distance of 12 mm and under best spherical refraction error correction. Given subjective measurements are the true clinical evaluation, which are used as the comparator against all measurements done using the automated topographers.
Automated topographers
Topography data were obtained using Orbscan IIz® (Bausch & Lomb Incorporated, Bridgewater, NJ, USA), Lenstar LS900® (Haag Streit, Koeniz, Switzerland), and Cassini (i-Optics). Minimum, maximum, and mean keratometry and astigmatism and its axis were evaluated. For the Cassini, these values were recorded for the corneal anterior surface and for total corneal astigmatism – total cassini (anterior + posterior surface).
Orbscan IIz is a Placido-based multidimensional system that provides a complete analysis of the corneal surface, evaluating all corneal curvatures. The slit light beams are emitted at an angle of 45° to the eye. Twenty slit light beams from the left and 20 slit light beams from the right side are projected on the cornea. Images are taken from 9,000 points in two time ranges of 0.75 seconds. Keratometry readings by Orbscan are simulated.6
The Lenstar LS 900 uses 32 measuring points arranged in two concentric rings (outer 2.3 mm and inner 1.65 mm) of 16 measuring points each. Each displayed keratometry measurement is a composite of the mean of four measurements, totaling 128 measuring points. With the recommended five scans, the keratometry is therefore calculated on the basis of 640 measuring points. Once the data are captured, the spherical equivalent radius is calculated for each individual measuring point. The keratometric calculation considers the best-fit ellipsoid built by the reflected points to determine the radii of the circumscribed ellipsoid. Results are then expressed in dioptric or millimeter notation.7
Cassini is a topographer that uses multicolor point-to-point (up to 700) ray tracing, combined with 2nd Purkinje Imaging Technology. An image processing algorithm locates feature points in the LED tear film-reflection image and accounts for smearing and deformation in irregular corneas.8 The software used provides a parameter to estimate the quality of the measurement. Only scans with good quality (error <0.2 D) were chosen. Cassini has the advantage, over Placido based systems, of not being affected by the Placido mismatch, given the reconstruction algorithm employs data that assure that there is no mismatch between the source and image points, resulting in an efficient reconstruction even in nonrotationally symmetrical corneal surfaces,9 and over Scheimpflug-based systems, of not having to compensate for motion artifacts, since with Cassini the acquisition is instantaneous.
Calibration of all topographers was performed according to the manufacturers’ instructions.
Measurements
All measurements were taken by experienced technicians. Assessed parameters were astigmatism (D), axis (°), and vectors J0 and J45. Vectors J0 and J45 for the cardinal (0°–180°) and oblique (45°–135°) meridians were calculated using the formulas:
J0 = D × cos(2π × axis/180) and |
J45 = D × sin(2π × axis/180), |
according to Thibos and Horner.10
Statistical analysis
All measurements were compared with the subjective measurements. When comparing axis, 180° was added to or subtracted from the measured axis so that measurement differences between methods were never >90°. For the calculation of centroids, the difference between each method of assessment and the subjective value of vectors J0 and J45 was determined. After Shapiro–Wilk tests of all variables, Spearman ρ coefficients were determined to assess correlations between parameters. The Wilcoxon test was used to compare measurements performed on the same eye. Comparison of J0 and J45 vectors between the four assessment methods was performed using ANOVA with post hoc Sidak. Analysis of agreement between each device and subjective measurement was performed using Bland–Altman plots. The limits of agreement were calculated based on the mean and SD of the difference between each device and the subjective assessment, as mean ±1.96 SD. Linear regressions of the form y = Bx + A were performed and standard errors σ of all parameters were calculated. Regression coefficients, slopes, and intercepts between the different regression models were compared according to Wuensch et al.11 Tests were considered significant at P<0.05 significance level (two-tailed). Data were processed using SPSS 21 software (IBM Corporation, Armonk, NY, USA).
Results
Comparison between assessment methods
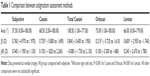
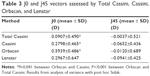
Univariate analysis comparing axis, J0, and J45 assessed by Total Cassini, Cassini, Orbscan, and Lenstar with subjective assessment showed that vector J0 measured by Cassini, Orbscan, and Lenstar was statistically different when compared with that of subjective assessment (Table 1). However, when comparing differences in astigmatism value for patients in whom the difference between axis was ≤|10°|, no method showed differences from subjective assessment (Table 2). Agreement between assessment methods and subjective assessment for J0 and J45 is further illustrated in the Bland–Altman plots (Figure 1).
  | Table 2 Comparison between assessment methods for patients with difference in axis ≤|10°| |
  | Figure 1 Bland–Altman plots for astigmatism axis, J0 and J45. |
Linear regression analysis
Linear regression analysis of axis considering subjective assessment as the independent variable is shown in Figure 2. Linear regression analysis of astigmatism value, for cases in which the difference between axis was ≤|10°|, is shown in Figure 3. For astigmatism axis models, all models showed very high R2 (Orbscan < Total Cassini < Lenstar < Cassini) with Total Cassini showing the least difference to the unit slope (0.052), and the least difference to a null constant (3.790). However, and although the higher R2 in the Total Cassini model points to a best fit, this comparison is observational, since there were no statistical differences between regression coefficients, slopes, or intercepts between models. Regarding astigmatism value, Total Cassini model showed the highest R2 (0.808), although the Cassini model showed the least difference to the unit slope (0.031) and the least difference to a null constant (0.034). Regression coefficients, slopes, and intercepts were not statistically different between the Total Cassini and the Cassini models. However, regression coefficient was lower for the Lenstar model compared with Total Cassini (Z=2.019, df=41, P<0.05), and the Lenstar model slope was also lower compared both with Total Cassini and Cassini (t=3.323, df=44, P<0.002 and t=2.972, df=42, P<0.005, respectively). Orbscan is not shown in Figure 3 because the regression was not statistically significant.
Centroids
Table 3 and Figure 4A–D show the centroids according to all assessment methods. J0 vectors were better for Cassini and Total Cassini compared with Orbscan, with no difference from Lenstar. There were no differences for J45 assessed by the four measurement techniques.
  | Figure 4 Centroids of the difference between each method of assessment and the subjective value of vectors J0 and J45 for (A) Total Cassini, (B) Cassini, (C) Orbscan, and (D) Lenstar. |
Discussion
Increasing demand for improved postoperative visual acuity after cataract surgery makes LOA correction increasingly challenging. Most of the efforts regarding LOAs correction for cataract surgery rely on accuracy of diagnosis, stratification, and correction of astigmatism, as the most prevalent residual postoperative LOA. Although there is a known error associated with the subjective evaluation of astigmatism and a poor correlation with K values,12 this remains the standard for postoperative evaluation and the most important measure of therapeutic success.
There is an ongoing debate on which instrument is more accurate on measuring corneal anterior and posterior surfaces,6,13 if measurement of the anterior corneal surface will suffice, or if the posterior corneal surface should also be directly measured14,15 to improve accuracy. Classically, corneal power calculation is based on anterior corneal surface measurements, assuming a constant and linear relationship between anterior and posterior corneal curvatures16 to estimate posterior corneal curvature and corneal refractive power. However, recent technologies allow direct measurement of posterior corneal curvature, giving a more precise corneal power calculation. Although the exact role of posterior corneal measurement is not clearly established, there has been a tendency to value the posterior corneal surface. Indeed, studies have shown that omission of the posterior corneal surface measurement while calculating the total corneal astigmatism can lead to significant inaccuracies in estimating the magnitude or axis of the total corneal astigmatism in some eyes.14 One large study concluded that the mean magnitude of posterior corneal astigmatism was 0.30 D and that anterior corneal measurements underestimated total corneal astigmatism by a mean of 0.22 D, exceeding 0.50 D in 5% of eyes. Moreover, it is known that ignoring posterior corneal astigmatism results in both hypocorrections and hypercorrections in patients with toric IOLs.15
As a continuing emerging field, different keratometers are available for the diagnosis and stratification of astigmatism. However, previous studies are not consistent regarding the hypothesis that no significant differences exist between keratometers6,17,18 and even small differences between different methods may be of concern.19,20 Given the available data, no recommendation can be given regarding one specific device. However, there are several limitations associated with those comparative studies, namely their retrospective nature and the fact they include healthy volunteers, making it difficult to create specific recommendations based on sound evidence.17 Based on clinical sense and expert opinions, the recommendation is that one should preferably use the device with which one has more experience.17
In the present study, subjective astigmatism was compared with four methods of astigmatism assessment: Orbscan, Lenstar, Cassini, and Total Cassini. Cassini is a new method of evaluation of corneal anterior and total (anterior + posterior) astigmatism. Recently, several studies have demonstrated its high repeatability, in normal corneas17,21–24 and in post-LASIK,21,24 postcataract,25 postkeratoplasty, and postcrosslinking corneas.24
Our results show that astigmatism value and axis assessment by each method tested was not different from subjective assessment. Although not statistically significant, the axis difference between Total Cassini and Cassini may have implications when implanting toric IOLs, given the alignment on the precise axis is crucial. According to linear regression models for astigmatism axis, all models showed high R2, Cassini and Total Cassini methods presented with the highest R2, with Total Cassini showing the least difference to the unit slope (0.052) and the least difference to a null constant (3.790). However, these comparisons are observational, given there were no statistical differences between models regarding regression coefficients, slopes, or intercepts. These data suggest that measuring both the anterior and posterior corneal surface translates into a more accurate measurement, as this model points to a best fit regarding subjective assessment of astigmatism axis. Although not statistically significant, an observational comparison suggests that Orbscan was the method with the lowest value, which may be explained by the fact that the posterior corneal measurement accuracy of Orbscan has not been fully validated.26,27 Also, it has been previously reported that, in eyes after keratorefractive surgery, Orbscan results in inaccurate measurements.28,29
As for astigmatism value, both Cassini and Total Cassini have very high R2 values in linear regression models. Statistically, both these models were comparable, with a better prediction compared with Lenstar, suggesting that these are the best methods when compared with subjective assessment. The Orbscan model was not statistically significant for astigmatism value. Centroid analysis led us to conclude that J0 from Total Cassini and Cassini have the less x deviation from the Cartesian origin when compared with Orbscan, which shows the highest x deviation from the Cartesian origin. J45 values did not differ between assessment methods.
These results confirm the importance of measuring total astigmatism and not just anterior astigmatism. A future work assessing the prediction error of Total Cassini astigmatism measurements in patients with toric IOLs would be interesting and add to these results.
This study has the following limitations. The confounders and bias associated with all observational studies and the number of patients needed to achieve a 90% power to assess differences between very similar measuring instruments with small effect differences; the fact that measurements were taken by two technicians, although they were very experienced and using automatic software; the inherent subjectivity of subjective refraction; and the fact that an initial version of the Cassini software was used, given it is in constant development.
Conclusion
Our study shows that Total Cassini and Cassini have no statistically significant differences when compared with subjective assessment. Cassini and Total Cassini showed a better performance than Lenstar regarding astigmatism value and also a better J0 when compared with Orbscan Total corneal measurement using the color-LED topographer seem to be a better technique for astigmatism assessment.
Acknowledgments
The authors wish to thank Ophtec Portugal for the funding for this study, which was used to access all necessary scientific bibliography. Ophtec Portugal had no role in the study design, collection, analysis and interpretation of data, in the writing of the paper, and in the decision to submit the paper for publication.
Disclosure
The authors report no conflicts of interest in this work and declare they have no commercial, proprietary, or financial conflicts of interest regarding this paper.
References
Ferrer-Blasco T, Montes-Mico R, Peixoto-de-Matos SC, Gonzalez-Meijome JM, Cervino A. Prevalence of corneal astigmatism before cataract surgery. J Cataract Refract Surg. 2009;35(1):70–75. | ||
Hoffmann PC, Hutz WW. Analysis of biometry and prevalence data for corneal astigmatism in 23,239 eyes. J Cataract Refract Surg. 2010;36(9):1479–1485. | ||
Khan MI, Muhtaseb M. Prevalence of corneal astigmatism in patients having routine cataract surgery at a teaching hospital in the United Kingdom. J Cataract Refract Surg. 2011;37(10):1751–1755. | ||
Villegas EA, Alcon E, Artal P. Minimum amount of astigmatism that should be corrected. J Cataract Refract Surg. 2014;40(1):13–19. | ||
Laurendeau C, Lafuma A, Berdeaux G. Modelling lifetime cost consequences of toric compared with standard IOLs in cataract surgery of astigmatic patients in four European countries. J Med Econ. 2009;12(3):230–237. | ||
Hashemi H, Yekta AA, Ostadimoghaddam H, Norouzirad R, Khabazkhoob M. Comparison of keratometric values using javal keratometer, oculus pentacam, and orbscan II. Iran J Ophthalmol. 2014;26(1):3–10. | ||
Instructions for use, Biometer, Lenstar LS 900®, 8th Edition [Biometer instruction manual]: Section 4.3.2. Haag-Streit AG, Koeniz; 2014. | ||
Kanellopoulos AJ, Asimellis G. Forme fruste keratoconus imaging and validation via novel multi-spot reflection topography. Case Rep Ophthalmol. 2013;4(3):199–209. | ||
Sicam VA, VAN der Heijde RG. Topographer reconstruction of the nonrotation-symmetric anterior corneal surface features. Optom Vis Sci. 2006;83(12):910–918. | ||
Thibos LN, Horner D. Power vector analysis of the optical outcome of refractive surgery. J Cataract Refract Surg. 2001;27(1):80–85. | ||
Wuensch KL, Jenkins KW, Poteat M. Misanthropy, idealism and attitudes towards animals. Anthrozoos. 2001;15(2):139–149. | ||
Teus MA, Arruabarrena C, Hernandez-Verdejo JL, Sales-Sanz A, Sales-Sanz M. Correlation between keratometric and refractive astigmatism in pseudophakic eyes. J Cataract Refract Surg. 2010;36(10):1671–1675. | ||
Wang Q, Savini G, Hoffer KJ, et al. A comprehensive assessment of the precision and agreement of anterior corneal power measurements obtained using 8 different devices. PLoS One. 2012;7(9):e45607. | ||
Ho JD, Tsai CY, Liou SW. Accuracy of corneal astigmatism estimation by neglecting the posterior corneal surface measurement. Am J Ophthalmol. 2009;147(5):788–795. | ||
Koch DD, Ali SF, Weikert MP, Shirayama M, Jenkins R, Wang L. Contribution of posterior corneal astigmatism to total corneal astigmatism. J Cataract Refract Surg. 2012;38(12):2080–2087. | ||
Fam HB, Lim KL. Validity of the keratometric index: large population-based study. J Cataract Refract Surg. 2007;33(4):686–691. | ||
Hidalgo IR, Rozema JJ, Dhubhghaill SN, Zakaria N, Koppen C, Tassignon MJ. Repeatability and inter-device agreement for three different methods of keratometry: Placido, Scheimpflug, and color LED corneal topography. J Refract Surg. 2015;31(3):176–181. | ||
Goggin M, Patel I, Billing K, Esterman A. Variation in surgically induced astigmatism estimation due to test-to-test variations in keratometry. J Cataract Refract Surg. 2010;36(10):1792–1793. | ||
Savini G, Barboni P, Carbonelli M, Hoffer KJ. Agreement between Pentacam and videokeratography in corneal power assessment. J Refract Surg. 2009;25(6):534–538. | ||
Savini G, Carbonelli M, Sbreglia A, Barboni P, Deluigi G, Hoffer KJ. Comparison of anterior segment measurements by 3 Scheimpflug tomographers and 1 Placido corneal topographer. J Cataract Refract Surg. 2011;37(9):1679–1685. | ||
Ventura BV, Wang L, Ali SF, Koch DD, Weikert MP. Comparison of corneal power, astigmatism, and wavefront aberration measurements obtained by a point-source color light-emitting diode–based topographer, a Placido-disk topographer, and a combined Placido and dual Scheimpflug device. J Cataract Refract Surg. 2015;41(8):1658–1671. | ||
Kanellopoulos AJ, Asimellis G. Distribution and repeatability of corneal astigmatism measurements (magnitude and axis) evaluated with color light emitting diode reflection topography. Cornea. 2015;34(8):937–944. | ||
Klijn S, Reus NJ, Sicam VA. Evaluation of keratometry with a novel Color-LED corneal topographer. J Refract Surg. 2015;31(4):249–256. | ||
Kanellopoulos AJ, Asimellis G. Color light-emitting diode reflection topography: validation of keratometric repeatability in a large sample of wide cylindrical-range corneas. Clin Ophthalmol. 2015;9:245–252. | ||
Ventura BV, Al-Mohtaseb Z, Wang L, Koch DD, Weikert MP. Repeatability and comparability of corneal power and corneal astigmatism obtained from a point-source color light-emitting diode topographer, a Placido-based corneal topographer, and a low-coherence reflectometer. J Cataract Refract Surg. 2015;41(10):2242–2250. | ||
Seitz B, Torres F, Langenbucher A, Behrens A, Suarez E. Posterior corneal curvature changes after myopic laser in situ keratomileusis. Ophthalmology. 2001;108(4):666–672; discussion 673. | ||
Giessler S, Duncker GI. Orbscan pachymetry after LASIK is not reliable. J Refract Surg. 2001;17(3):385–387. | ||
Cairns G, Ormonde SE, Gray T, et al. Assessing the accuracy of Orbscan II post-LASIK: apparent keratectasia is paradoxically associated with anterior chamber depth reduction in successful procedures. Clin Experiment Ophthalmol. 2005;33(2):147–152. | ||
Ciolino JB, Belin MW. Changes in the posterior cornea after laser in situ keratomileusis and photorefractive keratectomy. J Cataract Refract Surg. 2006;32(9):1426–1431. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.