Back to Journals » Neuropsychiatric Disease and Treatment » Volume 12
A functional MRI study of altered spontaneous brain activity pattern in patients with congenital comitant strabismus using amplitude of low-frequency fluctuation
Authors Tan G, Huang X, Zhang Y, Wu A, Zhong Y, Wu K, Zhou F , Shao Y
Received 22 January 2016
Accepted for publication 8 March 2016
Published 20 May 2016 Volume 2016:12 Pages 1243—1250
DOI https://doi.org/10.2147/NDT.S104756
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Professor Wai Kwong Tang
Gang Tan,1,2,* Xin Huang,1,3,* Ying Zhang,1 An-Hua Wu,2 Yu-Lin Zhong,1 Kai Wu,2 Fu-Qing Zhou,4 Yi Shao1
1Department of Ophthalmology, The First Affiliated Hospital of Nanchang University, Jiangxi Province Clinical Ophthalmology Institute and Oculopathy Research Centre, Nanchang, Jiangxi, 2Department of Ophthalmology, The First Affiliated Hospital of University of South China, Hengyang, Hunan, 3Department of Ophthalmology, The First People’s Hospital of Jiujiang City, Jiujiang, 4Department of Radiology, The First Affiliated Hospital of Nanchang University, Jiangxi Province Medical Imaging Research Institute, Nanchang, Jiangxi, People’s Republic of China
*These authors contributed equally to this work
Objective: The aim of this study was to use amplitude of low-frequency fluctuation (ALFF) to investigate local features of spontaneous brain activity in patients with congenital comitant strabismus and clarify their relationship with emotional and psychosocial problems.
Methods: A total of 20 patients with congenital comitant strabismus (ten males and ten females), and 20 healthy controls (ten males and ten females) closely matched in age, sex, and education underwent resting-state functional magnetic resonance imaging scans. The ALFF method was used to assess local features of spontaneous brain activity. Congenital comitant strabismus patients were distinguished from healthy controls by receiver operating characteristic curve. Correlation analysis was performed to explore the relationships between the observed mean ALFF signal values of the different areas and the Chinese version of the Hospital Anxiety and Depression Scale.
Results: Compared with healthy controls, patients with congenital comitant strabismus had significantly lower ALFF in the bilateral medialfrontal gyrus and higher values in the bilateral cerebellum posterior lobe and left angular gyrus. In the congenital comitant strabismus group, the Hospital Anxiety and Depression Scale-depression score showed a negative correlation with the ALFF signal values of the bilateral medial frontal gyrus (r=-0.550, P=0.012) and a negative correlation was noted between the mean ALFF signal values of the left angular gyrus and strabismus duration (r=-0.515, P=0.020).
Conclusion: Congenital comitant strabismus mainly involves dysfunction in the bilateral medial frontal gyrus, bilateral cerebellum posterior lobe, and left angular gyrus, which may reflect the underlying pathologic mechanism of congenital strabismus.
Keywords: ALFF, congenital comitant strabismus, resting state, spontaneous activity, anxiety and depression
Introduction
Strabismus is a common eye disease with monocular or binocular abnormal position. The incidence rate of adult-onset strabismus in Olmsted County, MN, USA, was 54.1 cases per 100,000 individuals.1 Strabismus often leads to compromised binocular vision and amblyopia. Clinically, strabismus also presents with stereopsis impairment. In addition to functional limitations (restriction in visual field and stereopsis), strabismic patients may suffer from significant psychosocial problems.2 It was worthy of attention that the strabismus had posed great pressures on patients in all age groups.3
Neuronal activity within the oculomotor nucleus could drive abnormal cross-axis eye movements. The frontal eye field (FEF) is an area of the frontal cortex that can trigger eye movements.4 In humans, gaze control systems also include the supplementary eye field, presupplementary eye field, dorsolateral prefrontal cortex, cingulate eye field within the anterior cingulate cortex, and dorsomedial frontal cortex. The FEF is involved in executing saccadic and smooth pursuit eye movements.5
Previous studies demonstrated that there were many psychiatric problems in patients with strabismus.6,7 The frontal gyrus played an important role in emotion.8 A previous study proved severely depressed patients with cortical thickening in left frontal brain regions compared favourably with healthy control (HCs).9 Moreover, the patients with depression showed enhanced default mode network connectivity with ventral striatum.10 The anxiety disorder also leads to the dysfunction of brain function. The patients with social anxiety disorder might have an insular volume reduction.11
Magnetic resonance imaging (MRI) has been used to study strabismus. A previous report described reduced gray matter volume in the occipital eye field and parietal eye field and increased gray matter volume in FEF of adults with strabismus.12 Another group demonstrated reduced functional connections in the V1 and V2 areas of macaque monkeys with strabismic amblyopia.13 Another study showed increased mean diffusivity in the occipital tracts of patients with strabismic amblyopia.14 Although these findings have revealed morphological changes in the neurons of subjects with strabismus, there is far less evidence for neuromechanical changes.
Resting state functional MRI (fMRI) is a functional brain imaging technique that is increasingly used to evaluate spontaneous brain activity in subjects at rest.15 Amplitude of low-frequency fluctuation (ALFF) is a resting state-fMRI analysis technique used to measure spontaneous fluctuations in blood-oxygen level-dependent signal, which reflects regional spontaneous brain activity at rest. ALFF has been used to investigate neurological conditions, including optic neuritis,16 glaucoma,17 and Parkinson’s disease.18 The current study is the first, to our knowledge, to evaluate spontaneous brain activity in subjects with congenital comitant strabismus and its relationship with behavioral measures.
Materials and methods
Subjects
A total of 20 patients with congenital comitant strabismus (ten males and ten females, five esotropia and 15 exotropia) were recruited from the First Affiliated Hospital of South China University and the Ophthalmology Department of the First Affiliated Hospital of Nanchang University Hospital. The diagnostic criteria of congenital comitant strabismus were: 1) strabismus from birth; 2) stereo vision defects (no visual fusion); 3) binocular corrected visual acuity (VA) is equal; and 4) with alternated cover, the experimental and strabismus angle were equal, and the large squint angle range was 34±9.12 triple prism degree. Subjects were excluded if they met any one of the following criteria: 1) acquired strabismus, incomitant strabismus, and concealed oblique; 2) condition due to eye disease (infection, inflammation, and ischemic disease); 3) patients with eye surgery (outside the eye surgery and intraocular surgery); 4) psychiatric disorders (obsessive compulsive disorder, anxiety disorder, schizophrenia, depression, etc), diabetes, cardiovascular disease, and cerebral infarction disease; and 5) addiction (eg, drugs or alcohol).
Twenty HCs (ten males and ten females) who were age-, sex-, and education status-matched to subjects in the strabismus group were also recruited for this study. The HCs were recruited from healthy volunteers of Nanchang in Jiangxi province. All HCs met the following criteria: 1) no abnormalities in the brain parenchyma on cranial MRI; 2) no ocular disease with uncorrected or corrected VA >1.0; 3) no psychiatric disease (obsessive compulsive disorder, anxiety disorder, schizophrenia, depression, etc); and 4) able to undergo MRI (eg, no cardiac pacemaker or implanted metal devices). This study was authorized by the First Affiliated Hospital of Nanchang hospital’s ethics committee. All research methods followed the Declaration of Helsinki and conformed to the principles of medical ethics. All volunteers participated voluntarily and were informed of the purposes, methods, and potential risks before signing an informed consent.
MRI parameters
MRI scanning was performed on a 3-Tesla MR scanner (Trio, Siemens, Munich, Germany). All the participants were required to keep awake and maintain quiet breathing until the end of the scan. Structural data and functional data were acquired with a 3D spoiled gradient-recalled echo sequence with the following parameters: 176 structural images (repetition time =1,900 ms, echo time =2.26 ms, thickness =1.0 mm, gap =0.5 mm, acquisition matrix =256×256, field of view =250×250 mm, flip angle =9°). We also obtained 240 functional images (repetition time =2,000 ms, echo time =30 ms, thickness =4.0 mm, gap =1.2 mm, acquisition matrix =64×64, flip angle =90°, field of view =220×220 mm, 29 axial). The duration of scan time was 15 minutes.
fMRI data analysis
Functional data were classified by MRIcro software (www.MRIcro.com) to eliminate incomplete data. The first ten volumes were discarded due to magnetization equilibration. The rest of the data preprocessing was performed by DPARSFA (http://rfmri.org/DPARSF) software, including Digital Imaging Communications in Medicine form transformation, slice timing, head-motion correction, spatial normalization, and smooth with a Gaussian kernel of 6×6×6 mm3 full-width at half-maximum. The subjects who had more than 1.5 mm maximum shift in x, y, or z and 1.5 of angular motion would be dismissed. The Friston six head-motion parameters were used to regress out head-motion effects based on recent work showing that higher-order models were more effective in removing head-motion effects.19,20 Linear regression was also applied to remove other sources of false variables, which contain the signal from the ventricular system and a region centered in the brain white matter.21 After head-motion correction, the functional images were spatially normalized to the Montreal Neurological Institute space using the standard echoplanar image template. The details of ALFF calculation can be referred to a previous study.22 To reduce the global effects of variability across the participants, the ALFF of each voxel was divided by the global mean ALFF value for each participant.
A general linear model analysis
A general linear model analysis was performed with the SPM8 toolkit to investigate the ALFF signal group differences in resting state between patients with strabismus and HCs, after controlling for the effects of age and sex. The significance level was set at P<0.05, Gaussian random field theory corrected, minimum z>2.3.
Brain-behavior linear correlation analyses
Brain areas with different ALFF findings between groups were classified as regions of interest with REST software. For each region of interest, the mean ALFF value was extracted by averaging the ALFF value over all voxels. Linear correlation analysis was performed to investigate the relationship between the mean ALFF value in each area in the strabismus group and behavioral performances. P<0.05 was considered statistically significant.
Independent t-tests on clinical data analysis
Our previous study reported that the Chinese version of the Hospital Anxiety and Depression Scale (HADS) scores were higher in child strabismus patients compared with HCs.23 The HADS has been widely used to evaluate patients’ mental state in many diseases.24,25 It includes seven anxiety and seven depressive symptom items and has demonstrated good reliability. Our patient questionnaire scores were obtained. The maximum anxiety and depression scores are both 21. A subject is with significant depression if his or her score is ≥8, and significant anxiety if his or her score is ≥11. The clinical data of the comitant strabismus patients were collected, including the course of the disease and best-corrected VA. Two-sample Student’s t-test was used for clinical measures between strabismus group and HCs. All the statistical analysis was done with the IBM SPSS version 20.0 statistical software (IBM Corporation, Armonk, NY, USA).
Results
Demographics and visual measurements
The mean ± standard deviation of age for strabismus group and HCs were 26.95±9.05 (years) and 27.45±8.99 years. The scores of HADS-anxiety and HADS-depression were 7.55±1.54 and 9.20±1.36 for strabismus group. The average weight for strabismus group and HCs was 59.00±8.28 (kg) and 58.75±6.37 (kg). There were no obvious differences in weight (P=0.915), age (P=0.862), best-corrected VA-Right (P=0.351) and best-corrected VA-Left (P=0.540) between the two groups (Table 1).
ALFF differences
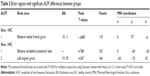
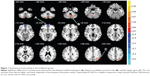
Compared with HCs, strabismus patients had significantly decreased ALFF values in the bilateral medial frontal gyrus (Figure 1 [blue] and Table 2). The brain areas with significantly increased ALFF values in the strabismus group were the bilateral cerebellum posterior lobe and left angular gyrus (Figure 1 [red] and Table 2). The mean values of altered ALFF between the strabismus and HC groups are shown in Figure 2.
Correlation analyses
In the strabismus group, the mean HADS-depression score was negatively correlated with the ALFF signal values of the bilateral medial frontal gyrus (r=−0.550, P=0.012; Figure 3A). Duration of strabismus was negatively correlated with the ALFF signal values of the left angular gyrus (r=−0.515, P=0.020; Figure 3B).
Receiver operating characteristic curve
We considered that ALFF differences between the strabismus and HC groups might be useful diagnostic markers. To test this possibility, the mean ALFF values of the different brain regions were extracted and used to analyze receiver operating characteristic curves. The values for the areas under the curves of the bilateral medial frontal gyrus were 0.915 (Figure 4).
Discussion
To our knowledge, this is the first study to evaluate the effect of strabismus on resting-state brain activity using the ALFF technique. Compared with HCs, subjects with strabismus had significant ALFF value changes in many brain regions. Furthermore, the HADS-depression score in strabismus patients was negatively correlated with the ALFF signal values of the bilateral medial frontal gyrus (r=−0.550, P=0.012) and there was a negative correlation between the mean ALFF signal values of the left angular gyrus and strabismus duration (r=−0.515, P=0.020).
Both the FEF in the prefrontal cortex and the superior colliculus are implicated in strabismus.26 The location of the FEF is proposed to be within a larger oculomotor region in the posterior part of the middle frontal gyrus.27 A previous study demonstrated that FEF played an important role in saccade selection and execution.28 It was also involved in sustained attention.29 Yan et al30 reported reduced white matter volumes in the right frontal lobe/subgyral areas of patients with comitant exotropia. In support of these findings, we also found that patients with strabismus had lower ALFF values in the bilateral medial frontal gyrus. The decreased ALFF values in these regions may reflect FEF functional damage in patients with strabismus. Furthermore, the ALFF signal values of the bilateral medial frontal gyrus were negatively correlated with the HADS-depression score in the strabismus group. Previous studies had demonstrated that frontal gyrus dysfunction was related to depression.31,32 A previous study found that there were lesions in the medial orbital frontal region in depressed patients.33 Meanwhile, many studies have demonstrated that the patients with strabismus often accompanied with psychological abnormality of depressive symptoms.34,35 We therefore hypothesized that strabismus may be related to medial frontal gyrus dysfunction, which may give an explanation to depression in patients with strabismus. The mean and standard deviation HADS-anxiety in strabismus patient was 7.55±1.54, which reflected strabismus patients accompanied by feelings of anxiety. However, we did not find a relationship between the HADS-anxiety scores and ALFF signal values of different regions.
The cerebellum is involved in balance and motor control as well as the execution of accurate eye movements.36 One group reported that the cerebellum is involved in the execution of eye and hand movements.37 A previous study showed that cerebellar vermis activation is related to visually guided saccades.38 Joshi and Das39 found that the function of posterior interposed nucleus in the cerebellum played an important role in conjugate eye movements in strabismic monkeys. In support of these findings, we also observed higher ALFF values in the bilateral cerebellum posterior lobe in strabismus, which may reflect functional reorganization to compensate for conjugate eye movement abnormalities.
The angular gyrus occupies a posterior part of the inferior parietal lobule corresponding to Brodmann area 39,40 which is one of the major connecting hubs of the brain.41 The parietal and occipital lobes were involved in gaze, movement, and body guidance.42 Yang et al43 showed that the left cingulate gyrus, bilateral precuneus, and left angular gyrus visual cortex may compensate for fusion dysfunction in infantile esotropia. In our study, we found higher ALFF values in the left angular gyrus, which may reflect a compensation for visual fusion dysfunction in patients with strabismus. The higher ALFF values indicated the compensatory function of the region. Furthermore, we found a negative correlation between the mean ALFF value of the left angular gyrus and strabismus duration. That is to say, the shorter the duration of strabismus, the higher the ALFF values in the left angular gyrus. We therefore concluded that the compensation of function in the left angular gyrus may relate to the duration of strabismus.
Conclusion
In summary, our results showed that strabismus was characterized by abnormal spontaneous activities in various brain regions. These findings provided important information that clarifies the underlying neural mechanisms of strabismus. The correlation analyses suggested that changes in these areas could be related to the incidence of depression in the strabismus group.
Prospects and problems
The rapid development of fMRI technology has facilitated its wide use in many fields of neurologic diseases, including strabismus. ALFF is a useful measurement because it can accurately reflect whole-brain activity. Future research should be performed to clarify the brain regions involved in strabismus and possibly develop new treatments. The present study also had several limitations. Firstly, the sample size was small; future research should expand the size for more accurate results. Second, the clinical characteristics were not strict; we included both exo- and esotropic patients. Future research should distinguish between different types of strabismus to more accurately assess brain function activity changes. It would also be important to streamline the scanning protocol. For some subjects, the scan time was too long, and body movement can affect ALFF findings. Despite these shortcomings, the present study of congenital comitant strabismus revealed that dysfunction in specific brain areas underlies the pathogenesis of congenital comitant strabismus.
Acknowledgments
This study was supported by the National Natural Science Foundation of China (81160118, 81100648, and 81400372); Jiangxi Province Voyage Project (2014022); Jiangxi province Degree and Postgraduate Education Reform Project (2015); Science and Technology Platform Construction Project of Jiangxi Province (2013116); Youth Science Foundation of Jiangxi Province (20151BAB215016); Technology and Science Foundation of Jiangxi Province (20151BBG70223); Hunan Province Education Department Outstanding Youth Science Foundation (GJJ14170); Health Development Planning Commission Science Foundation of Jiangxi Province (20155154); and Scholor Project of Ganjiang River (2015). This was not an industry supported study.
Disclosure
The authors report no conflicts of interest in this work.
References
Martinez-Thompson JM, Diehl NN, Holmes JM, Mohney BG. Incidence, types, and lifetime risk of adult-onset strabismus. Ophthalmology. 2014;121(4):877–882. | ||
Uretmen O, Egrilmez S, Kose S, Pamukçu K, Akkin C, Palamar M. Negative social bias against children with strabismus. Acta Ophthalmol Scand. 2003;81:138–142. | ||
Archer SM, Musch DC, Wren PA, Guire KE, Del Monte MA. Social and emotional impact of strabismus surgery on quality of life in children. J AAPOS. 2005;9(2):148–151. | ||
Vernet M, Quentin R, Chanes L, Mitsumasu A, Valero-Cabré A. Frontal eye field, where art thou? Anatomy, function, and non-invasive manipulation of frontal regions involved in eye movements and associated cognitive operations. Front Integr Neurosci. 2014;8:66. | ||
Tehovnik EJ, Sommer MA, Chou IH, Slocum WM, Schiller PH. Eye fields in the frontal lobes of primates. Brain Res Brain Res Rev. 2000;32(2–3):413–448. | ||
Cumurcu T, Cumurcu BE, Ozcan O, et al. Social phobia and other psychiatric problems in children with strabismus. Can J Ophthalmol. 2011;46(3):267–270. | ||
Alpak G, Coskun E, Erbagci I, et al. Effects of corrective surgery on social phobia, psychological distress, disease-related disability and quality of life in adult strabismus patients. Br J Ophthalmol. 2014;98(7):876–879. | ||
Grecucci A, Giorgetta C, Bonini N, Sanfey AG. Reappraising social emotions: the role of inferior frontal gyrus, temporo-parietal junction and insula in interpersonal emotion regulation. Front Hum Neurosci. 2013;7:523. | ||
Fonseka BA, Jaworska N, Courtright A, MacMaster FP, MacQueen GM. Cortical thickness and emotion processing in young adults with mild to moderate depression: a preliminary study. BMC Psychiatry. 2016;16:38. | ||
Hwang JW, Xin SC, Ou YM, et al. Enhanced default mode network connectivity with ventral striatum in subthreshold depression individuals. J Psychiatr Res. 2016;76:111–120. | ||
Kawaguchi A, Nemoto K, Nakaaki S, et al. Insular volume reduction in patients with social anxiety disorder. Front Psychiatry. 2016;7:3. | ||
Chan ST, Tang KW, Lam KC, Chan LK, Mendola JD, Kwong KK. Neuroanatomy of adult strabismus: a voxel-based morphometric analysis of magnetic resonance structural scans. Neuroimage. 2004;22(2):986–994. | ||
Bi H, Zhang B, Tao X, et al. Neuronal responses in visual area V2 (V2) of macaque monkeys with strabismic amblyopia. Cereb Cortex. 2011;21(9):2033–2045. | ||
Duan Y, Norcia AM, Yeatman JD, Mezer A. The structural properties of major white matter tracts in strabismic amblyopia. Invest Ophthalmol Vis Sci. 2015;56(9):5152–5160. | ||
Biswal BB. Resting state fMRI: A personal history. Neuroimage. 2012;62(2):938–944. | ||
Huang X, Cai FQ, Hu PH, et al. Disturbed spontaneous brain-activity pattern in patients with optic neuritis using amplitude of low-frequency fluctuation: a functional magnetic resonance imaging study. Neuropsychiatr Dis Treat. 2015;11:3075–3083. | ||
Huang X, Zhong YL, Zeng XJ, et al. Disturbed spontaneous brain activity pattern in patients with primary angle-closure glaucoma using amplitude of low-frequency fluctuation: a fMRI study. Neuropsychiatr Dis Treat. 2015;11:1877–1883. | ||
Kwak Y, Peltier SJ, Bohnen NI, Müller ML, Dayalu P, Seidler RD. L-DOPA changes spontaneous low-frequency BOLD signal oscillations in Parkinson’s disease: a resting state fMRI study. Front Syst Neurosci. 2012;4(6):52. | ||
Li H-J, Dai X-J, Gong H-H, Nie X, Zhang W, Peng DC. Aberrant spontaneous low-frequency brain activity in male patients with severe obstructive sleep apnea revealed by resting-state functional MRI. Neuropsychiatr Dis Treat. 2015;11:207–214. | ||
Satterthwaite TD, Elliott MA, Gerraty RT, et al. An improved framework for confound regression and filtering for control of motion artifact in the preprocessing of resting-state functional connectivity data. Neuroimage. 2013;64:10. | ||
Yan CG, Cheung B, Kelly C, et al. A comprehensive assessment of regional variation in the impact of head micromovements on functional connectomics. Neuroimage. 2013;76:183–201. | ||
Zang YF, He Y, Zhu CZ, et al. Altered baseline brain activity in children with ADHD revealed by resting-state functional MRI. Brain Dev. 2007;29(2):83–91. | ||
Chai Y, Shao Y, Lin S, et al. Vision-related quality of life and emotional impact in children with strabismus: a prospective study. J Int Med Res. 2009;37(4):1108–1114. | ||
van Eeden M, Kootker JA, Evers SM, van Heugten CM, Geurts AC, van Mastrigt GA. An economic evaluation of an augmented cognitive behavioural intervention vs. computerized cognitive training for post-stroke depressive symptoms. BMC Neurol. 2015;15(1):266. | ||
Liyue H, Chiang PP, Sung SC, Tong L. Dry eye-related visual blurring and irritative symptoms and their association with depression and anxiety in eye clinic patients. Curr Eye Res. 2015;4:1–10. | ||
Hanes DP, Wurtz RH. Interaction of the frontal eye field and superior colliculus for saccade generation. J Neurophysiol. 2001;85(2):804–815. | ||
Blanke O, Spinelli L, Thut G, et al. Location of the human frontal eye field as defined by electrical cortical stimulation: anatomical, functional and electrophysiological characteristics. Neuroreport. 2000;11(9):1907–1913. | ||
Fernandes HL, Stevenson IH, Phillips AN, Kording KP. Saliency and saccade encoding in the frontal eye field during natural scene search. Cereb Cortex. 2014;24(12):3232–3245. | ||
Esterman M, Liu G, Okabe H, Reagan A, Thai M, DeGutis J. Frontal eye field involvement in sustaining visual attention: evidence from transcranial magnetic stimulation. Neuroimage. 2015;111:542–548. | ||
Yan X, Lin X, Wang Q, et al. Dorsal visual pathway changes in patients with comitant extropia. PLoS One. 2010;5(6):e10931. | ||
Kerestes R, Ladouceur CD, Meda S, et al. Abnormal prefrontal activity subserving attentional control of emotion in remitted depressed patients during a working memory task with emotional distracters. Psychol Med. 2012;42(1):29–40. | ||
Kerestes R, Bhagwagar Z, Nathan PJ, et al. Prefrontal cortical response to emotional faces in individuals with major depressive disorder in remission. Psychiatry Res. 2012;202(1):30–37. | ||
MacFall JR, Payne ME, Provenzale JE, Krishnan KR. Medial orbital frontal lesions in late-onset depression. Biol Psychiatry. 2001;49(9):803–806. | ||
Hatt SR, Leske DA, Liebermann L, Philbrick KL, Holmes JM. Depressive symptoms associated with poor health-related quality of life in adults with strabismus. Ophthalmology. 2014;121(10):2070–2071. | ||
McBain HB, MacKenzie KA, Au C, et al. Factors associated with quality of life and mood in adults with strabismus. Br J Ophthalmol. 2014;98(4):550–555. | ||
Herzfeld DJ, Kojima Y, Soetedjo R, Shadmehr R. Encoding of action by the Purkinje cells of the cerebellum. Nature. 2015;526(7573):439–442. | ||
Nitschke MF, Arp T, Stavrou G, Erdmann C, Heide W. The cerebellum in the cerebro-cerebellar network for the control of eye and hand movements – an fMRI study. Prog Brain Res. 2005;148:151–164. | ||
Hayakawa Y, Nakajima T, Takagi M, Fukuhara N, Abe H. Human cerebellar activation in relation to saccadic eye movements: a functional magnetic resonance imaging study. Ophthalmologica. 2002;216(6):399–405. | ||
Joshi AC, Das VE. Muscimol inactivation of caudal fastigial nucleus and posterior interposed nucleus in monkeys with strabismus. J Neurophysiol. 2013;110(8):1882–1891. | ||
Triarhou LC. A proposed number system for the 107 cortical areas of Economo and Koskinas, and Brodmann area correlations. Stereotact Funct Neurosurg. 2007;85(5):204–215. | ||
Tomasi D, Volkow ND. Association between functional connectivity hubs and brain networks. Cereb Cortex. 2011;21(9):2003–2013. | ||
Zhang S, Li CS. Functional clustering of the human inferior parietal lobule by whole brain connectivity mapping of resting-state functional magnetic resonance imaging signals. Brain Connect. 2014;4(1):53–69. | ||
Yang X, Zhang J, Lang L, Gong Q, Liu L. Assessment of cortical dysfunction in infantile esotropia using fMRI. Eur J Ophthalmol. 2014;24(3):409–416. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.