Back to Journals » The Application of Clinical Genetics » Volume 8
22q11 deletion syndrome: current perspective
Authors Hacıhamdioğlu B, Hacıhamdioğlu DO, Delil K
Received 3 February 2015
Accepted for publication 20 March 2015
Published 18 May 2015 Volume 2015:8 Pages 123—132
DOI https://doi.org/10.2147/TACG.S82105
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Martin Maurer
Bülent Hacihamdioğlu,1 Duygu Hacihamdioğlu,2 Kenan Delil3
1Department of Pediatric Endocrinology, 2Department of Pediatric Nephrology, GATA Haydarpasa Training Hospital, 3Department of Medical Genetics, Marmara University, School of Medicine, Istanbul, Turkey
Abstract: Chromosome 22q11 is characterized by the presence of chromosome-specific low-copy repeats or segmental duplications. This region of the chromosome is very unstable and susceptible to mutations. The misalignment of low-copy repeats during nonallelic homologous recombination leads to the deletion of the 22q11.2 region, which results in 22q11 deletion syndrome (22q11DS). The 22q11.2 deletion is associated with a wide variety of phenotypes. The term 22q11DS is an umbrella term that is used to encompass all 22q11.2 deletion-associated phenotypes. The haploinsufficiency of genes located at 22q11.2 affects the early morphogenesis of the pharyngeal arches, heart, skeleton, and brain. TBX1 is the most important gene for 22q11DS. This syndrome can ultimately affect many organs or systems; therefore, it has a very wide phenotypic spectrum. An increasing amount of information is available related to the pathogenesis, clinical phenotypes, and management of this syndrome in recent years. This review summarizes the current clinical and genetic status related to 22q11DS.
Keywords: DiGeorge syndrome, velocardiofacial syndrome, TBX1
Introduction
Congenital absence of a thymus and parathyroid gland was reported by Dr Angelo M DiGeorge in 1965. Later, cardiac anomalies were added to the phenotype, and the syndrome was named DiGeorge syndrome (DGS; Mendelian Inheritance in Man [MIM] number 188400).1 Most patients with DGS have monosomic deletions on the long arm of chromosome 22. This deletion might present with a variety of phenotypes, including DGS and velocardiofacial syndrome. 22q11 deletion syndrome (22q11DS) is an umbrella term that describes various clinical phenotypes.2,3 22q11DS is the most common microdeletion syndrome in humans, although it is likely to be more prevalent than reported and underrecognized because of its inherent clinical variability and heterogeneity. 22q11DS can affect many organs and systems.4,5 An increasing amount of information has been reported regarding the pathogenesis, clinical phenotypes, and management of this syndrome in recent years. This review summarizes the current clinical and genetic status of 22q11DS.
Nomenclature
A long-arm deletion of chromosome 22 might present with a variety of phenotypes, including DGS, velocardiofacial syndrome (MIM number 192430), conotruncal anomaly face syndrome (MIM number 217095) (or Takao syndrome), and isolated outflow tract (OFT) defects of the heart.2 CATCH22 (Cardiac Abnormality/abnormal facies, T-cell deficit due to thymic hypoplasia, Cleft palate, Hypocalcemia due to hypoparathyroidism resulting from 22q11 deletion) was proposed as a collective acronym for these differing presentations of a common genetic etiology.2,3 Many clinicians believe that 22q11.2 deletion is a single syndrome rather than several distinct syndromes.2 Therefore, the term 22q11DS is an umbrella term used to describe all deletion-associated phenotypes. The term 22q11DS is used in this review to cover all of the phenotypic variations described before.
Pathogenesis
Human chromosome 22 is acrocentric, and is the second-smallest human chromosome. It spans ~51 million DNA building blocks (base pairs) and represents 1.6% of the human genome in cells. Recurrent acquired and somatic rearrangements of chromosome 22 are associated with multiple diseases and developmental abnormalities. Most of these recurrent rearrangements occur within 22q11, suggesting genomic instability of this region of chromosome 22. Deletions of 22q are associated with 22q11DS.6 The deletion occurs near the middle of the chromosome at a location designated q11.2, and results in a 1.5–3 Mb microdeletion on the long arm of chromosome 22. Although different-sized lesions have been identified, ~90% of patients have a common ~3 Mb deletion, which is defined the typically deleted region (TDR), whereas most other (~7%) patients have a smaller ~1.5 Mb deletion. A small percentage of affected individuals have shorter deletions in the same region.2
Mechanism of the deletion at 22q11.2
Complex low-copy repeats (LCRs, also termed segmental duplications), which are composed of multiple repeat elements, provide the structural basis for a diverse range of genomic variations and combinations of variations. These regions of chromosomes are susceptible to translocations, inversions, deletions, and duplications. LCRs are region-specific DNA blocks usually sized >5–10 kb that share >95%–97% similarity with each other. Nonallelic homologous recombination (NAHR) is a form of homologous recombination that occurs between two lengths of DNA that share high sequence similarity but are not alleles. NAHR is one of the major genomic rearrangements, and most recurrent genomic rearrangements are caused by NAHR between two LCRs. Due to their high sequence identity, nonallelic copies of LCRs, instead of copies at the usual allelic positions, can sometimes be aligned during meiosis or mitosis. This so-called misalignment and the subsequent crossover between them can result in genomic rearrangements in progeny cells. Thus, the nonallelic copies act as mediators of homologous recombination and are responsible for the observed breakpoint clustering. NAHR between LCRs causes duplication and/or deletions. The misalignment of LCRs during NAHR is an important mechanism underlying chromosomal microdeletion disorders, including 22q11DS.7–10
The proximal region of 22q11.2 is enriched with LCRs. This region contains eight chromosome 22-specific LCRs (LCR22s; LCR22-A to LCR22-H). There is a relationship between four LCR22s (LCR22-A, -B, -C, and -D) and 22q11DS (Figure 1). These proximal LCRs are larger than the distal ones, and have a complex modular structure. The typical 3 Mb deletion occurs between the most proximal (LCR22-A) and most distal (LCR22-D) units, whereas a 1.5 Mb deletion could be an A–B or an A–C deletion.2,7
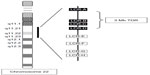  | Figure 1 Schematic view of chromosome 22 indicating the position of the low-copy repeats in 22q11.2. |
The LCR22s comprise 11% of the 22q11.2 region and contain both genes and unprocessed pseudogene copies. The BCR pseudogene is present once in LCR22-A, and twice in LCR22-D. The sequences that correspond to the BCR-like module within the LCRs were suggested as a potential rearrangement hotspot.11,12
It was demonstrated that deletions in individuals with 22q11DS had more frequently maternal origin than paternal origins (56% versus 44%). But maternal age does not act as an etiologic factor for the finding of enhanced maternal origin of the deletion. Also, there is no association between the paternal age and the frequency of the deletion.13
Results of 22q11.2 deletion and its contribution to clinical phenotypes
The diminished gene expression on 22q11.2 is responsible for the clinical findings associated with 22q11DS; however, little is known about how such changes lead to the phenotypes of 22q11DS. The 3 Mb chromosomal region contains >35 genes, many of which have not been well characterized (Figure 2). The diminished dose of these genes, or their haploinsufficiency, likely compromises early morphogenesis in the pharyngeal arches, heart, skeleton, and brain. However, there is no correlation between the size or type of deletion and the resulting phenotype.2,7,8
Numerous candidate genes have been linked with the 22q11DS phenotype. In 1999, murine models identified TBX1 as a candidate gene for this syndrome. TBX1, which encodes a T-box-containing transcription factor that belongs to a large family of transcription factors, has distinct roles in a wide range of embryonic differentiation or response pathways. TBX1 is the most important gene for 22q11DS.14
The pharyngeal apparatus is an embryonic structure that becomes remodeled to form the face, neck, and cardiac OFT. The transcription factors expressed in pharyngeal mesoderm progenitors form a regulatory network that coordinates normal heart and craniofacial development. TBX1 is expressed in the endoderm and mesoderm of pharyngeal arches, and the ectoderm of the distal pharyngeal apparatus. Animal models have shown that the haploinsufficiency of TBX1 causes abnormal growth and remodeling in the pharyngeal apparatus and related structures. This information might explain many of the clinical findings of the syndrome, including facial dysmorphia, palatal defects, hypoplasia of the parathyroid glands and thymus, and dental, feeding, and swallowing problems.14,15
New data are available in the literature about molecular mechanism of dental anomalies in 22q11DS. It was shown that TBX1 regulates the proliferation of dental progenitor cells and craniofacial development through microRNA-96-5p.16
Neuroepithelium-derived cardiac neural crest cells (cNCCs) are needed for the proper septation of the OFT into the aorta and pulmonary trunk, as well as for the development of the cardiac valves. TBX1 regulates the differentiation and migration of cNCCs. Cardiac progenitor cells from the second heart field (SHF) contribute to the rapid growth of the embryonic heart, giving rise to the right ventricle and OFT, the myocardium at the arterial pole of the heart, and the atrial myocardium at the venous pole. TBX1 is required for both inflow tract and OFT morphogenesis because it regulates the segregation and deployment of progenitor cells in the posterior SHF. The primary heart field gives rise to the primitive linear tube, and is not dependent on TBX1. TBX1 knockout animal models supported the importance of this gene in cardiac development. In summary, TBX1 haploinsufficiency contributes to the conotruncal and cardiac OFT anomalies that are observed commonly in 22q11DS.17–19
WNT5A is an important gene for embryogenesis and is critically required for SHF deployment. Recent study showed that TBX1 is likely to be promoting SHF development through activating WNT5A transcription, and disruption of WNT5A-mediated SHF deployment may contribute significantly to the pathogenesis of OFT malformations in 22q11DS.20
Various pathways downstream of TBX1 and modifiers of TBX1 activity seem to play an important role in the pathogenesis of 22q11DS. TBX1 regulates the expression of several growth factors and transcription factors, including FGF8, FGF10, PITX2, CHD7, VEFR3, EYA1, WNT5A, BMPER, and Otog-MyoD.18,19 Disruption of the expression of these genes by the loss of function of TBX1 contributes to the pathogenesis of 22q11DS. TBX1 expression is regulated negatively by retinoic acid, and positively by SHH via FOXA2.17–19 The manipulation of these pathways might be a cornerstone of future advances in 22q11DS.
TBX1 is the best-known and most studied gene on 22q11.2. The current literature suggests that TBX1 is largely responsible for the clinical findings in patients with 22q11DS, particularly the physical malformations. However, TBX1 haploinsufficiency cannot explain all the clinic phenotypes of 22q11DS. Nevertheless, as mentioned above, the TDR that causes 22q11DS contains many genes.7,19
Recently, it was shown that haploid 22q11 gene insufficiency, including but not limited to TBX1, disrupts orofacial and cranial nerve development by modifying retinoic acid-modulated anterior–posterior hindbrain differentiation. These disruptions likely contribute to dysphagia in infants and young children with 22q11DS.21
Recent studies showed that reduced doses of 22q11 genes could modify the initial forebrain patterning, subsequent cortical neurogenesis and migration, and the mitochondrial support of activity-dependent synapse formation and elimination in the early postnatal brain. Nevertheless, it remains unclear which genes have a cause-and-effect relationship with these processes.22
Catechol-O-methyl transferase (COMT) degrades catecholamines such as dopamine and epinephrine; its gene is located on chromosome 22q11.2. The proline dehydrogenase (oxidase) 1 (PRODH) gene is also located in the same region, which encodes a mitochondrial enzyme that degrades proline. The deficiency of this enzyme results in hyperprolinemia. COMT and PRODH haploinsufficiency was implicated by some studies in the behavioral and psychiatric disturbances associated with 22q11DS.23 SMARCB1 is a tumor suppressor gene that is also located on 22q11.2 distal of the TDR for 22q11DS. The haploid deficiency of this gene might be associated with head-and-neck tumors such as rhabdoid tumors in some 22q11DS patients.24 In addition, the haploinsufficiency of glycoprotein Ib β (GP1BB) might contribute to the mild thrombocytopenia observed in patients with 22q11DS. GP1BB is also located on chromosome 22q11.2. Bernard–Soulier syndrome, which is characterized by giant platelets, thrombocytopenia, and a prolonged bleeding time, was also described in patients with 22q11DS.25 Several other genes in the 22q11 region, such as histone cell cycle regulator gene (HIRA), ubiquitin fusion degradation 1-like gene (UFD1L), and Crk-like protein gene (CRKL), have been implicated in the pathogenesis of 22q11DS.7,19
Epidemiology
22q11DS is the most common microdeletion syndrome in humans. However, population-based estimates of the incidence and prevalence of 22q11DS differ. Most studies reported a prevalence of one in every 4,000 newborns; however, reports range from one in 2,000 to one in 6,395.3,26,27 Nevertheless, many researchers believe that this number is artificially low due to under-diagnosis. Consistent with this, familial occurrence is the most frequent cause of diagnosis in adults at some genetic centers.28
Male and female sexes are affected equally by 22q11DS. In addition, the deletion of 22q11.2 is more prevalent within certain ethnic groups. Specifically, 22q11DS occurs more frequently among Hispanics compared with Whites, African Americans, and Asians.26
Generally, >90% of DGS cases are de novo or novel deletions caused by a random occurrence during fetal development. An unaffected parent might then carry the deletion in his or her eggs or sperm, and the risk of recurrence is ~1%. However, it can also be inherited, and familial autosomal dominant recurrence is reported in ~8%–28% of patients in various series.29 Some cases appear to have a vigorous diagnosis but no deletion; 35%–90% of patients with DGS and 80%–100% of velocardiofacial syndrome patients have the 22q deletion.2,30
Clinical presentation
22q11DS presents with a very wide phenotypic spectrum, including the following: facial dysmorphisms; congenital cardiac defects; velopharyngeal insufficiency with or without cleft palate; thymic hypoplasia; immune deficiency; parathyroid hypoplasia; developmental delay; learning disabilities; psychiatric disorders; renal, ocular, and skeletal malformations; hearing loss; and laryngeal abnormalities. The phenotypes associated with the syndrome might be recognized during the prenatal period, or in newborns, children, and even adults.31–33 Clinical phenotypes of 22q11DS are summarized in Table 1.
Fetal phenotype
Congenital heart defects are the major prenatal sonographical feature of 22q11 deletions. Among these, conotruncal defects are the most common cardiac anomalies, although vascular abnormalities and hypoplastic left hearts were also reported.34 Thymus abnormalities are also an important prenatal sonographic feature of this syndrome. Urinary tract defects, neurological problems such as neural tube defects, cerebral anomalies, and polyhydramnios have also been reported.35 However, facial anomalies in fetuses are difficult to diagnose.
Neonatal and childhood phenotype
The clinical presentation of 22q11DS in pediatric patients and neonates is highly variable. The manifestations involve multiple organ systems and vary in severity and from patient to patient; the symptoms also vary depending on the age of the patient. Nevertheless, they commonly include the following classic findings: behavioral problems, developmental and/or learning disabilities, conotruncal cardiac anomalies, palatal defects, hypernasal speech, immunodeficiency, hypocalcemia, and characteristic facial features.2,3,31,32
Congenital heart disease is present in ~80% of patients with 22q11DS, and conotruncal and aortic arch defects are the most typical cardiac malformations associated with 22q11DS. The conotruncal defects include tetralogy of Fallot, pulmonary atresia, truncus arteriosus, an interrupted aortic arch, and a double outlet right ventricle. Nonconotruncal defects such as ventricular septal defects, atrial septal defects, and atrioventricular septal defects have also been reported. Tetralogy of Fallot is the most prevalent cardiac defect in 22q11DS, but interrupted aortic arch type B (distal to the left common carotid artery) is the most specific defect. Cardiopathies might appear shortly after birth with cyanosis or cardiovascular collapse, or could be defined in adulthood. An aberrant subclavian artery might present with feeding difficulties or respiratory symptoms.31,32,35
Although hypoparathyroidism is a rare endocrine disorder in pediatric-aged patients, the hypocalcemia caused by hypoparathyroidism is one of the classic symptoms of 22q11DS, and is present in 16%–70% of patients.2 Hypoparathyroidism can be diagnosed in children of all ages with 22q11DS; diagnosis occurs commonly in the newborn period but can also occur during the late adolescent period.36 Mild hypocalcemia without symptoms might last for several years.37 Hypoparathyroidism is often transient and resolves after the neonatal period, but it may manifest later in life as episodes of hypocalcemia during stresses such as infectious diseases, surgery, or pregnancy. Patients develop permanent hypoparathyroidism only rarely. Neonatal hypocalcemia is not associated with the later development of permanent hypoparathyroidism.38 However, the early onset of hypoparathyroidism is associated with a high risk of later recurrence.39 A recent study concluded that the occurrence of neonatal seizures related to hypocalcemia might increase the risk of more severe intellectual deficits in patients with 22q11DS.40
The metabolic features of hypoparathyroidism include hypocalcemia, hyperphosphatemia, and reduced or low-range parathyroid hormone levels. The usual signs and symptoms are muscle cramps and tingling, numbing, seizures, tetany, positive Chvostek signs, and positive Trousseau signs. Stridor can also be a symptom, but it must be differentiated from laryngeal web. Hypocalcemia in 22q11DS has a wide clinical manifestation, ranging from only paresthesia and numbness to convulsions.3,31,32,41
The congenital cardiac defects associated with neonatal hypocalcemia are the most frequent features that lead to diagnosis in the first 2 years of life. The most common symptoms leading to diagnosis in patients older than 2 years are neuropsychological manifestations, otorhinolaryngologic manifestations, and typical facial findings.2,3,28,31–33
Hypotonia and ligamentous laxity are very common in the infantile period. An unsteady gait, a lack of coordination, and clumsy hand skills are also observed commonly. Patients with 22q11DS also have an increased risk of spinal deformities such as cervical spinal abnormalities and scoliosis, and idiopathic leg pains are seen commonly in childhood.3,31–33,42
The neurocognitive profile of 22q11DS is also highly variable, both among individuals and throughout its development. Almost all individuals with 22q11DS cope with the resulting cognitive deficits. Borderline intellectual function (an IQ of 70–75) is the most common intellectual disability in these patients. The mathematic ability is usually weak, but their memory is good. Attention difficulties, visual spatial abnormalities, and impaired executive function are also common. Most children with 22q11DS achieve higher scores in verbal tasks than in non-verbal tasks. In addition, learning difficulties are very common during the preschool and in primary school-aged children. Psychiatric problems related to 22q11DS have also been described in children and adolescents, including attention-deficit/hyperactivity disorders, anxiety disorders, depression, and autism spectrum disorders.43–46
Most 22q11DS patients have speech or language difficulties. The most common speech abnormality is velopharyngeal insufficiency, which manifests typically as hypernasal speech, increased nasal resonance, and nasal regurgitation. Velopharyngeal insufficiency that becomes increasingly apparent with age and submucous cleft palate might also be observed, although overt cleft palate is rare. In addition to immune deficiency, palatal weakness and Eustachian tube dysfunction lead to recurrent ear infections in these patients. Hearing loss is a frequent problem in patients with 22q11DS.31,32,47,48
Immunodeficiency is another key feature of 22q11DS. The observed immunodeficiencies are secondary to thymic aplasia or hypoplasia with subsequent impaired thymocyte development. The degree of immunodeficiency seen in patients with 22q11DS is highly variable, and might include defects in T-lymphocyte number and function, as well as humoral defects. The thymus and the T-cells are absent completely (complete DGS) in a very small number of patients, but most subjects have a milder form of immunodeficiency (incomplete DGS). Despite the low-for-age T-cell counts in most patients in infancy, this usually improves during the first year of life.43,49 Antibody deficiencies (hypogammaglobulinemia) have also been described in a minority of patients, most commonly IgA deficiency. An increased frequency of infections, mainly respiratory tract infections, is common in children with 22q11DS, but the frequency commonly diminishes with increasing age.43,49,50 An increased prevalence of autoimmune conditions was reported in both children and adults with 22q11DS.49
Despite the phenotypic variability, most children with 22q11DS share a combination of features and have a characteristic dysmorphic facial appearance (Figure 3).36 The facial characteristics described in individuals with 22q11DS are a long face, malar flattening, hypertelorism, short palpebral fissures, hooded/swollen eyelids, a wide and prominent nasal root, a wide/broad nasal bridge, a low nasal bridge, a bulbous nasal tip (becoming evident with age), hypoplastic alae nasi, micrognathia, a small mouth, asymmetric facial movements, and malformed, small, low-set ears. Children with 22q11DS usually have a mild pattern of the characteristic facial features, which might not be recognized easily. However, a physician experienced in 22q11DS could observe the typical facial features in most patients. Postaxial polydactyly might also occur.30,51
Renal problems are frequent in patients with 22q11DS, including structural renal anomalies such as renal agenesis or dysplastic kidneys, obstructive abnormalities, and vesicoureteric reflux.2,3,30–33 Morphological and functional thyroid alternations have also been reported. Thyroid hypoplasia is common, but hypothyroidism is rare in 22q11DS.52 Gastrointestinal involvement is observed sometimes in patients, including gastroesophageal reflux, chronic constipation, abdominal pain, and vomiting. However, intestinal malrotation is rare. Refractive errors, strabismus, amblyopia, and structural ocular abnormalities are encountered frequently in children with 22q11DS.2,3,30–33 Growth deficiencies are common in patients, particularly during infancy and early childhood. Nevertheless, growth hormone deficiency has been described only rarely.53
Adult phenotype
Due to variation in the phenotypic features and their severity, the diagnosis of 22q11DS could be missed in children, and the syndrome might be diagnosed during adulthood instead. The main presenting symptoms in adults are developmental delays with psychiatric disorders and cardiac anomalies.54 A recent study showed that 22q11DS might increase the risk of early-onset Parkinson’s disease.55 Hypoparathyroidism might be the main reason for diagnosis during adulthood. It was reported that familial inheritance is the most frequent reason for adults with 22q11DS to be referred to the genetic clinic. If concomitant findings such as the typical facial features and voice abnormalities (such as hypernasality) associated with 22q11 deletions are observed in patients evaluated at psychiatry and cardiology clinics, the diagnosis of 22q11DS should be considered.28,54
Diagnosis
The decision to test for 22q11DS is easy if multiple defects and/or symptoms associated with the syndrome are present simultaneously. However, physicians should note that the signs and symptoms might be subtle; therefore, clinical clues could be overlooked easily. As mentioned above, patients with this syndrome usually have mild facial features. As such, careful physical examinations using anthropometric measures are very important for suspected cases of 22q11DS. It should be noted that the diagnosis of 22q11DS, particularly in adolescents and adults, often requires an enhanced index of suspicion.30–32 Detailed suggestions for clinicians have been published elsewhere.56
Fluorescence in situ hybridization (FISH) is the current method of choice for detecting 22q11.2 microdeletions. FISH is a highly accurate and reliable test that can also be used for prenatal diagnosis. However, it is limited to a single target sequence within the proximal 22q11.2 deletion region, and some atypical deletions do not include the region analyzed using FISH with commonly used probes (such as TUPLE1). A polymerase chain reaction-based assay (multiplex ligand-dependent probe amplification) is used widely in Europe, and is becoming accepted increasingly in the US because it has a rapid turnaround time, it is more cost-effective, and can detect the smaller deletions missed by FISH. This novel technique is capable of detecting atypical 22q11.2 deletions that are not routinely tested or detected using routine FISH.5,57 Advanced molecular methods that identify the deletion or duplication of genomic sequences at high resolution, such as microarrays, can also be used. The detection capacity of microarrays depends on the density of the probes used. This is particularly important when patients present with classical features of the syndrome but no evidence of gene deletions using FISH; diagnosis is challenging in these patients. For example, point mutations in TBX1 have been described in a small number of patients.58
There is a need for a rapid, cost-effective, and easy laboratory method for screening and diagnosis of 22q11DS. A recent study shows promise in this regard. A multiplex droplet digital polymerase chain reaction is sensitive and specific for the detection of 22q11DS.59
Management
22q11DS is a multisystem syndrome with remarkable variability and expression among individuals. Moreover, the presence of one feature does not predict the presence of any other feature. As such, the management of 22q11DS patients is highly dependent on age and phenotype; therefore, treatment is individualized according to the underlying lesion and severity.31,32
In infants and young children with feeding problems, recurrent infections, hypocalcemia, and structural cardiac and palatal anomalies might be accompanied by speech, learning, and/or developmental difficulties. The combination of poor suck reflexes, palatal weakness, and dysfunctional swallowing often means that formula rests in abnormal anatomic locations or regurgitates into the Eustachian tube or sinuses. Gastroesophageal reflux is also common in these patients. The management of feeding difficulties includes thickeners, anti-reflux medications, and nasogastric or gastrostomic feeding tubes when necessary.2,3,31,32
Hypocalcemia due to hypoparathyroidism is a common problem during the neonatal period, but it could occur at any age, including adulthood. The standard treatment for hypoparathyroidism is to correct hypocalcemia using oral vitamin D analogs and calcium. However, physicians should be careful to avoid overtreatment, which results in hypercalciuria, hypercalcemia, nephrolithiasis, nephrocalcinosis, and renal failure.60 Teriparatide recombinant human parathyroid hormone (1–34) is a promising novel treatment for chronic hypocalcemia in hypoparathyroid syndromic children, and it might solve this problem in the future.41 A recent study demonstrated the efficacy of parental parathyroid transplantation combined with allogeneic thymus transplantation in a patient.61 Daily vitamin D is advised for 22q11DS patients of all ages with hypocalcemia; the dose should be the recommended daily allowance or as indicated therapeutically.32
Recurrent infections, particularly otitis media, might be an important problem during this period, and hearing loss might occur. Children should be treated appropriately for infections and followed carefully for potential hearing problems. Unrecognized hearing loss might contribute to delayed speech and cognitive development.31,32,43,49
Reconstituting the immune system is essential for patients with complete DGS, which can be accomplished by two methods: thymus tissue transplantation and a fully matched peripheral blood T-cell transplantation. Patients with complete DGS need to be protected from infections and blood products. Antifungal, antiviral, and antipneumocystis prophylaxis, and immunoglobulin replacement therapy should be commenced in these patients. Blood products could induce graft-versus-host disease when T-cells are absent. If necessary, patients should receive cytomegalovirus-negative and irradiated blood products. In addition, live viral vaccines should be avoided in patients with severe immunodeficiency.43,49 Adverse events following live immunizations are typically minor and self-limited, suggesting that live vaccines could be considered in patients with mild-to-moderate immunosuppression.62 As mentioned above, hypogammaglobulinemia might develop in patients with 22q11DS. For example, severe antibody deficiencies that are associated with lower respiratory tract infections and autoimmune conditions might occur. Therefore, patients should be screened for potential antibody deficiency.49 Importantly, the degree of immunodeficiency cannot be predicted based on other phenotypic features and must be assessed individually in each patient with 22q11DS.63
Patients with 22q11DS have high death rates. Most deaths occur during the first year of life, and are associated with the presence of congenital heart diseases, particularly severe cardiac defects.64 Right-sided heart failure, which is related to pulmonary vascular resistance, is a common complication of these anomalies, and was proposed to be an important contributor to mortality.64 Surgical treatment is necessary for many of the cardiac problems in patients with 22q11DS. Nevertheless, individualized surgical approaches are needed according to the underlying cardiac lesion in each patient.65 Laryngeal abnormalities are not rare and are important to recognize, particularly if cardiac surgery is planned. Therefore, complete ear, nose, and throat examinations and airway evaluations should be performed before any surgical procedure.66
Speech during childhood should be given careful attention, and speech therapy might be necessary in 22q11DS patients. Submucosal cleft palate can be detected easily using careful physical examinations, and can be corrected using surgery. Patients with velopharyngeal insufficiency should be followed up and treated by an experienced team. Surgery is often necessary and useful to correct velopharyngeal insufficiency with or without palatal defect. Adenoidectomy might worsen speech articulation; therefore, it should be avoided as much as possible. In addition, head-and-neck vascular anomalies are common in patients with 22q11DS, and there is an increased risk of carotid artery injury because of medical displacement during pharyngeal surgery. This possibility should be considered before and during relevant operations.19,67,68 Finally, the risk of obstructive sleep apnea is increased in patients with 22q11DS after velopharyngeal insufficiency surgery.69
Preschool and school-aged children with 22q11DS should be screened for neurocognitive and psychiatric problems. These patients should be followed carefully because early support and treatment are vital in these individuals. Adjusting the child’s school environment might also maximize learning. Behavioral issues and psychiatric illnesses are likely to become more problematic with increasing age. Although psychotic disorders are chronic in most cases, they can also be transient. Anxiety disorders are a major risk factor for psychosis in patients with 22q11DS. As such, accurate psychiatric management should start in childhood and continue throughout adulthood in these individuals.45,46
As mentioned above, 22q11DS might affect many systems, and urinary ultrasonography should be performed after diagnosis. Children with 22q11DS should be screened for scoliosis, and surgical treatment might be necessary to correct this condition. Symmetric leg pain is seen frequently in 22q11DS patients during childhood, whereas asymmetric leg pain suggests other pathologies. Patients should also be screened for thyroid function and if necessary, thyroid morphology. Vomiting is common with 22q11DS, and can indicate a problem in the gastrointestinal system such as reflux or malrotation. If indicated clinically, patients should also be screened for autoimmune disorders such as Celiac disease. Subjects should also be screened for strabismus and refractive errors at 2 years or 3 years of age.31,32
Children with 22q11DS should be followed up using the specialized growth charts available for this syndrome. If growth problems are detected, an endocrinologist could be consulted.53,70
The optimal management of patients with 22q11DS requires a comprehensive team approach, including specialists in genetics, pediatrics, endocrinology, plastic surgeons, immunologists, otolaryngologists, and speech therapists. 22q11DS is not a rare syndrome, and there is a need to form a local specialist team to ensure optimal management of affected patients. Appropriate guidelines for the management of patients are available in the literature, which contain useful information for physicians interested in 22q11DS syndrome.31,32,71 22q11DS might be difficult to recognize and diagnose in some patients, although the clinical findings for early diagnosis are known. Early diagnosis provides the best opportunity for modifying the course of the illness and optimizing patient outcome.
Disclosure
The authors report no conflicts of interest in this review.
References
DiGeorge AM. Discussions on a new concept of the cellular basis of immunology. J Pediatr. 1965;67(5):907–908. | |
Kobrynski LJ, Sullivan KE. Velocardiofacial syndrome, DiGeorge syndrome: the chromosome 22q11.2 deletion syndromes. Lancet. 2007;370(9596):1443–1452. | |
McDonald-McGinn DM, Sullivan KE. Chromosome 22q11.2 deletion syndrome (DiGeorge syndrome/velocardiofacial syndrome). Medicine (Baltimore). 2011;90(1):1–18. | |
Tézenas Du Montcel S, Mendizabai H, Aymé S, Lévy A, Philip N. Prevalence of 22q11 microdeletion. J Med Genet. 1996;33(8):719. | |
Kimberley AM. FISH diagnosis of 22q11.2 deletion syndrome. Newborn Infant Nurs Rev. 2008;8:e11–e19. | |
Yu S, Graf WD, Shprintzen RJ. Genomic disorders on chromosome 22. Curr Opin Pediatr. 2012;24(6):665–671. | |
Emanuel BS. Molecular mechanisms and diagnosis of chromosome 22q11.2 rearrangements. Dev Disabil Res Rev. 2008;14(1):11–18. | |
Hurles M. How homologous recombination generates a mutable genome. Hum Genomics. 2005;2(3):179–186. | |
Gu W, Zhang F, Lupski JR. Mechanisms for human genomic rearrangements. Pathogenetics. 2008;1(1):4. | |
Dittwald P, Gambin T, Gonzaga-Jauregui C, et al. Inverted low-copy repeats and genome instability – a genome-wide analysis. Hum Mutat. 2013;34(1):210–220. | |
Pavlicek A, House R, Gentles AJ, Jurka J, Morrow BE. Traffic of genetic information between segmental duplications flanking the typical 22q11.2 deletion in velo-cardio-facial syndrome/DiGeorge syndrome. Genome Res. 2005;15(11):1487–1495. | |
Cole CG, McCann OT, Collins JE, et al. Finishing the human chromosome 22 sequence. Genome Biol. 2008;9(5):R78. | |
Delio M, Guo T, McDonald-McGinn DM, et al. Enhanced maternal origin of the 22q11.2 deletion in velocardiofacial and DiGeorge syndromes. Am J Hum Genet. 2013;92(3):439–447. | |
Gao S, Li X, Amendt BA. Understanding the role of TBX1 as a candidate gene for 22q11.2 deletion syndrome. Curr Allergy Asthma Rep. 2013; 13(6):613–621. | |
Scambler PJ. 22q11 deletion syndrome: a role for TBX1 in pharyngeal and cardiovascular development. Pediatr Cardiol. 2010;31(3):378–390. | |
Gao S, Moreno M, Eliason S, et al. TBX1 protein interactions and microRNA-96-5p regulation controls cell proliferation during craniofacial and dental development: implications for 22q11.2 deletion syndrome. Hum Mol Genet. 2015;24(8):2330–2348. | |
Rana MS, Théveniau-Ruissy M, De Bono C, et al. TBX1 coordinates addition of posterior second heart field progenitor cells to the arterial and venous poles of the heart. Circ Res. 2014;115(9):790–799. | |
Castellanos R, Xie Q, Zheng D, Cvekl A, Morrow BE. Mammalian TBX1 preferentially binds and regulates downstream targets via a tandem T-site repeat. PLoS One. 2014;9(5):e95151. | |
Scambler PJ. The 22q11 deletion syndromes. Hum Mol Genet. 2000; 9(16):2421–2426. | |
Sinha T, Li D, Théveniau-Ruissy M, Hutson MR, Kelly RG, Wang J. Loss of Wnt5a disrupts second heart field cell deployment and may contribute to OFT malformations in DiGeorge syndrome. Hum Mol Genet. 2015;24(6):1704–1716. | |
Karpinski BA, Maynard TM, Fralish MS, et al. Dysphagia and disrupted cranial nerve development in a mouse model of DiGeorge (22q11) deletion syndrome. Dis Model Mech. 2014;7(2):245–257. | |
Meechan DW, Maynard TM, Tucker ES, LaMantia AS. Three phases of DiGeorge/22q11 deletion syndrome pathogenesis during brain development: patterning, proliferation, and mitochondrial functions of 22q11 genes. Int J Dev Neurosci. 2011;29(3):283–294. | |
Raux G, Bumsel E, Hecketsweiler B, et al. Involvement of hyperprolinemia in cognitive and psychiatric features of the 22q11 deletion syndrome. Hum Mol Genet. 2007;16(1):83–91. | |
Marom T, Roth Y, Goldfarb A, Cinamon U. Head and neck manifestations of 22q11.2 deletion syndromes. Eur Arch Otorhinolaryngol. 2012;269(2):381–387. | |
Rosa RF, Rosa RC, Dos Santos PP, Zen PR, Paskulin GA. Hematological abnormalities and 22q11.2 deletion syndrome. Rev Bras Hematol Hemoter. 2011;33(2):151–154. | |
Botto LD, May K, Fernhoff PM, et al. A population-based study of the 22q11.2 deletion: phenotype, incidence, and contribution to major birth defects in the population. Pediatrics. 2003;112(1 pt 1):101–107. | |
Devriendt K, Fryns JP, Mortier G, van Thienen MN, Keymolen K. The annual incidence of DiGeorge/velocardiofacial syndrome. J Med Genet. 1998;35(9):789–790. | |
Vogels A, Schevenels S, Cayenberghs R, et al. Presenting symptoms in adults with the 22q11 deletion syndrome. Eur J Med Genet. 2014;57(4):157–162. | |
Sandrin-Garcia P, Macedo C, Martelli LR, et al. Recurrent 22q11.2 deletion in a sibship suggestive of parental germline mosaicism in velocardiofacial syndrome. Clin Genet. 2002;61(5):380–383. | |
Kitsiou-Tzeli S, Kolialexi A, Fryssira H, et al. Detection of 22q11.2 deletion among 139 patients with Di George/velocardiofacial syndrome features. In Vivo. 2004;18(5):603–608. | |
Bassett AS, McDonald-McGinn DM, Devriendt K, et al; International 22q11.2 Deletion Syndrome Consortium. Practical guidelines for managing patients with 22q11.2 deletion syndrome. J Pediatr. 2011;159(2):332–339. | |
Habel A, Herriot R, Kumararatne D, et al. Towards a safety net for management of 22q11.2 deletion syndrome: guidelines for our times. Eur J Pediatr. 2014;173(6):757–765. | |
Cancrini C, Puliafito P, Digilio MC, et al; Italian Network for Primary Immunodeficiencies. Clinical features and follow-up in patients with 22q11.2 deletion syndrome. J Pediatr. 2014;164(6):1475–1480. | |
Noël AC, Pelluard F, Delezoide AL, et al. Fetal phenotype associated with the 22q11 deletion. Am J Med Genet A. 2014;16(11):2724–2731. | |
Momma K. Cardiovascular anomalies associated with chromosome 22q11.2 deletion syndrome. Am J Cardiol. 2010;105(11):1617–1624. | |
Hacıhamdioğlu B, Berberoğlu M, Şiklar Z, et al. Case report: two patients with partial DiGeorge syndrome presenting with attention disorder and learning difficulties. J Clin Res Pediatr Endocrinol. 2011;3(2):95–97. | |
Bertola G, Giambona S, Bianchi R, Girola A, Berra SA. Sindrome di Di George: una diagnosi non sempre pediatrica. [Di George syndrome: not always a pediatric diagnosis]. Recenti Prog Med. 2013; 104(2):69. Italian. | |
Lima K, Abrahamsen TG, Wolff AB, et al. Hypoparathyroidism and autoimmunity in the 22q11.2 deletion syndrome. Eur J Endocrinol. 2011;165(2):345–352. | |
Cheung EN, George SR, Costain GA, et al. Prevalence of hypocalcaemia and its associated features in 22q11·2 deletion syndrome. Clin Endocrinol (Oxf). 2014;81(2):190–196. | |
Cheung EN, George SR, Andrade DM, Chow EW, Silversides CK, Bassett AS. Neonatal hypocalcemia, neonatal seizures, and intellectual disability in 22q11.2 deletion syndrome. Genet Med. 2014;16(1):40–44. | |
Matarazzo P, Tuli G, Fiore L, et al. Teriparatide (rhPTH) treatment in children with syndromic hypoparathyroidism. J Pediatr Endocrinol Metab. 2014;27(1–2):53–59. | |
Tsirikos AI, Khan LA, McMaster MJ. Spinal deformity in patients with DiGeorge syndrome. J Spinal Disord Tech. 2010;23(3):208–214. | |
Maggadottir SM, Sullivan KE. The diverse clinical features of chromosome 22q11.2 deletion syndrome (DiGeorge syndrome). J Allergy Clin Immunol Pract. 2013;1(6):589–594. | |
Baker K, Vorstman JA. Is there a core neuropsychiatric phenotype in 22q11.2 deletion syndrome? Curr Opin Neurol. 2012;25(2):131–137. | |
Demily C, Rossi M, Schneider M, et al. Neurocognitive and psychiatric management of the 22q11.2 deletion syndrome. Encephale. Epub 2014 Dec 15. | |
Schneider M, Debbané M, Bassett AS, et al; International Consortium on Brain and Behavior in 22q11.2 Deletion Syndrome. Psychiatric disorders from childhood to adulthood in 22q11.2 deletion syndrome: results from the International Consortium on Brain and Behavior in 22q11.2 Deletion Syndrome. Am J Psychiatry. 2014;171(6):627–639. | |
Persson C, Friman V, Óskarsdóttir S, Jönsson R. Speech and hearing in adults with 22q11.2 deletion syndrome. Am J Med Genet A. 2012; 158(12):3071–3079. | |
Ruda JM, Krakovitz P, Rose AS. A review of the evaluation and management of velopharyngeal insufficiency in children. Otolaryngol Clin North Am. 2012;45(3):653–669. | |
Gennery AR. Immunological aspects of 22q11.2 deletion syndrome. Cell Mol Life Sci. 2012;69(1):17–27. | |
Björk AH, Óskarsdóttir S, Andersson BA, Friman V. Antibody deficiency in adults with 22q11.2 deletion syndrome. Am J Med Genet A. 2012;158A(8):1934–1940. | |
Oskarsdóttir S, Holmberg E, Fasth A, Strömland K. Facial features in children with the 22q11 deletion syndrome. Acta Paediatr. 2008;97(8):1113–1137. | |
Stagi S, Lapi E, Gambineri E, et al. Thyroid function and morphology in subjects with microdeletion of chromosome 22q11 (del(22)(q11)). Clin Endocrinol (Oxf). 2010;72(6):839–844. | |
Weinzimer SA. Endocrine aspects of the 22q11.2 deletion syndrome. Genet Med. 2001;3(1):19–22. | |
Fung WL, Chow EW, Webb GD, Gatzoulis MA, Bassett AS. Extracardiac features predicting 22q11.2 deletion syndrome in adult congenital heart disease. Int J Cardiol. 2008;131(1):51–58. | |
Butcher NJ, Kiehl TR, Hazrati LN, et al. Association between early-onset Parkinson disease and 22q11.2 deletion syndrome: identification of a novel genetic form of Parkinson disease and its clinical implications. JAMA Neurol. 2013;70(11):1359–1366. | |
Monteiro FP, Vieira TP, Sgardioli IC, et al. Defining new guidelines for screening the 22q11.2 deletion based on a clinical and dysmorphologic evaluation of 194 individuals and review of the literature. Eur J Pediatr. 2013;172(7):927–945. | |
Fernández L, Lapunzina P, Arjona D, et al. Comparative study of three diagnostic approaches (FISH, STRs and MLPA) in 30 patients with 22q11.2 deletion syndrome. Clin Genet. 2005;68(4):373–378. | |
Driscoll DA. Molecular and genetic aspects of DiGeorge/velocardiofacial syndrome. Methods Mol Med. 2006;126:43–55. | |
Pretto D, Maar D, Yrigollen CM, Regan J, Tassone F. Screening newborn blood spots for 22q11.2 deletion syndrome using multiplex droplet digital PCR. Clin Chem. 2015;61(1):182–190. | |
Horwitz MJ, Stewart AF. Hypoparathyroidism: is it time for replacement therapy? J Clin Endocrinol Metab. 2008;93(9):3307–3309. | |
Chinn IK, Markert ML. Induction of tolerance to parental parathyroid grafts using allogeneic thymus tissue in patients with DiGeorge anomaly. J Allergy Clin Immunol. 2011;127(6):1351–1355. | |
Hofstetter AM, Jakob K, Klein NP, et al. Live vaccine use and safety in DiGeorge syndrome. Pediatrics. 2014;133(4):946–954. | |
Sullivan KE, Jawad AF, Randall P, et al. Lack of correlation between impaired T cell production, immunodeficiency, and other phenotypic features in chromosome 22q11.2 deletion syndromes. Clin Immunol Immunopathol. 1998;86(2):141–146. | |
Repetto GM, Guzmán ML, Delgado I, et al. Case fatality rate and associated factors in patients with 22q11 microdeletion syndrome: a retrospective cohort study. BMJ Open. 2014;4(11):e005041. | |
Carotti A, Digilio MC, Piacentini G, Saffirio C, Di Donato RM, Marino B. Cardiac defects and results of cardiac surgery in 22q11.2 deletion syndrome. Dev Disabil Res Rev. 2008;14(1):35–42. | |
Leopold C, De Barros A, Cellier C, Drouin-Garraud V, Dehesdin D, Marie JP. Laryngeal abnormalities are frequent in the 22q11 deletion syndrome. Int J Pediatr Otorhinolaryngol. 2012;76(1):36–40. | |
Kirschner RE, Baylis AL. Surgical considerations in 22Q11.2 deletion syndrome. Clin Plast Surg. 2014;41(2):271–282. | |
Stransky C, Basta M, McDonald-McGinn DM, et al. Perioperative risk factors in patients with 22q11.2 deletion syndrome requiring surgery for velopharyngeal dysfunction. Cleft Palate Craniofac J. 2015;52(2):183–191. | |
Kennedy WP, Mudd PA, Maguire MA, et al. 22q11.2 Deletion syndrome and obstructive sleep apnea. Int J Pediatr Otorhinolaryngol. 2014;78(8):1360–1364. | |
Tarquinio DC, Jones MC, Jones KL, Bird LM. Growth charts for 22q11 deletion syndrome. Am J Med Genet A. 2012;158(11):2672–2681. | |
Fung WL, Butcher NJ, Costain G, et al. Practical guidelines for managing adults with 22q11.2 deletion syndrome. Genet Med. Epub 2015 Jan 8. |
 © 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2015 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.



