Back to Journals » Drug, Healthcare and Patient Safety » Volume 10
Therapeutic potential of medicinal marijuana: an educational primer for health care professionals
Authors Mouhamed Y , Vishnyakov A, Qorri B , Sambi M, Frank SMS , Nowierski C, Lamba A, Bhatti U, Szewczuk MR
Received 16 January 2018
Accepted for publication 30 April 2018
Published 11 June 2018 Volume 2018:10 Pages 45—66
DOI https://doi.org/10.2147/DHPS.S158592
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Rajender R Aparasu
Yara Mouhamed,1,* Andrey Vishnyakov,1,* Bessi Qorri,2,* Manpreet Sambi,2,* SM Signy Frank,1 Catherine Nowierski,1 Anmol Lamba,1 Umrao Bhatti,1 Myron R Szewczuk2
1Graduate Diploma & Professional Master in Medical Sciences, School of Medicine, Queen’s University, Kingston, ON, Canada; 2Department of Biomedical and Molecular Sciences, Queen’s University, Kingston, ON, Canada
*These authors contributed equally to this work
Abstract: With the proposed Canadian July 2018 legalization of marijuana through the Cannabis Act, a thorough critical analysis of the current trials on the efficacy of medicinal marijuana (MM) as a treatment option is necessary. This review is particularly important for primary care physicians whose patients may be interested in using MM as an alternative therapy. In response to increased interest in MM, Health Canada released a document in 2013 for general practitioners (GPs) as an educational tool on the efficacy of MM in treating some chronic and acute conditions. Although additional studies have filled in some of the gaps since the release of the Health Canada document, conflicting and inconclusive results continue to pose a challenge for physicians. This review aims to supplement the Health Canada document by providing physicians with a critical yet concise update on the recent advancements made regarding the efficacy of MM as a potential therapeutic option. An update to the literature of 2013 is important given the upcoming changes in legislation on the use of marijuana. Also, we briefly highlight the current recommendations provided by Canadian medical colleges on the parameters that need to be considered prior to authorizing MM use, routes of administration as well as a general overview of the endocannabinoid system as it pertains to cannabis. Lastly, we outline the appropriate medical conditions for which the authorization of MM may present as a practical alternative option in improving patient outcomes as well as individual considerations of which GPs should be mindful. The purpose of this paper is to offer physicians an educational tool that provides a necessary, evidence-based analysis of the therapeutic potential of MM and to ensure physicians are making decisions on the therapeutic use of MM in good faith.
Keywords: medicinal marijuana, cannabis, endocannabinoid system, Cannabis Act, multiple sclerosis, Parkinson’s disease, Tourette’s syndrome, gastrointestinal disorders, pregnancy, epilepsy, Access to Cannabis for Medical Purposes Regulations
Introduction
In Canada, marijuana or cannabis (used interchangeably hereafter) has been used recreationally and medicinally for generations but was first legally available as medicinal marijuana (MM) in 2001 through the Medical Marijuana Access Regulations.1 In its most recent form, the Access to Cannabis for Medical Purposes Regulations states that physicians have the responsibility of authorizing patients to access MM.2,3 Health Canada and the provincial medical colleges have published guidelines for physicians to follow and approve MM for their patient’s safety.4 Despite these guidelines, physicians remain uncomfortable authorizing MM due to a lack of evidence-based literature and the perceived lack of education surrounding the subject.5–7 Many physicians feel that a robust understanding of cannabis would increase their comfort with MM.6,7 The basis of this knowledge is particularly relevant for a large demographic of the population presenting with chronic conditions that have reported to be self-medicating with marijuana where conventional therapies have failed in improving the overall quality of life (QOL).7
Therefore, this review aims to serve as an educational tool that provides relevant information of which physicians must be mindful when authorizing MM. The information is primarily appropriate due to the expected increase in use following the proposed legalization of marijuana for recreational purposes by July 2018 through the Cannabis Act. Here, we provide a summary of the basic science behind cannabis and the endocannabinoid system, as well as the current Canadian laws and authorization guidelines for MM. We simplify and analyze new literature that has emerged since the 2013 release of the Canadian medical marijuana guidelines, delineate therapeutic uses of cannabis and its contraindications and outline gaps present in the current literature. We ultimately hope that this succinct review provides physicians with the necessary resources required for MM-related decision-making and improves the general practitioner’s level of comfort with MM and their capacity to attend to such patients.
Methods
This literature search identified articles using PubMed, EMBASE Ovid, and the Cochrane Library to determine high-quality, multicenter randomized controlled trials, systematic reviews, meta-analyses, and practice guidelines from February 2013 to August 2017. The assessment of the therapeutic potential of MM allowed in the identification of gaps including conflicting and inconclusive results in our knowledge since the release of the 2013 Health Canada guidelines that may pose a challenge for physicians. This review aims to supplement the Health Canada document by providing physicians with a critical yet concise update on the recent advancements for the prescribed use of MM. This paper presents an overview of previously published reviews and, as such, requires no ethics approval.
Canadian medical regulatory authorities’ policies and guidelines
Although the Cannabis Act is currently on track to its projected enactment taking place in July 2018, some challenges regarding MM use that are not addressed by the 2013 Health Canada guidelines remain. Specifically, under the ACMPR,2 physicians are required to sign a medical document to authorize patients to access a specific quantity of cannabis. This medical report resembles a prescription; however, unlike all other prescribed medications, Health Canada has not reviewed data on the safety or efficacy of MM.
In light of the scarcity of data available to physicians, the medical regulatory authorities (colleges) have recently implemented policies on MM to assist physicians in making informed decisions that are most beneficial for their patients.8–16 Current guidelines and policies issued to date by these colleges repeatedly state that physicians should only sign the medical document if they have the necessary clinical knowledge; furthermore, physicians are not obligated to prescribe marijuana if they do not believe it is clinically appropriate for their patients.17 Collectively, the colleges agree that MM is not appropriate in a number of circumstances including for patients under the age of 25 years, have a current or past substance use disorder, have personal or family history of mental illness (psychosis), have a history of chronic lung, cardiovascular, and/or kidney disease, and who are pregnant or breastfeeding. Moreover, all colleges recommend that informed consent should be obtained from patients before authorizing MM.8–16 During this process, physicians must discuss the risks and benefits of MM with their patients, including the necessary precautions that patients need to take when engaging in activities requiring mental alertness such as driving and operation of heavy machinery.
While the rules and restrictions that govern the authorization of MM may be challenging to interpret, determining the safe therapeutic dose for each patient will present a more significant challenge for physicians. Therefore, all colleges advise physicians to proceed cautiously where patients “start low and go slow” until a dose is reached that achieves symptom management while causing minimal euphoria or cognitive impairment.18–20 To ensure that these expectations are met, physicians must specify the quantity of marijuana to be dispensed to the patients as well as the (-)-∆9-trans-(6aR,10aR)-tetrahydrocannabinol (∆9-THC or THC) content (the relevance of this is discussed below) on every medical document. Furthermore, most colleges recommend that physicians follow up with their patients every 3 months to monitor for any emerging complications or risks of abuse, misuse, or diversion, even though the authorization of medical cannabis is valid for up to 1 year. To minimize risks, some medical regulatory authorities such as the Colleges of Physicians and Surgeons in Ontario, Saskatchewan, and Quebec require physicians to obtain a signed written treatment agreement from their patients before MM authorization.8,10,11 This agreement must contain a statement from patients that they will not seek marijuana from another physician or any other source, will only use marijuana as prescribed, will store their marijuana safely and securely, and will not sell or give away their marijuana. Additional province-specific details can be found in Table S1.
Brief overview of the mechanisms of action of MM
Given the pending legalization of MM for recreational purposes through the enactment of the Cannabis Act, it is important for family physicians to understand the underlying effects of cannabis. This statute is to provide legal access to marijuana and to control and regulate its production, distribution, and sale.
The endocannabinoid system and MM
The endocannabinoid system is a naturally occurring communication network that plays a role in many physiological processes.21 Currently, this system has been found to be implicated in gastrointestinal (GI) function,22 appetite and metabolism,23–25 pain,26,27 memory,28 movement,29 immunity,30 and inflammation.31 The endocannabinoid system comprises two G-protein-coupled receptors (GPCRs): cannabinoid receptors 1 (CB1) and 2 (CB2).32,33 CB1 possesses psychoactive potential and is expressed in the central nervous system (CNS), Gastrointestinal (GI) system, adipocytes, liver tissue, and skeletal muscle.32,34,35 In contrast, CB2 receptors are more restricted in their distribution and are primarily found on immune cells located in the tonsils, thymus, spleen, and bone marrow,32,34,35 as well as in the enteric nervous system within the GI tract.36 Activation of these receptors is dependent on endogenous endocannabinoids anandamide (AEA) and 2-arachidonoylglycerol (2-AG).37,38
Due to its abundance in the body, particularly in the nervous system, CB1 and its subsequent psychoactive effects have been extensively studied. As illustrated in Figure 1, cannabinoid binding regulates presynaptic Ca++ levels generally leading to a reduced release of neurotransmitters. This mechanism plays an essential role in maintaining homeostasis, thereby implicating this system in several physiological and pathological conditions that have been previously reported in detail.39
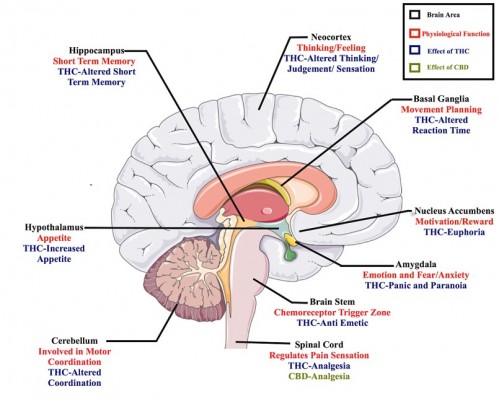
The medicinal properties of cannabis can be attributed primarily to phytocannabinoids ∆9-THC or THC and cannabidiol (CBD).40–42 THC and CBD are the most biologically active phytocannabinoids and are capable of mimicking human endocannabinoids AEA and 2-AG, respectively.40–42 ∆9-THC has been shown to bind to CB1 in the nervous system,21 and the effects of THC on the CNS and peripheral body are outlined in Figure 2 and Table 1, respectively.
  | Table 1 Specific effects of THC in the peripheral system Abbreviations: THC, (-)-∆9-trans-(6aR,10aR)-tetrahydrocannabinol; GIT, gastrointestinal tract. |
In contrast, non-psychoactive CBD has high binding affinity to the CB2 receptor and exerts its effects on the immune system, resulting in its application for the treatment and management of neuropathic pain.43 However, conflicting reports suggest that CBD indirectly mediates its effects by interacting with CB1 and CB2, the mechanism(s) of which is not well understood.44 Given this inconclusive information, it is omitted from Table 1.
The potency of the mediating effects of THC on the endocannabinoid system depends on several factors that need to be considered before prescribing its use for treatment. In the unprocessed form, ∆9-THC and CBD concentrations depend on the species, strain, cultivation, and storage of the plant.45,46 Of the three species of cannabis identified (Cannabis sativa, C. sativa, C. indica, and C. ruderalis), C. sativa contains higher THC than CBD levels while the C. indica is richer in CBD compared to THC.47 CBD attenuating the psychotropic actions of ∆9-THC on the body is thought to be due to affecting ∆9-THC metabolism and inhibiting the formation of 11-OH-THC, its more psychoactive metabolite.47–49 To summarize, a higher THC:CBD ratio is associated with more prominent psychoactive symptoms, whereas lower THC:CBD ratio suppresses psychoactive symptoms and has more sedative and relaxing effects.50 Due to the varying effects of MM, pharmacokinetics is another critical aspect that physicians need to consider before authorizing the use of MM.
Pharmacokinetics of MM
In addition to understanding the effects of phytocannabinoids on the endocannabinoid system, physicians should be mindful of the chemical composition and available routes of administration if considering the authorization of MM. Phytocannabinoids are lipophilic and require heat for activation, as accomplished through both the inhalation routes of administration.51–53 The course of administration also determines the absorption and metabolism of phytocannabinoids. The currently available routes of administration of cannabinoids are discussed as follows, with the most common forms summarized in detail in Table 2.
Inhalation: smoking or vaporization
Inhalation is the most commonly used route of administration with the quickest onset of action54 and shortest duration,55 giving patients the capacity to titrate their dose through adaptive smoking behavior. Of the two inhalation options, vaporization is more discreet and has fewer toxic by-products,56,57 while inhalation is an appropriate option for patients requiring rapid relief for a shorter duration.
Oral
Oral cannabinoid administration offers a longer duration and a slower onset of action compared to inhalation, making titration challenging for patients attempting to achieve desired effects. Cannabinoids administered through the oral route can be taken as pills, such as nabilone (Cesamet®) and dronabinol (Marinol®) (which is no longer available in Canada), or mixed in with foods such as butter, oils, or teas. Administration of oral cannabis can be presented as a potential option for individuals in need of relief of symptoms such as chronic pain, arthritis, movement disorders, and select psychiatric disorders. At this time, there is no robust evidence to support cannabis as a treatment for any psychiatric disorders. The cannabis trials for acute anxiety, schizophrenia, and posttraumatic stress disorder (PTSD) are rather still preliminary, and cannabis is not standard of care treatment for any mental illness at this time.
Oromucosal
Oromucosal cannabinoid administration offers a balance between speed of onset and duration of action when compared to inhalation and oral routes. Nabiximol is currently the only oromucosal product approved for prescription, containing a combination of ∆9-THC and CBD in spray form allowing simple self-titration. Oromucosal cannabinoid administration is recommended for the symptomatic relief of spasticity in adults with multiple sclerosis (MS) but may also be a good option for patients in need of rapid relief for longer durations, such as in neuropathic pain.
Rectal
The rectal route of cannabinoid administration, though uncommon, has been shown to be efficacious in patients presenting with chemotherapy-related nausea and emesis.58 ∆9-THC-hemisuccinate, a prodrug, is delivered as opposed to ∆9-THC because it is quickly absorbed, having a higher bioavailability than oral administration. Although rectal products are currently unavailable in Canada, they may be of future interest for patients unable to tolerate oral medications, for the pediatric population, for palliative use, and for patients unable to take oral medication or via inhalation.
Topical
Topical cannabinoid administration has been considered as a treatment for glaucoma.59 However, due to its high lipophilicity, transport of ∆9-THC across aqueous layers in the body is a rate-limiting step55 but can be overcome through the use of ∆9-THC prodrugs resulting in improved penetration into the anterior eye, reducing intraocular pressure.59
Metabolism, excretion, and long-term detection of THC
The metabolism and excretion of cannabinoids are highly regulated and affect many other metabolic processes that need to be considered if advising the medicinal use of cannabis. In brief, cannabinoids are mainly metabolized in liver by the cytochrome P450 (CYP 450) enzymes.60 Once absorbed, ~97% of ∆9-THC and its metabolites bind to plasma proteins61–63 and are incorporated into fatty tissue and highly perfused organs, such as heart, brain, lungs, and liver,55 with the majority of ∆9-THC accumulating in cardiac and fat tissues.64 Cannabinoids and their metabolites that are not absorbed are excreted in feces (65%) and, to a lesser extent, in urine (20%).55 Given the complex processes involved in the metabolism and excretion of THC in addition to the prolonged detection of THC, it is essential to consider the underlying drug interactions and subsequent effects on patients presenting with additional chronic conditions.
Therapeutic options applicable for the authorization of MM use
As previously discussed, many physicians feel uncomfortable with authorizing MM use due to a lack of educational resources available. Although Health Canada released “Information for Healthcare Professionals, Cannabis (Marihuana, Marijuana) and the Cannabinoids” in February 2013 to educate health care professionals on cannabis, physicians continue to be apprehensive about recommending cannabis as a treatment option for patients who present with chronic conditions. A detailed summary of the Health Canada document can be found in Table S2. Updated evidence-based recommendations and short critical analyses on MM use for various chronic conditions are discussed below.
Multiple sclerosis
MS is a chronic inflammatory, demyelinating autoimmune disease of the CNS.65 Current therapies decrease additional MS attacks and delay progression but are unsuccessful in improving patient QOL.66 Patients with MS often seek psychoactive drugs to cope with their disabilities, with numerous studies showing increased rates of recreational and MM use in patients experiencing spasticity.67–69 In light of this, it is critical for primary care physicians to make educated assessments when deciding whether to authorize MM as a therapeutic option.
Recent studies on the use of MM in MS suggest that cannabinoid use is associated with improvements in spasticity, but they fail to show statistical significance.70–80 Nevertheless, clinical significance was observed where patients reported a subjective sense of a reduction in spasticity-related symptoms. Many observational open-labeled studies reported promising data on the role of cannabinoids in the treatment of MS in clinical practice.75–80 Overall, cannabinoids appear to be a well-tolerated add-on treatment associated with a more significant average improvement on the Ashworth Scale ( is a measure of spasticity, as indicated by the amount of resistance encountered during passive stretching of soft-tissue, and the Modified Ashworth Scale (MAS) has an additional scoring category) or spasticity compared to placebo, although not statistically significant. However, there are conflicting studies that failed to demonstrate statistical significance in the efficacy of MM on the progression of MS after use for 36 months (95% CI, 2.0–0.2).71,72 Similarly, a study investigating the time to treatment failure and maintenance efficacy, an oromucosal spray which has an equal (1:1) ratio of THC:CBD (Sativex®), as an add-on treatment in the management of central neuropathic pain revealed conflicting results in the long-term efficacy maintenance of this treatment option.70 The primary endpoint of time to treatment failure was statistically significant (P=0.04) in favor of THC:CBD spray, where 57% of the placebo group failed treatment, compared to only 24% of the THC:CBD group.
There is a scientific rationale for the role of MM in MS based on the understanding of the endocannabinoid system as well as improvements in subjective assessments of spasticity and other related symptoms. However, there is residual uncertainty about whether the effects of cannabinoids are real. These results may not be detected by “objective” outcome measures like the Ashworth scale, or if the perceived consequences are owing to the general psychoactive effect of THC on the CNS. Furthermore, although there were some promising findings in the Health Canada document, the fact remains that adverse effects of cannabis on cognition in people with MS does occur, as changes in cognitive function affects 40%–60% of patients with MS.81 Therefore, changes in cognitive function should be appropriately monitored in individuals who begin a cannabis regimen. In addition, new clinical trials should explore other objective modalities such as the stretch reflex test which has demonstrated a statistically significant reduction in stretch reflex amplitude as well as statistically significant reductions in numeric rating scale (NRS) and MAS scores in assessing the improvement of MS-related spacticity.74
Although there are indications that MM is effective in reducing patient-reported symptoms such as spasticity and pain, studies also show that cannabinoids have no proven overall effect on the progression of MS.71,72 Additional research on the long-term outcomes of MM in MS patients is required.
Epilepsy
As with MS patients who do not see an improvement in QOL following treatment, approximately one third of epileptic patients fail to respond to currently available antiepileptic drugs fully. Patients with treatment-resistant epilepsy have a higher prevalence of comorbidities,82,83 psychosocial and cognitive problems,84 negative public attitudes,82,83 decreased QOL and increased risk of mortality.85–87 According to the 2013 Health Canada document on cannabinoids, the action of cannabinoid THC was too broad for therapeutic purposes, and there was insufficient evidence on CBD4 to recommend MM as a potential treatment option for patients with epilepsy.
We identified five new trials published since 2013 investigating the therapeutic potential of CBD in the treatment of drug-resistant epilepsy in children or young adults failing to respond to conventional anticonvulsive medications.88–92 In addition to being administered CBD, these participants also continued their anticonvulsant drug regimen, most commonly clobazam (marketed under the brand names Frisium, Urbanol, Onfi, and Tapclob) and valproates, for the duration of the trials. Partial and atonic seizures had the most significant reduction in frequency followed by tonic and tonic–clonic seizures. CBD has shown some promise as a potential medical alternative in the treatment of drug-resistant epilepsy with minimal side effects. Based on the high-quality multicentered randomized controlled trials (RCTs) enrolling hundreds of patients to date,90,92,93 there is evidence that CBD is effective on Lennox Gastaut, Dravet syndrome, and other types of childhood treatment-resistant epilepsy. In one study, a wide range of CBD is administered (from 0.5 to 50 mg/kg/day) with no correlation to the amount administered and adverse events.90 Also, the mechanism(s) behind CBD therapy in the treatment of drug-resistant epilepsy is not well understood; thus, elucidating the pathway(s) of action is required to develop a more targeted treatment. Since CBD most potently inhibited the catalytic activity of human CYP3A4 and CYP3A5,94,95 co administered anticonvulsant medication needs to be monitored and adjusted on a regular basis.
Movement disorders
Given the location of cannabis receptors in the CNS, the scientific rationale for the use of MM to alleviate the symptoms associated with movement disorders is perhaps not surprising. Although several disorders could be considered, the therapeutic value of MM has only been investigated in Parkinson’s disease (PD) and Tourette’s syndrome (TS).96
Parkinson’s Disease
PD is the second most common neurological illness in Canada following Alzheimer’s disease 97 and is characterized by the loss of nigrostriatal dopamine neurons leading to a tetrad of tremors, bradykinesia, rigidity, and postural instability.98 Levodopa that replaces dopamine to improve motor symptoms is the current medication for PD, but fails to improve QOL, and is associated with many adverse effects such as dyskinesia.98 Given the increasing evidence that suggests a prominent modulatory function of the endocannabinoids in the basal ganglia, the use of cannabinoids as a new therapeutic target has been recommended as a promising therapy for PD as well as for levodopa-induced dyskinesia.99
In a double-blind clinical trial,100 PD patients without dementia or comorbid psychiatric conditions were assigned to one of three groups: placebo, CBD 75 mg/day, and CBD 300 mg/day. There were no statistically significant differences in motor symptoms, neuroprotective effects, or magnetic resonance spectroscopy measures between the three groups; however, the 300 mg/day CBD group had a significantly different mean total score in well-being and QOL (P=0.05) compared to placebo, suggesting a possible effect of CBD in improving QOL in PD patients. In two open-label observational studies101,102, PD patients demonstrated statistically significant improvements in their United Parkinson’s Disease Rating Scale (P<0.001), tremor (P<0.001), rigidity (P=0.004), and bradykinesia (P<0.001). They also demonstrated significant improvement in their sleep and pain scores just 30 minutes after smoking cannabis. Moreover, a case-series study that treated four PD patients suffering from “random eye movement” sleep behavior disorder (RBD) with 75–300 mg/day of CBD found that patients had a prompt and substantial reduction in the frequency of RBD-related events without side effects.103
More extensive, controlled, randomized, and blinded clinical trials are required to better assess the role of cannabinoids in the treatment of PD and levodopa-associated dyskinesia, as small sample size and variability in study design limit our ability to draw definitive conclusions. Additional research is required to determine whether subsets of individuals with various neurological and psychiatric diseases derive the same therapeutic benefits from cannabis. However, these studies collectively demonstrate that marijuana plays a role in improving QOL measures in PD, with further studies being required to elucidate the exact effects/mechanisms of action.
Tourette’s Syndrome
TS is a common neurobehavioral disorder characterized by multiple motor and phonic tics, generally starting in childhood.104 There are a substantial number of TS patients who are unsatisfied with the current treatment strategies due to either minimal efficacy or significant adverse effects.105 Moreover, there is a lack of medications effective against both behavioral disorders and the tics associated with TS, resulting in many TS patients seeking alternative or complementary treatments including special diets, nutritional supplements, and drugs such as nicotine, alcohol, and C. sativa to alleviate their symptoms.106 Therefore, it is exceedingly important for physicians to understand the efficacy of MM when advising patients on alternate treatment options.
According to Health Canada,18 anecdotal and case reports have suggested an improvement in symptoms associated with TS when smoking cannabis. The Health Canada document also cites two small RCTs that assessed the effects of short duration. To our knowledge since then, there have been no recent clinical trials that study the role of MM in TS except for two case reports, both investigating the role of Sativex® in the treatment of TS. In the first study,107 the patient received 10.8 mg THS and 10 mg CBD daily, in the form of two oromucosal sprays of Sativex®, twice daily. In the second case report,108 the patient started on at a dose of 1 puff per day and slowly increased up to a dosage of 3×3 puffs per day. Both the studies demonstrated a significant reduction in motor and vocal tic severity and frequency following MM treatment. Moreover, the second case report showed a substantial improvement in the QOL associated with MM treatment. More extensive clinical trials studying the effects of MM on alleviating TS symptoms are required for physicians to comfortably decide whether the use of MM would be an appropriate alternative option.
GI disorders
The endocannabinoid system is vastly integrated within the GI tract, particularly within the enteric nervous system.109 A high expression of CB1 on epithelial cells, submucosal neurons, and myenteric neurons and elevated expression of CB2 on immune cells within the GI tract suggest that there is a therapeutic rationale for MM use as treatment options for patients with GI disorders. 110,111
Inflammatory bowel disease
Inflammatory bowel disease (IBD) includes Crohn’s disease (CD) and Ulcerative Colitis (UC), causing inflammation of the bowel.112 Significant morbidity occurs in IBD patients whose symptoms are uncontrolled by conventional therapies. Trials reported in Health Canada’s document demonstrated that cannabinoids might attenuate intestinal inflammation and symptoms of IBD in animal models through the activation of cannabinoid receptors in the GI tract.4 Although cannabis could be used in the treatment of refractory IBD, clinical data did not show a strong association between cannabis and symptom relief in IBD patients.
A significant portion of self-medicating IBD patients found cannabinoids helpful for symptoms such as abdominal pain,113–115 poor appetite,113,114 nausea,113,114 diarrhea,113–115 and joint pain.115 It was also found that CD patients were more likely to be cannabis users compared to those with UC and IC.114 RCT set out to examine the therapeutic effects of smoked cannabis,116 and the effects of CBD in treatment-refractory CD,116 as defined by the Crohn Disease Activity Index score.117 While these reports initially demonstrated that THC was involved, the role of CBD was unclear. Furthermore, anecdotal data focused on the positive effects of cannabis use in the treatment of IBD, making it challenging to conclude the therapeutic efficacy of such compounds as treatment options. Due to the small sample sizes and the short course marked differences in the dose administered (115 mg ∆9-THC/negligible CBD and 10 mg CBD twice a day, respectively), there remains a lack of reliable clinical evidence to support the use of MM in the treatment of IBD. A concerning finding was the correlation between long-term cannabis use and increased rate of surgical procedures in IBD patients,115 with cannabis use potentially masking disease activity leading to worsened disease outcomes. Future studies should focus on more substantial double-blinded RCTs to assess the efficiency and safety of MM treatment in IBD patients, focusing on optimal routes of administration and dosing.
Anorexia
Anorexia is often associated with a variety of chronic illnesses such as Anorexia Nervosa (AN), HIV infection, and cancer.118 Health Canada’s 2013 document reported several promising findings on the use of MM as an alternative agent for patients presenting with anorexia as a result of HIV infection. Specifically, patients with HIV who were administered non-dronabinol were reported to have a statistically significant increase in caloric intake compared to placebo, particularly in patients with substantial cachexia.119 Furthermore, most public anorexia trials published in the Health Canada document,4 as well as one of two new trials we found published since,120 have used dronabinol, a synthetic Δ9-THC compound that is no longer available in Canada. Theoretically, dronabinol studies may be applied to other forms of THC; however, the dosing, side effects, long- and short-term safety, and comparative efficacy against placebo or other appetite stimulants may differ among different formulations.
Since the Health Canada document, there have been only two ongoing trials using cannabinoids in anorexia, both in the context of cancer. A pilot study out of Israel is currently analyzing the use of “Cannabis Capsules” (THC extract) for cancer-related anorexia.121 The second trial, a randomized double-blinded study in Mexico, is looking at the effect of nabilone as an appetite stimulant in terminal lung-cancer patients.122 Both the trials may have future utility as they offer alternatives to dronabinol and new evidence in a cancer population. However, despite the potential of MM as a therapeutic option, the fact remains that there is little-to-no clinical trial evidence guiding the use of non-dronabinol cannabinoids in anorexia. For future trials, we suggest the use of available THC sources and incorporate cannabis naïve populations or use comparison against other appetite stimulants as opposed to placebo. With these tenets in mind, evidence can guide the use of cannabinoids in anorexia and potentially improve patient outcomes.
Nausea and vomiting
According to the Health Canada document, nabilone, dronabinol, and levonantradol perform significantly better than placebo and slightly better than conventional dopamine D2-receptor antagonist anti-emetics in suppressing chemotherapy-induced nausea and vomiting (CINV).4 Ondansetron and dronabinol provided same relief of CINV, but there was no additive benefit.4 The Δ9-THC capsule had an equivalent effect to smoked cannabis. Although cannabinoids were associated with higher incidence of adverse events such as dizziness, dysphoria, euphoria, and sedation, some participants expressed a preference for cannabinoids over other antiemetics. There is still limited information on the relative efficacy of cannabinoids over the newer antiemetics such as 5-HT3 (ondansetron and granisetron) or neurokinin-1 receptor antagonists.
Two placebo-controlled trials on the effect of cannabinoids on postoperative nausea and vomiting were identified. Participants have been pretreated with 0.5 mg nabilone before surgery,123 or administered 0.125 mg/kg THC intravenously at the end of surgery.124 There was no significant difference in nausea and vomiting reduction between cannabinoids and placebo groups in both the trials, and clinically relevant psychotropic THC side effects such as sedation and confusion that were deemed unacceptable were reported.124 Therefore, while chemotherapy patients should be aware of cannabinoids as an alternative treatment of CINV, the side effects have been deemed unacceptable in the outpatient and acute settings.
Pain
The endocannabinoid system is a critical endogenous pain control system27,125, as such, the targeting of this system with cannabis may provide a therapeutic advantage in the treatment of pain.125 This system is present throughout several pain pathways, with cannabinoid receptor agonists demonstrating antinociceptive effects in animal models of acute, inflammatory, and neuropathic pain. The modulation of pain is thought to be due to inhibition of presynaptic neurotransmitter release and modulation of postsynaptic excitability.39,126
Acute pain
The Health Canada document presented mixed results in the efficacy of cannabinoids in acute, experimentally induced pain.4 The variety of administration modes, such as nabiximol, smoked cannabis, and oral THC, as well as small sample sizes may explain this inconsistent result.4 Since 2013, there has been one randomized, placebo-controlled, double-blind clinical trial on this subject, finding that smoked marijuana and dronabinol decreased pain sensitivity (3.56% THC, 20 mg, respectively) and increased pain tolerance (1.98% THC, 20 mg, respectively) when compared against placebo.127 However, the small sample size (N=30), exclusion of naïve users, including only THC content, and use of dronabinol necessitate further research before commenting on the efficacy of cannabis in the treatment of acute pain.
Chronic neuropathic pain
Neuropathic pain is a complex, chronic pain state that affects over 2 million Canadians,128,129 with half of the sufferers failing to achieve adequate relief.130,131 In 2015, the Canadian Pain Society updated their guidelines for the management of neuropathic pain moving cannabis from the fourth- to a third-line medication.132 In recognition of the growing body of evidence, the 2013 Health Canada document also indicated that the addition of cannabinoid medications to conventional therapy was a moderately active short-term treatment of neuropathic pain.4 However, additional research needs to be done examining modes of administration further to inhalation, as well as the use of non-dronabinol to maintain consistency with currently available medications.
Since the publication of the document, 10 relevant studies were published about cannabinoids in neuropathic pain (see Table S3 for a detailed summary of trial data).130,131,133–140 These studies addressed several gaps present in the Health Canada document including examining both THC131,136–138,140 and THC/CBD blends at various concentrations and routes of administration,130,135,139 such as oral tablets,137,138 oromucosal spray,130,135,139 vaporizing,131,136 and metered-dose inhaler.140 Specifically, two studies examined the mode of action of cannabinoids in neuropathic pain by using functional magnetic resonance imaging (fMRI), demonstrating that THC may act on the active qualities of chronic pain by reducing sensory limbic functional connectivity between the amygdala and the primary somatosensory cortex.133,134 Also, three long-term trials demonstrated long-term efficacy, safety, and tolerability.130,138,139 Lastly, in the remaining eight studies, six studies were blinded, randomized-controlled trials130,131,135–138 and two were open-label trials,139,140 all of which had differing experimental designs. They unanimously demonstrated statistical significance in at least one or more measurements of neuropathic pain, including some responders with 30% reduction in pain, visual analog scale, and (NRS).130,131,135–140 These data have strengthened the evidence for the use of cannabinoids as adjuvant therapy in chronic neuropathic pain; however, gaps remain that need to be addressed in future research, such as the use of other cannabinoids, terpenes, and additional investigations regarding modes of administration. Nonetheless, these gaps should not prevent health care professionals from using marijuana and its analogs to combat neuropathic pain.
Chronic non-cancer-related pain
Health Canada initially grouped chronic non-cancer pain with neuropathic pain; however, we believe that chronic non-cancer pain best fits into its category. Four trials found that causes of pain included functional chest pain,141 chronic pancreatitis-related pain,142 chronic abdominal pain,143 and unspecified chronic non-cancer pain.144 Each trial examined a different cause of pain, and the results were inconsistent with the neuropathic pain trials regarding efficacy. This contradiction of the findings creates a need for each case to be examined individually to determine the effectiveness and is the main reason for the separation of the data from the neuropathic pain section. The results of each trial have been summarized and included in Table S3.
Cancer-related pain
In Canada, it is estimated that in 2017 there will be over 200,000 newly diagnosed cancer patients.145 Because pain is the most commonly experienced symptom by cancer patients,146 Health Canada reviewed the therapeutic efficacy of dronabinol and nabiximols in the management of cancer-related pain and found them to be efficacious in providing relief, although not all results were statistically significant.4 However, trials with larger sample sizes investigating alternative modes of administration of cannabinoids are required to comment on the efficacy of cannabis in cancer conclusively.
Since 2013, three studies have been published regarding cannabis use in cancer pain. An observational study demonstrated that 70% of patients who were prescribed marijuana for pain management reported subjective improvement in their pain control.5 Similarly, an open-label extension study on the long-term efficacy and safety of Sativex spray reported a decrease from the mean baseline pain of 0.63 (P=0.014) in THC/CBD spray group versus placebo.147 To further confirm these results, an extension of this study demonstrated a decrease in mean Brief Pain Inventory Short Form (BPI-SF) scores for pain, severity, worst pain, and pain interference domains with the THC/CBD spray.147 Unfortunately, this study had a significant dropout rate (42/43 patients), with almost half citing adverse events as the reason for leaving the study, suggesting that the harmful effects may outweigh the benefits of cannabinoid use in cancer.147 Finally, a blinded RCT study examining nabilone in head and neck cancers determined that there was no difference in pain between intervention and placebo groups (P=0.6048) and that nabilone did not alter the time required for progression of illness by 20% (P=0.46).148
The study results, excluding the observational questionnaire, are in contrast to the trials analyzed in the Health Canada document and may be attributed to small sample sizes and significant dropout rates. Given the quality of the evidence reviewed, it can be concluded that these studies have not significantly added to the current knowledge on treatment of pain in cancer, and thus more research will be needed to clarify this. Future blinded RCT studies on the role of cannabis in the treatment of cancer pain should include examining a variety of modes of administration in large patient populations and examining both short-term and long-term efficacy and safety profiles of cannabis products.
Headaches
Since the Health Canada review, many survey studies,149–152 and a chart review153 have studied the therapeutic efficacy of MM in the treatment of headaches, however only one controlled clinical trial was conducted.154 In this trial, nabilone (0.5 mg) was used in a randomized, double-blind, crossover design against ibuprofen (400 mg) in 30 patients with a medication-overuse headache (MOH) and daily analgesic intake. Primary outcome measures included headache frequency, daily analgesic intake, pain intensity and duration, level of dependence, and pain-free days. While both the drugs resulted in statistically significant improvement in all primary outcomes, nabilone was superior to ibuprofen (greater effect size) in all parameters. In addition, subgroup analyses showed that patients who received ibuprofen in the second half of the study (crossing over from nabilone) did not demonstrate ibuprofen-associated improvements seen in the overall data. Furthermore, these patients did not experience continued improvement 2 weeks following the study endpoint, unlike patients who received nabilone following treatment with ibuprofen. This methodologically sound study makes a compelling case for the efficacy of nabilone compared to ibuprofen in the MOH population but is limited by a small sample size, patient dropout (four of 30 patients), missing controls for cannabis-experienced or naïve patients, and a lack of a psychoactive placebo (affecting patient blinding). However, given the subjective nature of pain, the psychoactive effects of cannabinoids may be considered a new part of the therapeutic profile of cannabis if they affect the perception of pain.
Special considerations
Although there are some promising therapeutic applications of MM in the treatment of several conditions outlined above, a thorough understanding of patient history and specific patient subpopulations presenting with other states should be considered. These contradictions are outlined in detail below.
Mental health
According to the 2013 Health Canada report,4 there was a dose–response relationship between cannabis use and the risk of psychotic disorders. Early exposure and greater use were linked to initial symptom onset, particularly in those predisposed to mental illness. Furthermore, cannabis use after the first psychotic episode or schizophrenia diagnosis was associated with weak prognostic features, such as multiple relapses and worse symptoms.
Since the Health Canada report, literature has confirmed a dose-dependent relationship between cannabis use and the risk of psychotic disorders.155–157 Early exposure (ie, before the age of 15 years158,159 or during adolescence160), greater use,158–160 and escalation to daily use160 have all been linked to an earlier initial psychotic episode relative to nonusers. Specifically, patients with a history of cannabis use experienced their first psychotic episode from 2.6161 to 2.9 years earlier than nonusers.162 This information is particularly relevant for individuals at a higher risk for psychiatric illness, with predictive factors for conversion to psychotic disorders including psychotic features with cannabis use,159 high potency cannabis, and high frequency of use.158,163 Furthermore, studies on the effects of other substances in attenuating the relationship between cannabis use and mental health outcomes seem to be insignificant.164,165 In addition, these materials were not significant predictors of psychosis onset,158,159,163 which could be due to the relatively low rate of other substance abuse.
Schizophrenia
Patients with schizophrenia have been found to be ~10 times more likely to use cannabis than the general population.166,167 For schizophrenia, there is early evidence that CBD may be a helpful treatment, while THC seems to worsen psychosis. Eight recent correlational studies not included in Health Canada Report investigated the effects of marijuana on schizophrenia severity, including positive and negative symptoms and level of function. However, it is noteworthy to mention that these studies are meant to provide information on patients with psychosis who use recreational cannabis and are not treatment studies. Across all reviewed studies, cannabis use had no significant effect on negative symptoms based on the Positive and Negative Syndrome Scale (PANSS).157,168–174 Some studies reported an increased prevalence of positive symptoms with cannabis use (PANSS-P),157,172,173 while others reported no significant effect.168–171 In a meta-analysis, history of or current cannabis use had a moderate effect on positive symptoms when compared to cannabis naïve participants.174 However, due to the high heterogeneity between the included studies, we advise interpreting results with caution.
Lastly, there was no significant difference between cannabis users and nonusers in the ability to adapt to various problems-in-living, based on the Global Assessment of Functioning (GAF) scale.157,169–173 It is possible that an upper limit on the safe quantity of cannabis exists after which GAF declines. During a follow-up period, a change in cannabis use, whether escalation or de-escalation, exhibited a reverse relationship with GAF.157,170,171 The change indicates that the effects of cannabis were reversible and corresponded to the amount used. As an alternative, there could have been confounding variables that were not accountable. Overall, these findings imply that not all people are affected equally by cannabis and that physicians should advocate against heavy and early cannabis use.
Treatment adherence
The majority of studies did not control for treatment adherence, which is an important confounding variable, as current cannabis users are less likely to adhere to psychiatric medical therapy than nonusers and former users by a factor of 4.8 and 4.5, respectively.175 High potency (defined as a high ratio of THC:CBD), cannabis being particularly noxious, is a statistically better predictor of nonadherence than low potency or infrequent use.176 Nonadherence to medical treatment is a significant risk for clinical and psychosocial remission.177 Nonadherence can also partially confound the effect of cannabis use on the risk of relapse, some relapses, time until relapse, and care intensity.178 Future studies need to control for a wide array of confounding variables including treatment adherence, other substance use, and baseline differences.
Cognition
People with psychotic illness develop a more significant decline in their cognitive abilities relative to other mood disorders.179 We identified seven recent articles that addressed the relationship between cannabis use and cognitive skills in psychotic illness. Only one study detected a diminished cognitive performance in social cognition with a long-term cannabis use.180 However, other cognitive domains were unaffected. After controlling for confounders, such as age, the age of illness onset, socioeconomic status, premorbid IQ, the effect of cannabis on cognitive function was not significant based on The Digit Symbol Coding Test.181,182 Paradoxically, some studies report that cannabis use was associated with small but statistically significant improvement in global cognitive index,183,184 attention and psychomotor speed,184 verbal learning and memory,184 processing speed,183 executive function,183 working memory,183 and visual memory.183 A reverse association was detected in control populations without psychiatric illness. It is possible that the disease itself exerts a stronger effect on cognitive performance than cannabis. Alternatively, a subpopulation of patients who uses marijuana could be functioning better relative to nonusers. This could explain that abstinence from cannabis resulted in statistically significant improvement in memory and learning.185,186 Cannabis users could also develop compensatory mechanisms. Based on the functional imaging studies between healthy cannabis users and nonusers, despite no difference in cognitive performance, cannabis users exhibited slightly different brain activity relative to nonusers, which was described as a “compensatory” effort.187 Overall, there is no convincing evidence due to cannabis use for a diminished cognitive performance in patients with psychiatric illness.
Physicians should strongly advise against daily or high potency cannabis use, early onset of use, and any use if it is associated with subthreshold psychotic features to prevent future psychiatric complications. However, evidence around cannabis use during mental illness is conflicting. Currently, there is no evidence of active adverse effects for cannabis use, except for moderate exacerbation of positive symptoms, reversible effects on global function, and some cognitive domains. Additional longitudinal research is needed to examine various levels of cannabis use on psychiatric symptoms and cognitive function with better control for confounding variables.
Post-Traumatic Stress Disorder
PTSD can have a variety of triggers that affect multiple populations that are encountered within primary care, such as veterans and sexual assault victims.188 Despite this, there has been limited research into the management of treatment-refractory PTSD.189 Within Health Canada’s document, only one pilot study on PTSD was covered, showing a positive effect of nabilone on helping with PTSD-associated nightmares.190 Of the patients with treatment-refractory nightmares, 60% reported a total cessation of nightmares, 13% reported a “satisfactory reduction” of nightmares, and 28% withdrew the study due to adverse events.
Since Health Canada’s review, we identified two studies exploring the effects of cannabis on PTSD-associated nightmares. A recent open-label pilot study administering 5 mg THC in oil daily for 3 weeks showed a reduction in nightmare frequency.191 The blinded placebo-controlled trial conducted by the Canadian Forces randomized patients with PTSD to 7 weeks of placebo or nabilone in a crossover design with a 2-week washout period between regimens.192 The nabilone group had significantly less frequent and intense distressing dreams compared to placebo (P=0.03). For these studies, the cognitive effects (acute or chronic) associated with cannabinoid use should be examined carefully in patients with cognitively demanding occupations such as active military duty, as PTSD is highly prevalent in this population. Currently, there are multiple ongoing trials, including two in Canada,193,194 which investigate smoked, vaporized, and ingested cannabis for use in PTSD which would help address the gaps in current knowledge and solidify the evidence for or against the use of marijuana in PTSD.
Cannabis and pregnancy
Cannabinoid receptors have been detected in the placenta,195 and some cannabinoids, such as THC, can cross the placenta,196,197 accumulating in breast milk.198 Concerns are raised about potential adverse effects of cannabinoid exposure on fetal development. According to the 2013 Health Canada report, the short-term effects of cannabis on neonatal outcomes were inconsistent, with some studies reporting reduced birth weight and length,199–201 as well as a non-statistically significant trends toward sudden death,202 while others reported no effect.203–205 Long-term effects included poor attention, visual analysis, and executive function but no IQ changes.206,207 Exposure to cannabis in breast milk also transiently hindered motor development at 1 year of age.208
Smoking marijuana during pregnancy had no direct effect on maternal health, labor complications, or postnatal problems; however, increased maternal anemia was reported.209 It is possible that this finding is secondary to a confounding variable or type I error. Cannabis users are more likely to be single,210,211 have a low income,211 or be unemployed,212 which may predispose infants toward nutritional deficiency. It is possible that cannabis use during pregnancy has an equivalent effect on maternal health as on any other adult user. However, according to various reports, marijuana use during pregnancy falls between 3.1% to 29.6%,213 thus sufficiently powered, and well-controlled matched cohort studies are warranted to identify adverse effects on maternal health.
Furthermore, maternal cannabis consumption was associated with a 109.42 g reduction in newborn birth weight.209 However, that decline is not clinically significant and is not associated with a statistically significant increase in the risk of developing teratogenic effects, fetal deformities, fetal distress, fetal demise, or abnormal lab values among cannabis users.209,214 However, neonatal intensive care unit/intensive care unit (NICU/ICU) admissions significantly increased from 54% to 102% for newborns exposed to cannabis as compared to nonusers.209,214 Torri et al213 reported a significant cumulative effect on morbidity and mortality for newborns of marijuana smokers, particularly in infection-related morbidity, such as sepsis, pneumonia, or bacterial meningitis, and neurological morbidity. However, the study is not sufficient to detect individual risks as it comprises only 48 marijuana users compared to 1562 nonusers. Large-scale trials, with sufficient power, are required to identify the underlying cause of NICU/ICU admissions and cumulative morbidity.
We could not identify any recent research on the effect of cannabis use on breastfeeding or long-term outcomes since the 2013 Health Canada report. Such research is challenging due to the extended follow-up period needed and the presence of many confounding variables, such as parental cannabis use, socioeconomic status, family dynamic, and neighborhood influence. Although studies have reported no or transient effects of early cannabinoids exposure on growth,215 motor,216–218 and cognitive development,216–219 these earlier findings have limited applications today, given that new cannabis strains are more potent than before.220
Since cannabis use during pregnancy has a noticeable effect on early childhood morbidity, physicians should strongly advise against its recreational use during pregnancy. Pregnant women refusing or incapable of stopping cannabis use should be encouraged to obtain cannabis from approved sources where the exact amount of marijuana used can be monitored. Such information could be used in future research to quantify better cannabinoids consumed and identify dose-dependent outcomes. The new study should also consider various routes of cannabis administration, whether edible, smoked, or vaporized, and control confounding variables such as maternal health and socioeconomic status.
Cannabis and opioids
The widespread abuse of opioids has led to a spike in opioid-related death to 8.8 per 100,000 in Canada.221 The increased prescribing practices of these drugs and the introduction of highly addictive, potent synthetics such as fentanyl may be attributed to the rampant spread of this epidemic. Methadone, buprenorphine, and naltrexone are the only three US Food and Drug Administration-approved drugs for long-term treatment of opiate addiction.222 Several studies have hypothesized the potential use of cannabis for the treatment of opioid addiction; however, results from studies conducted on these proposed uses have shown conflicting results. Cannabis smoking during a methadone taper demonstrated no evidence for cannabis smoking reducing opioid-withdrawal symptoms (P=0.52).223 Although smoked cannabis was not shown to be successful in reducing opioid withdrawal symptoms, it is yet to be seen if isolated cannabinoids such as CBD or different concentrations of cannabinoids have a role in opioid withdrawal. CBD may play a role due to its anti-anxiety effect,224 curbing the extreme anxiety associated with opioid withdrawal.225
Additional considerations
First, it is essential to remark that a single dose of ∆9-THC in chronic smokers can be detected up to 13 days following intake,226 while in others, 80%–90% of a total ∆9-THC dose will be excreted within 5 days.227 Additional evidence has shown that both ∆9-THC and 11-OH-THC (an active ∆9-THC metabolite) can be detected in circulation for up to 1 month after intake, causing neurocognitive impairment in the first weeks of abstinence.228
Second, it has been shown that cannabinoids can cause increased glucose intake and lipogenesis.229 Therefore, if authorizing the use of medicinal cannabis for obese diabetic patients who are receiving insulin injections, the effects of MM on blood glucose levels and the patients’ response to their current treatment regimen should be examined with these underlying impacts in mind, particularly when considering a change in treatment or dose.
Cannabis abuse
Tolerance to THC is theorized to be due to downregulation and desensitization of CB1230,231 and has been documented in heavy and therapeutic users, but not in social users.232,233 Physical and psychological dependence also occurs with heavy usage.234,235 However, according to National Epidemiological Survey on Alcohol and Related Conditions, the rate of transition to dependence for cannabis is 8.9%, which is small percentage relatively to 22.7% and 67.5% for alcohol and nicotine, respectively.236 Moreover, the withdrawal symptoms of marijuana are milder than other drugs,231 such as alcohol, cocaine, heroin, and include anger, depressed mood, irritability, anxiety, restlessness, insomnia, strange dreams, weight loss, and decreased appetite.40 The delayed onset of withdrawal due to THC’s relatively long half-life and relative mildness of symptoms compared to other substances contributes to apprehensions of its clinical implications.231,237
A few studies examined agonist therapy with synthetic cannabinoids to attenuate withdrawal symptoms and promote cannabis use cessation. In the placebo-controlled trial, dronabinol suppressed cannabis withdrawal symptoms in a dose-dependent manner based on the withdrawal discomfort score (P<0.05).238 Another study using nabiximols significantly attenuated withdrawal symptoms relative to placebo (P=0.01) but did not have a better effect than placebo on a complete cessation of cannabis use (P=0.75).239 A similar study using Sativex was found to reduce withdrawal symptoms (P<0.01) with high fixed doses but was also unable to demonstrate long-term cessation.240 The attenuation of withdrawal could be due to the tapering off effect created by supplementing cannabis with synthetic cannabinoids. However, because opioids and cannabinoids have been shown to interact synergistically with each other, if a patient is prescribed both opioid and cannabis, care providers should know that opioid may need to be reduced to avoid dependency.241 Further research needs to be done on the amount and THC/CBD ratio of cannabinoids necessary to safely taper withdrawal.
Other studies investigated vilazadone,242 escitalopram,243 buspirone,244 lithium carbonate,245 and a combination of lofexidine and dronabinol,246 to treat cannabis dependence, but none showed any significant results. Only gabapentin significantly reduced the amount of marijuana smoked per week based on patient self-report (P=0.004) and the biochemical urine analysis (P=0.001).247 However, gabapentin also carries abuse potential.248–250 The addiction potential of cannabis is a concern to clinicians and should be discussed with patients. The risk of addiction must be weighed against the benefit on a case-by-case basis. Currently, an accepted pharmacological treatment for cannabis-use disorders does not exist.
Conclusion
In summary, the effect of cannabis has been intensely studied in several disease states, as previously discussed; however, gaps in our knowledge remain. Although recent research has advanced our understanding from the release of the 2013 Health Canada document, there is a need for additional research that addresses different modes of administration, controlling for cannabis users and cannabis naïve individuals, as well as for other contraindications. Bearing this in mind, our current knowledge on cannabis use suggests that cannabis presents as an appropriate alternative therapy option for patients who have epilepsy, movement disorders, and pain. For individuals with MS, GI disorders, anorexia, and headaches, further research is recommended to improve our understanding of the effects of MM, and caution is advised when considering the authorization of MM use. For patients who are under the age of 25 years, pregnant, or present with a history of mental health and substance use, it is safe to err on the side of caution and avoid MM authorization. Overall, MM is an exciting field of exploration, and the diverse range of receptor expression in the human body offers many therapeutic benefits, yet additional research is required for a more robust understanding and characterization of the mechanism of action of MM to achieve maximal therapeutic efficacy.
Author information
YM (MBBCh), AV (MD), SMSF (MBBS), CN (MSc, MD), AL (MD), and UB (MBBS) are postgraduate medical trainees in the Graduate Diploma and Professional Master in Medical Sciences (GDPM), Postgraduate Medical Education, School of Medicine, Faculty of Health Sciences, Queen’s University, Kingston, ON, K7L 3N6, Canada. BQ (BSc) and MS (MSc) are graduate research trainees in the laboratory of Prof. Dr. Myron R Szewczuk, Department of Biomedical and Molecular Sciences (DBMS), Faculty of Health Science, Queen’s University. MRS (BSc, MSc, PhD) is Full Professor in DBMS and Academic and Research Lead of the GDPM program.
Data sharing statement
The data sets supporting the conclusions of this article are included within the article and in the supplementary material.
Acknowledgments
The authors are grateful to the initial internal peer-reviewers with expertise in medicinal marijuana for their comments and suggestions for the improvement of this review article. The internal reviewers are from the Faculty of Arts & Sciences, University of Toronto, Toronto; Pharmacology and Toxicology, the Department of Biomedical and Medical Sciences, Queen’s University; the Department of Psychiatry, School of Medicine, Queen’s University; and the Department of Oncology and Undergraduate Medical Education for Palliative Care, School of Medicine, Queen’s University, Kingston, ON, Canada. The authors acknowledge support from the Graduate Diploma & Professional Master in Medical Sciences, School of Medicine, Queen’s University, Kingston, ON, Canada. This review was an independent research study funded in part by Postgraduate Medical Education, Queen’s University, Kingston, ON, Canada, and the Natural Sciences and Engineering Research Council of Canada and a private sector cancer funding from the Josefowitz Family to MRS. The views expressed in this article are those of the authors and not the funding bodies.
Author contributions
MRS conceived the review of the article and obtained funding; YM, AV, BQ, MS, SMSF, CN, AL, and UB designed the study, carried out the searches, refined the study design, selected studies and extracted data, and conducted the thematic analyses; YM, AV, BQ, MS, and MRS led the writing of the draft manuscript as contributing first authorship. All Authors contributed toward data analysis, drafting and revising the paper and agree to be accountable for all aspects of the work.
Disclosure
B Qorri is a recipient of the Queen’s Graduate Award (QGA) and the 2017 Terry Fox Research Institute Transdisciplinary Training Program in Cancer Research. M Sambi is a recipient of the QGA. The authors report no other conflicts of interest in this work.
References
Belle-Isle L, Walsh Z, Callaway R, et al. Barriers to access for Canadians who use cannabis for therapeutic purposes. Int J Drug Policy. 2014;25(4):691–699. | ||
Minister of Justice. Access to Cannabis for Medical Purposes Regulations. Canada: Minister of Justice; 2016. Available from: http://www.gazette.gc.ca/rp-pr/p2/2016/2016-08-24/html/sor-dors230-eng.html. Accessed November 1, 2017. | ||
The College of Physicians and Surgeons of Ontario. Marijuana for Medical Purposes. Toronto, ON: The College of Physicians and Surgeons of Ontario; 2015. Available from: http://www.cpso.on.ca/Policies-Publications/Policy/Marijuana-for-Medical-Purposes. Accessed November 1, 2017. | ||
Health Canada. Information for Health Care Professionals: Cannabis (Marihana, Marijuana) and the Cannabinoids. Canada: Government of Canada; 2013. Available from: https://www.canada.ca/en/health-canada/services/drugs-health-products/medical-use-marijuana/information-medical-practitioners/information-health-care-professionals-cannabis-marihuana-marijuana-cannabinoids.html. Accessed November 1, 2017. | ||
Waissengrin B, Urban D, Lesham Y, Garty M, Wolf I. Patterns of use of medical cannabis among Israeli cancer patients: a single instituition experience. J Pain Sympt Manag. 2015;49(2):223–230. | ||
Ziemianski D, Capler R, Tekanoff R, Lacasse A, Luconi F, Ware MA. Cannabis in medicine: a national educational needs assessment among Canadian physicians. BMC Med Educ. 2015;15(1):52. | ||
Kondrad E, Reid A. Colorado family physicians’ attitudes toward medical marijuana. J Am Board Fam Med. 2013;26(1):52–60. | ||
The College of Physicians and Surgeons of Ontario. Policy Statement on Marijuana for Medical Purposes; 2015. Available from: http://policyconsult.cpso.on.ca/?page_id=4090. Accessed May 1, 2018. | ||
College of Physicians and Surgeons of Nova Scotia. Policy Regarding the Authorization of Marijuana for Medical Purposes; 2014. Available from: http://www.cpsns.ns.ca/DesktopModules/Bring2mind/DMX/Download.aspx?PortalId=0&TabId=129&EntryId=52. | ||
College of Physicians and Surgeons of Saskatchewan. Regulatory Bylaws; 2015. Available from: http://cps.sk.ca/Documents/Legislation/Legislation/2015_Regulatory_Bylaws_-_June_2015.pdf. | ||
Collège Des Médecins, Québec. Guidelines Concerning the Prescription of Dried Cannabis for Medical Purposes; 2015. Available from: http://www.cmq.org/publications-pdf/p-1-2014-04-01-en-directives-concernant-ordonnance-cannabis-seche-fins-medicales.pdf?t=1455740574019. | ||
The College of Physicians and Surgeons of Manitoba. Standards of Practice of Medicine (Bylaw 11); 2016. Available from: http://cpsm.mb.ca/cjj39alckF30a/wp-content/uploads/ByLaws/By-Law-11.pdf. | ||
The College of Physicians and Surgeons of Prince Edward Island. Policy on Prescribing of Medical Marijuana; 2016. Available from: http://cpspei.ca/wp-content/uploads/2017/03/Marijuana-Prescribing-Nov-3016.pdf. | ||
The College of Physicians and Surgeons of Newfoundland and Labrador. Advisory and Interim Guideline; 2014. Available from: http://www.cpsnl.ca/default.asp?com=Policies&m=340&y=&id=98. | ||
The College of Physicians and Surgeons of British Columbia. Professional Standards and Guidelines on Marijuana for Medical Purposes; 2015. Available from: https://www.cpsbc.ca/files/pdf/PSG-Marijuana-for-Medical-Purposes.pdf. | ||
The College of Physicians and Surgeons of Alberta. Standard of Practice on Cannabis for Medical Purposes; 2014. Available from: http://www.cpsa.ca/standardspractice/cannabis-for-medical-purposes/. | ||
Canadian Medical Protective Association. Medical Marijuana: Considerations for Canadian Doctors; 2016. Available from: https://www.cmpa-acpm.ca/en/advice-publications/browse-articles/2014/medical-marijuana-new-regulations-new-college-guidance-for-canadian-doctors. | ||
Government of Canada. Information for Health Care Professionals: Cannabis (marihuana, marijuana) and the cannabinoids [Health Canada, 2013]; 2013. Available from: https://www.canada.ca/en/health-canada/services/drugs-health-products/medical-use-marijuana/information-medical-practitioners/information-health-care-professionals-cannabis-marihuana-marijuana-cannabinoids.html. Accessed November 1, 2017. | ||
CAMH. Cannabis Policy Framework; 2014. Available from: https://www.ijdp.org/article/S0955-3959(16)30114-1/fulltext. Accessed May 1, 2017. | ||
The College of Family Physicians of Canada. Authorizing Dried Cannabis for Chronic Pain or Anxiety: Preliminary Guidance; 2014. Availale from: http://www.cfpc.ca/Release_Dried_Cannabis_Prelim_Guidance/. | ||
Ligresti A, De Petrocellis L, Di Marzo V. from phytocannabinoids to cannabinoid receptors and endocannabinoids: pleiotropic physiological and pathological roles through complex pharmacology. Physiol Rev. 2016;96(4):1593–1659. | ||
Izzo AA, Mascolo N, Capasso F. The gastrointestinal pharmacology of cannabinoids. Curr Opin Pharmacol. 2001;1(6):597–603. | ||
Di Marzo V, Melck D, Bisogno T, De Petrocellis L. Endocannabinoids: endogenous cannabinoid receptor ligands with neuromodulatory action. Trends Neurosci. 1998;21(12):521–528. | ||
Navarro M, Carrera MRA, Fratta W, et al. Functional interaction between opioid and cannabinoid receptors in drug self-administration. J Neurosci. 2001;21(14):5344. | ||
Gómez R, Navarro M, Ferrer B, et al. A peripheral mechanism for CB1 cannabinoid receptor-dependent modulation of feeding. J Neurosci. 2002;22(21):9612. | ||
Calignano A, La Rana G, Loubet-Lescoulié P, Piomelli D. A role for the endogenous cannabinoid system in the peripheal control of pain initiation. Prog Brain Res. 2000;129:471–482. | ||
Pertwee RG. Cannabinoid receptors and pain. Prog Neurobiol. 2001;63(5):569–611. | ||
Castellano C, Rossi-Arnaud C, Cestari V, Costanzi M. Cannabinoids and memory: animal studies. Curr Drug Targets CNS Neurol Disord. 2003;2(6):389–402. | ||
Rodrı́guez de Fonseca F, Del Arco I, Martı́n-Calderón JL, Gorriti MA, Navarro M. Role of the endogenous cannabinoid system in the regulation of motor activity. Neurobiol Dis. 1998;5(6):483–501. | ||
Cabral GA. Marijuana and cannabinoids. J Cannabis Ther. 2001;1(3–4):61–85. | ||
Robson PJ. Therapeutic potential of cannabinoid medicines. Drug Test Anal. 2014;6(1–2):24–30. | ||
Munro S, Thomas KL, Abu-Shaar M. Molecular characterization of a peripheral receptor for cannabinoids. Nature. 1993;365(6441):61–65. | ||
Matsuda LA, Lolait SJ, Brownstein MJ, Young AC, Bonner TI. Structure of a cannabinoid receptor and functional expression of the cloned cDNA. Nature. 1990;346(6284):561–564. | ||
Herkenham M, Lynn AB, Little MD, et al. Cannabinoid receptor localization in brain. Proc Natl Acad Sci U S A. 1990;87(5):1932–1936. | ||
Mackie K. Cannabinoid receptors as therapeutic targets. Annu Rev Pharmacol Toxicol. 2006;46:101–122. | ||
Duncan M, Mouihate A, Mackie K, et al. Cannabinoid CB2 receptors in the enteric nervous system modulate gastrointestinal contractility in lipopolysaccharide-treated rats. Am J Physiol Gastrointestinal Liver Physiol. 2008;295(1):G78–G87. | ||
Devane WA, Hanus L, Breuer A, et al. Isolation and structure of a brain constituent that binds to the cannabinoid receptor. Science (New York, NY). 1992;258(5090):1946–1949. | ||
Stella N, Schweitzer P, Piomelli D. A second endogenous cannabinoid that modulates long-term potentiation. Nature. 1997;388(6644):773–778. | ||
Aizpurua-Olaizola O, Elezgarai I, Rico-Barrio I, Zarandona I, Etxebarria N, Usobiaga A. Targeting the endocannabinoid system: future therapeutic strategies. Drug Discov Today. 2017;22(1):105–110. | ||
Baron EP. Comprehensive review of medicinal marijuana, cannabinoids, and therapeutic implications in medicine and headache: what a long strange trip it’s been. Headache. 2015;55(6):885–916. | ||
Hill AJ, Williams CM, Whalley BJ, Stephens GJ. Phytocannabinoids as novel therapeutic agents in CNS disorders. Pharmacol Ther. 2012;133(1):79–97. | ||
Elsohly MA, Slade D. Chemical constituents of marijuana: the complex mixture of natural cannabinoids. Life Sci. 2005;78(5):539–548. | ||
Racz I, Nadal X, Alferink J, et al. Crucial role of CB(2) cannabinoid receptor in the regulation of central immune responses during neuropathic pain. J Neurosci. 2008;28(46):12125–12135. | ||
Pertwee RG. The diverse CB(1) and CB(2) receptor pharmacology of three plant cannabinoids: Δ(9)-tetrahydrocannabinol, cannabidiol and Δ(9)-tetrahydrocannabivarin. Br J Pharmacol. 2008;153(2):199–215. | ||
Hillig KW, Mahlberg PG. A chemotaxonomic analysis of cannabinoid variation in Cannabis (Cannabaceae). Am J Bot. 2004;91(6):966–975. | ||
Mehmedic Z, Chandra S, Slade D, et al. Potency trends of Δ9-THC and other cannabinoids in confiscated cannabis preparations from 1993 to 2008. J Forensic Sci. 2010;55(5):1209–1217. | ||
Fasinu PS, Phillips S, ElSohly MA, Walker LA. Current status and prospects for cannabidiol preparations as new therapeutic agents. Pharmacotherapy. 2016;36(7):781–796. | ||
Morgan CJA, Freeman TP, Schafer GL, Curran HV. Cannabidiol attenuates the appetitive effects of [delta]9-tetrahydrocannabinol in humans smoking their chosen cannabis. Neuropsychopharmacology. 2010;35(9):1879–1885. | ||
Yucel M, Lorenzetti V, Suo C, et al. Hippocampal harms, protection and recovery following regular cannabis use. Transl Psychiatry. 2016;6:e710. | ||
Russo E, Guy GW. A tale of two cannabinoids: the therapeutic rationale for combining tetrahydrocannabinol and cannabidiol. Med Hypotheses. 2006;66:234–246. | ||
Huestis MA. Pharmacokinetics and metabolism of the plant cannabinoids, Δ9-tetrahydrocannibinol, cannabidiol and cannabinol. In: Pertwee RG, editor. Cannabinoids. Berlin, Heidelberg: Springer Berlin Heidelberg; 2005:657–690. | ||
Whittle BA, Guy GW. Development of cannabis-based medicines: risk, benefit and serendipity. In: Guy GW, Robson PJ, Whittle BA, editors. The Medicinal Uses of Cannabis and Cannabinoids. London: Pharmaceutical Press; 2004:427–463. | ||
Dussy FE, Hamberg C, Luginbühl M, Schwerzmann T, Briellmann TA. Isolation of Δ9-THCA-A from hemp and analytical aspects concerning the determination of Δ9-THC in cannabis products. Forensic Sci Int. 2005;149(1):3–10. | ||
Iversen L, editor. The pharmacology of THC, the psychoactive ingredient in Cannabis. In: The Science of Marijuana. New York, NY: Oxford University Press; 2000:29–37. | ||
Huestis MA. Human cannabinoid pharmacokinetics. Chem Biodivers. 2007;4(8):1770–1804. | ||
Abrams DI, Vizoso HP, Shade SB, Jay C, Kelly ME, Benowitz NL. Vaporization as a smokeless cannabis delivery system: a pilot study. Clin Pharmacol Ther. 2007;82(5):572–578. | ||
Pomahacova B, Van der Kooy F, Verpoorte R. Cannabis smoke condensate III: the cannabinoid content of vaporised Cannabis sativa. Inhal Toxicol. 2009;21(13):1108–1112. | ||
Mattes RD, Shaw LM, Edling-Owens J, Engelman K, Elsohly MA. Bypassing the first-pass effect for the therapeutic use of cannabinoids. Pharmacol Biochem Behav. 1993;44(3):745–747. | ||
Adelli GR, Bhagav P, Taskar P, et al. Development of a Δ9-tetrahydrocannabinol amino acid-dicarboxylate prodrug with improved ocular bioavailability Δ9-THC prodrugs for improved ocular bioavailability. Invest Ophthalmol Vis Sci. 2017;58(4):2167–2179. | ||
Kerstrin I, Franjo G. An update on safety and side effects of cannabidiol: a review of clinical data and relevant animal studies. Cannabis Cannabinoid Res. 2017;2(1):139–154. | ||
Garrett ER, Hunt CA. Pharmacokinetics of Δ9-tetrahydrocannabinol in dogs. J Pharm Sci. 1977;66(3):395–407. | ||
Widman M, Agurell S, Ehrnebo M, Jones G. Binding of (+)- and (-)-Δ1-tetrahydrocannabinols and (-)-7-hydroxy-Δ1-tetrahydrocannabinol to blood cells and plasma proteins in man. J Pharm Pharmacol. 1974;26(11):914–916. | ||
Wahlqvist M, Nilsson IM, Sandberg F, Agurell S, Granstrand B. Binding of δ1-tetrahydrocannabinol to human plasma proteins. Biochem Pharmacol. 1970;19(9):2579–2582. | ||
Truitt EB. Biological disposition of tetraydrocannabinols. Pharmacol Rev. 1971;23(4):273–278. | ||
Public Health Agency of Canada. Multiple sclerosis. Available from: http://www.phac-aspc.gc.ca/cd-mc/ms-sp/index-eng.php. Accessed November 1, 2017. | ||
Olsen SA. A review of complementary and alternative medicine (CAM) by people with multiple sclerosis. Occup Ther Int. 2009;16(1):57–70. | ||
Pryce G, Baker D. Endocannabinoids in multiple sclerosis and amyotrophic lateral sclerosis. In: Pertwee RG, editor. Endocannabinoids. Cham: Springer International Publishing; 2015:213–231. | ||
Kindred JH, Li KG, Ketelhut NB, et al. Cannabis use in people with Parkinson’s disease and multiple sclerosis: a web-based investigation. Complement Ther Med. 2017;33:99–104. | ||
Brenton JN, Schreiner T, Karoscik K, et al. Attitudes, perceptions, and use of marijuana in youth with multiple sclerosis. J Neurol. 2018;265(2):417–423. | ||
Langford RM, Mares J, Novotna A, et al. A double-blind, randomized, placebo-controlled, parallel-group study of THC/CBD oromucosal spray in combination with the existing treatment regimen, in the relief of central neuropathic pain in patients with multiple sclerosis. J Neurol. 2013;260(4):984–997. | ||
Ball S, Vickery J, Hobart J, et al. The cannabinoid use in progressive inflammatory brain disease (CUPID) trial: a randomised double-blind placebo-controlled parallel-group multicentre trial and economic evaluation of cannabinoids to slow progression in multiple sclerosis. Health Technol Assess. 2015;19(12):vii–viii, xxv–xxxi, 1–187. | ||
Zajicek J, Ball S, Wright D, et al. Effect of dronabinol on progression in progressive multiple sclerosis (CUPID): a randomised, placebo-controlled trial. Lancet Neurol.12(9):857–865. | ||
Leocani L, Nuara A, Houdayer E, et al. Sativex® and clinical–neurophysiological measures of spasticity in progressive multiple sclerosis. J Neurol. 2015;262(11):2520–2527. | ||
Marinelli L, Mori L, Canneva S, et al. The effect of cannabinoids on the stretch reflex in multiple sclerosis spasticity. Int Clin Psychopharmacol. 2016;31(4):232–239. | ||
Flachenecker P, Henze T, Zettl UK. Nabiximols (THC/CBD oromucosal spray, Sativex®) in clinical practice – results of a multicenter, non-interventional study (MOVE 2) in patients with multiple sclerosis spasticity. Eur Neurol. 2014;71(5–6):271–279. | ||
Flachenecker P, Henze T, Zettl UK. Long-term effectiveness and safety of nabiximols (tetrahydrocannabinol/cannabidiol oromucosal spray) in clinical practice. Eur Neurol. 2014;72(1–2):95–102. | ||
Fernández LL, Boquet EM, Pérez-Miralles F, et al. Clinical experiences with cannabinoids in spasticity management in multiple sclerosis. Neurología (English Edition). 2014;29(5):257–260. | ||
Koehler J, Feneberg W, Meier M, Pöllmann W. Clinical experience with THC:CBD oromucosal spray in patients with multiple sclerosis-related spasticity. Int J Neurosci. 2014;124(9):652–656. | ||
Flachenecker P. A new multiple sclerosis spasticity treatment option: effect in everyday clinical practice and cost–effectiveness in Germany. Expert Rev Neurother. 2013;13(Suppl 1):15–19. | ||
García-Merino A. Endocannabinoid system modulator use in everyday clinical practice in the UK and Spain. Expert Rev Neurother. 2013; 13(Suppl 1):9–13. | ||
Honarmand K, Tierney MC, O’Connor P, Feinstein A. Effects of cannabis on cognitive function in patients with multiple sclerosis. Neurology. 2011;76(13):1153–1160. | ||
Gaitatzis A, Johnson AL, Chadwick DW, Shorvon SD, Sander JW. Life expectancy in people with newly diagnosed epilepsy. Brain. 2004;127(11):2427–2432. | ||
Trinka E. Epilepsy: comorbidity in the elderly. Acta Neurol Scand. 2003;108(s180):33–36. | ||
McCagh J, Fisk JE, Baker GA. Epilepsy, psychosocial and cognitive functioning. Epilepsy Res. 2009;86(1):1–14. | ||
Mohanraj R, Norrie J, Stephen LJ, Kelly K, Hitiris N, Brodie MJ. Mortality in adults with newly diagnosed and chronic epilepsy: a retrospective comparative study. Lancet Neurol. 2006;5(6):481–487. | ||
Trinka E, Bauer G, Oberaigner W, Ndayisaba JP, Seppi K, Granbichler CA. Cause-specific mortality among patients with epilepsy: results from a 30-year cohort study. Epilepsia. 2013;54(3):495–501. | ||
Gaitatzis A, Sisodiya SM, Sander JW. The somatic comorbidity of epilepsy: a weighty but often unrecognized burden. Epilepsia. 2012;53(8):1282–1293. | ||
Hess EJ, Moody KA, Geffrey AL, et al. Cannabidiol as a new treatment for drug-resistant epilepsy in tuberous sclerosis complex. Epilepsia. 2016;57(10):1617–1624. | ||
Porter BE, Jacobson C. Report of a parent survey of cannabidiol-enriched cannabis use in pediatric treatment-resistant epilepsy. Epilepsy Behav. 2013;29(3):574–577. | ||
Devinsky O, Marsh E, Friedman D, et al. Cannabidiol in patients with treatment-resistant epilepsy: an open-label interventional trial. Lancet Neurol. 2016;15(3):270–278. | ||
Tzadok M, Uliel-Siboni S, Linder I, et al. CBD-enriched medical cannabis for intractable pediatric epilepsy: the current Israeli experience. Seizure. 2016;35:41–44. | ||
Devinsky O, Cross JH, Laux L, et al. Trial of cannabidiol for drug-resistant seizures in the dravet syndrome. N Engl J Med. 2017;376(21):2011–2020. | ||
Thiele EA, Marsh ED, French JA, et al. Cannabidiol in patients with seizures associated with Lennox-Gastaut syndrome (GWPCARE4): a randomised, double-blind, placebo-controlled phase 3 trial. Lancet. 2018;391(10125):1085–1096. | ||
Yamaori S, Ebisawa J, Okushima Y, Yamamoto I, Watanabe K. Potent inhibition of human cytochrome P450 3A isoforms by cannabidiol: role of phenolic hydroxyl groups in the resorcinol moiety. Life Sci. 2011;88(15):730–736. | ||
Jiang R, Yamaori S, Takeda S, Yamamoto I, Watanabe K. Identification of cytochrome P450 enzymes responsible for metabolism of cannabidiol by human liver microsomes. Life Sci. 2011;89(5):165–170. | ||
Lim K, See YM, Lee J. A systematic review of the effectiveness of medical cannabis for psychiatric, movement and neurodegenerative disorders. Clin Psychopharm Neurosci. 2017;15(4):301–312. | ||
Wong SL, Gilmour H, Ramage-Morin PL. Parkinson’s disease: prevalence, diagnosis and impact; 2015. Available from: http://www.statcan.gc.ca/pub/82-003-x/2014011/article/14112-eng.pdf. Accessed May 1, 2018. | ||
Babayeva M, Assefa H, Basu P, Chumki S, Loewy Z. Marijuana compounds: a nonconventional approach to Parkinson’s disease therapy. Parkinsons Dis. 2016;2016:19. | ||
More SV, Choi D-K. Promising cannabinoid-based therapies for Parkinson’s disease: motor symptoms to neuroprotection. Mol Neurodegener. 2015;10(1):17. | ||
Chagas MHN, Zuardi AW, Tumas V, et al. Effects of cannabidiol in the treatment of patients with Parkinson’s disease: an exploratory double-blind trial. J Psychopharmacol. 2014;28(11):1088–1098. | ||
Lotan I, Treves TA, Roditi Y, Djaldetti R. Cannabis (medical marijuana) treatment for motor and non-motor symptoms of Parkinson disease: an open-label observational study. Clin Neuropharmacol. 2014;37(2):41–44. | ||
Shohet A, Khlebtovsky A, Roizen N, Roditi Y, Djaldetti R. Effect of medical cannabis on thermal quantitative measurements of pain in patients with Parkinson’s disease. Eur J Pain. 2017;21(3):486–493. | ||
Chagas M, Eckeli A, Zuardi A, et al. Cannabidiol can improve complex sleep-related behaviours associated with rapid eye movement sleep behaviour disorder in Parkinson’s disease patients: a case series. J Clin Pharm Ther. 2014;39(5):564–566. | ||
Jankovic J, Kurlan R. Tourette syndrome: evolving concepts. Mov Disord. 2011;26(6):1149–1156. | ||
Müller-Vahl KR. Treatment of Tourette syndrome with cannabinoids. Behav Neurol. 2013;27(1):119–124. | ||
Müller-Vahl K, Kolbe H, Dengler R. Gilles de la Tourette syndrome. Effect of nicotine, alcohol and marihuana on clinical symptoms. Der Nervenarzt. 1997;68(12):985. | ||
Trainor D, Evans L, Bird R. Severe motor and vocal tics controlled with Sativex®. Australas Psychiatry. 2016;24(6):541–544. | ||
Kanaan AS, Jakubovski E, Müller-Vahl K. Significant tic reduction in an otherwise treatment-resistant patient with Gilles de la Tourette syndrome following treatment with nabiximols. Brain Sci. 2017;7(5):47. | ||
DiPatrizio NV. Endocannabinoids in the gut. Cannabis Cannabinoid Res. 2016;1(1):67–77. | ||
Mackie K. Cannabinoid receptors: where they are and what they do. J Neuroendocrinol. 2008;20:10–14. | ||
Izzo AA, Coutts AA. Cannabinoids and the digestive tract. Handb Exp Pharmacol. 2005;(168):573–598. | ||
Rocchi A, Benchimol EI, Bernstein CN, et al. Inflammatory bowel disease: a Canadian burden of illness review. Can J Gastroenterol. 2012;26(11):811–817. | ||
Phatak UP, Rojas-Velasquez D, Porto A, Pashankar DS. Prevalence and patterns of marijuana use in young adults with inflammatory bowel disease. J Pediatr Gastroenterol Nutr. 2017;64(2):261–264. | ||
Allegretti JR, Courtwright A, Lucci M, Korzenik JR, Levine J. Marijuana use patterns among patients with inflammatory bowel disease. Inflamm Bowel Dis. 2013;19(13):2809. | ||
Storr M, Devlin S, Kaplan GG, Panaccione R, Andrews CN. Cannabis use provides symptom relief in patients with inflammatory bowel disease but is associated with worse disease prognosis in patients with Crohn’s disease. Inflamm Bowel Dis. 2014;20(3):472–480. | ||
Naftali T, Mechulam R, Marii A, et al. Low-dose cannabidiol is safe but not effective in the treatment for Crohn’s disease, a randomized controlled trial. Dig Dis Sci. 2017:62(6):1615-1620. | ||
Naftali T, Bar-Lev Schleider L, Dotan I, Lansky EP, Sklerovsky Benjaminov F, Konikoff FM. Cannabis induces a clinical response in patients with crohn’s disease: a prospective placebo-controlled study. Clin Gastroenterol Hepatol. 2013;11(10):1276–1280.e1271. | ||
Controlled Substances and Tobacco Directorate. Information for health care professionals: cannabis (marihuana, marijuana) and the cannabinoids; 2013. Available from: https://www.canada.ca/content/dam/hc-sc/migration/hc-sc/dhp-mps/alt_formats/pdf/marihuana/med/infoprof-eng.pdf. Accessed November 1, 2017. | ||
Haney M, Rabkin J, Gunderson E, Foltin RW. Dronabinol and marijuana in HIV(+) marijuana smokers: acute effects on caloric intake and mood. Psychopharmacology. 2005;181(1):170–178. | ||
Andries A, Frystyk J, Flyvbjerg A, Stoving RK. Dronabinol in severe, enduring anorexia nervosa: a randomized controlled trial. Int J Eat Disord. 2014;47(1):18–23. | ||
Abbracchio MP, Di Luca M, Di Giulio AM, Cattabeni F, Tenconi B, Gorio A. Denervation and hyperinnervation in the nervous system of diabetic animals: III. Functional alterations of G proteins in diabetic encephalopathy. J Neurosci Res. 1989;24(4):517–523. | ||
ClinicalTrials.gov. Identifier NCT02802540, Nabilone effect on the attenuation of anorexia, nutritional status and quality of life in lung cancer patients; 2016. Available from: https://clinicaltrials.gov/show/NCT02802540. Accessed November 1, 2017. | ||
Levin DN, Dulberg Z, Chan A-W, Hare GM, Mazer CD, Hong A. A randomized-controlled trial of nabilone for the prevention of acute postoperative nausea and vomiting in elective surgery. Can J Anesth. 2017;64(4):385–395. | ||
Kleine-Brueggeney M, Greif R, Brenneisen R, Urwyler N, Stueber F, Theiler LG. Intravenous delta-9-tetrahydrocannabinol to prevent postoperative nausea and vomiting: a randomized controlled trial. Anesth Analg. 2015;121(5):1157–1164. | ||
Woodhams SG, Chapman V, Finn DP, Hohmann AG, Neugebauer V. The cannabinoid system and pain. Neuropharmacology. 2017;124(Suppl C):105–120. | ||
Starowicz K, Finn DP. Chapter thirteen – cannabinoids and pain: sites and mechanisms of action. In: Kendall D, Alexander SPH, editors. Advances in Pharmacology. Vol 80. Cambridge, MA: Academic Press; 2017:437–475. | ||
Cooper ZD, Sandra DC, Haney M. Comparison of the analgesic effects of dronabinol and smoked marijuana in daily marijuana smokers. Neuropsychopharmacology. 2013;38(10):1982–1992. | ||
Bouhassira D, Lanteri-Minet M, Attal N, Laurent B, Touboul C. Prevalence of chronic pain with neuropathic characteristics in the general population. Pain. 2008;136(3):380–387. | ||
Torrance N, Smith BH, Bennett MI, Lee AJ. The epidemiology of chronic pain of predominantly neuropathic origin. Results from a general population survey. J Pain. 2006;7(4):281–289. | ||
Serpell M, Ratcliffe S, Hovorka J, et al. A double-blind, randomized, placebo-controlled, parallel group study of THC/CBD spray in peripheral neuropathic pain treatment. Eur J Pain. 2014;18(7):999–1012. | ||
Wilsey B, Marcotte T, Deutsch R, Gouaux B, Sakai S, Donaghe H. Low-dose vaporized cannabis significantly improves neuropathic pain. J Pain. 2013;14(2):136–148. | ||
Moulin DE, Boulanger A, Clark AJ, et al. Pharmacological management of chronic neuropathic pain: revised consensus statement from the Canadian Pain Society. Pain Res Manag. 2014;19(6):328–335. | ||
Walter C, Oertel BG, Felden L, et al. Brain mapping-based model of [delta]9-tetrahydrocannabinol effects on connectivity in the pain matrix. Neuropsychopharmacology. 2016;41(6):1659–1669. | ||
Lee MC, Ploner M, Wiech K, et al. Amygdala actviity contributes to the dissociative effect of cannabis on pain perception. Pain. 2013;154(1):124–134. | ||
Lynch ME, Cesar-Rittenberg P, Hohmann A. A double-blind, placebo-controlled, crossover pilot trial with extension using and oral mucosal cannabinoid extract for treatment of chemotherapy-induced neuropathic pain. J Pain Symptom Manage. 2014;47(1):166–173. | ||
Wallace MS, Marcotte TD, Umlauf A, Gouaux B, Atkinson JH. Efficacy of inhaled cannabis on painful diabetic neuropathy. J Pain. 2015;16(7):616–627. | ||
van Amerongen G, Kanhai K, Baakman AC, et al. Effects on spasticity and neuropathic pain of an oral formulation of Δ9-tetrahydrocannabinol in patients with progressive multiple sclerosis. Clin Ther. 2017 Epub Feb 9. | ||
Turcotte D, Doupe M, Torabi M, et al. Nabilone as an adjunctive to gabapentin for multiple sclerosis-induced neuropathic pain: a randomized controlled trial. Pain Med. 2015;16(1):149–159. | ||
Hoggart B, Ratcliffe S, Ehler E, et al. A multicentre, open-label, follow-on study to assess the long-term maintenance of effect, tolerance and safety of THC/CBD oromucosal spray in the management of neuropathic pain. J Neurol. 2015;262(1):27–40. | ||
Eisenberg E, Ogintz M, Almog S. The pharmacokinetics, efficacy, safety, and ease of use of a novel portable metered-dose cannabis inhaler in patients with chronic neuropathic pain: a phase 1a study. J Pain Palliat Care Pharmacother. 2014;28(3):216–225. | ||
Malik Z, Bayman L, Valestin J, Rizvi-Toner A, Hashmi S, Schey R. Dronabinol increases pain threshold in patients with functional chest pain: a pilot double-blind placebo-controlled trial. Dis Esophagus. 2017;30(2):1–8. | ||
de Vries M, Van Rijckevorsel DCM, Vissers KCP, Wilder-Smith OHG, Van Goor H. Single dose delta-9-tetrahydrocannabinol in chronic pancreatitis patients: analgesic efficacy, pharmacokinetics and tolerability. Br J Clin Pharmacol. 2016;81(3):525–537. | ||
de Vries M, van Rijckevorsel DCM, Vissers KCP, Wilder-Smith OHG, van Goor H. Tetrahydrocannabinol does not reduce pain in patients with chronic abdominal pain in a phase 2 placebo-controlled study. Clin Gastroenterol Hepatol. 2017;15(7):1079–1086.e1074. | ||
Ware MA, Wang T, Shapiro S, Collet J-P. Cannabis for the management of pain: assessment of safety study (COMPASS). J Pain. 2015;16(12):1233–1242. | ||
Canadian Cancer Society. Canadian cancer statistics 2017. Available from: http://www.cancer.ca/~/media/cancer.ca/CW/publications/Canadian%20Cancer%20Statistics/Canadian-Cancer-Statistics-2017-EN.pdf. Accessed November 1, 2017. | ||
Deandrea S, Montanari M, Moja L, Apolone G. Prevalence of undertreatment in cancer pain. A review of published literature. Ann Oncol. 2008;19(12):1985–1991. | ||
Johnson JR, Lossignol D, Brunell-Nugent M, Fallon MT. An open-label extension study to investigate the long-term safety and tolerability of THC/CBD oromucosal spray and oromucosal THC spray in patients with terminal cancer-related pain refractrory to strong opioid analgesics. J Pain Sympt Manage. 2013;46(2):207–218. | ||
Côté M, Trudel M, Wang C, Fortin A. Improving quality of life with nabilone during radiotherapy treatments for head and neck cancers. Ann Otol Rhinol Laryngol. 2016;125(4):317–324. | ||
Beckmann YY, Seçkin M, Manavgat Aİ, Zorlu N. Headaches related to psychoactive substance use. Clin Neurol Neurosurg. 2012;114(7):990–999. | ||
Rossi P, Allena M, Tassorelli C, et al. Illicit drug use in cluster headache patients and in the general population: a comparative cross-sectional survey. Cephalalgia. 2012;32(14):1031–1040. | ||
Lorenzo CD, Coppola G, Lorenzo GD, Bracaglia M, Rossi P, Pierelli F. The use of illicit drugs as self-medication in the treatment of cluster headache: results from an Italian online survey. Cephalalgia. 2016;36(2):194–198. | ||
Pearce DD, Mitsouras K, Irizarry KJ. Discriminating the effects of Cannabis sativa and Cannabis indica: a web survey of medical cannabis users. J Altern Complement Med. 2014;20(10):787–791. | ||
Rhyne DN, Anderson SL, Gedde M, Borgelt LM. Effects of medical marijuana on migraine headache frequency in an adult population. Pharmacotherapy. 2016;36(5):505–510. | ||
Pini LA, Guerzoni S, Cainazzo MM, et al. Nabilone for the treatment of medication overuse headache: results of a preliminary double-blind, active-controlled, randomized trial. J Headache Pain. 2012;13(8):677–684. | ||
Marconi A, Di Forti M, Lewis CM, Murray RM, Vassos E. Meta-analysis of the association between the level of cannabis use and risk of psychosis. Schizophr Bull. 2016;42(5):1262–1269. | ||
Davis GP, Compton MT, Wang S, Levin FR, Blanco C. Association between cannabis use, psychosis, and schizotypal personality disorder: findings from the National Epidemiologic Survey on Alcohol and Related Conditions. Schizophr Res. 2013;151(1):197–202. | ||
Stone J, Fisher H, Major B, et al. Cannabis use and first-episode psychosis: relationship with manic and psychotic symptoms, and with age at presentation. Psychol Med. 2014;44(3):499–506. | ||
Di Forti M, Marconi A, Carra E, et al. Proportion of patients in south London with first-episode psychosis attributable to use of high potency cannabis: a case-control study. Lancet Psychiatry. 2015;2(3):233–238. | ||
McHugh M, McGorry P, Yung A, et al. Cannabis-induced attenuated psychotic symptoms: implications for prognosis in young people at ultra-high risk for psychosis. Psychol Med. 2017;47(4):616–626. | ||
Kelley ME, Wan CR, Broussard B, et al. Marijuana use in the immediate 5-year premorbid period is associated with increased risk of onset of schizophrenia and related psychotic disorders. Schizophr Res. 2016;171(1):62–67. | ||
Myles N, Newall H, Nielssen O, Large M. The association between cannabis use and earlier age at onset of schizophrenia and other psychoses: meta-analysis of possible confounding factors. Curr Pharm Des. 2012;18(32):5055–5069. | ||
Helle S, Ringen PA, Melle I, et al. Cannabis use is associated with 3years earlier onset of schizophrenia spectrum disorder in a naturalistic, multi-site sample (N=1119). Schizophr Res. 2016;170(1):217–221. | ||
Valmaggia L, Day F, Jones C, et al. Cannabis use and transition to psychosis in people at ultra-high risk. Psychol Med. 2014;44(12):2503–2512. | ||
Power BD, Dragovic M, Jablensky A, Stefanis NC. Does accumulating exposure to illicit drugs bring forward the age at onset in schizophrenia? Aust N Z J Psychiatry. 2013;47(1):51–58. | ||
van der Meer F, Meijer J, Meijer C, van den Brink W, Velthorst E. Cognitive functioning associated with stimulant use in patients with non-affective psychosis, their unaffected siblings and healthy controls. Psychol Med. 2014;44(9):1901–1911. | ||
Hasin DS, Saha TD, Kerridge BT, et al. Prevalence of marijuana use disorders in the United States between 2001-2002 and 2012-2013. JAMA Psychiatry. 2015;72(12):1235–1242. | ||
Koskinen J, Löhönen J, Koponen H, Isohanni M, Miettunen J. Rate of cannabis use disorders in clinical samples of patients with schizophrenia: a meta-analysis. Schizophr Bull. 2010;36(6):1115–1130. | ||
van Dijk D, Koeter MW, Hijman R, Kahn RS, van den Brink W. Effect of cannabis use on the course of schizophrenia in male patients: a prospective cohort study. Schizophr Res. 2012;137(1):50–57. | ||
Tosato S, Lasalvia A, Bonetto C, et al. The impact of cannabis use on age of onset and clinical characteristics in first-episode psychotic patients. Data from the Psychosis Incident Cohort Outcome Study (PICOS). J Psychiatr Res. 2013;47(4):438–444. | ||
Barrowclough C, Emsley R, Eisner E, Beardmore R, Wykes T. Does change in cannabis use in established psychosis affect clinical outcome? Schizophr Bull. 2013;39(2):339–348. | ||
Barrowclough C, Gregg L, Lobban F, Bucci S, Emsley R. The impact of cannabis use on clinical outcomes in recent onset psychosis. Schizophr Bull. 2015;41(2):382–390. | ||
Seddon JL, Birchwood M, Copello A, et al. Cannabis use is associated with increased psychotic symptoms and poorer psychosocial functioning in first-episode psychosis: a report from the UK national EDEN study. Schizophr Bull. 2015;42(3):619–625. | ||
Clausen L, Hjorthøj C, Thorup A, et al. Change in cannabis use, clinical symptoms and social functioning among patients with first-episode psychosis: a 5-year follow-up study of patients in the OPUS trial. Psychol Med. 2014;44(1):117–126. | ||
Szoke A, Galliot A-M, Richard J-R, et al. Association between cannabis use and schizotypal dimensions–a meta-analysis of cross-sectional studies. Psychiatry Res. 2014;219(1):58–66. | ||
Foglia E, Schoeler T, Klamerus E, Morgan K, Bhattacharyya S. Cannabis use and adherence to antipsychotic medication: a systematic review and meta-analysis. Psychol Med. 2017;47(10):1691–1705. | ||
Schoeler T, Petros N. Continued cannabis and substance use in the first 2 years following onset of psychosis. Schizophr Bull. 2017;43(Suppl_1):S80–S81. | ||
Bernardo M, Cañas F, Herrera B, Dorado MG. Adherence predicts symptomatic and psychosocial remission in schizophrenia: naturalistic study of patient integration in the community. Rev Psiquiatr Salud Ment. 2017;10(3):149–159. | ||
Schoeler T, Petros N, Di Forti M, et al. Poor medication adherence and risk of relapse associated with continued cannabis use in patients with first-episode psychosis: a prospective analysis. Lancet Psychiatry. 2017;4(8):627–633. | ||
Barch DM, Sheffield JM. Cognitive impairments in psychotic disorders: common mechanisms and measurement. World Psychiatry. 2014;13(3):224–232. | ||
Sánchez-Torres AM, Basterra V, Rosa A, et al. Lifetime cannabis use and cognition in patients with schizophrenia spectrum disorders and their unaffected siblings. Eur Arch Psychiatry Clin Neurosci. 2013;263(8):643–653. | ||
Power BD, Dragovic M, Badcock JC, et al. No additive effect of cannabis on cognition in schizophrenia. Schizophr Res. 2015;168(1):245–251. | ||
Waterreus A, Badcock JC, Di Prinzio P, Martin-Iverson M, Morgan VA. The impact of current cannabis use on general cognitive function in people with psychotic illness. Schizophr Res. 2017;190:164–171. | ||
Yücel M, Bora E, Lubman DI, et al. The impact of cannabis use on cognitive functioning in patients with schizophrenia: a meta-analysis of existing findings and new data in a first-episode sample. Schizophr Bull. 2012;38(2):316–330. | ||
Donoghue K, Doody GA. Effect of illegal substance use on cognitive function in individuals with a psychotic disorder, a review and meta-analysis. Neuropsychology. 2012;26(6):785–801. | ||
Rabin RA, Barr MS, Goodman MS, et al. Effects of extended cannabis abstinence on cognitive outcomes in cannabis dependent patients with schizophrenia vs non-psychiatric controls. Neuropsychopharmacology. 2017;42(11):2259–2271. | ||
Schoeler T, Kambeitz J, Behlke I, Murray R, Bhattacharyya S. The effects of cannabis on memory function in users with and without a psychotic disorder: findings from a combined meta-analysis. Psychol Med. 2016;46(1):177–188. | ||
Batalla A, Bhattacharyya S, Yücel M, et al. Structural and functional imaging studies in chronic cannabis users: a systematic review of adolescent and adult findings. PLoS One. 2013;8(2):e55821. | ||
Van Ameringen M, Mancini C, Patterson B, Boyle MH. Post-traumatic stress disorder in Canada. CNS Neurosci Ther. 2008;14(3):171–181. | ||
Ipser JC, Stein DJ. Evidence-based pharmacotherapy of post-traumatic stress disorder (PTSD). Int J Neuropsychopharmacol. 2012;15(6):825–840. | ||
Fraser GA. The use of a synthetic cannabinoid in the management of treatment-resistant nightmares in posttraumatic stress disorder (PTSD). CNS Neurosci Ther. 2009;15(1):84–88. | ||
Roitman P, Mechoulam R, Cooper-Kazaz R, Shalev A. Preliminary, open-label, pilot study of add-on oral Delta9-tetrahydrocannabinol in chronic post-traumatic stress disorder. Clin Drug Investig. 2014;34(8):587–591. | ||
Jetly R, Heber A, Fraser G, Boisvert D. The efficacy of nabilone, a synthetic cannabinoid, in the treatment of PTSD-associated nightmares: a preliminary randomized, double-blind, placebo-controlled cross-over design study. Psychoneuroendocrinology. 2015;51:585–588. | ||
ClinicalTrials.gov. Identifier: NCT02517424, Evaluating Safety and Efficacy of Cannabis in Participants With Chronic Posttraumatic Stress Disorder; 2015. Available from: https://clinicaltrials.gov/show/NCT02517424. Accessed November 1, 2017. | ||
Identifier: 192675, Placebo-Controlled, Triple-Blind, Crossover Study of the Safety and Efficacy of Three Different Potencies of Vaporized Cannabis in 42 Participants with Chronic, Treatment-Resistant Posttraumatic Stress Disorder (PTSD); 2016. Available from: https://health-products.canada.ca/ctdb-bdec/search-recherche.do;jsessionid=831B8B6717B50580890DCCBED62CBCCE. Accessed November 1, 2017. | ||
Park B, Gibbons H, Mitchell M, Glass M. Identification of the CB1 cannabinoid receptor and fatty acid amide hydrolase (FAAH) in the human placenta. Placenta. 2003;24(10):990–995. | ||
Hutchings DE, Martin BR, Gamagaris Z, Miller N, Fico T. Plasma concentrations of delta-9-tetrahydrocannabinol in dams and fetuses following acute or multiple prenatal dosing in rats. Life Sci. 1989;44(11):697–701. | ||
Bailey J, Cunny H, Paule M, Slikker W. Fetal disposition of Δ9-tetrahydrocannabinol (THC) during late pregnancy in the rhesus monkey. Toxicol Appl Pharmacol. 1987;90(2):315–321. | ||
Perez-Reyes M, Wall M. Presence of AMetrahydrocannabinol in human milk. N Engl J Med. 1982;307(13):819–820. | ||
Hurd Y, Wang X, Anderson V, Beck O, Minkoff H, Dow-Edwards D. Marijuana impairs growth in mid-gestation fetuses. Neurotoxicol Teratol. 2005;27(2):221–229. | ||
El Marroun H, Tiemeier H, Steegers EA, et al. Intrauterine cannabis exposure affects fetal growth trajectories: the Generation R Study. J Am Acad Child Adolesc Psychiatry. 2009;48(12):1173–1181. | ||
Gray TR, Eiden RD, Leonard KE, Connors GJ, Shisler S, Huestis MA. Identifying prenatal cannabis exposure and effects of concurrent tobacco exposure on neonatal growth. Clin Chem. 2010;56(9):1442–1450. | ||
Scragg R, Mitchell E, Ford R, Thompson J, Taylor B, Stewart A. Maternal cannabis use in the sudden death syndrome. Acta Paediatr. 2001;90(1):57–60. | ||
Shiono PH, Klebanoff MA, Nugent RP, et al. The impact of cocaine and marijuana use on low birth weight and preterm birth: a multicenter study. Am J Obstet Gynecol. 1995;172(1):19–27. | ||
Fried PA, Watkinson B, Gray R. Growth from birth to early adolescence in offspring prenatally exposed to cigarettes and marijuana. Neurotoxicol Teratol. 1999;21(5):513–525. | ||
van Gelder MM, Reefhuis J, Caton AR, Werler MM, Druschel CM, Roeleveld N. Characteristics of pregnant illicit drug users and associations between cannabis use and perinatal outcome in a population-based study. Drug Alcohol Depend. 2010;109(1):243–247. | ||
Fried P. Conceptual issues in behavioral teratology and their application in determining long-term sequelae of prenatal marihuana exposure. J Child Psychol Psychiatry. 2002;43(1):81–102. | ||
Richardson GA, Ryan C, Willford J, Day NL, Goldschmidt L. Prenatal alcohol and marijuana exposure: effects on neuropsychological outcomes at 10 years. Neurotoxicol Teratol. 2002;24(3):309–320. | ||
Astley SJ, Little RE. Maternal marijuana use during lactation and infant development at one year. Neurotoxicol Teratol. 1990;12(2):161–168. | ||
Gunn J, Rosales C, Center K, et al. Prenatal exposure to cannabis and maternal and child health outcomes: a systematic review and meta-analysis. BMJ open. 2016;6(4):e009986. | ||
Chabarria KC, Racusin DA, Antony KM, et al. Marijuana use and its effects in pregnancy. Am J Obstet Gynecol. 2016;215(4):506.e501–506.e507. | ||
Hasin DS, Kerridge BT, Saha TD, et al. Prevalence and correlates of DSM-5 cannabis use disorder, 2012-2013: findings from the National Epidemiologic Survey on Alcohol and Related Conditions–III. Am J Psychiatry. 2016;173(6):588–599. | ||
Mark K, Desai A, Terplan M. Marijuana use and pregnancy: prevalence, associated characteristics, and birth outcomes. Arch Womens Ment Health. 2016;19(1):105–111. | ||
Metz TD, Allshouse AA, Hogue CJR, et al. Maternal marijuana use, adverse pregnancy outcomes and neonatal morbidity. Am J Obstet Gynecol. 2017;217(4):478.e1–478.e8. | ||
Warshak C, Regan J, Moore B, Magner K, Kritzer S, Van Hook J. Association between marijuana use and adverse obstetrical and neonatal outcomes. J Perinatol. 2015;35(12):991. | ||
Fried PA, James DS, Watkinson B. Growth and pubertal milestones during adolescence in offspring prenatally exposed to cigarettes and marihuana. Neurotoxicol Teratol. 2001;23(5):431–436. | ||
Fried P, Watkinson B. 12-and 24-month neurobehavioural follow-up of children prenatally exposed to marihuana, cigarettes and alcohol. Neurotoxicol Teratol. 1988;10(4):305–313. | ||
Richardson GA, Day NL, Goldschmidt L. Prenatal alcohol, marijuana, and tobacco use: infant mental and motor development. Neurotoxicol Teratol. 1995;17(4):479–487. | ||
El Marroun H, Tiemeier H, Steegers EA, et al. A prospective study on intrauterine cannabis exposure and fetal blood flow. Early Hum Dev. 2010;86(4):231–236. | ||
Fried PA, Watkinson B, Gray R. Differential effects on cognitive functioning in 9- to 12-year olds prenatally exposed to cigarettes and marihuana. Neurotoxicol Teratol. 1998;20(3):293–306. | ||
Cascini F, Aiello C, Di Tanna G. Increasing delta-9-tetrahydrocannabinol (Δ-9-THC) content in herbal cannabis over time: systematic review and meta-analysis. Curr Drug Abuse Rev. 2012;5(1):32-40. | ||
Health Canada. National report: apparent opioid-related deaths (2016); 2017. Available from: https://www.canada.ca/en/health-canada/services/substance-abuse/prescription-drug-abuse/opioids/national-report-apparent-opioid-related-deaths.html. Accessed November 1, 2017. | ||
Bart G. Maintenance medication for opiate addiction: the foundation of recovery. J Addict Dis. 2012;31(3):207–225. | ||
Epstein DH, Preston KL. No evidence for reduction of opioid-withdrawal symptoms by cannabis smoking during a methadone dose taper. Am J Addict. 2015;24(4):323–328. | ||
Zuardi AW. Cannabidiol: from an inactive cannabinoid to a drug with wide spectrum of action. Rev Bras Psiquiatr. 2008;30:271–280. | ||
Health Canada. Best Practices: Methadone Maintenance Treatment; 2002. Available from: http://www.hc-sc.gc.ca/hc-ps/alt_formats/hecs-sesc/pdf/pubs/adp-apd/methadone-bp-mp/methadone-bp-mp-eng.pdf. Accessed November 1, 2017. | ||
Johansson EVA, Agurell S, Hollister LE, Halldin MM. Prolonged apparent half-life of Δ1-tetrahydrocannabinol in plasma of chronic marijuana users. J Pharm Pharmacol. 1988;40(5):374–375. | ||
Wall ME, Sadler BM, Brine D, Taylor H, Perez-Reyes M. Metabolism, disposition, and kinetics of delta-9-tetrahydrocannabinol in men and women. Clin Pharmacol Ther. 1983;34(3):352–363. | ||
Bergamaschi MM, Karschner EL, Goodwin RS, et al. Impact of prolonged cannabinoid excretion in chronic daily cannabis smokers’ blood on per se drugged driving laws. Clin Chem. 2013;59(3):519–526. | ||
Matias I, Belluomo I, Cota D. The fat side of the endocannabinoid system: role of endocannabinoids in the adipocyte. Cannabis Cannabinoid Res. 2016;1(1):176–185. | ||
Di Marzo V, Berrendero F, Bisogno T, et al. Enhancement of anandamide formation in the limbic forebrain and reduction of endocannabinoid contents in the striatum of delta9-tetrahydrocannabinol-tolerant rats. J Neurochem. 2000;74(4):1627–1635. | ||
Gonzalez S, Cebeira M, Fernandez-Ruiz J. Cannabinoid tolerance and dependence: a review of studies in laboratory animals. Pharmacol Biochem Behav. 2005;81(2):300–318. | ||
Haney M, Ward AS, Comer SD, Foltin RW, Fischman MW. Abstinence symptoms following oral THC administration to humans. Psychopharmacology. 1999;141(4):385–394. | ||
Jones RT, Benowitz NL, Herning RI. Clinical relevance of cannabis tolerance and dependence. J Clin Pharmacol. 1981;21(8–9 Suppl):143s–152s. | ||
Hall W, Solowij N. Adverse effects of cannabis. Lancet. 1998; 352(9140):1611–1616. | ||
Vandrey R, Haney M. Pharmacotherapy for cannabis dependence: how close are we? CNS Drugs. 2009;23(7):543–553. | ||
Lopez-Quintero C, de los Cobos JP, Hasin DS, et al. Probability and predictors of transition from first use to dependence on nicotine, alcohol, cannabis, and cocaine: Results of the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC). Drug Alcohol Depend. 2011;115(1–2):120–130. | ||
Budney AJ, Roffman R, Stephens RS, Walker D. Marijuana dependence and its treatment. Addict Sci Clin Pract. 2007;4(1):4–16. | ||
Vandrey R, Stitzer ML, Mintzer MZ, Huestis MA, Murray JA, Lee D. The dose effects of short-term dronabinol (oral THC) maintenance in daily cannabis users. Drug Alcohol Depend. 2013;128(1–2):64–70. | ||
Allsop DJ, Copeland J, Lintzeris N, et al. Nabiximols as an agonist replacement therapy during cannabis withdrawal: a randomized clinical trial. JAMA Psychiatry. 2014;71(3):281–291. | ||
Trigo JM, Lagzdins D, Rehm J, et al. Effects of fixed or self-titrated dosages of Sativex on cannabis withdrawal and cravings. Drug Alcohol Depend. 2016;161:298–306. | ||
Abrams DI, Couey P, Shade SB, Kelly ME, Benowitz NL. Cannabinoid-opioid interaction in chronic pain. Clin Pharmacol Ther. 2011;90(6):844–851. | ||
McRae-Clark AL, Baker NL, Gray KM, Killeen T, Hartwell KJ, Simonian SJ. Vilazodone for cannabis dependence: a randomized, controlled pilot trial. Am J Addict. 2016;25(1):69–75. | ||
Weinstein AM, Miller H, Bluvstein I, et al. Treatment of cannabis dependence using escitalopram in combination with cognitive-behavior therapy: a double-blind placebo-controlled study. Am J Drug Alcohol Abuse. 2014;40(1):16–22. | ||
McRae-Clark AL, Baker NL, Gray KM, et al. Buspirone treatment of cannabis dependence: a randomized, placebo-controlled trial. Drug Alcohol Depend. 2015;156:29–37. | ||
Johnston J, Lintzeris N, Allsop DJ, et al. Lithium carbonate in the management of cannabis withdrawal: a randomized placebo-controlled trial in an inpatient setting. Psychopharmacology. 2014;231(24):4623–4636. | ||
Levin FR, Mariani JJ, Pavlicova M, et al. Dronabinol and lofexidine for cannabis use disorder: a randomized, double-blind, placebo-controlled trial. Drug Alcohol Depend. 2016;159:53–60. | ||
Mason BJ, Crean R, Goodell V, et al. A proof-of-concept randomized controlled study of gabapentin: effects on cannabis use, withdrawal and executive function deficits in cannabis-dependent adults. Neuropsychopharmacology. 2012;37(7):1689–1698. | ||
Schifano F. Misuse and abuse of pregabalin and gabapentin: cause for concern? CNS Drugs. 2014;28(6):491–496. | ||
Smith RV, Havens JR, Walsh SL. Gabapentin misuse, abuse and diversion: a systematic review. Addiction. 2016;111(7):1160–1174. | ||
Mersfelder TL, Nichols WH. Gabapentin: abuse, dependence, and withdrawal. Ann Pharmacother. 2016;50(3):229–233. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.



