Back to Journals » Therapeutics and Clinical Risk Management » Volume 10
Superselective transcatheter renal artery embolization for the treatment of hemorrhage from non-iatrogenic blunt renal trauma: report of 16 clinical cases
Authors Rao D, Yu H, Zhu H, Yu K, Hu X, Xie L, Jin S
Received 24 December 2013
Accepted for publication 17 March 2014
Published 16 June 2014 Volume 2014:10 Pages 455—458
DOI https://doi.org/10.2147/TCRM.S59671
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Dapang Rao,1 Haifeng Yu,2 Haibo Zhu,2 Kaiyuan Yu,2 Xiao Hu,3 Liping Xie1
1Department of Urology, First Affiliated Hospital, Medical College, Zhejiang University, Hangzhou, People's Republic of China; 2Department of Urology, Second Affiliated Hospital of Wenzhou Medical College, Wenzhou, People’s Republic of China; 3Zhejiang University Medical College, Hangzhou, People’s Republic of China
Objective: To explore the therapeutic efficacy and outcome of superselective transcatheter renal artery embolization for the treatment of hemorrhage from non-iatrogenic blunt renal trauma (BRT).
Methods: Sixteen patients who received superselective transcatheter renal artery embolization for non-iatrogenic BRT hemorrhage between January 2003 and December 2012 were reviewed retrospectively. Spring steel coils with gelatin sponge particles were used to embolize branches of the renal artery in 15 patients with injuries to the segmental or distal renal arteries; superselective internal iliac artery branch embolization was used to occlude hemorrhage from the branch of the renal artery in two patients with pelvic fracture complicated with internal iliac artery branch laceration; and balloon catheter occlusion was used to embolize the branch of the renal artery in one patient with renal artery trunk laceration.
Results: Embolization was achieved successfully in a one-stop procedure in all cases. The patient who received balloon catheter occlusion for renal artery trunk laceration was transferred immediately to surgery for emergency nephrectomy. Another patient died of intracranial trauma 1 day after surgery, although macroscopic hematuria disappeared at the time. Macroscopic hematuria disappeared within 1 day after surgery in the other 14 patients. Follow-up visits at times ranging from 6 months to 9 years after the procedure showed normal renal function without evidence of complications in all surviving patients.
Conclusion: Superselective transcatheter renal artery embolization is an effective minimally invasive therapy for the treatment of BRT hemorrhage.
Keywords: blunt renal trauma, superselective cannulation, renal artery embolization
Introduction
Renal injuries include injury to the renal parenchyma, pelvis, and pedicle. In most cases they are usually mild and can be cured spontaneously with conservative treatment.1,2 However, surgical intervention is often necessary in patients whose perirenal hemorrhage extends progressively, and whose hemodynamics remains unstable despite positive anti-shock treatment.3 With advances in intervention technology in recent years, superselective transcatheter artery embolization has come into widespread use and has become an important and effective option for the treatment of traumatic renal hemorrhage.4 This article reports our experience with the successful use of superselective transcatheter renal artery embolization for the treatment of 16 patients with hemorrhage from non-iatrogenic blunt renal trauma (BRT) between January 2003 and December 2012.
Material and methods
Clinical data
The 16 patients with non-iatrogenic BRT hemorrhage included eleven men and five women ranging in age from 18 to 61 years with a mean age of 34.7 years. Of these, 13 patients were injured in road traffic accidents, two were injured as a result of falling from a height, and one was injured by a blunt object. Abdominal B-ultrasound and chest-abdominal plain computed tomography (CT) scans showed complications of unstable pelvic fracture in two cases, cerebral laceration and contusion in two cases, liver rupture in one case, and hemopneumothorax in one case. The remaining ten cases had simple renal lacerations. After emergency fluid replacement, transfusion and anti-shock therapies, blood pressure remained unstable. Digital subtract angiography (DSA) and superselective transcatheter renal artery embolization were performed. Intraoperative DSA showed grade III injury in 12 cases, grade IV injury in three cases, and grade V injury in one case according to the 1996 American Association for the Surgery of Trauma guidelines for injury classification.5,6,7
Treatment
All the instruments were purchased from ASAHI INTECC CO., LTD., Aichi, Japan. A modified Seldinger technique of renal angiography4 was employed via the left or right femoral artery to insert the approximately 5–6F Cobra catheter selectively into the opening of the renal artery, which was confirmed by manual push of 3–5 mL contrast medium. Subsequently, Ultravist® (Bayer AG, Leverkusen, Germany) or Omnipaque™ (GE Healthcare Japan Corporation, Tokyo, Japan), was injected via a high-pressure syringe at a total dose of approximately 15–30 mL, a flow rate of approximately 3–4 mL/s and a pressure of approximately 300–500 PI. The location and degree of hemorrhage were determined by effusion of the contrast medium or pseudoaneurysm formation. Superselective cannulation was performed under the guidance of the super smooth guide wire. The head end of the Margaret II micro catheter was inserted to the renal artery branch of the affected site. In cases with simple renal artery hemorrhage, a 300–700 μm particle was used to embolize the trunk of the grade III branch, and in cases complicated with pseudoaneurysm, the embolization was enhanced by the use of spring steel coils. Angiography was performed again 5–10 minutes after embolization. Embolization would be performed again should there be effusion of the contrast medium. The arterial catheter was removed when no effusion of the contrast medium was confirmed. The femoral puncture site was compressed manually for 15 minutes and then pressure dressed. Balloon-catheter-guided embolization (first the balloon catheter was used to occlude the renal artery, and then a switch was made to a spring steel ring and face glue embolization, before removing the balloon catheter) was performed first in the patient with renal artery trunk laceration, and the same method was used to stop bleeding in the patient complicated with pelvic fracture. As angiography did not show effusion of the contrast medium in the patient complicated with liver rupture, no special treatment was applied to the hemorrhagic focus. Preoperative thoracic closed drainage was applied in the patient complicated with hemopneumothorax. As no sign of cerebral hernia was detected preoperatively in the two patients complicated with cerebral injury, vascular embolization for the renal laceration was performed first (Figure 1 and 2).
  | Figure 1 Before treatment two segmental renal arteries, both the anterior and the posterior branches, were injured, (the arrows point to the bleeding sites). |
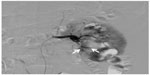  | Figure 2 After treatment two segmental renal arteries, both the anterior and the posterior branches, were injured, (the arrows point to the embolization sites). |
Results
Renal arteriography presented as injuries to the segmental or distal renal arteries, including injuries to the anterior branch in seven cases, to the posterior branch in five cases, to both the anterior and the posterior branches in three cases, and to the renal artery trunk in one case. In the one patient complicated with pelvic fracture, hemorrhage rose from rupture of the internal iliac artery branch, and in the patient complicated with liver rupture, hemorrhage rose from rupture of the right hepatic lobe. Blood pressure, hemoglobin and hematocrit became stable within 1 hour of embolization in all cases, and macroscopic hematuria disappeared completely 1 day after surgery in all 16 cases. There was one patient who died of cerebral trauma 3 days after surgery, although his macroscopic hematuria also disappeared at the time. The patient who received balloon catheter occlusion for renal artery trunk laceration was transferred immediately to surgery for an emergency nephrectomy. Three patients in our series developed post-embolization syndrome, presenting as nausea and vomiting, local abdominal distension and low-grade fever. These symptoms disappeared 3–7 days after symptomatic treatment. The 15 surviving patients were followed up for periods from 8 months to 9 years, with a mean of 6 years and 8 months, showing that the outcome was good without recurrence of hemorrhage or renovascular hypertension. Intravenous urography 6 months after surgery showed good renal function in the 14 patients who received kidney-preservation surgery.
Discussion
Renal injuries are common in the urinary system. They are treated in different ways according to the type of injury and the presence or absence of severe complications. For renal laceration and contusion, conservative treatment is often preferred unless it is ineffective. Surgical treatment includes renal repair, and partial or complete nephrectomy. However, open surgery has obvious disadvantages, including: 1) difficulty in identifying the affected part or finding injuries to small renal arteries, and the low intraoperative detection rate of hemorrhage; 2) the low success rate of intraoperative hemostasis because of tissue adhesion and unclear anatomic structures due to iatrogenic renal injury; 3) difficulty in quickly finding extrarenal bleeding points so that hemostasis is often ineffective, especially in cases complicated with pelvic fracture and injuries to other solid organs; and 4) the likelihood of secondary hemorrhage after renal repair or partial nephrectomy; to prevent this from occurring, intraoperative resection of the affected kidney is often recommended.8 Considering the iatrogenic trauma, the unreliability of the outcome, and the great physiological and psychological impact, most patients are reluctant to receive open surgery.
Since 1973 when Bookstein and Ernst9 reported successful use of the renal artery embolization technique for the treatment of BRT hemorrhage, this technique has been increasingly applied to clinical practices owing to simple manipulation, few surgical contraindications, high technical success, curative effectiveness, and few complications. Ample evidence has demonstrated that selective renal artery embolization is the optimal option for the treatment of postoperative hemorrhage arising from severe renal trauma, arteriovenous (A-V) shunt, renal biopsy, lithotomy, and fistulation.10,11 Indications for arteriography of the affected kidney and superselective renal artery embolization are:
- continuous increasing perirenal hematoma;
- severe renal injuries such as renal lacerations;
- renal A-V fistula or pseudoaneurysm formation; and
- persistent hematuria or fall of blood pressure after active Anti shock therapy.11
However, open surgery is still suggested in cases with both arterial and venous vascular injuries or pelvic injuries.11 Before initiation of this intervention therapy, CT and other imaging examinations should be performed, to confirm the location and degree of injury and determine whether or not there are complicated injuries to the brain, lungs and other organs in the pelvic and abdominal cavities, as long as conditions permit, after emergency fluid resuscitation and anti-shock treatment. The 16 patients in our study all received a whole-body CT scan and preoperative renal arteriography, confirming that hemorrhage was in the renal artery or the segmental or distal renal artery branches. There was one patient who received balloon-catheter occlusion for renal artery trunk laceration and was transferred immediately to surgery for emergency nephrectomy. In the remaining 15 patients, superselective cannulation was performed to the hemorrhagic artery, and spring steel coils with gelatin sponge particles were used to permanently embolize the affected artery. Hematuria disappeared 5–12 days after surgery, indicating that the hemostatic effect was satisfactory. In addition, no significant impairment to renal function was observed after surgery. Internal iliac angiography showed rupture of the arterial branches in two patients complicated with pelvic fracture, in whom artery embolization was performed successfully. It is reported in the literature that the success rate of using arterial embolization for the treatment of hemorrhage from pelvic fracture is 85%–94%.12
Short-term complications after superselective renal artery embolization include embolization syndrome, recurrence of renal hemorrhage due to falling off of emboli, renal function impairment, and nephrogenic hypertension. Long-term complications include perirenal or renal abscess, renal function impairment, and nephrogenic hypertension.10 It is often difficult to identify embolization syndrome because it may be confused with, or clouded by, the underlying traumatic symptoms. Three patients in our series developed post-embolization syndrome presenting as nausea and vomiting, local abdominal distension and low-grade fever. These symptoms disappeared after symptomatic treatment on the basis of excluding any significant cerebral injury. Renovascular hypertension from non-specific embolism of the renal artery branch is a more serious complication. Although it is quite rare, it may lead to nephrectomy. No postoperative nephrogenic hypertension, perirenal abscess or renal function impairment was observed in our 14 patients who received kidney-preservation surgery during the follow-up periods from 8 months to 9 years.
In conclusion, superselective transcatheter renal artery embolization is an effective, minimally invasive option for the treatment of BRT hemorrhage, and is well worthy of wider clinical applications.
Disclosure
The authors report no conflict of interest in this work.
References
Santucci RA, Wessells H, Bartsch G, et al. Evaluation and management of renal injuries: consensus statement of the renal trauma subcommittee. BJU Int. 2004;93:937–954. | |
Gourgiotis S, Germanos S, Dimopoulos N, Vougas V, Anastasiou T, Baratsis S. Renal injury: 5-year experience and literature review. Urol Int. 2006;77:97–103. | |
McAninch JW, Carroll PR, Klosterman PW, Dixon CM, Greenblatt MN. Renal reconstruction after injury. J Urol. 1991;145(5):932–937. | |
Sofocleous CT, Hinrichs C, Hubbi B, et al. Angiographic findings and embolotherapy in renal arterial trauma. Cardiovasc Intervent Radiol. 2005;28(1):39–47. | |
Kuan JK, Wright JL, Nathens AB, Rivara FP, Wessells H. American Association for the Surgery of Trauma Organ Injury Scale for kidney injuries predicts nephrectomy, dialysis, and death in patients with blunt injury and nephrectomy for penetrating injuries. J Trauma. 2006;60:351–356. | |
Tinkoff G, Esposito TJ, Reed J, Kilgo P, Fildes J, Meredith JW. American Association for the Surgery of Trauma Organ Injury Scale I: spleen, liver, and kidney, validation based on the National Trauma Data Bank. J Am Coll Surg. 2008;207(5):646–655. | |
Shariat SF, Roehrborn CG, Karakiewicz PI, Dhami G, Stage KH. Evidence-based validation of the predictive value of the American Association for the Surgery of Trauma kidney injury scale. J Trauma. 2007;62:933–939. | |
Buckley JC, McAninch JW. Selective management of isolated and nonisolated grade IV renal injuries. J Urol. 2006;176(6 Pt 1):2498–2502. | |
Bookstein JJ, Ernst CB. Vasodilatory and vasoconstrictive pharmacoangiographic manipulation of renal collateral flow. Radiology. 1973;108(1):55–59. | |
Dinkel HP, Danuser H, Triller J. Blunt renal trauma: minimally invasive management with microcatheter embolization experience in nine patients. Radiology. 2002;223(3):723–730. | |
Breyer BN, McAninch JW, Elliott SP, Master VA. Minimally invasive endovascular techniques to treat acute renal hemorrhage. J Urol. 2008;179:2248–2252. | |
Dondelinger RF, Trotteur G, Ghaye B, Szapiro D. Traumatic injuries: radiological hemostatic intervention at admission. Eur Radiol. 2002;12(5):979–993. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
