Back to Journals » Therapeutics and Clinical Risk Management » Volume 15
Severe Atopic Dermatitis In Spain: A Real-Life Observational Study
Authors Sicras-Mainar A, Navarro-Artieda R, Armario-Hita JC
Received 8 August 2019
Accepted for publication 3 November 2019
Published 2 December 2019 Volume 2019:15 Pages 1393—1401
DOI https://doi.org/10.2147/TCRM.S226456
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Garry Walsh
Antoni Sicras-Mainar,1 Ruth Navarro-Artieda,2 José C Armario-Hita3
1Scientific Direction, Real Life Data, Madrid, Spain; 2Medical Documentation, Germans Trias i Pujol Hospital, Barcelona, Spain; 3Dermatology Service, Puerto Real University Hospital, Cadiz University, Cádiz, Spain
Correspondence: Antoni Sicras-Mainar
Scientific Direction, Real Life Data, c/Cronos, 24–26, P3 - Bajo E36, Madrid 08037, Spain
Tel +34 91 007 15 92
Email [email protected]
Objective: To determine the epidemiology and characterize the treatment prescribed for severe atopic dermatitis (AD) in children/adults in usual clinical practice.
Methods: Observational, retrospective study made through review of medical records of Spanish patients aged ≥6 years. Patients diagnosed with severe AD who required care between 2013 and 2017 were included. The study groups were: 6–12 years; 13–18 years; and > 18 years. Patients were followed for 5 years. The main measurements were the prevalence of AD, comorbidity and treatment duration. Statistical significance was established as p <0.05.
Results: We included 2323 patients with severe AD. The overall prevalence was 0.10% (95% CI: 0.09–0.11%) and was 0.39%, 0.23% and 0.07% in the 6–12 years, 13–18 years and >18 years age groups, respectively (p <0.001), the percentage of males was 58%, 48.6% and 39%, respectively, and general comorbidity was 0.1, 0.2 and 0.9 points, respectively (p <0.001).The most frequent comorbidities were asthma in 49.0%, 44.9% and 20.8%, respectively (p <0.001), and anxiety in 79.7%, 65.8% and 67.3%, respectively (p <0.001). Oral corticosteroids were administered in 97.3%, 90.9% and 81.7%, respectively (concomitant-medication). Cyclosporine (45.3%), azathioprine (15.9%) and methotrexate (9.0%) were the most frequently prescribed drugs; biologic agents were administered in 5.8% of patients (for AD).
Conclusion: In AD the presence of comorbidities was significant, especially in the psychological, immunoallergic and cardiovascular areas. Cyclosporine was the most widely used immunosuppressant. There was a degree of variability in the use and duration of the treatments prescribed.
Keywords: severe atopic dermatitis, epidemiology, comorbidity, treatment, immunosuppressants, biologics
Introduction
Atopic dermatitis (AD) is a recurrent chronic inflammatory skin disease.1 It is pruritic, and the morphological expression varies with age, although there is a predominance of recurrent eczematous forms.2 The aetiology is unknown but involves genetic factors and a combination of allergic and non-allergic-based immune factors, such as epidermal barrier dysfunction, and environmental trigger factors.1,2
The prevalence varies but may affect up to 10% of the general population, of whom up to 15–30% have moderate/severe forms, that may affect up to 10–20% in children and 1–5% in adults, especially in developed countries.3–5 Reports suggest that mild infantile forms disappear after puberty in up to 75% of cases. The prevalence incidence is higher in females, although in childhood there is a predominance of males.2
AD has a significant economic impact and affects the quality of life and the psychosocial wellbeing of patients and families, increasing the risk of food allergies, asthma, allergic rhinitis, other inflammatory autoimmune diseases, and mental health disorders.6–8 Inflammatory flares may affect the entire skin and results in complications such as dehydration, hypernatremia, and cutaneous and systemic infection. Patients with a family history, a late onset, disseminated disease in childhood, females and patients in whom AD is associated with other allergic pathologies, such as asthma and rhinitis, have a worse prognosis. Adult AD is usually severe.1,9 In the severe forms of AD, drugs are used systemically and, although there is a considerable variation in the specific drug used, the clinical response is frequently insufficient, in addition to the burden of frequent adverse events.10,11
Topical corticosteroids are the cornerstone of pharmacological treatment.1,2 However, in moderate/severe cases, a wide variety of medications is used, some of which do not have an approved indication, including topical immunomodulators (tacrolimus and pimecrolimus), oral corticosteroids, cyclosporine, azathioprine, mycophenolate mofetil, methotrexate, cyclophosphamide, biologic agents (omalizumab, rituximab, etanercept, adalimumab, ustekinumab, infliximab, secukinumab), apremilast, intravenous immunoglobulins and/or interferon gamma. Current advances in the long-term treatment of AD suggest that better symptom management may have a greater impact on quality of life. Prevention of the cardiovascular comorbidity associated with severe forms of AD may result in increased longevity and decreased mortality in patients with AD.12,13
Available population-based evidence on the prevalence of severe AD is unclear and poorly documented, with only a few case series reports from specialized care, mainly by dermatologists, but with little evidence on the impact in the population. In Spain, there are no population-based studies. Nowadays, there is a growing need for naturalistic studies, representative of the real clinical conditions of health interventions that adequately reflect the impact on these patients from a population-based perspective. The objective of this study was to determine and characterize the treatment prescribed for severe AD in Spanish children and adults in usual clinical practice and quantify the prevalence of associated comorbidities.
Patients And Methods
Design And Study Population
An observational, multicentre, longitudinal retrospective study was performed based on review of medical records (computerized databases, with dissociated data) and complementary databases from seven Spanish Regions. The sample analysed was of 2.2 million patients, with wide representativeness of the Spanish population. The sample was obtained from health databases of various Spanish centres (unified in the BIG-PAC, Real Life Data dissociated database: http://www.encepp.eu/encepp/search.htm). The population analysed was mostly urban, with low-medium socioeconomic status, and predominantly industrial.
Inclusion And Exclusion Criteria
Patients requesting care with regard to AD between 2013 and 2017 were included. For the recruitment period, the last available date was considered the index date. Inclusion criteria were: a) age ≥ 6 years, b) patients with a diagnosis of AD of a least one year prior to the index date, c) patients prescribed of any medication for AD (with verification of the dosage, the time interval and duration of each treatment administered), d) patients receiving ≥ 2 prescriptions during the follow-up period, e) patients who underwent regular monitoring (≥ 2 health records in the computerized system, including ≥ 1 dermatology unit visit. Exclusion criteria were: a) subjects transferred out to other centres or regions or due to change of address, b) permanently-institutionalized patients, and c) patients with a history of seborrhoeic dermatitis, contact dermatitis and/or fungal eczema.
Study Groups
Three age groups were differentiated: 6–12 years, 13–18 years, and > 18 years. Patients were followed retrospectively for 5 years from the date of inclusion/index.
Description Of Severe Atopic Dermatitis
Records of patients with AD were obtained according to the International Classification of Diseases (ninth edition) Clinical Modification (ICD-9-CM; 691.8, 692.9, 706.8), and/or ICD-10-CM (L20, L28, L85.3), which includes AD, allergic dermatitis, allergic eczema, atopic eczema and atopic neurodermatitis. The diagnosis of AD was made by the reference dermatologist according to the Hanifin and Rajka criteria.14 Severe AD was defined by the following criteria: a) the administration of immunosuppressive treatment, b) the administration of biological treatment, and/or c) hospitalization due to an AD flare.
Sociodemographic And Comorbidity Variables
The following variables were collected: age (continuous and by ranges), sex, time since diagnosis, the history of hypertension, diabetes, dyslipidaemia, ischemic heart disease, cerebrovascular accident, heart/kidney failure, COPD, bronchial asthma, allergic rhinitis, depressive syndrome, anxiety or agitation, celiac disease, and the body mass index (BMI, Kg/m2). As a summary variable of general comorbidity, the Charlson comorbidity index15 was used as an approximation to the severity of the patient, and the number of chronic comorbidities. In addition, the comorbidities of patients with severe AD were compared with those of the general population through pairing by age and sex.
Medication Administered
The medication (active ingredients and biological drugs) indicated for the treatment of severe AD were obtained according to the Anatomical Therapeutic Chemical Classification System (ATC).16 The information was obtained from the records of pharmacological prescriptions of medicines and/or hospital pharmacy services. The choice of drug was at the physician’s discretion. The following medications were collected: a) immunosuppressants (frequent use in AD): cyclosporine (L04AD01), methotrexate (L04AX03), azathioprine (L04AX01), mycophenolate mofetil (L04AA06), cyclophosphamide (L01AA01); b) biological agents: omalizumab (R03DX05), rituximab (L01XC*), infliximab (L04AB02), secukinumab (L04AC10), ustekinumab (L04AC05), tocilizumab (L04AC07), mepolizumab (R03DX09); and c) other medications (indication not approved): apremilast (L04AA32), immunoglobulins (J06B*), interferon-gamma (L03AB*), hydroxychloroquine (P01BA*), tofacitinib (L04AA29) and baricitinib (L04AA37). Number of treatment cycles of immunosuppressants and the duration of biological therapy were recorded. Systemic corticosteroids (H02A*) administered in patients with severe AD were quantified as rescue treatment (concomitant-medication).
Epidemiology: Prevalence
The prevalence rate was calculated according to patients diagnosed with AD by a dermatologist and prescribed of immunosuppressant or biological agents and/or hospitalized (numerator), as a proportion of patients assigned to primary healthcare centres (denominator). Standardization of the results was not required, due to the similarity of the demographic characteristics of the sample in comparison with general Spanish population.
Confidentiality Of Information
Data confidentiality (anonymous and dissociated) was respected according to the Spanish Organic Law on Data Protection (Law 15/1999 of December 13). The study was classified by the Spanish Agency for Medicines and Health Products (EPA-OD), and was approved by the Clinical Research Ethics Committee, International University of Catalonia (Barcelona).
Statistical Analysis
A data validation was carried out to ensure the quality of the results. Descriptive statistics were expressed as absolute and relative frequencies. Qualitative data was presented in percentage and 95% confidence intervals (CI). Data was retrieved according to the total number of subjects with non-missing records. Means and standard deviation (SD) were used to describe quantitative data. A bivariate analysis was made according to the distribution of data (chi-square test or ANOVA). Comorbidities in patients with severe AD were compared with those in the general population using propensity score matching (pairing). The estimators were age and sex. The tolerance of the model was 2, with sampling with substitution and giving priority to exact matches (1:2). Statistical significance was established as p <0.05. The statistical analysis was performed using SPSSWIN v. 23.
Results
Of the 2.2 million patients aged ≥6 years assigned to the centres, 62,849 received a diagnosis of AD (Table 1), of which 2323 (3.69%) were severe. 28 patients were excluded from the study (reasons: inclusion/exclusion criteria, 8; missing data: 14; loss follow-up: 6). The overall prevalence of severe AD, according to the defined criteria, was 0.10% (95% CI: 0.09–0.11%).The prevalence in the different age groups was 0.39%, 0.23% and 0.07% in the 6–12 years (N = 600), 13–18 years (N = 244) and >18 years (N = 1479), respectively (p <0.001). In all age groups asthma frequency was higher than in the general population (49%, 44.9% and 20.8%, respectively, p<0.001). Asthma severity (intermittent, mildly persistent, moderately persistent and severely persistent) was 16.1%, 25.4%, 45.0% and 13.5%, respectively, in patients aged 6–12 years, 14.5%, 30.4%, 44.3% and 10.8%, respectively, in those aged 13–18 years, and 12%, 36.7%, 42.8% and 8.5%, respectively, in patients aged > 18 years (p = 0.013). Anxiety/agitation diagnosis was higher in severe atopic patients than in general population in all age groups. In adults, the most frequent comorbidities were dyslipidaemia (46.0%), hypertension (38.9%), obesity (27.7%), and diabetes mellitus (14.9%), which were higher than in the general population (Table 2).
 |
Table 1 Prevalence Of Atopic Dermatitis According To Age Group |
 |
Table 2 Baseline Characteristics And Comorbidities Of The Study Population And The General Population By Age Group |
Cyclosporine (N = 1053, 45.3%), azathioprine (N = 370, 15.9%) and methotrexate (N = 209, 9.0%) were the most frequently used drugs; biological agents were used by 5.8% (in AD), Table 3. Cyclosporine (38.5%), immunoglobulins (34.3%) and azathioprine (25.0%) were the most frequent in patients aged 6–12 years; cyclosporine (45.5%), azathioprine (20.9%) and immunoglobulins (18%) in patients aged 13–18 years; and cyclosporine (48.1%), methotrexate (13.5%) and azathioprine (11.4%) in patients aged > 18 years. The most frequently used biological agent was omalizumab (3.7% in patients aged 13–18 years and 3.0% in those aged > 18 years). Three or more treatment cycles were administered in 34.2%, 10.3% and 10.0% of patients, respectively (p <0.001). Systemic corticosteroids were administered in 97.3%, 90.9% and 81.7% of patients, respectively (p <0.001; concomitant-medication). The mean number of cycles of systemic corticosteroids administered during the 5 years of follow-up was 7.5 (SD: 3.3), with a mean duration of 12.1 (SD: 3.8) days; 1.1% of patients were hospitalized due to atopic dermatitis.
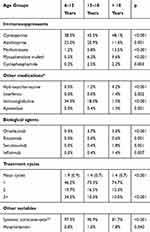 |
Table 3 Medication Administered For Severe Atopic Dermatitis According To Age Group |
Table 4 shows the medication administered and the duration of the cycles. The two most frequently used immunosuppressants represented 61.2% of the consumption. Cyclosporine was the most frequently used second-line immunosuppressant. There were variations in the duration of each cycle in each of the drugs administered.
 |
Table 4 Medication Administered And Duration Of Cycles In Patients With Severe Atopic Dermatitis |
Discussion
There is a lack of evidence on the prevalence of severe AD, although some authors place it at around 5%17,18,20 We found a lower figure, which may be due to the method of measurement. The severity of AD was classified according to the treatment administered, instead of the use of a clinical scale. The fact is that AD has a fluctuating course and the degree of severity is not substantially modified over time in most patients, and the possible classification bias (depending on the treatment) may substantially disappear. In moderate/severe cases a wide variety of drugs are used in combination; therefore, these results may reflect the type of systemic prescription used in usual clinical practice of the most severe/recurrent forms.
The results show a close association between AD and other immunoallergic expressions such as asthma and rhinitis. Patients with a late-onset, females, and patients with AD associated with other allergic diseases (asthma and rhinitis) have a worse prognosis.1,2 The percentage of patients with allergic comorbidity (asthma and rhinitis) may have been underdiagnosed compared with other reports.1,2 This might be because the comorbidities of these patients are not always included in the computerized medical record. We also found an association between AD and anxiety in all age groups and with depression in adults, in line with other reports.1,19,21,22 It is known that.10,19 Comparison of comorbidity in adult patients with severe AD with that of the general population showed a marked association with various metabolic/cardiovascular risk factors, such as hypertension, diabetes, dyslipidaemia and obesity. Although our results are similar to those of other studies,23 more data is required to reinforce the consistency of our results and identify associations between chronic severe AD and cardiovascular risk, which reduces life expectancy.24,25
In our study, after 5 years of follow up, all patients had received at least two types of systemic treatments for the treatment of AD, with a frequent need for several cycles of immunosuppressive treatment due to recurrences.
Management of signs and symptoms of AD with immunosuppressive agents has been widely described.26,27 Despite the difficulty in making comparisons, our results are also consistent with previous publications, agreeing that cyclosporine stands out as the most effective drug. However, the treatments administered by physicians in our study were short- or medium-term, showing a conservative attitude despite the existing variability.
However, data on the efficacy of systemic treatment and the long-term safety of immunosuppressants are limited, and further studies are needed to standardize and agree on their use. Cyclosporine is the only first-line immunosuppressant approved by the EMA for the systemic treatment of AD.28,29 There is ample evidence on the lack of control of AD with current treatments and the need for rescue medication,6,30 which was confirmed in our study by the high use of concomitant systemic corticosteroids.
Recently, dupilumab, a biological agent, has been suggested as a reference treatment for AD. The safety profile was more effective to conventional immunosuppressants (cyclosporine or methotrexate). Dupilumab was approved by the EMA in September 2017 for the treatment of adult patients with moderate/severe AD not adequately controlled with topical therapies or when these are not advisable.31
It should be noted that the prevalence of AD (total and severe) decreases according to the increase in the age of the patients (temporary follow-up).32 Two studies published in our country conclude that moderate to severe AD requiring treatment with systemic immunosuppressants has a low prevalence in adults and children; and that more studies will be needed to determine the real epidemiology of the disease. Our results are consistent with these publications.33,34
The possible limitations of the study affect the categorization of the disease and the possible aforementioned classification bias (treatment vs. scales), attributable to the information system used. Therefore, the study shows the usual limitations of retrospective studies, such as, for example, disease underreporting and variability in the physicians and patients, due to the observational design. In this regard, the possible inaccuracy of the diagnostic coding of moderate/severe AD and other comorbidities, or the non-inclusion of variables that could influence the final results (socioeconomic level, evolution of the pharmacological dose prescribed, therapeutic adherence, phenotypes, etc.) should also be considered as limitations. Likewise, we did not detail the possible overlap of medications between flares or maintenance phase due to difficulties in their measurement. The main limitation is shown in the evaluation method, the lack of measurement of clinical effectiveness and/or the lack of measurement of adverse reactions. Conversely, conducting the study in children, adolescents and adults simultaneously, and the large number of patients diagnosed with AD included, may be considered as the strengths of the study.
This disease results in a substantial comorbidities burden, including psychological and immunoallergic and, in adults, metabolic/cardiovascular components. Management of severe AD may become challenging, as many treatments have not received approval for use in severe AD, and the clinical control is inadequate, as shown by the high use of systemic corticosteroids. These difficulties in the disease control show the unmet medical need of these patients. Cyclosporine is the most widely used immunosuppressant.
The treatment of AD in general and of severe AD in particular may require more-personalized therapy depending on the phenotype. At present, clinical trials of biological agents that may revolutionize the evolution and treatment of AD are ongoing. Further studies are needed to determine the real effectiveness of many of these treatments. Moreover, future studies will require cost-effectiveness analyses and improved diagnostic and severity measurement tools. In addition, coordination strategies between the different health levels and effective prevention programs are necessary to delay the progression to more advanced stages of AD and reduce flares.
Author contributions
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Disclosure
The abstract of this paper was presented at the Conference: International Society for Pharmaco-economics and Outcomes Research (ISPOR). May 18-22, 2019 | New Orleans, LA, USA. as a poster presentation talk with interim findings. The poster’s abstract (PNS73): was published in “Poster Abstracts” in: Value in Health. 2019; 2 (Supplement 2):S298. Hyperlink with DOI: https://doi.org/10.1016/j.jval. 2019.04.1432. The study was sponsored by Sanofi A Sicras to Antoni Sicras-Mainar. The authors report no conflicts of interest in this work.
References
1. Wollenberg A, Oranje A, Deleuran M; European Task Force on Atopic Dermatitis/EADV Eczema Task Force, et al. ETFAD/EADV eczema task force 2015 position paper on diagnosis and treatment of atopic dermatitis in adult and paediatric patients. J Eur Acad Dermatol Venereol. 30;2016:729–747. doi:10.1111/jdv.13599
2. Muraro A, Lemanske RF
3. Silverberg JI. Public health burden and epidemiology of atopic dermatitis. Dermatol Clin. 2017;35:283–289. doi:10.1016/j.det.2017.02.002
4. Garnacho-Saucedo G, Salido-Vallejo R, Moreno-Giménez JC. Atopic dermatitis: update and proposed management algorithm. Actas Dermosifiliogr. 2013;104:4–16. doi:10.1016/j.ad.2011.12.008
5. DaVeiga SP. Epidemiology of atopic dermatitis: a review. Allergy Asthma Proc. 2012;33:227–234. doi:10.2500/aap.2012.33.3569
6. Sicras-Mainar A, Navarro-Artieda R, Carrascosa Carrillo JM. Economic impact of atopic dermatitis in adults: a population-based study (IDEA study). Actas Dermosifiliogr. 2018;109:35–46. doi:10.1016/j.ad.2017.09.003
7. Torrelo A, Ortiz J, Alomar A, Ros S, Pedrosa E, Cuervo J. Health-related quality of life, patient satisfaction, and adherence to treatment in patients with moderate or severe atopic dermatitis on maintenance therapy: the CONDA-SAT study. Actas Dermosifiliogr. 2013;104:409–417. doi:10.1016/j.ad.2012.12.003
8. Filanovsky MG, Pootongkam S, Tamburro JE, Smith MC, Ganocy SJ, Nedorost ST. The financial and emotional impact of atopic dermatitis on children and their families. J Pediatr. 2016;169:284–290. doi:10.1016/j.jpeds.2015.10.077
9. Boguniewicz M, Alexis AF, Beck LA, et al. Expert perspectives on management of moderate-to-severe atopic dermatitis: a multidisciplinary consensus addressing current and emerging therapies. J Allergy Clin Immunol Pract. 2017;5:1519–1531. doi:10.1016/j.jaip.2017.08.005
10. Nicol NH, Boguniewicz M. Wet wrap therapy in moderate to severe atopic dermatitis. Immunol Allergy Clin North Am. 2017;37:123–139. doi:10.1016/j.iac.2016.08.003
11. Roekevisch E, Spuls PI, Kuester D, Limpens J, Schmitt J. Efficacy and safety of systemic treatments for moderate-to-severe atopic dermatitis: a systematic review. J Allergy Clin Immunol. 2014;133:429–438. doi:10.1016/j.jaci.2013.07.049
12. Silvestre Salvador JF, Romero-Pérez D, Encabo-Durán B. Atopic dermatitis in adults: a diagnostic challenge. J Investig Allergol Clin Immunol. 2017;27:78–88. doi:10.18176/jiaci
13. Werfel T, Wollenberg A, Pumnea T, Heratizadeh A. New aspects in systemic treatment of atopic dermatitis. Hautarzt. 2018;69:217–224. doi:10.1007/s00105-018-4131-8
14. Hanifin JM, Rajka G. Diagnostic features of atopic eczema. Acta Dermatovenerol Suppl (Stockh). 1980;92:44–47.
15. Charlson ME, Pompei P, Ales KL, Mackenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–383. doi:10.1016/0021-9681(87)90171-8
16. The Anatomical Therapeutic Chemical Classification System with Defined Daily Doses (ATC/DDD): world Health Organization. Available from: http://www.who.int/classifications/atcddd/en/.
17. Kim MJ, Kang TW, Cho EA, et al. Prevalence of atopic dermatitis among Korean adults visiting health service center of the catholic medical center in Seoul Metropolitan Area, Korea. J Korean Med Sci. 2010;25:1828–1830. doi:10.3346/jkms.2010.25.12.1828
18. Tanei R, Hasegawa Y. Atopic dermatitis in older adults: a viewpoint from geriatric dermatology. Geriatr Gerontol Int. 2016;16(Suppl 1):75–86. doi:10.1111/ggi.12771
19. Werfel T, Heratizadeh A, Aberer W, et al. S2k guideline on diagnosis and treatment of atopic dermatitis - short version. Allergo J Int. 2016;25:82–95. doi:10.1007/s40629-016-0110-8
20. Kaufman BP, Guttman-Yassky E, Alexis AF. Atopic dermatitis in diverse racial and ethnic groups-variations in epidemiology, genetics, clinical presentation and treatment. Exp Dermatol. 2018;27:340–357. doi:10.1111/exd.2018.27.issue-4
21. Silverberg JI. Selected comorbidities of atopic dermatitis: atopy, neuropsychiatric, and musculoskeletal disorders. Clin Dermatol. 2017;35:360–366. doi:10.1016/j.clindermatol.2017.03.008
22. Dizon MP, Yu AM, Singh RK, et al. Systematic review of atopic dermatitis disease definition in studies using routinely collected health data. Br J Dermatol. 2018;178:1280–1287. doi:10.1111/bjd.16340
23. Thyssen JP, Halling-Overgaard AS, Andersen YMF, Gislason G, Skov L, Egeberg A. The association with cardiovascular disease and type 2 diabetes in adults with atopic dermatitis: a systematic review and meta-analysis. Br J Dermatol. 2018;178:1272–1279. doi:10.1111/bjd.16215
24. Totri CR, Eichenfield LF, Logan K, et al. Prescribing practices for systemic agents in the treatment of severe pediatric atopic dermatitis in the US and Canada: the PeDRA TREAT survey. J Am Acad Dermatol. 2017;76:281–285. doi:10.1016/j.jaad.2016.09.021
25. Proudfoot LE, Powell AM, Ayis S, et al. European Dermato-The European TREatment of severe Atopic eczema in children Taskforce (TREAT) survey. Epidemiology Network (EDEN). Br J Dermatol. 2013;169:901–909. doi:10.1111/bjd.2013.169.issue-4
26. Megna M, Napolitano M, Patruno C, et al. Systemic treatment of adult atopic dermatitis: a review. Dermatol Ther (Heidelb). 2017;7:1–23. doi:10.1007/s13555-016-0170-1
27. Shah N, Alhusayen R, Walsh S, Shear NH. Methotrexate in the treatment of moderate to severe atopic dermatitis: a retrospective study. J Cutan Med Surg. 2018;1:1203475418781336.
28. Hegazy S, Tauber M, Bulai-Livideanu C, et al. Systemic treatment of severe adult atopic dermatitis in clinical practice: analysis of prescribing pattern in a cohort of 241 patients. J Eur Acad Dermatol Venereol. 2017;31:e423–e424. doi:10.1111/jdv.2017.31.issue-9
29. Wollenberg A, Barbarot S, Bieber T, et al.; European Dermatology Forum (EDF), the European Academy of Dermatology and Venereology (EADV), the European Academy of Allergy and Clinical Immunology (EAACI), the European Task Force on Atopic Dermatitis (ETFAD), European Federation of Allergy and Airways Diseases Patients’ Associations (EFA), the European Society for Dermatology and Psychiatry (ESDaP), the European Society of Pediatric Dermatology (ESPD), Global Allergy and Asthma European Network (GA2LEN) and the European Union of Medical Specialists (UEMS). Consensus-based European guidelines for treatment of atopic eczema (atopic dermatitis) in adults and children: part II. J Eur Acad Dermatol Venereol. 2018;32:850–878.
30. Wei W, Anderson P, Gadkari A, et al. Extent and consequences of poor disease control among adults with a history of moderate to severe atopic dermatitis. J Invest Dermatol. 2016;136.
31. Seegräber M, Srour J, Walter A, Knop M, Wollenberg A. Dupilumab for treatment of atopic dermatitis. Expert Rev Clin Pharmacol. 2018;11:467–474. doi:10.1080/17512433.2018.1449642
32. ClinicalTrials.gov [Internet]. A pediatric longitudinal evaluation to assess the long-term safety of protopic for the treatment of atopic dermatitis (APPLES). Available from: https://ichgcp.net/clinical-trials-registry/NCT00475605.
33. Barroso B, Vera-Berrios RN, Rial JM, Fariña-Sabaris MC, Santos LC, Sastre J. Prevalence of severe atopic dermatitis in adults and children in a health area of Madrid, Spain. J Investig Allergol Clin Immunol. 2019;29:77–79. doi:10.18176/jiaci
34. Sicras-Mainar A, Navarro-Artieda R, Sánchez L, Sastre J. Prevalence of severe atopic dermatitis in adults in 3 areas of Spain. J Investig Allergol Clin Immunol. 2018;28:195–197. doi:10.18176/jiaci
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
