Back to Journals » International Medical Case Reports Journal » Volume 13
Salpingo Enteric Fistula: A Case Report
Authors Behrouzi-Lak T, Aghamohammadi V , Afshari N, Kashefi S
Received 27 February 2020
Accepted for publication 8 May 2020
Published 22 May 2020 Volume 2020:13 Pages 221—224
DOI https://doi.org/10.2147/IMCRJ.S251652
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Ronald Prineas
Tahereh Behrouzi-Lak,1 Vahideh Aghamohammadi,2 Niloofar Afshari,3 Saeed Kashefi4
1Department of Obstetrics, Gynecology and Reproductive Sciences, Urmia University of Medical Science, Urmia, Iran; 2Department of Nutrition, Khalkhal University of Medical Sciences, Khalkhal, Iran; 3Department of Dermatology, Tabriz University of Medical Science, Tabriz, Iran; 4Department of General Surgery, Urmia University of Medical Science, Urmia, Iran
Correspondence: Saeed Kashefi
Department of General Surgery, Urmia University of Medical Science, Resalat Blvd, Emergency Alley, Urmia, Iran
Tel +98 4431988000
Email [email protected]
Background: Few cases with fistulous communication between the GI system and female adnexal structure have been reported in the literature, and bilateral contrast spillage has been reported only in one case, and this case is the second one all over the world.
Case Presentation: The case was a 27-year-old woman with a diagnosis of primary infertility. She was booked with hysterosalpingogram (HSG) as part of the routine workup in the infertility clinic. There was a positive history of pelvic surgery for bilateral adnexal cysts for her in 2014. In this case, previous pelvic surgery without any medical problems was the strongest risk factor for tubo-intestinal fistula. Cystectomy performed for the left adnexal cyst and the right adnexal cyst was only drained. The pathologic report for the left ovarian cyst was endometriosis. HSG result showed evidence of bilateral fallopian tube opacification with contrast outlining from the fallopian tubes. Contrast leakage happened to the adjacent small intestine in the right side and peritoneal cavity on the left side.
Conclusion: Fistulous connections between fallopian tube and intestine will remain an exceptional rarity. The reported case could be a good lesson illustrating that the adherence to general surgical principles (meticulous hemostasis, careful applying of diathermy, etc.) and a watchful postoperative care could protect the patient from both usual and unusual complications.
Keywords: fallopian tubes, tubo-intestinal fistula, hysterosalpingogram, endometriosis, infertility
Background
Fistulous between the GI system and female adnexal structure rarely occurs. The rarity of this condition is reflected in the fact that only 50 cases have been reported until this date in the literature about tubo-intestinal fistulas.1 Also, the HSG feature of bilateral contrast leaking from fallopian tubes is reported only in one case from Saudi Arabia in 2012.2 Our case is the second one reported until this date with bilateral contrast leakage from fallopian tubes in all over the world.3–5 Hysterosalpingogram (HSG), a common radiological examination, is routinely used in the investigation of infertility and sub-fertility in women. The proximity of the uterus to adjacent pelvic structures results in various types of pelvic fistulas after pelvic disease, pelvic radiation therapy, and pelvic surgery. Because of the proximity of the female reproductive organs with other pelvic organs, fistulation can occur between the ureter and small or large bowels resulting in vesicovaginal, vesicouterine, vesicoenteric, ureterovaginal, ureteroenteric and uterovaginal fistulas.6–8 A wide variety of complaints in a woman are investigated for infertility suspected with fistulization. This ranges from the asymptomatic to the history of cyclic hematuria, and discharge of urine, feces, foul-smelling secretions, or air through unfamiliar orifices with perineal dermatitis.9–11 Regarding this fact that endometriosis a leading cause of infertility, endometriosis has a prevalence of 0.5–5% infertile and 25–40% in infertile women. The optimal choice of management for endometriosis-associated infertility remains unclear. Removal or suppression of endometrial deposits by medical or surgical ways constitutes the basis of endometriosis management.12
Ethics Approval
This study, approved by the Medical Ethics Committee of Urmia University of medical sciences, Urmia, Iran, is in accordance with the Declaration of Helsinki (approval number: IR. UMSU. REC. 9742).
Consent for Publication
The written informed consent was obtained from patient for publication and included publication of the images.
Case Presentation
A 27-years-old female presented to Motahari University Hospital infertility clinic with primary infertility for 4 years in 2017. She had been referred to the infertility clinic from 1 year after her marriage. The patient had a history of dysmenorrhea and dyspareunia without any unusual bowel disease. Family history for any disease including tuberculosis was negative. Also, her sister had married for 2 years and had a healthy child at the time of presentation. She had a history of laparotomy 3 years ago for left ovarian cystectomy in 2014. A pathologic report for cystectomy was endometriosis. In the post-operation course (2014–2017) she was admitted several times without any medical problem in our infertility clinic. Physical examination revealed a healthy female with no relevant abnormal general or local genital physical findings apart from the scar of previous Pfannenstiel incision. Her husband was clinically normal and all investigations for malefactors of infertility were normal. The last Hysterosalpingogram (HSG) performed under normal sterile procedures using non-ionic contrast (iohexol 300 mg). Following initial injection of about 8 mL of contrast, normal endometrium outline with no filling defect, contrast filled both tubes till fimbrial ends but contrast joined small intestine on the right side and leaked to the peritoneal cavity in the left side (Figure 1). The biochemistry assays revealed a negative result for HIV Ab (ELISA). Tissue specimens for tuberculosis investigation were collected by biopsy but the report was negative. The following of the patient was continued.
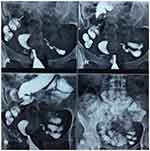 |
Figure 1 Hysterosalpingography shows bi-salpingeal contrast leakage. |
After consultation with the patient and her husband, she opted for fistula resection. This carried out successfully by our general surgery department in imam Khomeini university hospital. Closure of enteric fistula performed under general anesthesia in the supine position with lower midline laparotomy incision. Laparotomy revealed many adhesion bands and debris in the pelvic region with fistulous communication between Ileum (60 cm to Ileocecal valve) and right fallopian tube. On the left side, there was much suppurative debris with the destructed tube. Because of strong intestine adhesions to the right fallopian tube, involved segment resected and primary anastomosis performed by our teammates. Finally, because of this strong adhesion and destructed tubes bilateral salpingectomy performed by obstetrics and gynecology teammates. She follows up for infertility problems in an infertility clinic.
Discussion
Salpingo enteric fistula is a very rare disease. It possibly occurs in post-operative or post-inflammatory conditions (mainly adnexal tuberculosis).1 Our case had a pelvic surgery history in 2014 and probably that is the main predisposing factor for tubo-intestinal fistula. Only a few case reports were found describing salpingoenteric fistulas, and only one of them was bilateral fistulae that reported in Saudi Arabia in 2012. Patients with salpingoenteric fistula may be asymptomatic as appeared in our case and reported cases.2 When symptoms present, they are usually related to an underlying disorder, such as tuberculosis, endometriosis, pelvic inflammatory disease or appendicitis. Other possible causes of this rare type of fistula include Crohn’s disease and colon diverticulosis. While the rectum and bladder are some of the more common sites of fistula formation in Crohn’s disease, the fallopian tube is extremely rare.3 Fistulae to the fallopian tubes are rare, so their management is not well defined. It is suggested fistula closure with salpingectomy is an efficient procedure to treat this disease and to prevent the ectopic pregnancy.13–16 In fistulae resulting from Crohn’s disease and complicated diverticulitis, en-bloc fistula resection with salpingectomy is also recommended.3–5
Conclusions
Salpingo enteric fistulae as a rare and silent disease can induce infertility. The use of hysterosalpingography as a complementary modality for the investigation of infertility is again strengthened.2 A typical feature of hysterosalpingography confirms the diagnosis. This differential diagnosis should always be kept in mind when such hysterosalpingography findings appear due to the increasing number of tuberculosis cases secondary to HIV infection in developed countries and developing countries whereas tuberculosis is endemic.1 The availability and accessibility to assisted reproductive technology will help this type of patient achieve a successful pregnancy. Finally, the reported case could be a good lesson illustrating that the adherence to general surgical principles (meticulous hemostasis, careful application of diathermy, etc.) and a watchful postoperative care could protect the patient from both usual and unusual complications.
Abbreviations
HSG, hysterosalpingogram; GI, gastrointestinal.
Acknowledgments
We hereby express our gratitude to the study’s case.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
No conflict of interest was declared by the authors.
References
1. Sanjeeb KS, Murari LA, Ashok B. The silent disease “tubo-intestinal fistula”. Eur J Radiol. 2008;67:e115–116.
2. Al Sinani NS. Bi-salpingo colonic fistula report of both fallopian tubes fistulizing with sigmoid diverticulum with literature review. JKAU: Med Sci. 2012;19(3):103–110. (2012 A.D. / 1433 A.H.).
3. Michelassi F, Stella M, Balestracci T, Giuliante F, Marogna P, Block GE. Incidence, diagnosis, and treatment of enteric and colo-rectal fistulae in patients with Crohn’s disease. Ann Surg. 1993;218(5):660–666. doi:10.1097/00000658-199321850-00012
4. Williams SM, Nolan DJ. Colosalpingeal fistula: a rare complication of colonic diverticular disease. Eur Radiol. 1999;9(7):1432–1433. doi:10.1007/s003300050864
5. Palnaes-Hansen C, Bülow S, Karlsen J. Tubocutaneous fistula. Case report. Acta Chir Scand. 1987;153(7–8):465–466.
6. Bennett JK, Trulock TS, Finnerty DP. Urachal adenocarcinoma presenting as vesicoenteric fistula. Urology. 1985;25(3):297–299. doi:10.1016/0090-4295(85)90333-4
7. Fadel HE. Ileo-uterine fistula as a complication of myomectomy. Case report. Br J Obstet Gynaecol. 1977;84(4):312–313. doi:10.1111/j.1471-0528.1977.tb12584.x
8. Kilinc F, Bagis T, Guvel S, Egilmez T, Ozkardes H. Unusual case of post-cesarean vesicouterine fistula (Youssef’s syndrome). Int J Urol. 2003;10(4):236–238. doi:10.1046/j.0919-8172.2003.00599.x
9. Okafor PI, Orakwe JC, Mbonu OO. Cyclical haematuriasequel to uterine myomectomy: a case report. West Afr J Med. 2002;21(4):341–342. doi:10.4314/wajm.v21i4.28017
10. Catalano D, Conte R. Colo-uterine fistula. Report of a case. Radiol Med (Torino). 1994;87:350–351.
11. Mcfarlane MEC, Plummer JM, Remy T, et al. Jejunouterine fistula: a case report. Gynecol Surg. 2008;5:1613–1616. doi:10.1007/s10397-007-0353-y
12. Ozkan S, Murk W, Aricib A. Endometriosis and infertility epidemiology and evidence-based treatments. Ann N Y Acad Sci. 2008;1127:92–100. doi:10.1196/annals.1434.007
13. Emmert C, Kohler U. Management of genital fistula inpatients with cervical cancer. Arch Gynecol Obstet. 1996;259:19–24. doi:10.1007/BF02505304
14. Selzman AA, Patrick SJ, Kursh ED. The changing management of ureterovaginal fistulas. J Urol. 1995;153:626–628. doi:10.1016/S0022-5347(01)67668-7
15. Lee BH, Choe DH, Lee JH, et al. Device for occlusion of rectovaginal fistula: clinical trials. Radiology. 1997;203:65–69. doi:10.1148/radiology.203.1.9122417
16. Nagy V, Valansky L, Milichovsky I. Urologic complications of gynecologic surgery and their treatment in our clinical data. Ceska Gynekol. 1998;63:192–195.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
