Back to Journals » International Medical Case Reports Journal » Volume 13
Panophthalmitis and Orbital Inflammation with Cavernous Sinus Thrombosis Following Cataract Surgery
Authors Marinos E , McCall D, Tumuluri K , Rowe N, Do H
Received 27 July 2020
Accepted for publication 15 September 2020
Published 3 November 2020 Volume 2020:13 Pages 569—572
DOI https://doi.org/10.2147/IMCRJ.S274140
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Scott Fraser
Emmanuel Marinos, Dominic McCall, Krishna Tumuluri, Neil Rowe, Helen Do
Ophthalmology Department, Westmead Hospital, Sydney, NSW, Australia
Correspondence: Emmanuel Marinos
Ophthalmology Department, Westmead Hospital, Sydney Hospital/Sydney Eye Hospital, Sydney, NSW, Australia
Tel +61 400 498 037
Email [email protected]
Background: Panophthalmitis is a severe inflammation of the globe that can result as a rare complication of ophthalmic surgery. In severe cases, it may also be associated with orbital inflammation and cavernous sinus thrombosis.
Purpose: This case demonstrates a rare and life-threatening post-operative complication of cataract surgery. We also hope to highlight the importance of considering the relevant risk factors associated with developing potential infections after cataract surgery, including the use of corneal sutures, high-risk behaviours such as excessive eye-rubbing, and non-compliance with appointments and post-operative medications.
Case Report: We report the case of a 35-year-old female with severe autism and developmental delay who developed panophthalmitis, orbital inflammation and cavernous sinus thrombosis 6 weeks post cataract surgery. The likely cause was corneal suture-related microbial keratitis, and the patient required enucleation due to sepsis.
Conclusion: Post-surgical panophalmitis is a rapidly progressive disease that is not only sight- but life-threatening and demands urgent and intensive treatment. Consideration of early enucleation may be required to prevent deterioration in such patients.
Keywords: panophthalmitis, suture abscess, orbital cellulitis, cavernous sinus thrombosis, enucleation
Introduction
Panophthalmitis is a rapidly progressive disease that is both sight- and life-threatening and demands urgent and intensive treatment. Most cases of panophthalmitis in the literature arise from endogenous sources, with cases of exogenous panophthalmitis being extremely rare in the literature. We report a rare case of panophthalmitis likely secondary to a corneal suture abscess post cataract surgery, with associated orbital cellulitis and cavernous sinus thrombosis. We hope to highlight not only the management principles of this severe infection, including early consideration of enucleation in order to prevent sepsis, but also to reflect upon ways to mitigate the risk of such infections from developing in similar cases in the future.
Case Report
A 35-year-old female with level 3 autism and severe developmental delay was referred to a tertiary Australian hospital for management of a unilateral white cataract of unknown cause. She was otherwise healthy, with no recent infections or risks of endogenous bacteraemia, and had no other medical conditions. She did not have diabetes, nor was she immunosuppressed.
Due to difficulty in assessment, an examination under anesthetic (EUA) was performed, where she was noted to have posterior synechiae and a calcific white cataract with adherent lens capsule in the left eye, and an unremarkable right eye aside from early minimal cataract. No posterior segment pathology was noted bilaterally (B-scan performed in left eye). Following viscodissection of the posterior synechiae and circular capsulorhexis, the wrinkled lens capsule was noted to be firmly adherent to the fibrous lens plaque. She thus underwent central lensectomy with the vitrector, followed by an anterior vitrectomy with the aid of intracameral triamcinolone, and a sulcus IOL was inserted. Five 10–0 Vicryl sutures were used to close the limbal wounds and intracameral cefuroxime was used.
Two weeks post-operatively, a limited examination showed no conjunctival injection and a clear cornea in her operated eye. Chloramphenicol and dexamethasone eyedrops were each prescribed four times daily for 1-month post-operatively. Having missed her 4-week post-operative review, the patient was next seen at 6 weeks post-operatively after being referred to the emergency department by her carers. She presented with a 4-day history of left periorbital erythema associated with a red eye and significant eye-rubbing. She underwent an EUA along with CT imaging of the brain and orbits to assess the globe and check for radiological signs of orbital cellulitis.
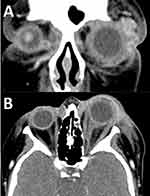
Examination revealed left periorbital swelling and erythema, conjunctival chemosis, moderate proptosis, a dense corneal infiltrate with subtotal hypopyon and no fundus view. The Vicryl sutures had dissolved. CT imaging showed proptosis of the left globe, left intraconal soft tissue enhancement with scleral thickening, and an enlarged left superior ophthalmic vein with features of cavernous sinus thrombosis (Figure 1). She had an elevated C-Reactive Protein (CRP) of 128 with a normal white cell count (WCC). She was admitted to the high dependency unit and underwent an urgent vitreous tap and injection of ceftazidime and vancomycin, plus a corneal scrape. She was commenced on intravenous ceftriaxone and vancomycin, hourly topical ofloxacin, and subcutaneous enoxaparin for cavernous sinus thrombosis, although treatment was difficult due to poor patient co-operation. Vitreous cultures grew pan-sensitive Streptococcus pneumoniae, and her corneal scrape grew methicillin-sensitive Staphylococcus aureus. A second EUA was performed two days later, and with no clinical improvement in the hypopyon or keratitis, a second vitreous tap and antibiotic injection was performed showing the vitreous cavity filled with pus (Figure 2). She subsequently deteriorated clinically with febrile episodes, tachycardia and spreading periorbital inflammation. She began to develop a leukocytosis (WCC: 11.0) and her CRP rose to 214. She then underwent left eye enucleation for control of potentially life-threatening sepsis. Intraoperatively, Tenon’s capsule, the conjunctiva and periorbital tissues were inflamed, with healthy intraconal fat noted. Histopathological analysis showed neutrophilic panophthalmitis with extensive suppurative inflammation within the sclera, retina, and uveal tissue, associated with stromal melt and mild optic nerve inflammation (Figure 3). Following enucleation, the periorbital inflammation and cavernous sinus thrombosis resolved over 1 week. She was discharged 2 weeks later.
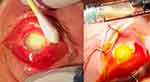 |
Figure 2 Examination under anesthetic demonstrating marked chemosis, dense corneal infiltrate with a large hypopyon and periorbital erythema. Note the purulent fluid aspirated from vitreous tap. |
 |
Figure 3 (A) Cross-section of the left globe following enucleation and (B) histology slide showing severe neutrophilic inflammation within the sclera, uvea, and retina. |
Discussion
Panophthalmitis is a severe and fulminant inflammation of the globe which can ultimately lead to phthisis bulbi and will often require evisceration or enucleation.1 It is a rare condition most often caused by endogenous infections, with Klebsiella pneumoniae, Streptococcus spp., and Bacillus cereus accounting for the majority of cases.2,3 Most cases of exogenous panophthalmitis occur after a penetrating eye injury, with Clostridium perfringens being a common causative organism.4 The incidence of post-surgical panophthalmitis is limited to case reports. These include 3 cases of panophthalmitis post cataract surgery in India,1 a case of panophthalmitis following trabeculectomy surgery in a child,5 a case of panophthalmitis and orbital cellulitis following penetrating keratoplasty,6 and a case of panophthalmitis post vitrectomy.7 None of these cases reported cavernous sinus thrombosis.
In this case, the panophthalmitis caused by the Streptococcus pneumoniae was most likely related to a corneal suture abscess. For pediatric and developmentally delayed patients, absorbable sutures (eg Vicryl) are often used to eliminate the need for suture removal. However, multifilament Vicryl sutures are associated with increased infection risk compared with monofilament nylon sutures.8 It may therefore be preferable to use nylon sutures in cases in which eye rubbing is likely to be significant and where multiple sutures are required to close corneal wounds.
Post-surgical panophalmitis is a rapidly progressive disease that is not only sight- but life-threatening and demands urgent and intensive treatment. Consideration of early enucleation may be required to prevent deterioration in such patients.
Ethical Considerations
Informed consent was provided by the patient’s public guardian for the patient’s medical details to be used for the material of this case report. The guardian has reviewed this manuscript and has given consent for the material to be published.
Acknowledgments
This study has not been published previously in print or electronic format and is not under consideration by another publication or electronic medium.
Disclosure
Dr Marinos is currently affiliated with Concord Repatriation General Hospital, Sydney, NSW, Australia. The authors report no conflicts of interest in this work.
References
1. Pappuru RR, Dave VP, Pathengay A, et al. Endophthalmitis progressing to panophthalmitis: clinical features, demographic profile, and factors predicting outcome. Semin Ophthalmol. 2018;33(5):671–674. doi:10.1080/08820538.2017.1416411
2. Chen KJ, Chen YP, Chao AN, et al. Prevention of evisceration or enucleation in Endogenous bacterial panophthalmitis with no light perception and scleral abscess. PLoS One. 2017;12:1.
3. Shamsuddin D, Tuazon CU, Levy C, Curtin J. Bacillus cereus panophthalmitis: source of the organism. Rev Infect Dis. 1982;4(1):97–103. doi:10.1093/clinids/4.1.97
4. Levitt JM, Stam J. Clostridium perfringens panophthalmitis. Arch Ophthalmol. 1970;84(2):227–228. doi:10.1001/archopht.1970.00990040229017
5. Esporcatte BL, Teixeira LF, Rolim-de-Moura C. Panophthalmitis with orbital cellulitis following glaucoma drainage implant surgery in a pediatric patient. Arq Bras Oftalmol. 2016;79(2):123–125. doi:10.5935/0004-2749.20160037
6. Schein OD, Miller JW, Wagoner MD. Panophthalmitis after penetrating keratoplasty. Arch Ophthalmol. 1989;107(1):21. doi:10.1001/archopht.1989.01070010023013
7. Wang TJ, Huang JS, Hsueh PR. Acute postoperative Morganella morganii panophthalmitis. Eye. 2005;19(6):713. doi:10.1038/sj.eye.6701613
8. Sharp WV, Belden TA, King PH, Teague PC. Suture resistance to infection. Surgery. 1982;91(1):61–63.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.