Back to Journals » Patient Preference and Adherence » Volume 15
Medication Belief is Associated with Improved Adherence to Exclusive Enteral Nutrition in Patients with Crohn’s Disease
Authors Li S, Li P, Sun H, Hu W, Hu S, Chen Y, Lv M
Received 30 July 2021
Accepted for publication 4 October 2021
Published 16 October 2021 Volume 2021:15 Pages 2327—2334
DOI https://doi.org/10.2147/PPA.S330842
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Naifeng Liu
Shuyan Li,1,* Peiwei Li,2,* Hongling Sun,1 Wen Hu,3 Shurong Hu,2 Yan Chen,2 Minfang Lv2
1Department of Nursing, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, 310009, People’s Republic of China; 2Center for Inflammatory Bowel Diseases, Department of Gastroenterology, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, 310009, People’s Republic of China; 3State Key Laboratory for Diagnosis and Treatment of Infectious Diseases, National Clinical Research Center for Infectious Diseases, Collaborative National Clinical Research Center for Infectious Diseases, The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, 310003, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Minfang Lv; Yan Chen
Center for Inflammatory Bowel Diseases, Department of Gastroenterology, The Second Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, 310009, People’s Republic of China
Tel/Fax +86-571-87783540
; +86-571-87783936
Email [email protected]; [email protected]
Background: The prevalence of Crohn’s disease (CD) has been increasing rapidly in China, and the role of exclusive enteral nutrition (EEN) in the management of adult patients with active CD is evolving. Adherence is a key factor in the effective treatment of many chronic diseases.
Aim: The aim of this study was to assess adherence to EEN of CD patients and to evaluate the relationship between medication belief and EEN adherence.
Methods: A cross-sectional study was conducted, and demographic information, adherence to EEN, and beliefs about EEN were investigated. Medication belief was measured using the Beliefs about Medicines Questionnaire (BMQ)-Specific.
Results: In all, 131 CD patients completed the questionnaire and were enrolled in this study. The high adherence rate was 73.3% (96 of 131 patients), and we found that medication belief, residency, medical insurance, and history of enteral nutrition therapy were factors affecting EEN adherence. More patients with a high BMQ score had high adherence to EEN (n = 54, 56.2%) compared to those with a low BMQ (n = 42, 43.8%). Moreover, price, taste, storage method, portability, and purchase convenience of EEN were not associated with adherence.
Conclusion: The adherence to EEN among patients with CD is relatively high and is related to medication belief, residency and history of enteral nutrition. The type of enteral nutrition, taste, storage, and convenience of purchase were not associated with EEN adherence. Future study is warranted to explore the possible role of improving patients’ beliefs in increasing adherence.
Keywords: exclusive enteral nutrition, adherence, Crohn’s disease
Introduction
Crohn’s disease (CD) is a chronic and relapsing intestinal inflammatory disease of unclear etiology.1 With the rapid development of China, the prevalence of CD has been increasing rapidly.2 Various treatments have been used for CD, including corticosteroids, immunomodulators, biological agents, and exclusive enteral nutrition (EEN).3 The role of EEN in the management of adult patients with active CD is evolving.4–6 EEN not only improves the nutritional status but also promotes mucosal healing, inducing and sustaining clinical remission.7 In patients with childhood CD, EEN is as effective as traditional corticosteroid therapy, with an approximately 80% remission rate significantly fewer adverse effects.8 In a randomized controlled trial, the remission rate of EEN in patients with active CD was 60% in adults.9
Adherence to prescription drugs is a key factor in the treatment of many chronic diseases. The World Health Organization (WHO) defined adherence as
To what extent does a person’s behavior conform to the recommendations agreed upon by the health care provider, including medication, diet, or lifestyle change.10
Patients with CD require medication adherence, because low adherence increases the risk of recurrence and the medical costs. The non-adherence rate of oral medications in patients with CD is 30–40%.11 In some cases, patients fail to meet target nutritional goals during EEN (eg, poor palatability, disruption of normal life, lack of peer support).12 The efficacy of EEN is largely determined by adherence behavior; poor adherence is related to EEN treatment failure in adults.13 Therefore, adherence to EEN has a positive influence on the course of CD.
Multiple factors influence medication adherence, such as medication belief, education level, and course of treatment. Among them, medication belief is an important predictor of medication adherence.14 Medication belief can reflect the cost-benefit analysis of patients’ beliefs about the medicine needed to maintain health and the possible adverse effects. A study shows that 38.2% of inflammatory bowel disease (IBD, including CD) patients were worried about taking medicines, 61.8% were worried about the side effects of long-term medication.15 Low medication belief about IBD oral medication was significantly associated with non-adherence,15 the same as epileptic patient16. However, adherence to EEN among Chinese CD patients and its association with medication belief are unclear.
We assessed adherence to EEN among patients with CD and evaluated the relationship between medication belief and EEN adherence. The findings will facilitate improvement of adherence to EEN, the treatment effect, and the quality of life of patients with CD.
Methods
Study Design and Participants
This was a cross-sectional study of adherence to EEN among patients with CD. Adult CD patients who received EEN therapy in the Second Affiliated Hospital, School of Medicine, Zhejiang University from December 2020 to May 2021 were included. Three enteral nutrition were used: Short peptide enteral nutrition Suspension (Nutricia Advanced Medical Nutrition), Total protein enteral nutritional powder (Abbott Laboratories B.V), Enteral Nutritional Emulsion (Fresubin). The inclusion criteria were as follows: diagnosed with CD for more than 3 months; require EEN according to a gastroenterologist; and agreed to participate in the study. The exclusion criteria were treatment by a mental health professional for any mental or cognitive impairment; other serious diseases, such as heart, brain, lung, liver, and kidney dysfunction; and severe infection, anemia, cachexia, or other serious complications. The enteral nutrition prescription of patients with CD was formulated by IBD specialists and clinical nutritionists after evaluating the patient’s condition. Patients’ dispensing records were obtained from the electronic medical records (EMRs). This study was approved by the Ethics Committee of the Second Affiliated Hospital, School of Medicine, Zhejiang University (Hangzhou, Zhejiang Province, China). The Institutional Review Board approved the informed consent process. Every participant signed the written informed consent form before the study began. This study has been registered in ClinicalTrials.gov (NCT04933214). This study was conducted in accordance with the Declaration of Helsinki.17
Clinical Data Collection
Adherence to EEN and beliefs about EEN were investigated using independent questionnaire and telephone. Demographic data were collected from EMRs, including age, sex, education, residence, working status, marital status and medical insurance. The disease related data collected included course of disease, Montreal classification, Erythrocyte Sedimentation Rate (ESR), C-reactive protein (CRP) and fecal calprotectin. The EEN-related data collected were the duration of EEN (according to the prescription) and the most commonly used type of EEN. The patients were also asked, on a 5-point Likert scale, to what extent they were satisfied with the cost, taste, storage method, portability, and purchase convenience of the enteral nutrition (EN) used. Also, reasons for the low adherence were asked from the questionnaire, including: I do not know what EEN requires; I cannot execute EEN because of other people’s ideas or comments; although I know the requirements of EEN, I cannot resist the temptation of other foods; due to the influence of work or study, I cannot strictly implement EEN. I could not purchase an EEN preparation in time; I cannot tolerance and stopped EEN. These variables were based on the adherence model proposed by the WHO.18
The ratio of daily actual intake of energy to daily target energy was used to assess adherence to EEN, which was refer to the method of previous study.19–22 In detail, the actual daily energy intake was calculated using the dispensing record and EEN duration for those patients purchased enteral nutrition preparations from the research hospital; otherwise, the actual daily energy intake was obtained by self-report using frequency questions and 24 h recall questions.23 The daily target energy was calculated in accordance with guideline.1 The definition of low adherence was: patients daily actual energy intake < 75% of daily target energy;11 or consumption of prohibited food or liquid every 2 weeks during EEN (except for water, tea and coffee without sweetener);7 or patients experienced side effects, such as diarrhea and nausea.7 Telephone or face-to-face conversations were performed for evaluation of EEN adherence.
Medication belief was measured using the Beliefs about Medicines Questionnaire (BMQ)-Specific.24 The BMQ-Specific has 10 items, including medication necessity and medication concern (5 items each) (Appendix 1). Responses to the questionnaire items were scored on a 5-point Likert scale; each item scored 1–5 points, ranging from “strongly disagree” to “strongly agree.” The higher the score, the stronger the perceived necessity or concern over taking medicine. The BMQ was the difference between the score for the need to take medicine and the concern over taking medicine, with a range of −20 to 20. A positive score indicates that the need to take medicine was stronger than the concern over taking the medicine, and a higher score suggests a stronger medical belief. The patients were divided into the High-BMQ and Low-BMQ groups based on whether they had a BMQ score above or below the median, respectively.
Statistical Analysis
Statistical analysis was conducted using SPSS ver. 26.0 (IBM, Armonk, NY). Descriptive statistics were calculated to summarize the participants’ characteristics and outcome measures. A χ2 test or Fisher’s exact test was performed to explore the relationship between participants’ characteristics and adherence to EEN. A P-value < 0.05 was considered indicative of statistical significance.
Results
Participants’ Characteristics
In all, 131 CD patients completed the questionnaire and were enrolled in this study. The characteristics of the enrolled patients are listed in Table 1. The mean age of the patients was 33.44 years, and 77 patients (58.8%) were men, 90 (68.7%) were from urban areas, and 69 (52.7%) had a full-time job. The duration of EEN was 2 weeks (n = 45, 34.4%), 4 weeks (n = 47, 35.9%), and 8 weeks (n = 39, 29.8%). Eighty-nine patients (67.9%) most commonly used Enteral Nutritional Powder, and 42 (32.1%) most frequently used Enteral Nutritional Suspension. Among the enrolled patients, 52 (30.7%) were aware of EEN therapy for the first time, 11 (8.4%) had heard of EN, 43 (32.8%) had ever received EEN therapy, and 25 (19.1%) had ever received partial enteral nutrition (PEN). Montreal classification, ESR, CRP and fecal calprotectin are listed in Table 1.
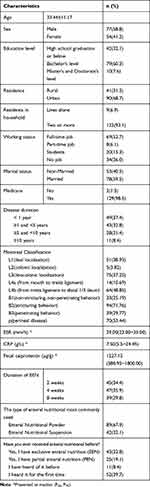 |
Table 1 Participants’ Characteristics (N=131) |
Adherence to EEN and Reasons for Low Adherence
A total of 96 (73.3%) patients had high adherence and 35 (26.7%) had low adherence. The major reasons for low adherence were: I do not know what EEN requires (38.9%); I cannot execute EEN because of other people’s ideas or comments (38.9%); although I know the requirements of EEN, I cannot resist the temptation of other foods (18.3%); due to the influence of work or study, I cannot strictly implement EEN (14.5%). A small number of patients (3.8%) had to eat other food because they could not purchase an EEN preparation in time; and 3.1% had intolerance and stopped EEN themselves.
Associations Between Participants’ Characteristics and Adherence to EEN
We identified factors influencing EEN adherence by univariate analyses. Patients living in urban areas had higher adherence (n = 71, 74.0%) than those from rural areas (n = 19, 54.3%) (P = 0.032). Medical insurance was positively associated with adherence (P = 0.018). Moreover, patients previously treated with enteral nutritional had higher adherence. No significant association with EEN adherence was found for sex, education level, employment status, and marital status (Table 2). In addition, the cost, taste, storage method, portability, and purchase convenience of EEN were not associated with adherence (Table 3).
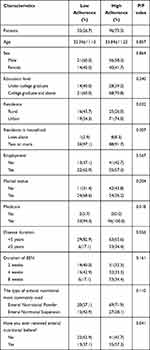 |
Table 2 Predictive Factors for Adherence to EEN (Univariate Analysis) |
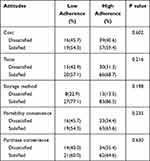 |
Table 3 Attitudes of Patients Towards Enteral Nutrition and Adherence to EEN |
Influence of Medication Belief on Adherence to EEN
The BMQ-specific necessity score ranged from 11–25, with a median of 18. For specific concern, the score ranged from 6–25 with a median of 15. The medication belief score ranged from –8 to 16, with a median of 3 (Table 4).
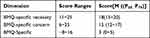 |
Table 4 The BMQ-Specific Score of Each Dimension and the Median Score |
Patients were divided into the high-BMQ group (BMQ-Specific score < 3) and low-BMQ group (BMQ-Specific score ≥ 3). More patients with a high BMQ score had high adherence to EEN (n = 54, 56.2%) compared to those with a low BMQ score (n = 42, 43.8%), suggesting that medication belief is significantly associated with adherence to EEN (P = 0.026) (Table 5).
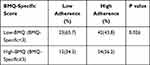 |
Table 5 Influence of Medication Belief on Adherence to EEN |
Discussion
The incidence of CD in China is increasing annually. Enteral nutrition induces and maintains clinical remission and mucosal healing for patients with CD.25–28 Appropriate nutritional support for patients with CD can not only improve the quality of life and prognosis, but also control inflammation and ameliorate the disease.29 Xue et al showed that the efficacy rate of EEN was 67.2% for CD patients in our center.30 Adherence to medication is very important for the treatment of chronic diseases.31 High adherence is associated with positive health outcomes.32 Thus, the patient’s adherence directly affects the therapeutic effects of enteral nutrition. We investigated adherence to EEN among CD patients and the factors associated with EEN adherence.
Several studies have assessed oral medicine adherence in CD patient,33,34 and reported a high non-adherence rate. For example, Kane et al showed that 43%~60% of IBD patients had non-adherence to medication.35 For pediatric patients the non-adherence rates to oral medication were as high as 64–88%.36 The eight-item Morisky Medication Adherence Scale (MMAS-8) was wildly used to assess oral medicine adherence in CD patients.15 However, there is no specific questionnaire to evaluate adherence for EEN. Patients’ diaries, self-report and prescription drug records are mostly used for EEN adherence measurement.10 We used prescription records combined with patient report for adherence measurement, which might be less reliable. In this study, 73.3% of patients with CD had high EEN adherence. Previous study suggested that adherence to EEN in pediatric CD patients was > 80%,8 which was higher than our study. One possible reason is that adult patients prefer to eat and drink compared with their peers,37 and thus EEN is more challenging.
We also investigated the possible factors associated with adherence, and found that medication belief, residency, medical insurance, and history of enteral nutrition therapy influenced EEN adherence. Medication belief had been identified as a significant predictor of low adherence in the previous research.14,15 It would affect patient’s perspective about disease and disease symptoms.38 For many IBD patients, they do not take medicine when they feel good about themselves, on the contrary, they were more worried about adverse drug reactions.38 Medication concerns are about adverse drug reactions and drug dependence, and medication necessities are the perceived benefits, including reduction of symptoms and disease remission.39 When taking medicine, patients conduct an internal cost-benefit analysis, that is, they make a trade-off between the need to take the medicine and the adverse reactions caused by the medicine.24 The difference between the two reflects the strength of the patient’s belief in the medicine.24 In this study, the median medication belief of the patients CD was 3 points, indicating a positive attitude to taking EEN and leading to high adherence. Medication belief may be related to, for instance, family support and understanding of the disease.40,41 Kelly et al showed that family support, culture, disease-related factors, communication and so on could affect beliefs.42 Therefore, medication belief can be improved by patient education and/or family support. We also showed that place of residence was related to adherence. This may be related to the patient’s economic condition, whether it is convenient to obtain drugs and experience.11,15,16 Previous research found that the severe economic burden and the difficulty of obtaining medical care are the two major difficulties faced by inflammatory bowel disease in China.43 Patients with history of enteral nutrition therapy had better adherence, one possible reason was that they had better cognitive capacity about disease and EEN treatment. Therefore, we should focus on rural areas, low-income individuals, and patients on enteral nutrition for the first time. For the latter, gastroenterologists should pay attention to acceptance by the patients and provide individualized guidance. If necessary, the awareness of these patients of EEN can be improved by peer support, to improve adherence. At present, many studies have confirmed the positive effect of peer support on adherence.44–46 Kanters et al showed that patients who had peer support were more likely to receive adjuvant chemotherapy than those who reported no peer support.47
Economic burden has been indicated to be a major difficult for IBD patients,37 and taste or volume of enteral nutrition was associated with adherence in a study with small sample size.48 Thus, we speculated factors such as cost, taste and storage might impact adherence. Interestingly, the analyses suggested that type of enteral nutrition, taste, storage, and convenience of purchase did not affect adherence. One possible reason might be that if the CD patients trust the effect of EEN, the characteristics of enteral nutrition are not particularly important.
We analyzed the EEN adherence of patients with CD and its influencing factors; however, the study had limitations. Firstly, our study was a retrospective study, the adherence to EEN were assessed by dispensing records combined with patient self-report, in which recall bias may affect the results; Secondly, the sample size was small, which may lead to inaccurate results. For example, although medical insurance was associated with adherence in the analysis, the result should be explained with caution because only two of the selected subjects did not have medical insurance. Thirdly, the data came from one center and there was selection bias. Therefore, a large prospective study is needed to evaluate EEN adherence among CD patients.
In summary, we found that adherence to EEN among CD patients was relatively high and was related to medication belief, residency, and history of enteral nutrition therapy. The type of enteral nutrition, taste, storage, and convenience of purchase were not significantly associated with EEN adherence. By enhancing knowledge and peer support, improving patients’ medication beliefs may increase adherence.
Highlights
- The role of exclusive enteral nutrition (EEN) in the management of adult patients with active CD is evolving. The efficacy of EEN is largely determined by adherence behavior; poor adherence is related to EEN treatment failure in adults.
- The adherence to EEN is related to medication belief, residency and history of enteral nutrition.
Abbreviations
CD, Crohn’s disease; EEN, exclusive enteral nutrition; BMQ, Beliefs about Medicines Questionnaire; WHO, World Health Organization; EN, enteral nutrition; IBD, inflammatory bowel disease.
Funding
This study was supported by National Natural Science Foundation of China (Grant No.81802881).
Disclosure
The authors declared no conflicts of interest.
References
1. Lamb CA, Kennedy NA, Raine T, et al. British society of gastroenterology consensus guidelines on the management of inflammatory bowel disease in adults. Gut. 2019;68:s1–s106.
2. Zhao J, Ng SC, Lei Y, et al. First prospective, population-based inflammatory bowel disease incidence study in mainland of China: the emergence of “western” disease. Inflamm Bowel Dis. 2013;19:1839–1845.
3. Gomollon F, Dignass A, Annese V, et al. 3rd European evidence-based consensus on the diagnosis and management of crohn’s disease 2016: part 1: diagnosis and medical management. J Crohns Colitis. 2017;11(1):3–25. doi:10.1093/ecco-jcc/jjw168
4. Green N, Miller T, Suskind D, Lee D. A review of dietary therapy for IBD and a vision for the future. Nutrients. 2019;11(5):947. doi:10.3390/nu11050947
5. Wall CL, McCombie AM, Gearry RB, Day AS. Newly diagnosed crohn’s disease treated with standard care or enteral nutrition: psychological outcomes over 6 months. Inflamm Intest Dis. 2019;4(1):7–13. doi:10.1159/000497323
6. Ruemmele FM, Veres G, Kolho KL, et al. Consensus guidelines of ecco/espghan on the medical management of pediatric crohn’s disease. J Crohns Colitis. 2014;8:1179–1207.
7. Wall CL, McCombie A, Mulder R, Day AS, Gearry RB. Adherence to exclusive enteral nutrition by adults with active crohn’s disease is associated with conscientiousness personality trait: a sub-study. J Hum Nutr Diet. 2020;33(6):752–757. doi:10.1111/jhn.12787
8. Heuschkel RB, Menache CC, Megerian JT, Baird AE. Enteral nutrition and corticosteroids in the treatment of acute crohn’s disease in children. J Pediatr Gastroenterol Nutr. 2000;31(1):8–15. doi:10.1097/00005176-200007000-00005
9. Feng Y, Li Y, Mei S, et al. Exclusive enteral nutrition ameliorates mesenteric adipose tissue alterations in patients with active crohn’s disease. Clin Nutr. 2014;33(5):850–858. doi:10.1016/j.clnu.2013.10.009
10. Gea Cabrera A, Sanz-Lorente M, Sanz-Valero J, Lopez-Pintor E. Compliance and adherence to enteral nutrition treatment in adults: a systematic review. Nutrients. 2019;11(11):2627. doi:10.3390/nu11112627
11. Jackson CA, Clatworthy J, Robinson A, Horne R. Factors associated with non-adherence to oral medication for inflammatory bowel disease: a systematic review. Am J Gastroenterol. 2010;105(3):525–539. doi:10.1038/ajg.2009.685
12. Vrijens B, De Geest S, Hughes DA, et al. A new taxonomy for describing and defining adherence to medications. Br J Clin Pharmacol. 2012;73(5):691–705. doi:10.1111/j.1365-2125.2012.04167.x
13. Wall CL, Day AS, Gearry RB. Use of exclusive enteral nutrition in adults with crohn’s disease: a review. World J Gastroenterol. 2013;19(43):7652–7660. doi:10.3748/wjg.v19.i43.7652
14. Nakhutina L, Gonzalez JS, Margolis SA, Spada A, Grant A. Adherence to antiepileptic drugs and beliefs about medication among predominantly ethnic minority patients with epilepsy. Epilepsy Behav. 2011;22(3):584–586. doi:10.1016/j.yebeh.2011.08.007
15. de Castro ML, Sanroman L, Martin A, et al. Assessing medication adherence in inflammatory bowel diseases. A comparison between a self-administered scale and a pharmacy refill index. Rev Esp Enferm Dig. 2017;109:542–551.
16. Niriayo YL, Mamo A, Gidey K, Demoz GT. Medication belief and adherence among patients with epilepsy. Behav Neurol. 2019;2019:2806341. doi:10.1155/2019/2806341
17. Association WM. World Medical Association Declaration of Helsinki ethical principles for medical research involving human subjects. JAMA. 2013;310(20):2191–2194.
18. Burkhart PV, Sabate E. Adherence to long-term therapies: evidence for action. J Nurs Scholarsh. 2003;35(3):207. doi:10.1111/j.1547-5069.2003.tb00001.x
19. Harvey SE, Parrott F, Harrison DA, et al. A multicentre, randomised controlled trial comparing the clinical effectiveness and cost-effectiveness of early nutritional support via the parenteral versus the enteral route in critically ill patients (calories). Health Technol Assess. 2016;20(28):1–144. doi:10.3310/hta20280
20. Stow R, Ives N, Smith C, Rick C, Rushton A. A cluster randomised feasibility trial evaluating nutritional interventions in the treatment of malnutrition in care home adult residents. Trials. 2015;16(1):433. doi:10.1186/s13063-015-0952-2
21. Shirakawa H, Kinoshita T, Gotohda N, et al. Compliance with and effects of preoperative immunonutrition in patients undergoing pancreaticoduodenectomy. J Hepatobiliary Pancreat Sci. 2012;19(3):249–258. doi:10.1007/s00534-011-0416-3
22. Lawson RM, Doshi MK, Ingoe LE, et al. Compliance of orthopaedic patients with postoperative oral nutritional supplementation. Clin Nutr. 2000;19(3):171–175. doi:10.1054/clnu.1999.0094
23. Liljeberg E, Andersson A, Blom Malmberg K, Nydahl M. High adherence to oral nutrition supplements prescribed by dietitians: a Cross-Sectional Study on hospital outpatients. Nutr Clin Pract. 2019;34(6):887–898. doi:10.1002/ncp.10243
24. Horne R, Weinman J, Hankins M. The beliefs about medicines questionnaire: the development and evaluation of a new method for assessing the cognitive representation of medication. Psychol Health. 1999;14(1):1–24. doi:10.1080/08870449908407311
25. Akobeng AK, Zhang D, Gordon M, MacDonald JK. Enteral nutrition for maintenance of remission in crohn’s disease. Cochrane Database Syst Rev. 2018;8:CD005984.
26. Hansen T, Duerksen DR. Enteral nutrition in the management of pediatric and adult crohn’s disease. Nutrients. 2018;10(5):537. doi:10.3390/nu10050537
27. Hartman C, Eliakim R, Shamir R. Nutritional status and nutritional therapy in inflammatory bowel diseases. World J Gastroenterol. 2009;15(21):2570–2578. doi:10.3748/wjg.15.2570
28. Levine A, Wine E, Assa A, et al. Crohn’s disease exclusion diet plus partial enteral nutrition induces sustained remission in a randomized controlled trial. Gastroenterology. 2019;157(2):440–50e8. doi:10.1053/j.gastro.2019.04.021
29. Montgomery SC, Williams CM, Maxwell P. Nutritional support of patient with inflammatory bowel disease. Surg Clin North Am. 2015;95(6):1271–9, vii. doi:10.1016/j.suc.2015.08.006
30. Xue M, Zhang H, Wang X, et al. Efficacy predictors of a 2-month exclusive enteral nutrition for inducing remission of active crohn’s disease. Eur J Clin Nutr. 2018;72(8):1183–1186. doi:10.1038/s41430-018-0198-7
31. Brown MT, Bussell JK. Medication adherence: who cares? Mayo Clin Proc. 2011;86(4):304–314. doi:10.4065/mcp.2010.0575
32. Cramer JA, Roy A, Burrell A, et al. Medication compliance and persistence: terminology and definitions. Value Health. 2008;11(1):44–47. doi:10.1111/j.1524-4733.2007.00213.x
33. Stone JK, Shafer LA, Graff LA, et al. Utility of the Mars-5 in assessing medication adherence in IBD. Inflamm Bowel Dis. 2021;27(3):317–324. doi:10.1093/ibd/izaa056
34. Lim JK, Lee YJ, Park JH. Medication-related knowledge and medication adherence in pediatric and adolescent patients with inflammatory bowel disease. J Korean Med Sci. 2020;35(14):e92. doi:10.3346/jkms.2020.35.e92
35. Kane S, Huo D, Aikens J, Hanauer S. Medication nonadherence and the outcomes of patients with quiescent ulcerative colitis. Am J Med. 2003;114(1):39–43. doi:10.1016/S0002-9343(02)01383-9
36. Hommel KA, Davis CM, Baldassano RN. Objective versus subjective assessment of oral medication adherence in pediatric inflammatory bowel disease. Inflamm Bowel Dis. 2009;15(4):589–593. doi:10.1002/ibd.20798
37. Myszkowska-Ryciak J, Harton A, Lange E, Laskowski W, Gajewska D. Nutritional behaviors of Polish adolescents: results of the wise nutrition-healthy generation project. Nutrients. 2019;11(7):1592. doi:10.3390/nu11071592
38. Clatworthy J, Bowskill R, Parham R, et al. Understanding medication non-adherence in bipolar disorders using a necessity-concerns framework. J Affect Disord. 2009;116(1–2):51–55. doi:10.1016/j.jad.2008.11.004
39. Niriayo YL, Kumela K, Kassa TD, Angamo MT. Drug therapy problems and contributing factors in the management of heart failure patients in Jimma University Specialized Hospital, southwest Ethiopia. PLoS One. 2018;13(10):e0206120. doi:10.1371/journal.pone.0206120
40. Horne R, Chapman SC, Parham R, et al. Understanding patients’ adherence-related beliefs about medicines prescribed for long-term conditions: a meta-analytic review of the necessity-concerns framework. PLoS One. 2013;8(12):e80633. doi:10.1371/journal.pone.0080633
41. Schuz B, Marx C, Wurm S, et al. Medication beliefs predict medication adherence in older adults with multiple illnesses. J Psychosom Res. 2011;70(2):179–187. doi:10.1016/j.jpsychores.2010.07.014
42. Kelly M, McCarthy S, Sahm LJ. Knowledge, attitudes and beliefs of patients and carers regarding medication adherence: a review of qualitative literature. Eur J Clin Pharmacol. 2014;70(12):1423–1431. doi:10.1007/s00228-014-1761-3
43. Yu Q, Zhu C, Feng S, et al. Economic burden and health care access for patients with inflammatory bowel diseases in China: web-based survey study. J Med Internet Res. 2021;23(1):e20629. doi:10.2196/20629
44. Blackard J, Chikovani I, Ompad DC, et al. On the way to hepatitis c elimination in the republic of Georgia—barriers and facilitators for people who inject drugs for engaging in the treatment program: a Formative Qualitative Study. PLoS One. 2019;14:e0216123.
45. Wu C-L, Liou C-H, Liu S-A, et al. Quality improvement initiatives in reforming patient support groups—three-year outcomes. Int J Environ Res Public Health. 2020;17(19):7155. doi:10.3390/ijerph17197155
46. Santo K, Isiguzo GC, Atkins E, et al. Adapting a club-based medication delivery strategy to a hypertension context: the CLUBMEDS Study in Nigeria. BMJ Open. 2019;9(7):e029824. doi:10.1136/bmjopen-2019-029824
47. Kanters AE, Morris AM, Abrahamse PH, Mody L, Suwanabol PA. The effect of peer support on colorectal cancer patients’ adherence to guideline-concordant multidisciplinary care. Dis Colon Rectum. 2018;61(7):817–823. doi:10.1097/DCR.0000000000001067
48. Hogan SE, Solomon MJ, Carey SK. Exploring reasons behind patient compliance with nutrition supplements before pelvic exenteration surgery. Support Care Cancer. 2019;27(5):1853–1860. doi:10.1007/s00520-018-4445-1
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
