Back to Journals » Vascular Health and Risk Management » Volume 18
Laparoscopic Surgery for Median Arcuate Ligament Syndrome (MALS): A Prospective Cohort of 52 Patients
Authors Kazmi SSH , Safi N , Berge ST, Kazmi M, Sundhagen JO , Hisdal J
Received 2 December 2021
Accepted for publication 17 February 2022
Published 24 March 2022 Volume 2022:18 Pages 139—151
DOI https://doi.org/10.2147/VHRM.S350841
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Prof. Dr. Pietro Scicchitano
Syed Sajid Hussain Kazmi,1,2 Nathkai Safi,1,2 Simen Tveten Berge,2,3 Marryam Kazmi,1,4 Jon Otto Sundhagen,1 Jonny Hisdal1,2
1Department of Vascular Surgery, Division of Cardiovascular and Pulmonary Diseases, Oslo University Hospital, Ullevål, Oslo, Norway; 2Institute of Clinical Medicine, Faculty of Medicine, University of Oslo, Oslo, Norway; 3Department of Vascular Surgery, Innlandet Hospital Trust, Hamar, Norway; 4Faculty 2, Poznan University of Medical Sciences, Poznan, Poland
Correspondence: Syed Sajid Hussain Kazmi, Department of Vascular Surgery, Division of Cardiovascular and Pulmonary Diseases, Oslo University Hospital, Ullevål, Kirkeveien 166, Oslo, 0450, Norway, Tel +47 92468309, Email [email protected]
Background: The selection of patients with MALS for surgical treatment depends upon the reliability of the symptom interpretation and the diagnostic work-up. We aimed to follow up the results of the laparoscopic decompression of the patients with MALS.
Patients and Methods: In a single-center, 52 consecutive MALS patients were followed-up, prospectively, after transperitoneal laparoscopic decompression. MALS was diagnosed with a computed tomography angiography (CTA) verified stenosis, ≥ 50% of the celiac artery (CA), and with duplex ultrasound, a peak systolic velocity (PSV) ≥ 2.0 m/s. Postoperative, CTA, and duplex ultrasound were performed, and the patients were followed-up at 3, 6, 12 months, and yearly after that.
Results: Mean age of the patients was 47 ± 21 years, and 65% were females. The patients had a mean weight loss of 8.4 ± 7.2 kg. Fifty-one patients had the laparoscopic operation with a mean operation time of 102 ± 28 minutes. Forty-seven patients (90%) achieved relief from the symptoms either completely (67%) or partially (23%) at 3– 6 months of follow-up. Significant improvement in postoperative PSV was found compared to the preoperative values, p< 0.001. Five patients (10%) with no immediate effect of the operation, but two of them became free from symptoms during the mean study follow-up of 2.4 ± 2 years. Five patients (10%) had operative complications, including one trocar injury to the liver, one pneumothorax, and three cases of bleeding from the branches of CA. Two patients died of cancer disease during the study period. Only two patients (4%) had symptoms relapse, both later treated successfully.
Conclusion: Laparoscopic transperitoneal decompression provides most of the patients a persistent relief from MALS symptoms.
Keywords: median arcuate ligament syndrome, postprandial pain, laparoscopy, mesenteric ischemia
Background
MALS is a disorder known to be due to external compression of the CA by the fibrotic preaortic celiac ganglionic tissue and the median arcuate ligament.1–3 External compression of the CA is a common radiological finding; however, it is asymptomatic in most patients.4 The incidence of MALS has been estimated to be about 1–2/100,000 patient years.5,6
Symptoms of MALS are postprandial abdominal pain, nausea, vomiting, changes in eating habits, and ultimately, weight-loss. Many other more common diseases share these symptoms, and hence the diagnosis is often delayed. Abundant case reports have been published about MALS, but few large case series.7–9 Since 2000, laparoscopic surgery has been incorporated as a preferred treatment of patients with MALS.10 Different laparoscopic approaches have been applied to release the median arcuate ligament and dissect CA free from any constricting connective tissue.11–14 Although there is a potential of operative injuries, the risk of complications is reported to be low during laparoscopic surgery for MALS.7,11,12
We present the results of our ten years’ experience with MALS patients, with an aim to add to the collective evidence about its existence and increase our understanding of this long-debated and disputed disease.
Materials and Methods
The patients were referred to the Department of Vascular Surgery at the Oslo University Hospital from either primary health care or other departments or hospitals. The department is the only center in Norway with a dedicated group of physicians to investigate and treat patients with MALS. In addition, all MALS patients, despite treatment, are regularly followed-up with the circulation laboratory.
From March 2011 to August 2021, seventy-eight patients suspected of chronic mesenteric ischemia (CMI) were identified to have external compression of the CA on computed tomography angiography (CTA). Further investigation showed that twenty-one (27%) had an asymptomatic CA compression.4 A total of fifty-seven patients were diagnosed as suffering from MALS and therefore eligible for laparoscopic surgery. Figure 1 illustrates the inclusion of the patients in this study.
 |
Figure 1 Flow chart of patients included in the study. Abbreviations: CTA, computed tomography angiography; MALS, median arcuate ligament syndrome. |
A detailed medical history was taken, and a careful clinical examination was performed by a dedicated team of physicians at the Department of Vascular Surgery, Oslo University Hospital.
Symptoms of MALS were defined as postprandial pain in the epigastrium and upper abdomen, changes in food intake pattern (smaller food portions with increased frequency), and weight-loss. Other symptoms of autonomic character like nausea, vomiting, diarrhea, constipation, palpitation, sweating, clammy skin, nervosity were also registered. All patients included in the study had an extensive gastrointestinal investigation to exclude hepatic, pancreatic, and other gastrointestinal diseases prior to the inclusion. The patients were examined with duplex ultrasound and CTA before the surgery and were followed postoperatively, with duplex ultrasound and clinical examination, at 2–3 months, 6 months, 12 months, and yearly, thereafter.
The patients with the symptoms of MALS and CTA verified stenosis ≥50% of lumen diameter of the CA, or with a peak, systolic velocity (PSV) ≥2.0 m/s were diagnosed as MALS. The findings and the clinical status were discussed in a multiple-disciplinary team, comprising of vascular surgeons, intervention radiologists, gastroenterologists, and ultrasound technicians, before a decision for surgical treatment was made.
The study’s primary endpoint was the relief from at least one of the MALS symptoms. Secondary endpoints were morbidity, recurrence of symptoms, and reinterventions.
Duplex Ultrasound
A dedicated, experienced physiologist (JH) performed a transabdominal duplex ultrasound, using a curvilinear transducer (C1-6) with Vivid E 95 scanner (General Electric Healthcare, Chicago, IL) on all the patients before and after the surgical treatment. All patients were examined after a minimum of six hours of fasting. Peak systolic velocity (PSV) of ≥ 2.0 m/s was considered as significant stenosis of the CA.15 End diastolic velocity (EDV), flow profile, and the effect of respiration on the flow profile was also registered.
Computed Tomography Angiography (CTA)
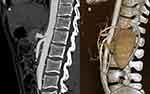
Multi-sliced CTA (64 row-multidetector, Siemens Medical Systems; Forchheim, Germany) was obtained in deep inspiration and expiration of the abdominal aorta and the mesenteric arteries.16 The scans were scrutinized in multiple plans. CA stenosis of ≥50% lumen reduction was considered significant stenosis (Figure 2).
Laparoscopic Decompression Technique
The operation was performed in general anesthesia and with the patient in the supine on a split-leg operation table. The operator positioned between the legs and one assistant on both sides of the table. Figure 3 shows the positions of the trocars. A 30° video laparoscope (Olympus Corporation, Tokyo, Japan) was used through this trocar. The left liver lobe was elevated with Nathanson liver retractor (Cook Medical, Bloomington, Indiana, United States), placed through a small incision distally and to the left side of xiphisternum to achieve a good exposure of the lesser omentum. The liver retractor was held with an autostatic instrument stabilizer, ENDOBOY (ASFS Medic’s, Niort, France). The gastro-hepatic ligament was incised along the upper border of the pancreas.
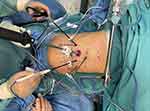 |
Figure 3 Trocar position on the abdominal wall for transperitoneal laparoscopic decompression of the celiac artery in a patient with median arcuate ligament syndrome. |
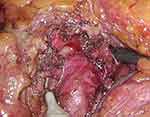
The patient was positioned in a reverse Trendelenburg, and if required, a slight distal retraction of the duodenum and pancreas by the assistant provided good exposure of the CA. The common hepatic artery was carefully approached along the upper border of the pancreas and followed centrally towards the CA bifurcation. Care was taken to keep a safe distance from the left gastric artery, and in a few cases (n = 3), also from the aberrant left hepatic artery. Ultracision Harmonic ACE+ (Ethicon Inc., Somerville, New Jersey, United States) and monopolar electrocautery hook were alternately used to dissect celiac artery from any nerve or fibrous tissue on its cranial surface. The left gastric artery and the inferior phrenic arteries were respected and preserved. The right diaphragmatic crus and median arcuate ligament were divided, and dissection was continued 1–2 cm cranially on the aorta, proximal to the origin of CA. The decompression of the CA was considered accomplished only when the CA was completely skeletonized on its cranial surface (Figure 4). Fascia at the 12 mm trocar position was closed with Polysorb braided sutures (Medtronic), and the skin incisions were closed with intracutaneous sutures. No wound drain was used. The patients were allowed to take oral food on the same day after surgery. They were mobilized fully on the first postoperative day.
Ethics and Trial Registration
The study complies with the Declaration of Helsinki. The patients were prospectively registered in the database for chronic mesenteric ischemia since 2016, approved by the Regional Committees for Medical and Health Research Ethics in the South-Eastern region of Norway (REK sør-øst B 2016/682). It was also registered in ClinicalTrails.org Protocol Registration and Results System (NCT02914912). Informed written consent was obtained from the patients for the treatment.
Statistics
Normalized data are presented as mean values with standard deviations. Proportions are given in percentage. Changes after surgical intervention are investigated with the Mann–Whitney test. The statistical significance was set at 5% (p<0.05).
Results
During ten years, fifty-two patients, with a mean age of 47 ±21 years, underwent surgical treatment for MALS. All operations were performed by one surgeon (SSHK). Eighteen (35%) patients also suffered from depression and anxiety, and thirty-three (65%) used analgesics. Table 1 illustrates the coexisting diseases, and Table 2 summarizes patients’ demographics, clinical findings, and investigation results.
 |
Table 1 Comorbidities in the Patients Diagnosed with MALS |
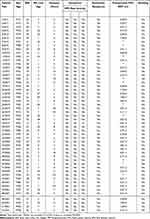 |
Table 2 Patient Characteristics, Symptoms, and Investigations |
The typical symptoms were postprandial abdominal pain, changes in eating patterns, and weight loss in fifty-one patients (98%). However, sixteen patients (31%) also had various autonomic symptoms like nausea, diarrhea, obstipation, palpitation, nervosity, chest pain, and clammy skin. Thirty-five (67%) patients also had abdominal pain during activity and exercise. Twenty-two (42%) patients had constant abdominal pain with postprandial aggravation. The patients in the study had a mean BMI of 21.6 ±3.5 kg/m2 and had a mean weight loss of 8.4 ±7.2 kg. The mean duration of symptoms before their first evaluation with the vascular surgery department was 4.7 ±3.5 years.
All patients were investigated with CTA. Four (8%) had the common hepatic artery origin from the superior mesenteric artery (SMA). One patient (patient 11) treated with open surgical decompression of the CA has had multiple laparotomies after colon cancer surgery and had a double-barrel colostomy due to enterocutaneous fistula. CTA disclosed external compression of both CA and SMA from a very hypertrophied diaphragmatic crux. After decompression, the patient underwent a successful reversal of the colostomy. The patient died of cancer disease two years after the decompression of the mesenteric arteries. Another patient (patient 13) also died of cancer two years after the laparoscopic decompression. After eight months, this patient had a relapse of postprandial abdominal pain, and duplex ultrasound confirmed PSV of 3.0 m/s; CTA confirmed stenosis of CA (although better lumen diameter than before laparoscopic decompression). The patient received a stent in the CA and again got relief from symptoms.
One patient (patient 51) included in his study was previously treated with a stent in CA for atherosclerotic stenosis, with an excellent response on symptoms. However, within three months, the patient experienced a relapse of symptoms. Investigation with duplex ultrasound showed a significant increase in PSV to 4.0 m/s, and CTA demonstrated a stent fracture in the CA due to a previously overlooked external compression from the median arcuate ligament. The patient underwent laparoscopic decompression and realignment of the fractured stent the day after surgery. PSV normalized after the treatment, and at three months follow-up, the patient was without any symptoms and had gained weight.
The mean operation time for the study population was 102 ±28 minutes. Perioperative findings and results are summarized in Table 3. Forty-seven (90%) patients achieved either complete or partial improvement of their symptoms at follow-up time-points of 3–6 months. Thirty-five (67%) patients had a complete recovery from their symptoms, and another twelve (23%) patients had partial improvement of their symptoms. The patients in this study have been followed for a mean period of 2.4 ±2 years. Mean weight gain was 5 ±4.4 kg at one-year follow-up after the surgery.
 |
Table 3 Postoperative Patients’ Characteristics and Clinical Data |
Five patients (10%) had no improvement of their preoperative symptoms at 3–6 months of follow-up. One of these was lost to follow-up. Another had postoperative PSV of 4.0 m/s and on CTA although a better postoperative CA lumen diameter, but still >50% stenosis in the CA. This patient had known occlusion in the SMA from before. The patient is scheduled to undergo endovascular CA and SMA occlusion treatment. In another patient, both CTA and DUS at follow-up do not show any significant residual stenosis of the CA. The patient had microscopic hematuria and is under further investigation for superior mesenteric artery syndrome and Nut-Cracker syndrome. Two patients were referred to the pain clinic, and at 2–3 years follow-up, they no longer had abdominal pain, did not use analgesics, and could eat regular food.
Five patients (10%) had complications during the surgery. In one patient (patient 44) with a body height of 155 cm, the left liver lobe was perforated during 12 mm trocar insertion. However, there was no serious operative bleeding, and the patient recovered without any early or late sequelae. Two patients (patients 1 and 43) had bleeding from the inferior phrenic artery. In one of these patients (patient 1), a laparoscopic suturing for hemostasis led to persistent stenosis of the CA, confirmed on a postoperative CTA. However, the lumen diameter of CA was still better than before the decompression, and the patient achieved symptom relief; therefore, no intervention was done to improve the lumen diameter. In the other patient, an endoscopic clip was used for hemostasis. One patient (patient 5) had an injury to the left gastric artery, which had to be ligated with endo-clips. The patient had a complete remission of her symptoms through a follow-up period of 5 years. In one patient (patient 12), the tip of the liver retractor perforated the diaphragm and caused pneumothorax. The laparoscopic decompression could be completed after the patient received a thoracic pleural drain.
In one patient (patient 11) with external compression of both CA and SMA, a stent was placed in SMA to ensure patency and sufficient circulation to the intestine for a successful colostomy reversal. In another patient (patient 47), a stent in CA was placed a day after laparoscopic decompression. SMA had a long occlusion in this patient, and the CA was extremely gracile despite laparoscopic decompression.
One patient (patient 35) with partial improvement in symptoms developed severe symptoms and had multiple hospital admissions one year post-operatively. Despite follow-up with a pain clinic, the patient had an extremely high daily use of opioids and other analgesics. Based on CTA findings of residual stenosis, severe symptoms of abdominal pain, and steadily increasing use of analgesics, the patients underwent re-exploration of CA with open surgery. A fibrous scar, possibly compressing the CA from lateral sides, was the only finding during the operation. No external compression on the cranial surface of the CA was found. Histopathology of the biopsy tissue confirmed scar tissue and excluded any neurinoma. The patient has been followed in one year and partially improved his symptoms.
Preoperative duplex ultrasound with PSV measurement in CA was successfully performed in thirty-nine patients (78%). Mean preoperative PSV was 2.8 ±0.6 m/s. In eight patients (16%), the CA could not be visualized, or a reliable flow measurement could not be performed. Two of these eight patients had near occlusion of the CA. In three patients (6%), a preoperative duplex ultrasound and velocity measurements were not performed. Postoperative duplex ultrasound with PSV could be performed in 48 patients (96%). Median postoperative PSV was 1.6 ±0.5 m/s. One patient was lost to follow-up, and CA could not be visualized properly in another. Comparisons of the pre-and postoperative duplex ultrasound flow velocities showed a statistically significant improvement in PSV and EDV after the surgical treatment (p< 0.001) (Figure 5).
All patients with either complete or partial decompression gave positive feedback about the effect of the operative treatment. In the patients’ opinion, MALS decompression had been helpful, and they recommended this treatment to the other patients suffering from MALS.
Discussion
This study demonstrates symptom relief achieved in 90% of patients with MALS operated with laparoscopic decompression. The symptom relief was either complete (67%) or partial (23%) within 3–6 months after laparoscopic decompression of the CA. The operation time is shorter than the earlier reports.9,11 The majority of the patients could be fully mobilized and discharged from the hospital the day after surgery. Only a few patients (n=2) had recurrent symptoms requiring intervention during a mean follow-up period of 2.4 years. This finding confirms that the patients in this study seem to have a persistent relief from the symptoms after laparoscopic surgery. Furthermore, it is interesting to observe that even some of the patients (n = 2) who did not have any effect of the surgical treatment at 3–6 months of follow-up time point did achieve relief from any symptoms of MALS later time-point.
The patients in our study group had a mean duration of symptoms for 4.7 years prior to the referral to our Vascular Surgery Department. The doctors’ poor understanding of this disease may contribute to the delay in its diagnosis and treatment. In 33% of patients, symptoms of autonomic activation were found in addition to the typical symptoms of MALS. This clinical picture could have contributed to the delay in referral and diagnosis. The patients experienced that when the doctors had difficulty interpreting their symptoms, they were assigned a psychiatric diagnosis. Thirty-five percent of the patients in this study had depression and anxiety diagnoses.8 Careful history taking during the investigation revealed that these psychiatric diagnoses were assigned to them after the start of their symptoms.
Laparoscopic decompression of the CA and a surgical dissection until completely skeletonized CA is a minimally invasive surgical technique for treating MALS.12 However, the patients are also at risk of surgical complications with this technique.7,9,11 Injury to the left liver lobe could have been avoided by placing the trocar under direct vision through the abdominal wall, especially in a patient with short height. Placement of the trocar through the ventral abdominal wall for a 30° endoscope, below the level of the CA origin from the aorta, may not provide a good vision of the artery, mainly where it lies compressed behind the median arcuate ligament. If the trocar is not placed high enough, the upper margin of the pancreas may hamper the surgical field. Alternatively, a 50° laparoscope or traction of the left gastric artery and common hepatic artery with tape can be used to facilitate the free dissection of the CA.13 CTA scans may help to plan the optimal trocar position for the laparoscope.
In the patient with the injury to the left gastric artery, hemostasis was achieved with surgical clips. The patient still had complete recovery despite occlusion of the left gastric artery and gained weight during the follow-up. It was probably due to the incremental improvement in circulation through the splenic artery and the gastroepiploic artery arcade.
Through a physiological test, gastric exercise tonometry, it has been shown that MALS has an ischemic origin.17 However, the instruments for conduction of this test have not been available to be used in our study population. In a previous study, we have found reduced preoperative circulation with the help of gastroscopy-assisted transmucosal laser Doppler flowmetry and visible light spectroscopy in patients with MALS compared to a control group of healthy individuals.18 It was a small study population, and the transmucosal microcirculatory assessment was performed in a fasting state. The increase in the transmucosal circulation could partially have occurred due to the division of the nerve fibers overlying the ventral surface of the celiac artery. However, during the laparoscopic decompression, the segment of CA underlying the median arcuate ligament had relatively sparsely crossed by any nerve fibers. In a study by Weber et al, a strong correlation between the celiac plexus block and a positive response to operation has been shown in the patients with MALS.19 Although 20% of patients had no pain relief after celiac plexus block, but still had a positive response to a subsequent surgery. They found that 14% had an unsuccessful effect of surgery despite a positive effect of preoperative celiac plexus block. Previously, neurolysis with phenol or alcohol in otherwise healthy patients has resulted in complications as serious as permanent paraplegia.20–22 In the present study, all patients with partial effect and in need of opioid analgesics, particularly those with no effect of the operation, were referred to the pain clinic.
We have been restrictive about the adjuvant endovascular treatment of the patients having the partial effect of the laparoscopic decompression. In the multi-disciplinary team, it was concluded that the clinical consequences of restenosis or occlusion of the stent are probably more severe; therefore, we chose to follow these patients.23,24 Postoperative CA lumen diameter, although better than the diameter before the operation, was still around 50% in some cases. However, PSV in most of these patients was reduced below 2.0 m/s. Later in the follow-up, most of these patients had a stable clinical picture, ie, better than before surgery, or even complete relief from the symptoms. Previously, in a small study on 13 patients, a retrospective analysis showed better outcomes results for patients with >70 stenoses of the CA. However, the study was underpowered to find that difference besides two of three patients with CTA-verified stenosis grade 50–70%, remained symptom-free during a median follow-up period of 117 months.25
Despite controversies about its pathophysiology, most of the patients with MALS seem to have a good effect of laparoscopic decompression.26 Laparoscopic surgical technique will continue to be regarded as one of the most minimally invasive surgical procedures for treating MALS. The patients with MALS should preferably be investigated and follow-up with the dedicated departments.
Conclusion
Laparoscopic decompression of the celiac artery seems to provide persistent relief from symptoms in most patients with median arcuate ligament syndrome.
Data Sharing Statement
Detailed individual participant data that underlie the results reported in the article is given in Tables 2 and 3. Further de-identified data can be shared with investigators whose proposed use of the data has been approved by an independent review committee identified for this purpose. The proposal should be directed to the project leader, Syed Sajid Hussain Kazmi, [email protected]. Data requestors will need to sign a data access agreement to gain access.
Author Contributions
All authors made a significant contribution to the work reported, whether that is the conception, study design, execution, acquisition of data, analysis, and interpretation, or in all these areas; took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Branco R. Anatomia et medicine operatoire du tronc coeliaque en particulier de lartere hepatique. Paris: G.Steinheil; 1912.
2. Harjola PT. A rare obstruction of the celiac artery: report of a case. Ann Chir Ginecol Fenniae. 1982;52:574.
3. Dunbar D, Molnar W, Beman FF, Marable SA. Compression of the celiac trunk and abdominal angina. Am J Roentgenol Radium Ther Nucl Med. 1965;95:731–744. doi:10.2214/ajr.95.3.731
4. Park CM, Chung JW, Kim HB, et al. Celiac axis stenosis: incidence and etiologies in asymptomatic individuals. Korean J Radiol. 2001;2(1):8–13. doi:10.3348/kjr.2001.2.1.8
5. Grotenmeyer D, Duran M, Iskandar F, et al. Median arcuate ligament syndrome: vascular surgical therapy and follow-up of 18 patients. Langenbecks Arch Surg. 2009;394(6):1085–1092. doi:10.1007/s00423-009-0509-5
6. Terlouw LG, Verbeten M, van Noord D, et al. The incidence of chronic mesenteric ischemia in the well-defined region of a Dutch mesenteric ischemia expert center. Clin Transl Gastroenterol. 2020;11:e00200. doi:10.14309/ctg.0000000000000200
7. Kim EN, Lamb K, Relles D, Moudgill N, DiMuzio PJ, Eisenberg JA. Median arcuate ligament syndrome-review of the rare disease. JAMA Surg. 2016;151(5):471–477. doi:10.1001/jamasurg.2016.0002
8. Goodall R, Langridge B, Onida S, Ellis M, Lane T, Davies AH. Median arcuate ligament syndrome. J Vasc Surg. 2020;71:2170–2176. doi:10.1016/j.jvs.2019.11.012
9. Podda M, Gusai GP, Balestra F, et al. Robotic-assisted approach to median arcuate ligament syndrome with left gastric artery originating directly from the aorta. Report of a case and review of the current mini-invasive treatment modalities. Int J Med Robotics Comput Assist Surg. 2018;14:e1919. doi:10.1002/rcs.1919
10. Roayaie S, Jossart G, Gitlitz D, et al. Laparoscopic release of celiac artery compression syndrome facilitated by laparoscopic ultrasound scanning to confirm restoration of flow. J Vasc Surg. 2000;32(4):814–817. doi:10.1067/mva.2000.107574
11. Van Petersen AS, Vriens BH, Huisman AB, et al. Retroperitoneal endoscopic release in the management of celiac artery compression syndrome. J Vasc Surg. 2009;50:140–147. doi:10.1016/j.jvs.2008.12.077
12. Roseborough GS. Laparoscopic management of celiac artery compression syndrome. J Vasc Surg. 2009;50(1):124–133. doi:10.1016/j.jvs.2008.12.078
13. Aday U, Boyuk A, Gulturk B, Bozan MB. Safe laparoscopic surgery in median arcuate ligament syndrome. Videosurgery Miniinv. 2018;13(4):539–541. doi:10.5114/wiitm.2018.76116
14. Fernstrum C, Pryor M, Wright P, Wolf AM. Robotic surgery for median arcuate ligament syndrome. JSLS. 2020;24(2):
15. Moneta GL, Lee RW, Yeager RA, Taylor LM
16. Van Petersen AS, Kolkman JJ, Meerwaldt R, et al. Mesenteric stenosis, collaterals and compensatory blood flow. J Vasc Surg. 2014;60:111–119. doi:10.1016/j.jvs.2014.01.063
17. Mensink PBF, van Pettersen AS, Kolkman JJ, Otte JA, Huisman AB, Geelkerken RH. Gastric exercise tonometry: the key investigation in patients with suspected celiac artery compression syndrome. J Vasc Surg. 2006;44:277–281. doi:10.1016/j.jvs.2006.03.038
18. Berge ST, Safi N, Medhus AW, Sundhagen JO, Hisdal J, Kazmi SH. Perioperative microcirculatory changes detected with gastroscopy assisted laser Doppler flowmetry and visible light spectroscopy in patients with median arcuate ligament syndrome. Vasc Health Risk Manag. 2020;16:331–341. doi:10.2147/VHRM.S252192
19. Weber JM, Boules M, Fong K, et al. Median arcuate ligament syndrome is not a vascular disease. Ann Vasc Surg. 2016;30:22–27. doi:10.1016/j.avsg.2015.07.013
20. Davies DD. Incidence of major complications of neurolytic coeliac plexus block. J R Soc Med. 1993;86:264–266.
21. Eisenberg E, Carr DB, Chalmers TC. Neurolytic celiac plexus block for treatment of cancer pain: a meta-analysis. Anesth Analg. 1995;80:290–295. doi:10.1097/00000539-199502000-00015
22. Raj PP. Celiac plexus/splanchnic nerve blocks. Tech Reg Anesth Pain Manag. 2001;5(3):102–115. doi:10.1053/trap.2001.24272
23. Malgor RD, Oderich GS, McKusick MA, et al. Results of single- and two-vessel mesenteric artery stents for chronic mesenteric ischemia. Ann Vasc Surg. 2010;24(8):1094–1101. doi:10.1016/j.avsg.2010.07.001
24. Bjork M, Koelemay M, Acosta S, et al. Management of the diseases of mesenteric arteries and veins. Clinical practice guidelines of the European Society of Vascular Surgery (ESVS). Eur J Vasc Endovasc Surg. 2017;53:460–510. doi:10.1016/j.ejvs.2017.01.010
25. Cienfuegos JA, Estevez MG, Ruiz-Canela M, et al. Laparoscopic treatment of median arcuate ligament syndrome: analysis of long-term outcomes and predictive factors. J Gastrointest Surg. 2008;22:713–721. doi:10.1007/s11605-017-3635-3
26. Jimenez JC, Harlander-Locke M, Duston EP. Open and laparoscopic treatment of median arcuate ligament syndrome. J Vasc Surg. 2012;56:869–873. doi:10.1016/j.jvs.2012.04.057
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.