Back to Journals » International Journal of Women's Health » Volume 11
Induction Of Labor Among Singleton Pregnancies In Six Palestinian Governmental Hospitals: A Population-Based Cohort Study
Authors Hassan S , Laine K , Fosse E, Abu-Rmeileh NME, Ali-Masri HY, Zimmo M , Zimmo K , Vikanes Å, Ismail KM
Received 24 May 2019
Accepted for publication 20 August 2019
Published 7 November 2019 Volume 2019:11 Pages 597—605
DOI https://doi.org/10.2147/IJWH.S215781
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Everett Magann
Sahar Hassan,1 Katariina Laine,2,3 Erik Fosse,4,5 Niveen ME Abu-Rmeileh,6 Hadil Y Ali-Masri,4,5,7 Mohammed Zimmo,4,5,8 Kaled Zimmo,4,5,9 Åse Vikanes,4 Khaled M Ismail10,11
1Department of Nursing, Faculty of Pharmacy, Nursing and Health Professions, Birzeit University, Ramallah, Palestine; 2Department of Obstetrics, Oslo University Hospital, Ullevål, Oslo, Norway; 3Department of Health Management and Health Economics, Institute for Health and Society, University of Oslo, Oslo, Norway; 4Intervention Centre, Oslo University Hospital, Rikshospitalet, Oslo, Norway; 5Institute of Clinical Medicine, Faculty of Medicine, University of Oslo, Oslo, Norway; 6Institute of Community and Public Health, Birzeit University, Ramallah, Palestine; 7Department of Obstetrics, Palestine Medical Complex, Ramallah, Palestine; 8Department of Obstetrics, Al Shifa Hospital, Gaza, Palestine; 9Department of Obstetrics, Al Aqsa Martyrs Hospital, Gaza, Palestine; 10Department of Gynecology and Obstetrics, Faculty of Medicine in Pilsen, Charles University, Pilsen, Czech Republic; 11Biomedical Center, Faculty of Medicine in Pilsen, Charles University, Pilsen, Czech Republic
Correspondence: Sahar Hassan
Department of Nursing, Faculty of Pharmacy, Nursing and Health Professions, Birzeit University, PO Box 14, Ramallah 627, Palestine
Tel +972599830158
Email [email protected]
Objective: To explore rates and review practices regarding induction of labor (IOL) among singleton pregnancies in Palestine.
Design: A prospective population-based cohort study.
Setting: Six secondary and tertiary governmental hospitals located in the two regions of Palestine: West Bank and Gaza.
Participants: Singleton pregnancies who had IOL in participating units during the study period were included (n=8290). Women having multiple gestations (1004), planned cesarean births (703), those admitted with cervical dilation >6cm (11228), and pregnancies with no record of cervical dilation and/or gestational age on admission (219) were excluded.
Primary outcome measure: Rates of IOL in participating units and regions.
Results: There were a total of 33,402 singleton births during the study period with an IOL rate of 24.8%. Rates of IOL significantly varied between units, ranging from 12.9% to 45.6% (P-value <0.05). The majority of women with no previous uterine scar were induced at gestational ages ≤40 weeks where 43.8% were induced at 39–40 gestational weeks (29.9% multiparous; 13.9% nulliparous) and 17.7% were induced between 37 and 38 gestational weeks (11.9% multiparous; 5.8% nulliparous).
Conclusion: Significant variations in IOL practices between Palestinian hospitals and regions suggest overuse of IOL among singleton pregnancies in some units with the majority of these being performed before 40 weeks’ gestation. These findings indicate a gap between implementation of best evidence and current clinical practice.
Keywords: childbirth, cohort study, induction of labor, Palestine, singleton, variations
Introduction
Induction of labor (IOL) is the artificial stimulation of uterine contractions aiming to start labor. It can be performed by administering medications or rupturing the amniotic membranes.1 IOL is associated with increased risks for operative deliveries, tachysystole, cord prolapse, uterine rupture, chorioamnionitis, and obstetric anal sphincter injuries.2 Therefore, the World Health Organization (WHO) has recently emphasized that induction of labor should be only used with clear medical indications and only to improve pregnancy outcomes.1 However, IOL continues to be one of the most frequently used peripartum interventions with a prevalence exceeding 20% in many countries.3,4
There is high-level evidence demonstrating the benefits of IOL for post-maturity and suggesting that, when performed after 41 weeks, IOL does not seem to be associated with an increased risk for cesarean delivery.1,2,5,6 Moreover, there is consensus regarding pre-labor rupture of membranes (PROM)1,2,5 and intrauterine fetal growth restriction as evidence-based indications for induction of labor.1,2,5 Although not supported by the same evidence level, several professional organizations consider hypertensive disorders, diabetes mellitus, cardiac diseases, oligohydramnios, fetal death, chorioamnionitis, multiple pregnancies, and vaginal bleeding as recommended indications for induction of labor before or at term.2,7,8 However, a significant number of inductions seem to be undertaken without medical indication. Indeed, reports from the US showed more than 15% of all induced births had no medical indication.9,10 A recent randomized trial involving nulliparous healthy low-risk women reported that, although IOL at 39 weeks did not improve the primary outcome of death or serious complications for babies, it was linked with lower cesarean section rates among IOL group compared to expectant management group and prolonged hospital stay in labor.11
Pharmacological methods used for induction of labor and supported by high-level evidence include oxytocin (syntocinon), dinoprostone (prostin E2), and Misoprostol (Cytotec).1,12 While mechanical methods (for example, amniotomy, cervical balloons, and membrane sweeping) are of moderate quality of evidence, nevertheless, strongly recommended.1,12 In practice, often a combination of two or more methods are used.12
Non-evidence-based interventions in maternity care may add unnecessary cost to the health-care system, compromise quality, and may increase risk of morbidity among women and newborns during childbirth.13 We previously reported that many practices and interventions used during childbirth in Palestine were not consistent with the best available evidence.14 In a hospital-based study of 1209 women, we showed that induction of labor was common among nulliparous women, about half of inductions occurred before reaching 40 weeks of gestation and about a quarter of these women suffered morbidities such as hemorrhage and two women were identified as near-miss.14 In Palestine, national IOL guidelines have been available since 2006 and were updated in 2016.15 The aim of this study was to explore rates of singleton IOL and review induction practices for singleton pregnancies in Palestinian government hospitals.
Materials And Methods
Study Design And Settings
An observational, prospective, population-based birth cohort study in the maternity units of six governmental hospitals located in the West Bank and Gaza regions of Palestine was conducted between March 2015 and February 2016. Most deliveries in Palestine occur in governmental hospitals; 27 hospitals with a total capacity of 3384 beds.16 In this study, the hospitals were selected based on their high workload and geographical location and, in 2015, had 47,046 live births constituting 62.1% of the total live births in Palestine for that year.17 Physicians decide on interventions during labor and delivery such as IOL. Midwives assist low-risk women to give birth and provide all necessary aspects of care for high-risk women in labor wards. The cesarean section rate in the participating hospitals ranged from 15.6% to 35.8% in the West Bank hospitals16 and 13.6% to 16% in Gaza hospitals.17 Five of the six included hospitals are tertiary referral centers and teaching maternity units which we previously described.18
Study Population
The target study population comprised all singleton IOLs undertaken in participating units during the study period. To identify this population, we used a stepwise selection process where we first excluded multiple pregnancies, women admitted for planned cesarean section, and women admitted to labor ward in active spontaneous labor (cervix > 6cm dilated).19 During the study period, 35,109 women gave birth in the 6 participating units. Following exclusion of multiple pregnancies (n=1004) and women scheduled for a planned cesarean section (n=703), there were a total of 33,402 women (12,213 in the West Bank pregnancies and 21,189 pregnancies in Gaza) singleton births that went into spontaneous labor or had an IOL (Figure 1). For the cohort of singleton pregnancies who gave birth during the study period and were admitted to the labor ward with a cervix <6cms dilated, the maternal intrapartum registration forms were used to exclude women who were admitted in early labor, latent phase or had labor augmentation. Once our target population was identified, the cohort was stratified into different Nippita groups based on parity and gestational age at the time of induction.20 Data are presented by unit and region.
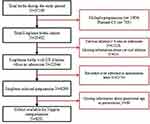 |
Figure 1 Study flowchart. |
Data Collection
Data were collected as part of system developed for the Palestinian Perineum and Birth Complications Study.18 Data on maternal intrapartum care were collected prospectively from bespoke case registration forms completed by the attending midwife or physician. Women were asked about aspects of their antenatal care that were missing from their records. Data were then entered into web-based District Health Information Software 2 (dhis2), and were transferred from dhis2 to be stored on a special platform “Tjeneste for Sensitive Data” (TSD) at the University of Oslo; a platform developed to store and share sensitive data compliant with Norwegian regulations for individuals’ privacy. Data management and quality assurance were described in our previous publication.18
Variables
Parity was recoded in one of two categories (0=Nulliparous, ≥1=Multiparous) while previous cesarean section and pregnancy complications were dichotomized into yes/no.
Options for the reason to attend labor ward were “contractions”, “rupture of membranes”, “abdominal pain”, and “vaginal bleeding”. Cervical dilation on admission was recoded into one of the two categories; 0–5 cm and 6–10. Gestational age was based on the last menstrual period and was recoded in one of the four categories; <36, 37–38, 39–40, and ≥41 weeks. Other variables collected included: onset of labor (“spontaneous” or “labor induction”); indication for induction of labor (“reduced fetal movement”, “hypertensive disorder”, “fetal growth restriction”, “PROM”, “post term pregnancy”, “diabetes”, and “large baby”); and method of induction (“balloon catheter”, “amniotomy”, “Misoprostol”, “Prostin E2”, and “Oxytocin”). The main outcomes of interest for this study were IOL rates and practices amongst singleton pregnancies in the different participating units and regions.
Statistical Analysis
Data were analyzed using IBM Statistical Package for Social Sciences (SPSS) (version 24.0). Descriptive analysis was used to present induction rates by participating unit and region. The Nippita classification system was used to categorize IOLs. Unlike previous ad hoc methods of stratification, the Nippita classification system is a robust a standardized tool to review inductions that takes into consideration parity, gestational age, number of fetuses, fetal presentation, and previous uterine scars.20 Pearson’s Chi-square test was used to compare the differences between units and regions. Statistical significance was defined as p<0.05.
Results
The total number of singleton births in the study period were 33,402 women; of these, 8290 (excluding cases with dilation >6cm) were admitted for IOL giving an overall IOL rate of 24.8% (45.6% in the WB and 12.9% in Gaza; OR=5.67, 95% CI 5.37–5.98, p<0.0001). The Singleton pregnancy IOL rates by unit and region are presented in Table 1.
 |
Table 1 Singleton Pregnancy Induction Of Labor Rates By Unit And Region (n=8290) |
Complete information required for the Nippita’s categorization was available for 8201 IOLs, which are presented among participating units for both regions in Table 2. In both regions, the highest contributing group to inductions was Nippita group G5 (multiparous women at 39–40 weeks’ gestation and with no previous cesarean sections), which represented 31.2% and 27.3% of the inductions in the West Bank and Gaza, respectively. The majority of women (68.5% in the WB and 63% in Gaza) were induced at or before 40 weeks’ gestation. Several of these were undertaken at ≤38 weeks where Nippita groups G1, G4, and G7 represented 23.7% and 21.3% of the IOLs in the WB and Gaza, respectively. Additionally, variations were noted between different hospitals in the same region with regards to the contribution of the different Nippita groups to the total number of IOLs such as variations between groups 1, 2, 3, 4, 6, and 8 among the West Bank hospitals, and groups 2, 3, 5, and 8 among Gaza hospitals (Table 2). The ranking order of the different Nippita induction groups in both regions is presented in Table 3.
 |
Table 2 Labor Inductions Among Singleton Pregnancies According To Nippita Groups By Unit And Region (n=8201) |
 |
Table 3 Labor Induction In The Studies Cohort Ranked By Nippita Group Frequency |
Information relating to indications of induction of labor was missing for 5595 of the 8290 (67.5%) women. For the 2695 pregnancies where the information about indication for induction was recorded, the most frequently recorded indication was post-term pregnancy in 1296 (48.1%) followed by premature rupture of membranes in 866 (32.1) pregnancies. With regards to methods used for cervical ripening, a cumulative total of 9130 methods of IOL were used in the study cohort (as more than one method was sometimes used for the same woman). These methods included amniotomy (4681; 51.3%), Prostin E2 (3028; 33.2%), oxytocin (716; 7.8%), misoprostol (341; 3.7%), and balloon catheter (364; 4.1%). The rates of relevant maternal and fetal outcomes in women who had IOL compared to spontaneous labor are presented in Table 4. The outcomes show that 6.5% of the women gave birth by emergency cesarean section due to obstructed labor after IOL. A quarter of women (24.7%) underwent IOL spent a duration more than 7 hrs for the first stage of labor compared to 16.5% of those recorded to be admitted in spontaneous labor. Additionally, the risk of fetal distress at 5 and 10 mins and meconium-stained amniotic fluid were higher for newborns after IOL. Moreover, we examined some maternal and fetal morbidities among Nippita groups. As one would anticipate, groups 7, 8, and 9 have the highest rates of such morbidities.
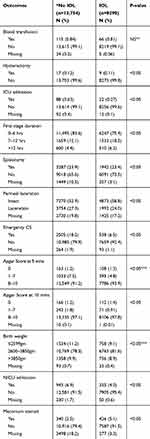 |
Table 4 Selected Maternal And Neonatal Outcomes |
Discussion
Our study demonstrated that 24.8% of the singleton pregnancies had IOL. The rate in the WB was more than three-folds higher than that in Gaza. The overall rate for IOL in this study, and particularly, the IOL rate in the WB is much higher than rates previously recommended by the WHO, which suggest that these should not exceed 10% in any region.1,21 Compared with the IOL rates reported in the WHO multi-country study; the overall rate in our study was higher than those reported from Algeria (6.8%), India (12.8%), and Japan (19.0%) but lower than Sri Lanka (35.5%).8 The most established reason for IOL is prolonged pregnancy. According to Olesen et al, only 5–10% pregnant women will continue their pregnancy till 42 weeks or beyond.22 Most women in our study were induced before reaching 41 weeks’ gestation which seems to be at odds with recommended evidence.1,5 However, our results are similar to the findings of an audit of IOL practices involving 20,439 births in 3 Australian hospitals which also used the Nippita IOL categorization. The Australian audit reported an IOL rate of 24.7% with variations observed among hospitals. The proportion of singleton cephalic pregnancies induced between 37 and 38 weeks’ gestation was high for both nulliparous (38.8%) and multiparous groups (30.2%), albeit, higher than rates of similar groups in our study.23
Despite the presence of clear and evidence-based guidelines for IOL in Palestine at the time of this study,15 variations were still observed in the contribution of the different Nippita groups to the IOL cohorts within the different participating units and regions. Our findings concur with observations made by other investigators.24 Indeed, these variations have been reported to be happening at individual professional,25 hospital,23 regional,24,26 and country8 levels. Variations in clinical practice are common in obstetrics, yet problematic and can lead to errors.27 They can add unnecessary cost to the health system, affect the quality of care, and may increase morbidity among women and newborns during childbirth.13 Indeed, early hospital admission, for a non-clinically indicated IOL in this case, might increase a woman’s risk for further medical interventions,3 neonatal morbidity, and cost to the Palestinian health system.
We did not explore the reasons for these variations; therefore, we can only speculate that such variation could be attributed to several factors such as perceived lack of strong evidence, differences in knowledge level among physicians, lack of adherence to the clinical guidelines, and differences in resource availability between the two studied regions where Gaza has several resource constraints.
In spite of our relatively large sample size, we look cautiously to the outcomes of IOL in our cohort as estimates of outcomes can be confounded by several aspects including the indication for induction, maternal medical history, fetal condition, and intrapartum management. Hence, some authors suggest that IOL outcomes are examined against expectant women who were managed within the same gestational week and not with women who had spontaneous labor as in our study.28,29 Recently, the ARRIVE trial compared the elective IOL at 39 weeks to expectant management of labor among healthy low-risk nulliparous women. It is worth noting that although the study suggested that IOL at 39th week of pregnancy resulted in fewer cesarean rates and no significant difference in perinatal mortality and severe perinatal morbidity, only 27% (6106 out of 22,533) of women agreed to participate. This reflects that elective IOL is not something desired by women.11
Strengths And Limitations
A major strength of this study is the large number of births that were prospectively included, which enabled us, for the first time, to highlight detailed aspects of the actual IOL practice in Palestine. Nonetheless, our study had some limitations. First, the missing information relating to indications of induction did not enable us to undertake a comprehensive analysis of this aspect. Second, data on favorability of the cervix were not collected, which, if available, could have provided better understanding of the decision to undertake an induction and the choice of method to do so.
Information relating to IOL indication was missing in nearly two-thirds of participants (5114; 65.5%), hindering our ability to undertake a meaningful analysis of this aspect. Although post-term pregnancy was the most commonly documented indication, the majority of women were induced before reaching 41 weeks’ gestation. Given that the attending midwife or physician had the responsibility to complete the intrapartum registration forms, it is not clear why the fields related to IOL, where applicable, were not completed. It is possible that the missing data is a reflection of unclear documentation in the woman’s pregnancy records of the reason why she was booked for IOL by the physician when the procedure was decided or the possibility that women with missing indication could have been induced for a reason that is not in line with the local evidence-based policy. Although lack of documented reason for induction has been demonstrated in several studies, the rate we report is higher than those reported from South America (44%),30 Australia (16.1%),31 and the United States (7.9%).9 However, it is important to note that some of these studies categorized women with no documented reason for induction as elective (no medical indication) inductions.8,9,30 Effective and efficient use of available resources and ensuring safe childbirth practices for optimal outcomes are crucial for any health service and indeed, for a country with limited resources like Palestine. IOL is an invasive and costly procedure that could be associated with complications and adverse outcomes, nonetheless, it is reported that sometimes women undergo such procedure without sufficient information.32 It is imperative that such procedure should only be performed if there is a clear medical indication and the woman’s informed consent.
Conclusions
Of the two Palestinian regions we studied, IOL seems to be an overused policy in the WB and frequently performed at or before 40 weeks’ gestation in both regions. There were clear variations in practice among participating units and regions. These variations may reflect lack of implementation of national IOL guidelines. This study is a crucial initial step to inform quality improvement interventions aimed at closing the gap between evidence and practice with regards to IOL in Palestine. A comprehensive understanding of IOL practice within a low-income setting like the Palestinian context would require future studies that aim to compare the outcomes of IOL while considering expectant management of women, indications for IOL and the health-care cost of the utilized IOL methods.
Implications For Clinical Practice
Clinical guidelines serve as a tool to guide and standardize clinical practice and minimize variations among clinicians.27 Moreover, standardization of clinical care improves patient outcomes, increases quality, reduces variation, decreases cost, and reduces medico-legal liability.27 The clinical obstetric guidelines in Palestine were developed by obstetricians and midwives and recommend that:
If no pregnancy complications exist, review at 40 weeks and offer membrane sweeping. If sweeping does not induce labor, appropriate fetal surveillance should continue until 40 weeks +7 days when other IOL method should be commenced.15
Our analysis sheds light on the current actual practice of IOL in Palestine. We believe that a national obstetric clinical audit program should be introduced and mandated to monitor guidelines adherence and relate these to clinical indicators and outcomes.
Abbreviations
IOL, induction of labor; WHO, World Health Organization; dhis2, District Health Information Software; TSD, Tjeneste for Sensitive Data; PROM, premature rupture of membranes; SPSS, Statistical Package for Social Sciences; WB, West Bank.
Ethics Approval And Informed Consent
Ethical approval for the study was obtained from the Helsinki Committee for Ethical Approval in Gaza (PHRC/HC/13/15), the Palestinian Ministry of Health, each participating hospital, the Norwegian Data Inspectorate (17/00082-2/GRA) and the Regional Committee for Medical and Health Research Ethics in South-Eastern Norway (REK 2014/1727) and the Norwegian Data Inspectorate (17/00082-2/GRA) reviewed and approved this study as health-quality research which can be implemented without its approval within the ordinary health services arrangements; as long it is done in accordance with common rules for health care services in Palestine and Norway regarding confidentiality and privacy. Verbal consent was considered valid. As per standard practice, verbal consent was obtained from women to include their data in the intrapartum registration forms.
Data Sharing Statement
The dataset generated and analyzed during the current study is not publicly available. The data is securely stored in a special platform (Service for Sensitive Data (TSD)) owned by the University of Oslo. Access to the data required special permission.
Acknowledgments
We acknowledge the Palestinian Ministry of Health, the participating hospitals' administrators, and the heads of maternity wards, for their facilitation of the study, and all the midwives for their efforts in data registration and entry. We acknowledge the Norwegian Research Council for supporting this study (grant number 234452).
Author Contributions
All authors contributed towards data analysis, drafting and critically revising the paper, gave final approval of the version to be published, and agreed to be accountable for all aspects of the work.
Funding
This study was supported by the Norwegian Research Council (grant number 234452). The funding source had no role in the study design, data collection, analysis, interpretation or writing of this manuscript.
Disclosure
The authors report no conflicts of interest in this work.
References
1. World Health Organization, Department of Reproductive Health and Research. WHO Recommendations for Induction of Labour: Evidence Base. Geneva: WHO; 2011.
2. Leduc D, Biringer A, Lee L, Dy J. Induction of labour: SOGC Clinical Practice Guideline No. 296. J Obstet Gynaecol Can. 2013;35(9):S1–S18. doi:10.1016/S1701-2163(15)30699-X
3. Ruhl C, Bingham D. Midwives and nonmedically indicated induction of labor. J Midwifery Womens Health. 2014;59(3):233–236. doi:10.1111/jmwh.12197
4. Bonsack CF, Lathrop A, Blackburn M. Induction of labor: update and Review. J MidwiferyWomens Health. 2014;59(6):606–615.
5. Mozurkewich E, Chilimigras J, Koepke E, Keeton K, King VJ. Indications for induction of labour: a best-evidence review. BJOG. 2009;116(5):626–636. doi:10.1111/j.1471-0528.2008.02065.x
6. Gulmezoglu AM, Crowther CA, Middleton P, Heatley E. Induction of labour for improving birth outcomes for women at or beyond term. Cochrane Database Syst Rev. 2012;6:Cd004945.
7. The American College of Obstetricians and Gynecologists: Women’s Health Care Physicisns. Induction of labor: clinical management guidelines for obstetrician –gynecologists number. 107. Obstetrics Gynecology. 2009;114(2):386–397.
8. Vogel JP, Souza JP, Gulmezoglu AM. Patterns and outcomes of induction of labour in Africa and Asia: a secondary analysis of the WHO Global Survey on Maternal and Neonatal Health. PLoS One. 2013;8(6):e65612. doi:10.1371/journal.pone.0065612
9. Lydon-Rochelle MT, Cárdenas V, Nelson JC, Holt VL, Gardella C, Easterling TR. Induction of labor in the absence of standard medical indications: incidence and correlates. Med Care. 2007;45(6):505–512. doi:10.1097/MLR.0b013e3180330e26
10. Declercq ER, Sakala C, Corry MP, Applebaum S, Herrlich A. Listening to MothersSM III: Pregnancy and Birth. New York: Childbirth Connection; May 2013.
11. Grobman WA, Rice MM, Reddy UM, et al. Labor induction versus expectant management in low-risk nulliparous women. N Engl J Med. 2018;379(6):513–523. doi:10.1056/NEJMoa1800566
12. Mozurkewich EL, Chilimigras JL, Berman DR, et al. Methods of induction of labour: a systematic review. BMC Pregnancy Childbirth. 2011;11(84):1–19.
13. Tillett J. Elective induction of labor prior to 39 weeks: initiating a change in culture. J Perinat Neonatal Nurs. 2012;26(3):190–192. doi:10.1097/JPN.0b013e3182611bb7
14. Hassan S, Wick L, DeJong J. A glance into the hidden burden of maternal morbidity and patterns of management in a Palestinian governmental referral hospital. Women Birth. 2015;S1871-5192(1815):00272–00273.
15. Ministry of Health, UNFPA. Obstetric Guidelines and Labour Ward Protocols.
16. Ministry of Health, PHIC. Health Status, Palestine, 2017. Ramallah: Ministry of Health; 2018.
17. Ministry of Health, PHIC. Health Status, Palestine 2015. Ramallah, Palestine: Ministry of Health;2016.
18. Hassan S, Vikanes A, Laine K, et al. Building a research registry for studying birth complications and outcomes in six Palestinian governmental hospitals. BMC Pregnancy Childbirth. 2017;17(1):112. doi:10.1186/s12884-017-1296-6
19. World Health Organization. WHO Recommendations: Intrapartum Care for a Positive Childbirth Experience.; 2018. Geneva: World Health Organization; 2018.
20. Nippita TA, Khambalia AZ, Seeho SK, et al. Methods of classification for women undergoing induction of labour: a systematic review and novel classification system. BJOG. 2015;122(10):1284–1293. doi:10.1111/1471-0528.13478
21. World Health Organization. WHO (1985) Appropriate technology for birth. Lancet. 1985;(August 24):436–437.
22. Olesen AW, Westergaard JG, Olsen J. Perinatal and maternal complications related to postterm delivery: a national register-based study, 1978-1993. Am J Obstet Gynecol. 2003;189(1):222–227. doi:10.1067/mob.2003.446
23. Biro MA, East CE. Using the Nippita classification system for women undergoing induction of labour in a large metropolitan maternity service: bringing simplicity and certainty to an important quality improvement process. Aust N Z J Obstet Gynaecol. 2017;57(2):228–231. doi:10.1111/ajo.12598
24. Nippita TA, Trevena JA, Patterson JA, Ford JB, Morris JM, Roberts CL. Variation in hospital rates of induction of labour: a population-based record linkage study. BMJ Open. 2015;5(9):e008755. doi:10.1136/bmjopen-2015-008755
25. Heazell AE, Green M, Wright C, Flenady V, Froen JF. Midwives’ and obstetricians’ knowledge and management of women presenting with decreased fetal movements. Acta Obstet Gynecol Scand. 2008;87(3):331–339. doi:10.1080/00016340801902034
26. Nippita TA, Trevena JA, Patterson JA, Ford JB, Morris JM, Roberts CL. Inter-hospital variations in labor induction and outcomes for nullipara: an Australian population-based linkage study. Acta Obstet Gynecol Scand. 2016;95(4):411–419. doi:10.1111/aogs.12854
27. The American College of Obstetrciians and Gynecologists: Women’s Health Care Physicisns. Committee opinion No. 629. Clinical guidelines and standardization of practice to improve outcomes. Obstet Gynecol. 2015;125(629):1027–1029. doi:10.1097/01.AOG.0000462932.18418.7a
28. Danilack VA, Triche EW, Dore DD, Muri JH, Phipps MG, Savitz DA. Comparing expectant management and spontaneous labor approaches in studying the effect of labor induction on cesarean delivery. Ann Epidemiol. 2016;26(6):405–411. doi:10.1016/j.annepidem.2016.04.009
29. Little SE, Caughey AB. Induction of labor and cesarean: what is the true relationship? Clin Obstet Gynecol. 2015;52(2):269–281. doi:10.1097/GRF.0000000000000112
30. Guerra GV, Cecatti JG, Souza JP, et al. Factors and outcomes associated with the induction of labour in Latin America. BJOG. 2009;116(13):1762–1772. doi:10.1111/j.1471-0528.2009.02348.x
31. Zhao Y, Flatley C, Kumar S. Intrapartum intervention rates and perinatal outcomes following induction of labour compared to expectant management at term from an Australian perinatal centre. Aust N Z J Obstet Gynaecol. 2017;57(1):40–48. doi:10.1111/ajo.12576
32. Gatward H, Simpson M, Woodhart L, Stainton MC. Women’s experiences of being induced for post-date pregnancy. Women Birth. 2010;23(1):3–9. doi:10.1016/j.wombi.2009.06.002
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
