Back to Journals » International Journal of Nanomedicine » Volume 14
Ethosomal Gel for Improving Transdermal Delivery of Thymosin β-4
Authors Fu X, Shi Y , Wang H, Zhao X, Sun Q, Huang Y, Qi T, Lin G
Received 27 August 2019
Accepted for publication 16 November 2019
Published 27 November 2019 Volume 2019:14 Pages 9275—9284
DOI https://doi.org/10.2147/IJN.S228863
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Phong A Tran
Xianglei Fu,1 Yanbin Shi,2 Hui Wang,1 Xiaogang Zhao,3 Qifeng Sun,3 Yi Huang,1 Tongtong Qi,1 Guimei Lin1
1School of Pharmaceutical Science, Shandong University, Jinan 250012,People’s Republic of China; 2School of Mechanical & Automotive Engineering, Qilu University of Technology (Shandong Academy of Sciences), Jinan 250353, People’s Republic of China; 3The Second Hospital of Shandong University, Jinan 250033, People’s Republic of China
Correspondence: Guimei Lin
School of Pharmaceutical Science, Shandong University, 44 West Wenhua Road, Jinan 250012, People’s Republic of China
Tel +86-531- 88382548
Fax +86-531-89631517
Email [email protected]
Purpose: Thymosin β-4(Tβ-4) is a macromolecular protein drug with potential for drug development in wound repair but is limited by the shortcomings of macromolecular protein, such as large volumes, poor membrane permeability, and unstable physicochemical characteristics. Ethosomes could enhance cell membrane fluidity and reduce epidermal membrane density to make macromolecular drugs through the stratum corneum into the deeper layers of the skin easily. Herein, we developed and characterized a novel transdermal delivery vehicle to load macromolecular protein peptides and use Tβ-4 as a model drug wrapped into ethosomes.
Methods: We used the orthogonal method to optimize the formulation of the ethosome preparation prepared by the ethonal infusion method. Ethosomal gels were characterized by using different analytical methods. Transdermal release rate in vitro have been demonstrated in Franz diffusion cells and the efficacy of drug-loaded nanocarriers in vivo was investigated in a mouse model.
Results: Optimized Tβ-4 ethosomal gels have good physicochemical properties. The drug amounts of the cumulative release in the ethosomal gel within 5 hours were 1.67 times that of the T-β4 gel in vitro release study, and the wound healing time of ethosomal gel group was only half of the T-β4 gel group in vivo pharmacokinetic study. Compared with the free drug group, the ethosome preparation not only promotes the percutaneous absorption process of the macromolecular protein drugs but also shortened wound recovery time.
Conclusion: Hence, we provide a possible good design for ethosomal gel system that can load macromolecular protein peptide drugs to achieve transdermal drug administration, promoting the percutaneous absorption of the drug and improving the effect.
Keywords: ethosomes, transdermal drug delivery system, macromolecular protein drugs, skin wound healing
Introduction
Thymosin β-4 (Tβ-4) is an important actin regulatory molecule with multiple functions in the human body that can promote cell differentiation and maturation, promote tissue regeneration and remodeling, repair blood vessels and hair follicles, among other functions. It is easily soluble in water and has a large molecular weight.1 Negatively charged Thymosin β-4 is composed of 34 amino acid residues. Its molecular weight is 4963Da and isoelectric point is 5.1. However, as a protein peptide drug, the molecular structure is easily destroyed in the gastrointestinal tract via oral administration and they have poor medication compliance. The transdermal drug delivery system (TDDS) can make drugs directly exert the local effect and avoid the hepatic first-pass effect and gastrointestinal tract damage to maintain a constant blood concentration. Additionally, medication compliance in patients can significantly improve.2 Therefore, the protein polypeptide is very suitable for TDDS to exert local efficacy. However, the molecular weight of Tβ-4 is much larger than that of the drug that is suitable for delivery by the TDDS and transdermal administration alone cannot penetrate well into the skin to exert its efficacy.
As the outermost barrier of the skin, the stratum corneum is tightly connected and is the main obstacle and rate-limiting step for drug penetration into the skin.3 In recent studies, to increase the penetration rate of drugs, some physical and chemical methods have been used in pharmacy such as the use of iontophoresis,4 microneedles,5 chemical penetration enhancers,6 nanocarriers,7 and liposomes8 to promote the drug through the skin barrier. However, these physicochemical methods also have potential disadvantages such as poor stability, a complicated preparation process and severe skin irritation.
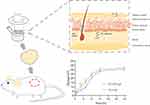
Traditional liposomes, due to their limited penetrating ability, cannot penetrate the stratum corneum and can only take drugs to the surface of the skin, failing to achieve the effect of deep treatment.8 Therefore, to overcome the limitations of liposomes in the TDDS, we have studied a novel drug carrier-loaded system, ethosomes, to encapsulate the drug.9 Ethosomes, which are similar to liposomes with a cell membrane-like phospholipid bilayer structure and excellent biocompatibility, are nanoparticle preparations comprising phospholipid, cholesterol (CHOL) and ethanol. Compared with liposomes, a higher concentration of ethanol (20–50%) is added in the preparation process.10 As a chemical penetration enhancer, ethanol can change the dense alignment of the cell lipid layer in the skin stratum corneum and reduce structural density (Figure 4A).11 Studies have shown that ethosomes have a smaller particle size and higher stability than traditional liposomes. Additionally, the unique advantages of nontoxic and non-irritating ethosomes make them a research focus of TDDS.12 In the prior related experiments, no ethosomes were found to load macromolecular protein polypeptide drugs to achieve transdermal drug delivery.
In the present study, we designed a Tβ-4 ethosome delivery system using the ethanol agitation method, which is simple and environmentally friendly. The Tβ-4 ethosomes were then loaded onto the gel. Using high performance liquid chromatography (HPLC), transmission electron microscope (TEM), scanning electron microscope (SEM), and Rheology tests, we explored the preferred formulation process of Tβ-4 ethosomal gels.The efficacy of drug-loaded nanocarriers was tested by the transdermal release rate in vitro and in vivo pharmacokinetic study. The purpose of this study is to develop ethosome gel system that can load macromolecular protein peptide drugs to achieve transdermal drug administration, significantly promoting the percutaneous absorption of the drug and improving the effect.
Materials and Methods
Materials
Thymosin beta-4 (Tβ-4 (98%, purity)) was purchased from Nanjing Luomaimei Biological Technology Co., Ltd. (Nanjing, China). l- alpha- phosphatidylcholine from soybean (SPC) was supplied from Sigma Aldrich (Shanghai) Trading Co., Ltd. (San Francisco, USA). Cholesterol (CHOL) was obtained from Sigma Aldrich (Shanghai) Trading Co., Ltd. (San Francisco, USA). Sodium deoxycholate and phosphotungstic acid were obtained from Beijing Wokai Biological Technology Co., Ltd. (Beijing, China). Carbomer 934 was acquired from Dalian Meilun Biotechnology Co., Ltd. (Dalian, China). Phosphate-buffered saline (PBS) was from Beijing Solarbio Science And Technology Co., Ltd. (Beijing, China). The experimental water was made using a Milli-Q ultrapure water system (Millipore, Ireland). The acetonitrile and triethanolamine used were chromatographic grade, and other reagents were of analytical grade.
Animals
Female Kunming mice (25±3 g, 4 weeks old) were supplied by the Experimental Animal Center of Shandong University (Jinan, China), and New Zealand rabbits (2.5±0.5 kg) were supplied by Jinan Jinfeng Experimental Animal Co., Ltd. (Jinan, China). All the animals were kept and used for the experiment in accordance with the ethics and regulation of animal experiments of Pharmaceutical Sciences, Shandong University, China. The work described has been carried out in accordance with The Code of Ethics of the World Medical Association (Declaration of Helsinki) for experiments.
Preparation and Characterization of Tβ-4 Ethosomal Gels
Preparation of Tβ-4 Ethosomal Gels (Figure 1)
The Tβ-4 ethosomes were prepared by ethonal infusion. The appropriate amounts of SPC and CHOL dissolved in ethanol were added into a glass flask as the alcohol phase. The appropriate amount of Tβ-4 was dissolved in phosphate-buffered saline (PBS, pH 7.4; 10 mM Na2 HPO4, 1.76 mM KH2PO4, 137 mM NaCl, 2.7 mM KCl) as the aqueous phase with some sodium deoxycholate to promote the stability of alcohol plastids.13 While maintaining the water bath temperature at 30±2°C using the RCT basic thermostatic magnetic stirrer (IKA, Staufen, Germany), the aqueous phase was injected into the alcohol phase at a certain rate under magnetic stirring and hydration was continued for 15 min. Next, the Tβ-4 ethosomes were filtered through the 0.22-μm filter and were stored at 4 °C. The carbomer was slowly added to the distilled water at a ratio of 1:50 (w/w) in a beaker and then was mixed at 700 rpm for 3 hrs to form a uniformly dispersed gel matrix.
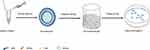 |
Figure 1 Preparation of Tβ-4 ethsomal gel. Abbreviation: CHOL, cholesterol. |
According to the preparation process of the ethanol injection method, other conditions were fixed to change the single factor (dosage amount, CHOL dosage, sodium deoxycholate dosage, hydration speed, hydration temperature, hydration time, water injection speed), and the encapsulation efficiency (EE) was mainly investigated considering the particle size, morphology, stability, and uniformity of the nanoparticles, and screening out the factors that have significant effects for the orthogonal design.14 Next, the Tβ-4 ethosomes were mixed with a suitable amount of fully swollen gel to obtain the Tβ-4 ethosomal gel.
Characterization of Tβ-4 Ethosomes
The nanoparticle size, size distribution and zeta potentials of diluted Tβ-4 ethosome solution were measured using the Malvern Zetasizer Nano ZS system (Malvern, Westborough, UK).15 The microstructure of Tβ-4 ethosomes was detected using a TEM (JEM 1200EX, JEOL, Tokyo, Japan) by dropping Tβ-4 ethosome solution onto special carbon-coated copper grids and dyeing with phosphotungstic acid (2%, w/w) for 10–15 s.
The entrapment efficiency (EE%) and drug loading of Tβ-4 (DL%) were determined by high-speed centrifugation using high-performance liquid chromatography (HPLC) with the method of gradient elution and the prepared Tβ-4 ethosomes solution was centrifuged at 10,000 r/min for 10 min, resulting in nonentrapped Tβ-4 suspended in the supernatant and Tβ-4 ethosomes forming precipitates at the bottom of the centrifuge tube. The supernatant was filtered through a 0.22-µm filter to absorb 20 µL and was determined by HPLC using a Shimadzu HPLC system (Shimadzu, Kyoto, Japan) at a UV absorption wavelength of 228 nm and a reversed-phase C18 column (4.6 mm×250 mm; 5 μm; Dikma). The mobile phases were 0.5% trifluoroacetic acid acetonitrile solution and 0.5% aqueous trifluoroacetic acid solution eluting with a gradient speed of 1.0 mL/min. The drug loading (DL) and encapsulation efficiency were calculated as follows, EE=(W2-W1)/W2*100%, DL=(W2-W1)/W3*100%, where W1 is the weight of nonentrapped Tβ-4, W2 is the total weight of added Tβ-4, and W3 is the total weight of the formulation materials.16
Characterization of the Tβ-4 Ethosomal Gel
To evaluate the formulation’s adhesion, the viscosity of the Tβ-4 ethosomal gel was detected using a high-temperature and high-pressure rheometer (MCR302; Anton Paar, Austria) and shear stress-shear rate curves were measured at 25°C using a 79039 CP25-2 cone (D=25 mm; 1°). When the gel is placed between the stationary plate and rotated cone, the shear rate ranged from 0.1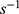 to 100
to 100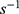 and the gap was set at 106 µm. The viscosity of the gel stored at a temperature of 25 °C, 4 °C, and 40 °C for 7 days was measured to examine the influence of different temperatures on the rheology of the gel.
and the gap was set at 106 µm. The viscosity of the gel stored at a temperature of 25 °C, 4 °C, and 40 °C for 7 days was measured to examine the influence of different temperatures on the rheology of the gel.
The PRO liposomal gel mixed with freeze-dried protective agents was prefrozen in the ultra-low-temperature refrigerator at −80 °C (DW-86L, Haier, Qingdao, China) for 24 h to prepare for long-term preservation. Freeze-dried products were sprayed with gold and were observed by SEM (JSM-6700F, JEOL, Tokyo, Japan).
In vitro Drug Release Study
Kunming mice weighing approximately 25 g were anesthetized with 4% chloral hydrate at a dose of 0.01 mL/g, and their back hair was depilated with a hair removal cream and a pet shaver. Kunming strain mice were randomly divided into two treatment groups, 4 mice in each group. The exposed back skin was cleaned with saline, and the mice were sacrificed after 24 hrs. The skin on the back was quickly excised, and the subcutaneous tissue was removed, washed in normal saline and dried using filter paper. Skin samples needed to be prepared at the time of use and confirmed by microscopic observation to show no damage. Other methods like radiotracers17,18 and electrochemical methods19,20 could also be used to pre-screen skin.21
The skin was fixed in Franz diffusion cells which were custom built in Jinan Chuanxu Glass Instrument Co., Ltd. with an effective diffusion area of 3.14 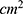 where 10 mL of phosphate-buffered saline was added to the receiving cell and Tβ-4 ethosomal gel, and the Tβ-4 gel containing both 0.1 mg of drug and free gel was placed on the side of the stratum corneum of the isolated skin. The receptor medium was stirred at 100 rpm, and the water bath temperature was controlled at 37±0.5°C throughout the experiment. For each experiment, 400 µL of receptor medium was taken and 400 µL of phosphate-buffered saline was added at predetermined time intervals (0.5, 1, 3, 5, 8, 12, 24 h).22 The removed receptor medium was filtered through 220-nm filters, stored at −20 °C for use and assayed for their Tβ-4 by HPLC. The accumulative permeation of Tβ-4 was calculated according to the formula
where 10 mL of phosphate-buffered saline was added to the receiving cell and Tβ-4 ethosomal gel, and the Tβ-4 gel containing both 0.1 mg of drug and free gel was placed on the side of the stratum corneum of the isolated skin. The receptor medium was stirred at 100 rpm, and the water bath temperature was controlled at 37±0.5°C throughout the experiment. For each experiment, 400 µL of receptor medium was taken and 400 µL of phosphate-buffered saline was added at predetermined time intervals (0.5, 1, 3, 5, 8, 12, 24 h).22 The removed receptor medium was filtered through 220-nm filters, stored at −20 °C for use and assayed for their Tβ-4 by HPLC. The accumulative permeation of Tβ-4 was calculated according to the formula 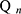 = (
= (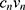 +
+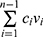 )/S, where Cn is the mass concentration of the drug measured at the nth time point, V0 is the total volume of the Franz diffusion cell’s receptor medium, Ci is the measured drug concentration before the nth time point, Vi is each sample volume, and S is the effective diffusion area of the isolated skin.
)/S, where Cn is the mass concentration of the drug measured at the nth time point, V0 is the total volume of the Franz diffusion cell’s receptor medium, Ci is the measured drug concentration before the nth time point, Vi is each sample volume, and S is the effective diffusion area of the isolated skin.
In Vivo
Skin Irritation Test
To evaluate and compare the skin irritation of the Tβ-4 ethosomal gel and blank Tβ-4 gel, the study was carried out on New Zealand rabbits. Weighed rabbits were anesthetized with 10% chloral hydrate in the ear vein, and the back hair of New Zealand rabbits was removed by mild hair removal cream at 24 h prior to application of the formulations. The exposed back skin was cleaned with saline and confirmed to show no damage. The back skin was scratched with a scalpel to ooze blood and was divided into three groups as follows: Tβ-4 ethosomal gel, Tβ-4 gel and gel (control). Using the same body control method, both the intact skin of rabbits and damaged skin of rabbits were given 0.5 g of Tβ-4 ethosomal gel, Tβ-4 gel and blank gel. The presence or absence of irritation and redness was observed at 1, 24, 48, and 72 hrs after administration. The Draize scale was applied to evaluate the skin irritation, and irritation scores between 0 and 4 were used to grade the stimulus intensity, which ranged from no response to a severe response.
In vivo Pharmacokinetic Study
The Kunming mice were anesthetized and depilated according to the method of 2.4, and the skin was confirmed to be intact after 24 hrs. The circular filter paper with a diameter of 0.6 cm infiltrated with 5 mol/L of sodium hydroxide was placed on the back skin of Kunming mice for 30 s,23 and then the back skin was cleaned with saline to remove residual sodium hydroxide solution to form a deep second-degree burn model. Each Kunming mouse was scalded in three places to put up control experiments and three scald parts of each mouse were daily given different preparations: Tβ-4 ethosomal gel, Tβ-4 gel and blank gel. The wound area was measured every day. Meanwhile, the wound inflammatory reaction, wound scarring time, healing time and rate of scar formation were recorded. After all the treatments, the Kunming mice were sacrificed and the skins of the mice were removed according to the method of 2.4 and were immediately fixed in 10% formaldehyde solution for 24 hrs. The sample was then dehydrated and transparent using ethanol and xylene, embedded in paraffin, and then stained with hematoxylin and eosin (H&E). Finally, the skin was sliced with a paraffin slicer and analyzed using the Olympus VS120 panoramic digital slice scanning microscope (Tokyo, Japan) in the bright-field mode for scanning HE section analysis.24
Statistical Analysis
All experiments in this study were repeated at least three times, and the data were presented as the means ± standard deviation (SD). One- and two-way analyses of variance were used when making multiple comparisons, the two tailed t-test was used to compare two groups, and a P-value <0.05 was statistically considered significant. All statistical analyses were performed using GraphPad Prism 8 software and SPSS 19.0 software. Statistical significance was noted as follows: *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001.
Results and Discussion
Preparation of Tβ-4 Ethosomes
The main factors affecting the particle size of the Tβ-4 ethosomes are as follows: stirring speed and injection speed, CHOL dosage, ethanol concentration and different concentrations of sodium deoxycholate.
A smaller particle size and better deformability makes it easier for Tβ-4 ethosomes to pass through the skin barrier. Using the ethanol injection method, Tβ-4 ethosomes with a smaller particle size could be obtained under the action of a specific stirring rate and water injection speed. The larger the stirring speed is, the better the hydration effect is (Figure 2A). If the stirring speed is too fast, Tβ-4 ethosomes are easily broken by mechanical action, reducing low encapsulation efficiency and drug-loading capacity (DL). From TEM photographs, we found that Tβ-4 ethosomes were not easily broken and were dispersed when the hydration speed was 700 rpm and the water injection rate was 200 µL/min without ultrasonic disruption or liposome extrusion. The concentration of CHOL significantly affected the size of Tβ-4 ethosomes (Figure 2B), and studies have shown that the addition of CHOL helps to increase the drug encapsulation efficiency.25 Compared with ordinary liposomes, Tβ-4 ethosomes were added a higher concentration (20–50%) of ethanol to change the dense arrangement of lipid bilayers in the stratum corneum cells, enhance the flexibility and deformability of the membrane and promote transdermal absorption. As the amount of ethanol increased, the particle size of the alcohol body also became larger (Figure 2C). From the transmission electron micrograph, the ethosomes containing a higher concentration of ethanol were more likely to be broken or polymerized. In general, Tβ-4 is a hydrophilic macromolecular protein drug with poor transdermal permeability and a low encapsulation efficiency. It was reported that the surfactant sodium deoxycholate changed the filling properties of the lipid in the bilayer, resulting in higher deformability, and it could be inserted between the lipid bilayers, resulting in a lower phase transition temperature of the skin lipid.26 The addition of sodium deoxycholate to Tβ-4 ethosomes could significantly improve the particle size (Figure 2D) and enhance the negative charge which is good for stability.
Factors affecting the encapsulation efficiency of Tβ-4 ethosomes by single-factor experiments were the CHOL dosage, ethanol concentration, different concentrations of sodium deoxycholate and Tβ-4 concentration. The optimal prescription was screened by orthogonal experiment using the encapsulation efficiency as an indicator. The final molar ratio of SPC: CHOL: sodium deoxycholate: Tβ-4 was 10:7:8:1, and the ethanol/liquid (v/v) rate was 30%.
Characterization of Tβ-4 Ethosomes
After the prescription was optimized, from the TEM (Figure 3A), we observed that the Tβ-4 ethosomes that had large single intermediate hydrophilic cavities suitable for the encapsulation of hydrophilic drug had a rounded appearance, a uniform particle size and good dispersibility. As shown in Figure 3A, the size of the Tβ-4 ethosomes was 127.8 ± 3.2 nm, and the zeta potential was −25.1 ± 2.8 mv using the Malvern Zetasizer Nano ZS system.27 The EE measured was (63.2±4.5) %, and the DL was (2.34±0.53) %. Although the DL of Tβ-4 ethosomes was low, it could be very effective when it was used to repair wounds because Tβ-4 is a powerful biological factor in which microdrug penetration into the skin could play a role.
 |
Figure 3 The TEM photograph and size distribution of Tβ-4 ethosomes (A) and the characterization of ethosomal gel: shear stress–shear rate curves (B) and the SEM photograph (C). |
Characterization of the Tβ-4 Ethosomal Gel
The results of the rheological test of the Tβ-4 ethosomal gel are shown in the figure (Figure 3B). As the shear rate increased, the slope of the shear stress-shear rate curve decreased gradually, indicating that the viscosity of the formulation decreased and the gel exhibited pseudoplastic flow. When the shear rate was 0.1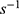 , the viscosity of the preparation was 517 Pa·s, proving that the gel could effectively adhere to the skin. The rheological properties did not change significantly after the formulation was placed in the dark at 4 °C, 25 °C, and 40 °C for 7 days, and the stability was good.
, the viscosity of the preparation was 517 Pa·s, proving that the gel could effectively adhere to the skin. The rheological properties did not change significantly after the formulation was placed in the dark at 4 °C, 25 °C, and 40 °C for 7 days, and the stability was good.
Under the scanning condition of SU8010 5.0 kV 10.3 mm*100 k SE (UL), the morphology of the freeze-dried powder of the Tβ-4 ethosomal gel was observed using the SEM (Figure 3C). The Tβ-4 ethosomes were evenly distributed inside the gel matrix, and there were many protrusions on the surface of the gel matrix. The size of the ethosomes was equal to the particle size measured under transmission electron microscopy, indicating that it was not significantly changeable for ethosomes in the morphology and size of the gel matrix after freeze drying.
In vitro Drug-Release Study
Transdermal experiments in vitro demonstrated that the permeation rate of the Tβ-4 by the ethosomal gel was greater than that by the Tβ-4 gel within 8 h after administration (Figure 4). Regression was performed to fit zero-order, first-order, Higuchi and Weibull infiltration behavioral dynamics equations based on the relevant data.28 During 0.5~5 h, accumulative release percent (Ԛt) of the Tβ-4 EP gel to t fitted the first-order kinetic equation Ԛt =−0.1260t-0.0608 R=0.9990. Ԛt of the Tβ-4 gel to t1/2 fitted the Higuchi equation Ԛt =0.1352t1/2−0.0101 R=0.9983. During 5~24 h, Ԛt of both the Tβ-4 EP gel and Tβ-4 gel to t fitted the first-order kinetic equation as follows Tβ-4 EP gel:Ԛt =−0.3990t+1.565 R=0.9977; Tβ-4 gel: Ԛt =−0.1561t+0.1413 R=0.9721.
The amounts of the cumulative release in the ethosomal gel and Tβ-4 gel within 5 hrs were respectively determined to be 15.77 μg/cm2 and 9.430 μg/cm2, indicating that the ethosomal gel acted as a drug carrier to promote the transdermal rate of the macromolecular protein drug. During 0.5~5 h, Ԛt of the Tβ-4 EP gel to t fitted the first-order kinetic equation, indicating that the drug passed through the skin quickly while Ԛt of the Tβ-4 gel to t1/2 fitted the Higuchi equation in the initial phase, indicating a slow rate of penetration. During 5~24 h, the ethosomal group had a higher permeation rate than the free drug group. Additionally, due to individual differences in the body weight and skin thickness of Kunming mice, the correlation coefficient can be appropriately reduced considering that the ripple factor is large, and a correlation coefficient below 0.99 is acceptable.29
In Vivo
Skin Irritation Test
One of the major drawbacks of TDDSs is the irritation of the formulation to the skin. Rabbits are highly sensitive to skin irritation and are easy to feed in the laboratory. Thus, rabbits are widely used in skin penetration studies to predict human skin irritation and determine the safety.30 The results of the skin irritation study listed in Table 1 indicated that the skin of New Zealand rabbits were not allergic to the Tβ-4 ethosomal gel, Tβ-4 gel, and the blank gel after 24 h of application and 7 days of repeated applications. The carbomer gel and T-β4 used in this experiment had good biocompatibility. The phospholipids, CHOL and ethanol used in the preparation of ethosomal gel were mild, a finding consistent with the drug design principle of Quality by Design (QbD).31
 |
Table 1 The Irritation Scores of Gels to the Rabbit Skin After Administration of 24h and 7 Days |
In vivo Pharmacokinetic Study
To determine the repair efficacy for wound healing in vivo, the Tβ-4 ethosomal gel, Tβ-4 gel and blank gel preparation were given to the scalded skin of Kunming rats every day. As shown in Figure 5A and Table 2, the Tβ-4 EP gel group revealed a superior therapeutic effect. The healing time of the scalded skin administered with the Tβ-4 ethosomal gel was significantly shorter than that administered with the Tβ-4 gel. The scar time of the Tβ-4 gel group was also shorter than that of the blank gel group, and the retention rate was small, confirming that Tβ-4 had a wound repair effect. The healing time of the Tβ-4 ethosomal gel group was shorter than that of the Tβ-4 gel group, and the retention rate was smaller.
 |
Table 2 Time of Wound Healing, Time of Forming Scab and the Percentage of the Scar on the Healing Wound After Administering Different Pharmaceutical Preparations |
Histopathology Examination
Combined with the previous research results, we speculated that the nanodelivery drug system could make more drug pass through the skin stratum corneum and form drug depots in the deep layer, thus effectively promoting the effect of wound healing. Photographs of hematoxylin and eosin staining for repaired skin administered with different formulations are illustrated in Figure 5B. As indicated by the black arrow, the damaged skin showed a degree of thickening, but the blank control group was not obvious. As indicated by the red arrow, new capillaries were seen in groups of the Tβ-4 ethosomal gel preparation and Tβ-4 gel, indicating that Tβ-4 has an effect on wound skin. As marked by the yellow arrow, the group of the Tβ-4 gel showed embolization and localized parakeratosis, suggesting that the ethosomes were enhanced Tβ-4 to promote healing.
Conclusion
Although macromolecular protein drugs have attracted much attention due to their high biological activity, they have low skin permeability and easily cause skin irritation in TDDSs because of their large molecular weight and easy inactivation. We hypothesized that nanotechnology-mediated TDDSs can provide some help. Thus, in this study, we successfully prepared ethosomes packaging Tβ-4 that were used for wound repair as a model protein peptide drug. The preparation of the ethosomes without ultrasonic disruption or liposome extrusion was simple. The ethosomes showed good physical and chemical properties, such as a uniform particle size and complete morphology. We have demonstrated their transdermal release rate in vitro and drug effects in vivo through a series of experiments. Based on the experimental results, we observed that the ethosomal gel formulation has a better drug transdermal rate than the free drug group and significantly shortens the time of wound skin healing. Skin irritation experiments further determined that the ethosomal gel has excellent biocompatibility. HE staining showed that the ethosomal gel preparation with loaded drug can promote skin wound healing.
Combining the above results, we conclude that this nano drug delivery system for the transdermal administration of macromolecular protein drugs has excellent clinical application potential and provides a possible good design for ethosomal gels with various transdermal delivery drugs (e.g., Chinese medicine, vaccines, and cytokines) for further exploration.
Ethics Approval and Informed Consent
School of Pharmaceutical Science, Shandong University ethics committee has approved the animal model experiments.
Acknowledgments
This work was supported by the Fundamental Research Funds of Shandong University (No. 2018JC006), the National Natural Science Foundation of China (No. 21873057), Shandong Provincial Natural Science Foundation of China (No. ZR2019MB041), and the Major Basic Research Project of Shandong Natural Science Foundation, P.R. China (No. ZR2018ZC0232).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Crockford D, Turjman N, Allan C, Angel J. Thymosin beta4: structure, function, and biological properties supporting current and future clinical applications. Ann N Y Acad Sci. 2010;1194:179–189. doi:10.1111/j.1749-6632.2010.05492.x
2. Paudel KS, Milewski M, Swadley CL, Brogden NK, Ghosh P, Stinchcomb AL. Challenges and opportunities in dermal/transdermal delivery. Ther Deliv. 2010;1(1):109–131. doi:10.4155/tde.10.16
3. Alexander A, Dwivedi S, Ajazuddin A, et al. Approaches for breaking the barriers of drug permeation through transdermal drug delivery. J Control Release. 2012;164(1):26–40. doi:10.1016/j.jconrel.2012.09.017
4. Rac V, Lević S, Balanč B, Olalde Graells B, Bijelić G. PVA cryogel as model hydrogel for iontophoretic transdermal drug delivery investigations. Comparison with PAA/PVA and PAA/PVP interpenetrating networks. Colloids Surf B Biointerfaces. 2019;180:441–448. doi:10.1016/j.colsurfb.2019.05.017
5. Donnelly RF, Larraňeta E. Slowly dissolving intradermal microneedles. Nat Biomed Eng. 2019;3(3):169–170. doi:10.1038/s41551-019-0369-4
6. Li N, Quan P, Wan X, Liu C, Liu X, Fang L. Mechanistic insights of the enhancement effect of sorbitan monooleate on olanzapine transdermal patch both in release and percutaneous absorption processes. Eur J Pharm Sci. 2017;107:138–147. doi:10.1016/j.ejps.2017.07.006
7. Anirudhan TS, Nair AS, Bino SJ. Nanoparticle assisted solvent selective transdermal combination therapy of curcumin and 5-flurouracil for efficient cancer treatment. Carbohydr Polym. 2017;173:131–142. doi:10.1016/j.carbpol.2017.05.045
8. Ashtikar M, Nagarsekar K, Fahr A. Transdermal delivery from liposomal formulations - evolution of the technology over the last three decades. J Control Release. 2016;242:126–140. doi:10.1016/j.jconrel.2016.09.008
9. Yang L, Wu L, Wu D, Shi D, Wang T, Zhu X. Mechanism of transdermal permeation promotion of lipophilic drugs by ethosomes. Int J Nanomedicine. 2017;12:3357–3364. doi:10.2147/IJN
10. Mbah CC, Builders PF, Attama AA. Nanovesicular carriers as alternative drug delivery systems: ethosomes in focus. Expert Opin Drug Deliv. 2014;11(1):45–59. doi:10.1517/17425247.2013.860130
11. Wang W, Song T, Wan X, Liu C, Zhao H, Fang L. Investigate the control release effect of ion-pair in the development of escitalopram transdermal patch using FT-IR spectroscopy, molecular modeling and thermal analysis. Int J Pharm. 2017;529(1–2):391–400. doi:10.1016/j.ijpharm.2017.06.089
12. Fang YP, Tsai YH, Wu PC, Huang YB. Comparison of 5-aminolevulinic acid-encapsulated liposome versus ethosome for skin delivery for photodynamic therapy. Int J Pharm. 2008;356(1–2):144–152. doi:10.1016/j.ijpharm.2008.01.020
13. Song H, Wen J, Li H, et al. Enhanced transdermal permeability and drug deposition of rheumatoid arthritis via sinomenine hydrochloride-loaded antioxidant surface transethosome. Int J Nanomedicine. 2019;14:3177–3188. doi:10.2147/IJN.S188842
14. Zhang Z, Wo Y, Zhang Y, et al. In vitro study of ethosome penetration in human skin and hypertrophic scar tissue. Nanomedicine. 2012;8(6):1026–1033. doi:10.1016/j.nano.2011.10.006
15. Malik A, Gupta M, Mani R, Bhatnagar R. Single-dose Ag85B-ESAT6-loaded poly(lactic–glycolic acid) nanoparticles confer protective immunity against tuberculosis. Int J Nanomedicine. 2019;14:3129–3143. doi:10.2147/IJN.S172391
16. Gu Z, Wang Q, Shi Y, et al. Nanotechnology-mediated immunochemotherapy combined with docetaxel and PD-L1 antibody increase therapeutic effects and decrease systemic toxicity. J Control Release. 2018;286:369–380. doi:10.1016/j.jconrel.2018.08.011
17. Baswan SM, Leverett J, Pawelek J. Clinical evaluation of the lightening effect of cytidine on hyperpigmented skin. J Cosmet Dermatol. 2019;18(1):278–285. doi:10.1111/jocd.12784
18. Baswan SM, Yim S, Leverett J, Pawelek J. LB1591 in-vitro and in-vivo evaluation of skin lightening efficacy of cytidine. J Investig Dermatol. 2018;138(9):B21. doi:10.1016/j.jid.2018.06.130
19. Baswan SM, Li SK, LaCount TD, Kasting GB. Size and charge dependence of ion transport in human nail plate. J Pharm Sci. 2016;105(3):1201–1208. doi:10.1016/j.xphs.2015.12.011
20. Baswan SM, Li SK, Kasting GB. Diffusion of uncharged solutes through human nail plate. Pharm Dev Technol. 2016;21(2):255–260. doi:10.3109/10837450.2014.991876
21. Baswan SM Transport of charged and uncharged solutes in hydrated human nail plate [Electronic Thesis or Dissertation].University of Cincinnati; 2014:243.
22. Liu C, Quan P, Li S, Zhao Y, Fang L. A systemic evaluation of drug in acrylic pressure sensitive adhesive patch in vitro and in vivo: the roles of intermolecular interaction and adhesive mobility variation in drug controlled release. J Control Release. 2017;252:83–94. doi:10.1016/j.jconrel.2017.03.003
23. Chen X, Peng LH, Shan YH, et al. Astragaloside IV-loaded nanoparticle-enriched hydrogel induces wound healing and anti-scar activity through topical delivery. Int J Pharm. 2013;447(1–2):171–181. doi:10.1016/j.ijpharm.2013.02.054
24. Perini JA, Angeli-Gamba T, Alessandra-Perini J, Ferreira LC, Nasciutti LE, Machado DE. Topical application of acheflan on rat skin injury accelerates wound healing: a histopathological, immunohistochemical and biochemical study. BMC Complement Altern Med. 2015;15:203. doi:10.1186/s12906-015-0745-x
25. Liu X, Liu H, Liu J, et al. Preparation of a ligustrazine ethosome patch and its evaluation in vitro and in vivo. Int J Nanomedicine. 2011;6:241–247. doi:10.2147/IJN.S16044
26. Song CK, Balakrishnan P, Shim CK, Chung SJ, Chong S, Kim DD. A novel vesicular carrier, transethosome, for enhanced skin delivery of voriconazole: characterization and in vitro/in vivo evaluation. Colloids Surf B Biointerfaces. 2012;92:299–304. doi:10.1016/j.colsurfb.2011.12.004
27. Malik A, Gupta M, Mani R, Gogoi H, Bhatnagar R. Trimethyl chitosan nanoparticles encapsulated protective antigen protects the mice against anthrax. Front Immunol. 2018;9:562. doi:10.3389/fimmu.2018.00562
28. An K, Sun Y, Wu Y, Yuan H, Cui Z, Xu L. Preparation and in vitro percutaneous penetration of simvastatin ethosome gel. Artif Cells Nanomed Biotechnol. 2013;41(5):315–318. doi:10.3109/10731199.2012.743903
29. Zhang YT, Shen LN, Wu ZH, Zhao JH, Feng NP. Comparison of ethosomes and liposomes for skin delivery of psoralen for psoriasis therapy. Int J Pharm. 2014;471(1–2):449–452. doi:10.1016/j.ijpharm.2014.06.001
30. Ishihara T, Yamashita H, Sakurai T, et al. Morphological analysis of patchy thickening and reddish discoloration of active hair growth areas in the skin of New Zealand white rabbits. J Toxicol Pathol. 2017;30(4):315–322. doi:10.1293/tox.2017-0033
31. Singh SK. Impact of product-related factors on immunogenicity of biotherapeutics. J Pharm Sci. 2011;100(2):354–387. doi:10.1002/jps.22276
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.