Back to Journals » Patient Preference and Adherence » Volume 8
Electronically monitored medication adherence predicts hospitalization in heart failure patients
Received 15 September 2013
Accepted for publication 9 October 2013
Published 5 December 2013 Volume 2014:8 Pages 1—13
DOI https://doi.org/10.2147/PPA.S54520
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Barbara Riegel,1,2 George J Knafl3
1University of Pennsylvania School of Nursing, 2University of Pennsylvania Leonard Davis Institute, Philadelphia, PA, USA; 3University of North Carolina School of Nursing, Chapel Hill, NC, USA
Background: Hospitalization contributes enormously to health care costs associated with heart failure. Many investigators have attempted to predict hospitalization in these patients. None of these models has been highly effective in prediction, suggesting that important risk factors remain unidentified.
Purpose: To assess prospectively collected medication adherence, objectively measured by the Medication Event Monitoring System, as a predictor of hospitalization in heart failure patients.
Materials and methods: We used recently developed adaptive modeling methods to describe patterns of medication adherence in a sample of heart failure patients, and tested the hypothesis that poor medication adherence as determined by adaptive methods was a significant predictor of hospitalization within 6 months.
Results: Medication adherence was the best predictor of hospitalization. Besides two dimensions of poor adherence (adherence pattern type and low percentage of prescribed doses taken), four other single factors predicted hospitalization: low hemoglobin, depressed ejection fraction, New York Heart Association class IV, and 12 or more medications taken daily. Seven interactions increased the predictive capability of the model: 1) pattern of poor adherence type and lower score on the Letter–Number Sequencing test, a measure of short-term memory; 2) higher number of comorbid conditions and higher number of daily medications; 3) higher blood urea nitrogen and lower percentage of prescribed doses taken; 4) lower hemoglobin and much worse perceived health compared to last year; 5) older age and lower score on the Telephone Interview of Cognitive Status; 6) higher body mass index and lower hemoglobin; and 7) lower ejection fraction and higher fatigue. Patients with none of these seven interactions had a hospitalization rate of 9.7%. For those with five of these interaction risk factors, 100% were hospitalized. The C-index (the area under the receiver-operating characteristics [ROC] curve) for the model based on the seven interactions was 0.83, indicating excellent discrimination.
Conclusion: Medication adherence adds important new information to the list of variables previously shown to predict hospitalization in adults with heart failure.
Keywords: heart failure, outcomes, hospitalization, patient compliance, medication adherence, self-care
Introduction
Heart failure (HF) is the most prevalent and fastest-growing cardiovascular disease worldwide.1 In the US among those 80 years of age and older, almost 12% of men and women have HF, and the prevalence is projected to increase by 25% by 2030.1 Outcomes associated with HF include poor quality of life, high mortality, and frequent hospitalizations that contribute enormously to health care costs.1
In 2010, the Patient Protection and Affordable Care Act was enacted to address the rising costs of health care in the US.2 In 2012, value-based purchasing was introduced, and hospitals began being financially spurred to produce quality outcomes while reducing inappropriate spending. Specifically, the Centers for Medicare and Medicaid Services Readmissions Reduction Program financially penalizes health care systems when the 30-day all-cause readmission rates for Medicare patients are higher than expected in particular diagnostic categories. HF is one of the targeted diagnoses, so efforts to identify modifiable factors predicting HF hospitalizations are increasingly important.
Numerous investigators have attempted to predict hospitalization in adults with HF. In a recent review, Giamouzis et al2 summarized risk factors for hospitalization as sociodemographic, clinical, blood and other test results, comorbidity burden, and cardiovascular, noncardiovascular, quality of life, psychosocial, and disease-management factors.2 Others have attempted to synthesize these results by developing models that can be used to predict hospitalization risk.3–9 None of these models has been highly effective in prediction. The C-index (the area under the receiver-operating characteristics [ROC] curve) in the various studies ranged from 0.57 to 0.74, suggesting that important risk factors remain unidentified. The purpose of this study was to assess medication adherence as a predictor of hospitalization in adults with HF in conjunction with other possible predictors.
Poor medication adherence is ubiquitous in chronically ill patient populations.10 In a review of medication adherence in HF, Wu et al11 noted that most investigators have found nonadherence rates of 40%–60% of HF patients. Prior studies have demonstrated that disease-management interventions emphasizing evidence-based medications can decrease hospitalization rates,12 but few studies have addressed the risk of hospitalization associated with medication nonadherence in adults with HF. The few studies that have been done suggest that hospitalization rates are higher when medication adherence is poor.13–16 These studies are limited, however, to retrospective analyses of such electronic data as pharmacy records.
In this study, we describe patterns of prospectively collected, objectively measured medication adherence in a sample of HF patients and test the hypothesis that medication adherence is a significant predictor of hospitalization within 6 months. This approach addresses several important gaps in the literature. First, collecting the data prospectively negates the need for decision rules regarding the coding of electronic data. Second, medication adherence was measured objectively with the Medication Event Monitoring System (MEMS®) (Aardex; MW Healthcare, Richmond, VA, USA), which is more accurate than self-reported medication-adherence data. Third, we used a statistical approach17,18 that allowed us to utilize more fully these medication-adherence data to characterize patients’ adherence patterns and to identify adherence types with similar patterns, rather than the usual approach of classifying adherence using an arbitrarily devised cutoff (usually >80%).19 Fourth, while these methods have been used before to model MEMS adherence data for human immunodeficiency virus-positive patients17,20 and for African-American patients with hypertension,21 they have not been used before with adherence data from HF patients.
Materials and methods
This was a planned analysis of longitudinal data from a prospective cohort study of a consecutive sample of 280 adults with HF. Subjects were enrolled from three outpatient settings in the northeastern US. Institutional review board approval was obtained at each site, and all participants gave informed consent. Data were collected between 2007 and 2009. A detailed description of study methods has been published previously.22
Patients with a confirmed diagnosis of chronic HF were enrolled, regardless of etiology or ejection fraction. Inclusion criteria addressed the ability to participate (eg, vision, hearing, English literacy, and cognition).15 Cognition was screened using the Telephone Interview of Cognitive Status (TICS).23 Exclusion criteria were major depressive illness, dementia, renal failure requiring dialysis, or a recent history of serious drug or alcohol abuse.
Participants were followed for 6 months, with study visits at baseline, 3, and 6 months. Data on self-care and cognition were collected at each study visit. Most data were collected during home visits by research assistants. Nurses abstracted clinical information from medical records. For this analysis, we tested a wide range of demographic, social support, clinical, self-care, symptom, and cognition variables, so as to add to the knowledge of significant predictors previously identified by others.2
The outcome variable of hospitalization was measured using the electronic medical record at each participating institution. In addition, participants were telephoned monthly and asked about hospitalizations (and also emergency department visits). Medical records were obtained if the visit took place at a hospital outside of the home institution. In this analysis, all hospitalizations were analyzed, regardless of cause (not including emergency department visits).
Measures
MEMS was used to measure medication adherence objectively. Our methods for collecting MEMS data are described in detail elsewhere;24 the MEMS data were used differently in that study. In brief, using a microprocessor in the cap, the MEMS® 6 device measures openings that are presumed to be for the purpose of removing a pill to take it orally. MEMS data were collected on one medication scheduled to be taken at fixed times. MEMS data were collected over a 6-month interval and downloaded at 3 and 6 months. Deviations in use, such as accidental openings, were noted in study diaries and used to correct the time-stamped medication events stored in the device before analysis. In this study, we considered three aspects of adherence based on MEMS data: adherence-pattern types, consistency of adherence patterns with the prescribed rate, and the percentage of prescribed doses taken (PDT). The medication controlled by MEMS did not change for any of the patients during the study. For one patient, the prescribed rate for the medication controlled by MEMS changed during the study. The adherence pattern for this patient was adjusted to account for this change.
Demographic variables, such as age, race, and sex were collected by self-report. In addition to measuring education as the number of years of formal schooling, the American National Adult Reading Test (ANART) was administered as a test of premorbid intellect.
Social support was measured in multiple ways. Marital status was self-reported, as was living alone (yes/no) and the overall quality of the support received defined as “emotional support, information, material help, errands, etc,” with responses ranging from 1 (poor) to 4 (very good). In addition, support from family, friends, and significant others was assessed using the Multidimensional Scale of Perceived Social Support (MSPSS).25 Responses range from 1 (very strongly disagree) to 7 (very strongly agree), with higher scores indicating higher perceptions of support.
Clinical variables included health-related factors, such as exercise in the last week, which was assessed by self-report with responses of 1 (none) to 4 (more than 3 hours). Body mass index (BMI) was calculated from self-reported height and measured body weight. Variables abstracted from the medical record included months since diagnosed with HF, most recent blood urea nitrogen (BUN), creatinine, hemoglobin (Hgb), serum sodium, and ejection fraction. The Charlson Comorbidity Index26 was completed based on chart review. Any history of sleep apnea, atrial fibrillation, hypertension, diabetes, cerebral disease, renal disease, anemia, or pulmonary hypertension was noted. Pulse and systolic and diastolic blood pressure were measured during the enrollment visit. Treatment quality was rated separately for systolic and diastolic HF, using those treatments advocated in HF clinical guidelines (eg, angiotensin-converting enzyme-inhibitor use, beta-blocker use) in place at the time.27
Self-care was measured with the Self-Care of HF Index (SCHFI), which assesses self-care maintenance, management, and confidence.28 Each scale is standardized to a score of 100, with higher scores indicating better self-care. Knowledge of HF was assessed using the Dutch HF Knowledge Scale29 with 15 dichotomously scored items; higher scores indicate higher knowledge of HF treatment, HF symptoms, and symptom recognition. The number of medications taken daily was calculated based on a review of medication containers by research assistants during home visits.
Symptoms measured by self-report included trouble breathing or ankle swelling in the past month (yes/no), general health perceptions, rated 1 (excellent) to 5 (poor), and health perception compared to 1 year prior, rated 1 (much better now than 1 year ago) to 5 (much worse now than 1 year ago). Information on functional class was gathered during the home visit using a standardized interview. A single cardiologist scored New York Heart Association (NYHA) class in every subject. Fatigue was measured using two items from the Kansas City Cardiomyopathy Questionnaire.30 Each item is scored 1 to 7; scores were reversed so that higher scores indicated more fatigue. Sleepiness was assessed with the Stanford Sleepiness Scale31 and the Epworth Sleepiness Scale (ESS).32 ESS respondents rate the likelihood of falling asleep in eight soporific situations on a scale ranging from 0 (never dozing) to 3 (high chance of dozing). ESS scores are summed, with higher scores indicating higher sleepiness or categorized as sleepy (≥11) or not sleepy (<11). Sleep quality was assessed with the Pittsburgh Sleep Quality Index.33 A global score (0–21 points) is obtained by summing the scale domain scores. Higher scores indicate poorer sleep quality; a score >5 is categorized as poor sleep. Depression was measured using the Patient Health Questionnaire.34 Responses range from 0 (not at all) to 3 (nearly every day), with higher scores indicating more depression.
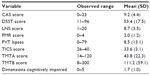
A neuropsychological test battery was administered to measure simple attention (Psychomotor Vigilance Task [PVT]), complex attention (Trail Making Test B), processing speed (Digit Symbol Substitution Test, Trail Making Test A), working memory (Probed Recall Memory task), and short-term memory (Letter–Number Sequencing [LNS] test).35 Transformed lapses >4.69 on the PVT were scored as abnormal.36 Scores on each of the other tests were classified based on age-based norms. In addition, the number of tests scored as abnormal was used as a summary measure of cognitive status. Anyone scoring >1.5 standard deviations on two or more of the cognition tests was scored as having cognitive decline. Efforts made to compensate for perceived memory issues were measured and summarized in the Compensatory Activities Scale.
Data analysis
Other than standard analyses (eg, descriptive statistics), analyses were conducted using the adaptive methods of Knafl et al.17 These methods were used to characterize adherence patterns for individual patients over their 6 months in the study, classify these patterns into adherence types, and identify dichotomous risk factors, individually and in combination, for hospitalization.
Likelihood cross-validation
Adaptive methods use a K-fold likelihood cross-validation (LCV) approach for evaluating and comparing alternative models. Observations (eg, daily MEMS use) are randomly partitioned into K disjoint subsets called folds. For a given model, the likelihood for the data in each fold is computed from model parameter values estimated using the data in the other folds. These deleted fold likelihoods are normalized by the sample size and multiplied up into the LCV score for the model. Larger LCV scores indicate better models for the data under analysis. LCV scores can be used for model selection in any analysis context where parameter estimation is based on maximizing a likelihood or any likelihood-like function (eg, a quasi-likelihood). All analyses used 10-fold LCV scores.
A larger LCV score does not necessarily mean the model is preferable. If the smaller LCV score is not too much smaller and the associated model has a simpler structure (eg, using an untransformed predictor compared to using the log transform of that predictor), then this model is preferable as a parsimonious, competitive alternative. LCV-ratio tests, analogous to likelihood-ratio tests, can be used to assess whether a smaller LCV score is substantially (significantly or distinctly) smaller or not. These are χ2-based tests and are expressed in terms of a cutoff for a substantial percent decrease in the LCV score. The cutoff changes with the sample size (for the formula, see [6] of Knafl et al17).
Individual adherence patterns
The study-participation period for each patient was subdivided into equally sized intervals of length at least 3 days with no more than 100 intervals. Counts of MEMS cap openings and opening rates per day per dose were computed for each interval. These counts and rates were modeled using Poisson regression models (as is appropriate for such data). Both mean adherence and adherence variability based on dispersion parameters37 were modeled as possibly nonlinear functions of time during study participation. LCV scores were based on extended quasi-likelihoods.
The predictors for the Poisson regression models were power transforms of time with possibly fractional (ie, noninteger) powers, and so these are called fractional polynomial models.38 An adaptive process was used to identify an effective set of such power transforms. The adaptive process starts from the constant model and systematically expands the model, adding in power transforms of time to either the mean adherence or dispersion component of the model, continuing as long as the LCV score does not decrease by too much (as determined by an expansion-stopping tolerance parameter). The expanded model is then contracted by removing transforms of time or possibly the intercept term as long as the LCV score does not decrease by too much (as determined by a contraction-stopping tolerance parameter). The transforms of the contracted model determine the adherence pattern underlying the data for how both mean adherence and adherence variability change over time (examples are given in Figure 1, as described in the “Results” section).
Since the prescribed rates were not the same for all patients (ranging from one to three doses per day), adherence patterns were normalized by the prescribed number of doses to be comparable. The ideal adherence pattern is then the one with constant mean adherence equal to 1 and constant adherence variability equal to 0. A summary measure of how consistent the observed adherence pattern is with this ideal pattern is calculated for each patient as a percentage, and so is called percentage consistency.
Adherence types
Mean adherence and adherence variability were estimated at 20 proportionally spaced times within each patient’s study participation period (5%, 10%, … 100%). The 40 vectors formed from these two types of estimates were clustered into adherence types, ie, sets of patients with similar mean adherence and adherence variability over time. A wide variety of clustering procedures with varying numbers of clusters were considered.17 These were compared using LCV scores based on likelihoods for multivariate normal-mixture models (as is appropriate for cluster analyses). The selected clustering alternative was the one generating the best score among those with at least 5% of the patients in each cluster (to avoid sparse clusters). Plots of averages of mean adherence and adherence variability (ie, the centroids) were used in interpreting the clusters (see Figure 2, as described in the “Results” section).
  | Figure 2 Plots of average mean adherence and of average adherence variability for patients in adherence types. |
Identifying risk factors for hospitalization
Potential dichotomous risk factors were identified for the dichotomous hospitalization-outcome variable. Most categorical predictors with more than two values were reduced to dichotomous predictors expected to be risk factors. For example, income level was reduced to not enough as the risk factor versus enough or more than enough. Otherwise, categorical predictors were represented by multiple dichotomous risk factors. For example, employment status was represented by being retired versus not and being unemployed or disabled versus not. For each continuous and ordinal predictor, its observed values were adaptively grouped into two subsets of contiguous values. For each observed value of the predictor (or a rounded value to reduce the number of decimal digits) as a cutoff, LCV scores were computed for the model based on the indicator for having values above or below the cutoff. When a variable had missing values, these were conservatively grouped with the non-risk-factor values so that the effect of the associated risk factor held only for patients with nonmissing values for the underlying variable. The cutoff generating the best LCV score was chosen and the risk factor defined in terms of values either above or below the cutoff, depending on which of these choices had a positive effect on the outcome variable, ie, with odds ratio >1. To avoid sparse cases, only those cutoffs were considered for which at least 5% of the observations fell both above and below the cutoff. When a standard cutoff existed for a predictor (eg, PVT >4.69), that categorization was considered as well.
To be consistent with the handling of other predictors, adherence type was adaptively reduced to a dichotomous risk factor of poor-adherence types versus better-adherence types. Models of hospitalization were used for this purpose. The decision regarding which adherence types to assign to the two alternatives was made adaptively using LCV scores. In contrast to the handling of values for continuous and ordinal predictors, the alternate adherence types were not considered to be ordered.
Data for patients with at least some MEMS data were used to model hospitalization in terms of adherence and other available risk factors, and so data for patients with no MEMS data were missing for these analyses. Only outcome means were adaptively modeled and not outcome dispersions, using unit dispersions for all models (as for standard logistic regression modeling). Bivariate models were generated for all potential risk factors. Then, a multiple risk-factor model was generated considering only the risk factors with a significant (P<0.05) bivariate effect. The adaptive modeling process, as used for generating individual patient adherence patterns in terms of the single predictor of time, was used for this purpose. This multiple risk-factor model provides a parsimonious depiction of the combination of risk factors that affect hospitalization. Next, interactions between the poor-adherence type risk factor with each of the other available risk factors were considered by starting with the model based on these two risk factors and their interaction and adaptively reducing that model to identify cases when an interaction term remained in the model. A multiple risk-factor model was generated considering these identified interaction effects along with the noninteraction risk factors with significant individual effects. Finally, an adaptive model was generated considering this same set of risk factors as well as possible interactions between any two of them to obtain a fuller assessment of interactions between risk factors.
Results
Sample
A total of 280 HF patients participated in the study. Summary statistics are presented in Tables 1–6 for available variables within the six categories described earlier. For example, patients were primarily male (64.3%), white (62.5%), and retired (43.9%). Ages ranged from 24 to 89 years with a mean of 62.0 (standard deviation =12.5) years, while education ranged from 8 to 29 years with mean of 13.9 (standard deviation =2.9) years. Over the course of the 6-month study, 103 (36.8%) of the patients were hospitalized.
  | Table 2 Summary statistics for available social support variables |
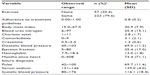  | Table 3 Summary statistics for available clinical variables |
Individual patient adherence patterns
MEMS adherence data were available for 218 (77.9%) patients. Of these patients, 79 (36.2%) were hospitalized during the study. Hospitalization rates were not significantly different for patients with no MEMS data versus some MEMS data (χ2[1]=0.13, P=0.722).
Figure 1 contains plots of adherence patterns for seven exemplar patients. The y-axis of these plots is openings per day per dose with an ideal value of 1, while the x-axis is cumulative days of study participation. The raw data are plotted as diamonds. The middle curve is the estimated mean adherence over time, while the other curves are unit error bands, ±1 estimated standard deviation (as extended to account for nonlinear dispersion) around mean adherence.
Patient 1 had mean adherence close to the prescribed rate with small variability, which was 93.4% consistent with adherence at the prescribed rate. Patient 2’s mean adherence was close to the prescribed rate, with small variability up to about 120 days of study participation. After that, mean adherence decreased somewhat with increased variability for 79.9% consistency with the prescribed rate. Patient 3 had deteriorating mean adherence from about the prescribed rate to around half the prescribed rate, with low variability and 61.7% consistency. Patient 4’s mean adherence was close to the prescribed rate, with small variability up to about 150 days of study participation, after which adherence dropped to essentially zero for 40.0% consistency. Patient 5 had relatively consistent mean adherence at around half the prescribed rate, with moderate variability and 15.5% consistency. Patient 6’s mean adherence started at about the prescribed rate and decreased to zero by about 90 days of study participation, with variability decreasing for a while and then increasing. After that, adherence remained at zero. This pattern was only 1.0% consistent with prescribed adherence. In contrast, the PDT for this patient was 48.9%, suggesting that the patient was adherent at around half the prescribed rate. The plot indicates that patient 6 was adherent around the prescribed rate for about half the time and zero adherent the rest of the time, resulting in a percentage PDT close to 50%, but never around 50% at any time. In cases like this, percentage PDT provides a misleading assessment of adherence, since it is based on an assumption of constant adherence over time. Patient 7 had mean adherence starting around half the prescribed rate and deteriorating quickly to nearly zero, with low variability and 0.1% consistency.
Adherence types
Cluster analysis identified seven adherence types. Figure 2 contains plots of averages of mean adherence and of adherence variability for patients in the seven clusters. These plots were used to generate the interpretations of the adherence types given in Table 7. The clusters were numbered so that averages of percentage consistency and percentage PDT decreased. Consequently, cluster 1 corresponded to the best adherence type, with mean adherence consistently very close to the prescribed rate and adherence variability consistently low. Cluster 7 corresponded to the worst adherence type, with mean adherence starting at about half the prescribed rate and moderate adherence variability, then deteriorating quickly to low, not too much above zero mean adherence and adherence variability. The adherence patterns of patients 1–7 were allocated to clusters 1–7, respectively. The individual patterns of Figure 1 are only similar to the associated plots of Figure 2 since these latter plots are based on averages.
  | Table 7 Description of adherence types. |
Risk factors for hospitalization
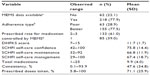
The adaptively generated dichotomous risk factor based on the seven adherence types for predicting hospitalization was the poor-adherence type, consisting of clusters 4, 6, and 7, versus better adherence, consisting of clusters 1–3 and 5. Table 8 presents results for characterizing hospitalization, considering the variables of Tables 1–6. Individual risk-factor analyses identified 21 significant (P<0.05) risk factors for hospitalization: two demographic, zero social support, seven clinical, five self-care, six symptom, and one cognition. The cutoff for a substantial percentage decrease in LCV scores for a sample of size 218 is 0.68%. The percentage decrease exceeded this cutoff for 16 (76.2%) of the 21 variables (LCV scores not reported), indicating that LCV ratio tests are more conservative than tests for zero coefficients, and so are similar to multiple-comparison approaches. All standard classifications except the one for BUN were nonsignificant, but this was equivalent to the adaptive BUN classification.
Results for the adaptive multiple risk-factor model generated considering the 21 significant risk factors of Table 8 are reported in Table 9. This model had five risk factors: lower Hgb, lower ejection fraction, poor adherence type, higher total number of prescribed medications, and NYHA class IV. The model had two clinical, two self-care, and one symptom risk factors, and no demographic, social support, or cognition risk factors. The LCV score was 0.56979. In contrast, the best individual risk-factor model based on poor MEMS adherence had an LCV score of 0.53527, with substantial percentage decrease of 6.06%, indicating that the multiple risk-factor model substantially improved on each of the individual risk-factor models.
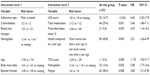
Interactions with poor-adherence type were identified for three risk factors: poor-adherence type with lower ANART score (≤34, 32 [14.7%] patients), with higher MSPSS score (≥54, 59 [27.1%] patients), and with lower LNS score (≤8, 41 [18.8%] patients). The percentage decrease in LCV score for the model based on the poor-adherence type was insubstantial at 0.35% for the second of these interactions (with MSPSS score), but was substantial at 1.35% for the first and at 1.68% for the third.
The adaptive multiple risk-factor model generated considering these three interactions and the 21 significant risk factors of Table 8 included the single interaction between the poor-adherence type and lower LNS score. It also included the same four nonadherence risk factors from the noninteraction model of Table 9. The LCV score was 0.58318, which was a substantial improvement on the noninteraction multiple risk-factor model with percentage decrease in the LCV score of 2.30%.
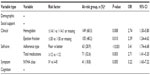
The adaptive model considering pair-wise interactions is described in Table 10 and included seven interactions (and no noninteraction risk factors):
- poor-adherence type and lower LNS score
- higher number of comorbid conditions and higher number of medications
- higher BUN and lower percentage PDT
- lower Hgb and much worse perceived health now compared to last year
- older age and lower TICS score
- higher BMI and lower Hgb
- lower ejection fraction and higher fatigue.
The C-index for this model was 0.83 (values between 0.8 to 0.9 are considered to provide excellent discrimination39).
To assess the possibility of collinearity between these seven interactions, we computed logistic regression models predicting each of these seven interactions as a function of the other six. The largest Nagelkerke R2 value for these models was 9.5%, indicating that collinearity was not a problem for the seven-interaction model.
Patients had zero to five of these risk factors. Of the 62, 63, 59, 19, eleven, and four patients with zero to five of these interaction risk factors, respectively, the percentage hospitalized was 9.7%, 19.1%, 54.2%, 79.0%, 90.9%, and 100%. The hospitalization risk index model based on the count of the number of these risk factors as the only predictor of hospitalization had an LCV score of 0.61594, which provided a substantial improvement over the seven-interaction model, with percentage decrease in the LCV score of 1.18%. This model has a C-index of 0.82. As an example, using a cutoff of 0.5 for generating predictions (ie, predictions based on maximum likelihood), the sensitivity is 77.2% and the specificity 77.0%, and so well balanced.
Discussion
In this prospective study, we confirmed that both a poor type of medication adherence pattern and a low percentage of prescribed doses taken were important predictors of hospitalization in adults with HF. In addition, we identified low Hgb, depressed ejection fraction, NYHA class IV, and taking 12 or more medications daily as risk factors for hospitalization. When interactions were considered, seven combinations of factors increased the predictive capability of the model: 1) poor-adherence type and lower score on a test of short-term memory, 2) higher number of comorbid conditions and higher number of daily medications, 3) poor kidney function (higher BUN) and lower percentage prescribed doses taken, 4) lower Hgb and perceptions of poor health, 5) older age and lower score on the TICS, 6) higher BMI and lower Hgb, and 7) lower ejection fraction and higher fatigue. Patients with none of these seven interactions were unlikely to be hospitalized, but all of those with five of the seven interaction risk factors were hospitalized over the 6-month period.
A pattern of poor medication adherence and taking a low percentage of prescribed doses were both associated with hospitalization in this sample. These results are consistent with prior research,13,14,40,41 but those studies measured adherence using administrative claims data or retrospective review of hospital records, so the pattern of adherence and the percentage of doses taken could only be inferred. What this study adds is the prospective analysis of individual patterns of medication-taking behavior in relation to hospitalization.
An important factor interacting with a poor medication-adherence type was impaired cognition. Cognitive deficits occur in a significant proportion of adults with chronic HF,42 including deficits in memory.43 Prospective memory has been demonstrated to be related to medication adherence.44 Although short-term memory as measured by the LNS and prospective memory are related, prospective memory is more encompassing, referring specifically to the ability to remember to do something in the future.44 As taking medication on a schedule requires that patients remember to do so, this result suggests that HF patients who have not compensated for poor memory with a strategy to assist them to remember medications are at increased risk of hospitalization. One physiologic factor known to be associated with impaired cognition is poor kidney function.45 In this study, higher BUN levels interacted with taking a lower percentage of prescribed medication doses to predict hospitalization. A memory device to facilitate adherence may be particularly important in HF patients with impaired kidney function.
We found that patients taking multiple daily medications were likely to be hospitalized, perhaps because they were not taking their medications as prescribed.46 This was especially true in patients with more comorbid illnesses, where the number of medications and comorbid illnesses interacted to predict hospitalizations. This result is not surprising, considering the profile of those individuals with multiple chronic conditions who are taking numerous medications. Illness symptoms and medication side effects can be expected to make routine medication adherence challenging.47
Low Hgb, low ejection fraction, and poor functional status all predicted hospitalization. Previous investigators have identified a wide variety of clinical factors associated with hospitalization, including anemia.48 Although correction of anemia has been shown to slow the progression of HF and reduce hospitalization rates,49 more than one-third of the participants in our study were anemic using the World Health Organization definitions of <13% for men and <12% for women. Correction of anemia with subcutaneous erythropoietin is advocated in clinical guidelines and covered in the US by Medicare,50 but expense still may be limiting its widespread use. Low Hgb interacted with self-reported perceptions of poor health, suggesting that those patients who were anemic were symptomatic enough to label themselves as getting worse over time. Low Hgb also interacted with high BMI, as might be expected for two conditions that cause high output failure. Depressed ejection fraction and poor NYHA functional class were both independently associated with hospitalization, as has been shown by other investigators.2
Limitations of this study include the relatively small sample size, compared to epidemiologic studies conducted with thousands of respondents, collected from a single region in the US. Participants were younger and better educated than other community samples. Strengths include the prospective design, the objective measurement of medication adherence, and the sophisticated statistical approach that accounted for general nonlinear adherence trajectories rather than simply categorizing adherence using the >80% cutoff in percentage PDT used by most prior investigators. This nuanced approach to understanding medication-adherence patterns provides important insights into patient behavior that cannot be discerned from epidemiologic research.
Future research is needed to identify predictors of nonadherence. The World Health Organization adherence model suggests that socioeconomic, condition, therapy, patient, and health care-system dimensions contribute to nonadherence,51 and further research is needed to explore these dimensions. Efforts to identify the strategies used by HF patients to remember medications is needed. Finally, it will be important to include cost in future studies, because Sokol et al40 demonstrated that although nonadherence was associated with higher hospitalization risk in HF patients, there were no differences in costs compared to those who were more adherent.
Acknowledgments
This work was funded by a grant from the National Heart, Lung and Blood Institute (R01 HL084394-01A1) and by the Philadelphia Veterans Affairs Medical Center, VISN 4 Mental Illness Research, Education, and Clinical Center (MIREC). The authors gratefully acknowledge Megan Patey, RN, BSN for her assistance with preparation of the data for analysis.
Disclosure
The authors report no conflicts of interest in this work.
References
Heidenreich PA, Albert NM, Allen LA, et al. Forecasting the Impact of Heart Failure in the United States: a policy statement From the American Heart Association. Circ Heart Failure. 2013;6(3):606–619. | |
Giamouzis G, Kalogeropoulos A, Georgiopoulou V, et al. Hospitalization epidemic in patients with heart failure: risk factors, risk prediction, knowledge gaps, and future directions. J Card Fail. 2011;17(1):54–75. | |
Philbin EF, DiSalvo TG. Prediction of hospital readmission for heart failure: development of a simple risk score based on administrative data. J Am Coll Cardiol. 1999;33(6):1560–1566. | |
Krumholz HM, Chen YT, Wang Y, Vaccarino V, Radford MJ, Horwitz RI. Predictors of readmission among elderly survivors of admission with heart failure. Am Heart J. 2000;139(1 Pt 1):72–77. | |
Felker GM, Leimberger JD, Califf RM, et al. Risk stratification after hospitalization for decompensated heart failure. J Card Fail. 2004; 10(6):460–466. | |
Pocock SJ, Wang D, Pfeffer MA, et al. Predictors of mortality and morbidity in patients with chronic heart failure. Eur Heart J. 2006; 27(1):65–75. | |
Yamokoski LM, Hasselblad V, Moser DK, et al. Prediction of rehospitalization and death in severe heart failure by physicians and nurses of the ESCAPE trial. J Card Fail. 2007;13(1):8–13. | |
Keenan PS, Normand SL, Lin Z, et al. An administrative claims measure suitable for profiling hospital performance on the basis of 30-day all-cause readmission rates among patients with heart failure. Circ Cardiovasc Qual Outcomes. 2008;1(1):29–37. | |
Au AG, McAlister FA, Bakal JA, Ezekowitz J, Kaul P, van Walraven C. Predicting the risk of unplanned readmission or death within 30 days of discharge after a heart failure hospitalization. Am Heart J. 2012;164(3):365–372. | |
Coleman CI, Limone B, Sobieraj DM, et al. Dosing frequency and medication adherence in chronic disease. J Manage Care Pharm. 2012;18(7):527–539. | |
Wu JR, Moser DK, Lennie TA, Burkhart PV. Medication adherence in patients who have heart failure: a review of the literature. Nurs Clin North Am. 2008;43(1):133–153; vii–viii. | |
Correia J, Silva FF, Roque C, Vieira H, Providencia LA. Impact of a specialized outpatient heart failure follow-up program on hospitalization frequency and functional status of patients with advanced heart failure. Rev Port Cardiol. 2007;26(4):335–343. | |
Esposito D, Bagchi AD, Verdier JM, Bencio DS, Kim MS. Medicaid beneficiaries with congestive heart failure: association of medication adherence with healthcare use and costs. Am J Manag Care. 2009; 15(7):437–445. | |
Fitzgerald AA, Powers JD, Ho PM, et al. Impact of medication nonadherence on hospitalizations and mortality in heart failure. J Card Fail. 2011;17(8):664–669. | |
Ambardekar AV, Fonarow GC, Hernandez AF, Pan W, Yancy CW, Krantz MJ. Characteristics and in-hospital outcomes for nonadherent patients with heart failure: findings from Get With The Guidelines – Heart Failure (GWTG-HF). Am Heart J. 2009;158(4):644–652. | |
Cole JA, Norman H, Weatherby LB, Walker AM. Drug copayment and adherence in chronic heart failure: effect on cost and outcomes. Pharmacotherapy. 2006;26(8):1157–1164. | |
Knafl GJ, Delucchi KL, Bova CA, Fennie KP, Ding K, Williams AB. A systematic approach for analyzing electronically monitored adherence data. In: Ekwall B, Cronquist M, editors. Micro Electro Mechanical Systems (MEMS) Technology, Fabrication Processes and Applications. Hauppauge (NY): Nova Science; 2010:1–66. | |
Knafl GJ, Fennie KP, Bova C, Dieckhaus K, Williams AB. Electronic monitoring device event modelling on an individual-subject basis using adaptive Poisson regression. Stat Med. 2004;23(5):783–801. | |
Wu JR, Moser DK, De Jong MJ, et al. Defining an evidence-based cutpoint for medication adherence in heart failure. Am Heart J. 2009;157(2):285–291. | |
Bova C, Fennie KP, Dieckhaus K, Knafl GJ, Watrous E, Williams AB. Use of electronic monitoring devices to measure antiretroviral adherence: practical considerations. AIDS Behav. 2005;9(1):103–110. | |
Knafl GJ, Schoenthaler A, Ogedegbe G. Secondary analysis of electronically monitored medication adherence data for a cohort of hypertensive African-Americans. Patient Prefer Adherence. 2012;6:207–219. | |
Riegel B, Moelter ST, Ratcliffe SJ, et al. Excessive daytime sleepiness is associated with poor medication adherence in adults with heart failure. J Card Fail. 2011;17(4):340–348. | |
Buckwalter JG, Crooks VC, Petitti DB. A preliminary psychometric analysis of a computer-assisted administration of the Telephone Interview of Cognitive Status – modified. J Clin Exp Neuropsychol. 2002;24(2):168–175. | |
Riegel B, Lee CS, Ratcliffe SJ, et al. Predictors of objectively measured medication nonadherence in adults with heart failure. Circ Heart Fail. 2012;5(4):430–436. | |
Zimet GD, Dahlem NW, Zimet SG, Farley GK. Multidimensional scale of perceived social support. In: Fischer J, Corcoran, K, editors. Measures for Clinical Practice: A Sourcebook. Volume 2 – Adults. 2nd ed. New York: Free Press; 1994. | |
Charlson M, Pompei P, Ales K, MacKenzie C. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–383. | |
Heart Failure Society of America. HFSA 2006 Comprehensive Heart Failure Practice Guideline. J Card Fail. 2006;12(1):e1–e2. | |
Riegel B, Lee CS, Dickson VV, Carlson B. An update on the self-care of heart failure index. J Cardiovasc Nurs. 2009;24(6):485–497. | |
van der Wal MH, Jaarsma T, Moser DK, van Veldhuisen DJ. Development and testing of the Dutch Heart Failure Knowledge Scale. Eur J Cardiovasc Nurs. 2005;4(4):273–277. | |
Green CP, Porter CB, Bresnahan DR, Spertus JA. Development and evaluation of the Kansas City Cardiomyopathy Questionnaire: a new health status measure for heart failure. J Am Coll Cardiol. 2000;35(5):1245–1255. | |
MacLean AW, Fekken GC, Saskin P, Knowles JB. Psychometric evaluation of the Stanford Sleepiness Scale. J Sleep Res. 1992;1(1):35–39. | |
Johns MW. Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep. 1992;15(4):376–381. | |
Buysse D, Reynolds CF 3rd, Monk TH, Berman SR, Kupfer, DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213. | |
Kroenke K, Spitzer R, Williams J. The PHQ-9: Validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–613. | |
Lezak M, Howieson D, Lorig D. Neuropsychological Assessment. 4th ed. New York: Oxford University Press; 2004. | |
Dinges D, Powell J. Microcomputer analyses of performance on a portable, simple visual RT task during sustained operations. Behav Res Methods Instrum Comput. 1985;17(6):652–655. | |
McCullagh P, Nelder JB. Generalized Linear Models. Boca Raton (FL): Chapman and Hall/CRC; 1999. | |
Royston P, Altman DG. Regression using fractional polynomials of continuous covariates: parsimonious parametric modeling. Appl Stat. 1994;43(3):429–467. | |
Hosmer DW, Lemeshow S. Applied Logistic Regression. 2nd ed. New York: John Wiley & Sons; 2000. | |
Sokol MC, McGuigan KA, Verbrugge RR, Epstein RS. Impact of medication adherence on hospitalization risk and healthcare cost. Med Care. 2005;43(6):521–530. | |
Michalsen A, Konig G, Thimme W. Preventable causative factors leading to hospital admission with decompensated heart failure. Heart. 1998;80(5):437–441. | |
Pressler SJ. Cognitive functioning and chronic heart failure: a review of the literature (2002-July 2007). J Cardiovasc Nurs. 2008;23(3):239–249. | |
Pressler SJ, Subramanian U, Kareken D, et al. Cognitive deficits in chronic heart failure. Nurs Res. 2010;59(2):127–139. | |
Zogg JB, Woods SP, Sauceda JA, Wiebe JS, Simoni JM. The role of prospective memory in medication adherence: a review of an emerging literature. J Behav Med. 2012;35(1):47–62. | |
Hailpern SM, Melamed ML, Cohen HW, Hostetter TH. Moderate chronic kidney disease and cognitive function in adults 20 to 59 years of age: Third National Health and Nutrition Examination Survey (NHANES III). J Am Soc Nephrol. 2007;18(7):2205–2213. | |
Tsai KT, Chen JH, Wen CJ, et al. Medication adherence among geriatric outpatients prescribed multiple medications. Am J Geriatr Pharmacother. 2012;10(1):61–68. | |
Dickson VV, Buck H, Riegel B. Multiple comorbid conditions challenge heart failure self-care by decreasing self-efficacy. Nurs Res. 2013;62(1):2–9. | |
Pitt B. Male gender, diabetes, COPD, anemia, and creatinine clearance <30 mL/min predicted hospitalization after heart failure diagnosis. Ann Intern Med. 2010;152(8):JC4-2, JC4-3. | |
Silverberg DS, Wexler D, Blum M, et al. The correction of anemia in severe resistant heart failure with erythropoietin and intravenous iron prevents the progression of both the heart and the renal failure and markedly reduces hospitalization. Clin Nephrol. 2002;58 Suppl 1:S37–S45. | |
Naci H, de Lissovoy G, Hollenbeak C, et al. Historical clinical and economic consequences of anemia management in patients with end-stage renal disease on dialysis using erythropoietin stimulating agents versus routine blood transfusions: a retrospective cost-effectiveness analysis. J Med Econ. 2012;15(2):293–304. | |
World Health Organization. Adherence to long-term therapies: Evidence for action. Geneva: World Health Organization; 2003. Available from: http://www.who.int/chp/knowledge/publications/adherence_full_report.pdf. Accessed November 22, 2013. |
 © 2013 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2013 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.