Back to Journals » Patient Preference and Adherence » Volume 11
Confidence in correct inhaler technique and its association with treatment adherence and health status among US patients with chronic obstructive pulmonary disease
Authors Amin AN, Ganapathy V, Roughley A, Small M
Received 21 April 2017
Accepted for publication 9 June 2017
Published 12 July 2017 Volume 2017:11 Pages 1205—1212
DOI https://doi.org/10.2147/PPA.S140139
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Johnny Chen
Alpesh N Amin,1 Vaidyanathan Ganapathy,2 Adam Roughley,3 Mark Small3
1Department of Medicine, University of California, Irvine, USA; 2Global Health Economics & Outcomes Research, Sunovion Pharmaceuticals Inc, Marlborough, USA; 3Respiratory Research, Adelphi Real World, Bollington, UK
Background: Improper use of bronchodilators is associated with poor disease control, nonadherence to long-term therapy, and poor clinical outcomes. Our current understanding of factors associated with correct inhaler use and adherence is limited. We measured physician- and patient-reported confidence in device usage and associations with treatment adherence and COPD-related health status.
Methods: This was an analysis of a US observational, point-in-time survey of physicians and patients. Physicians who met study eligibility criteria completed surveys for 5 consecutive, eligible patients who were then invited to respond to questionnaires. We assessed patient demographics, type of prescribed inhaler device(s), device training, COPD severity, comorbidities, physician- and patient self-reported confidence in device usage, treatment adherence, and health status.
Results: Completed questionnaires for 373 patients were provided by 134 physicians. Complete confidence in device usage was observed for 22% and 17% of patients as reported by patients and physicians, respectively. Greater confidence was associated with higher self-reported adherence to inhaler usage. Physicians were more likely than patients to report lower levels of patient confidence in device usage. High physician- and patient-reported confidence were associated with more favorable health status. Predictors of confidence in device usage included fewer comorbidities, no depression, and higher education levels.
Conclusion: Low confidence in inhaler usage was associated with lower adherence and poor COPD-related health status. Choice of inhaler device tailored to patients’ ability to use specific devices and ongoing education to support optimal inhaler usage may improve patient confidence and enhance both adherence and health status.
Keywords: chronic obstructive pulmonary disease, inhaler technique, adherence, health status, patient satisfaction
Introduction
COPD is a progressive condition associated with chronic morbidity, reduced quality of life, and premature mortality.1,2 COPD was the third leading cause of mortality in the USA in 2011,3 and imposes a substantial economic burden with total medical costs estimated at US$50 billion and 60% attributed to direct expenditures.4 Despite the significant morbidity and mortality associated with it, COPD is a treatable condition,5,6 with medical therapies tailored to individual patients based on symptom severity, risk for exacerbations, and response to therapy.7 Traditional management of COPD exacerbation, however, has been reactive instead of proactive.8
Bronchodilators are the mainstay of treatment and have established efficacy for symptom control, reduced risk of complications, and prevention of exacerbations.5–7,9 The effectiveness of inhaler therapies depends on device type,10 patients’ ability to use devices correctly,10,11 device reliability for medication delivery,12,13 and patient adherence with prescribed timing, dosage, and frequency.7,14,15 The most frequently observed types of nonadherence are underuse and improper use of inhaled therapies, with the majority of patients unable to properly use inhalers.16–19
A systematic review of studies directly observing patients’ inhaler use technique reported an overall prevalence of 31% (95% CI: 27%–36%) for poor technique, 41% (95% CI: 36%–47%) acceptable technique, and 31% (95% CI: 28%–35%) correct usage in patients with asthma or COPD. Error rates were higher for pressurized metered-dose inhalers (MDIs), with 38% of patients demonstrating poor technique compared to 23% of those using dry-powder inhalers (DPIs). Acceptable usage was reported for 37% and 44% of users of MDIs and DPIs, respectively.20
Poor inhaler technique and inadequate inhaler instruction contribute to suboptimal control of COPD,9,21 nonadherence, and poor clinical outcomes.18,21,22 We lack an understanding of factors that contribute to incorrect inhaler usage,23 although research suggests higher error rates in patients who self-educate on usage and those who are female, older, and have fewer years of education.11,18,24,25
A greater understanding of relationships between patient characteristics and inhaler technique may facilitate efforts to identify patients at risk for incorrect inhaler usage. This information can guide clinicians’ efforts to prescribe the device type that is most likely to be used correctly. The objectives of this analysis were to: 1) quantify the level of concordance between physician and patient ratings of confidence in device usage, 2) assess the association of treatment adherence with physician-perceived and patient self-reported confidence in patients’ ability to correctly use inhaler(s), 3) identify patient characteristics associated with low confidence in inhaler usage, and 4) assess associations between inhaler technique and COPD-related health status.
Methods
Study design
This was a prospective analysis of the 2013 Adelphi Respiratory Disease Specific Program, a large, multinational, observational, cross-sectional survey that collects real-world data from physicians and patients.26 Physicians were identified from publicly available lists and contacted by telephone to determine if they met the eligibility criteria for the survey. Eligible, consenting primary care physicians and pulmonologists practicing in the US completed surveys for the next five consecutive, eligible patients who were consulting for any reason and were compensated at fair market rates for their participation.
Patients for whom their physician completed a survey were invited to respond to a questionnaire, which was voluntarily and independently completed with no input or direction from clinicians. Patients provided written informed consent before participation. No tests, treatments, or investigations were performed as part of this survey. The survey was conducted as a market research survey adhering to the ICC/ESOMAR International code on observational research and performed in full accordance with the rules of the US Health Insurance Portability and Accountability Act 1996.27 IRB approval was not necessary or sought.
Subjects
Physicians eligible for participation included those who completed medical training in the last 5–35 years, were personally responsible for treating patients with COPD, and treated at least 3 COPD patients per week. Patient eligibility criteria were age ≥40 years, a physician-confirmed diagnosis of COPD, a history of tobacco use, and a prescription for ≥1 inhaled medication. Patients with asthma were ineligible and those who declined to complete a questionnaire despite availability of a physician-completed survey were excluded from all analyses.
Assessments
Physicians reported patient demographics, type of prescribed inhaler(s), provision of device training, severity of COPD, and comorbid health conditions. They assessed patients’ confidence in the use of inhaler device(s) on a 5-point Likert scale ranging from 1 (not at all confident) to 5 (completely confident) in response to the question, “How confident are you that your patient is using their inhaler correctly”. Completion of each survey took ~20 minutes, with compensation provided for each completed survey.
The patient-completed survey included items comparable to the physician instrument, with confidence in use of inhalers assessed by the question, “How confident are you that you are using your inhaler correctly” and responses recorded on a 5-point Likert scale. Physician- and patient-reported confidence ratings were used as a proxy for correct inhalation technique.
Patients also completed the EuroQoL 5 (EQ-5D-3L) including the graduated visual analog scale (VAS) and five dimensions of health,28 and the COPD assessment test (CAT)29 to assess the impact of COPD on their health status. Patient-reported treatment adherence was assessed with the 8-item Morisky Medication Adherence Scale (MMAS-8),30 with low adherence validated for MMAS-8 scores ranging from 0 to <6, medium for scores of 6 to <8, and high for scores of 8. Completion of the patient survey and standardized questionnaires required about 15 minutes and no compensation was provided.
Statistical analysis
Percent responses were calculated for categorical variables and means and standard deviations for continuous variables. Spearman correlation evaluated the relationship between confidence in the use of inhaler(s) and adherence. Wilcoxon and weighted kappa (κ) statistics31 determined the degree of concordance between physician and patient ratings of confidence in correct inhaler usage. Kappa values <0 were equal to poor concordance, 0.0–0.20 slight, 0.21–0.40 fair, 0.41–0.60 moderate, 0.61–0.80 substantial, and 0.81–1.00 almost perfect concordance.32 Ratings of not at all, slightly, and moderately confident were summed to represent low confidence, while ratings of completely and very confident indicated high confidence in device usage.
Stepwise logistic regression identified relationships between high versus low confidence in inhaler technique and patient demographic and clinical characteristics. Patients receiving their COPD medication by nebulizers alone were excluded due to very small sample size. Standard errors were adjusted for a possible correlation between patients consulting the same physician. Multiple linear regression evaluated relationships between high versus low confidence in inhaler usage and measures of health status. Logistic regression analysis assessed relationships between confidence in the use of inhaler(s) and patient-reported treatment satisfaction. Covariates included age, COPD severity, person providing inhaler education, number of comorbidities, education level, adherence, and concomitant nebulizer use. Kruskal–Wallis tests were performed to determine the significance of relationships between confidence in use of inhaler(s) and treatment adherence. All statistical analyses were performed with Stata/SE version 12.1.33
Results
A total of 76 (56.7%) primary care physicians and 58 (43.3%) pulmonologists completed questionnaires for 373 patients. The median patient age was 67.0 years, with 171 (45.8%) indicating high school as their highest level of educational attainment (Table 1). More than half of patients were prescribed DPIs and MDIs together; 44 (11.8%) were prescribed nebulized medications plus a DPI or MDI. Almost all patients indicated they received inhaler training from a health care professional.
  | Table 1 Demographic and clinical characteristics of patients |
Physician versus patient-reported confidence in the correct use of inhaler device(s)
Complete confidence in device usage was observed for 22% and 17% of patients, whereas 33% and 41% of patients indicated moderate, slight, or no confidence in correct use of inhaler(s) as reported by patients and physicians, respectively (Figure 1). Low confidence was reported by 91 (37%) patients for DPIs and 86 (33%) for MDIs. Physicians reported 104 (42%) and 112 (43%) patients had low confidence in the use of DPIs and MDIs, respectively. Evaluation of concordance between physician- and patient-reported confidence ratings for inhaler use resulted in κ=0.397, equivalent to fair agreement.32
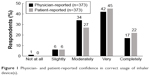  | Figure 1 Physician- and patient-reported confidence in correct usage of inhaler device(s). |
Physicians overestimated confidence in inhaler usage in 18% of patients compared with patient ratings, while 30% of patients overestimated confidence relative to physician ratings. Significantly more patients with low confidence had comorbid depression, anxiety, and congestive heart failure compared to those with high confidence (Figure 2; Table 2).
  | Figure 2 Anxiety and depression in patients reporting low and high confidence in correct usage of inhaler device(s). |
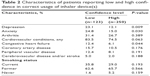  | Table 2 Characteristics of patients reporting low and high confidence in correct usage of inhaler device(s) |
Association of treatment adherence with physician- and patient-reported confidence in device usage
High confidence ratings by physicians and patients were associated with the highest levels of treatment adherence, with 33% and 38% of patients with high confidence ratings by both physicians and patients demonstrating high and medium adherence, respectively (Figure 3). Low adherence was reported for 64% of patients with low confidence ratings by physicians and patients compared to 30% of patients with high physician and patient confidence ratings (P<0.0001).
  | Figure 3 Association of treatment adherence with physician- and patient-reported confidence in correct usage of inhaler device(s). |
Patient characteristics associated with physician- and patient-reported confidence in device usage
Complete covariate data for the stepwise logistic regression analysis of predictors of confidence in inhaler use were available for 289 patients. Lack of physician diagnosis of depression and college education were significantly associated with high patient-reported confidence in device usage (Table 3). Fewer comorbidities, and training provided by self or family members were significantly associated with high physician-reported confidence in inhaler use (Table 3). Patient age, physician-reported severity of COPD, and use of one or more types of hand-held inhaler devices (MDI only, DPI only, or both) were not significant predictors of physician- or patient-reported confidence.
Association of physician- and patient-reported confidence with health status
High physician-reported confidence in inhaler usage was significantly associated with lower CAT scores, higher EQ-5D VAS, and greater overall patient satisfaction with inhaler treatment. Similar results were found for patient-reported confidence in device usage for CAT scores and inhaler satisfaction (Table 4).
Discussion
This real-world study of community-based, US primary care physicians and pulmonologists and their patients demonstrated that both physicians and patients expressed low confidence in patients’ ability to correctly use inhaler(s). Notably, physicians reported lower confidence in patients’ ability to use inhalers than patients’ self-reported confidence, and the level of agreement between their responses was only fair suggesting that patients may overestimate their ability to correctly use inhaler(s). Alternatively, physicians might underestimate patients’ proficiency in the use of inhalers.
Our objective was to determine if confidence was significantly associated with patient-reported outcomes, including adherence. We found that physician- and patient-reported ratings of confidence in device usage were significantly associated with overall self-reported treatment adherence. The lowest adherence was evident in patients who reported low confidence and were perceived to be the least confident in device usage by their physicians. These results suggest that physician recognition of the factors associated with patient confidence in inhaler usage may help to identify patients who are likely to benefit from additional education or choose a different inhaler device that would suit their needs. Interestingly, we did not find an association between confidence and age or physician-reported COPD severity although previous research suggests the existence of an association between older age34 and confidence. Additional research to identify other factors that influence confidence may improve patient outcomes.
Self-education or training provided by family members were associated with significantly higher physician-reported confidence levels, which might suggest some benefit of training both patients and caregivers. These results, however, should be interpreted cautiously given the low proportion of patients who did not also receive training from a person other than a health professional. The important findings of this study lie in the fact that the report of low confidence in inhaler usage is seen despite receipt of training by the patient. However, the extent of training received by the patient could not be ascertained in this research and can be perceived as a limitation that precludes from making any strong conclusion about the role of education. Other characteristics significantly associated with greater confidence in device usage were fewer comorbidities, the absence of depression, and higher education levels. Overall, these results suggest that, clinicians may need to consider patient characteristics in inhaler device selection for patients at risk of having low confidence to avoid subsequent non adherence. Other factors, such as medication costs and higher cost sharing by patients, are also likely to influence adherence and should be considered when prescribing inhaler devices.
Approximately 75% of patients in our study used more than one inhaler, further highlighting the importance of device instruction and education. Previous research suggests that patients’ ability to properly use inhalers is improved by instruction from clinicians in the proper use of inhaler(s), regular follow-up assessment of inhaler technique, and remedial training.9,11,21,35–39
Interestingly, literature suggests that even health professionals require training in the use of inhaler devices before they can effectively educate their patients,37 with many clinicians not optimally informed about the appropriate use of inhaler devices and effective patient education strategies.10,12,17 One study reported that only 14% of >1,500 physicians had adequate knowledge of inhaled therapy, <50% knew correct inhalation maneuvers required for DPI inhalers, and only 25% checked patients’ inhalation technique before prescribing new device(s) or drug combinations.40
Typically, observation, oral instructions, and demonstration are essential for effective education on optimal device usage.25,37,39,41 Successful device training reduces the frequency of exacerbations and dyspnea and improves quality of life.42 Repeated instruction in inhalation techniques increases adherence and improves patients’ health status43 because patients are likely to forget what has been taught as time elapses from the point of training.12
Choice of inhaler device tailored to the individual patient’s ability to use a particular type of device as well as patient needs and preferences can also enhance patients’ confidence and maintain long-term treatment adherence.9,24,25,36 Patient preferences and their ability to generate the appropriate level of inspiratory flow for inhaler(s) are critical factors to consider when prescribing device(s).37,44 Patients with spontaneous breathing, good dexterity, and poor inspiratory flow may benefit from a pressurized MDI, while those with inadequate coordination but sufficient inspiratory flow may do well with a DPI or a pressurized MDI with a spacer.37 Nebulizers are an alternative to pressurized MDIs plus a spacer and DPI, particularly for elderly patients, those with severe disease and frequent exacerbations, and those with physical or cognitive limitations.45 Many patients, particularly those with moderate or severe COPD, have difficulty achieving the minimum inhalation rate required for a DPI.44 Patients with severe airflow obstruction may only achieve the full benefits of inhaled therapy by using a spacer37 or a nebulizer.37,45 Spacer devices and nebulized medications may benefit patients for whom low confidence is related to diminished inspiratory flow or difficulties using inhalers due to impaired cognitive function, manual dexterity, or hand strength.25
The results of this observational survey must be considered within the context of several limitations that are inherent to all surveys – selection bias, potential lack of generalizability, and recall bias. The data source was a cross-sectional survey meaning adherence could only be measured by one-time patient self-report through validated questionnaire and not monitored longitudinally. The use of a single-item question about confidence in device usage could be perceived as another limitation. However, several validated instruments including the CAT, MMAS-8, and the EQ-5D-3L were used in the study, and the direction of association between confidence, adherence and health status had the expected trend. These findings suggest high concurrent validity with our results about patient confidence in device usage. The list of patient characteristics was not an exhaustive list of all factors that might affect confidence, such as cognitive abilities and motor coordination. Furthermore, this study was unable to assess whether HCPs were accurate in their instructions to patients for correct inhaler technique, which if incorrect could have undermined the benefits and, therefore, confidence the inhaler was being used correctly. Finally, confidence in device usage was not always specific to a single inhaler because a high percentage of patients used multiple inhalers. Despite these limitations, the findings of the study suggest that considering various patient factors for inhaler selection and training can help increase patient’s confidence in correct inhaler usage. This may, in turn, help achieve better outcomes for COPD patients.
Conclusion
Our results indicate that 1 in 3 COPD patients have low confidence in correct usage of inhaler devices and further poor inhaler confidence is associated with lower COPD-related health status. These findings may motivate a more individualized approach by health care professionals when considering inhaler delivery mechanisms and patient education to ensure better patient outcomes.
Acknowledgments
This study was supported by Sunovion Pharmaceuticals Inc. Medical writing support was provided by Carole Alison Chrvala, PhD of Health Matters, Inc, funded by Sunovion Pharmaceuticals Inc.
Data collection was undertaken by Adelphi Real World as part of a syndicated survey, entitled the Respiratory Disease Specific Programme, sponsored by multiple pharmaceutical companies of which one was Sunovion Pharmaceuticals Inc. Sunovion Pharmaceuticals Inc. did not influence the original survey through either contribution to the design of questionnaires or data collection. The study described here using data from the Respiratory Disease Specific survey was funded by Sunovion Pharmaceuticals Inc.
Disclosure
ANA is on the speaker’s bureau for Sunovion Pharmaceuticals Inc. VG is an employee of Sunovion Pharmaceuticals Inc. AR is an employee of Adelphi Real World. MS is an employee of Adelphi Real World. The authors report no other conflicts of interest in this work.
References
Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease. 2016. Available from: http://www.goldcopd.org/guidelines-global-strategy-for-diagnosis-management.html. Accessed May 1, 2016. | ||
Soriano JB, Lamprecht B. Chronic obstructive pulmonary disease: a worldwide problem. Med Clin North Am. 2012;96(4):671–680. | ||
Hoyert DL, Xu JQ. Deaths: preliminary data for 2011. Natl Vital Stat Rep. 2012;61(6):1–65. | ||
Guarascio AJ, Ray SM, Finch CK, Self TH. The clinical and economic burden of chronic obstructive pulmonary disease in the USA. Clinicoecon Outcomes Res. 2013;5:235–245. | ||
Osthoff M, Jenkins C, Leuppi J. Chronic obstructive pulmonary disease – a treatable disease. Swiss Med Wkly. 2013;143:w13777. | ||
Tashkin DP, Ferguson GT. Combination bronchodilator therapy in the management of chronic obstructive pulmonary disease. Respir Res. 2013;14:49. | ||
Darbà J, Ramírez G, Sicras A, Francoli P, Torvinen S, Sánchez-de la Rosa R. The importance of inhaler devices: the choice of inhaler device may lead to suboptimal adherence in COPD patients. Int J Chron Obstruct Pulmon Dis. 2015;10:2335–2345. | ||
Fromer L. Implementing chronic care for COPD: planned visits, care coordination, and patient empowerment for improved outcomes. Int J Chron Obstruct Pulmon Dis. 2011;6:605–614. | ||
Virchow JC, Crompton GK, Dal Negro R, et al. Importance of inhaler devices in the management of airway disease. Respir Med. 2008;102(1):10–19. | ||
Inhaler Error Steering Committee; Price D, Bosnic-Anticevich S, et al. Inhaler competence in asthma: common errors, barriers to use and recommended solutions. Respir Med. 2013;107(1):37–46. | ||
Melani AS, Bonavia M, Cilenti V, et al. Gruppo Educazionale Associazione Italiana Pneumologi Ospedalieri. Inhaler mishandling remains common in real life and is associated with reduced disease control. Respir Med. 2011;105(6):930–938. | ||
Lavorini F. Inhaled drug delivery in the hands of the patient. J Aerosol Med Pulm Drug Deliv. 2014;27(6):414–418. | ||
Roy A, Battle K, Lurslurchachai L, Halm EA, Wisnivesky JP. Inhaler device, administration technique, and adherence to inhaled corticosteroids in patients with asthma. Prim Care Respir J. 2011;20(2):148–154. | ||
Barnestein-Fonseca P, Leiva-Fernández J, Vidal-España F, García-Ruiz A, Prados-Torres D, Leiva-Fernández F. Is it possible to diagnose the therapeutic adherence of patients with COPD in clinical practice? A cohort study. BMC Pulm Med. 2011;11:6. | ||
Cramer JA, Roy A, Burrell A, et al. Medication adherence and persistence: terminology and definitions. Value Health. 2008;11(1):44–47. | ||
Chorão P, Pereira AM, Fonseca JA. Inhaler devices in asthma and COPD – an assessment of inhaler technique and patient preferences. Respir Med. 2014;108(7):968–975. | ||
Lavorini F, Magnan A, Dubus JC, et al. Effect of incorrect use of dry powder inhalers on management of patients with asthma and COPD. Respir Med. 2008;102(4):593–604. | ||
Sanduzzi A, Balbo P, Candoli P, et al. COPD: adherence to therapy. Multidiscip Respir Med. 2014;9(1):60. | ||
Sriram KB, Percival M. Suboptimal inhaler medication adherence and incorrect technique are common among chronic obstructive pulmonary disease patients. Chron Respir Dis. Epub 2015 Sep 22. | ||
Sanchis J, Gich I, Pedersen S. Systematic review of errors in inhaler use: has patient technique improved over time? Chest. 2016;150(2):394–406. | ||
Chapman KR, Fogarty CM, Peckitt C, et al. Delivery characteristics and patients’ handling of two single-dose dry-powder inhalers used in COPD. Int J Chron Obstruct Pulmon Dis. 2011;6:353–363. | ||
Small M, De Courcy J, Roughley A, Bollu V. Confidence in correct inhaler device technique and its association with overall treatment adherence: a retrospective database analysis of real-world US COPD patients. Am J Respiratory Crit Care Med. 2015;191:A6180. | ||
VanderSchaaf K, Olson KL, Billups S, Hartsfield CL, Rice M. Self-reported inhaler use in patients with chronic obstructive pulmonary disease. Respir Med. 2010;104(1):99–106. | ||
Arora P, Kumar L, Vohra V, et al. Evaluating the technique of using inhalation device in COPD and bronchial asthma patients. Respir Med. 2014;108(7):992–998. | ||
Barrons R, Pegram A, Borries A. Inhaler device selection: special considerations in elderly patients with chronic obstructive pulmonary disease. Am J Health Syst Pharm. 2011;68(13):1221–1232. | ||
Anderson P. Real-world physician and patient behavior across countries: disease-specific programmes a means to understand. Curr Med Res Opin. 2008;24(11):3063–3072. | ||
U.S. Department of Health & Human Services, Summary of the HIPAA Privacy Rule 2009. Available from: http://www.hhs.gov/ocr/privacy/. Accessed April 20, 2016. | ||
EuroQol Group. EuroQol – a new facility for the measurement of health-related quality of life. Health Policy. 1990;16(3):199–208. | ||
Jones PW, Harding G, Berry P, Wiklund I, Chen WH, Kline Leidy N. Development and first validation of the COPD assessment test. Eur Respir J. 2009;34(3):648–654. | ||
Morisky DE, Green LW, Levine DM. Concurrent and predictive validity of a self-reported measure of medication adherence. Med Care. 1986;24(1):67–74. | ||
Cohen J. Weighted kappa: nominal scale agreement with provision for scaled disagreement or partial credit. Psychol Bull. 1968;70(4):213–220. | ||
Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33(1):159–174. | ||
StataCorp. Stata Statistical Software: Release 12.1. College Station, TX: StataCorp LP; 2013. | ||
Jarvis S, Ind PW, Shiner RJ. Inhaled therapy in elderly COPD patients; time for re-evaluation? Age Ageing. 2007;36(2):213–218. | ||
Crompton GK, Barnes PJ, Broeders M, et al. Aerosol drug management improvement team. The need to improve inhalation technique in Europe: a report from the aerosol drug management improvement team. Respir Med. 2006;100(9):1479–1494. | ||
Aydemir Y. Assessment of the factors affecting the failure to use inhaler devices before and after training. Respir Med. 2015;109(4):451–458. | ||
Broeders ME, Sanchis J, Levy ML, Crompton GK, Dekhuijzen PN; ADMIT Working Group. The ADMIT series – issues in inhalation therapy. 2 Improving technique and clinical effectiveness. Prim Care Respir J. 2009;18(2):76–82. | ||
Rootmensen GN, van Keimpema AR, Jansen HM, de Haan RJ. Predictors of incorrect inhalation technique in patients with asthma or COPD: a study using a validated videotaped scoring method. J Aerosol Med Pulm Drug Deliv. 2010;23(5):323–328. | ||
Sanchis J, Corrigan C, Levy ML, Viejo JL; ADMIT Group. Inhaler devices from theory to practice. Respir Med. 2013;107(4):495–502. | ||
Plaza V, Sanchis J, Roura P, et al. Physicians’ knowledge of inhaler devices and inhalation techniques remains poor in Spain. J Aerosol Med Pulm Drug Deliv. 2012;25(1):16–22. | ||
Lavorini F, Levy ML, Corrigan C, Crompton G; ADMIT Working Group. The ADMIT series issues in inhalation therapy. 6) Training tools for inhalation devices. Prim Care Respir J. 2010;19(4):335–341. | ||
Göriş S, Taşci S, Elmali F. The effects of training on inhaler technique and quality of life in patients with COPD. J Aerosol Med Pulm Drug Deliv. 2013;26(6):336–344. | ||
Takemura M, Mitsui K, Itotani R, et al. Relationships between repeated instruction on inhalation therapy, medication adherence, and health status in chronic obstructive pulmonary disease. Int J Chron Obstruct Pulmon Dis. 2011;6:97–104. | ||
Geller DE. Comparing clinical features of the nebulizer, metered-dose inhaler, and dry powder inhaler. Respir Care. 2005;50(10):1313–1321. | ||
Dhand R, Dolovich M, Chipps B, Myers TR, Restrepo R, Farrar JR. The role of nebulized therapy in the management of COPD: evidence and recommendations. COPD. 2012;9(1):58–72. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


