Back to Journals » Clinical Ophthalmology » Volume 10
Clinical, optical coherence tomography, and fundus autofluorescence findings in patients with intraocular tumors
Authors Samuelsson D , Sznage M, Engelsberg K, Wittström E
Received 25 March 2016
Accepted for publication 9 June 2016
Published 7 October 2016 Volume 2016:10 Pages 1953—1964
DOI https://doi.org/10.2147/OPTH.S109222
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Daniel Samuelsson, Monika Sznage, Karl Engelsberg, Elisabeth Wittström
Department of Ophthalmology, Lund University, Skane University Hospital, Lund, Sweden
Purpose: To describe clinical, optical coherence tomography (OCT) and fundus autofluorescence (FAF) findings in patients with intraocular tumors and determine if OCT and FAF could be helpful in the differential diagnosis and management of different choroidal tumors.
Methods: Forty-nine patients with untreated, macular, midperipheral, and extrapapillary intraocular tumors were included. All patients underwent ophthalmic examination: best-corrected visual acuity, slit-lamp biomicroscopy, funduscopy, and standardized B mode, and if possible A mode, ultrasonography, and OCT and FAF imaging of the surface of the intraocular tumors.
Results: Of the 49 patients studied, 19 had choroidal nevi, ten had indeterminate choroidal melanocytic lesions (IMLs), ten had malignant melanomas, and ten had other choroidal tumors. The choroidal nevi revealed subretinal fluid (SRF) on OCT in only 11%. FAF detected isoautofluorescence in 42%, hypoautofluorescence in 37%, patchy FAF pattern in 16%, and a diffuse FAF pattern in 5%. Seventy percent of patients with IML showed SRF on OCT and 20% showed tumor growth on follow-up, detected only by OCT and FAF imaging. FAF revealed a patchy pattern in 50% and a diffuse pattern in 40% of cases with IML. Ninety percent of the patients with choroidal melanoma had SRF on OCT and FAF revealed a patchy pattern in 60% and a diffuse pattern in 40%. Patients with other choroidal tumors had SRF on OCT in 30% of cases and no characteristic pattern on FAF.
Conclusion: Both OCT and FAF were helpful in the differential diagnosis of choroidal nevi versus IMLs, choroidal melanomas, and other choroidal tumors. Also, detailed and periodical clinical evaluation of patients with intraocular tumors using OCT and FAF imaging for the detection of both SRF and FAF patterns overlying the tumor can be useful for detection of tumor growth.
Keywords: intraocular tumors, optical coherence tomography, fundus autofluorescence, tumor growth
Introduction
During the past 2 decades, two noninvasive imaging methods, optical coherence tomography (OCT) and fundus autofluorescence (FAF) photography, have become available in routine clinical practice. These methods provide qualitative and quantitative information about retinal changes that are not only important for the management of patients with many retinal diseases but also for patients with intraocular tumors.1–3 OCT and FAF imaging, when used together and combined with fundus photography, fluorescein angiography/indocyanine green angiography (FA/ICG), and ultrasonography, have been shown to be useful for early tumor diagnosis, monitoring of tumor growth, and follow-up of the results of therapies.1–11
Today, spectral domain (SD)-OCT can provide cross-sectional images of the individual retinal layers and SD-OCT scans have been used for the detection and quantification of secondary retinal, retinal pigment epithelium (RPE), and choroidal changes overlying ocular tumors, for example, subretinal fluid (SRF), which may have predictive value for ocular tumor growth and could be a clinical indicator for malignancy in eyes with indeterminate choroidal melanocytic lesions (IMLs).1,6,10–12 OCT was found to be more sensitive than clinical examination or ultrasonography for the identification of SRF.13 SD-OCT findings have recently been reported to be helpful in the diagnosis, follow-up, and treatment of different choroidal tumors, such as nevi, melanomas, metastases, hemangiomas, and lymphomas.6,14–18
Secondary retinal and RPE changes associated with various intraocular tumors can also be documented by FAF. FAF imaging is a noninvasive method that provides a topographical map of lipofuscin, which is the main fundus fluorophore.19 Lipofuscin (a mixture of proteins, lipids, and small chromophores) is the end product of phagocytosed photoreceptor outer segments, mostly accumulating within the RPE cells. It has been shown that excessive accumulation of lipofuscin may impair the function of RPE cells, which may cause atrophy or death of the cells and, secondarily, the death of the overlying photoreceptors.20,21 Using FAF, it is possible to assess the metabolic health and functionality of the RPE cells.20
Today, FAF can be measured using a confocal scanning laser ophthalmoscope. FAF images can also be obtained using a Topcon fundus-based camera system. The autofluorescence images produced by a confocal scanning laser ophthalmoscope and fundus camera are similar.2,3 Several authors have used confocal scanning laser ophthalmoscope to examine FAF images in patients with intraocular tumors,8–10,22–25 while others have studied the autofluorescence using a fundus camera.9,26–31
The documented growth of an IML has been used as a surrogate for malignancy or a risk factor for the malignancy of the lesion since 1994.32–35 There is evidence that large tumors are associated with a poor prognosis and higher metastatic rates.36–38 Shields et al37 reported that each extra millimeter in melanoma thickness meant a 5% higher risk of metastasis. Recently, Damato et al38 revealed that ocular treatment of choroidal melanoma may prevent tumor growth, dedifferentiation, and metastatic disease in younger patients with small and less malignant tumors. The findings in these two reports illustrate the importance of early detection and treatment of malignant uveal melanomas to ensure a more favorable prognosis. Apart from clinical risk factors, such as large tumor size, documented tumor growth, the presence of chromosome 3 monosomy (loss of heterozygosity), and somatic mutations in genes, GNAQ or GNA11 have also been found to be strongly associated with death due to metastases in patients with uveal melanoma.39–42
A good clinical evaluation of intraocular tumors, especially, of IML should include examination with ultrasound, OCT, FAF, FA/ICG and, if necessary, biopsy for histological, cytological, and genetic analysis to enhance the accuracy of early diagnosis and improve prognosis.35
In this study, we have evaluated the clinical, OCT, and FAF findings in 49 patients with intraocular tumors to determine if OCT and FAF could be helpful in the differential diagnosis and management of different choroidal tumors.
Subjects and methods
Forty-nine patients with untreated, macular, midperipheral, and juxtapapillary intraocular tumors, who had been periodically examined or who were referred for examination due to the finding of a new intraocular tumor between 2014 and 2015, were prospectively included in the study and follow-up between 5 and 23 months. Patients were excluded if they had a choroidal tumor that had been treated previously, had nonclear media that would reduce the quality of the OCT scans and FAF images, or had very peripheral choroidal tumors that could not be imaged using OCT and FAF.
A diagnostic decision was made by an experienced specialist in ocular oncology for each patient included in this study, on the basis of clinical manifestation, including A- and B-scan ultrasonography, biomicroscopy, fundus photography, and in some cases FA/ICG characteristics. The characteristics showed in OCT and FAF under study were not used to confirm the initial diagnosis. In one patient, the choroidal melanoma was diagnosed by transretinal biopsy. The patients studied were divided into four groups: nevi, IMLs, melanomas, and other choroidal tumors, which were compared. All patients included in the study underwent ophthalmic examination, including best-corrected visual acuity (VA), slit-lamp biomicroscopy, funduscopy, standardized B mode, and if possible A mode, ultrasonography, and color fundus photography. Some patients also underwent FA and ICG. In addition, all patients underwent OCT and FAF imaging of the surface of intraocular tumors and macula.
A- and B-scan ophthalmic ultrasonography was performed on all patients using a CineScan S (Quantel Medical, Clermont-Ferrand, France).
OCT was performed using the SD 3D OCT-1000, version 3.00 software (Topcon, Tokyo, Japan). The 3D macular scan option was used for all scans in this study, centered on the tumor and the fovea, covering 6×6 mm, with a resolution of 512×128 pixels. The presence of SRF was documented in each studied group and compared between groups.
FAF was performed with a Topcon TRC-50DX retinal camera (Topcon, with an excitation bandpass filter of 535–585 nm and a barrier bandpass filter of 605–715 nm). All OCT and FAF images were reviewed by two reviewers. The FAF patterns in choroidal tumors were classified as patchy or diffuse when applicable. The patchy pattern was defined as the presence of distinct areas of increased FAF between areas of normal autofluorescence. The diffuse pattern was characterized by the presence of increased FAF with indistinct borders over a larger part of the tumor in the absence of intervening areas of normal FAF.8 Abnormal autofluorescence was also defined as either increased or decreased FAF in comparison with background FAF, and classified as isoautofluorescence, hypoautofluorescence, or a combination of hypoauto and hyperautofluorescence (mixed).23,27
The following patient characteristics and clinical examination findings at the time of OCT and FAF imaging were recorded and analyzed: sex (male, female), age, affected eye (right eye, left eye), initial Snellen VA, tumor location (distance to the optic nerve and to the foveola [mm]) and largest basal diameter (mm) measured using fundus photography, tumor thickness (mm) measured by B-scan ultrasonography, tumor color (pigmented, partially pigmented, and nonpigmented), tumor configuration (flat, dome-shaped), SRF on OCT (yes/no), and FAF findings (patchy, diffuse, isoautofluorescence, hypoautofluorescence, or a combination of hypoauto and hyperautofluorescence [mixed]).
The study was approved by the Ethics Committee of Lund University and all the participants gave their written consent to participate according to the principles outlined in the Universal Declaration of Helsinki.
Statistical analysis
The data were analyzed using computer software SPSS version 22 (IBM Corporation, Armonk, NY, USA). VA was measured using a Snellen chart and then converted to the logarithm of the minimum angle of resolution (logMAR) before statistical analysis. The Mann–Whitney U-test was used for continuous variables and Fisher’s exact test was used for categorical variables. Values of P≤0.05 were considered to indicate statistical significance.
Results
The study consisted of 49 patients with intraocular tumors (19 males and 30 females). The mean age was 64 years (median, 68 years; range, 18–93 years). The intraocular tumors were in the right eye in 24 patients and in the left eye in 25 patients. The mean VA (logMAR) was 0.26 (median, 0.16; range, 0.0–2.0). The mean distance from the tumor margin to the optic nerve was 2.6 mm (median, 2.1 mm; range, 0.0–9.3 mm) and the mean distance to the foveola was 1.7 mm (median, 0.8; range, 0.0–7.5 mm). The mean tumor thickness was 2.3 mm (median, 2.4 mm; range, 0.0–11 mm) and the mean value of the larger basal diameter of the tumor was 6.4 mm (median, 6.0 mm; range, 1.6–14.5 mm). Of the 49 patients studied, 19 had choroidal nevi, ten had IMLs, ten had malignant choroidal melanomas, and ten had other choroidal tumors (two choroidal metastases, three choroidal osteomas, and five choroidal hemangiomas) (Table 1). The mean follow-up (months) for all tumors was 13.5±5.4; choroidal nevi, 14.8±4.7; IMLs, 16.9±4.8; choroidal melanomas, 10.4±5.5; and other choroidal tumors, 10.7±4.8. Both patchy and diffuse FAF patterns were found to be associated with decreased VA in all studied tumor groups (Tables 1 and 2).
Patients with choroidal nevi under observation
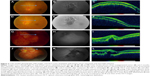
Nineteen of the patients had a diagnosis of choroidal nevus and had been managed by regular observation. The characteristics, clinical, OCT, and FAF findings, are given in Tables 1 and 3. Fundus photographs, FAF images, and OCT scans of two patients with choroidal nevi are presented in Figure 1.
No significant difference was observed between patients with choroidal nevi and IMLs, melanomas, and other choroidal tumors regarding sex, age, affected eye, and distance from the tumor margin to the optic nerve and foveola (Table 1). Patients with choroidal nevi had significantly better VA (logMAR) than those with IMLs and melanomas (P=0.016 and P=0.040, respectively) (Table 1).
Significant differences were observed between choroidal nevus and IMLs, choroidal melanomas, and other choroidal tumors regarding tumor thickness, largest basal diameter, tumor color, configuration, and fluid on OCT and FAF findings (Tables 1 and 3). Choroidal nevi were often pigmented (89%), had a flat configuration (79%), had no fluid on OCT (89%), and often demonstrated isoautofluorescence (42%) and hypoautofluorescence (37%) on FAF imaging (Table 3).
Patients with indeterminate choroidal melanocytic lesion under observation
Ten of the patients had a diagnosis of IML and had been managed by regular observation. The characteristics, clinical, OCT, and FAF findings, are given in Tables 1–4. Fundus photographs, FAF images, and OCT scans of two patients with IML are presented in Figure 1.
No significant difference was observed between patients with IML and patients with choroidal melanoma and other choroidal tumors regarding sex, age, affected eye, VA (logMAR), distance from the tumor margin to the optic nerve and foveola, tumor thickness, largest basal diameter, and fluid on OCT and FAF findings (Tables 2 and 4).
A significant difference was observed only between IML and other choroidal tumors regarding tumor color (P=0.001) (Table 4). Two of ten (20%) patients with IML exhibited tumor growth on follow-up <12 months. This was detected only with OCT and FAF imaging. Color fundus photographs, FAF images, and OCT scans before and 11 months after presentation of one patient with IML who showed tumor growth and FAF pattern changes from patchy to diffuse are shown in Figure 1.
Patients with choroidal melanoma
Ten of the patients had a diagnosis of choroidal melanoma. The characteristics, clinical, OCT, and FAF findings, are given in Tables 1–4. Color fundus photographs, FAF images, and OCT scans of two patients with melanoma are presented in Figure 2. No significant difference was observed between patients with choroidal melanoma and IML and other choroidal tumors regarding sex, age, affected eye, distance from the tumor margin to the optic nerve and foveola, tumor thickness, or largest basal diameter (Table 2). Significant differences were observed between patients with choroidal melanoma and other choroidal tumors regarding tumor color and fluid on OCT (P=0.011 and P=0.020, respectively) (Table 4). One patient with a tumor thickness of 1.9 mm, which was nonpigmented, was diagnosed as having choroidal melanoma by transretinal biopsy (Figure 2).
Patients with other choroidal tumors
Ten of the patients had been classified as having other choroidal tumors. Five of them had choroidal hemangiomas, three osteomas, and two metastases (one breast cancer and one systemic lymphoma). The characteristics, clinical, OCT, and FAF findings, are given in Tables 1–4. Color fundus photographs, FAF images, and OCT scans of four patients with other choroidal tumors are presented in Figures 3 and 4.
There was no significant difference between other choroidal tumors and IML and choroidal melanoma regarding sex, age, affected eye, VA, distance from tumor margin to the optic nerve and foveola, tumor thickness, or largest basal diameter (Table 2). All other choroidal tumors were nonpigmented; 70% of them had no fluid on OCT images and 40% showed isoautofluorescence on FAF images (Table 4).
Discussion
The results of the present study demonstrate that the choroidal nevi located in the macular region, midperiphery, and juxtapapillary regions were pigmented in 89%, flat in 79%, and only 11% showed SRF on OCT. These findings can be compared with those of several other studies on choroidal nevi using OCT imaging in which it was reported that between 16% and 30% of the patients with choroidal nevi had SRF on OCT.7,13,14 The choroidal nevi included in the present study exhibited isoautofluorescence in 42%, hypoautofluorescence in 37%, a patchy FAF pattern in 16%, and a diffuse pattern in 5% of the cases. The FAF abnormalities in the choroidal nevi identified in our study were somewhat different from FAF findings reported by Shields et al26 who found hypoautofluorescence in 56% and isoautofluorescence in only 18% of cases with choroidal nevi. The higher rate of isoautofluorescence in our study could be due to the fact that maybe we included less chronic choroidal nevi with less chronic RPE degenerative features compared to Shields et al.26 We also found both patchy FAF patterns and diffuse patterns in choroidal nevi, while Gündüz et al8 reported that all the choroidal nevi in their study showed a patchy FAF pattern. The present study demonstrates that apart from tumor features, such as tumor thickness, and the largest basal diameter, OCT and FAF findings were also very valuable in differentiating choroidal nevi from IMLs and choroidal melanomas.
The IMLs in this study exhibited significantly greater tumor thickness and larger basal diameter than the choroidal nevi, and did not show any significant differences between choroidal melanoma and other choroidal tumors regarding VA, all tumor characteristics, or OCT and FAF findings. Singh et al10 studied 38 patients with IML or with a small tumor according to the size-based nomenclature used in the Collaborative Ocular Melanoma Study using SD-OCT and FAF imaging and found that nearly 60% of cases had SRF on OCT. Espinoza et al4 detected SRF in 63% of cases of IML. SRF was detected in 70% of the cases of IML using OCT in this study, which is very similar to the OCT findings reported in the two studies mentioned above. Patients with IMLs had both patchy and diffuse FAF patterns. These FAF findings are almost identical to the FAF findings in patients with choroidal melanoma in the present study. Only a few authors have studied FAF overlying IML and found no characteristic patterns of FAF.8,10,23 Our study demonstrates that tumor characteristics, OCT, and FAF findings, were not valuable in differentiating an IML from choroidal melanoma or other choroidal tumors, but were valuable in monitoring tumor growth. Two of ten patients (20%) with IML in this study showed tumor growth on follow-up <12 months. Tumor growth was only detected using OCT and FAF imaging. The presence of documented growth of an IML has been used as a surrogate for malignancy for many years and is important in identifying IMLs that require treatment.4,32–35 The two most important predictive clinical risk factors for tumor growth are the presence of SRF overlying the tumor and orange pigment on the surface of the tumor. The evaluation of these two risk factors is most useful using OCT and FAF imaging.4,10
The choroidal melanomas in this study were nonpigmented in 40% of the cases, and 90% of the cases had SRF on OCT. Muscat et al7 detected SRF overlying the untreated choroidal melanomas in 100% of their cases using OCT. The FAF patterns of choroidal melanomas were classified as either patchy or diffuse in this study. This classification was used previously by Gündüz et al.8 They defined the patchy FAF pattern over choroidal melanomas as the presence of distinct areas of increased FAF between areas of normal autofluorescence, and the diffuse pattern of FAF was characterized by the presence of increased FAF with indistinct borders over a larger area of the tumor. We found that 60% of the cases of choroidal melanoma had a patchy FAF pattern, while Gündüz et al8 reported that 68% of choroidal melanoma cases had a diffuse FAF pattern. The higher rate of diffuse FAF patterns reported by Gündüz et al8 compared to the present results could be due to the fact that they included larger choroidal melanomas in their study, and their observations that the diffuse FAF pattern was significantly associated with increased tumor thickness and increased largest basal diameter. Shields et al27 also found that the hyperautofluorescence of choroidal melanomas increased with larger tumors, pigmented tumors, and those with disrupted overlying RPE. Only one of the ten (10%) patients with choroidal melanoma in this study was diagnosed by transretinal biopsy. The majority of patients with malignant choroidal melanoma are today managed by brachytherapy. This is often done without biopsy for histopathological, molecular, or cytological analysis, which prevents adequate prognosis based on histopathological and genetic analysis. Kivelä and Kujala43 reported that the most adequate criteria for prognosis of choroidal melanomas were analysis of chromosomal alternations and gene expression profiling. The presence of only one copy of chromosome 3 (complete monosomy 3) was observed in many choroidal melanomas that had metastasized and at 3-year follow-up, for tumors with complete monosomy 3, the occurrence of metastasis was 0% for small, 24.4% for medium, and 57.5% for large melanomas.41,43 The recent findings by Shields et al37 that each extra millimeter increase in melanoma thickness was associated with 5% increased risk of metastasis and Damato et al38 that ocular treatment of choroidal melanoma may prevent tumor growth, dedifferentiation, and metastatic disease in younger patients with small and less malignant tumors indicate the importance of early and accurate diagnosis by sound clinical evaluation, including OCT, FAF imaging, and biopsy.
Patients with other choroidal tumors in this study exhibited no significant difference regarding clinical and tumor characteristics compared with IMLs and choroidal melanoma cases. All were nonpigmented, and only 30% of the cases had SRF on OCT. None of our cases of choroidal hemangioma showed SRF on OCT. A low rate of the SRF on OCT (in only 19% of the cases with choroidal hemangioma) was also reported by Ramasubramanian et al.31 We found SRF on OCT in 67% of the cases with osteoma (all had choroidal neovascularization), while Freton and Finger16 found SRF in only 27% of the cases with osteoma. Our patients with choroidal metastatic lesions exhibited SRF in 50% of cases, whereas Collet et al24 found SRF in 73% of their cases. In two of our cases (breast cancer metastasis and choroidal lymphoma metastasis), OCT was valuable in monitoring the response to treatment (Figures 3 and 4). OCT and FAF imaging have been demonstrated to be important for monitoring the response to treatment of intraocular tumors by several authors.20 No characteristic patterns of FAF were found in our patients with other choroidal tumors.
Previous studies on FAF imaging in intraocular tumors have revealed that choroidal nevi typically had overlying hypoautofluorescence due to the degeneration or atrophy of RPE cells, and choroidal melanomas, especially large melanomas, generally had confluent/diffuse overlying hyperfluorescence due to the accumulation of lipofuscin within the RPE cells and within SRF.8–10,22,27,30 Patients with choroidal metastases and choroidal hemangiomas in the present study showed both a patchy FAF pattern and isoautofluorescence. It has been reported that choroidal metastases and choroidal hemangiomas often exhibit overlying hyperautofluorescence that is correlated to focal lipofuscin accumulation in the overlying RPE cells as well as in SRF, particularly in acute tumors.24,30,31 Two patients with osteoma in this study had both hypo- and hyperautofluorescence (mixed) overlying the tumors. Characteristic FAF patterns have recently been reported in patients with osteomas, with isoautofluorescence overlying calcified regions of the tumor due to the intact RPE, and general hypoautofluorescence in decalcified regions due to hyperplasia, metaplasia, and atrophy of the RPE.25,30
Our study had several limitations, including the small patient number in each studied group, and the grading of patchy versus diffuse FAF pattern of intraocular tumors was not done in a masked fashion but interobserver variability was tested in the classification of FAF pattern. All patients but one had the preliminary diagnosis based on clinical tumor features, funduscopy, ultrasound measurements, and FA/ICG findings.
There is thus considerable evidence that OCT and FAF imaging should be incorporated into diagnostic algorithms for intraocular tumors in clinical care in order to improve the characterization of tumors, and promote early diagnosis and treatment to improve patient survival and decrease the risk of metastasis, especially in patients with IML.4,6–8,10,11,20,22–31
Conclusion
This study demonstrates that both OCT and FAF were helpful in the differential diagnosis of choroidal nevi versus IMLs, choroidal melanomas, and other choroidal tumors. The accurate and periodical clinical evaluation of patients with intraocular tumors using ultrasound in combination with OCT and FAF for the detection of both SRF and characteristic FAF patterns overlying the tumors may be useful for detection of tumor growth.
Acknowledgments
This study was supported by Stiftelsen för synskadade I fd Malmöhus län and Skane University Hospital.
Disclosure
The authors report no conflicts of interest in this work.
References
Heimann H, Jmor F, Damato B. Imaging of retinal and choroidal vascular tumours. Eye. 2013;27(2):208–216. | ||
Schmitz-Valckenberg S, Holz FG, Bird AC, Spaide RF. Fundus autofluorescence imaging. Review and perspectives. Retina. 2008;28(3):385–409. | ||
Spaide R. Autofluorescence from the outer retina and subretinal space, hypothesis and review. Retina. 2008;28(1):5–35. | ||
Espinoza G, Rosenblatt B, Harbour JW. Optical coherence tomography in the evaluation of retinal changes associated with suspicious choroidal melanocytic tumors. Am J Ophthalmol. 2004;137(1):90–95. | ||
Schlitt MA, Kaliki S, Shields CL. Reduction of orange pigment overlying choroidal melanoma following plaque radiotherapy. Retina Today. 2013;(9):35–36. | ||
Say EA, Shah SU, Ferenczy S, Shields CL. Optical coherence tomography of retinal and choroidal tumors. J Ophthalmol. 2011;2011:385058. | ||
Muscat S, Parks S, Kemp E, Keating D. Secondary retinal changes associated with choroidal naevi and melanomas documented by optical coherence tomography. Br J Ophthalmol. 2004;88(1):120–124. | ||
Gündüz K, Pulido JS, Pulido JE, Link T. Correlation of fundus autofluorescence with fluorescein and indocyanine green angiography in choroidal melanocytic lesions. Retina. 2008;28(9):1257–1264. | ||
Shields CL, Bianciotto C, Pirondini C, Materin MA, Harmon SA, Shields JA. Autofluorescence of orange pigment overlying small choroidal melanoma. Retina. 2007;27(8):1107–1111. | ||
Singh A, Belfort RN, Sayanagi K, Kaiser PK. Fourier domain optical coherence tomographic and auto-fluorescence findings in indeterminate choroidal melanocytic lesions. Br J Ophthalmol. 2010;94(4):474–478. | ||
Materin MA, Raducu R, Bianciotto C, Shields CL. Fundus autofluorescence and optical coherence tomography findings in choroidal melanocytic lesions. Middle East Afr J Ophthalmol. 2010;17(3):201–206. | ||
Wojtkowski M, Bajraszewski T, Gorczyńska I, et al. Ophthalmic imaging by spectral optical coherence tomography. Am J Ophthalmol. 2004;138(3):412–419. | ||
Shields CL, Mashayekhi A, Materin MA, et al. Optical coherence tomography of choroidal nevus in 120 patients. Retina. 2005;25(3):243–252. | ||
Shah SU, Kaliki S, Shields CL, Ferenczy SR, Harmon SA, Shields JA. Enhanced depth imaging optical coherence tomography of choroidal nevus in 104 cases. Ophthalmology. 2012;119(5):1066–1072. | ||
Shields CL, Kaliki S, Rojanaporn D, Ferenczy S, Shields JA. Enhanced depth imaging optical coherence tomography of small choroidal melanoma. Arch Ophthalmol. 2012;130(7):850–856. | ||
Freton A, Finger PT. Spectral domain-optical coherence tomography analysis of choroidal osteoma. Br J Ophthalmol. 2012;96(2):224–228. | ||
Egawa M, Mitamura Y, Hayashi Y, Naito T. Spectral-domain optical coherence tomographic and fundus autofluorescence findings in eyes with primary intraocular lymphoma. Clin Ophthalmol. 2014;8:335–341. | ||
Egawa M, Mitamura Y, Hayashi Y, Semba K, Naito T. Changes of fundus autofluorescence and spectral-domain optical coherence tomographic findings after treatment of primary intraocular lymphoma. J Ophthalmic Inflamm Infect. 2014;4(1):7. | ||
Delori FC, Dorey K, Staurenghi G, Arend O, Goger DG, Weiter JJ. In vivo fluorescence of the ocular fundus exhibits retinal pigment epithelium lipofuscin characteristics. Invest Ophthalmol Vis Sci. 1995;36(3):718–729. | ||
Nandakumar N, Buzney S, Weiter JJ. Lipofuscin and the principles of fundus autofluorescence: a review. Semin Ophthalmol. 2012;27(5–6):197–201. | ||
Nilsson SE, Sundelin SP, Wihlmark U, Brunk UT. Aging of cultured retinal pigment epithelial cells: oxidative reactions, lipofuscin formation and blue light damage. Doc Ophthalmol. 2003;106(1):13–16. | ||
Gündüz K, Pulido JS, Bakri SJ, Petit-Fond E. Fundus autofluorescence in choroidal melanocytic lesions. Retina. 2007;27(6):681–687. | ||
Lavinsky D, Belfort RN, Navajas E, Torres V, Martins MC, Belfort R Jr. Fundus autofluorescence of choroidal nevus and melanoma. Br J Ophthalmol. 2007;91(10):1299–1302. | ||
Collet LC, Pulido JS, Gündüz K, et al. Fundus autofluorescence in choroidal metastatic lesions. A pilot study. Retina. 2008;28(9):1251–1256. | ||
Sisk RA, Riemann CD, Petersen MR, et al. Fundus autofluorescence findings of choroidal osteoma. Retina. 2013;33(1):97–104. | ||
Shields CL, Pirondini C, Bianciotto C, Materin MA, Harmon SA, Shields JA. Autofluorescence of choroidal nevus in 64 cases. Retina. 2008;28(8):1035–1043. | ||
Shields CL, Bianciotto C, Pirondini C, Materin MA, Harmon SA, Shields JA. Autofluorescence of choroidal melanoma in 51 cases. Br J Ophthalmol. 2008;92(5):617–622. | ||
Ishida T, Ohno-Matsui K, Kaneko Y, et al. Fundus autofluorescence patterns in eyes with primary intraocular lymphoma. Retina. 2010;30(1):23–32. | ||
Casady M, Faia L, Nazemzadeh M, Nussenblatt R, Chan CC, Sen HN. Fundus autofluorescence patterns in primary intraocular lymphoma. Retina. 2014;34(2):366–372. | ||
Almeida A, Kaliki S, Shields CL. Autofluorescence of intraocular tumours. Curr Opin Ophthalmol. 2013;24(3):222–232. | ||
Ramasubramanian A, Shields Cl, Harmon SA, Shields JA. Autofluorescence of choroidal hemangioma in 34 consecutive eyes. Retina. 2010;30(1):16–22. | ||
Shields CL, Shields JA, Kiratli H, De Potter P, Cater JR. Risk factors for growth and metastasis of small choroidal melanocytic lesions. Ophthalmology. 1995;102(9):1351–1361. | ||
COMS Report no 5. Factors predictive of growth and treatment of small choroidal melanoma. Arch Ophthalmol. 1997;115(12):1537–1544. | ||
Shields CL, Cater J, Shields JA, Singh AD, Santos MCM, Carvalho C. Combination of clinical factors predictive of growth of small choroidal melanocytic tumors. Arch Ophthalmol. 2000;118(3):360–364. | ||
Rishi P, Koundanya VV, Shields CL. Using risk factors for detection and prognostication of uveal melanoma. Indian J Ophthalmol. 2015;63(2):110–116. | ||
Singh AD, Turell ME, Topham AK. Uveal melanoma: Trends in incidence, treatment, and survival. Ophthalmology. 2011;118(9):1881–1885. | ||
Shields CL, Furuta M, Thangappan A, et al. Metastasis of uveal melanoma millimeter-by-millimeter in 8033 consecutive eyes. Arch Ophthalmol. 2009;127(8):989–998. | ||
Damato BE, Heimann H, Kalirai H, Coupland SE. Age, survival predictors, and metastatic death in patients with choroidal melanoma. JAMA Ophthalmol. 2014;132(5):605–613. | ||
Shields CL, Ganguly A, Materin MA, et al. Chromosome 3 analysis of uveal melanoma using fine-needle aspiration biopsy at the time of plaque radiotherapy in 140 consecutive cases. Trans Am Ophthalmol Soc. 2007;105:43–53. | ||
Van Raamsdonk CD, Griewank KG, Crosby MB, et al. Mutations in GNA 11 in uveal melanoma. N Engl J Med. 2010;363(23):2191–2199. | ||
Shields CL, Ganguly A, Bianciotto CG, Turaka K, Tavallali A, Shields JA. Prognosis of uveal melanoma in 500 cases using genetic testing of fine-needle aspiration biopsy specimens. Ophthalmology. 2011;118(2):396–401. | ||
Finger PT, Chin KJ, Semenova EA. Intravitreal anti-VEGF therapy for macular radiation retinopathy: a 10-year study. Eur J Ophthalmol. 2016;26(1):60–66. | ||
Kivelä T, Kujala E. Prognostication in eye cancer: the latest tumor, node, metastasis classification and beyond. Eye. 2013;27(2):243–252. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.