Back to Journals » Clinical Ophthalmology » Volume 17
Causes of Immediate and Early IOP Spikes After Circumferential Gonioscopy-Assisted Transluminal Trabeculotomy Using ASOCT
Authors Rao A , Khan SM, Mukherjee S
Received 17 November 2022
Accepted for publication 5 January 2023
Published 22 January 2023 Volume 2023:17 Pages 313—320
DOI https://doi.org/10.2147/OPTH.S397816
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Aparna Rao,* Sardar Mohd Khan,* Sujoy Mukherjee
Glaucoma Service, LV Prasad Eye Institute, Bhubaneswar, Odisha, 751024, India
*These authors contributed equally to this work
Correspondence: Aparna Rao, Glaucoma Service, LV Prasad Eye Institute, MTC Campus, Bhubaneswar, Odisha, 751024, India, Tel +91 674 2653001, Fax +91 674 2653130, Email [email protected]; [email protected]
Purpose: To report the early postoperative causes of intraocular pressure (IOP) spikes after complete circumferential gonioscopy-assisted transluminal trabeculotomy (GATT) using anterior segment optical coherence tomography (ASOCT).
Methods: This was retrospective interventional case series of patients who underwent circumferential GATT by a single surgeon (APR) from 2021 to 2022 at a tertiary eye care in East India and who developed IOP spikes at 1 day-2 weeks (immediate) or early (> 2 weeks– 2 months) after GATT. The intraocular pressure (IOP), glaucoma medications, and angle evaluation by ASOCT at 1 week, and 1 month were compared between the two groups.
Results: Thirty-two eyes of 32 consecutive patients, aged 40± 20.1 years (20 exfoliation glaucoma, 9 juvenile open-angle, and 3 developmental glaucoma), that developed IOP spikes between immediate (n=20) or early (n=12) IOP spikes after GATT, were included. Immediate postoperative spikes were seen in 20 eyes due to retained viscoelastic (n=8), hyphema (n=8) in uncontrolled hypertension, and peripheral anterior synechiae (PAS) (n=6) of which only one eye required medication at 2 months. Causes of immediate IOP spikes on ASOCT included an inverted/reattached trabecular shelf, iris strands in eyes with abnormal iris in developmental glaucoma, and PAS in 1– 2 quadrants. Causes of early IOP spikes included PAS > 3 quadrants (n=8), and hyperreflective fibrotic tissue over TM (n=4) with 50% requiring medications at 2 months. The ASOCT features predicting the need for medications were PAS > 3 quadrants (OR=8.4[2.2– 14.3], p=0.03) and fibrotic TM closure (OR=5.4, [3.6– 10.2], p=0.003). One eye with macrohyphema 3 days after surgery owing to uncontrolled hypertension (owing to the stoppage of medicines), required additional incisional trabeculectomy within 1 month of surgery.
Conclusion: Immediate IOP spikes are mostly self-resolving as opposed to early IOP spikes > 2 weeks that require medications after GATT. Gonioscopic PAS > 3 quadrants, and fibrotic TM closure were the main identifiable ASOCT causes predicting the need for medications after GATT.
Keywords: GATT, MIGS, angle surgery, intraocular pressure, anterior segment OCT, glaucoma surgery
Introduction
Gonioscopy-assisted transluminal trabeculotomy (GATT) has proved itself as a feasible alternative over trabeculectomy for glaucoma surgeons allowing effective means for reducing intraocular pressure (IOP) cost-effectively while sparing the conjunctiva for future filtering surgeries.1–3 This has been reported to be effective in all types of glaucoma including primary adult, congenital glaucoma, juvenile open-angle glaucoma, exfoliation, uveitis, and steroid glaucoma.1,3,4 As one of the minimally invasive glaucoma surgeries (MIGS), it helps reduce recovery time and operative time while offering an alternative to bleb-forming trabeculectomy in the modern era of glaucoma surgery.1,2 The 2 years results show an efficacy of 80–90% success in terms of IOP control over 12–24 months across studies.2–5 While this surgery has been adopted globally after its introduction, the better safety profiles over ab-externo trabeculectomy and its efficacy have resulted in the adoption of this surgery for increasing indications as a stand-alone procedure or combined with cataract surgery.2,5
Several studies have identified several predictors of success after GATT.3–5 Older age >60 years, use of post-operative steroids, incomplete (<360 degrees) trabeculotomy, peripheral anterior synechia (PAS), eyes that develop IOP spikes (defined as IOP >30mmHg), African American race, and primary glaucoma are some of the factors identified in different studies influencing the short-or long-term success after GATT.1,3,6–8 While IOP spikes after surgery are the second most common complication reported with this procedure after micro- or macrohyphema, causes of such spikes and identification of factors using anterior segment imaging are scarce.3,6,7 Although incomplete or unsuccessful GATT is one cause for IOP spikes after GATT, identifying causes of IOP spikes after complete successful circumferential GATT is crucial to ensure a better surgical outcome and safety profile.
Anterior segment imaging using anterior segment optical coherence tomography (ASOCT) has revolutionized glaucoma management and allows us to visualize angle structures in-vivo while studying the effect of any surgical intervention on the angle anatomy.9–11 This has been used to identify the Schlemm’s canal and to visualize the trabecular shelf after GATT.11 ASOCT can help identify anatomical features in the early-immediate postoperative period predicting failure in GATT.4,7,10,11 We present an ASOCT study of patients that develop IOP spikes after successful GATT to identify additional anterior segment predictors of IOP spikes and surgical outcomes.
Methods
This was part of a retrospective review of the hospital database to identify patients who underwent GATT with or without cataract surgery at a tertiary eye centre in East India. The study was approved by the institutional review board of LV Prasad Eye Institute, MTC campus, Bhubaneswar (IEC-2016-IM-3) and adhered to the tenets of the Declaration of Helsinki.
Patients with open-angle glaucoma (juvenile glaucoma, exfoliation glaucoma, or developmental glaucoma) that underwent GATT using 5–0 blue prolene suture by a single surgeon (APR) for uncontrolled IOP with or without cataract surgery, were identified and those who developed IOP spikes in the immediate (1d-2 weeks) or early postoperative period (>2 weeks–2 months) were included. Glaucoma diagnosis is made at the institute in eyes with open angles on gonioscopy, raised IOP >22mm Hg, rim thinning or retinal nerve fibre layer defects with corresponding field changes in patients aged 3–40 years (juvenile glaucoma), associated with anatomical structural defects in the anterior segment (developmental glaucoma) in patients aged 3–25 years, or aged >40 years with exfoliation material in the anterior segment.
Preoperative and postoperative IOP, number of glaucoma medications, surgical complications, operative notes, and need for additional procedures in the early (2 months) postoperative period, were recorded. Patients were excluded if there was a history of steroid use, previous or concurrent vitreoretinal/vitrectomy procedures, neovascular glaucoma, congenital glaucoma, absent follow-up at 1 month or immediate period, patients with bleeding diathesis, <2 months of follow-up, or incomplete details in the hospital database. When combined with cataract surgery, GATT was performed first, followed by cataract surgery through the same incision. Briefly, a 5–0 blue prolene suture with blunted tip was threaded through an ab-interno goniotomy incision at the nasal quadrant using a surgical goniotomy lens after injecting viscoelastic into the anterior chamber. The suture, once confirmed to be in the Schlemm’s canal under direct visualization, was advanced using a 23-gauge serrated microforceps until the end was visualized at the other end of the goniotomy incision. This end was held with the forceps, while the other end is pulled to strip off the trabecular meshwork circumferentially. The anterior chamber is filled with sodium hyaluronate 1% and intracameral pilocarpine after a thorough wash of the bleed, if any seen intraoperatively. The postoperative follow-up schedule was typically at 1 day, 1 week, 1 month, and 2 months with tapering doses of prednisolone acetate for 4 weeks. Emergency unscheduled visits in between for pain or other causes were also recorded and findings/investigations noted at that visit. The IOP spikes were treated with systemic acetazolamide for 3–7 days, while topical medications were started only for eyes with persistently raised IOP at 1 month after surgery.
The details that were recorded from the hospital database included age at surgery, best-corrected visual acuity (BCVA), diagnosis, preoperative IOP, preoperative/postoperative number of medications, postoperative details and gonioscopy, slit-lamp details, operative details including the degree of angle incised, intraoperative complications/problems, need for additional procedures, and final IOP at 2 months. An IOP spike was defined as a rise in IOP in the operated eye to >30mm Hg, or an increase of at least 6 mm Hg from the last recorded IOP. Surgical success was defined as a post-operative 2 months IOP of <22mm Hg with or without glaucoma medications. Failure was defined as persistent IOP >21mm Hg at 2 months with medicines or requirement of additional procedures for IOP control at any postoperative period.
ASOCT Protocol
Anterior segment Optical Coherence Tomography (Visante, Carl Zeiss Meditec, USA) was performed on postoperative day 1, 1 week,1 month, 2 months, and at the onset of postoperative IOP spike in cases where this occurred. The angle was imaged at four quadrants including additional areas in the nasal quadrant where the angle was incised. The degrees of open TM shelf or visible TM leaflet (Figure 1) and presence of PAS, supraciliary effusions/cleft or clots, or additional angle features, were quantified by noting the number of quadrants of that feature seen on ASOCT.
Statistical Analysis
Descriptive analysis was used to present demographic and clinical data. Normally distributed data were presented as mean and SD, and non-normally distributed data were presented as median and interquartile intervals. Regarding the comparison between groups, continuous data were compared using the paired t-test or the Wilcoxon test, depending on the data distribution. Multivariate regression was used to investigate factors associated with the need for additional medication for IOP control at 2 months.
Results
A total of 72 patients that underwent GATT during the period were screened. Of these, those that had an incomplete follow-up, incomplete GATT (<360 degrees), IOP spikes after 2 months of GATT, or had vitrectomy later (n=40 patients), were excluded. A total of 32 eyes of 30 patients who developed IOP spikes within the first 2 months after GATT were included. This included 20 exfoliation glaucoma, 9 juvenile open-angle glaucoma, and 3 developmental glaucoma, with a mean age of 48±20.1 years. The baseline demographic and clinical profiles are listed in Table 1. All eyes had advanced glaucoma (visual field mean deviation >-12dB), with all eyes requiring three or more medications for IOP control at the time of surgery, Table 1.
 |
Table 1 Baseline Clinical Profile of Patients Who Developed IOP Spikes After Undergoing Successful GATT |
Of these, 20 eyes developed an immediate rise in IOP (1 day–2 weeks after surgery) while early IOP spikes were seen in 12 eyes, Table 2. The final IOP at 1 month reduced in all eyes from 23±14.7 mm Hg to 17±5.8 (p=0.002), with a reduction of anti-glaucoma medications from 3±0.9 to 0.2±0.6, p=0.001. One eye with macrohyphema 3 days after surgery owing to uncontrolled hypertension (owing to the stoppage of anti-hypertensive medicines by self-discretion) required additional anterior chamber wash followed by incisional trabeculectomy within 1 month of surgery, Figure 2. Nineteen of 20 eyes with immediate spikes resolved over time, while 6 eyes with early spikes required medications for IOP control, Table 2. ASOCT identified PAS at 1–2 months in 14 eyes that included 6 eyes with immediate and 8 with early IOP spikes (all aged <40 years). The eyes with immediate IOP spikes had PAS in 1–2 quadrants, while those with early IOP spikes had PAS in >3 quadrants.
 |
Table 2 Complications Seen in Postoperative Period in Eyes That Developed Intraocular Pressure Spikes After Successful GATT |
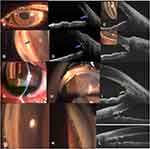
Immediate postoperative spikes (<2 weeks after surgery) were seen in 20 eyes due to retained viscoelastic (n=8), hyphema (n=8, including 2 eyes with the combined cause of retained viscoelastic) in undiagnosed hypertension, peripheral anterior synechiae (PAS) in 1–2 quadrants (n=6). Of the eight eyes with retained viscoelastic causing immediate IOP spike, spontaneous normalization of IOP was seen in six eyes within 1 week, while one eye normalized at 12 days after surgery after having 3 days course of systemic acetazolamide inhibitors. One eye with macrohyphema required additional surgery for persistently raised IOP. None of the other eyes required medications or repeat intervention with all eyes achieving surgical success and IOP <21mm Hg at 2 months. The PAS in the immediate spike was detected at 1 week on ASOCT in four eyes, and at 2 months in two eyes developing PAS in 1–2 quadrants. None of the eyes developed progressive PAS over follow-up visits. Surgical success was achieved in seven of these eight eyes with immediate IOP spike and PAS <3 quadrants, with one eye requiring additional surgery. The other ASOCT features that were seen in eyes that developed immediate spikes included an inverted/reattached trabecular leaflet (n=11), and iris strands in eyes with abnormal iris in developmental glaucoma (n=3). The iris strands in developmental glaucoma were seen as broad extensions or outpouchings of the iris that adhered to the cut end of the trabecular open shelf causing relative angle closure in those focal areas which appeared gonioscopically as iris strands/thick iris process, Figure 2. These were detected on ASOCT at 1–2 weeks with none of these strands causing progressive angle changes on ASOCT over time or requiring medications for IOP control.
Early spikes (>2 weeks–2 months) were seen in 12 eyes, which included eight patients aged <40 years (23±3.2 years). Uncontrolled/unmedicated hypertension was found in two patients of which one required anti-glaucoma medication at 2 months for IOP control. No other discernible causes were found in one eye that was evaluated in detail with ASOCT.
The ASOCT causes of early IOP spikes included PAS >3 quadrants (n=8), and hyperreflective fibrotic tissue over TM (n=4), Figure 2. The eyes with early spikes had PAS in >3 quadrants, with younger patients (n=8) developing it more commonly even after successful GATT. Three of eight patients developed complete angle closure in all quadrants. Six eyes required medications for IOP control at 2 months, while the other two eyes retained normal IOP despite open trabecular shelf in the rest of the angle on ASOCT and gonioscopy. The eyes with fibrotic closure manifested as a hyperreflective membrane in the proposed TM area, while gonioscopically the trabecular shelf appeared open owing to the transparency of the thin film that forms over the cut TM shelf, Figure 2. Comparison of the membrane over time did not reveal any significant change in the appearance or angle anatomy on gonioscopy or ASOCT.
Surgical success was therefore seen in 31 of 32 eyes developing IOP spikes after complete circumferential GATT. One eye with macrohyphema required additional AC wash and trabeculectomy within a month for persistently raised IOP. On multivariate analysis, ASOCT features predicting the need for medications included PAS >3 quadrants (OR=8.4[2.2–14.3], p=0.03) and fibrotic TM closure (OR =5.4, [3.6–10.2], p=0.003, R2=39.3%).
Discussion
This study found surgical success in 31 of 32 eyes despite immediate or early IOP spikes after complete GATT in eyes with advanced exfoliation glaucoma or juvenile open-angle glaucoma. ASOCT features associated with the need for medications included PAS >3 quadrants in younger age groups and fibrotic closure of the TM.
GATT has revolutionized glaucoma surgery owing to its wide applicability and effective IOP reduction.1,7,8,12–19 This is a conjunctival-sparing surgery that allows future incisional filtering surgery even after GATT.1,2 It has been reported to have good IOP outcomes in several studies on POAG, XFG, and severe JOAG.1,4,7,13,15,16,19 This also helps reduce the number of medications, and this is a boon in patients allergic to glaucoma medications. This procedure allows surgeons to offer this as a solution or alternative to trabeculectomy, with comparable efficacy in terms of IOP control while combining the advantages of a goniotomy. This study also concurs with previous studies in terms of IOP control or reduction in the need for AGM in glaucoma. This study in addition observed that most eyes with immediate spikes within 2 weeks resolved over time, while those with late spikes after 2 weeks–2 months were more likely to require medications despite successful GATT. This is attributed to the differences in causes for IOP spikes in the immediate or early period after surgery, as seen in this study.
In this study, the need for medications after GATT was more in eyes with PAS>3 quadrants in patients aged <40 years. This may suggest intense bleeding and inflammation inciting PAS formation in eyes with pre-operative open angles after GATT, with younger patients known to have a pronounced inflammatory response. While a difficult cannulation of the SC can be associated with a severe inflammatory response or bleeding, this was not the case in the eyes with immediate or early IOP spikes seen in this study. While eyes with immediate spikes had fewer quadrants of PAS possibly by minimal bleeding, eyes with early spikes were associated with greater quadrants and the need for medications for IOP control, indicating a more pronounced inflammatory response or bleeding after GATT. It is unclear from this study if this response can be predicted before surgery or intraoperatively apart from younger age being a risk factor. This may be prevented by either intensive steroids or possibly atropine in the postoperative period in younger patients. Studies have identified predictors of success or failure after GATT.2,3,5,6 This includes PAS or macrohyphema, and severe disease at presentation.2,3,6 Studies have reported conflicting reported outcomes of GATT in severe glaucoma with some studies reporting good IOP control, while others reporting a high risk of failure in severe glaucoma.2,5–8,16 PAS after GATT has been reported to be one specific cause of failure or rise in IOP postoperatively and this may be attributed to the shearing force required for threading the suture or microcatheter or tearing of the trabecular shelf apart during GATT.3,6 ASOCT is a valuable tool for imaging the angle in a non-invasive manner while allowing to study of the angle anatomy after any surgical intervention in glaucoma.10 This study identified that PAS that develops in 1–2 quadrants may not affect the final IOP with an open TM shelf in the rest of the quadrants. Yet, it remains to be seen if these PAS are progressive in nature and if long- or short-term atropine or pilocarpine helps prevent their formation after GATT in younger patients.
Failure after incisional trabeculectomy is attributed to aggressive wound healing after surgery.20,21 This leads to blockage of the trabeculectomy ostium or subconjunctival scarring. ASOCT has demonstrated the closure of the ostium and bleb fibrosis and has been valuable to study the bleb characteristics after incisional surgery in glaucoma.11 Yet, fibrosis of the trabecular region after GATT has not been reported; we had four eyes with fibrotic closure of the trabecular shelf in this study. This hyperreflective membrane that is evident on ASOCT can imply fibrotic response from adjoining tissues or can also imply reattachment of the ripped shelf to the inner wall of the Schlemm’s canal. Yet, transparency of the membrane and hyperreflectivity indicate this is a new fibrotic membrane rather than the reattached trabecular shelf that is well appreciated on gonioscopy. This can be triggered by bleeding in the Schlemm’s canal, which is common after GATT, that possibly triggers fibroblasts from adjoining regions. A related hemorrhagic Descemet detachment is commonly reported after ab-interno canaloplasty that is suggestive of sudden forces at the levels of TM or SC.13 Although we did not encounter this complication in this cohort, this calls for safer methods to cut open the trabecular shelf with minimal shearing or ripping forces. Nevertheless, the appearance of this fibrotic membrane in some quadrants did not seem to affect the IOP outcomes in the rest of the eyes, suggesting that the 360-degree opening of the trabecular shelf offsets the effect of this type of focal angle closure in those specific quadrants.
This was a retrospective study with its inherent limitations. We did not evaluate the intraoperative collector system function with dye, which may also have been responsible for IOP spikes in at least some of the eyes with severe glaucoma. Preoperative ASOCT was not done owing to a retrospective design that precluded comparison of pre and postoperative ASOCT. We also had a lot of exfoliation glaucoma patients which could be a cause for selection bias. Yet, this study observed good IOP response to GATT in these patients, which does not suggest diagnosis as a confounding factor for IOP spikes. We also did not study steroid responsiveness in this study, yet we did not see any persistent IOP elevation with the continuation of steroids in the postoperative period even in eyes with immediate IOP spikes suggesting alternate causes. Nevertheless, complete GATT while being effective for IOP control, the development of PAS and fibrotic closure of the TM shelf on ASOCT are causes that are to be kept in mind as causes for IOP spikes in some eyes, after this porcedure, some of which may require medications and close follow-up.
Acknowledgments
Hyderabad Eye Research Foundation. This manuscript has been professionally edited by a professional editing service.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Grover DS, Godfrey DG, Smith O, Feuer WJ, Montes de Oca I, Fellman RL. Gonioscopy-assisted transluminal trabeculotomy, ab interno trabeculotomy: technique report and preliminary results. Ophthalmology. 2014;121(4):855–861. doi:10.1016/j.ophtha.2013.11.001
2. Saheb H, Ahmed II. Micro-invasive glaucoma surgery: current perspectives and future directions. Curr Opin Ophthalmol. 2012;23(2):96–104. doi:10.1097/ICU.0b013e32834ff1e7
3. Cubuk MO, Unsal E. One-year results of gonioscopy-assisted transluminal trabeculotomy: evaluation of prognostic factors. Eur J Ophthalmol. 2021;31(2):460–468. doi:10.1177/1120672120908716
4. Wang Y, Wang H, Han Y, et al. Outcomes of gonioscopy assisted transluminal trabeculotomy in juvenile-onset primary open-angle glaucoma. Eye. 2021;35(10):2848–2854. doi:10.1038/s41433-020-01320-0
5. Guo CY, Qi XH, Qi JM. Systematic review and meta-analysis of treating open angle glaucoma with gonioscopy-assisted transluminal trabeculotomy. Int J Ophthalmol. 2020;13(2):317–324. doi:10.18240/ijo.2020.02.17
6. Chen J, Wang YE, Quan A, et al. Risk factors for complications and failure after gonioscopy-assisted transluminal trabeculotomy in a young cohort. Ophthalmol Glaucoma. 2020;3(3):190–195. doi:10.1016/j.ogla.2020.02.002
7. Grover DS, Smith O, Fellman RL, et al. Gonioscopy assisted transluminal trabeculotomy: an ab interno circumferential trabeculotomy for the treatment of primary congenital glaucoma and juvenile open angle glaucoma. Br J Ophthalmol. 2015;99(8):1092–1096. doi:10.1136/bjophthalmol-2014-306269
8. Loayza-Gamboa W, Martel-Ramirez V, Inga-Condezo V, Valderrama-Albino V, Alvarado-Villacorta R, Valera-Cornejo D. Outcomes of combined prolene gonioscopy assisted transluminal trabeculotomy with phacoemulsification in open-angle glaucoma. Clin Ophthalmol. 2020;14:3009–3016. doi:10.2147/OPTH.S272298
9. Maslin JS, Barkana Y, Dorairaj SK. Anterior segment imaging in glaucoma: an updated review. Indian J Ophthalmol. 2015;63(8):630–640. doi:10.4103/0301-4738.169787
10. Kan JT, Betzler BK, Lim SY, Ang BCH. Anterior segment imaging in minimally invasive glaucoma surgery - a systematic review. Acta Ophthalmol. 2022;100(3):e617–e634. doi:10.1111/aos.14962
11. Ramos JLB, Li Y, Huang D. Clinical and research applications of anterior segment optical coherence tomography—a review. Clin Experiment Ophthalmol. 2009;37(1):81–89. doi:10.1111/j.1442-9071.2008.01823.x
12. Grover DS, Godfrey DG, Smith O, Shi W, Feuer WJ, Fellman RL. Outcomes of Gonioscopy-assisted Transluminal Trabeculotomy (GATT) in eyes with prior incisional glaucoma surgery. J Glaucoma. 2017;26(1):41–45. doi:10.1097/IJG.0000000000000564
13. Lewis RA, von Wolff K, Tetz M, et al. Canaloplasty: circumferential viscodilation and tensioning of Schlemm canal using a flexible microcatheter for the treatment of open-angle glaucoma in adults: two-year interim clinical study results. J Cataract Refract Surg. 2009;35(5):814–824. doi:10.1016/j.jcrs.2009.01.010
14. Chin S, Nitta T, Shinmei Y, et al. Reduction of intraocular pressure using a modified 360-degree suture trabeculotomy technique in primary and secondary open-angle glaucoma. J Glaucoma. 2012;21(6):401–407. doi:10.1097/IJG.0b013e318218240c
15. Salimi A, Nithianandan H, Al Farsi H, Harasymowycz P, Saheb H. Gonioscopy-assisted transluminal trabeculotomy in younger to middle-aged adults: one-year outcomes. Ophthalmol Glaucoma. 2021;4(2):162–172. doi:10.1016/j.ogla.2020.08.014
16. Sharkawi E, Lindegger DJ, Artes PH, et al. Outcomes of gonioscopy-assisted transluminal trabeculotomy in pseudoexfoliative glaucoma: 24-month follow-up. Br J Ophthalmol. 2021;105(7):977–982. doi:10.1136/bjophthalmol-2020-315954
17. Aktas Z, Ucgul AY, Bektas C, Sahin Karamert S. Surgical outcomes of prolene gonioscopy-assisted transluminal trabeculotomy in patients with moderate to advanced open-angle glaucoma. J Glaucoma. 2019;28(10):884–888. doi:10.1097/IJG.0000000000001331
18. Rahmatnejad K, Pruzan NL, Amanullah S, et al. Surgical outcomes of gonioscopy-assisted transluminal trabeculotomy (GATT) in patients with open-angle glaucoma. J Glaucoma. 2017;26(12):1137–1143. doi:10.1097/IJG.0000000000000802
19. Boese EA, Shah M. Gonioscopy-assisted transluminal trabeculotomy (GATT) is an effective procedure for steroid-induced glaucoma. J Glaucoma. 2019;28(9):803–807. doi:10.1097/IJG.0000000000001317
20. Broadway DC, Chang LP. Trabeculectomy, risk factors for failure and the preoperative state of the conjunctiva. J Glaucoma. 2001;10(3):237–249. doi:10.1097/00061198-200106000-00017
21. Landers J, Martin K, Sarkies N, Bourne R, Watson P. A twenty-year follow-up study of trabeculectomy: risk factors and outcomes. Ophthalmology. 2012;119(4):694–702. doi:10.1016/j.ophtha.2011.09.043
 © 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2023 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.