Back to Journals » Clinical Ophthalmology » Volume 8
Bilateral macular infarction as an ocular manifestation of systemic lupus erythematosus (SLE)
Received 27 April 2014
Accepted for publication 24 June 2014
Published 12 September 2014 Volume 2014:8 Pages 1845—1848
DOI https://doi.org/10.2147/OPTH.S66886
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Chih-Ling Hu, Kai-Ling Peng
Department of Ophthalmology, Chi Mei Medical Center, Tainan, Taiwan, Republic of China
Abstract: We report a rare case of bilateral macular infarction as an ocular presenting sign of systemic lupus erythematosus (SLE). A 29-year-old woman presented to our ophthalmologic clinic with a 1-week history of progressive visual loss in her left eye after she had visited a rheumatologic clinic where SLE was diagnosed. At examination, best-corrected visual acuity (BCVA) of the right eye was 6/6, and for the left was counting fingers. Fundus examination revealed perivascular hard exudates along some branches of vessels in both eyes. After pulse therapy, her BCVA in the right eye declined to 6/30 and in the left improved to 3/60. She was administered sub-Tenon’s injections of triamcinolone acetonide 50 mg/week in both eyes for 3 weeks. Her BCVA improved to 3/6 in her right eye and remained at 3/60 in her left eye. Macular infarction is an uncommon but most severe complication of SLE. Early and regular exam of the fundus in patients with SLE is necessary to avoid progression of severe ocular complications.
Keywords: bilateral macular infarction, systemic lupus erythematosus
Introduction
Systemic lupus erythematosus (SLE) is an autoimmune inflammatory disease affecting multiple systems by circulating autoantibodies and the destruction of the accumulating immune complex. Visual system involvement has been found in up to a third of patients with SLE.1 In the majority of cases, visual prognosis is excellent. However, vaso-occlusive retinopathy, even inducing macular ischemia and infarction, a rare and severe ocular complication of SLE, can result in poor visual outcome.
Initial treatment for vaso-occlusive retinopathy is usually high-dose systemic corticosteroids. During the treatment period, such visual symptoms as deterioration of vision and visual field defect are indicators of progression of SLE retinopathy. Sub-Tenon’s injection of corticosteroids, steroid-sparing immunosuppressive agents, anticoagulation agents, and panretinal photocoagulation are applied in more severe cases or worse conditions.
We report a rare case of bilateral macular infarction occurring in a patient who was simultaneously diagnosed with SLE. Under treatment with pulse therapy and intravenous steroids, her vision deteriorated progressively. When this was combined with an adjuvant therapy of multiple shots of posterior sub-Tenon’s injection of triamcinolone acetonide (TA), the vision in one eye unexpectedly improved and was maintained at follow-up.
Case report
The 29-year-old female patient suffered from loss of vision in the left eye for 1 week. She came to our ophthalmologic clinic, where best-corrected visual acuity (BCVA) of the right eye was 6/6, and the left was counting fingers at 20 cm. According to the patient, she had been to the rheumatologic clinic, where SLE was diagnosed according to the symptoms of arthralgia over the bilateral fingers and knees for 2–3 months and fever on and off for 1 month. Laboratory testing revealed anemia with a low hemoglobin level of 8.0 g/dL, proteinuria, an antinuclear antibody titer of 1:2,560, anti-double-stranded deoxyribonucleic acid (dsDNA) titer of >400 IU/mL, and an anticardiolipin antibody titer in normal range. Therefore, the diagnosis of SLE was confirmed, and she was treated with oral steroids for a week. In our clinic, the results of the external and anterior segments were unremarkable. Posterior segment examination showed white perivascular exudate in her right eye and multiple patches of cotton-wool spots around the disk and macula in her left eye (Figure 1).
  | Figure 1 There was white perivascular hard exudate (yellow arrow) along the vessels in both eyes, and multiple patches of cotton-wool spots around the disk and macula in her left eye. |
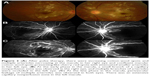
She was admitted to the rheumatology ward for further evaluation and treatment. However, BCVA of the right eye declined to 6/10. Fundus examination showed new multiple soft exudates in the macula, with a small branch of sheathing vessels and perivascular hard exudate along multiple branches in her right eye. Due to progressively worse vision in the right eye, intravenous steroids with methylprednisolone 1,000 mg/day for 3 days were given and then 80 mg/day for 10 days thereafter. Her anti-dsDNA titer regressed from >400 to 90 IU/mL. Arthralgia of the bilateral fingers and knees was resolved. Unfortunately, her right eye vision went down to 6/30 on the 4th day at a dose of 80 mg intravenously, with less perivascular exudate but increasing cotton-wool spots and multiple arterioles narrowing at the macula in her right eye, while her left eye improved to 3/60, with confluent macular cotton-wool spots presenting like cherry-red spots and attenuated smaller arterioles (Figure 2A). Fluorescein angiography (FA) showed an extensive macular nonperfusion area in the left eye (Figure 2B) and a small branch of a capillary nonperfusion zone at the macula in the early phase, with perivascular leakage of multiple arterioles at the late phase in the right eye (Figure 2C). Ocular coherence tomography (OCT) showed localized retina edema with subfoveal fluid in both eyes.
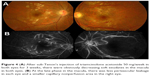
She underwent posterior sub-Tenon’s injections of TA 50 mg per week for 3 weeks in both eyes (Figure 3). Simultaneously, she was given oral antiplatelet medication of pentoxifylline 250 mg twice a day and steroids tapering to 40 mg/day 2 weeks later. Her anti-dsDNA titer regressed from 90 to 45 IU/mL, while her right eye vision gradually improved to 3/6 and the left eye remained at 3/60 after a month of first posterior sub-Tenon’s injections. There was obviously decreasing macular soft exudates in both eyes (Figure 4A), with less perivascular leakage in each eye and a smaller capillary nonperfusion area in the right eye from FA (Figure 4B). OCT showed no more subfoveal fluid and fovea edema in either eye, with macular thinning in the left eye.
  | Figure 3 The relationship of visual acuity and steroid use under sub-tenon injection and intravenous way. |
She kept following up at our clinic, with the dose of oral steroids tapering according to the manifestations of her bilateral posterior segments. BCVA of the right eye upgraded to 6/7.5, and the left eye remained at 3/60 after 6 weeks of first posterior sub-Tenon’s injections. Her bilateral vision was maintained for 4 months. There were no cotton-wool spots over the posterior pole in either eye (Figure 5A), with a smaller nonperfusion area in the right eye (Figure 5B).
Discussion
Retinal disease affects around 10% of patients with SLE. Mild lupus retinopathy showed cotton-wool spots, perivascular hard exudates, retinal hemorrhages and vascular tortuosity.2 Moderately severe cases may have focal or generalized arteriolar constriction and venous tortuosity. In severe groups, there is occlusion of retinal arterioles and consequent retinal infarction, vaso-occlusive retinopathy, or retinal vasculitis.3,4 This means the progression of SLE retinopathy is at first from perivascular hard exudates, then arteriole constriction and finally arteriole occlusion. Microscopically, autoantibodies attacking the walls of arterioles make vascular permeability increase, with presentations of perivascular exudates along vessels and severe vascular leakage on FA. Immune-complex deposition in the arterioles allows intravascular space narrowing. The perivascular neural cells become ischemic, with manifestations of more cotton-wool spots.5,6 FA shows the nonperfusion area. As the arterioles around the macula totally occlude with sheathing vessels, the vision deteriorates irreversibly. Shein et al concluded after reviewing the literature that the visual prognosis of macular ischemia or infarction presenting as the initial sign of SLE with no evidence of elevated anticardiolipin antibody titers tends to be poor, despite treatment with high-dose systemic corticosteroids and noncorticosteroid immunosuppressive agents.7
From our case, the perivascular hard exudation of both eyes was partially resolved, with anti-dsDNA decreasing after pulse therapy. FA revealed continued vascular leakage at the late phase representing high vascular permeability induced by vascular continuous inflammation. However, the cotton-wool spots dispersed over the macular area increased rapidly with worse vision. We supposed that perivascular exudates seemed to be resolved at initial periods by high-dose intravenous steroids through arterioles without occlusion. Accumulation of a large amount of autoantibodies or immune complexes makes intravascular space narrow or totally occluded. Thereafter, the concentration of intravenous steroids could be too low to wash out excessive autoantibodies or the immune complex. The area of the perivascular neural cells short of nutrition and oxygen gradually expands and advances.
Increasing steroid levels over the posterior pole to eliminate excessive autoantibodies or immune complex in the vessels should be achieved. Posterior sub-Tenon’s injection of TA, a long-acting corticosteroid, might be a good adjuvant treatment. Delivery of TA from the posterior sub-Tenon’s space to the extracellular choroidal matrix through transscleral diffusion, demonstrated by Kovacs et al could boost the localized concentration of steroids lasting at least 1 month.8 We assume that increasing steroid density over posterior segments could not only deplete more autoantibodies or immune complexes to widen the narrowing vessels with reversing the condition of ischemia but also relieve the edema of perivascular neural cells and extracellular tissue induced by inflammation simultaneously. For totally occluded vessels with infarction, the situation would be irreversible. With regard to our case, cotton-wool spots over the posterior pole of bilateral eyes became obviously diminished after injections in both eyes. FA showed less vascular leakage in both eyes, with a smaller area of capillary dropout in the right eye. OCT showed resolved subfoveal fluid in both eyes. The vision in the right eye improved, but the left eye remained the same.
As the systemic symptoms of SLE resolved quickly with significant reducing of anti-dsDNA, systemic corticosteroids were considered to taper gradually. However, retinal signs and vision in our case improved gradually; not as fast as the systemic ones. Tapering systemic corticosteroids should be controlled carefully according to the retinal presentations and the visual change, which often parallel the severity of systemic inflammation and may indicate inadequate control of the systemic disease.9 In conclusion, posterior sub-Tenon’s injection of TA is an adjuvant treatment for refractory macular infarction, an uncommon but sight-threatening ocular complication, even if vision is worse after the use of high-dose systemic corticosteroids.
Disclosure
The authors report no conflicts of interest in this work.
References
Read RW. Clinical mini-review systemic erythematosus and the eye. Ocul Immunol Inflamm. 2004;12:87–99. | ||
Coppeto J, Lessel S. Retinopathy in systemic lupus erythematosus. Arch Ophthalmol. 1977;95:794–797. | ||
Jabs DA, Fine SL, Hochberg MC, Newman SA, Heiner GG, Stevens MB. Severe retinal vaso-occlusive disease in systemic lupus erythematosus. Arch Ophthalmol. 1986;104:558–563. | ||
Hall S, Buettner H, Luthra HS. Occlusive retinal vascular disease in systemic lupus erythematosus. J Rheumatol. 1984;11:846–850. | ||
Nag TC, Wadhwa S. Histopathological changes in the eyes in systemic lupus erythematosus: an electron microscope and immunohistochemical study. Histol Histopathol. 2005;20:373–382. | ||
Nag TC, Wadhwa S. Vascular changes of the retina and choroid in systemic lupus erythematosus: pathology and pathogenesis. Curr Neurovasc Res. 2006;3:159–168. | ||
Shein J, Shukla D, Reddy S, Yannuzzi LA, Cunningham ET. Macular infarction as a presenting sign of systemic lupus erythematosus. Retin Cases Brief Rep. 2008;2:55–60. | ||
Kovacs K, Wagley S, Quirk MT, et al. Pharmacokinetic study of vitreous and serum concentrations of triamcinolone acetonide after posterior sub-Tenon’s injection. Am J Ophthalmol. 2012;153:939–948. | ||
Areval JF, Lowder CY, Muci-Mendoza R. Ocular manifestations of systemic lupus erythematosus. Curr Opin Ophhthalmol. 2002;13:404–410. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.