Back to Journals » International Medical Case Reports Journal » Volume 12
Behcet’s Disease Presenting With Bilateral Hypopyon Masquerading Post Cataract Surgery Endophthalmitis
Authors Mohammadpour M, Kosari M, Khorrami-Nejad M
Received 30 September 2019
Accepted for publication 7 November 2019
Published 28 November 2019 Volume 2019:12 Pages 363—365
DOI https://doi.org/10.2147/IMCRJ.S232948
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Mehrdad Mohammadpour, Meysam Kosari, Masoud Khorrami-Nejad
Eye Research Center, Farabi Eye Hospital, Tehran University of Medical Sciences, Tehran, Iran
Correspondence: Mehrdad Mohammadpour
Eye Research Center, Farabi Eye Hospital, Tehran University of Medical Sciences, Tehran, Iran
Tel +98 21 5540 0010
Email [email protected]
Purpose: To report a case of Behcet’s disease presented with bilateral hypopyon after sequential cataract surgery masquerading delayed onset post-operative endophthalmitis.
Methods: A 53-year-old man with a history of sequential uneventful cataract surgeries came to our clinic with decreased vision (0.3 LogMAR) since 2 days ago and bilateral hypopyon in his both eyes. The primary diagnosis was chronic late-onset endophthalmitis.
Results: There was no lid edema or chemosis on the external examination. On slit-lamp examination, the cornea was clear, the pupil was well reactive with no posterior synechia, the intraocular lens was centered with good red reflex, however, bilateral hypopyon was detected in his both eyes which was more prominent in the left eye. The eyes were fairly calm and absence of vitreous reaction on slit-lamp examination, there was no pain and photophobia. Further, on physical examination, oral mucosal ulcerations were detected. His systemic workup revealed Behcet’s disease with HLA-B5 positive serology.
Conclusion: In cases with delayed onset hypopyon following cataract surgery, inflammatory diseases such as Behcet’s disease should be considered. Appropriate history taking and physical examinations in the context of serologic laboratory investigations may lead to the proper diagnosis.
Keywords: Behcet’s disease, bilateral hypopyon, uveitis, cataract surgery
Introduction
Hypopyon refers to a layered inflammation and collection of cells in anterior chamber of the eye and settles inferiorly due to gravitational feature.1 It indicates a severe inflammation of anterior segment of the eye, so its causes are referred to ones related to anterior or panuveitis, that are infectious (bacterial, parasitic, mycotic or viral) or inflammatory.2–7
Hypopyon after cataract surgery can occur in acute or chronic form, which differs in etiology.8,9 It can also be associated with postoperative endophthalmitis. Chronic hypopyon formation usually arises from an infectious process but, less common an inflammatory process had affected eye before surgery.10
Behcet’s disease is a recurrent and multisystem disorder, caused by a chronic vasculitis.7,11 It characterizes with genital ulceration, oral aphthous ulcer, skin eruption and some eye involvements that are the most serious presentation of the disease, causing blindness in some cases,7 so its diagnosis is ascertained by clinical suspicion. In addition to uveitis, Poor visual acuity, posterior synechia, hypotony (intraocular pressure lesser than 5 mm Hg), cataract formation and hypopyon are the most serious ones.1,7,11–13
There are reports on the presence of hypopyon after cataract surgery following endophthalmitis or uveitis, but none of them mentioned about bilateralism. Also, we found no report about Behest’s disease which caused hypopyon formation after cataract surgery.
Case Report
A 53-year-old man with a history of sequential uneventful cataract surgeries came to our clinic with decrease vision since 2 days ago. His visual acuity was 0.3 LogMAR in his both eyes. A written informed consent letter has been signed by the patient to allow any case details and any accompanying images published. Based on our hospital policy, Institutional Review Board (IRB) was not required as it was a case report.
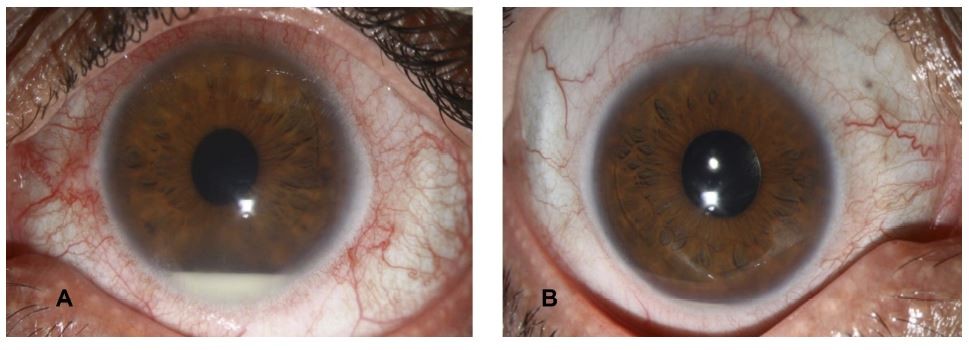
There was no lid edema or chemosis on the external examination. However, a subtle pre-limbal injection was seen that was more prominent in the left eye. On slit-lamp examination, the cornea was clear, the pupil was well reactive with no posterior synechia, the intraocular lens was centered with good red reflex; however, bilateral hypopyon was detected in his both eyes which was more prominent in the left eye (Figure 1). The intraocular pressure was 9 mmHg in his both eyes. The fundus examination was unremarkable.
 |
Figure 1 Bilateral Hypopyon in a pseudophakic patient with Behcet’s disease. (A) Left eye with significant hypopyon. (B) Right eye less hypopyon than left. |
The primary diagnosis was chronic late-onset endophthalmitis. However, as there was no pain and photophobia and the eyes were fairly calm and absence of vitreous reaction on slit-lamp examination, the diagnosis was on debate. Further, on physical examinations, oral mucosal ulcerations and genital aphthosis were detected. This case referred to a rheumatologist, and his systemic workup revealed Behcet’s disease with HLA-B5 positive serology and a higher C-reactive protein (CRP) level. This was the first diagnosis of Behcet’s disease for this patient. The interesting thing about this case was the detection of bilateral hypopyon without any other routine ocular manifestations of Behcet. Infection screening did not perform for this patient because he had no any other signs and symptoms of post-cataract surgery endophthalmitis except bilateral hypopyon. After systemic treatments (corticosteroids to control inflammation) by the rheumatologist, bilateral hypopyon was diminished.
Discussion
Behcet’s disease is a chronic and multisystem disorder which its prevalence differs in various regions.7 Also, it is a global disease, but the majority of incidences are seen along the ancient Silk Road extending from eastern Asia to the Mediterranean basin.7,14,15 The mucocutaneous manifestation is the hallmark of Behcet disease. Recurrent oral aphthae (small, shallow, painful ulcerations that usually affects the oral mucosa) in addition to the same lesions in genital organs lead to considering about this disorder, also the other criteria like uveitis/retinitis and positive pathergy test are demanded for more definite diagnosis.7,16 Also, the pathogenesis remained unknown, but histopathology of Behcet’s disease shows a vasculitis in all-sized vessels (small, medium and large), and it may cause systemic features including arthritis, thrombophlebitis migrans, erythema nodosum, meningoencephalitis, and arterial aneurysms.16,17
A variety of ocular involvement was reported in Behcet’s disease. Anterior uveitis with hypopyon is a rare manifestation and posterior uveitis almost always is a constant involvement. The other manifestations are cataract, glaucoma, retinitis, and retinal edema.7
Matsuo et al in a study with 16 eyes with Behcet’s disease reported that 4 eyes experienced ocular attacks during 1 year after cataract surgery. They showed that experience of ocular attacks after cataract surgery has a significant association with ocular attacks during 1 year before surgery.12
Berker et al reported posterior synechiae formation (17.5% of patients), severe inflammation (12.5%), cystoid macular edema (12.5%), epiretinal membrane (7.5%), and optic atrophy (5%) as the postoperation complications of cataract surgery in patients with Behcet disease.13
We did not find any review article or RCT in the literature including PubMed about the usage of anti-TNF administrations like Infliximab, also some case reports showed that it is safe and effective in patients with Behcet’s disease.18–20
Postoperative endophthalmitis following cataract surgery may occur as acute, subacute or chronic inflammation. We report a 53-year-old man with bilateral hypopyon late after sequential cataract surgeries. According to these presentations with regard to high prevalence and incidence rate of Behcet’s disease in Middle-East region, we report this case for ophthalmologists to be aware about this disease. Our case shows that Behcet’s disease can begin just with ocular involvement like uveitis at first. Therefore, in a country with high prevalence of Behcet’s disease, at any patient with uveitis, this disease should be considered. Early and appropriate therapies can relief the ocular complication of cataract disease in patients with Behcet disease.
To the best of our knowledge, this is the first case report of Behcet’s disease presented with bilateral hypopyon following cataract surgery masquerading delayed onset post-operative endophthalmitis. Relevant history taking and physical examinations in the context of serologic laboratory investigations may lead to proper diagnosis.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Zaidi AA, Ying GS, Daniel E, et al. Hypopyon in patients with uveitis. Ophthalmology. 2010;117(2):366–372. doi:10.1016/j.ophtha.2009.07.025
2. Lee JH, Mi H, Lim R, et al. Ocular autoimmune systemic inflammatory infectious study – report 3: posterior and panuveitis. Ocul Immunol Inflamm. 2019;27(1):89–98. doi:10.1080/09273948.2017.1358377
3. Biswas J. Epidemiology and pathogenesis of uveitis: a review. Indian J Inflamm Res. 2017;21(1):1.
4. Watanabe T, Keino H, Nakayama K, Taki W, Echizen N, Okada AA. Clinical features of patients with diabetic anterior uveitis. Br J Ophthalmol. 2019;103(1):78–82. doi:10.1136/bjophthalmol-2017-311453
5. Sakal M, Takaseb H, Namba K, Mizuuchi K, Iwata D, Ishida S. Two cases of cytomegalovirus panuveitis in immunocompetent patients. Am J Ophthalmol Case Rep. 2018;10:189–191. doi:10.1016/j.ajoc.2018.01.025
6. Hausmann JC, Mans C, Gosling A, et al. Bilateral Uveitis and Hyphema in a Catalina Macaw (Ara ararauna× Ara macao) with multicentric lymphoma. J Avian Med Surg. 2016;30(2):172–179. doi:10.1647/2015-105
7. Saadoun D, Wechsler B. Behcet’s disease. Orphanet J Rare Dis. 2012;7(1):20. doi:10.1186/1750-1172-7-20
8. Hunter JW. Early postoperative sterile hypopyons. Br J Ophthalmol. 1978;62(7):470–473. doi:10.1136/bjo.62.7.470
9. Agarwal A, Testi I, Singh A, Gupta V. Differential diagnosis of hypopyon uveitis. The Uveitis Atlas. 2019;1–8.
10. Wejde G, Montan P, Lundstrom M, Stenevi U, Thorburn W. Endophthalmitis following cataract surgery in Sweden: national prospective survey 1999-2001. Acta Ophthalmol Scand. 2005;83(1):7–10. doi:10.1111/j.1600-0420.2005.00377.x
11. Citirik M, Berker N, Songur MS, Soykan E, Zilelioglu O. Ocular findings in childhood-onset Behcet disease. J Aapos. 2009;13(4):391–395. doi:10.1016/j.jaapos.2009.04.016
12. Matsuo T, Takahashi M, Inoue Y, Egi K, Kuwata Y, Yamaoka A. Ocular attacks after phacoemulsification and intraocular lens implantation in patients with Behcet disease. Ophthalmologica. 2001;215(3):179–182. doi:10.1159/000050854
13. Berker N, Soykan E, Elgin U, Ozkan SS. Phacoemulsification cataract extraction and intraocular lens implantation in patients with Behcet’s disease. Ophthalmic Surg Lasers Imaging. 2004;35:215–218. doi:10.3928/1542-8877-20040501-08
14. Welsh JP, Skvarka CB, Ko C, Cusack CA. Mystery of the silk road. Am J Med. 2007;120(4):322–324. doi:10.1016/j.amjmed.2006.11.007
15. Rosenbaum JT. New developments in uveitis associated with HLA B27. Curr Opin Rheumatol. 2017;29(4):298–303. doi:10.1097/BOR.0000000000000403
16. Ozen S. The spectrum of vasculitis in children. Best Pract Res Clin Rheumatol. 2002;16(3):411–425. doi:10.1053/berh.2002.0237
17. Erkan F, Gul A, Tasali E. Pulmonary manifestations of Behcet’s disease. Thorax. 2001;56(7):572–578. doi:10.1136/thorax.56.7.572
18. Handa T, Tsunekawa H, Zako M. Cataract surgery in Behcet’s disease patients one week after infliximab administration. Case Report Ophthalmol. 2011;2(2):176–178. doi:10.1159/000329091
19. Noda E, Yamanishi S, Shiraishi A, Ohashi Y. Cataract surgery under infliximab therapy in a patient with Behcet’s disease. J Ocul Pharmacol Ther. 2009;25(5):467–470. doi:10.1089/jop.2009.0054
20. Sakai T, Kanetaka A, Noro T, Tsuneoka H. Intraocular surgery in patients receiving infliximab therapy for Behcet disease. Jpn J Ophthalmol. 2010;54(4):360–361. doi:10.1007/s10384-010-0824-y
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
