Back to Journals » Local and Regional Anesthesia » Volume 14
Anatomic Landmark Technique Thoracic Paravertebral Nerve Block as a Sole Anesthesia for Modified Radical Mastectomy in a Resource-Poor Setting: A Clinical Case Report
Authors Zemedkun A , Destaw B, Milkias M
Received 16 November 2020
Accepted for publication 30 December 2020
Published 14 January 2021 Volume 2021:14 Pages 1—5
DOI https://doi.org/10.2147/LRA.S291308
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Stefan Wirz
Abebayehu Zemedkun, Belete Destaw, Mesay Milkias
Department of Anesthesiology, College of Medicine and Health Science, Dilla University, Dilla, Ethiopia
Correspondence: Abebayehu Zemedkun
Department of Anesthesiology, College of Medicine and Health Science, Dilla University, PO Box 419/13, Dilla, Ethiopia
Tel +251900053426
Email [email protected]
Abstract: Mastectomy is mostly performed as definitive management for resectable breast cancer. Implementing paravertebral nerve block for patients with metastasis features of cancer to lungs and other organs, patients with co-morbidity, geriatrics, and malnourished individuals will eliminate the risks and complications of general anesthesia. Though thoracic paravertebral block is an established technique as postoperative pain management for breast surgery, there is no conclusive evidence on its use as a sole anesthetic for modified radical mastectomy. In this case report, we present a 33-year-old woman who underwent a successful modified radical mastectomy for stage IIIb breast cancer associated with clinical and radiological features of metastasis to the lung under a multiple injection landmark technique paravertebral nerve block. We believe that the anatomic landmark technique paravertebral nerve block can be used as an alternative anesthetic technique for modified radical mastectomy in a resource-limited setting for patients who are expected to have a high risk of perioperative complications under general anesthesia.
Keywords: mastectomy, breast cancer, paravertebral block, metastasis, landmark technique
Introduction
The incidence of breast cancer (BC) in the last decades has increased dramatically. Mastectomy is mostly performed as definitive management of resectable BC, but it is frequently associated with perioperative complications like nausea, vomiting, and pain which in turn leads to prolonged hospital stay, increase risk of hospital-acquired infections, and associated treatment costs.1–4
General anesthesia (GA), which is the frequently used type of anesthesia for breast surgery, is considered as the main cause of perioperative complications, and the risk of nausea and vomiting is estimated to be 50%. Thoracic paravertebral block (TPVB) is one of the options for intraoperative and postoperative pain management for patients who undergo breast surgery. Besides, it has been associated with a shorter duration of hospital stay and decreased postoperative opioid requirement compared to GA. Furthermore, studies also suggested that TPVB attenuates perioperative immunosuppression and decrease cancer metastasis.1,5
A thoracic paravertebral nerve block is a form of regional anesthesia that provides ipsilateral somatosensory and sympathetic nerve block by injecting local anesthetics in the paravertebral space, near to the point where spinal nerves emerge from intervertebral foramina.1,6
The anatomic landmark technique TPVB involves eliciting loss of resistance. At the appropriate dermatome under aseptic precautions, the nerve block needle is inserted 2.5–3 cm lateral to the most cephalad aspect of the spinous process and advanced perpendicular to the skin in all planes to contact the transverse process. The needle is then withdrawn to the skin and reintroduced 1 cm beyond the transverse process until a loss of resistance is felt, allowing the positioning of the needle past the transverse process. After gentle aspiration, local anesthetic will be injected6 (Figure 1). The median skin-to-paravertebral depth has been demonstrated to be 55.0 mm, with the depth being greater at the upper (T1–T3) and lower (T9–T12) thoracic levels. However, body mass index has been shown to significantly affect the skin-to-paravertebral depth at these levels.7
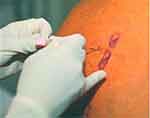 |
Figure 1 Technique of paravertebral block. |
Ultrasound-guided TPVB has shown that it is a promising option for mastectomy in providing a comfortable surgical field.5 Implementing regional anesthesia techniques like a paravertebral block for patients with metastasis features of cancer to lungs and other organs, patients with co-morbidity, geriatrics, and malnourished individuals eliminate the risks and complications of GA and decreases patient morbidity and mortality. Also, it has the advantage of a better hemodynamic profile, early ambulation, and shorter hospital stay. Though TPVB is an established technique as postoperative pain management for breast surgery, there is no conclusive evidence on its use as sole surgical anesthesia for modified radical mastectomy.5,8,9 In this report, we present perioperative management of a patient with breast cancer with evidence of metastasis to the lungs, and who had undergone a modified radical mastectomy (MRM) under TPVB using an anatomic landmark multiple injection technique as sole intraoperative anesthesia. This report adheres to the applicable CARE checklist.
Case Presentation
A 33-year-old female patient (35 kilograms and 155 centimeters) was presented with a right side breast lump of 01 year duration associated with shortness of breath, cough, chest pain, and significant weight loss. Stage IIIB breast cancer was diagnosed and she was scheduled for Modified radical mastectomy (MRM). On presentation, her vital signs were: blood pressure (BP), 110/70mmHg; pulse rate (PR), 84beat/min; respiratory rate (RR), 18breath/min, and oxygen saturation (SPO2), 97%. She had a previous history of surgery 02 years back for the same indication which was excised under local infiltration because the lump was small in size and mobile; otherwise, she had no history of previous medical illness and medication. In the past 01 years, the mass again started to grow progressively to attain the current size. Also, the patient started to complain of shortness of breath, cough, and chest pain with significant weight loss.
On physical examination, there was a 4×4 cm and 6×4 cm sized lump which was hard, irregular, immobile, and febrile to touch and was fixed to the chest wall. Her preoperative metabolic equivalent of tasks was greater than six. Chest examination revealed a decreased air entry in the lower 1/3 of both lung fields. Otherwise, there was no pertinent finding on cardiovascular and other systemic examinations. A thorough preoperative airway assessment was done and she had Mallampati class III, thyromental distance of 7 cm, and a jaw slide of class A.
Summary of Preoperative Laboratory findings; Complete Blood Count: hemoglobin, 12.3g/dl; hematocrit, 39.5%; White Blood Cell, 5.37 ×103 cells/L, platelet count, 522×103 cells/L. Fine needle aspiration cytology (FNAC): 4×3 and 5×5 cm firm to hard mass over the right inner quadrant of the breast, the largest is fixed to the chest wall. Bilateral Breast Ultrasound: The right upper and mid quadrant mammary zones revealed an irregular border of approximately 8×6 cm hypoechoic mass which confirmed the diagnosis of breast cancer. Postero-anterior Chest X-ray: There was left lower and mid lung zone air space opacity with bilateral scattered pulmonary nodules showing a possible metastasis (given primary malignancy). Electrocardiography (ECG) was normal and renal and liver function tests were within the normal range. The coagulation profile of the patient was not determined because the service is not available in our center. However, the patient was assessed clinically by any history of bleeding tendency and by platelet count.
Preoperatively, a risk-benefit analysis of doing and deferring the surgery was discussed in detail between the general surgeon and the consultant anesthetist in charge since there was no oncologist in our center. The patient and her family were involved in the decision-making process. Finally, it was decided to operate the procedure, and to start chemotherapy thereafter. Since the cancer was metastasized to the lungs and the patient was emaciated and could not tolerate general anesthesia, the surgical team decided to perform the surgical procedure under TPVB alone. Then, written informed consent was obtained for both surgery and anesthesia as per the hospital’s protocol.
The patient was premedicated with paracetamol (1 gm), dexamethasone (8 mg). The available standard monitors (NIBP, Pulse oximetry, Capnograph, and ECG) were attached and the values for baseline vital signs were within the normal range (BP=115/70mmHg, PR=88 beat/min, RR=18breath/min, and SPO2=95%).
In the sitting position, the needle insertion sites were marked 2.5 cm lateral to the spinous processes of T3, T5, and T7 for right side anatomic landmark technique TPVB. The site was cleaned using iodine and alcohol. After giving 100 mcg of intravenous fentanyl and local infiltration of the site of needle insertion by 2% plain lidocaine, a 21 gauge × 50-millimeter nerve block needle was introduced perpendicularly at each marked site. When the tip of the needle encountered the transverse process, it was redirected cephalad, and immediately after appreciating the loss of resistance the local anesthetic agent was injected. The block was done by a consultant anesthetist using 5 mL of 0.5% isobaric bupivacaine at each level (a total of 15 mL). Twenty minutes after the block, the extent of the sensory loss was assessed by pinprick testing, and it was successful that the surgical procedure started. Ketamine 30 mg and propofol 30 mg were given intravenously to relieve anxiety. Oxygen, 3 L/min was delivered via nasal prong throughout the procedure. There was no significant derangement in vital signs during incision and intraoperative time.
Modified radical mastectomy was done successfully without any apparent anesthesia or surgery-related complication. The total duration of surgery and anesthesia was 90 and greater than 120 minutes, respectively. The total surgical blood loss was about 600mL and the patient was transfused 01 unit of cross-matched whole blood. During the intraoperative time, 1000 mL of normal saline was infused and her total urine output was 350 mL. Postoperatively, she was followed at the post-anesthesia care unit (PACU) for the first two hours, and then at the surgical ward until she was discharged to home. The whole postoperative period was uneventful, and she is on continuous follow up for chemotherapy.
Discussion
In the developing world, mastectomy is the primary option in the management of resectable breast cancer. Usually, it can be the only treatment modality due to limited resource capacity for the adjuvant treatment options.10 Data from east Africa showed that more than 99% of breast cancer patients undergo a mastectomy due to lack of other treatment options.3
Although TPVB and GA are often combined for modified radical mastectomy, for some patients GA is either contraindicated or undesirable due to factors including frailty, co-morbidities, anxiety, and patient choice.11 In our case, since the breast cancer had metastasized to the lungs and the patient was emaciated, it was better to avoid general anesthesia; a decision was made to perform the surgery using multiple injection TPVB as it decreases the possible intraoperative and postoperative complications associated with general anesthesia.
Regional anesthesia (RA) options for breast surgery include TPVB, epidural anesthesia, and an intercostal nerve block. Epidural and TPVB blocks are commonly performed as intraoperative anesthesia or analgesia and post-mastectomy pain control.9 An epidural kit was not available in our set up so that we considered TPVB as the only option we could utilize in our case. For breast surgery, a paravertebral block is usually performed between thoracic spinal nerves two (T2) and six (T6) with either single or multiple injection techniques. It can be performed in lateral, sitting, or prone position using anatomic landmark technique or ultrasound guidance. Though it is an established technique as postoperative pain management for breast surgery, there is no conclusive evidence on the use of anatomic landmark technique TPVB as a sole surgical anesthesia for modified radical mastectomy in resource-constrained settings.6,12 This technique is associated with a superior analgesic profile for patients who undergo a unilateral or bilateral mastectomy with a lower incidence of postoperative nausea and vomiting and decreased length of hospital stay.1 Having these scientific grounds in mind and reports on the effectiveness of ultrasound-guided paravertebral block for mastectomy, we decided to perform the surgical procedure in our case under landmark technique TPVB. A senior anesthetist with experience of doing the block for different surgical procedures had performed the procedure successfully.
Thoracic paravertebral block for mastectomies has shown that it is a promising option in providing a comfortable surgical field in addition to reducing the complications and risks of GA. Furthermore, it is associated with minimal hemodynamic instability, early discharge from hospital with reduced cost of the treatment.5 In almost all of these cases, the block was performed under ultrasound guidance which benefits of direct visualization of the needle, local anesthetic (LA) spread and the pleura. Besides, in some of the cases, a continuous epidural catheter was inserted into the paravertebral space.9,11–13 In our case, the block was performed by landmark technique without a catheter since ultrasound and epidural catheter was not available.
Cooperation and communication between surgeon, anesthetist, and oncologist are very important in enhancing cancer patient’s surgical outcome.14 In our setup, detail risk-benefit analysis was done only by the consultant anesthetist and the general surgeon with experience of more than 6 years in their field since there is no oncologist.
Conclusion
We presented a woman who underwent a successful modified radical mastectomy under multiple injection landmark technique TPVB. She was diagnosed with stage IIIb breast cancer with clinical and radiological features of metastasis to the lung. We believe anatomic landmark technique TPVB can be used as an alternative anesthesia technique for MRM in resource-limited settings for patients who have a high risk of perioperative complication under general anesthesia.
Abbreviations
BC, breast cancer; CARE, case report; ECG, electrocardiography; GA, general anesthesia; LA, local anesthetic; MRM, modified radical mastectomy; SpO2, peripheral arterial oxygen saturation; TPVB, thoracic paravertebral block.
Data Sharing Statement
Data is available on request.
Ethics Statement
This case report has been exempted by the Institutional Review Board of Dilla University College of Medicine and Health Science from requiring ethical approval.
Consent for Publication
Informed, written consent for the publication of this data was obtained from the patient. No institutional approval was required to publish the case details.
Acknowledgment
We would like to thank the staff of the department of anesthesia and surgery for their professional and technical support.
Funding
There was no source of funding for this case report.
Disclosure
The authors declare no conflicts of interest in this work.
References
1. Cassi LC, Biffoli F, Francesconi D, Petrella G, Buonomo O. Anesthesia and analgesia in breast surgery: the benefits of peripheral nerve block. Eur Rev Med Pharmacol Sci. 2017;21(6):1341–1345.
2. Dagne S. Assessment of breast cancer treatment outcome at Tikur Anbessa Specialized Hospital Adult Oncology Unit, Addis Ababa, Ethiopia. Eur J Oncol Pharm. 2019;2(February):1–8.
3. Edge J, Buccimazza I, Cubasch H, Panieri E. The challenges of managing breast cancer in the developing world - A perspective from sub-Saharan Africa. South African Med J. 2014;104(4):377–379. doi:10.7196/samj.8249
4. Abebe E, Demilie K, Lemmu B, Abebe K. Female Breast Cancer Patients, Mastectomy-Related Quality of Life: experience from Ethiopia. Int J Breast Cancer. 2020;2020:6. doi:10.1155/2020/8460374
5. Kulkarni KRR. Single Needle Thoracic Paravertebral Block with Ropivacaine and Dexmeditomidine for Radical Mastectomy: experience in 25 Cases. Int J Anesthesiol Pain Med. 2016;2(1):1–6. doi:10.21767/2471-982X.100013
6. Warltier DC. Thoracic Paravertebral Block. Anesthesiology. 2001;95(3):771–780. doi:10.1097/00000542-200109000-00033
7. Naja MZ, Gustafsson AC, Ziade MF, et al. Distance between the skin and the thoracic paravertebral space. Anaesthesia. 2005;60(7):680–684. doi:10.1111/j.1365-2044.2005.04232.x
8. Garg R. Regional anaesthesia in breast cancer: benefits beyond pain. Indian J Anaesth. 2017;61(5):369–372. doi:10.4103/ija.IJA
9. Il PS, Kim Y, Han KC, Lee SY, Youn AM, Yoon SH. Thoracic paravertebral block for breast surgery in a pregnant woman. Korean J Anesth. 2010;59:73–76. doi:10.4097/kjae.2010.59.S.S73
10. Sengal AT, Mufunda J. Breast cancer clinicopathological presentation, gravity and challenges in Eritrea, East Africa: management practice in a resource-poor setting. South African Med J. 2013;103:8. doi:10.7196/samj.6829
11. Santonastaso DP, de Chiara A, Russo E, et al. Single shot ultrasound-guided thoracic paravertebral block for opioid-free radical mastectomy: a prospective observational study. J Pain Res. 2012;12:2701–2708. doi:10.2147/JPR.S211944
12. Coveney E, Weltz CR, Greengrass R, et al. Use of paravertebral block anesthesia in the surgical management of breast cancer experience in 156 Cases. Ann Surg. 1998;227(4):496–501. doi:10.1097/00000658-199804000-00008
13. Simpson J, Ariyarathenam A, Dunn J, Ford P. Breast Surgery using thoracic paravertebral blockade and sedation alone. Anesthesiol Res Pract. 2014;2014:4. doi:10.1155/2014/127467
14. Gudaitytė J. Anaesthetic challenges in cancer patients: current therapies and pain management. ACTA MEDICA Litu. 2017;24(2):121–127.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
