Back to Journals » Open Access Journal of Contraception » Volume 10
The Association of Public Insurance with Postpartum Contraception Preference and Provision
Authors Verbus E, Ascha M , Wilkinson B, Montague M , Morris J, Mercer BM, Arora KS
Received 16 September 2019
Accepted for publication 7 December 2019
Published 19 December 2019 Volume 2019:10 Pages 103—110
DOI https://doi.org/10.2147/OAJC.S231196
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Igal Wolman
Emily Verbus,1 Mustafa Ascha,2 Barbara Wilkinson,1 Mary Montague,1 Jane Morris,3 Brian M Mercer,3 Kavita Shah Arora3
1School of Medicine, Case Western Reserve University, Cleveland, OH, USA; 2Cleveland Institute for Computational Biology, Case Western Reserve University, Cleveland, OH, USA; 3Department of Obstetrics and Gynecology, MetroHealth Medical Center, Cleveland, OH, USA
Correspondence: Kavita Shah Arora
Department of Obstetrics and Gynecology, MetroHealth Medical Center, 2500 MetroHealth Drive, Cleveland, OH 44109, USA
Tel +1 216-778-4444
Fax +1 216-778-8642
Email [email protected]
Background: Prior studies have noted that public insurance status is associated with increased uptake of postpartum contraception whereas others have pointed to public insurance as a barrier to accessing highly effective forms of contraception.
Objective: To assess differences in planned method and provision of postpartum contraception according to insurance type.
Study Design: This is a secondary analysis of a retrospective cohort study examining postpartum women delivered at a single hospital in Cleveland, Ohio from 2012–2014. Contraceptive methods were analyzed according to Tier-based effectiveness as defined by the Centers for Disease Control and Prevention. The primary outcome was postpartum contraception method preference. Additional outcomes included method provision, postpartum visit attendance, and subsequent pregnancy within 365 days of delivery.
Results: Of the 8281 patients in the study cohort, 1372 (16.6%) were privately and 6990 (83.4%) were publicly insured. After adjusting for the potentially confounding clinical and demographic factors through propensity score analysis, public insurance was not associated with preference for a Tier 1 versus Tier 2 postpartum contraceptive method (matched adjusted odds ratio [maOR] 0.89, 95% CI 0.69–1.15), but was associated with a preference for Tier 1/2 vs Tier 3/None (maOR 1.41, 95% CI 1.17–1.69). There was no difference between women with private or public insurance in terms of method provision by 90 days after delivery (maOR 0.94, 95% CI 0.75–1.17). Public insurance status was also associated with decreased postpartum visit attendance (maOR 0.54, 95% CI 0.43–0.68) and increased rates of subsequent pregnancy within 365 days of delivery (maOR 1.29, 95% CI 1.05–1.59).
Conclusion: Public insurance status does not serve as a barrier to either the preference or provision of effective postpartum contraception. Women desiring highly- or moderately effective methods of contraception should have these methods provided prior to hospital discharge to minimize barriers to method provision.
Keywords: postpartum contraception, disparities, insurance, Medicaid, sterilization, LARC
Introduction
The postpartum period is a key time to initiate contraception to prevent unintended, short-interval pregnancies that can lead to maternal and neonatal complications as well as family stressors.1–3 For this reason, provision of postpartum contraception is recommended by the World Health Organization and the American College of Obstetricians and Gynecologists (among other societies) as a component of quality postpartum care.4,5 However, multiple barriers exist to the patient obtaining postpartum contraception including financial barriers, stress of parenting, systemic racial inequities, physician practice and conscientious refusal, and lack of patient knowledge.6–11 Whether insurance coverage is one of these external barriers impacting postpartum contraceptive method choice and provision is unclear. Several studies have noted that Medicaid insurance status is associated with increased uptake of postpartum contraception whereas others have pointed to Medicaid insurance as a barrier to accessing highly effective forms of contraception.8,12–15 Many of these studies were completed prior to passage of the Affordable Care Act and Medicaid expansion which may impact findings given improved contraceptive coverage and thus a presumed reduction in external barriers to access.
Yet, while improved contraceptive coverage due to the Affordable Care Act may have reduced some external barriers to postpartum contraception, it is also ethically and clinically important to understand and uphold the differences in individual patient wishes for future reproduction and pregnancy prevention.16 Even when financial barriers are minimized, contraceptive choice among women will vary based on their individual preferences and these may not be solely based on method effectiveness.17 For example, in one large study in a population with universal healthcare coverage and thus presumed removal of financial barriers to contraceptive preference and access, only 23.4% of women chose and obtained the highly effective methods of either long-acting reversible contraception (LARC) or sterilization with 36.8% declining any form of contraception in the postpartum period.18 Therefore, presuming the ideal postpartum contraceptive method based solely on clinical effectiveness does not fully recognize the autonomous choice of the patient and her reproductive goals.19 Further, women with public versus private insurance have important differences in terms of clinical and demographic factors that are known to impact contraceptive choice such as age, race/ethnicity, parity, and breastfeeding status.20–23
Therefore, it is unclear whether prior reported disparities in postpartum contraceptive plan and access based on insurance status remain. Better understanding the factors that impact choice of contraceptive method and barriers to method provision is necessary to provide optimal access to the patient’s preferred method of postpartum contraception. The primary objective of this study was to assess differences in method preference and provision of postpartum contraception according to insurance type. We hypothesized that patients with private insurance would be more likely to desire and obtain highly effective methods of contraception such as LARC and sterilization even after accounting for differences in clinical and demographic factors such as age, parity, gestational age, adequacy of prenatal care, route of delivery, race/ethnicity, marital status, and education.
Materials and Methods
This is a planned secondary analysis of women from a retrospective single-site cohort study involving all (8654) women at our urban, tertiary-care, academic hospital in Cleveland, Ohio who delivered at or beyond 20 weeks of gestation from January 1, 2012, and December 31, 2014. The goal of the primary analysis was to understand differences in postpartum sterilization plan preference and provision for women with public versus private insurance. For this analysis, the cohort was restricted to women who had either private or public (Medicaid, Medicare, or Tricare/Champus) insurance. Those without insurance, who had a previous sterilization, and those with a peripartum mortality were excluded (Figure 1). Full methodological details have been previously published.24 Briefly, the linked outpatient and inpatient electronic medical record for each subject was reviewed.
 |
Figure 1 Flow chart of the study population. |
We recorded contraceptive method preference at the time of hospital discharge as our primary outcome. All study subjects had a postpartum contraceptive plan documented in the electronic medical record in either the discharge delivery summary or inpatient postpartum daily progress notes. Contraceptive methods were categorized for analysis into four Tiers (Tier 1, Tier 2, Tier 3, and None) based on the Centers for Disease Control and Prevention’s Model of Tiered Contraceptive Effectiveness.25 Tier 1 included LARC as well as both female and male sterilization. Tier 2 included injectables, pills, patch, and vaginal ring. Tier 3 included barrier methods, fertility awareness, withdrawal, and abstinence. None included both no method of contraception as well as lactational amenorrhea since it is not considered effective for the full 12 months that was used to define the study outcome of subsequent pregnancy. Fewer than 10% of our patient population is exclusively breastfeeding at time of the outpatient six-week postpartum visit.
The primary outcome of contraceptive method preference by insurance status was compared between Tier 1 and Tier 2 methods to assess preference differences between highly effective methods that were invasive versus moderately effective methods that were non-invasive. We also compared by insurance status between Tier 1/2 and Tier 3/None to understand differences between those preferring high/moderate effectiveness versus lower effectiveness methods that do not require provider involvement. We felt choosing these two comparisons, rather than the six total comparisons if each Tier was compared individually, best represented the contraceptive counseling practices of providers toward a highly- or moderately effective method of contraception. Secondary outcomes included method provision, postpartum visit attendance, and subsequent pregnancy within 365 days of delivery. We defined contraceptive method provision as sterilization completion (either inpatient postpartum or as an interval procedure), LARC placement (interval placement), prescription of a short-acting method (either inpatient prior to discharge or at the outpatient postpartum visit), or patient’s report of use of a non-prescription method such as condom. Inpatient postpartum LARC was not available at our hospital (or any other hospital in our region) at the time of this study. Provision was reported as a binary outcome if it occurred within 90 days of delivery. Postpartum visit attendance by 90 days postpartum was recorded. Ninety days were used given our institutional policy to schedule the outpatient postpartum visit at six weeks after delivery, thus allowing additional time for service recovery and the separate scheduling for LARC insertion or sterilization surgery (as was our institution’s practice at the time of the study). Finally, the occurrence of subsequent pregnancy within 365 days of delivery was identified from documentation in our electronic medical record. Subsequent pregnancy was defined as either positive urine or serum pregnancy test, presentation for prenatal care, or notation of pregnancy care at an outside hospital in our hospital’s clinical documentation.
Insurance status was analyzed as private versus public (Medicaid, Medicare, and Champus/Tricare). The covariates of maternal age at delivery in years, parity at admission, gestational age at delivery in weeks, number of prenatal visits, delivery type, race/ethnicity, marital status, and education level were recorded. Adequate prenatal care was defined as six or more prenatal visits.26 The prespecified demographic and clinical variables listed above were calculated across insurance status using t-tests and χ2 tests for continuous and proportional outcomes, respectively. Two hundred fifty-three (2.9%) for adequate prenatal care, 196 (2.3%) for marital status, and 337 (3.9%) for education level were missing data. The remainder of covariates had no missing data. We had complete data for 7934 (91.7%) of records. For multiple comparisons of tier preference across insurance status, the Holm-Bonferroni correction was used to identify differences in proportions. The outcomes of contraceptive plan preference, provision, postpartum visit attendance, and subsequent pregnancy were analyzed via propensity score analysis. Propensity score matching was used to account for the differences in subject allocation to either public or private insurance providers. All covariates listed above were prespecified for inclusion as potential confounders in contraceptive choice. Propensity score analysis for subsequent pregnancy was calculated both with and without postpartum contraceptive plan provision as an additional covariate given the potential confounding effect. Nearest-neighbors matching was used with a 1:1 ratio of private to public-insured subjects, without replacement. Multiple imputation by chained equations was performed to impute missing data. All tests were two-tailed, and an α of 0.05 was used to define statistical significance.
Analyses for this study were performed using R Version 3.4.0.27 This study was approved by the institutional review board of MetroHealth Medical Center in Cleveland, Ohio. A waiver for written informed consent was granted from our IRB given this research represented de-identified analysis of retrospective data available in the medical record. The study was conducted in accordance with the principles of the Declaration of Helsinki.
Results
Of the 8281 patients in the study cohort, 1372 (16.6%) were privately insured and 6990 (83.4%) were publicly insured (Table 1). Five hundred twenty of 6926 (7.5%) women with public insurance had Medicare insurance, 21 (0.4%) had Champus/Tricare, and the remaining 6385 (92.2%) had Medicaid insurance. There were differences in age, parity, gestational age at delivery, adequacy of prenatal care, route of delivery, race/ethnicity, marital status, and education level across insurance groups. Overall, those with private insurance tended to be older, less parous, of white race, married, and college-educated. Women with private insurance also tended to deliver at a later gestational age, have adequate prenatal care, and deliver via cesarean section.
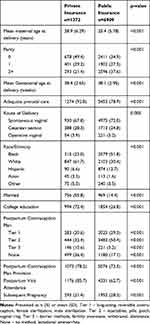 |
Table 1 Clinical/Demographic Differences and Postpartum Contraception Plan Preference Differences Among Women with Private versus Public Insurance |
Women with private versus public insurance differed in postpartum contraceptive method preference at the time of discharge when analyzed across Tiers. Privately insured women preferred Tier 1 and Tier 2 methods less often and Tier 3 methods more often than women with public insurance (Tier 1, 20.6% vs 29.3%; Tier 2, 32.4% vs 50.4%; Tier 3, 10.6% vs 3.2%; p <0.001 for private and public insurances, respectively). Women with private insurance were also more likely to prefer no method of postpartum contraception than women with public insurance (36.4% vs 17.1%, p <0.001) (Table 1).
The univariable and multivariable outcomes of postpartum contraceptive plan preference, provision, postpartum visit attendance, and subsequent pregnancy within 365 days of delivery after propensity score analysis to adjust for potentially confounding factors are shown in Table 2. There was no difference in frequency of plan for Tier 1 versus Tier 2 postpartum contraception at time of discharge between those with private versus public insurance after adjusting for maternal age, parity, gestational age, adequacy of prenatal care, delivery type, race/ethnicity, marital status, and education level (matched adjusted odds ratio [maOR] 0.89, 95% CI 0.69–1.15). Conversely, women with public versus private insurance preferred Tier 1/2 versus Tier 3/No method after controlling for other factors (maOR 1.41, 95% CI 1.17–1.69). There was no difference between insurance types in postpartum contraception plan provision by 90 days after delivery (maOR 0.94, 95% CI 0.75–1.17). However, women with public insurance were less likely to attend their outpatient postpartum visit (maOR 0.54, 95% CI 0.43–0.68) and more likely to have a subsequent pregnancy within 365 days of delivery (maOR 1.29, 95% CI 1.05–1.59) if contraceptive plan provision was not taken into account. Even after accounting for contraceptive plan provision as an additional covariate, there remained a difference in subsequent pregnancy within 365 days of delivery based on insurance status (maOR 1.27, 95% CI 1.03–1.56).
Discussion
There are significant differences in the population of patients insured by private versus public insurance at our hospital in terms of clinical and demographic factors. Many of these factors are associated with contraceptive preference, access to care, and unintended pregnancy rates.17,21,28–30 After adjusting for these relevant factors (maternal age, parity, gestational age, adequacy of prenatal care, delivery type, race/ethnicity, marital status, and education level), private versus public insurance status was not associated with a difference in plan for highly effective (Tier 1) versus moderately effective (Tier 2) method for postpartum contraception or plan provision within 90 days of delivery, contrary to our initial hypothesis.
Women with public compared with private insurance were more likely to choose a highly- or moderately effective versus Tier 3/No method for postpartum contraception. It is unclear whether this difference is due to patient-mediated or physician-level factors prompting differences in contraceptive plan preference. Patient-mediated factors include potential differences in future pregnancy intention between the two groups. However, women choose contraceptive methods based on multiple factors in addition to simply effectiveness; therefore, future pregnancy intention and choice of postpartum contraception method are not always linked.17,31 Physician-level factors may include potential implicit bias in counseling based on clinical, demographic, and insurance-based differences as well as practice pattern differences between individual providers.32–34 Regardless of the reason for these differences in preference, barriers to the provision of the desired contraceptive plan should be minimized.
Public insurance status was associated with decreased rates of postpartum visit attendance and increased rates of subsequent pregnancy within 365 days of delivery in our study, similar to the published literature.35–37 Known racial/ethnic variation in rates of contraceptive failure, adherence, discontinuation, and pregnancy planning and intendedness may have impacted our findings.38–43 Therefore, ideally, women desiring highly- or moderately effective methods of contraception should have these methods provided prior to hospital discharge. However, carefully nuanced contraceptive counseling is needed to ensure that patients receive accurate medical counseling regarding the risks of short-interval pregnancy without the assumption that patients themselves will similarly devalue short-interval pregnancy in terms of their own reproductive planning.
Our study is limited by its retrospective nature and potential loss to follow up. Women who did not return for postpartum visits may have received care elsewhere or outside of the 90-day window we considered for the outcome of provision. Future pregnancy intention was not measured which may impact the choice of postpartum contraceptive method. Additionally, as a single-center study, contraceptive practices and barriers related to our institution’s policies, practices, patient characteristics may limit generalizability of our results. For example, during the study timeframe, we did not generally perform same-day LARC insertion at time of the postpartum visit. As a county hospital that serves primarily the underserved, most of our patients remain Medicaid-eligible after the pregnancy-related coverage expires. Bearing in mind that this study is a secondary analysis, observational in nature, and odds ratios for outcomes are within the zone of potential bias, results should be interpreted with caution.
Implications for Practice and/or Policy
Better understanding patient decision-making regarding postpartum contraception is imperative to reducing external barriers to care and eradicating disparities in contraceptive and reproductive health outcomes. Prospective, longitudinal assessment of pregnancy intention, contraceptive goals, factors considered in method choice, sources of information, effect of insurance coverage, role of physician counseling, and impact of the social and medical environment on contraceptive decision-making is necessary.
Conclusions
In conclusion, after accounting for confounding clinical and demographic factors, public insurance does not serve as a barrier to effective postpartum contraceptive method preference or provision. Women with public insurance were more likely to plan on either a highly or moderately effective method of postpartum contraception at time of hospital discharge than those with private insurance. Strategies to individualize contraceptive counseling and planning surrounding future pregnancies are necessary.
Disclosure
Dr. Arora is funded by the Clinical and Translational Science Collaborative of Cleveland, KL2TR0002547 from the National Center for Advancing Translational Sciences (NCATS) component of the National Institutes of Health and NIH roadmap for Medical Research. This manuscript is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. The authors report no other conflicts of interest.
References
1. Hanley GE, Hutcheon JA, Kinniburgh BA, Lee L. Interpregnancy interval and adverse pregnancy outcomes: an analysis of successive pregnancies. Obstet Gynecol. 2017;129:408–415. doi:10.1097/AOG.0000000000001891
2. Shree R, Cuaghey AB, Chandrasekaran S. Short interpregnancy interval increases the risk of preterm premature rupture of membranes and early delivery. J Matern-Fetal Neo Med. 2017;2:1–17.
3. Jansa V, Blickstein I, Lucovnik M, Fabjan-Vodusek V, Verdenik I, Tul N. The impact of inter-pregnancy interval on subsequent risk of preterm birth. J Matern-Fetal Neo Med. 2017;11:1–7.
4. World Health Organization. WHO recommendations on postnatal care of the mother and newborn. Geneva, Switzerland: World Health Organization; 2013.
5. Optimizing postpartum care. ACOG committee opinion No. 736. American College of Obstetricians and Gynecologists. Obstet Gynecol. 2019;131:e140–50.
6. Higgins TM, Dougherty AK, Badger GJ, Heil SH. Comparing long-acting reversible contraception insertion rates in women with Medicaid vs. private insurance in a clinic with a two-visit protocol. Contraception. 2018;97(1):76–78. doi:10.1016/j.contraception.2017.08.016
7. Branum AM, Jones J. Trends in long-acting reversible contraception use among U.S. women aged 15–44. NCHS Data Brief. 2015;188:1–8.
8. White K, Potter JE, Hopkins K, Grossman D. Variation in postpartum contraceptive method use: results from the Pregnancy Risk Assessment Monitoring System (PRAMS). Contraception. 2014;89(1):57–62. doi:10.1016/j.contraception.2013.10.005
9. Block-Abraham D, Arora KS, Tate D, Gee RE. Medicaid consent to sterilization forms: historical, practical, ethical, and advocacy considerations. Clin Obstet Gynecol. 2015;58(2):409–417. doi:10.1097/GRF.0000000000000110
10. Access to contraception. Committee opinion No. 615. American College of Obstetricians and Gynecologists. Obstet Gynecol. 2015;125:250–255. doi:10.1097/01.AOG.0000459866.14114.33.
11. Potter JE, Coleman-Minahan K, White K, et al. Contraception after delivery among publicly insured women in Texas. Obstet Gynecol. 2017;130(2):393–402. doi:10.1097/AOG.0000000000002136
12. Wilkinson B, Ascha M, Verbus E, et al. Medicaid and receipt of interval postpartum long-acting reversible contraception. Contraception. 2019;99(1):32–35. doi:10.1016/j.contraception.2018.08.017
13. Zapata LB, Murtaza S, Whiteman MK, et al. Contraceptive counseling and postpartum contraceptive use. Am J Obstet Gynecol. 2015;212(2):
14. Dude A, Matulich M, Estevez S, Liu Y, Yee LM. Disparities in postpartum contraceptive counseling and provision among mothers of preterm infants. J Women’s Health. 2018;27(5):676–683. doi:10.1089/jwh.2017.6561
15. Oduyebo T, Zapata LB, Boutot ME, et al. Factors associated with postpartum use of long-acting reversible contraception. Am J Obstet Gynecol. 2019:
16. Dehlendorf C, Grumbach K, Schmittdiel J, Steinauer J. Shared decision making in contraceptive counseling. Contraception. 2017;95(5):452–455. doi:10.1016/j.contraception.2016.12.010
17. Madden T, Secura GM, Nease RF, Politi MC, Peipert JF. The role of contraceptive attributes in women’s contraceptive decision making. Am J Obstet Gynecol. 2015;213(1):
18. Brunson MR, Klein DA, Olsen CH, Weir LF, Roberts TA. Postpartum contraception: initiation and effectiveness in a large universal healthcare system. Am J Obstet Gynecol. 2017;217:
19. Gubrium AC, Mann ES, Borrero S, et al. Realizing reproductive health equity needs more than Long-Acting Reversible Contraception (LARC). Am J Public Health. 2016;106(1):18–19. doi:10.2105/AJPH.2015.302900
20. Center for Disease Control. Morbidity and mortality weekly report, MMWR. 2009;58(3):821–826. Available from https://www.cdc.gov/mmwr/preview/mmwrhtml/mm5830a1.htm#tab1. Accessed December 21, 2018.
21. Starr KA, Martins SL, Watson S, Gilliam ML. Postpartum contraception use by urban/rural status: an analysis of the michigan pregnancy risk assessment monitoring system data. Women’s Health Issues. 2015;25(6):622–627. doi:10.1016/j.whi.2015.06.014
22. Dehlendorf C, Foster DG, de Bocanegra HT, Brindis C, Bradsberry M, Darney P. Race, ethnicity and differences in contraception among low-income women: methods received by family PACT clients, California, 2001–2007. Perspect Sex Reprod Health. 2011;43(3):181–187. doi:10.1363/psrh.2011.43.issue-3
23. Dehlendorf C, Park SY, Emeremni CA, Comer D, Vincett K, Borrero S. Racial/ethnic disparities in contraceptive use: variation by age and women’s reproductive experiences. Am J Obstet Gynecol. 2014;210(6):
24. Arora KS, Wilkinson B, Verbus E, et al. Medicaid and fulfillment of desired postpartum sterilization. Contraception. 2018;97(6):559–564. doi:10.1016/j.contraception.2018.02.012
25. Centers for Disease Control and Prevention. Effectiveness of family planning methods. Available from: https://www.cdc.gov/reproductivehealth/unintendedpregnancy/pdf/contraceptive_methods_508.pdf.
26. Santos NET, Oliveira AE, Zandonade E, Leal MC. Access to prenatal care: assessment of the adequacy of different indices. Cad Saude Publica. 2013;29(8):1664–1674. doi:10.1590/S0102-311X2013001200018
27. R Core Team. R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2017. Available from: https://R-project.org.
28. Thiel de Bocanegra H, Braughton M, Bradsberry M, Howell M, Logan J, Schwarz EB. Racial and ethnic disparities in postpartum care and contraception in California’s Medicaid program. Am J Obstet Gynecol. 2017;217(1):
29. Callegari LS, Zhao X, Schwarz EB, Rosenfield E, Mor MK, Borrero S. Racial/ethnic differences in contraceptive preferences, beliefs, and self-efficacy among women veterans. Am J Obstet Gynecol. 2017;216:
30. Jackson AV, Karasek D, Dehlendorf C, Foster DG. Racial and ethnic differences in women’s preferences for features of contraceptive methods. Contraception. 2016;93:406–411. doi:10.1016/j.contraception.2015.12.010
31. Peterson R, Gazmararian J, Clark KA, Green DC. How contraceptive use patterns differ by pregnancy intention: implications for counseling. Womens Health Issues. 2001;11(5):427–435. doi:10.1016/S1049-3867(01)00090-1
32. Kusunoki Y, Barber JS, Ela EJ, Bucek A. Black-white differences in sex and contraceptive use among young women. Demography. 2016;53:1399–1428. doi:10.1007/s13524-016-0507-5
33. Dehlendorf C, Ruskin R, Grumbach K, et al. Recommendations for intrauterine contraception: a randomized trial of the effects of patients’ race/ethnicity and socioeconomic status. Am J Obstet Gynecol. 2010;203:
34. Kramer RD, Higgins JA, Godecker AL, Ehrenthal DB. Racial and ethnic differences in patterns of long-acting reversible contraceptive use in the United States, 2011–2015. Contraception. 2018;97(5):399–404. doi:10.1016/j.contraception.2018.01.006
35. Tully KP, Stuebe AM, Verbiest SB. The fourth trimester: a critical transition period with unmet maternal health needs. Am J Obstet Gynecol. 2017;217(1):37–41. doi:10.1016/j.ajog.2017.03.032
36. Access to Postpartum Sterilization. Committee opinion No. 530. American College of Obstetricians and Gynecologists. Obstet Gynecol. 2012;120(1):212–215. doi:10.1097/AOG.0b013e318262e354.
37. Iseyemi A, Zhao Q, McNichohlas C, Peipert J. Unintended pregnancy in the contraceptive CHOICE project. Obstet Gynecol. 2017;130(3):609–615. doi:10.1097/AOG.0000000000002189
38. Kost K, Singh S, Vaughan B, Trussell J, Bankole A. Estimates of contraceptive failure from the 2002 National Survey of Family Growth. Contraception. 2008;77(1):10–21. doi:10.1016/j.contraception.2007.09.013
39. Vaughan B, Trussell J, Kost K, Singh S, Jones R. Discontinuation and resumption of contraceptive use: results from the 2002 National Survey of Family Growth. Contraception. 2008;78(4):271–283. doi:10.1016/j.contraception.2008.05.007
40. Grunloh DS, Casner T, Secura GM, Peipert JF, Madden T. Characteristics associated with discontinuation of long-acting reversible contraception within the first 6 months of use. Obstet Gynecol. 2013;122(6):1214–1221. doi:10.1097/01.AOG.0000435452.86108.59
41. Borrero S, Zhao X, Mor MK, Schwarz EB, Good CB, Gellad WF. Adherence to hormonal contraception among women veterans: differences by race/ethnicity and contraceptive supply. Am J Obstet Gynecol. 2013;209(2):
42. Werth SR, Secura GM, Broughton HO, Jones ME, Dickey V, Peipert JF. Contraceptive continuation in Hispanic women. Am J Obstet Gynecol. 2015;212(3):
43. Guzman L, Wildsmith E, Manlove J, Franzetta K. Unintended births: patterns by race and ethnicity and relationship type. Perspect Sex Reprod Health. 2010;42:176–185. doi:10.1363/4217610
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

