Back to Journals » Psychology Research and Behavior Management » Volume 12
Verbal performance of total laryngectomized patients rehabilitated with esophageal speech and tracheoesophageal speech: impacts on patient quality of life
Authors Allegra E , La Mantia I , Bianco MR, Drago GD , Le Fosse MC, Azzolina A, Grillo C, Saita V
Received 18 April 2019
Accepted for publication 18 July 2019
Published 15 August 2019 Volume 2019:12 Pages 675—681
DOI https://doi.org/10.2147/PRBM.S212793
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Mei-Chun Cheung
Eugenia Allegra,1 Ignazio La Mantia,2 Maria Rita Bianco,1 Gaetano Davide Drago,3 Maria Cristina Le Fosse,1 Alfio Azzolina,4 Calogero Grillo,2 Vincenzo Saita4
1Otolaryngology, Department of Health Science, University of Catanzaro, Catanzaro, Italy; 2Otolaryngology, "G.F Ingrassia" Department, University of Catania, Catania, Italy; 3Grand Hôpital de l’Est Francilien, Jossigny, France; 4Otolaryngology Unit, Cannizzaro Hospital, University of Catania, Catania, Italy
Introduction: Total laryngectomy has important psychophysical and social consequences for patients’ quality of life because of the functional changes resulting from the removal of the larynx. Voice deprivation is perhaps the most relevant limiting factor in social relationships, increasing feelings of solitude and tending to drive individuals into social isolation. Multiple voice rehabilitation methods after total laryngectomy are available. This study aimed to determine the acoustic quality of the rehabilitated voice achieved with esophageal speech (ES) and tracheoesophageal speech (TES), and acoustic quality impacts on patients’ perceptions of their quality of life.
Materials and methods: The patient inclusion criterion was the completion of a speech rehabilitation course with ES or TES at least 6 months after total laryngectomy. The voice acoustic analysis was carried out automatically by using the Multidimensional Voice Program. The following parameters were extracted: fundamental frequency (F0), Jitter% (Jitt), Shimmer% (Shim), and noise-to-harmonic ratio (NHR). Subjective voice evaluation was performed by using the following questionnaires: Voice Handicap Index (VHI), Voice-related Quality of Life (V-RQOL), and Voice Performance Questionnaire (VPQ).
Results: The acoustic analysis showed a difference between ES and TES patients on all acoustic parameters; this difference was significant for F0 (133.09±2.4 and 119±3.3, respectively; p<0.001), NHR (0.43±0.21 and 0.31±0.14, respectively; p=0.02), and maximum phonation time (2.02±038 s and 10.64±0.28 s, respectively; p=0.01. Regarding patient-related outcomes, TES correlated with better total scores compared with ES; however, the differences in the total scores on the VHI (p=0.09), V-RQOL (p=0.39), and VPQ (p=0.52) were not statistically significant.
Conclusion: The rehabilitation of laryngectomized patients must be addressed by a multidisciplinary team that considers the personalities, personal needs, and relational conditions of individual patients in order to determine and apply the phonatory rehabilitation method most suitable for achieving a better quality of life.
Keywords: total laryngectomy, tracheoesophageal speech, esophageal speech, laryngeal cancer
Introduction
Laryngeal cancer represents 4.5% of all malignancies and is one of the most common cancers of the upper aerodigestive tract.1 The main modalities of surgical treatment include transoral laser microsurgery, open preservation surgery, and total laryngectomy. In recent years, open preservation surgeries have increased,2,3 which can be attributed to the improvement of the preoperative staging and follow-up as a result of enhanced imaging approaches.4,5 The purpose of organ preservation surgery is to avoid the highly mutilating intervention of total laryngectomy and to maintain laryngeal function with respect to the oncological radicality. However, several patients with advanced stage disease who required total laryngectomy have been observed thus far. Total laryngectomy intervention has important psychophysical and social consequences for patient quality of life.6,7 This effect on quality of life is due to the functional changes in vocalization resulting from the removal of the larynx, leading to immediate loss of phonatory function and permanent separation of the upper airways from the lower airways, which in turn, results in a disconnection between the airways and the mouth and nose, and a stoma is created to breathe. Voice deprivation is perhaps the most relevant limiting factor in social relationships, increasing feelings of solitude and tending to drive individuals into social isolation. Multiple voice rehabilitation methods after total laryngectomy are available, including electrolaryngeal speech, esophageal speech (ES), and tracheoesophageal voice prosthesis. An electrolaryngeal speech device is held against the neck, producing an electronic vibration that is shaped into speech when it reaches the mouth area; the result is a robotic and monotonous sound. However, in recent years, the use of such devices has been almost completely abandoned, and greater attention has been given to tracheoesophageal voice prosthesis8–10 for speech rehabilitation. The recovery of the phonatory function is, therefore, achieved mainly with an ES or with a tracheoesophageal voice prosthesis. In both methods of voice rehabilitation, an internal substitute sound source is produced in the pharyngoesophageal segment. Many studies have reported that tracheoesophageal speech (TES) provides a good quality of speech and represents an excellent means of communication.11–13 However, it is difficult to determine the most effective rehabilitation method in terms of both objective good quality of voice and greater satisfaction for the patient. Few studies12,13 have considered the correlation between quality of voice, assessed by using acoustic analysis, and patients’ perception of their rehabilitated voice. Therefore, this study aimed to determine the acoustic quality of the rehabilitated voice, achieved with ES and TES, and its impacts on patients’ perceptions of their quality of life.
Materials and methods
Patients
This multicentric study was carried out on patients submitted from 2004 to 2017 to total laryngectomy and recruited during follow-up visits over the period from October 2017 to September 2018 at the Otolaryngology, Department of Health Science, University of Catanzaro, Otolaryngology Unit, Cannizzaro Hospital, Catania, Otolaryngology Unit, University of Catania, Italy. The inclusion criterion was completion of a speech rehabilitation course with ES or TES at least 6 months. Patients who did not undergo any voice rehabilitation or who used electrolaryngeal speech, non–self-sufficient patients with disabilities of the upper limbs or with cognitive deficits, patients with locoregional recurrence, and patients who refused to participate in the study were excluded from the research. The rehabilitation program with esophageal voice began from the 15th to the 20th day after laryngectomy, as soon as the patient was able to eat orally. Injection and inhalational methods were used in various ways, adapting these methods to the individual patient. Rehabilitation with tracheoesophageal prosthesis (TEP) began the day immediately after the insertion of the prosthesis and provided for specific training that consisted of training the emission, initially, of isolated vowels, then of vowels tied together, then of disyllable words, and, finally, in the pronunciation of short sentences. The average time of administration of the planned speech therapy within which the pharyngoesophageal voice should be learned was 3 months. All patients were instructed by speech language pathologists with extensive experience in the rehabilitation of laryngectomized patients.
The study was approved by the review boards of the abovementioned institutions. All patients were informed of the purpose of the study before they gave their written informed consent. This study was conducted in accordance with the Declaration of Helsinki. The patients’ demographic and clinical data were collected, including education, marital status, and occupation.
Acoustic analysis
Voice analysis was conducted with the use of the commercially available software PRAAT.14 The recordings were carried out in a quiet room (36 dB) by using a microphone (Shure C606) at a distance of 15 cm from the mouth. Each recording consisted of the same speech passages. Each patient was instructed to pronounce, at the intensity and frequency of the conversation voice, a vocal/a/sustained in a prolonged way, three times, and the phrases “My name is …, ” “I was born …, ” “the …, ” and “I live … ” The audio recordings were imported and edited with the PRAAT software; the beginning and the end of the recording were discarded, and the most stable portion of the emission with a mean duration of 3 s was selected. The analysis of the acoustic parameters was carried out automatically by using the Multidimensional Voice Program. The following parameters were extracted: fundamental frequency (F0), Jitter% (Jitt), Shimmer% (Shim), and noise-to-harmonic ratio (NHR). The mean value of F0 speech was extracted from the recording of the reading of the text by using the PRAAT software. The maximum phonation time (MPT) was measured (in seconds) with the pronunciation of/aa/as the primary value.
Patient-reported outcomes
Subjective evaluation of the voice was conducted by using the following questionnaires: voice handicap index (VHI), voice-related quality of life (V-RQOL), and voice performance questionnaire (VPQ). The VHI15 consists of 10 items on emotional issues, 10 items on physical issues, and 10 items on functional issues. Scoring is from 0 to 120, with 120 representing the maximum perceived disability. Each item is scored on a 4-point scale: 0=never, 1=almost never, 2=sometimes, 3=almost always, and 4=always. A VHI score of 0–40 points indicates a handicap of slight impact, a score of 41–60 indicates moderate impact, and a score of 61 indicates severe impact. The VPQ16 is a 12-item instrument that examines the physical symptoms and socioeconomic impacts of the voice disorder. The VPQ applies a response format in which the patient selects the statement that best answers each question. The statements are graded in terms of severity of vocal performance. A score from 1 to 5 is assigned to each answer, with the total score indicating the severity. The maximum severity score is 60, and the minimum score is 12. The V-RQOL17 is a self-administered questionnaire that measures the subjective burden elicited by a voice disorder. The V-RQOL consists of 10 statements on voice-related aspects across the emotional, physical, and functional domains. Each patient responds according to the suitability or closeness of each item (ranging from 1=not a problem to 5=the problem is “as bad as it can be”) to his or her situation. The overall VR-QOL score ranges from 10 to 15 (excellent), 16 to 20 (very good), 21 to 25 (good), 26–30 (fair), and 31 to 50 (poor).
Statistical analysis
Statistical analysis was performed by using the MedCalc software version 9.0 (v 9.0; MedCalc Software bvba, Ghent, Belgium). The data collected included means, medians, and standard deviations. Pearson’s chi-square and/or Fisher’s exact test was used to identify differences in demographic and clinicopathologic data between cohorts. The descriptive data for all scales and items were obtained by using the mean scores and standard deviations. The paired sample t test was used to determine the mean difference between paired observations. A Kolmogorov–Smirnov test was used to assess normal distribution of continuous variables. As a normal distribution was found, parametric tests were used. The Mann–Whitney U test for independent samples was applied to analyze group differences. The tests were two-tailed, and significance was set at p<0.05.
Results
A total of 67 patients were included in the study; 2 (2.9%) were female, and 65 (97.1%) were male. The mean age at diagnosis was 64.5±8.0SD years. According to the clinical classification, 40 patients were at stage III, and 27 patients were at stage IV. Twenty-eight (41.7%) of the enrolled patients were subjected to total laryngectomy, 25 (37.4%) to TL and neck dissection, and 14 (20.9%) to total laryngectomy, neck dissection, and adjuvant radiotherapy with or without chemotherapy. The mean time since total laryngectomy was 7.3±3.4SD months. Of the 67 patients, 21 (31.3%) were still employed, and the rest (68.7%) were retired; 26 (38.8%) completed elementary education, 25 (37.4%) finished secondary school, and 16 (23.9%) completed high school. Fifty (74.6%) of the 67 patients were married or cohabiting, and 17 (25.3%) were single. Speech rehabilitation was achieved by esophageal voice (ES) in 32 (47.7%) patients and by TES in the remaining 35 (52.3%) patients. A primary TEP was performed in 10 patients, and a secondary TEP was performed in 25 patients. Provox Vega prosthesis (ATOS Medical) was placed in all of these patients. Table 1 shows the demographic and clinical data of the two groups of patients. There were no significant differences between the groups; however, the time since LT was longer in the ES patients than in the TES patients (p<0.001). The acoustic analysis showed a difference between the ES and TES patients on all acoustic parameters; this difference was significant for F0 (133.09±2.4 and 119±3.3, respectively; P<0.001), NHR (0.43±0.21 and 0.31±0.14, respectively; p=0.02), and MPT (2.02±038 s and 10.64±0.28 s, respectively; p=0.01, as shown in Table 2. Regarding patient-related outcomes, TEP use correlated with better total scores compared with ES, as reported in Table 3; however, the differences in the total scores on the VHI (p=0.09), V-RQOL (p=0.39), and VPQ (p=0.52) were not statistically significant. The analysis of the subscales showed a significant difference in the functional subscales, for both the VHI (p=0.02) and the VRQOL (p=0.001) questionnaire. There were no significant differences in the emotional subscales for either the VHI (p=0.51) or the V-RQOL (p=0.41) questionnaire. Moreover, there was no significant difference between the two groups regarding physical condition, based on the answers on the VHI (p=0.11) and VPQ (p=0.65) questionnaires and on the socioeconomic condition (VPQ p=0.07). The analysis of the correlation of demographic and clinical variables with patient-reported outcomes, reported in Table 4, indicated that patients with a longer time since TL had less discomfort, with a significant difference found for the VHI (p=0.008) and the V-RQOL (p=0007). Another variable, related to better V-RQOL, was level of education, with a statistically significant difference found for patients who completed high school (p=0.002, p=0.01, and p=0.003 for VHI, V-RQOL, and VPQ, respectively).
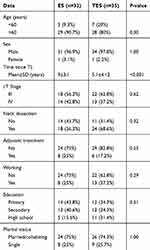 |
Table 1 Demographic and clinical data of the ES and TES groups |
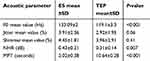 |
Table 2 Acoustic analysis of the two groups |
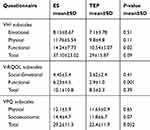 |
Table 3 Patient-related outcomes |
 |
Table 4 Correlation between demographic-clinical variables and patient-reported outcomes |
Discussion
Studies on the quality of life of laryngectomized patients in relation to the speech rehabilitation method used to restore oral communication are few and heterogeneous. Most of the research focused on the objective evaluation of by using acoustic analysis, compared with the perceptual evaluation,18 according to the different substitute sound sources in speech rehabilitation.11,19 By using PRO questionnaires, the present study evaluated the objective acoustic quality and the patients’ perceived quality of their rehabilitated voice with ES and TES. Patients who had not undergone rehabilitation or who used EL were excluded from the study given that their sound source was an external device. In contrast, both ES and TES use the air present in the esophagus, which reaches the oral cavity in different ways and is used for verbal communication. The acoustic analysis of the voice of the patients showed a difference in the parameters F0, NHR, and MFT between the patients rehabilitated with ES and those rehabilitated with TES. Granda et al,20 reported that patients rehabilitated with TES showed significantly better values in relation to the acoustic parameters F0 (mean value), NHR, and MPT, whereas Arias et al,21 found no significant differences in acoustic parameters between the two rehabilitation modalities. The different findings of these studies based on the acoustic analysis of voices rehabilitated with TEP might be attributed to several factors, including the type of prosthesis used. The analysis of the results of the PRO questionnaires showed a better overall QOL in the TES group, although both groups reported some degree of voice handicap. The present study found a significant difference in the functional subscale for both the VHI and the V-RQOL questionnaire, with improved voice performance in TES patients. The physical, emotional, and socioeconomic subscales showed no significant differences between the two groups. However, none of the methods of speech rehabilitation studies achieved a significant difference regarding satisfactory outcomes for self-reported vocal function, similar to the finding of Van Sluis et al.11 Among the demographic and clinical variables, level of education and time since laryngectomy seemed to have significant effects on the degree of disability perceived by the patients due to their verbal communication modality. In particular, higher level of education and longer time since laryngectomy correlated with a better subjective assessment of verbal performance. The best perception of quality of life found in long-term laryngectomized patients may indicate that the patients have adapted to their new condition over time, modifying their habits and social and family relationships. Therefore, it is not easy to determine if laryngectomized patients adapt to their new conditions over time or if they resign themselves to living with a different condition. In fact, Sharpe et al, reported the capacity of laryngectomized patients to adapt to the long-term changes in their communication with others, which has an impact on their quality of life. Moreover, personal factors, such as education, to which social economic conditions are linked,22 in addition to communication needs and demands, play an important role in the perceived quality of V-RQOL. For this reason, although rehabilitation with TES seemed to provide better results in terms of acoustic quality and better patient perception of communicative performance, speech therapy alone may not be sufficient for the patient to accept the new speech method. An integrated rehabilitation,23 including an evaluation of the patients’ anxiety and depression status,24 should be included to achieve better patient quality of life.
Conclusion
Based on the results obtained in the present work, the rehabilitation of laryngectomized patients must be addressed by a multidisciplinary team that considers the personalities, personal needs, and relational conditions of individual patients in order to determine and apply the phonatory rehabilitation method most suitable for achieving a better quality of life.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Parkin DMBF, Ferlay J, Pisami P. Global cancer statistics. CA Cancer J Clin. 2005;55:74–108.
2. Garozzo A, Allegra E, La Boria A, Lombardo N. Modified supracricoid laryngectomy. Otolaryngol Head Neck Surg. 2010;142(1):137–139. doi:10.1016/j.otohns.2009.09.020
3. Allegra E, Franco T, Trapasso S, Domanico R, La Boria A, Garozzo A. Modified supracricoid laryngectomy: oncological and functional outcomes in the elderly. Clin Interv Aging. 2012;7:475. doi:10.2147/CIA.S38410
4. Allegra E, Ferrise P, Trapasso S, et al. Early Glottic Cancer: role of MRI in the preoperative Staging. Biomed Res Int. 2014;2014:1–7. doi:10.1155/2014/890385
5. Allegra E, Saita V, De Natale M, et al. Use of PET/CT to detect local and regional laryngeal cancer recurrence after surgery. Rep Med Imaging. 2017;10:31–36. doi:10.2147/RMI.S124764
6. Hilgers FJ, Ackerstaff AH, Aaronson NK, Schouwenburg PF, Van Zandwijk ZN. Physical and psychosocial consequences of total laryngectomy. Clin Otolaryngol Allied Sci. 1990;15(5):421–425.
7. Li X, Li J, Shi Y, et al. Psychological intervention improves life quality of patients with laryngeal cancer. Patient Prefer Adherence. 2017;11:1723–1727. doi:10.2147/PPA.S147205
8. La Mantia I, Rossitto F, Andaloro C. Quality of life in head and neck cancer: patients’ and family caregivers’ perceptions. Egypt J Ear Nose Throat Allied sci. 2018;18(3):247–250. doi:10.1016/j.ejenta.2017.11.002
9. La Mantia I, Albanese G, Andaloro C. Primary versus secondary Tracheoesophageal puncture: how similar are they? Otorinolaringologia. 2018;68(1):28–32.
10. Grillo C, Saita V, Grillo CM, et al. Candida colonization of silicone voice prostheses: evaluation of device lifespan in laryngectomized patients. Otorinolaringologia. 2017;67(3):75–80.
11. van Sluis KE, van der Molen L, van Son RJJH, Hilgers FJM, Bhairosing A, van Den Brekel MWM. Objective and subjective voice outcomes after total laryngectomy: asystematic review. Eur Arch Otorhinolaryngol. 2018;275(1):11–26. doi:10.1007/s00405-017-4790-6
12. Ţiple C, Drugan T, Dinescu FV, Mureşan R, Chirilă M, Cosgarea M. The impact of vocal rehabilitation on quality of life and voice handicap in patients with total laryngectomy. J Res Med Sci. 2016;26(21):127.
13. Patel RS, Mohr T, Hartman C, et al. Tracheoesophageal prosthesis use is associated with improved overall quality of life in veterans with laryngeal cancer. Ann Otol Rhinol Laryngol. 2018;127(7):421–428. doi:10.1177/0003489418772067
14. Boersma P, Weenink D. Praat: Doing phonetics by computer. Version 5. 3.56. Amsterdam: University of Amsterdam; 2007.
15. Jacobs BH, Johnson A, Grywalski C, et al. The Voice Handicap Index (VHI): development and validation. Am J Speech Lang Pathol. 1997;6:66–70. doi:10.1044/1058-0360.0603.66
16. Hogikyan ND, Sethuraman G. Validation of an instrument to measure voice-related quality of life (V-RQOL). J Voice. 1999;13(4):557–569. doi:10.1016/S0892-1997(99)80010-1
17. Deary IJ, Webb A, Mackenzie K, Wilson JA, Carding PN. Short, self-report voice symptom scales: psychometric characteristies of the voice handicap Index-10 and the vocal performance questionnaire. Otolaryngol Head Neck Surg. 2004;131(3):232–235. doi:10.1016/j.otohns.2004.02.048
18. Eadie TL, Day AM, Sawin DE, Lamvik K, Doyle PC. Auditory-perceptual speech outcomes and quality of life after total laryngectomy. Otolaryngol Head Neck Surg. 2013;148(1):82–88. doi:10.1177/0194599812461755
19. Sharpe G, Camoes Costa V, Doubé W, Sita J, McCarthy C, Carding P. Communication changes with laryngectomy and impact on quality of life: a review. Qual Life Res. 2018. doi:10.1007/s11136-018-2033-y
20. Granda Membiela CM, Fernandez GMJ, Mamolar Andres S, Santamarina Rabanal L, Sirgo Rodriguez P, Alvarez Marcos C. Laryngectomized voice rehabilitation: handicap, perception and acoustic analysis. Rev Logop Foniatr Audiol. 2016;36(3):127–134. doi:10.1016/j.rlfa.2016.03.002
21. Arias MR, Ramón JL, Campos M, Cervantes JJ. Acoustic analysis of the voice in phonatory fistuloplasty after total laryngectomy. Otolaryngol Head Neck Surg. 2000;122(5):743–747. doi:10.1016/S0194-5998(00)70208-7
22. Agarwal SK, Gogia S, Agarwal A, Agarwal R, Mathur AS. Assessment of voice related quality of life and its correlation with socioeconomic status after total laryngectomy. Ann Palliat Med. 2015;4(4):169–175. doi:10.3978/j.issn.2224-5820.2015.09.05
23. Longobardi Y, Savoia V, Bussu F, et al. Integrated rehabilitation after total laryngectomy: a pilot trial study. Support Care Cancer. 2019;27:3537–3544. doi:10.1007/s00520-019-4647-1
24. Saltürk Z, Arslanoğlu A, Özdemir E, et al. How do voice restoration methods affect the psychological status of patients after total laryngectomy? HNO. 2016;64(3):163–168. doi:10.1007/s00106-016-0134-x
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
