Back to Journals » Journal of Pain Research » Volume 13
Translation and Validation of the Farsi Version of the Pain Management Self-Efficacy Questionnaire
Authors Rezaei H, Saeed AFM , Abdi K, Ebadi A , Ghanei Gheshlagh R , Kurdi A
Received 16 January 2020
Accepted for publication 24 March 2020
Published 7 April 2020 Volume 2020:13 Pages 719—727
DOI https://doi.org/10.2147/JPR.S246077
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Professor Robert B. Raffa
Hayedeh Rezaei,1 Ali Faiek M Saeed,2 Kamel Abdi,3 Abbas Ebadi,4 Reza Ghanei Gheshlagh,5 Amanj Kurdi6
1Department of Nursing, Faculty of Nursing and Midwifery, Kurdistan University of Medical Sciences, Sanandaj, Iran; 2Department of Management, College of Business Administration and Economic, Bayan University, Erbil, Kurdistan, Iraq; 3Nursing Department, Faculty of Medicine, Komar University of Science and Technology, Sulimaniya City, Kurdistan Region, Iraq; 4Behavioral Sciences Research Center, Life Style Institute, Baqiyatallah University of Medical Sciences, Tehran, Iran; 5Department of Nursing, Faculty of Nursing and Midwifery, Kurdistan University of Medical Sciences, Sanandaj, Iran, Social Determinants of Health Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran; 6Pharmacoepidemiology and Pharmacy Practice, Strathclyde Institute of Pharmacy and Biomedical Science, University of Strathclyde, Glasgow, UK, Department of Pharmacology, College of Pharmacy, Hawler Medical University, Erbil, Iraq
Correspondence: Reza Ghanei Gheshlagh
Social Determinants of Health Research Center, Research Institute for Health Development, Kurdistan University of Medical Sciences, Sanandaj, Iran
Tel +98 9144050284
Email [email protected]
Introduction: Pain management is a complex process that is managed through a multi-disciplinary team in which nurses have a significant role. The present study aimed at translating and examining the psychometric properties of the Pain Management Self-Efficacy Questionnaire (PMSEQ) among Iranian nurses.
Methods: This was a cross-sectional, methodological study conducted in 2019 among nurses working in two teaching hospitals in Sanandaj (Tohid and Kosar). The participants were selected using a convenience sampling method. Responsiveness; interpretability; and face, content, and construct validities were examined using exploratory and confirmatory factor analyses. In addition, internal consistency and stability were examined using the Cronbach’s alpha and test-retest, respectively.
Results: Overall, 410 nurses (210 for the EFA and 200 for the CFA) were included in the sample. In the exploratory factor analysis, two factors of comprehensive pain assessment and pain management with eigenvalues of 6.36 and 1.91, respectively, were extracted. The two factors together explained 56.64% of the variance of nurses’ pain management self-efficacy. The confirmatory factor analysis indicated that the model had a moderate fit to the data (RMSEA: 0.12; NFI: 0.84; NNFI: 0.86; CFI: 0.88; IFI: 0.88; RFI: 0.81; GFI: 0.76; AGFI: 0.69; PGFI: 0.59; RMR: 0.09; standardized RMR: 0.09). Total questionnaire and the two factors (i.e. comprehensive pain assessment and pain management) had internal consistency coefficients of 0.891, 0.876, and 0.803, respectively.
Conclusion: The Farsi version of PMSEQ had good internal consistency and reliability, as well as content and construct validity, and can be used in future studies.
Keywords: validation, pain, self-efficacy, pain management
Introduction
Pain is defined by the International Association for the Study of Pain (IASP) as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage”.1,2 It is a common experience in human life and one of the most common reasons for seeking medical care.3 The American Pain Society (APS) defines pain as the fifth vital sign that, if not controlled properly, can lead to impaired functioning, reduced quality of life (QOL), and irreparable health damage.4 Pain is common conditions worldwide, with about 76 million adults in the US suffer from pain.5,6 In addition to metabolic and physiologic complications of pain, unalleviated pain can increase the cost of care and risk of readmission, reduce patients’ QOL and independence, and lead to depression and aggression.7–9 Despite medical advances, pain is still regarded as a complex phenomenon, and evaluation of pain relief techniques is in an early stage.10 Given that nurses spend more time with patients compared to other healthcare providers, optimal pain management is one of their most important tasks, and they need to be adequately prepared for it. Relieving patient’s pain is a priority in nursing care activities,11 including decisions about assessing and controlling patients’ pain, which involves making decisions about the level of pain and required painkillers.12 This is important since pain management not only relieves patients physically, but also improves their QOL, facilitates their quick return to daily activities, reduces hospital length of stay, and also reduces treatment costs.13 In many cases, nurse may not able to properly assess patients’ pain due to lack of sufficient training, inaccurate assessments, or concerns about the complications of painkillers as well as lack of valid and reliable assessment tools and periodic assessments.14 In terms of the adequacy of pain management for patients with advanced types of cancer, Okuyama et al showed that 70% of patients did not receive adequate pain management, and that patients considered pain as their biggest problem.15 Various studies have shown that improving nurses’ self-efficacy in pain management can help relieve patients’ pain and reduce their depression, anxiety, and fear more effectively.16–21 Given that pain is a subjective feeling, nurses can only manage it based on patients’ report on the level of pain they feel.22 Therefore, nurses’ self-efficacy in pain management is closely related to their belief in their ability to manage patients’ pain.23
Self-efficacy in pain management depends on accurate and systematic assessment of pain. In order to standardize the quality of pain management across nursing profession, a common and efficient tool is required to document and assess pain management. Research evidence indicates the inadequacy of this process, and little research has been done on pain assessment, therefore, it seems helpful to use a common assessment chart in pain management.24
Assessment of a subjective phenomenon like pain management requires a valid and reliable tool, but, as far as we know, there is no instrument to assess pain management skills in Iran. The Pain Management Self-Efficacy Questionnaire (PMSEQ), developed by Masindo et al, is used to assess nurses’ pain management skills. The PMSEQ has 21 items that are rated on a 6-point Likert-type scale ranging from 0 (not sure at all) to 6 (totally sure), and higher scores on the questionnaire indicate better self-efficacy in pain management. The Comprehensive dimension has 14 items assessing cooperation with the medical team in controlling pain, selecting the best instrument for assessing pain, helping patients experiencing pain with activities, recording pharmacological treatments for pain, reducing pain-induced anxiety, reassessment of pain score, evaluation of pain history, recording non-pharmacological treatments for pain, safe prescription of pain relievers, combining supplementary and alternative treatments, and helping patients in coping with pain. The assessment dimension has 4 items assessing pain after intervention, pain while resting, verbal signs of pain, and non-verbal signs of pain. The supplemental dimension has three items assessing the pain ladder, complications of pain relievers, and assessment of pain in emergency situations.25
Given the lack of a valid and reliable tool in Iran to examine nurses’ pain management skills, most studies have used invalidated instruments that may not be able to adequately assess this subjective concept. Therefore, the present study aimed at translating and validating the PMSEQ among Iranian nurses.
Methods
Study Design
This was a cross-sectional, methodological study aimed at translation and validation of the PMSEQ in 2019 in Sanandaj, Iran.
Sample Size and Participants
The minimum sample size required to conduct exploratory factor analysis (EFA) is 3–10 participants per item.26 In the present study, a total of 210 nurses with at least 1 year of work experience who were selected among nurses working in internal, surgical, and intensive care units of two teaching hospitals in Sanandaj (Tohid and Kosar). Lack of interest to participate in the study, and participation in the self-efficacy in pain management classes for providing care for patients with chronic disorders suffering from pain inside the family, were among the exclusion criteria.
Measurement Instrument
Translation Process
First, permission was obtained from the original author of the PMSEQ to translate and validate the questionnaire in Iran. Then, the questionnaire was translated from English to Farsi and back-translated to English based on the WHO guidelines and using the Forward & Backward method. In the first step, two independent translators fluent in English translated the English version of the questionnaire into Persian. One of the translators was familiar with nursing and medical terms, while the other translator was not. Then, the two translations were examined by the research team, and the final Farsi version was developed. Finally, the final Farsi version was translated again into English.27
Face and Content Validities
In order to examine the psychometric properties of the PMSEQ, face, content, and construct validities were assessed. In order to assess face validity, the PMSEQ was distributed among 15 nurses who were asked to read the items out loud and provide feedback on the comprehensibility and relevance of the items. Then, the questionnaire was sent to 10 clinical researchers (who had written books on pain management or had research experience in this subject) who were asked to qualitatively asses the items of the questionnaire and provide feedback on grammar, use of proper words, etc.
Data Analysis
Exploratory factor analysis (EFA) and confirmatory factor analysis (CFA) were used to assess construct validity. A sample consisted of 210 nurses was used for the EFA and a sample consisted of another 200 nurses was used for the CFA. At this stage, latent factors were extracted, and the Kaiser-Meyer-Olkin (KMO) statistic and the Bartlett’s test were calculated.26 KMO values close to 1 indicate the adequacy of sample size for factor analysis.28 KMO values between 0.7 and 0.8 and between 0.80 and 0.90 are considered good and excellent, respectively.29 Latent factors were extracted using the Principal Axis Factoring using the Promax rotation.30 The number of extracted factors was determined based on eigenvalues and the Scree plot. Eigenvalues above 1 were retained.31 A loading value of ≥0.30 was considered acceptable.32 The greater this value, the better the variables are presented by the factors.33 The minimum sample size recommended for CFA is 200 participants,26 therefore a total of 200 nurses meeting the inclusion criteria were selected for the CFA, using a convenience sampling method. At this stage, goodness-of-fit indices, including the root mean square error of approximation (RMSEA), the comparative fit index (CFI), the Normed Fit Index (NFI), and the adjusted goodness of fit index (AGFI) were examined. The acceptable thresholds for the goodness of fit indices are shown in Table 1.34 All the analyses were performed using SPSS, version 18 and Lisrel, version 8.8
 |
Table 1 Acceptable Thresholds of the Fit Indices in the Confirmatory Factor Analysis Model |
The Cronbach’s alpha coefficient was used to examine the internal consistency of the PMSEQ. For this purpose, the questionnaire was distributed among 30 nurses (12 men and 18 women with a mean age of 34.6±4.8 years) who had been selected using a convenience sampling method. These participants were not included in the final analysis. A Cronbach’s alpha between 0.7 and 09 indicates good reliability.35 The reliability of the instrument was examined using the test-retest method and the intraclass correlation coefficient (ICC) with the two-way mixed-effects model and absolute agreement (a 95% confidence level); values higher than 0.75 were considered acceptable. At this stage, the questionnaires were distributed among 15 nurses (7 men and 8 women with a mean age of 35.46±6.12 years). The participants of the reliability examination did not participate in the main study. In order to assess responsiveness, Standard Error of Measurement (SEM) and Minimal Detectable Change (MDC) were calculated using the following formulas:
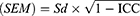
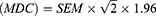
A reliability coefficient is an index that differs across populations and from one sample to another. In contrast, SEM is the measurement unit of a scale that its values are not as prone as reliability coefficients to be affected by the sample used for computing the estimate. In addition, in order to examine interpretability, both floor and ceiling effects were calculated and reported.36
Ethical Considerations
The ethics committee of Kurdistan University of Medical Sciences approved this study (no. IR.MUK.REC.1397.279). Before starting the study, the study objectives were explained to the participants, and their informed consents were obtained. In addition, the participants were reassured that their personal information remained completely confidential.
Results
Descriptive Statistics
The participants of the EFA were 210 nurses, including 103 (49%) men and 107 (51%) women, with a mean age of 36.9±8.3 years and an age range of 23–58 years. In the CFA, another 200 nurses with a mean age of 31.5±5.6 years and an age range of 23–53 years participated of which 52.5% were women. Further details are provided in Table 2.
 |
Table 2 Demographic Description of the Participants of the EFA and CFA |
Face and Content Validity
Due to being simple and clear, the items were not changed in the examination of face validity. In addition, in the examination of content validity, only several long sentences were shortened.
Construct Validity
Exploratory Factor Analysis
Face and qualitative content validities were confirmed by qualified nurses and medical experts. The KMO statistic was found to be 0.812 and the Bartlett’s test was significant (p= 0.001). By conducting several EFAs using different extraction and rotation methods, the best model was acquired using the Principal Axis Factoring and the Promax rotation. 4 elements (3, 5, 9, and 20) were discarded due to having factor loadings below 0.3. According to the results, two factors of Comprehensive pain assessment (items, 11, 4, 7, 6, 21, 2, 16, 13, and 1) and Pain management (items 19, 17, 15, 14, 18, 8, 10, and 12) were extracted with eigenvalues of 6.360 and 1.914, respectively. The two factors together explained 56.64% of the variance of nurses’ self-efficacy in pain management (Table 3).
 |
Table 3 Exploratory Factor Analysis of the Farsi Version of the PMSEQ |
A new sample consisted of 200 nurses was selected for the CFA. The results of the chi-squared test (X2 = 391.98, p = 0.01) and the other fit indices indicated good fit of the final model (Figure 1): (RMSEA: 0.12; NFI: 0.84; NNFI: 0.86; CFI: 0.88; IFI: 0.88; RFI: 0.81; GFI: 0.76; AGFI: 0.69; PGFI: 0.59; RMR: 0.09; Standardized RMR: 0.091). The results of the CFA indicated that the two-factor model extracted from the EFA had a moderate fit to the data.
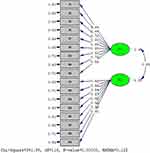 |
Figure 1 The final model. |
According to the results, the SEM and the MDC were found to be 2.42 and 6.68, respectively. In addition, the ceiling and floor effects for the total questionnaire were found to be 0% and 5%, respectively. A Cronbach’s alpha of 0.89 and alphas of 0.87 and 0.80 were found for the total questionnaire and the two factors of Comprehensive pain assessment and Pain management, respectively. In addition, the stability of the questionnaire was examined using the test–retest method and the Intraclass correlation coefficient (ICC) using two-way mixed effects and absolute agreement at a 95% confidence level; it was found to be 0.95 (0.91 to 0.98).
Reliability estimates of 0.90 (0.81–0.92, with 95% confidence interval) and 0.92 (0.84–0.97, with 95% confidence interval) were found for the Comprehensive pain assessment and Pain management dimensions, respectively.
Discussion
The aim of the present study was to examine the psychometric properties of the PMSEQ among Iranian nurses. The PMSEQ was first developed by Masindo et al to assess nurses’ self-efficacy in pain management in three dimensions (Comprehensive, Evaluative, and Supplemental).25 In our analysis which is presented in Table 2, two factors of Comprehensive pain assessment and Pain management were extracted that together explained 56.64% of the variance of nurses’ self-efficacy in pain management. These factors help nurses properly manage emergency situations resulting from pain and control patients’ pain more efficiently. The Chronic Pain Self-Efficacy Scale (CPSS) is another instrument for assessing self-efficacy in pain management. It has 22 items and 3 subscales of Physical pain, Coping, and Pain management. The Pain management dimension is similar in both the CPSS and the PMSEQ. Two Items of the Comprehensive pain assessment dimension of the Persian version of the PMSEQ (items no. 21 and 6) show pain coping strategies that are consistent with the Coping dimension of the CPSS.37
Pain is influenced by different factors, such as patient’s previous experiences, patient’s temperament, and pain’s negative consequences; this makes it particularly difficult to assess pain. Therefore, comprehensive pain assessment is important for effective pain management.38 Pain management dimension includes evaluation of pain history, use of supplement therapies, non-verbal symptoms of pain, and personal characteristics influencing pain, reassessment of pain and pain-related symptoms,39 and highlights the importance of comprehensive and individual assessment of pain along with the use of alternative and supplement methods.40 This dimension not only refers to the biological causes of pain, but also highlights the role of other factors in pain, including social, cultural, and psychological.41
Furthermore, the pain assessment dimension refers to cooperation with the treatment team, selection of proper tools to assess pain, reassessment of pain, helping the patient in coping with mild to moderate pain, and examination of the complications of painkillers. Efficient cooperation between nurses and other care providers implies that pain management is based on a multidisciplinary approach.42,43 The Nurses’ Self-Efficacy in Managing Children’s Pain has 6 items assessing Pain assessment, pain management, and Cooperation with the pain health care team. In the available Farsi version of the questionnaire, all of these dimensions are covered.42 However, due to the low number of items, it cannot adequately assess the multidimensional concept of pain management. Repeated assessment of patients’ pain is an important factor in the effective reduction of pain that has also been pointed out in the following items: effective examination of pain in emergency situations, helping patients in performing physical activities during experiencing pain, documenting and assessing pain based on the patient’s comments and not based on what the nurse thinks, and helping patients in coping with their own mild to moderate pain. Finally, pain assessment leads to effective pain management, reduces patients’ length of stay at hospital, reduces costs of treatment, and improves patients’ satisfaction with treatment.44
In pain management, there is a high focus on reducing pain using the analgesic ladder. The analgesic ladder is a three-step approach to control pain in patients in which first non-opioid pain medications are used, and if pain is not relieved, then opioid pain medications are administered.45 The item 3 of the PMSEQ referred to the analgesic ladder that was removed in the factor analysis. One of the reasons why this item was not loaded on any factor could be that the analgesic ladder for treating pain is not commonly used in Iran. This problem can be addressed in Iran by providing updated guidelines for pain management in medical centers and holding training workshops on this subject. Identification of pain in emergency situations is a necessary step in timely pain management before any other treatment; this is pointed out in the item 11 of the PMSEQ.46 Because nurses are faced with several acute health problems in the patient, identification of pain is often ignored or not given priority in emergency situations.
The PMSEQ assesses pain assessment and pain management completely and comprehensively; this indicates the superiority of this questionnaire over the previous ones. There are also other scales for assessing nurses’ self-efficacy in pain management. One of these is the 7-item Pain Management Survey (PMS), developed by Edwards et al in 2001, to identify pain symptoms; the psychometric properties of this scale have not been reported completely.47 Bandura’s scale (2006) is another scale for assessing nurses’ self-efficacy in pain management. It has 25 items of which 21 are related to treatment of pain and 9 are related to control of pain-related symptoms. The items are rated on an 11-point Likert-type scale.48 The large number of items may lead to response fatigue in the respondents. In addition, use of an 11-point scale can confuse the respondents.
Finally, it is suggested that by implementing programs aimed at improving nurses’ self-efficacy in pain management, comprehensive pain management can be realized. There is no doubt that paying attention to the dynamic process of self-efficacy in pain management that has led to the development of management standards can show the importance of continuous and reflective self-evaluation. One of the limitations of the present study were that that the nurses were assessed using the self-report method that may lead to certain biases.
Compared to other members of the medical team, nurses spend more time caring for patients, therefore they tend to notice patents’ pain before others. Nurses with higher self-efficacy in pain management can better monitor patients’ pain and prevent negative outcomes more efficiently. A valid and reliable instrument can help nurses gain a better insight into their own self-efficacy in pain management, and try to strengthen their weak points in this domain. Such an instrument can also be used by healthcare officials to monitor nurses’ efficacy in self-management, and hold workshops aimed at improving this capacity in nurses. Overall, the study results showed that the Farsi version of the PMSEQ can be used as a relevant, repeatable, valid, and reliable instrument to assess nurses’ self-efficacy in pain management. Overall, the results of EFA and CFA of the Farsi version of the PMSEQ confirmed two factors of Comprehensive pain assessment and Pain management. Therefore, it can be concluded that the two-factor structure of the PMSEQ has good validity and reliability, and that the questionnaire can be used to assess nurses’ self-efficacy in pain management.
Funding
The present study received financial support from the Kurdistan University of Medical Sciences.
Disclosure
No conflict of interest has been declared by the authors.
References
1. Treede R-D. The International Association for the Study of Pain definition of pain: as valid in 2018 as in 1979, but in need of regularly updated footnotes. Pain Rep. 2018;3(2):e643. doi:10.1097/PR9.0000000000000643
2. Kumar KH, Elavarasi P, David CM. Definition of pain and classification of pain disorders. J Adv Clin Res Insights. 2016;3(3):87–90. doi:10.15713/ins
3. Galinski M, Ruscev M, Gonzalez G, Kavas J, Ameur L, Biens D. Prevalence and management of acute pain in prehospital emergency medicine. Prehosp Emerg Care. 2010;14(3):334–339. doi:10.3109/10903121003760218
4. Shirazi M, Manoochehri H, Zagheri T, Zayeri F, Alipour V. Development of comprehensive chronic pain management model in older people: a qualitative study. J Iran Society Anaesthesiol Intensive Care. 2016;32(1):43–61.
5. Duke G, Haas B, Yarbrough S, Northam S. Pain management knowledge and attitudes of baccalaureate nursing students and faculty. Pain Manag Nurs. 2013;14(1):11–19. doi:10.1016/j.pmn.2010.03.006
6. Kerns R. Shining the LAMP on efforts to transform pain care in America. Ann Intern Med. 2018;168(7):517–518. doi:10.7326/M18-0061
7. Lai Y-H, Chen M-L, Tsai L-Y, et al. Are nurses prepared to manage cancer pain? A national survey of nurses’ knowledge about pain control in Taiwan. J Pain Symptom Manage. 2003;26(5):1016–1025. doi:10.1016/S0885-3924(03)00330-0
8. De Boer M, Struys M, Versteegen G. Pain‐related catastrophizing in pain patients and people with pain in the general population. Eur J pain. 2012;16(7):1044–1052. doi:10.1002/ejp.2012.16.issue-7
9. Middleton C. Understanding the physiological effects of unrelieved pain. Nurs Times. 2003;99(37):28–31.
10. Ready B. Practice guidelines for acute pain management in the perioperative setting. Anesthesiology. 1995;82(4):1071–1081. doi:10.1097/00000542-199504000-00032
11. Oshvandi K, Fallahinia G, Naghdi S, Moghimbeygi A, Karkhanei B. Effect of pain management training on knowledge, attitude and pain relief methods of recovery nurses. J Nurs Educ. 2017;6:31–40.
12. Aziznejad R, Alhani F, Mohammadi E. Challenges and practical solutions for pain management nursing in pediatric wards. JBUMS. 2015;17(12):57–64.
13. Aziato L, Adejumo O. The Ghanaian surgical nurse and postoperative pain management: a clinical ethnographic insight. Pain Manag Nurs. 2014;15(1):265–272. doi:10.1016/j.pmn.2012.10.002
14. Chung J, Lui J. Postoperative pain management: study of patients’ level of pain and satisfaction with health care providers’ responsiveness to their reports of pain. Nurs Health Sci. 2003;5(1):13–21. doi:10.1046/j.1442-2018.2003.00130.x
15. Okuyama T, Wang XS, Akechi T, et al. Adequacy of cancer pain management in a Japanese cancer hospital. Jpn J Clin Oncol. 2004;34(1):37–42. doi:10.1093/jjco/hyh004
16. Sardá J
17. Meredith P, Strong J, Feeney JA. Adult attachment, anxiety, and pain self-efficacy as predictors of pain intensity and disability. Pain. 2006;123(1–2):146–154. doi:10.1016/j.pain.2006.02.025
18. Woby SR, Urmston M, Watson PJ. Self‐Efficacy mediates the relation between pain‐related fear and outcome in chronic low back pain patients. Eur J Pain. 2007;11(7):711–718. doi:10.1016/j.ejpain.2006.10.009
19. Keller A, Brox JI, Reikerås O. Predictors of change in trunk muscle strength for patients with chronic low back pain randomized to lumbar fusion or cognitive intervention and exercises. Pain Med. 2008;9(6):680–687. doi:10.1111/j.1526-4637.2007.00333.x
20. Barlow JH, Cullen LA, Rowe I. Educational preferences, psychological well-being and self-efficacy among people with rheumatoid arthritis. Patient Educ Couns. 2002;46(1):11–19. doi:10.1016/S0738-3991(01)00146-X
21. Buckelew SP, Murray SE, Hewett JE, Johnson J, Huyser B. Self‐efficacy, pain, and physical activity among fibromyalgia subjects. Arthritis Rheum. 1995;8(1):43–50. doi:10.1002/art.1790080110
22. Wilcox CE, Mayer AR, Teshiba TM, et al. The subjective experience of pain: an FMRI study of percept-related models and functional connectivity. Pain Med. 2015;16(11):2121–2133. doi:10.1111/pme.12785
23. Kurnia TA, Trisyani Y, Prawesti A. Factors associated with nurses’ self-efficacy in applying palliative care in intensive care unit. Jurnal Ners. 2019;13(2):219–226. doi:10.20473/jn.v13i2.9986
24. Asadi Noghabi A, Gholizadeh Gerdrodbari M, Zolfaghari M, Mehran A. Effect of application of critical-care pain observation tool in patients with decreased level of consciousness on performance of nurses in documentation and reassessment of pain. J hayat. 2012;18(3):54–65.
25. Macindo JRB, Soriano CAF, Gonzales HRM, Simbulan PJT, Torres GCS, Que JC. Development and psychometric appraisal of the pain management self‐efficacy questionnaire. J Adv Nurs. 2018;74(8):1993–2004. doi:10.1111/jan.13582
26. Plichta SB, Kelvin EA, Munro BH. Munro‘s Statistical Methods for Health Care Research. Wolters Kluwer Health/Lippincott Williams & Wilkins; 2013.
27. World Health Organisation. Process of translation and adaptation of instruments. Geneva: WHO. Available from: https://www.who.int/substance_abuse/research_tools/translation/en/. Accessed March 31, 2020.
28. Mokhlesi SS, Kariman N, Ebadi A, Khoshnejad F, Dabiri F. Psychometric properties of the questionnaire for urinary incontinence diagnosis of married women of Qom city in 2015. J Rafsanjan Univ Med Sci. 2017;15(10):955–966.
29. SharifNia H, Ebadi A, Lehto RH, Mousavi B, Peyrovi H, Chan YH. Reliability and validity of the persian version of templer death anxiety scale-extended in veterans of Iran–Iraq warfare. Iran J Psychiatry Behav Sci. 2014;8(4):29.
30. Sharif Nia H, Haghdoost AA, Ebadi A, et al. Psychometric properties of the King Spiritual Intelligence Questionnaire (KSIQ) in physical veterans of Iran-Iraq warfare. J Mil Med. 2015;17(3):145–153.
31. Ho R. Handbook of Univariate and Multivariate Data Analysis with IBM SPSS. Chapman and Hall/CRC; 2013.
32. Clark LA, Watson D. Constructing validity: basic issues in objective scale development. Psychol Assess. 1995;7(3):309. doi:10.1037/1040-3590.7.3.309
33. Vakili MM, Hidarnia AR, Niknami S. Development and psychometrics of an interpersonal communication skills scale (ASMA) among Zanjan health volunteers. J Hayat. 2012;18(1):5–19.
34. Sharif Nia H, Pahlevan Sharif S, Goudarzian AH, Haghdoost AA, Ebadi A, Soleimani MA. An evaluation of psychometric properties of the templer’s death anxiety scale-extended among a sample of Iranian chemical warfare veterans. J Hayat. 2016;22(3):229–244.
35. DeVellis R. Scale development: Theory and applications. Sage publications; 2016.
36. Polit DF, Yang F. Measurement and the Measurement of Change: A Primer for the Health Professions. Wolters Kluwer Health; 2015.
37. Wells-Federman C, Arnstein P, Caudill M. Nurse-led pain management program: effect on self-efficacy, pain intensity, pain-related disability, and depressive symptoms in chronic pain patients. Pain Manag Nurs. 2002;3(4):131–140. doi:10.1053/jpmn.2002.127178
38. Oslund S, Robinson R, Clark T, Garofalo J, Behnk P, Walker B. Long-term effectiveness of a comprehensive pain management program: strengthening the case for interdisciplinary care. Proc Bayl Univ Med Cent. 2009;22(3):211–214. doi:10.1080/08998280.2009.11928516
39. Twycross A. Children’s nurses’ post-operative pain management practices: an observational study. Int J Nurs Stud. 2007;44(6):869–881. doi:10.1016/j.ijnurstu.2006.03.010
40. Trail-Mahan T, Mao C, Bawel-Brinkley K. Complementary and alternative medicine: nurses’ attitudes and knowledge. Pain Manag Nurs. 2013;14(4):277–286. doi:10.1016/j.pmn.2011.06.001
41. De Ruddere L, Goubert L, Stevens M, Deveugele M, Craig K, Crombez G. Health care professionals’ reactions to patient pain: impact of knowledge about medical evidence and psychosocial influences. J Pain. 2014;15(3):262–270. doi:10.1016/j.jpain.2013.11.002
42. Chiang L, Chen H, Huang L. Student nurses’ knowledge, attitudes, and self-efficacy of children’s pain management: evaluation of an education program in Taiwan. J Pain Symptom Manage. 2006;32(1):82–89. doi:10.1016/j.jpainsymman.2006.01.011
43. Vincent C, Wilkie D, Szalacha L. Pediatric nurses’ cognitive representations of children’s pain. J Pain. 2010;11(9):854–863. doi:10.1016/j.jpain.2009.12.003
44. Song W, Eaton L, Gordon D, Hoyle C, Doorenbos A. Evaluation of evidence-based nursing pain management practice. Pain Manag Nurs. 2015;16(4):456–463. doi:10.1016/j.pmn.2014.09.001
45. Morriss W, Goucke R. Essential Pain Management: Workshop Manual. Australian and New Zealand College of Anaesthetists; 2011.
46. Ruben M, van Osch M, Blanch-Hartigan D. Healthcare providers’ accuracy in assessing patients’ pain: a systematic review. Patient Educ Couns. 2015;98(10):1197–1206. doi:10.1016/j.pec.2015.07.009
47. Edwards H, Nash R, Yates P, Walsh A, Fentiman B, McDowell J. Improving pain management by nurses: a pilot peer intervention program. Nurs Health Sci. 2001;3(1):35–45. doi:10.1046/j.1442-2018.2001.00069.x
48. Bandura A. Guide for constructing self-efficacy scales. Self Efficacy Beliefs Adolescents. 2006;5(1):307–337.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
