Back to Journals » Cancer Management and Research » Volume 13
The Prognostic Value of Baseline Distant Metastasis in Icotinib-Treated Patients with EGFR-Mutated Stage IV Non-Small Cell Lung Cancer
Authors Wang L, Shi T, Feng L, Fan Z, Xu X, Zhou X, Zhang X, Han J, Jing L, Liu J, Shan Y, Liu F, Zuo J, Wang Y
Received 23 December 2020
Accepted for publication 22 February 2021
Published 18 March 2021 Volume 2021:13 Pages 2613—2622
DOI https://doi.org/10.2147/CMAR.S298579
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Sanjeev K. Srivastava
Long Wang,1,* Tiantian Shi,1,* Li Feng,1 Zhisong Fan,1 Xiaoli Xu,2 Xinliang Zhou,1 Xue Zhang,1 Jing Han,1 Li Jing,1 Jiayin Liu,1 Yujie Shan,1 Fengling Liu,1 Jing Zuo,1 Yudong Wang1
1Department of Medical Oncology, The Fourth Hospital of Hebei Medical University, Shijiazhuang, 050011, People’s Republic of China; 2Department of Medical Records, The Fourth Hospital of Hebei Medical University, Shijiazhuang, 050011, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Yudong Wang Email [email protected]
Purpose: Several studies have revealed the prognostic value distant metastasis in non-small-cell lung cancer (NSCLC) patients receiving first-line epidermal growth factor receptor (EGFR) inhibitors. However, the question of whether the specific metastatic site could predict survival outcomes remain elusive. This study evaluated the prognostic value of specific metastatic site at diagnosis in first-line icotinib-treated patients with EGFR-mutated advanced NSCLC.
Methods: A total of 216 patients with EGFR-mutated stage IV NSCLC who received first-line icotinib treatment were retrospectively enrolled. The associations between the presence of distant metastasis to certain organs at diagnosis and survival outcomes were analyzed.
Patients and methods: The presence of distant metastases was not associated with progression-free survival. Patients with liver metastasis showed a significantly shorter OS than those without liver metastasis (14.6m vs 33.0m, p=0.024). Patients with brain metastasis showed a marginally shorter OS than those without brain metastasis (26.5m vs 33.8m, p=0.051). Patients with lung metastasis showed a significantly longer OS than those without lung metastasis (36.0m vs 28.6m, p=0.038). Multivariable Cox regression analysis showed the presence of liver metastasis (HR [hazard ratio]: 2.265, 95% CI [confidence interval]: 1.239– 4.139, p=0.008) and brain metastasis (HR: 1.493, 95% CI: 1.012– 2.202, p=0.043) were independent predictors for unfavorable OS, while lung metastasis (HR: 0.669, 95% CI: 0.460– 0.971, p=0.034) was an independent predictor for favorable OS.
Conclusion: The presence of liver and brain metastasis predicted unfavorable OS, while the presence of lung metastasis predicted favorable OS in first-line icotinib-treated patients with EGFR-mutated stage IV NSCLC.
Keywords: metastasis, non-small cell lung cancer, EGFR mutations, icotinib, prognostic value
Introduction
Lung cancer is the leading cause of cancer-related deaths worldwide.1 Non-small cell lung cancer (NSCLC) accounts for approximately 85% of cases. More than 40% of NSCLC patients present with distant metastasis at initial diagnosis including bone metastasis, brain metastasis, pleural metastasis, lung metastasis, liver metastasis or metastasis to other organs.2 Until the last decade, the 5-year survival rate of patients with metastatic disease is less than 10%.3
Epidermal growth factor receptor (EGFR) tyrosine kinase inhibitors (TKIs) have revolutionized the treatment of advanced NSCLC patients over the past decade.4–6 Icotinib is a first-generation EGFR-TKI that has been approved for the first-line treatment of EGFR-mutated locally advanced or metastatic NSCLC by the National Medical Products Administration of China in November 2014.7–9 Icotinib has comparable efficacy and better safety than gefitinib in a Phase III clinical trial.10
Bone is the most commonly seen metastatic site in advanced NSCLC patients at initial diagnosis. Bone metastasis is found in approximately 40% of NSCLC cases, followed by metastasis to lung, brain, and liver.11,12 Several studies have documented the prognostic value of the presence of distant metastasis in EGFR-mutated NSCLC patients receiving first-line EGFR-TKIs.13–16 Wu and colleagues demonstrated that bone metastasis was an independent risk factor for overall survival (OS), but no correlation between brain metastasis and OS was observed in patients with EGFR-mutated lung adenocarcinoma receiving front-line gefitinib.13 Conversely, Taniguchi and colleagues found that the presence of brain metastasis was correlated with unfavorable OS, while bone metastasis had no impact on OS.14 In addition, the presence of liver metastasis was associated with shorter OS in EGFR-mutated advanced NSCLC patients receiving first-line EGFR-TKIs.13,16 Although several studies have demonstrated the prognostic implications of the presence of distant metastasis, data on the specific metastatic site that could predict survival outcomes in EGFR-mutated NSCLC patients treated with first-line EGFR-TKIs are limited. Moreover, the prognostic value of distant metastasis at initial diagnosis in EGFR-mutated stage IV NSCLC patients treated with first-line icotinib remains largely unknown.
In the present work, EGFR-mutated stage IV NSCLC patients treated with first-line icotinib were retrospectively enrolled to investigate the prognostic role of distant metastasis at initial diagnosis and its relationship with survival outcomes including progression-free survival (PFS) and OS.
Patients and Methods
Patients
Our retrospective, observational study included 216 metastatic NSCLC patients treated with oral icotinib (125 mg, three times per day) as first-line setting at the fourth hospital of Hebei Medical University between July 2011 and October 2017 who met the inclusion and exclusion criteria. On initial diagnosis, all patients received extensive examinations including chest computed tomography (CT), abdominal ultra-sonography, whole-body bone scan and brain magnetic resonance imaging (MRI). The inclusion criteria for the present study were as follows: (1) with confirmed diagnosis of stage IV NSCLC by histopathological examinations according to the 7th American Joint Committee on Cancer (AJCC) staging manual; (2) older than 18 years; (3) harboring EGFR sensitizing mutations; (4) having an Eastern Cooperative Oncology Group performance status (ECOG PS) of 0–2; (5) having at least 1 measurable lesion according to Response Evaluation Criteria in Solid Tumors (RECIST) version 1.1; (6) receiving first-line icotinib. The exclusion criteria were as follows: (1) with small cell lung cancer or mixed small cell histology; (2) previously treated by targeted therapy or chemotherapy; (3) patients who were intolerant to icotinib; (4) with other malignant tumors. This study was approved by the Ethics Committee of the Fourth Hospital of Hebei Medical University and conducted in accordance with the Declaration of Helsinki. As this study is retrospective, the requirement for informed consent by the ethics committee was waived. All data on the patients were anonymized or maintained with confidentiality.
Baseline clinical characteristics of patients, including age, gender, smoking history, histological subtype, ECOG PS score, EGFR mutation type and distant metastases, were collected. Smoking status was categorized as current smokers and non-smokers including never smokers and ex-smokers (quit ≥5 years before diagnosis).
Initial treatment response to first-line icotinib therapy was classified as complete response (CR), partial response (PR), stable disease (SD) or progressive disease (PD) based on serial imaging studies using RECIST version 1.1.23 Objective response rate (ORR) was defined as the percentage of patients having CR and PR. Responders indicated patients having a CR/PR. Non-responders were patients having a SD/PD. PFS was defined as the interval between the initiation of the icotinib treatment and the time of PD, intolerable toxicity or death. OS was defined as the interval from the date of diagnosis to the date of death from any cause. Patients without an event were censored at the time of the last follow-up visit.
EGFR Mutation Analysis
EGFR mutation analysis was performed on 168 tumor tissue samples by using amplification refractory mutation system (ARMS; Therascreen EGFR Mutation Test kit, Qiagen Manchester Ltd., Manchester, UK), 26 by using next-generation sequencing (Burning Rock Biotech, Guangzhou, China), 12 by using direct sequencing and 10 by using denatured high-performance liquid chromatography.17–19
Statistical Analysis
The baseline characteristics, including age, gender, smoking history, ECOG PS, the presence of distant metastasis were compared between patients harboring deletion in exon 19 (19del) and point mutation L858R in exon 21, between responders and non-responders. Differences between two groups were calculated by chi-square test or Fisher’s exact test for categorical data and t-test for continuous variables. Differences among three groups were calculated by one-way ANOVA. Kaplan–Meier curves were compared by using the Log rank test for survival analyses. Univariate analysis and multivariate analysis with the Cox proportional hazards model were applied to investigate the impact of different variables on PFS and OS. p<0.05 was considered as statistically significant. All statistical analyses were performed in SPSS 22.0 (IBM, Armonk, NY, USA) and R language (version R3.3.3., https://www.r-project.org/). Kaplan-Meier curves were depicted using Graphpad Prism 5.0 software (GraphPad Software, San Diego, CA, USA).
Results
Patient Characteristics
A total of 216 stage IV NSCLC patients harboring EGFR gene mutations taking icotinib as their first-line treatment between July 2011 and October 2017 were enrolled in this study. The baseline clinical characteristics of the study population were summarized in Table S1. Ninety-one (42.1%) males and 125 (57.9%) females were included, with a median age of 59.4 years (ranged from 31 to 83 years). A majority of patients were non-smokers (82.9%; n=179) and the remaining 37 patients (17.1%) were current smokers. A majority (96.8%; n=209) of patients were diagnosed with adenocarcinoma, 4 (1.8%) with adenosquamous cell carcinoma, 2 (0.9%) with squamous cell carcinoma and 1 (0.5%) with large cell carcinoma. ECOG PS at initial diagnosis was PS 0 in 47.2% of patients, PS 1 in 50.9% of patients and PS 2 in 1.9% patients. Of 216 patients, 112 patients (51.9%) harbored 19del, 99 (45.8%) harbored point mutation L858R in exon 21, and 5 (2.3%) harbored point mutation G719 in exon 18. Distant metastases at initial diagnosis were mainly located in bone (44.9%), lung (42.1%), pleura (32.9%), brain parenchyma (27.3%) and extrathoracic lymph node (24.1%). Moreover, 19 patients (8.8%) had liver metastasis, 4.6% had adrenal metastasis, 2.8% had pericardial metastasis, 1.9% had leptomeningeal metastases, 0.9% had peritoneal metastasis and 3.2% had metastasis to other organs.
Association Between Distant Metastasis and Treatment Response to First-Line Icotinib
The ORR was 69.4% for patients treated with first-line icotinib. Next, the correlations between clinical features and initial treatment response to icotinib were evaluated. We found significant associations between treatment response to icotinib and the status of liver metastasis (p=0.001), the status of extrathoracic lymph node metastasis (p=0.001) and the number of metastatic organs (p=0.037). Meanwhile, the EGFR mutation type had no impact on treatment response (Table 1).
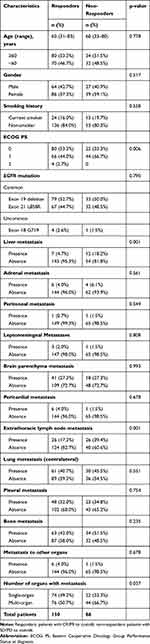 |
Table 1 The Difference of Basic Characteristics in Responders and Non-Responders |
The Predictive Value of Baseline Distant Metastasis on PFS
The median PFS of the study population was 10.3 months with 100% maturity (ranged from 1.0 to 43.4 months, Figure S1A). In order to determine the predictive value of distant metastasis and other clinical features on PFS, Cox proportional hazards regression model analysis was performed. The univariate analyses demonstrated that EGFR mutation type (hazard ratio [HR]: 0.694, 95% confidence intervals (CI): 0.530–0.909, p=0.008) and the status of extrathoracic lymph node metastasis (HR: 1.388, 95% CI: 1.014–1.899, p=0.04) were associated with PFS. In addition, a marginal association was observed between PFS and age (HR: 1.311, 95% CI: 0.999–1.720, `p=0.051; Table 2). The multivariate analysis revealed that only EGFR mutation type (HR: 0.707, 95% CI: 0.539–0.927, p=0.012) remained the significant association with PFS (Table 2).
 |
Table 2 Univariable and Multivariable Analyses for Identifying Risk Factors Associated with PFS |
Survival analyses using the Kaplan–Meier method and Log rank test showed the significantly different PFS in patients harboring G719 point mutations in exon 18, L858R point mutations in exon 21 and 19del (10.3 months vs 9.5 months vs 11.2 months, p=0.03, Figure S2A). The PFS was comparable between patients harboring G719 and those harboring 19del (10.3 months vs 11.2 months, p=0.23, Figure S2B). The comparable PFS was also observed in patients harboring G719 and those harboring L858R (10.3 months vs 9.5 months, p=0.99, Figure S2C). However, the significantly longer PFS in patients harboring 19del compared with those harboring L858R was observed in our study (11.2 months vs 9.5 months, p=0.009, Figure S2D). The baseline characteristics between patients harboring 19del and L858R were comparable (Table S2). Collectively, distant metastases were not associated with PFS; however, harboring EGFR 19del predicted longer PFS compared to other EGFR mutations.
The Prognostic Value of Baseline Distant Metastasis on OS
The median OS of the 216 patients was 32.1 months with 61.1% maturity (ranged from 2.3 to 67.0 months, Figure S1B). In order to determine whether the presence of distant metastases was associated with OS in patients, survival analysis and Cox proportional hazards regression model analysis were performed. Survival analyses showed that patients with liver metastasis had a significantly shorter OS than those without liver metastasis (14.6 months vs 33.0 months, p=0.024, Figure 1A). Patients with brain metastasis showed a marginally shorter OS compared with those without brain metastasis (26.5 months vs 33.8 months, p=0.051, Figure 1B). Meanwhile, patients with lung metastasis showed a longer OS than those without lung metastasis (36.0 months vs 28.6 months, p=0.038, Figure 1C).
In the univariate Cox proportional hazards regression model, age (HR: 1.491, 95% CI: 1.053–2.111, p=0.025), ECOG PS (HR: 0.596, 95% CI: 0.419–0.847, p=0.004), status of liver metastasis (HR: 1.867, 95% CI: 1.077–3.238, p=0.026), the status of extrathoracic lymph node metastasis (HR: 1.714, 95% CI: 1.177–2.496, p=0.005) and the status of lung metastasis (HR: 0.689, 95% CI: 0.483-0.982, p=0.040) were associated with OS. The status of brain parenchyma metastasis (HR: 1.453, 95% CI: 0.996–2.120, p=0.053) and the status of bone metastasis (HR: 1.367, 95% CI: 0.967–1.931, p=0.076) showed a marginal association with OS. In the multivariate Cox proportional hazards regression model, age (HR: 1.806, 95% CI: 1.238–2.633, p=0.002), the status of liver metastasis (HR: 2.265, 95% CI: 1.239–4.139 p=0.008), the status of brain parenchyma metastasis (HR: 1.493, 95% CI: 1.012–2.202, p=0.043) and the status of lung metastasis (HR: 0.669, 95% CI: 0.460–0.971, p=0.034) retained the significant association with OS (Table 3). Collectively, the presence of liver metastasis and the presence of brain metastasis and absence of lung metastasis were independent risk factors associated with OS outcomes.
 |
Table 3 Univariable and Multivariable Analyses for Identifying Risk Factors Associated with OS |
Association of Baseline Distant Metastasis with OS
In order to further investigate the associations of metastasis to certain organs with OS outcomes, survival analyses were performed in three groups as follows (1) patients with lung metastasis, without brain and liver metastasis (lung+ liver- brain- metastasis), (2) patients with brain metastasis, without lung and liver metastasis (brain+ lung- liver- metastasis), (3) patients with liver metastasis, without lung and brain metastasis (liver+ lung- brain- metastasis). The median OS was 46.5 months for patients with lung+ liver- brain- metastasis (n=60), 26.5 months for patients with brain+ lung- liver- metastasis (n=32), and 14.6 months for patients with liver+ lung- brain- metastasis (n=8). The OS was significantly different in three groups (p=0.002, Figure 2A). Furthermore, patients with lung+ liver- brain- metastasis had a significantly longer OS than those with liver+ lung- brain- metastasis (46.5 months vs 14.6 months, p=0.001, Figure 2B). Patients with brain+ lung- liver- metastasis also had a significantly longer OS than those with liver+ lung- brain- metastasis (26.5 months vs 14.6 months, p=0.040, Figure 2C). The significantly shorter OS was observed in patients with brain+ lung- liver-metastasis compared with those with lung+ liver- brain- metastasis (26.5 months vs 46.5 months, p=0.002, Figure 2D). Collectively, the presence of liver metastasis predicted unfavorable OS, while lung metastasis predicted more favorable OS in patients with lung/brain/liver metastasis.
Next, Kaplan–Meier estimates of OS were performed and subgroups were compared using the Log rank test to investigate the impact of bone metastasis on OS. OS was comparable in patients with bone- brain+ liver- lung- metastasis (n=12) and those with bone+ brain+ liver- lung- metastasis (n=20) (25.8 months vs 33.0 months, p=0.608, Figure S3A). OS did not differ significantly between patients with bone+ liver+ brain- lung- metastasis (n=4) and patients with bone- liver+ brain- lung- metastasis (n=4) (15.6 months vs 10.8 months, p=0.438, Figure S3B). In addition, there were no statistically significant differences between the Kaplan–Meier OS curves of patients with bone+ lung+ brain- liver- metastasis (n=15) and patients with bone- lung+ brain- liver- metastasis (n=45) (35.5 months vs 50.5 months, p=0.051, Figure S3C). These results were consistent with the results from the multivariate analysis with Cox proportional hazards regression model indicating that the presence of bone metastasis was not associated with OS.
Discussion
The prognostic value of distant metastasis at the time of diagnosis has been demonstrated in advanced NSCLC patients receiving gefitinib or erlotinib as first-line therapy;13,14,16 however, the prognostic value of distant metastasis in patients receiving first-line icotinib remains unclear. In this study, we analyzed the prognostic role of distant metastasis at diagnosis and its relationship with survival outcomes including PFS and OS in patients with EGFR-mutated stage IV NSCLC treated with first-line icotinib. Our work demonstrated that the presence of liver metastasis and brain metastasis were independent predictors of unfavorable OS, while the presence of lung metastasis was an independent predictor of favorable OS. In addition, harboring 19del predicted a longer PFS compared to other mutations.
Icotinib, a first-generation EGFR-TKI, has been approved for the treatment of locally advanced or metastatic EGFR-mutated NSCLC. The prior studies showed an ORR of 62.9% and a median PFS of 11.2 months in advanced NSCLC patients harboring 19 del or L858R treated with first-line icotinib.8,20 Our study observed a similar ORR of 69.6% and a median PFS of 10.3 months from our cohort.
Our data showed that the most frequently seen metastatic site at initial diagnosis were bone (44.9%), lung (42.1%) and pleura (32.9%), which were in an agreement with the previous studies that NSCLC metastasize predominantly to bone with a rate of 45–55%, lung with 33–45%, pleura with 30–62% at initial diagnosis in stage IV NSCLC patients.11,13,15 The rates of brain metastasis in stage IV NSCLC patients are variable. The previous studies reported that 10–37% of patients harbored brain metastases at initial diagnosis.12,21 The frequency of brain metastasis achieved 27.3% in this study. Liver is the least common metastatic site of NSCLC than bone, lung, pleura and brain.13,15 In this study, the rate of liver metastasis in patients was 8.8%. We found that the presence of liver metastasis was an independent predictor of shorter OS for patients with EGFR-mutated stage IV NSCLC who received icotinib as first-line treatment, which was in an agreement with prior studies.13,14
Bone and brain are common metastatic sites for NSCLC. Our work revealed that brain metastasis was the independent predictor of OS and bone metastasis had no impact on OS, which was consistent with a prior study indicating that brain metastasis rather than bone metastasis predicted poor OS in EGFR-mutated advanced NSCLC patients treated with first-line EGFR-TKIs.16 However, there are different opinions on associations of bone/brain metastasis with OS. Another study demonstrated that bone metastasis rather than brain metastasis predicts poor OS in patients.13 These inconclusive results may be attributed to the inclusion of a small sample size.
Lung is another common metastatic site for NSCLC. Compared to liver and brain metastasis, patients with lung metastasis had a significantly longer OS than those without lung metastasis at initial diagnosis. Furthermore, among patients with liver, brain or lung metastasis at initial diagnosis, patients with liver metastasis had the worst OS, followed by patients with brain metastasis, while patients with lung metastasis had the best OS. The OS risk for patients can be summarized as liver metastasis > brain metastasis > lung metastasis. Our results supported evidence from previous studies indicating that lung metastasis predicted the best chance of survival while liver metastasis predicted worst outcomes in patients with advanced NSCLC.22,23
Previous studies have shown that 19del predicted a better PFS and OS than L858R in patients treated with first-line EGFR-TKIs.24,25 In the present work, we also found that harboring 19del was associated with favorable PFS in patients treated with icotinib as first-line therapy.
Our study had several limitations. First, the sample size for investigating the associations between prognostic value of distant metastasis and survival outcomes was small, which might weaken the statistical significance of our conclusion. Second, the difference of OS in patients with liver metastasis alone, brain metastasis alone, lung metastasis alone was not evaluated due to the small sample size. Third, the status of EGFR T790M mutation and the type of subsequent treatment evidenced as prognostic factors associated with survival outcome were not included in multivariable analysis of OS, due to the status of EGFR T790M mutation at progression on first-line icotinib and the type of subsequent treatment in majority of patients were unknown. The prognostic implications of liver, brain and lung metastasis should be validated in larger cohorts.
Conclusion
In conclusion, our work demonstrated the prognostic value of distant metastasis at initial diagnosis in EGFR-mutated stage IV NSCLC patients treated with first-line icotinib. We found that the presence of liver and brain metastasis were independent predictors of unfavorable OS; while the presence of lung metastasis was an independent predictor of favorable OS. This study provided clinical evidence for the prognostic impact of distant metastases at initial diagnosis in patients with EGFR-mutated stage IV NSCLC treated with first-line icotinib, which might serve as an important reference for clinicians for disease management.
Acknowledgments
This work was supported by the Natural Science Foundation of Hebei Province (H2020206551).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70:7–30. doi:10.3322/caac.21590
2. Edge SB, Compton CC. The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol. 2010;17:1471–1474. doi:10.1245/s10434-010-0985-4
3. Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT. The eighth edition lung cancer stage classification. Chest. 2017;151:193–203. doi:10.1016/j.chest.2016.10.010
4. Zhou C, Wu YL, Chen G, et al. Erlotinib versus chemotherapy as first-line treatment for patients with advanced EGFR mutation-positive non-small-cell lung cancer (OPTIMAL, CTONG-0802): a multicentre, open-label, randomised, Phase 3 study. Lancet Oncol. 2011;12:735–742. doi:10.1016/S1470-2045(11)70184-X
5. Mok TS, Wu YL, Thongprasert S, et al. Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma. N Engl J Med. 2009;361:947–957. doi:10.1056/NEJMoa0810699
6. Yang JC, Wu YL, Schuler M, et al. Afatinib versus cisplatin-based chemotherapy for EGFR mutation-positive lung adenocarcinoma (LUX-Lung 3 and LUX-Lung 6): analysis of overall survival data from two randomised, phase 3 trials. Lancet Oncol. 2015;16:141–151. doi:10.1016/S1470-2045(14)71173-8
7. Zhou Q, Zhang XC, Chen ZH, et al. Relative abundance of EGFR mutations predicts benefit from gefitinib treatment for advanced non-small-cell lung cancer. J Clin Oncol. 2011;29:3316–3321. doi:10.1200/JCO.2010.33.3757
8. Shi YK, Wang L, Han BH, et al. First-line icotinib versus cisplatin/pemetrexed plus pemetrexed maintenance therapy for patients with advanced EGFR mutation-positive lung adenocarcinoma (CONVINCE): a phase 3, open-label, randomized study. Ann Oncol. 2017;28:2443–2450. doi:10.1093/annonc/mdx359
9. Shi Y, Sun Y, Ding C, et al. China experts consensus on icotinib for non-small cell lung cancer treatment (2015 version). Ann Transl Med. 2015;3:260. doi:10.3978/j.issn.2305-5839.2015.10.30
10. Shi Y, Zhang L, Liu X, et al. Icotinib versus gefitinib in previously treated advanced non-small-cell lung cancer (ICOGEN): a randomised, double-blind phase 3 non-inferiority trial. Lancet Oncol. 2013;14:953–961. doi:10.1016/S1470-2045(13)70355-3
11. Fujimoto D, Ueda H, Shimizu R, et al. Features and prognostic impact of distant metastasis in patients with stage IV lung adenocarcinoma harboring EGFR mutations: importance of bone metastasis. Clin Exp Metastasis. 2014;31:543–551. doi:10.1007/s10585-014-9648-3
12. Khalifa J, Amini A, Popat S, Gaspar LE, Faivre-Finn C. Brain metastases from NSCLC: radiation therapy in the era of targeted therapies. J Thorac Oncol. 2016;11:1627–1643. doi:10.1016/j.jtho.2016.06.002
13. Wu KL, Tsai MJ, Yang CJ, et al. Liver metastasis predicts poorer prognosis in stage IV lung adenocarcinoma patients receiving first-line gefitinib. Lung Cancer. 2015;88:187–194. doi:10.1016/j.lungcan.2015.02.012
14. Jiang T, Cheng R, Zhang G, et al. Characterization of liver metastasis and its effect on targeted therapy in EGFR-mutant NSCLC: a multicenter study. Clin Lung Cancer. 2017;18:631–639 e632. doi:10.1016/j.cllc.2017.04.015
15. Chang YP, Chen YM, Lai CH, et al. The impact of de novo liver metastasis on clinical outcome in patients with advanced non-small-cell lung cancer. PLoS One. 2017;12:e0178676. doi:10.1371/journal.pone.0178676
16. Taniguchi Y, Tamiya A, Nakahama K, et al. Impact of metastatic status on the prognosis of EGFR mutation-positive non-small cell lung cancer patients treated with first-generation EGFR-tyrosine kinase inhibitors. Oncol Lett. 2017;14:7589–7596. doi:10.3892/ol.2017.7125
17. Shaozhang Z, Ming Z, Haiyan P, Aiping Z, Qitao Y, Xiangqun S. Comparison of ARMS and direct sequencing for detection of EGFR mutation and prediction of EGFR-TKI efficacy between surgery and biopsy tumor tissues in NSCLC patients. Med Oncol. 2014;31:926. doi:10.1007/s12032-014-0926-3
18. Cohen V, Agulnik JS, Ang C, et al. Epidermal growth factor receptor mutations detected by denaturing high-performance liquid chromatography in nonsmall cell lung cancer: impact on response to therapy with epidermal growth factor receptor-tyrosine kinase inhibitors. Cancer. 2010;116:4309–4317. doi:10.1002/cncr.25214
19. Popper HH, Ryska A, Tímár J, Olszewski W. Molecular testing in lung cancer in the era of precision medicine. Transl Lung Cancer Res. 2014;3:291–300. doi:10.3978/j.issn.2218-6751.2014.10.01
20. Zhao Y, Liu J, Cai X, et al. Efficacy and safety of first line treatments for patients with advanced epidermal growth factor receptor mutated, non-small cell lung cancer: systematic review and network meta-analysis. BMJ. 2019;367:l5460. doi:10.1136/bmj.l5460
21. Gril B, Evans L, Palmieri D, Steeg PS. Translational research in brain metastasis is identifying molecular pathways that may lead to the development of new therapeutic strategies. Eur J Cancer. 2010;46:1204–1210. doi:10.1016/j.ejca.2010.02.033
22. Shan Q, Li Z, Lin J. et al. Tumor primary location may affect metastasis pattern for patients with stage IV NSCLC: a population-based study. J Oncol;2020. 1–8. doi:10.1155/2020/4784701
23. Yang J, Zhang Y, Sun X, et al. The prognostic value of multiorgan metastases in patients with non-small cell lung cancer and its variants: a SEER-based study. J Cancer Res Clin Oncol. 2018;144:1835–1842. doi:10.1007/s00432-018-2702-9
24. Jiang H, Zhu M, Li Y, Li Q. Association between EGFR exon 19 or exon 21 mutations and survival rates after first-line EGFR-TKI treatment in patients with non-small cell lung cancer. Mol Clin Oncol. 2019;11:301–308. doi:10.3892/mco.2019.1881
25. Choi YW, Jeon SY, Jeong GS, et al. EGFR Exon 19 deletion is associated with favorable overall survival after first-line gefitinib therapy in advanced non-small cell lung cancer patients. Am J Clin Oncol. 2018;41:385–390. doi:10.1097/COC.0000000000000282
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


