Back to Journals » Journal of Pain Research » Volume 12
The influence of patient race, sex, pain-related body postures, and anxiety status on pain management: a virtual human technology investigation
Authors Clark J, Robinson ME
Received 21 March 2019
Accepted for publication 2 August 2019
Published 30 August 2019 Volume 2019:12 Pages 2637—2650
DOI https://doi.org/10.2147/JPR.S209510
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Michael A Ueberall
Jaylyn Clark, Michael E Robinson
Department of Clinical and Health Psychology, University of Florida, Gainesville, FL, USA
Correspondence: Michael E Robinson
Department of Clinical and Health Psychology, University of Florida, 101 South Newell Drive, Rm 3151, PO Box 100165, Gainesville, FL 32610-9165, USA
Tel +1 352 273 5220
Fax +1 352 273 6156
Email [email protected]
Purpose: The purpose of this study was to examine mechanisms underlying disparities in pain management among patients with psychological comorbidities. Studies have consistently shown that health care providers, health care trainees, and laypeople are susceptible to biased assessment and treatment decisions for patients presenting with pain. Further, psychological factors may influence the use of demographic and behavioral cues in pain assessment and treatment decisions. The present study employed innovative virtual human technology to capture decision-making approaches at both the group- and individual-level to better elucidate the influence of psychological factors, demographic cues, and pain-related body postures on pain assessment and treatment decisions.
Patients and methods: One hundred and thirty-two providers and trainees in the areas of nursing, physical therapy, and medicine viewed separate, empirically validated virtual human profiles that systematically varied across pain behaviors, anxiety status, race, and sex. Participants provided pain assessment and treatment ratings using a visual analog scale for each virtual human profile.
Results: Idiographic analyses revealed that participants used patient pain-related body postures most consistently and reliably across ratings. Nomothetic analyses showed anxious virtual humans were identified as having more anxiety and more likely to be recommended anti-anxiety medications, especially by female participants.
Conclusion: This innovative study successfully explored the influence of patient pain-related body postures, anxiety status, and demographic characteristics on pain management decisions with virtual human technology and a Lens model design. Results of this study can be used to better inform clinical practice, research, and education regarding the influence of patient variables on pain assessment and treatment decisions.
Keywords: pain management, disparities, demographic variables
Introduction
Chronic pain affects approximately 116 million adults in the United States and is one of the most common reasons why individuals decide to seek medical treatment.1 Recent estimates suggest that chronic pain conditions account for 600 billion dollars per year in lost productivity and health care expenses.2 Unfortunately, the complex, multifaceted nature of this nearly universal condition contributes to difficulties with effective pain management. Furthermore, pain management is challenging due to subjective and emotional elements of pain perception.3 Health care providers also report complications in delivery of appropriate pain management due to inconsistent treatment guidelines that lack evidence-based support and adequate instruction.4 Although self-report remains the gold standard for pain assessment, research indicates health care providers underestimate the severity of patient pain when compared to self-report. As a result, health care providers, health care trainees, and laypeople often rely on their own judgments to make pain management decisions.5 Further, research shows there is meaningful variability in patient pain ratings within and across provider profession.6–11 Several studies using virtual human technology have shown much of this variability is related to patient demographic characteristics, such as patient race, sex, and age.12–20 While the use of cues can be logical and appropriate in certain contexts, biased provider judgments can contribute to negative patient outcomes, such as inappropriate, inadequate, and delayed care.
Sex disparities in patient care
Regarding sex disparities, studies have reported that women are more likely to receive psychotropic medication for pain,14,21 less likely to receive opioid analgesia,22,23 and more likely to have pain attributed to emotional/psychological factors when compared to men.24,25 Relatedly, previous studies using virtual human technology found that participants rated male virtual human patients as having higher pain than female virtual human patients even though all patients presented the same pain behaviors.26 Male virtual human patients were also more likely to have their pain treated more aggressively than female virtual human patients.27 Overall, the existing literature overwhelmingly reflects sex differences in provider management of pain.
Race disparities in patient care
Providers’ beliefs and expectations of patients are influenced by patient race and ethnicity. These beliefs and expectations have been shown to lead to variations in decision-making policies, often resulting in suboptimal pain management. This pattern is especially evident for ethnic minorities suffering from chronic pain. Some studies indicate ethnic differences in health care providers’ ability to correctly interpret their patient’s pain while other studies find no significant difference in pain interpretation across patient race.28 Fairly consistent evidence suggests racial/ethnic minorities suffer disproportionately from unrelieved pain. For example, African-Americans report higher levels of pain from conditions, such as AIDS,29 glaucoma,30 migraine headaches,31 and postoperative pain.32 Clinically, compared to other groups, racial/ethnic minorities are less likely to be prescribed pain medication than Caucasian patients across experimental settings.33 A meta-analysis concluded Caucasians were more likely to receive opioids than racial/ethnic minorities.34 Notably, research on pain care across race is not entirely consistent. One investigation35 found that – counter to previous reports – virtual human patients who were female, African-American, and older were rated as having greater pain and were more likely to be administered medication relative to their demographic counterparts. Taken together, disparities in pain management decisions among minorities have been reported across a variety of conditions and treatment settings.36
Patient anxiety and pain
Pain is affected by both sensory and emotional experiences;37 therefore, accurate assessment of patient pain can be confounded by psychological factors, such as anxiety.38 The terms fear and anxiety are often used interchangeably with regard to pain. The distinction between anxiety and fear is theoretically correct, but difficult to differentiate in clinical settings, especially when chronic pain is constantly present. Given the debate related to the clinical distinctiveness of fear and anxiety, we decided to use the term pain-related anxiety.
Unfortunately, less is known about discrepancies in the assessment and treatment of pain among patients with psychological disorders. The small literature suggests there are disparities in patient care based on psychological comorbidities. Evidence14,24 shows providers may perceive female patients’ pain as primarily psychological in nature, while they perceive males’ pain as being physical in nature. Rochlen et al39 found providers also perceive men as more resistant to psychological treatments. Pain management in the context of mood is further complicated by concerns regarding opioid prescribing and the higher risk of abuse in patients with comorbid mood disorders.40 The aforementioned results suggest clinically screening for anxiety is essential due to its independent, adverse effects on functional impairment, and treatment response. Screening and addressing pain-related anxiety may be a successful intervention in reducing disability among chronic pain patients. Thus, detecting and treating anxiety may be an important component of pain management.41 However, the relationship between anxiety status and pain management remains unclear. Further questions remain related to the interaction of anxiety status and patient demographic characteristics on pain management.
Patient pain behaviors
Health care providers also make conclusions regarding patients’ pain experience from observable pain behaviors. Unbiased assessment of patient pain (eg, behaviors that reflect a person is experiencing pain) is essential because providers base decisions about patient’s pain experience, in part, from observable behaviors.42,43 Individuals suffering from back pain commonly exhibit the following pain behaviors: guarded movement, bracing, rubbing, touching the painful area, grimacing, and sighing.42 These behaviors are readily assessed while walking patients to and from waiting rooms and while interacting with patients. This assessment is particularly advantageous when patients do not have the verbal skills to effectively communicate their pain experience or when verbal report is significantly influenced by external factors.43 Interpretation of pain-related body postures is a reliable and valid method of pain assessment. For example, study results indicate pain-related body postures correlate with patients’ ratings of pain among both clinicians and laypeople. Furthermore, changes in observed behaviors correlate with changes in patients’ ratings of pain.44 To our knowledge, there is one study examining the influence of pain-related body postures on pain management decisions for chronic pain patients. From this study, researchers26 found men were rated by laypeople as experiencing more pain than females exhibiting the same pain-related body postures. Additionally, these findings have not yet been generalized to clinical settings. Research has yet to determine whether health care providers base pain management decisions, in part, on pain-related body postures among patients with comorbid psychological disorders.
Provider characteristics and pain management
Provider characteristics potentially contribute to disparities in pain management, further highlighting the need for research in this area. Some evidence shows provider age, sex, and years of experience are correlated with pain management decisions. However, there is a surprisingly scarce amount of literature exploring this subject. Evidence suggests provider sex differentially influences pain treatment decisions, as three separate studies45–47 revealed male and female providers prescribe more analgesics to same sex patients. Provider sex may also interact with patient race to affect pain management. For example, a vignette study47 reported that African-American patients were more likely to receive higher doses of opioid and non-opioid analgesics from female providers, despite one study finding no differences in analgesic administration across provider sex.48 Specifically, one study found female providers were more likely to prescribe higher doses of hydrocodone to African-American than to Caucasian patients. Conversely, Caucasian patients were found to receive higher doses from male providers.47 Unfortunately, there are few studies examining the impact of provider race on pain management due to homogenous samples. Thus, the degree to which health care provider characteristics affect pain management is not clear. However, the previously mentioned studies provide consistent evidence that provider characteristics independently affect pain management decisions. In order to minimize disparities in pain management, it is important to become aware of these potential biases and cues that directly impact patient care.
Virtual human technology and pain assessment
Virtual human technology provides a model for exploring the influence of both provider and patient characteristics on pain management decisions in that it allows researchers to create systematic variations in patient pain behaviors and demographic characteristics (eg, sex, race, age). The standardization of these characteristics helps control for biases associated with other confounding factors that contribute to inequalities in pain management (eg, interactions between patient/provider). Virtual human technology is readily accessible, ultimately facilitating the identification of unknown factors that influence pain management decisions.
In the previous virtual human research, researchers found undergraduate students, health care trainees, and health care professionals used race and gender, in part, to make pain management decisions.18–20 More specifically, one investigation exploring depression and pain management49 found that patient mood had the strongest and most reliable influence on pain treatment decisions. A separate study found that participants assessed male virtual human patients as experiencing increased levels of pain as compared to female virtual human patients exhibiting the same validated pain-related body postures.26
Aims
Broadly, the purpose of this study was to explore the influence of patient psychological factors and pain-related body postures on provider pain assessment and treatment, particularly within the context of patient demographic cues. We hypothesized the overall sample of health care providers and trainees would give higher pain assessment and treatment ratings to virtual human patients presenting with symptoms of anxiety. We also hypothesized that the influence of patient anxiety status on pain assessment and treatment decisions made by health care providers and trainees would differ by patient race and sex. Finally, we hypothesized that the influence of patient anxiety status on pain assessment and treatment decisions made by health care providers and trainees would differ by provider race and sex.
Materials and methods
Participants were recruited via mail, advertisements, and fliers requesting volunteers to participate in this study. Eligibility requirements for participants were to be 1) at least 18 years of age or older, 2) able to read and understand English, and 3) a practicing health care professional or trainee. Recruiting efforts sought students and health care professionals in the areas of Physical Therapy, Medicine, and Nursing. Participation was contingent upon the ability to give consent. Participants who expressed interest in participating in the study were directed to a secure website to complete the study. Each participant was asked to read a description of the study including the time required to complete the study and a reminder that the study is voluntary. After reading the study description, all participants read and signed a computerized consent form acknowledging that the study procedures were explained and that they could withdraw from the study at any time, without penalty. Based on previous studies using virtual human technology and a power analysis, a total sample size of 100 was estimated to detect significant effects at power =0.80. For individual-level analyses, a sufficient profile-to-cue ratio was needed to estimate adequate power. However, this ratio was balanced with participant demand due to an increased number of profiles. The lowest recommended profile-to-cue ratio is 5:1;50 for this study, we adopted a profile-to-cue ratio of 8:1 to ensure adequate power. Previous work using idiographic analyses has consistently proven this ratio to be sufficient in estimating stable regression coefficients.35,49,50
Demographic questionnaire and pain ratings
Volunteers completed a brief demographic questionnaire that collected participants’ age, race, sex, and area of practice. Participants indicated whether they were a practicing health care provider and/or currently enrolled in a training program. Finally, participants rated their level of clinical experience with chronic pain on a 0–100 VAS anchored at “not at all experienced” and “very experienced”. Participants then read a set of instructions that provided information on how to approach the task and use VASs to give pain management ratings. Subsequently, participants indicated the likelihood that he/she would consider/recommend the pain assessment and treatment practices listed below in the care of their virtual human patient: 1) rating of pain intensity, 2) recommendation of anti-anxiety medication, 3) recommendation of opioid pain medication, 4) recommendation of over-the-counter (OTC) or nonsteroidal anti-inflammatory drugs (NSAIDs) pain medication (eg, ibuprofen), 5) referral to a mental health provider for counseling, 6) referral to a multi-disciplinary pain management center, and 7) rating of anxiety level. The 0–100 VAS were anchored from “not at all likely” to “extremely likely” and were presented randomly to each participant in order to control for order effects.
Procedures
Converging evidence support the use of virtual human technology in exploring the decision-making process of laypersons, health care trainees, and health care providers.19,20,35,51,52 Lens model design and virtual human technology were used to enhance experimental control and to parse individual differences in clinicians’ decisions. The Lens model is mostly used to determine how individuals attend to and use information in their environment to make decisions.50 Using this model, studies present participants with a series of profiles containing cues that are used to make a decision. When observing a patient profile, participants in our study read the following clinical vignette of a patient experiencing low back pain:
The patient presents with low back pain of approximately one-year duration. The patient reports that the pain began after lifting a heavy box at home. The pain is located in the lower back and limits the patient’s ability to perform normal daily activities. The patient expresses an openness to any treatment recommendation and has no absolute contraindications for the treatments listed below (e.g., there are no medical reasons to avoid certain treatments). The patient denies any other physical or mental health symptoms. (Alternative: The patient denies any other physical health symptoms. The patient does report symptoms of anxiety [e.g., muscle tension, restlessness, sleep disturbance, difficulty with concentration, irritability] over the past 6 months.)
Each participant viewed separate, empirically validated virtual human profiles along with a 20-s loop video of a virtual human, a clinical vignette of a patient with low back pain, and vital signs. The vital signs varied across patients but remained within normal limits. The patient profiles were also presented randomly to control for order effects. Text vignettes contained information about the patient’s medical and anxiety status (symptoms present or not). Each virtual human profile also displayed a different combination of demographic characteristics, including sex (male or female), race (African-American or Caucasian), and pain behavior (high or low). Sixteen unique patient profiles were needed to represent each possible cue combination once (2 levels of sex×2 levels of race×2 levels of anxiety status×2 levels of pain behavior =16). To enhance statistical power, we used 32 patient profiles so each cue combination was presented twice (8:1 profile-to-cue ratio).
In order to obtain realistic virtual human bodies displaying back pain, two physical therapists modeled behaviors of patients walking with and without back pain.42 The behaviors were recorded using Autodesk® MotionBuilder® which captured the physical therapists’ motions onto stick figures devoid of sex and race features. The two animations were created in order to accurately reflect patients expressing high and low back pain-related body postures. One hundred percent of a validation sample (17/17 participants) accurately identified high versus low pain stick figures which indicated representativeness of the stick figures. After the motion capture data were validated, virtual human bodies (eg, men, women, Caucasian, African-American patients) from Evolver® software were mapped onto the stick figures. Pilot testing of the profiles established that differences in the cues of interest were readily discernible upon viewing26 and independent t-test analysess validated that participants were able to distinguish between high and low pain-related body postures. The study took approximately 45 mins to complete and participants were compensated with a $15 Target gift card. This study was approved by the Institutional Review Board at the University of Florida (IRB201701280).
Statistical analyses
All data were analyzed using SPSS for Windows (v22). Descriptive analyses were conducted to summarize the demographic characteristics of the sample. Both individual (idiographic) and group-level (nomothetic) analyses were conducted to calculate the unique influence of the cues on pain management decisions. Individual-level multiple regressions were used to examine each participant’s data. Standardized regression coefficients (beta weights) for each independent variable indicated the unique contribution of that variable across the participant’s pain assessment and treatment decisions. Semi-partial correlation coefficients were squared to quantify the amount of variance accounted for by each cue in participants’ decisions. A significant R2 indicated the participant consistently used one or more of the cues in their decision-making approach.
For group-level analyses, average participant assessment and treatment ratings were calculated across anxiety cue (eg, anxiety status). Type of professional was used as a covariate due to potential differences among these groups in pain management ratings. Then, a series of repeated measures analysis of covariance were conducted to examine pain management decisions made by participants as a function of each virtual human’s anxiety status. Consistent with previous Lens model studies examining pain decision-making policies, we examined the results of individual-level analyses at both p<0.05 and p<0.10. The significance level for group-level analyses was set to p<0.05. Generalized eta-squared coefficients were calculated for effect size.
Results
Participants
One hundred and thirty-two individuals participated in the study and 71% were female. The majority of participants self-reported their race as Caucasian (75%), while 11% identified as Asian, 2.3% as “Other”, 6.8% as African-American or Black, and 3.8% as Hispanic. The average age of the sample was approximately 25 years (SD=5.23). About 86% of the sample reported being a student and the average years of experience was 1.71 (SD=4.34). The most frequently endorsed profession was Nursing (39%), followed by Medicine (37%), and Physical Therapy (24%). Detailed demographic and background information is provided in Table 1.
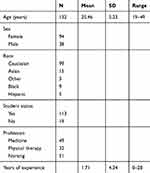 |
Table 1 Demographic and background characteristics of participants |
Nomothetic analyses
Average participant assessment and treatment ratings were calculated across virtual patients at each level of cue. These averages are presented in Table 2. Main effects are presented in Table 3; interaction effects of patient anxiety status and sex are presented in Table 4, interaction effects of patients anxiety status and race are presented in Table 5, and interaction effects of patient anxiety status and provider sex are presented in Table 6.
 |
Table 2 Means and standard deviations for ratings within cue use |
 |
Table 3 Main effects of patient anxiety status on ratings |
 |
Table 4 Interaction effect of patient anxiety status, patient sex, and ratings |
 |
Table 5 Interaction effects of patient anxiety status, patient race, and ratings |
 |
Table 6 Interaction effects of patient anxiety status, provider sex, and ratings |
Influence of anxiety
Results revealed a significant main effect for likelihood of recommending an anti-anxiety medication [F(1, 125)=6.919, p<0.05, partial η=0.052]. Participants assessed were more likely to recommend anti-anxiety medications for virtual humans presenting with anxiety (M=22.27, SD=23.55) as compared to non-anxious virtual patients (M=12.92, SD=15.81). Analyses also revealed a significant main effect for the anxiety assessment rating [F(1, 125)=5.799, p<0.05, partial η=0.044] such that participants rated anxiety levels higher in virtual humans presenting with anxiety (M=37.50, SD=22.10) as compared to virtual humans with no anxiety (M=25.72, SD=19.34). However, there were no main or interaction effects of patient anxiety status on likelihood of recommending an opioid medication for pain management [F(1, 125)=0.172, p>0.05, partial η=0.001].
Influence of patient race
Across ratings, there were no significant main or interaction effects between pain management decisions, patient anxiety status, and patient race.
Influence of patient sex
There were no significant main or interaction effects between pain management decisions, patient anxiety status, and patient sex.
Influence of provider sex
For the item exploring participants' likelihood of anti-anxiety medication, there were no significant main effects for patient anxiety status; however, a significant interaction effect was found for provider sex and patient anxiety status [F(1, 125)=3.966, p<0.05, partial η2=0.031]. For this item, female providers were more likely to recommend anti-anxiety medications (M=25.33, SD=22.69) for anxious virtual human patients when compared to male providers (M=15.38, SD=16.49). Means and standard deviations for ratings by provider sex are presented in Table 7.
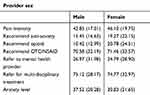 |
Table 7 Means and standard deviations for ratings by provider sex |
Influence of provider race
Analyses revealed no significant main or interaction effects between provider sex, patient anxiety status, and patient race.
Idiographic analyses
Two sets of results are reported for anxiety cue use (see Table 8). Idiographic analyses are described below based on regression models and standardized regression coefficients that were significant at p<0.05. Of note, standardized regression coefficients are presented for significant regression models. Consistent with previous Lens model studies, Table 8 also reports a more liberal analysis with p<0.10.
 |
Table 8 Significant policies for cue frequencies at the p<0.05 and p<0.10 levels |
Pain intensity
Results indicated that 115 of 132 participants had significant policies for pain intensity assessment. These results provide strong support for the validity of the Lens model approach in successfully capturing decision-making policies. When exploring significant standardized regression coefficients, patient pain-related body posture was the most influential cue across participants’ pain intensity ratings. One hundred and twelve participants used pain-related body posture as a prominent cue; all of these participants judged virtual humans expressing high pain behaviors as experiencing greater pain intensity. Eighteen participants gave higher pain intensity ratings for anxious virtual humans; the reverse was true for one participant. Six of these participants used sex as a significant cue in their policy. One participant gave higher pain intensity ratings for female virtual humans; the reverse was true for four participants. Finally, race was a prominent cue in the policies of eight of these participants, with six more likely to judge higher pain intensity in African-American virtual patients and two were more likely to judge higher pain intensity in Caucasian virtual patients. For this rating, 72% of the sample consistently used one cue in their decision-making process, whereas 22% of the sample used two or more cues in a reliable manner.
Anti-anxiety medication
Results indicated that 85 of 132 participants had significant policies for likelihood of recommending anti-anxiety medications. Patient anxiety status emerged as the most influential factor in this context. All 69 of these participants were more likely to recommend anti-anxiety medication to anxious virtual patients. Again, patient pain-related body posture was also a prominent cue. Twenty-six participants used pain-related body posture as a cue; 21 were more likely to recommend anti-anxiety medications for virtual patients exhibiting high pain behaviors, whereas the converse was true for five participants. Eight participants used sex as a significant cue in their policy and all of these participants were more likely to recommend anti-anxiety medications to female virtual patients. Finally, race was a prominent cue in the policies of seven participants and all were more likely to recommend anti-anxiety medications to African-American versus Caucasian virtual patients. For this rating, 57% of the sample consistently used one cue in their decision-making process, whereas 21% of the sample used more than two cues at once.
Opioid pain medications
Results indicated that 65 of 132 participants had significant policies for likelihood of recommending opioid medications. Patient pain-related body posture again proved to be the most influential factor for this treatment decision. Of the 62 participants with policies in which pain-related body posture was a significant cue, 61 were more likely to recommend opioid pain medications for virtual patients demonstrating high pain behaviors. One participant was more willing to recommend opioid pain medications to virtual patients demonstrating low pain behaviors. Twelve participants used patient anxiety status as a prominent cue and nine were more likely to recommend opioid pain medications for virtual patients presenting with anxiety; the reverse was true for three participants. Regarding sex, four participants had policies in which this cue was significant. One participant was more likely to recommend opioid pain medications to female virtual patients, whereas the converse was true for three participants. The one participant who used race as a significant cue was more likely to recommend opioid pain medication for African-American virtual patients. For this rating, 51% of the sample consistently used one cue in their decision-making process, as compared to the 10% that used two or more cues in a reliable manner.
OTC/NSAID medications
Results indicated that 45 of 132 participants had significant policies for recommending OTC/NSAID medications that reached statistical significance. Patient pain-related body posture was the most consistently used cue within the context of recommending OTC/NSAID medications. Of the 44 participants with policies in which pain-related body posture was a significant cue, 38 were more likely to recommend OTC/NSAID medications to patients demonstrating high pain behaviors; the converse was true for six participants. Patient anxiety status was a prominent cue in the policies of two participants. One was more likely to recommend OTC/NSAID medications for anxious virtual patients while the reverse was true for the remaining participant. Regarding patient sex, two participants were more likely to recommend OTC/NSAID medications to female patients, whereas one participant was more likely to recommend OTC/NSAID medications to male patients. The one participant who used race as a cue was more likely to recommend OTC/NSAID medications to African-American virtual patients. For this rating, 49% of the sample consistently used one cue in their decision-making process; 3% of the sample used two or more cues in a reliable manner.
Referral to mental health provider for counseling
Results indicated that 87 of 132 participants had policies for treatment that reached statistical significance. Pain-related body posture was a prominent cue for 23 participants; 17 of these participants were more likely to refer patients expressing high pain behaviors to a mental health provider for counseling; the reverse was true for six participants. Within the context of referring to a mental health provider for counseling, patient anxiety status emerged as the most influential cue. All 74 participants who used patient anxiety status as a cue were more likely to make a referral to a mental health provider for anxious virtual humans. Regarding patient sex, seven participants had policies in which this cue was significant. Two were more likely to refer females to mental health providers for counseling, whereas the converse was true for five participants. All two participants who used race as a cue were more likely to refer African-American virtual patients to a mental health provider for counseling. For this rating, 65% of the sample consistently used one cue in their decision-making process, whereas 14% of the sample used two or more cues in a reliable manner.
Referral to multi-disciplinary pain management center
Results indicated that 56 of 132 participants had significant policies for referring to pain management centers. Not surprisingly, patient pain-related body posture was the most influential factor in this referral decision. Forty-nine participants used pain-related body posture as a prominent cue; all 49 were more likely to refer patients with high pain behaviors to a multi-disciplinary pain management center. Patient anxiety status was a prominent cue for 15 participants. Eleven of those participants were more likely to refer anxious virtual humans to a multi-disciplinary pain management center; the reverse was true for four participants. Seven of these participants used sex as a significant cue in their policy. Three participants were more likely to refer female participants to multi-disciplinary pain management centers; the reverse was true for the remaining four participants. Finally, race was a prominent cue in the policies of three participants, and all three were more likely to refer African-American patients to a multi-disciplinary pain management center. For this rating, 45% of the sample consistently used one cue in their decision-making process, whereas 16% of the sample used more than two cues at once.
Anxiety level
Results indicated that 104 of 132 participants had policies for anxiety assessment that reached statistical significance. Of the 44 participants who used pain behavior as a significant cue, 41 were more likely to judge virtual patients exhibiting high pain behaviors as experiencing more anxiety, and the converse was true for three participants. For anxiety assessment, patient anxiety status emerged as the most influential cue in this context. All 81 participants who used patient anxiety status as a cue judged anxious virtual humans to be experiencing more anxiety relative to virtual patients presenting with no anxiety. Regarding sex, ten participants judged female virtual patients to be experiencing greater anxiety compared to males. Of the seven participants who used race as a significant cue, six assessed African-American virtual patients as experiencing greater anxiety. The remaining participant gave higher ratings to Caucasian virtual patients relative to African-American virtual patients. For this rating, 62% of the sample consistently used one cue in their decision-making process, as compared to the 28% that used two or more cues in a reliable manner.
Significance of contextual cues
To quantify the amount of explained variance accounted for by each cue across ratings, coefficients of multiple determination (R2) for each cue within each rating across participants were squared (Table 9). Results suggested that patient pain-related body postures, anxiety status, sex, and race cues accounted for as much as 63% of the variance in policies for pain assessment and 41% of the variance in policies for recommending anti-anxiety medications. Examination of the coefficients revealed that cues accounted for an average of 37% of the variance in opioid recommendations and 28% of the variance in OTC/NSAID recommendations. Furthermore, cues accounted for 43% of the variance in recommendations to a mental health provider, 31% of the variance in recommendations to a multi-disciplinary pain center, and 49% of the variance in pain assessment ratings. The aforementioned values represented the average amount of variance accounted for by each cue. Additional comparative data are presented in Table 9.
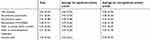 |
Table 9 Means and standard deviations for variance explained |
Discussion
This study was the first to explore the unique contribution of patient anxiety status and patient pain-related body postures on pain management decisions made by health care trainees and professionals and highlighted a principal advantage of employing Lens model methodology to study clinical decision making. At the nomothetic level, there were few significant main effects found between patient demographic variables, pain-related body postures, and pain-related decision making. However, idiographic analyses revealed patient demographic and pain-related body posture cues were consistently influential for approximately 90% of the sample, providing strong evidence of the validity of the Lens model approach in capturing individual decision-making policies. Consequently, the conclusions an individual might draw from the idiographic analyses may be very different from interpretations based solely on nomothetic results. This discrepancy can be attributed to the observation that a few participants with disproportionate cue use can significantly influence group-level analyses. Furthermore, meaningful individual-level differences can be averaged out in the group-level analysis. In a methodological manner, the Lens model approach used in this study allowed for a detailed analysis of each participant’s decision-making process, which is not possible when only examining group-level differences. Approximately 87% of the sample approached the study using a statistically reliable decision-making approach when making pain assessment and treatment decisions. It should also be noted that substantial study results emerged despite using a conservative analytic approach. Moreover, the fact that virtual patient cues were influential across ratings after controlling for provider type suggests observed influences were robust.
Out of all the demographic cues, patient pain-related body posture had the largest, most consistent impact across assessment and treatment ratings, with higher average ratings assigned to virtual patients presenting with high pain behaviors. Of note, not all participants used the pain behavior cue in the same manner (eg, some were less likely to refer patients exhibiting high pain behaviors to mental health providers or multi-disciplinary pain management centers). The prominent use of patient pain-related body posture cues by a majority of the sample was also consistent with previous investigative studies highlighting these behaviors as an important source of information for pain assessment and treatment decisions. It is logical that health care providers and trainees would rely on patient pain behaviors, given the clinical relevance over demographic cues in accurate pain assessment. The use of sex and race cues was significant for a subset of the sample as well, which was also consistent with previous virtual human studies. One novel aspect of the current study was the assessment of the unique impact of patient anxiety status across pain management decisions. Patient anxiety status was consistently influential across pain assessment and treatment decisions, which was supported by previous virtual human idiographic studies exploring the influence of patient psychological factors. Patient anxiety status emerged as the most influential and consistently used cue, above and beyond patient pain behaviors, for participants making anxiety assessment ratings, anti-anxiety medication recommendations, and referrals to mental health providers. The direction of the anxiety status cue was consistent with previous literature, and suggested that individuals with anxiety are actually more likely to be perceived as having anxiety, prescribed anti-anxiety medications, and referred to a mental health provider for counseling, particularly when treated by female providers. Regarding the clinical implications of patient anxiety cue use, a majority of individuals were not consistently biased in one direction. For example, of the 12 significant policies for likelihood of recommending opioid medications, nine were biased toward recommending anxious virtual humans opioid medications while three participants were less likely to recommend opioid medications for anxious patients. Moreover, of the 19 participants with significant policies for recommending anti-anxiety medications, one participant was biased against anxious patients and rated anxious virtual patients as experiencing less anxiety. It is important to note these differences are particularly meaningful, given that pain-related treatment recommendations differed by patient anxiety status among virtual patients presenting with the same amount of pain.
Relatedly, it is important to note not all cues were used by all participants, and not all participants had a reliable decision-making approach. Indeed, 34% of the participants were not influenced by patient anxiety status when deciding to refer pain patients to mental health providers for counseling; similarly, 93% of the participants did not consistently use patient anxiety status when recommending an opioid or narcotic medication for pain management. These results were reasonable given opioids are not a preferred treatment for pain patients presenting with anxiety. This study was the first to explore the influence of patient anxiety status using both virtual human technology and Lens methodology; therefore, we do not have a comparison to judge a standard of care for pain patients presenting with anxiety. However, accurate anxiety assessment in patients experiencing pain remains important because psychological factors significantly influence the effectiveness of pain treatment, especially for patients experiencing chronic pain. This discrepancy could be considered a weakness of the study; however, it could also be argued that this sample of health care providers and trainees do not have consistently reliable decision-making policies when treating real pain patients. Therefore, it is plausible these participants are engaging in inconsistent pain management practices. We argue it can be valuable and informative to capture small differences in individual cue use and policies based on the potential threat to effective pain management. For example, one health care provider with significant biases toward (or against) anxious pain patients will interact with countless patients throughout their career and serve as models for younger professionals, colleagues, and students. In this context, one bias could have an exponentially, negative impact on thousands of patients. Although this sample included younger health care providers and students who may not represent the traditional health care provider, this study was successful in capturing valuable information from individuals who have personal experience with pain, have directly observed pain in others (eg, family, friends), and who are likely to seek pain-related services at some point throughout their lives.
This study further illustrated the utility and validity of virtual human technology and Lens methodology within the context of assessing the influence of patient anxiety status on pain management decisions among health care providers and trainees. In some cases, nomothetic analyses could neglect to capture clinically meaningful variability in decision-making patterns that would otherwise be interpreted as error. The Lens model approach used in this study allowed for unique exploration of individual variations across pain assessment and treatment decisions. One limitation of this study was the participant population, which was homogeneously young and female with fewer years of practice. Furthermore, we recognize the limited external validity given the restrictions placed upon virtual human technology in recreation of both natural and clinical settings. With this method, there are some factors that could not be accurately reflected, such as detailed environments and interactions between both patient and provider. Further, the nature of the study may have been apparent to some participants which may have elicited socially desirable responses. The representativeness of the virtual human stimuli was also restricted and could explain why the influence of patient anxiety status on pain management decisions was less robust in this study relative to clinical literature indicating these differences play a substantial role in patient care.
Conclusion
In summary, both idiographic and nomothetic methodologies were sensitive to patient anxiety status influences on pain management decisions among our sample of health care professionals and trainees. Lens model methodology has been previously used to investigate the influence of patient facial expression cues on pain management decisions; however, this study contributed to the existing literature by using virtual human technology to explore the effects of patient anxiety status and pain-related body postures on pain assessment and treatment ratings. We found patient demographic and pain-related body postures influenced the assessment and treatment ratings for a majority of the sample, and that the Lens model approach and virtual human technology were effective in identifying these individuals. Similarly, a significant subset of the sample demonstrated patient anxiety status influences in their pain management decisions. The direction of these findings appeared to be consistent with previous literature and showed that in general, anxious patients were more likely to be identified as experiencing anxiety and recommended anti-anxiety medications. Results were more pronounced among female providers, who were more likely to recommend anti-anxiety medications for anxious patients as compared to male providers. These findings were consistent with pain-related gender role stereotypes about male and female providers.
Taken together, it appears especially important for health care providers and trainees involved in pain management to take into consideration the pain-related body postures and psychological status of their patients. Conversely, results of this study can significantly impact pain assessment and treatment decisions by identifying specific health care professionals and trainees that are using patient anxiety status or demographic cues instead of pain-related body postures to inform treatment decisions. More specifically, the Lens model approach can be effective in addressing cue use among individuals who are more likely to recommend opioid pain medications for anxious patients versus non-anxious patients presenting with the same amount of pain. Future studies may benefit from continued examination of impactful differences in pain management decisions in order to establish standard of care practices for pain patients presenting with anxiety. The findings of this study in addition to previous virtual human investigations have the potential to better inform clinical practice, research, and education regarding the importance of appropriate cue use when making pain assessment and treatment decisions.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Hing E, Cherry DK, Woodwell DA. National ambulatory medical care survey: 2004 summary. Adv Data. 2006;(374):1–33.
2. Institute of Medicine. Committee on Advancing Pain Research C, and Education. Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research. National Academies Press; 2011.
3. Dworkin SF, Sherman JJ. Relying on Objective and Subjective Measures of Chronic Pain: Guidelines for Use and Interpretation. 2001.
4. Hollingshead NA, Meints S, Middleton SK, Hirsh AT. Examining influential factors in providers’ chronic pain treatment decisions: a comparison of physicians and medical students. BMC Med Educ. 2015;15(1):1. doi:10.1186/s12909-015-0441-z
5. Martel MO, Thibault P, Sullivan MJ. Judgments about pain intensity and pain genuineness: the role of pain behavior and judgmental heuristics. J Pain. 2011;12(4):468–475. doi:10.1016/j.jpain.2010.10.010
6. Choinière M, Melzack R, Girard N, Rondeau J, Paquin M-J. Comparisons between patients’ and nurses’ assessment of pain and medication efficacy in severe burn injuries. Pain. 1990;40(2):143–152. doi:10.1016/0304-3959(90)90065-L
7. Davoudi N, Afsharzadeh P, Mohammadalizadeh S, Haghdoost AA. A comparison of patients’ and nurses’ assessments of pain intensity in patients with coronary artery disease. Int J Nurs Pract. 2008;14(5):347–356. doi:10.1111/j.1440-172X.2008.00712.x
8. Green CR, Wheeler JRC, Marchant B, LaPorte F, Guerrero E. Analysis of the physician variable in pain management. Pain Med. 2001;2(4):317–327. doi:10.1046/j.1526-4637.2001.01045.x
9. Green CR, Wheeler JR. Physician variability in the management of acute postoperative and cancer pain: a quantitative analysis of the Michigan experience. Pain Med. 2003;4(1):8–20. doi:10.1046/j.1526-4637.2003.03006.x
10. Luger TJ, Lederer W, Gassner M, Löckinger A, Ulmer H, Lorenz IH. Acute pain is underassessed in out-of-hospital emergencies. Acad Emergency Med. 2003;10(6):627–632.
11. Sloman R, Rosen G, Rom M, Shir Y. Nurses’ assessment of pain in surgical patients. J Adv Nurs. 2005;52(2):125–132. doi:10.1111/j.1365-2648.2005.03573.x
12. Anderson KO, Mendoza TR, Valero V, et al. Minority cancer patients and their providers. Cancer. 2000;88(8):1929–1938.
13. Aubrun F, Salvi N, Coriat P, Riou B. Sex-and age-related differences in morphine requirements for postoperative pain relief. J Am Soc Anesthesiologists. 2005;103(1):156–160.
14. Calderone KL. The influence of gender on the frequency of pain and sedative medication administered to postoperative patients. Sex Roles. 1990;23(11–12):713–725. doi:10.1007/BF00289259
15. Horgas AL, Elliott AF. Pain assessment and management in persons with dementia. Nurs Clinics. 2004;39(3):593–606. doi:10.1016/j.cnur.2004.02.013
16. Robinson ME, Wise EA. Prior pain experience: influence on the observation of experimental pain in men and women. J Pain. 2004;5(5):264–269. doi:10.1016/j.jpain.2004.04.003
17. Vallerand AH, Polomano RC. The relationship of gender to pain. Pain Manage Nurs. 2000;1(3):8–15.
18. Hirsh AT, Alqudah AF, Stutts LA, Robinson ME. Virtual human technology: capturing sex, race, and age influences in individual pain decision policies. Pain. 2008;140(1):231–238. doi:10.1016/j.pain.2008.09.010
19. Stutts LA, Hirsh AT, George SZ, Robinson ME. Investigating patient characteristics on pain assessment using virtual human technology. Eur J Pain. 2010;14(10):1040–1045. doi:10.1016/j.ejpain.2010.04.003
20. Wandner LD, Stutts LA, Alqudah AF, et al. Virtual human technology: patient demographics and healthcare training factors in pain observation and treatment recommendations. J Pain Res. 2010;3:241. doi:10.2147/JPR.S14708
21. Hamberg K, Risberg G, Johansson EE, Westman G. Gender bias in physicians’ management of neck pain: a study of the answers in a Swedish national examination. J Women’s Health Gender-based Med. 2002;11(7):653–666. doi:10.1089/152460902760360595
22. Lord B, Cui J, Kelly A-M. The impact of patient sex on paramedic pain management in the prehospital setting. Am J Emerg Med. 2009;27(5):525–529. doi:10.1016/j.ajem.2008.04.003
23. Michael GE, Sporer KA, Youngblood GM. Women are less likely than men to receive prehospital analgesia for isolated extremity injuries. Am J Emerg Med. 2007;25(8):901–906. doi:10.1016/j.ajem.2007.02.001
24. Fishbain DA, Goldberg M, Meagher BR, Steele R, Rosomoff H. Male and female chronic pain patients categorized by DSM-III psychiatric diagnostic criteria. Pain. 1986;26(2):181–197.
25. Hoffmann DE, Tarzian AJ. The girl who cried pain: a bias against women in the treatment of pain. J Law Med Ethics. 2001;28(s4):13–27. doi:10.1111/j.1748-720X.2001.tb00037.x
26. Wandner LD, George SZ, Lok BC, Torres CA, Chuah JH, Robinson ME. Pain assessment and treatment decisions for virtual human patients. Cyberpsychol Behav Social Networking. 2013;16(12):904–909. doi:10.1089/cyber.2012.0707
27. Borkhoff CM, Hawker GA, Wright JG. Patient gender affects the referral and recommendation for total joint arthroplasty. Clin Orthop Relat Res. 2011;469(7):1829–1837. doi:10.1007/s11999-011-1879-x
28. Sheiner EK, Sheiner E, Shoham-Vardi I, Mazor M, Katz M. Ethnic differences influence care giver’s estimates of pain during labour. Pain. 1999;81(3):299–305. doi:10.1016/S0304-3959(99)00019-6
29. Breitbart W, McDonald MV, Rosenfeld B, et al. Pain in ambulatory AIDS patients. I: pain characteristics and medical correlates. Pain. 1996;68(2):315–321.
30. Sherwood MB, Garcia-Siekavizza A, Meltzer MI, Hebert A, Burns AF, McGorray S. Glaucoma’s impact on quality of life and its relation to clinical indicators: a pilot study11 the authors have no proprietary interest in the development or marketing of this or a competing instrument. Ophthalmology. 1998;105(3):561–566. doi:10.1016/S0161-6420(98)93043-3
31. Stewart WF, Lipton RB, Liberman J. Variation in migraine prevalence by race. Neurology. 1996;47(1):52–59. doi:10.1212/wnl.47.1.52
32. White SF, Asher MA, Lai S-M, Burton DC. Patients’ perceptions of overall function, pain, and appearance after primary posterior instrumentation and fusion for idiopathic scoliosis. Spine. 1999;24(16):1693. doi:10.1097/00007632-199908150-00011
33. Shavers VL, Bakos A, Sheppard VB. Race, ethnicity, and pain among the US adult population. J Health Care Poor Underserved. 2010;21(1):177–220. doi:10.1353/hpu.0.0255
34. Meghani SH, Byun E, Gallagher RM. Time to take stock: a meta‐analysis and systematic review of analgesic treatment disparities for pain in the united states. Pain Med. 2012;13(2):150–174. doi:10.1111/j.1526-4637.2011.01310.x
35. Hirsh AT, George SZ, Robinson ME. Pain assessment and treatment disparities: a virtual human technology investigation. Pain. 2009;143(1):106–113. doi:10.1016/j.pain.2009.02.005
36. Green CR, Anderson KO, Baker TA, et al. The unequal burden of pain: confronting racial and ethnic disparities in pain. Pain Med. 2003;4(3):277–294. doi:10.1046/j.1526-4637.2003.03034.x
37. Merskey H, Bogduk N. Task force on taxonomy of the international association for the study of pain. Classification Chronic Pain. 1994;2.
38. Gatchel RJ, Turk DC. Psychosocial Factors in Pain: Critical Perspectives. Guilford Press; 1999.
39. Rochlen AB, Whilde MR, Hoyer WD. The real men. Real depression campaign: overview, theoretical implications, and research considerations. Psychol Men Masc. 2005;6(3):186. doi:10.1037/1524-9220.6.3.186
40. Seal KH, Shi Y, Cohen G, et al. Association of mental health disorders with prescription opioids and high-risk opioid use in US veterans of Iraq and Afghanistan. Jama. 2012;307(9):940–947. doi:10.1001/jama.2012.234
41. Stein MB, Roy-Byrne PP, Craske MG, et al. Functional impact and health utility of anxiety disorders in primary care outpatients. Med Care. 2005;43(12):1164–1170. doi:10.1097/01.mlr.0000185750.18119.fd
42. Keefe FJ, Wilkins RH, Cook WA. Direct observation of pain behavior in low back pain patients during physical examination. Pain. 1984;20(1):59–68.
43. Keefe FJ, Wren AA. Assessment of pain behaviors. Encycl Pain. 2013;224–227.
44. Keefe FJ, Block AR. Development of an observation method for assessing pain behavior in chronic low back pain patients. Behav Ther. 1982;13(4):363–375. doi:10.1016/S0005-7894(82)80001-4
45. Safdar B, Heins A, Homel P, et al. Impact of physician and patient gender on pain management in the emergency department—a multicenter study. Pain Med. 2009;10(2):364–372. doi:10.1111/j.1526-4637.2008.00524.x
46. Weisse CS, Sorum PC, Dominguez RE. The influence of gender and race on physicians’ pain management decisions. J Pain. 2003;4(9):505–510.
47. Weisse CS, Sorum PC, Sanders KN, Syat BL. Do gender and race affect decisions about pain management? J Gen Intern Med. 2001;16(4):211–217. doi:10.1046/j.1525-1497.2001.016004211.x
48. Raftery KA, Smith-Coggins R, Chen AH. Gender-associated differences in emergency department pain management. Ann Emerg Med. 1995;26(4):414–421. doi:10.1016/s0196-0644(95)70107-9
49. Hirsh A, Hollingshead N, Bair MJ, Matthias M, Wu J, Kroenke K. The influence of patient’s sex, race and depression on clinician pain treatment decisions. Eur J Pain. 2013;17(10):1569–1579. doi:10.1002/j.1532-2149.2013.00355.x
50. Cooksey RW. Judgment Analysis: Theory, Methods, and Applications. Academic Press; 1996.
51. Alqudah AF, Hirsh AT, Stutts LA, Scipio CD, Robinson ME. Sex and race differences in rating others’ pain, pain-related negative mood, pain coping, and recommending medical help. J Cyber Ther Rehabil. 2010;3(1):63.
52. Hirsh AT, Callander SB, Robinson ME. Patient demographic characteristics and facial expressions influence nurses’ assessment of mood in the context of pain: a virtual human and lens model investigation. Int J Nurs Stud. 2011;48(11):1330–1338. doi:10.1016/j.ijnurstu.2011.05.002
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
