Back to Journals » Open Access Journal of Sports Medicine » Volume 7
The elite young athlete: strategies to ensure physical and emotional health
Authors Sabato T, Walch T, Caine D
Received 17 May 2016
Accepted for publication 5 July 2016
Published 31 August 2016 Volume 2016:7 Pages 99—113
DOI https://doi.org/10.2147/OAJSM.S96821
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Andreas Imhoff
Todd M Sabato, Tanis J Walch, Dennis J Caine
Department of Kinesiology and Public Health Education, University of North Dakota, Grand Forks, ND, USA
Abstract: This article presents a current review of the risk of physical and psychological injury associated with participation in elite youth sport, and suggests strategies to ensure the physical and emotional health of these young athletes. Although there is lack of epidemiological data, especially with regard to psychological injury, preliminary data suggest that the risk of injury is high in this population. While there is lack of incident and follow-up data, there is also concern regarding burnout, disordered eating, and the long-term consequences of injury. Modifiable injury risk factors identified include postural control, competition anxiety, life events, previous injury, and volume of training. There are presently no studies designed to determine the effectiveness of injury prevention measures in elite youth sports. However, there is adequate evidence arising from injury prevention studies of youth sports participants – including neuromuscular training, protective equipment, mental training to enhance self-esteem, and sport rules modification – to prevent injuries in elite youth sports settings. Although not tested, psychosocial prevention strategies such as adoption of task-oriented coping mechanisms, autonomous support from parents, and a proactive organizational approach also show promise in injury prevention.
Keywords: elite, young athlete, athletic injury, psychological, risk factors, injury prevention
Introduction
Participation in youth sports is increasingly popular and widespread internationally. Trends over recent decades include increased numbers of participants in some sports, particularly girls, increased duration and intensity of training, earlier specialization and year-round training, and increased difficulty of skills practiced.1 In the United States, for example, more than 38 million children and adolescents participate in organized sports each year.2 It is not uncommon for young talented athletes from an age of 12 to 13 years to train 15–20 hours per week at regional training centers in tennis or gymnastics, or for youngsters as young as 6–8 years of age to play organized hockey or soccer and travel with select teams to other towns and communities to compete against other teams of similar caliber.
Sport is by its very nature competitive and even during youth it is performed at different levels, with elite young athletes at the top of the performance pyramid. The elite young athlete is one who has superior athletic talent, undergoes specialized training, receives expert coaching, and is exposed to early competition.3 At the elite level, national and international sporting federations have organized youth competitions in various age classes for athletes competing ranging from as low as under-13 up to under-21 depending on the sport.4 These competitions also represent important showgrounds where, in some sports, young talented athletes are identified for a future professional career.5
Since 1991, the European Youth Olympic Festival (EYOF), a biennial multisport event for youth athletes, has been sponsored by the association of European Olympic Committees. In recent years, the International Olympic Committee created a more extensive international sporting event for talented young athletes from all over the world. Just like the Olympic Games, the Youth Olympic Games (YOG) are held every 4 years. The first Summer YOG was held in Singapore from 14 to 26 August 2010, and the first Winter YOG was held in Innsbruck, Austria, from 13 to 22 January 2012.6 The YOG aim to bring together talented young athletes from ages 15 to 18 from around the world. The Summer YOG regularly feature over 3,500 athletes and are held over a 12-day period, and the Winter YOG feature over 1,100 athletes and last 10 days.6 In addition to all of the sports typically included in the Olympics, the YOG have also showcased several adventure and extreme sports that involve highly specialized gear or spectacular stunts and are well known for their inclusion of elements of real or perceived risk. For example, skateboarding, in-line skating, and sport climbing were showcased in the 2014 YOG in Nanjing. Bicycle motocross and mountain biking were also included in the Nanjing YOG.7
Engaging in sports activities at a young age has important physical health benefits, but also involves risk of injury. This would seem to be particularly true at the elite level given the intensive training programs and high-frequency participation in sports events.8 Inevitably, increased participation is associated with an increased risk of physical injury, or even sudden death.8 The young athlete may also incur psychological injury as a consequence of parents who exercise excessive pressure to perform or do not protect their children from harmful relationships, from emotionally abusive coaching behaviors, or from bullying and hazing behaviors from teammates.9 In addition to the immediate health care costs, these injuries may have long-term consequences on physical and psychological health, resulting in reduced levels of physical activity and, ultimately, reduction in wellness.9–11 Although it is impossible to eliminate all injuries, attempts to reduce risk of injury are obviously warranted.
The purpose of this article is to provide a current review of risks related to physical and psychological injury that may be encountered by elite youth athletes and to discuss strategies designed to minimize or eliminate these risks. Relevant research arising from youth athletes and elite-level adult athletes is included to augment the limited research related to elite youth athletes, especially with regard to psychological injury. Recommendations are made for further research that focuses on the physical and emotional health of young athletes.
Physical/physiological risks for injury in elite youth athletes
Challenges to physical health
Growth and maturation-related factors
Elite youth athletes may be particularly vulnerable to injury due to such growth-related factors as the adolescent growth spurt,12,13 susceptibility to growth plate injury,13,14 age- and maturity-associated variation,14,15 longer recovery and differing physiological response after concussion,16,17 and nonlinearity of growth.18,19 They might also be at risk because of immature or underdeveloped coordination, skills, and perception.20 Concern has also been raised regarding the young female athlete who may be at increased risk of noncontact anterior cruciate ligament (ACL) injuries due to such factors as anatomy, hormones and menstrual cycle, neuromuscular characteristics, muscle strength, and flexibility.21 The more frequent and intensive training and competition of young elite athletes now may create conditions under which these potential risk factors can more readily exert their influence.
Risk of injury
Recent data suggest that the risk of sport injury among elite youth athletes is high.22 If one adopts the predefined age range of 14–18 years, with “elite” reflecting competition at the national or international level,4 then a search of the literature reveals three studies presenting exposure-based (per 1,000 hours) seasonal injury data on adolescent elite soccer athletes.23–25 Training injury rates ranged from 1.4 to 4.6 injuries/1,000 hours, while competition rates were higher, ranging from 10.5 to 22.4 injuries per 1,000 hours. Injury rates in badminton were 2.8 for practice and 5.9 for games.26
Injury rates for U17 and U19 European and World soccer championships were generally higher than those reported for seasonal studies.27–30 Training injury rates at these championships ranged from 1.1 to 7.4 injuries per 1,000 hours.27,28 In contrast, competition injury rates ranged from 11.7 to 88.1 injuries per 1,000 hours.27–30 Injury rates in soccer were generally higher for females than males in both seasonal and tournament studies.
Several studies reported medical encounters for elite youth athletes at world and national championships. Caine and Nassar31 summarized results of injuries treated by the USA Gymnastics Medical Staff during the 2002–2004 Gymnastics National Women’s Gymnastics Championship. Depending on year, from 44.9% to 71.7% of registered gymnasts were treated for acute and/or overuse conditions. Overall, 16 treated conditions (11%) required surgery. During the 2014 YOG, there were 346 total medical encounters among 54 of the 94 registered US athletes (57.4%), for a rate of 3.7 medical encounters per athlete. No surgeries were required.32
Ruedl et al33 reported clinical incidence of injury incurred by young athletes participating in the first Winter YOG 2012 in Innsbruck, Austria. Among the 1,021 registered athletes, a total of 111 injuries were incurred, resulting in a reported incidence of 108.7 injuries per 1,000 registered athletes. Similarly, van Beijsterveld et al34 reported clinical incidence of injuries sustained during the 2013 Summer EYOF. Among the 2,072 registered athletes, a total of 207 injuries were incurred, resulting in a reported incidence of 91.1 injuries per 1,000 athletes. During the 2015 Winter EYOF, 899 registered athletes sustained 38 injuries for a rate of 42.3 injuries per 1,000 athletes.35
Unfortunately, clinical incidence does not account for the potential variance in exposure among participants and sports for risk for injury. Additionally, tournament rates may not be representative of the nature and incidence of injuries incurred by athletes during training and competition throughout the year, especially with regard to overuse injuries.
Risk factors for injury
There is little knowledge on injury risk factors specifically pertaining to elite youth athletes. However, analysis of sports injury risk factors in child and adolescent sport has identified a number of significant predictors of injury that may inform development and evaluation of injury prevention programs relative to the elite youth sport participant population. These include age/level of play,36–41 adolescent growth spurt,42–45 postural control,46–49 biologic maturity,50–52 body size,53–55 sex,56–59 previous injury,35,40,60–62 rules regarding body-checking in ice hockey,63–65 volume of training,66–71 and fatigue.72–75 There is also preliminary evidence that menstrual irregularity and low-energy availability may relate to increased risk of injury in youth athletes.60,76,77
Results of risk factor analyses in youth sports may suffer from one or more methodological limitations (eg, small-scale, short-term, inconsistent standards for determining exposure) and should, therefore, be viewed as initial steps in the important search for predictor variables that may provide interesting characteristics for manipulation in studies of elite youth athletes.78,79 Modifiable risk factors such as postural control, previous injury, volume of training, and fatigue may have particular application for elite youth athletes, given the rigor and volume of their training and competitive regimens.
Nutrition
A lack of research exists regarding the elite youth athlete and nutrition related to energy intake to support growth and, by extension, prevent injury. Most research on nutrition and elite youth athletes is focused on eating disorders. Energy intake is important for performance; however, elite athletes are at risk for developing eating disorders.80 On the basis of the literature of young adults, higher rates of eating disorders are found in female elite athletes (20%) compared to nonathletes (9%).81 Typically, male athletes are focused on weight gain and a muscular physique, whereas female athletes are pressurized to be thin, particularly in sports where having a small body size is beneficial for performance.82–84 Female athletes are at risk for failing to meet their estimated energy needs regarding their dietary intake.82 Additionally, female athletes suffer from cultural and social pressure to be thin and lean, which is more common in sports where body weight and shape affects performance.85 Ensuring the proper nutrition is critical in female athletes, as energy deficiency long term can lead to the female athlete triad, which is characterized by low-energy availability, irregular or missed menstrual periods, and stress fractures and other bone problems due to changes in hormone levels, as well as other eating disorders.82,86 This can result in a lower production of estrogen, which is used to slow down bone resorption and stimulate bone formation – important factors in maintaining bone health.
Elite youth athletes may be at-risk for poor nutrition and eating disorders.87 The German Young Olympic Athletes’ Lifestyle and Health Management Study collected data in 1,138 elite youth athletes with regard to eating disorders. Results showed that elite youth athletes who were most susceptible to eating disorders were athletes competing in weight-dependent sports, female athletes, and male athletes in endurance, technical, or power sports. Additionally, athletes who reported an eating disorder pathology were more likely to have depression and anxiety tendencies.88 Similar studies have shown elite youth athletes are more likely to be energy deficient and at greater risk for disordered eating compared to nonathletes.89,90
Long-term consequences of injury
Sport injury not only reduces future participation in physical activity that adversely affects long-term health but may also lead to posttraumatic osteoarthritis (PTOA).11,91–93 Osteoarthritis is characterized by joint pain and disability in the presence of radiographic changes such as cartilage loss, joint space narrowing, and osteophytes.92 OA is the most common form of arthritis and is one of the most common chronic health conditions and a leading cause of pain and disability among adults.94
Although OA generally affects older adults, evidence arising from several recent systematic reviews indicates that youth and younger adults may develop PTOA prematurely as a result of joint injury sustained in their youth.92,95 Specifically, Richmond et al96 identified previous joint injury and history of meniscectomy as significant risk factors for knee OA (odds ratio [OR] =3.8; 95% confidence interval [CI]: 2.0, 7.2 and OR = 7.4; 95% CI: 4.0, 13.7, respectively). Similarly, Ajuied et al95 reported that in individuals who suffered an ACL rupture, the relative risk of developing moderate-to-severe OA was 3.4 (95% CI: 1.84, 8.01) compared to an uninjured population.
These results are consistent with follow-up studies of young athletes who sustained meniscus or ACL injuries. In a study of 67 Swedish female soccer players with a confirmed ACL injury sustained before 20 years of age, radiographic evidence of OA was present in 51% of the injured knees after 12 years, compared with 8% in the uninjured knees.96 Similarly, in 219 male soccer players, 14 years after ACL injury (age range at injury, 16–42 years), the prevalence of radiographic knee OA was 41% in the injured knees versus 4% in the uninjured knees.97 In long-term follow-up of young athletes undergoing meniscus surgery, more than 50% developed knee OA with accompanying pain and physical decline.98–103 These epidemiologic studies are supported by evidence from animal models of ACL/meniscus injury and OA development.104,105
One recent study suggests that outcomes associated with early PTOA and other negative health consequences may be present as early as 3–10 years following knee injury in youth sport.92 In preliminary analysis of the first year of their historical cohort study, Whittaker et al92 reported evidence that youth/young adults report greater clinical symptomatology consistent with the onset and development of PTOA, and are at greater risk of being categorized as overweight/obese compared to matched uninjured controls.92
As such, knee injury and related meniscus or ACL surgery suffered during elite youth sports may reduce future involvement in physical activity, leading to a less than optimal health in later life.106 The knee, in particular, is the most common joint site for OA and, combined with the ankle, are the leading locations for injury in youth sports.107 Notably, the most common injury location during the 2012 Youth Olympic Winter Games, the 2013 European Youth Sports Festival, and the 2014 Youth Olympics Games (US team) was the knee.32–34
Overtraining, burnout and injury
According to the American Medical Society for Sports Medicine, a limited base of knowledge exists regarding burnout and overtraining injuries in elite youth athletes.108 The difficult nature of quantifying overtraining and injury with regard to “hours played” or “hours practiced” does not allow for concrete guidelines of how much sport or exercise is too much.109 Additionally, more and more pressure to succeed in sport has led to earlier sport specialization, and may increase rates of overuse injury and sport burnout. Sport burnout is a consequence of chronic stress that results in a young athlete stopping participation in a previously enjoyable sport. It is unknown what may cause burnout, but some theories suggest sport specialization, time conflicts or interest in other activities, or perhaps a psychological stressor. To aid in the prevention of burnout, diversified sports training may be more effective in developing elite-level skills that transfer over in the primary sport.108
Furthermore, every sport has different risks for overtraining and overuse injuries. For example, individual sport athletes and females competing at the highest level have a 20%–30% higher incidence of injury.110 Additionally, overtrained elite youth athletes are more likely to have frequent upper respiratory tract infections, muscle soreness, sleep disturbances, loss of appetite, mood disturbances, shortness of temper, decreased interest in training and competition, decreased self-confidence, and inability to concentrate.110
Psychological risks for injury in elite athletes
A discussion of injury affecting elite youth athletes would not be complete without consideration of psychological factors that may increase the risk of physical injury, and of the potential negative effects of elite level organized youth sport on the psychological well-being of its participants. A modified version of Hellstedt’s athletic triangle is used to identify risks of psychological injury that may be encountered by elite youth athletes.9,111 Hellstedt’s framework uses family systems theory to address the influence of the athlete, parents, and coaches on athletic development, and has implications for both physical and psychological performance and injury risk.9,111 As suggested in Kerr et al,9 the impact of peers on athletic development and injury is significant. It is thus imperative that an investigation of psychological injury risks of elite youth athletes be examined from a multifaceted approach, as seen in Figure 1.9
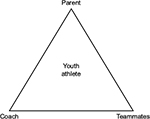  | Figure 1 Modified Hellstedt’s athletic triangle. |
Risk factors for injury
Life events
One of the most persistent findings in preinjury literature is research examining life-related stress.112 Paralleling Williams and Anderson’s112 model, literature has suggested that significant life event stress (defined as the perceived strain associated with stressors such as starting a new school, or the death of a family member), and more specifically negative event stress (the self-rated negative impact of those events), is highly predictive of injury occurrence in athletes.113 Kerr and Minden’s113 examination of stressful life events and injuries among young female gymnasts from the top two skill levels of the Canadian Gymnastic Federation, as well as Petrie’s review114 among female collegiate gymnasts, indicate that negative life stress accounts for 11%–22% of injury variance. Holmes’115 research among American football players further found 50% of those experiencing a high life stress reported injuries leading to at least three days of missed practice or one game, whereas one-quarter of those experiencing moderate life event stress reported injury. While receiving lesser focus, more common yet impactful life event stressors such as daily hassles or problems have similarly been found to accumulate over time, elevating the incidence of athletic injury.116
Stress
Elite athletes are exposed to both physical and psychological stresses on a consistent basis, ranging from exercise- and competition-based stressors (eg, loss of a competition, exercise costs, and efforts) to common and daily stressors.117 Research has increasingly examined the unique yet equally impairing contributions of competition-based and sport-unrelated stress. Worrying about athletic performance, the loss of a competition and resultant fear of failure and disaffection, conflicts with trainers, partners, or family, and costs associated with exercise and physical demands have all been implicated as having a significant impact on the stress levels of elite athletes such as youth and young adult figure skaters, golfers, and tennis players.118–121 Psychological stress has been shown to influence performance by narrowing an athlete’s attention and increasing his or her self-consciousness. In doing so, muscle tension is increased while simultaneously exposing coordination difficulties, thus enhancing injury risk.122 Steffen et al’s116 examination of female youth football players revealed that the risk of injury was 70% greater among those players with high perceived stress. The risk for such injuries is elevated among athletes self-reporting fewer social resources and/or coping skills to properly abate stress. Madison and Prapavessis’123 research among rugby players found that negative stress accounted for 31% of the injury variance among those who used avoidance-focused coping behaviors (eg, denial), who reported having inadequate social support, and had a history of previous injuries. Rogers and Landers124 similarly found that negative life stress and poor coping skills significantly contributed to injury occurring in young athletes. Simultaneously, high coping skills buffered the stress–injury relationship.
Athletic identity
The concept of athletic identity has similarly garnered increased focus in both sport and exercise psychology, and has significant implications for injury risk among elite youth athletes.125,126 Defined as “the degree to which an individual identifies with their athletic role”, athletic identity has been related to both positive and negative performance outcomes.127 From a positive dimension, a healthy athletic identity has been linked to stronger commitment to training and a greater focus on athletic goals.125,128 Likewise, strong athletic identities are associated with positive psychological outcomes such as enhanced body image, increased self-confidence, and decreased anxiety, as a result of intensive training and successful performance.128 Too little emphasis on alternative role identities, to the detriment of the athlete role, may however encourage the development of a unidimensional identity, often associated with negative impacts on an athlete’s well-being.129 Elite athletes with strong and exclusively athletic identities risk the possibility of their self-worth and esteem becoming dependent on athletic performance.130 Subsequently, if performance falls below perceived expectations, an athlete’s feelings of self-worth may be threatened.131 It has similarly been suggested that unidimensional identities may lead to greater performance stress and expectations to succeed, which can result in prevalent athlete burnout, anxiety, and injury risk.132
Depression
The relationship between stress, psychological disorders, and depression is well established, and has been similarly validated among elite athletes.133 While it is established that physical activity positively impacts mental health, reviews have found that intense physical activity performed at the elite level might instead compromise mental well-being, increasing symptoms of anxiety and depression through overtraining, injury, and burnout.134,135 The peak competitive years for elite athletes tend to overlap with the peak age for the risk of onset of mental disorders, increasing the likelihood of depression-based injuries.136 Research among collegiate athletes in the United States suggests the prevalence of depression ranges between 15.6% and 21%. Female athletes were found to experience greater depressive symptomatology, social anxiety, and nonsupport more frequently than male athletes, as well as male and female nonathletes.137 Hammond et al’s138 research among varsity swimmers at Canadian universities who were competing to represent Canada internationally found that 68% of athletes met criteria for a major depressive episode. The prevalence of depression doubled among the elite top 25% of athletes assessed, and performance failure was significantly associated with depression. Reported causes of depression among these elite athletes were varied, and included biological (eg, genetics), social (eg, conflicts), and psychological (eg, cognitive deficits) influences.133
It is also worth noting that depression may not only precipitate the likelihood and severity of disease in athletes, but may also impact recovery and return to sport, as well as possibility of additional injury. Compared with a matched healthy group of collegiate athletes, Leddy et al139 found that athletes who sustained a sport injury reported significantly greater depression symptoms at 1 week postinjury. At 2 months postinjury, athletes who were unable to participate reported greater depression symptoms of at least mild severity, and an estimated 12% of their sample exhibited depression symptoms of comparable severity to adults in outpatient treatment for depression. Manuel et al140 similarly reported depression symptoms of at least moderate severity immediately postinjury as high as 27% among a sample of youth athletes. They reported approximately 21%, 17%, and 13% of athletes exhibited mild-to-moderate depression symptom severity at 3, 6, and 12 weeks postinjury, respectively. It is, therefore, plausible that depression may not merely enhance the risk of injury, but similarly return to play, and reinjury upon return due to cognitive, physiological, and neuromuscular deficits.
Sport specialization and overtraining may similarly generate depressive symptomatology among elite youth athletes. Intense single-sport training, at the exclusion of other sports, increases with age, significantly impacting elite young athletes. A study of the United States Tennis Association junior tennis players found that 70% began specializing at an average age of 10.4 years. Specialization rates gradually increased after the age of 14, with 95% of players specializing by 18 years.141 The risks of intensive and specialized training include both adverse psychological stress and premature withdrawal from participation. Research supports the recommendation that child athletes avoid early sports specialization. Those who participate in a variety of sports and specialize only after reaching the age of puberty tend to be more consistent performers, have fewer injuries, and adhere to sports play longer than those who specialize early.142 Swimmers who specialize earlier spend less time on a national team, and retire earlier than those who specialize later.143 Minor league ice hockey players who retire from the sport began off-ice training earlier, and spent more time in off-ice training than those who continue to compete.144 Butcher et al’s145 retrospective review found that one in five youth athletes reported injury as the precipitating factor in their quitting or retiring from competition. Rhythmic gymnasts, those who specialized at earlier ages, and those spending more hours training from ages 4 to 16, rated their health lower and reported experiencing less fun.146 Junior tennis players reporting early burnout likewise had less input into their training, higher perceived criticism and expectations from parents, and compromised levels of extrinsic motivation.147
In addition to chronic muscle or joint pain, overtraining may similarly manifest itself in personality changes, decreased concentration and fatigue, and heightened levels of anxiety.148,149 Often overlooked, these symptoms place elite athletes at enhanced risk for injury. O’Conner et al,150 for example, found significant correlations between exercise loads and depressive mood states in collegiate-level swimmers. Nixdorf et al151 similarly noted a strong association between the balance of stress and recovery and depressive symptoms among elite German athletes. Athletes with heightened levels of exhaustion and lower levels of recovery experienced significantly greater depressive symptoms. Research on overtraining in sports has further demonstrated the influence of physiological adjustments, such as leptin and insulin levels, on psychological markers such as mood, feelings, or fatigue – each of which enhances injury risk.152 Yet despite enhanced risk, elite young athletes seek professional counseling or support less often, out of fear of appearing weak, losing training time, or losing respect of their coaches and peers.152
Competition anxiety
Ample literature similarly implicates maladaptive fatigue and an inability to control stress as impacting competitive anxiety, thus influencing injury risk. Maladaptive fatigue syndrome occurs when athletes are incapable of addressing stress, resulting in chronic anger, hostility, confusion, depression, apathy, or anxiety. Fatigue-based anxiety impacts balance among gymnasts, negatively impacting short- and long-term performance.153,154 Kolt and Kirkby’s 155 research involving young elite gymnasts similarly suggested that heightened cognitive anxiety impacts not only the risk, but also severity, of injury.155
Maladaptive perfectionist tendencies
Broadly considered a personality characteristic reflecting a compulsive pursuit of exceedingly high standards, coupled with a tendency to engage in overly critical appraisal, perfectionism is a construct whose core elements not only regulate different forms of achievement striving, but also give rise to psychological processes that may lead to maladaptive outcomes.156–158 Substantial impacts of perfectionist tendencies on anxiety, stress, depression, and fatigue have been documented. Although many sports require perfection, unhealthy patterns of behavior as well as negative and self-defeating outcomes are evident among athletes characterized by an extreme perfectionist personality.159 Research among varsity-level athletes found associations between concerns over mistakes and outcomes such as increased anxiety, thus influencing both risk and severity of injury.160
Potential for psychological injury
Parental influences
The parental impact on elite youth athlete development, success, and injury risk may be both valuable and detrimental. Parents often play a critical role in athletic development, introducing their children to sport while providing both financial and psychological support through the training and competition phases. Despite such benefits, our extensive review of the literature suggests that parental and caretaker behaviors may adversely impact elite young athletes’ psychological health.
Elite young athletes’ perceptions of parental overinvolvement have been positively correlated with both anxiety and burnout. Dunn et al161 found that perceived parental pressure was directly related to negative stress among athletes and that levels of motivation were negatively associated with increased levels of parental pressure. Similarly, Gould et al162 found that junior-level tennis players who felt that they had high levels of pressure from family members may feel high levels of worry and anxiety. Parental pressure has also been found to impact the athlete’s perception of self, thus impacting injury risk.162
Exaggerated performance expectations often elicit severe criticism from parents. While not focusing specifically on elite-level youth, Shields et al’s163 examination of parents of fifth- through eighth-grade athletes revealed that 13% had angrily criticized their child’s sport performance. Such findings mirror those of Kidman et al164 and Blom and Drane,165 both of whom reported that nearly one-third of verbal comments from parents of youth athletes were negative, ranging from corrective to scolding behaviors.
Another important mechanism of parental influence is modeling of dysfunctional eating attitudes and behaviors. Several studies among adolescent girls and their parents have shown significant associations between abnormal eating attitudes of mothers and daughters.166,167 Blackmer et al168 found greater body image disturbances and higher levels of disturbed eating attitudes among both female and male college athletes who reported family climates with low perceived support and autonomy. In a previous study examining individual and relational risk factors (eg, self-esteem, social pressure for thinness), Francisco et al169 found direct parental influences (eg, weight teasing) on disordered eating among elite athletes, yet not on that of nonelite athletes or participants in the control group.
In addition to directly influencing the psychological health of elite athletes, parents play a vital role in navigating their child’s relationships with others. Often socialized into the sport culture, and left to accept the authority and expertise of coaches, parents may indirectly contribute to emotionally abusive coaching practices by normalizing such behaviors as routine.170,171
Coaching influences
The influence of coaching strategies and/or practices on psychological harm among elite youth athletes should similarly not be overlooked. Often researched from the scope of adolescent development, psychology, sociology, and social work, a focus on emotional abuse in sport is at a formative level. Defined as “patterns of nonphysical harmful interactions” between a child and caregiver, studies of emotionally abusive coaching are limited to athletes and student-athletes 18 years of age and older.9,172 Alexander et al’s173 research among 18- to 22-year-old athletes in the United Kingdom found the risk of experiencing emotional harm was more than three times that of physical harm. More than one-third (34%) of athletes indicated being treated in an emotionally harmful manner by either a coach or trainer, with little sex-based variability. Emotionally abusive practices were more commonly reported among athletes from individual sports (eg, swimming and dance) than those participating in team sports (eg, football, hockey, rugby), and included yelling, belittlement, making degrading comments, and throwing objects with the purpose of intimidating the athlete.173
The continued growth of social media has continued to raise public awareness of coaching-related practices that are psychologically damaging to elite young athletes. For example, accounts of Olympic gold medalist Dominique Moceanu’s long-term struggles with psychological harm resulting from coaching and parental degradation have increased awareness of and advocacy for monitoring of training, practice, and competitive activities.174 Acts of omission, such as neglect, or failure to take action to prevent injury, which often occurs when coaches minimize the impact of bullying or hazing, similarly impact levels of athlete anxiety and depression, and have been widespread in the media.175
Strategies to ensure physical and emotional health
There are presently no studies designed to determine the effectiveness of injury prevention measures in elite youth sports specifically. However, there is adequate evidence arising from injury prevention studies of youth sport participants to inform practice and policy recommendations to prevent injuries in elite youth sport settings.91,176–178 The focus of this research has been primarily on neuromuscular training programs, protective equipment and sporting rules, and eating disorders intervention.
Physical/physiological prevention strategies
Multifaceted neuromuscular training programs
The most common injuries in youth sport involve the lower extremity, accounting for over 60% of the overall injury burden in youth sport.62,179 On the basis of relative burden, the focus of much of the evidence surrounding injury prevention in youth sport has been on reducing the risk of lower extremity injuries.116 These neuromuscular training strategies primarily target intrinsic risk factors such as previous injury, decreased strength, endurance, flexibility, and postural control.91
The results of a recent meta-analysis of randomized controlled trials (RCTs) reveal a substantial overall protective effect of neuromuscular training in reducing the risk of lower extremity injury in youth team sport (incidence rate ratio =0.64; 95% CI: 0.40–0.84) or a 36% reduction in lower extremity injury risk.118 In this study, the combined estimate for RCT studies examining the preventative effect of neuromuscular training in the reduction of knee injuries in youth team sport (soccer, European handball, basketball) suggests a protective effect of knee injuries specifically, but this finding was not statistically significant (incidence rate ratio =0.74 [95% CI: 0.51–1.07]).
Protective equipment
Using protective equipment may help to prevent injury in many sports. Although preventative studies have not often been conducted involving athletes in elite youth sports, the results of studies with youth and adult athletes are pertinent. Three systematic reviews involving a combination of youth and adult populations support the effectiveness of helmets in skiing and snowboarding in reducing the risk of head injuries.180–182 In studies that included children, the associated OR was 0.41 (95% CI: 0.27–0.59).180
Although no RCTs have evaluated face shields, several cohort studies have shown a protective effect of face shields on risk of injuries, including facial lacerations, facial fractures, dental injuries, and head injuries.183–185 Stuart et al185 documented a dose–response effect with the amount of facial protection provided among ice hockey players; risk of injury decreased by 54% with the use of partial face shields, and injury risk decreased by 85% with the use of full face shields. Benson et al183 also showed that the use of the full face shield significantly reduced the amount of playing time lost because of concussion, suggesting that concussion severity may be reduced by the use of a full face shield.
A systematic review examining wrist guards in snowboarding reveals a significant protective effect in reducing the risk of wrist injury (OR =2.3), wrist fracture (relative risk [RR] =0.29), and wrist sprains (RR =0.17).186
There is sufficient evidence arising from youth populations to endorse the use of protective equipment in elite youth sport, yet despite this evidence there is also evidence to support the less than optimal uptake of equipment strategies.91
Sporting rules
All sports have specific rules for the purpose of regulating the game or sporting activity. Some sporting rules have been developed for the specific purpose of decreasing the risk of injury in youth sports – for example, rules against “spearing” in gridiron football and rules mandating the use of face shields in ice hockey. Although these changes helped to reduce youth sports injuries, including catastrophic injuries such as blindness in hockey and paralysis in football, relatively few studies have systematically evaluated the effect of rules or rule changes on the risk of sports injuries. An exception is the evaluation of body checking in youth ice hockey. In a recent meta-analysis, policy allowing body checking in youth age groups was a significant injury risk factor (RR =2.45; 95% CI: 1.7–3.6).187 In a cohort study comparison of leagues with and without body checking in 11- and 12-year-old players showed a three- to fourfold increased risk of injury where body checking was allowed. These findings led to a national policy change in Canada and the United States.91
Social-cognitive eating disorders intervention
To combat the effects of eating disorders in elite young athletes, Martinsen et al188 conducted an RCT to prevent the development of new cases of eating disorders among elite Norwegian high-school athletes representing a variety of sports/disciplines. Their social-cognitive intervention was successful at preventing new cases of eating disorders and symptoms associated with eating disorders in adolescent elite female athletes. Similarly, a 1-year RCT targeted increased knowledge and strategies for healthy nutrition, eating behavior, and eating disorders. Results showed that coaches and athletes successfully increased knowledge for weight recognition and management, and coaches had more knowledge of eating disorders at the end of the intervention compared to controls.189 Thus, interventions that target eating disorders and knowledge of eating disorders have been shown to be successful. These interventions are necessary to achieve adequate nutrition and prevent eating disorders in elite youth athletes, especially to prevent injury.
Psychosocial prevention strategies
If not managed correctly, stress, anxiety, depression, and burnout can have substantial impacts on an athlete’s welfare, affecting both mental and physical readiness to perform.190 It is thus imperative that both physiological and psychological athletic wellness are consistently monitored. In the absence of intervention research, there are a number of ways in which the psychological wellness of elite junior athletes can be monitored and/or managed, thus limiting the risk of injury.
Coping mechanisms
Coping with stress in sport is an essential self-regulatory factor that promotes optimal levels of achievement.191 Individually focused factors such as personality, motivation, and cognitive evaluation are key predictors of sport-related coping. Task-oriented coping engages strategies to directly manage a stressful circumstance (eg, problem-focused) and its resulting cognitive and affective activation. Also referred to as approach or engagement coping, task orientation includes strategies such as effort expenditure, thought control, relaxation, logical analysis, mental imagery, and support seeking. Indicators of task-oriented coping have been associated with both objective and subjective achievement indicators, and thus decreased risk of injury among athletes.191
Burnout and optimism
Elite young athletes are at risk of developing burnout, as they face not only high physical demands but also psychological pressure to reach an elite level. Burnout appears to be linked to chronic emotional and interpersonal stressors in one’s relationship with his/her work.192 Related to stress associated with intense training and competition demands, exhaustion is a central contributor to burnout. Reduced sense of athletic accomplishment is manifested in a perception of low ability with regard to performance and skill level. Manifesting itself in a loss of motivation, such sport devaluation, may lead to enhanced risk of injury.108 By fostering protective factors such as optimism, elite young athletes may, therefore, reduce stress and burnout, thus minimizing injury risk.
Regarded as a generalized outcome expectancy or sense of confidence that a goal can be attained, optimism is associated with a sense of control and confidence, making optimists more likely to adopt active and proactive coping strategies, while less likely to engage in avoidance coping. Thus, negative consequences such as poor health, poor performance, and injury risk are abated. Studies among elite-level male and female wrestlers have shown a significantly inverse relationship between optimism and both stress and burnout, with optimistic athletes displaying lower levels of emotional/physical exhaustion and sport devaluation, and less of a reduced sense of accomplishment.123,192 It thus appears that optimism is associated with lower perceptions of burnout and consequently injury risk.108
Hardiness and mental toughness
Hardiness represents a trait-like characteristic that influences the manner in which individuals perceive and react to stressful circumstances. Research among adult athletes has shown that hardy individuals are more effective in coping with stress, thus offering protection against stress-induced health issues.191 Hardiness similarly reflects a state of mental toughness, in that it encapsulates control, commitment, and challenge. Utilized in an athletic setting, such concepts allow athletes to make appropriate decisions about how to cope with stressful situations. Mentally tough individuals are characterized by a strong tendency to view their personal environment as controllable, to perceive themselves as capable and influential, to stay committed even under adverse circumstances, and to consider problems as natural challenges.193 From an athletic performance standpoint, research indicates that elite youth cricketers (Mage =16.45 years) with elevated mental toughness possessed more developmental assets such as support, empowerment, and a positive identity, and lower levels of negative emotional states – each of which has been associated with optimal performance.194
Parent and coaching roles
Parents and coaches play an important role in helping elite young athletes learn about coping by creating a support context for learning, and by using a number of specific strategies to help athletes learn about coping, including questioning and reminding athletes about effective coping strategies, providing perspective, sharing their own experiences, dosing or structuring potentially stressful experiences for athletes, initiating formal conversations about coping, creating learning opportunities, and direct instruction about coping.195
Research has found specific preferences among elite young athletes for parental involvement, which may impact performance and risk of injury. Those preferences include making comments on effort and attitude, rather than performance, as well as providing practical advice that balanced supportive comments and nonverbal behaviors.196 Similarly, athletes preferred specific behaviors before, during, and after competition. Prior to competition, athletes wanted parents to help them prepare physically and mentally, including ensuring proper hydration while helping the athlete to relax. During competition, athletes wanted parents to encourage the entire team, focusing on the athletes’ efforts rather than on the outcome of the competition. Athletes similarly did not want parents to coach from the sidelines, argue with officials, or engage in behaviors that would draw attention to themselves or the athletes.195,197 Autonomous support from parents, such as showing an interest, listening wherever possible, supporting the athlete’s desires, and allowing him/her to participate in decisions, has similarly been shown to have positive influences on motivation and performance, thus minimizing injury risk.198
In deference to a controlling style where autocratic decisions are made, and control is asserted through threats, autonomous support from coaches has similarly been found to positively influence motivation and performance. In addition to providing autonomous support, providing encouragement after mistakes, as well as expertise in training and practice, plays a role in motivating an athlete to achieve while minimizing injury risk.198 This observation is critically important, since the specializing career stage of elite young athletes is partially characterized by a shift toward specialist coaching.199
Organizational culture
An effective, proactive, and preventive organizational approach to enhancing emotional health and reducing psychological risks for injury seeks to make changes in both the macro- and microenvironment, by impacting both organizational culture and task design and activity. A proactive approach that addresses the underlying causes of psychological distress, establishes effective coping mechanisms to recognize and respond to stressors, and properly identifies the perspectives of elite young athletes, has shown to moderate external pressures and reduce injury risk.200 An organizational culture with a proper focus on monitoring and modification of training demands would similarly abate psychological strain, and its impending contribution to athletic injury.
Conclusion
Elite youth athletes have competed in international sporting events for more than 50 years. However, international sporting events such as the YOG, designed exclusively for elite youth athletes, are a relatively new phenomenon. Engaging in elite youth sport not only has important health benefits but also involves risk of injury, given the intensive training programs and high frequency of elite youth participation. Although there is lack of epidemiological data, preliminary data suggest that the risk of physical and psychological injury is high.
Although there is a paucity of research on risk factors specifically related to injury affecting elite youth athletes, research involving other young athletes may be generalizable to elite youth athletes. In this regard, modifiable risk factors such as balance deficiency, competition anxiety, life events, previous injury, volume of training, and fatigue may have particular application for elite youth athletes, given the rigor and volume of their training and competitive regiments.
There are presently no studies designed to determine the effectiveness of injury prevention measures in elite sports specifically. However, there is adequate evidence arising from injury prevention studies of youth sports participants – including neuromuscular training, protective equipment, mental training to enhance self-esteem, and sport rules modification – to prevent injuries in elite youth sports settings. Although not tested, psychosocial prevention strategies such as adoption of task-oriented coping mechanisms, autonomous support from parents, and a proactive organizational approach also show promise in injury prevention.
Disclosure
The authors report no conflicts of interest in this work.
References
Caine DJ. Are kids having a rough time of it in sports? Br J Sports Med. 2010;44:1–3. | ||
National Institute of Arthritis and Musculoskeleletal and Skin Diseases. Preventing musculoskeletal sports injuries in youth: a guide for parents. June 2013. Available at http://www.niams.nih.gov/Health_Info/Sports_Injuries/child_sports_injuries.asp. Accessed May 25, 2014. | ||
Mountjoy M, Armstrong N, Bizzini L, et al. IOC consensus statement: training the elite child athlete. Br J Sports Med. 2008;42(3):163–164. | ||
Steffen K, Engebretsen L. More data needed on injury risk among elite young athletes. Br J Sports Med. 2010;44:485–489. | ||
Engebretsen L, Steffen K, Bahr R, et al. The International Olympic Committee Consensus Statement on age determination in high level young athletes. Br J Sports Med. 2010;44(7):476–484. | ||
Olympic.org. Official website of the Olympic Movement. What is the Youth Olympic Games? Available at: https://www.olympic.org/youth-olympic-games.Accessed March 30, 2016. | ||
Heggie, TW, Caine DJ, editors. Epidemiology of Injury in Adventure and Extreme Sports. Basel, Switzerland: Karger; 2012:1–16. | ||
Armstrong N, McManus AM. Preface. The elite young athlete. Med Sport Sci. 2011;56:1–3. | ||
Kerr G, Stirling A, MacPherson E. Psychological injury in pediatric and adolescent sports. In: Caine D, Purcell L, editors. Injury in Pediatric and Adolescent Sports: Epidemiology, Treatment and Prevention. New York, NY: Springer; 2016:179–190. | ||
Fields SK, Collins CL, Comstock RD. Violence in youth sports: hazing, brawling and foul play. Br J Sports Med. 2010;44:32–37. | ||
Caine DJ, Golightly YM. Osteoarthritis as an outcome of paediatric sport: an epidemiological perspective. Br J Sports Med. 2011;45(5):298–303. | ||
Wild CY, Steele JR, Munro BJ. Musculoskeletal and estrogen changes during the adolescent growth spurt in girls. Med Sci Sports Exerc. 2013,45:138–145. | ||
Micheli LJ. Overuse injuries in children’s sports: the growth factor. Orthop Clin North Am. 1983;14:337–360. | ||
Maffulli N, Caine D. The younger athlete. In: Brukner P, Khan K, editors. Clinical Sports Medicine. 4th ed. Sydney, Australia: McGraw-Hill; 2012:888–909. | ||
Malina RM, Bouchard C, Bar-Or O. Growth, Maturation, and Physical Activity. 2nd ed. Champaign, IL: Human Kinetics; 2004:267–273. | ||
Purcell L. Concussion in youth athletes. In: Caine D, Purcell L, editors. Injury in Pediatric and Adolescents Sports: Epidemiology, Treatment and Prevention. New York, NY: Springer; 2016:151–162. | ||
McCrory P, Meewisse WH, Aubry M, et al. Consensus statement on concussion in sport: the 4th International Conference on Concussion in Sport held in Zurich, November 2012. Br J Sports Med. 2013;47:250–258. | ||
Harmon KG, Drezner J, Gammons M, et al. American Medical Society for Sports Medicine position statement: concussion in sport. Clin J Sport Med. 2013;43:783–802. | ||
Caine D, Caine C. Child camel jockeys: a present-day tragedy involving children and sport. Clin J Sport Med. 2005;15(5):287–289. | ||
National Center for Injury Prevention and Control. CDC Injury Research Agenda 2009–2018. Atlanta, GA: Centers for Disease Prevention and Control. Available from: http://stacks.cdc.gov/view/cdc/21769. Accessed January 1, 2009. | ||
Griffin LY, Albohm MJ, Arendt EA, et al. Understanding and preventing noncontact anterior cruciate ligament injuries: a review of the Hunt Valley II meeting, January 2005. Am J Sports Med. 2006;34:1512–1532. | ||
Hastmann-Walsh T, Caine DJ. Injury risk and its long-term effects for youth. In: Baker J, Safai P, Fraser-Thomas J, editors. Health and Elite Sports: Is High Performance Sport a Healthy Pursuit? New York, NY: Routledge; 2015:65–80. | ||
Johnson A, Doherty DJ, Freemont A. Investigation of growth, development, and factors associated with injury in elite schoolboy footballers: prospective study. BMJ. 2009;338:b490. | ||
LeGall F, Carling C, Reilly T. Injuries in young elite female soccer players: an 8-season prospective study. Am J Sports Med. 2008;36:276–284. | ||
LeGall F, Carling C, Reilly T, Vandewalle H, Church J, Rochcongar P. Incidence of injuries in French youth soccer players: a 10 season study. Am J Sports Med. 2006;34:928–998. | ||
Yung PSH. Epidemiology of injuries in Hong Kong elite badminton athletes. Res Sports Med. 2007;15:133–146. | ||
Hägglund M, Waldén M, Ekstrand J. UEFA injury study-an injury audit of European championships 2006 to 2008. Br J Sports Med. 2009;43:483–489. | ||
Waldén M, Hägglund M, Ekstrand J. Football injuries during European Championships 2004–2005. Knee Surg Sports Traumatol Arthrosc. 2007;15:1155–1162. | ||
Junge A, Dvorak J. Injuries in female football players in top-level international tournaments. Br J Sports Med. 2007;41(Suppl 1):i3–i7. | ||
Junge A, Dvorak J, Graf-Baumann T, Peterson L. Football injuries during FIFA tournaments and the Olympic Games 1998–2000: development and implementation of an injury reporting system. Am J Sports Med. 2004;32(1 Suppl):805–895. | ||
Caine DJ, Nassar L. Gymnastics injuries. In: Caine DJ, Maffuli N, editors. Epidemiology of Pediatric Sports Injuries: Individual Sports. Basel, Switzerland: Karger; 2005:18–58. | ||
Nabhan D, Walden T, Street J, Linden H, Moreau B. Sports injury and illness epidemiology during the 2014 Youth Olympic Games: United States Olympic team surveillance. Br J Sports Med. 2016;50(11):688–693. | ||
Ruedl G, Schobersberger W, Pocecco E, et al. Sport injuries and illnesses during the first Winter Youth Olympic Games 2012 in Innsbruck, Austria. Br J Sports Med. 2012;46:1030–1037. | ||
van Beijsterveld AMC, Thizs KM, Backx FJG, Steffen K, Brozičević V, Stubbe JH. Sports injuries and illnesses during the European Youth Olympic Festival 2013. Br J Sports Med. 2015;49:448–452. | ||
Ruedl G, Schnitzer M, Kirschner W, et al. Sports injuries and illnesses during the 2015 Winter European Youth Olympic Festival. Br J Sports Med. 2016;50:631–636. | ||
Knowles SB, Marshall SW, Bowling MJ, et al. Risk factors for injury among high school football players. Epidemiol. 2009;20(2):302–310. | ||
Malina RM, Morano PJ, Barron M. Incidence and player risk factors for injury in youth football. Clin J Sport Med. 2006;16:214–222. | ||
Emery CA, Meeuwisse WH. Injury rates, risk factors, and mechanisms of injury in minor hockey. Am J Sports Med. 2006;34:1960–1969. | ||
McKay C, Campbell T, Meeuwisse W, Emery C. The role of psychological risk factors for injury in elite youth ice hockey. Clin J Sports Med. 2013;23(3)216–221. | ||
Emery CA, Meeuwisse WH, Hartmann SE. Evaluation of risk factors for injury in adolescent soccer. Implementation and validation of an injury surveillance system. Am J Sports Med. 2005;33:1882–1891. | ||
Caine D, Knutzen K, Howe W, et al. A three-year epidemiological study of injuries affecting young female gymnasts. Phys Ther Sport. 2003;4:10–23. | ||
Bailey DA, Wedge JH, McCulloch RG, Martin AD, Bernhardson SC. Epidemiology of fractures of the distal end of the radius in children as associated with growth. J Bone Joint Surg Am. 1989;71:1225–1231. | ||
Duggleby T, Kumar S. Epidemiology of juvenile low back pain: a review. Disabil Rehabil. 1997;19:505–512. | ||
DiFiori JP, Puffer JC, Aish B, Dorey F. Wrist pain in young gymnasts: frequency and effects on training over 1 year. Clin J Sport Med. 2002;12:348–353. | ||
Niemeyer P, Weinberg A, Schmitt H. Stress fracture in the juvenile skeletal system. Int J Sport Med. 2006;27:242–249. | ||
Plisky PJ, Rauh MJ, Kaminski TW, Underwood FB. Start excursion balance test as a predictor of lower extremity injury in high school basketball players. J Orthop Sports Phys Ther. 2006;36:911–919. | ||
Wang HK, Chen CH, Shiang TY, Jan MH, Lin KH. Risk-factor analysis of highs school basketball player ankle injuries: a prospective controlled cohort study evaluating postural sway, ankle strength, and flexibility. Arch Phys Med Rehabil. 2006;87(6):821–825. | ||
Trojiian TH, McKeag DB. Single leg balance test to identify risk of ankle sprains. Br J Sports Med. 2006;40:610–613. | ||
McGuine TA, Greene JJ, Best T, Leverson G. Balance as a predictor of ankle injuries in high school basketball players. Clin J Sport Med. 2000;10:239–244. | ||
Backous DD, Friedl KE, Smith NJ, Parr TJ, Carpine WD Jr. Soccer injuries and their relation to physical maturity. Am J Dis Child. 1988;142:839–842. | ||
Linder MM, Townsend DJ, Jones JC, Balkcom IL, Anthony CR. Incidence of adolescent injuries in junior high school football and its relationship to sexual maturity. Clin J Sport Med. 1995;5:167–170. | ||
LeGall F, Carling C, Reilly T. Biological maturity and injury in elite youth football. Scand J Med Sci Sports. 2007;17(5):564–572. | ||
Stuart MJ, Morrey MA, Smith AM, et al. Injuries in youth football: a prospective observation cohort analysis among players aged 9–13 years. Mayo Clin Proc. 2002;77(4):317–322. | ||
Gomez JD, Ross SK, Calmbach W, Kimmel RB, Schmidt DR, Dhanda R. Body fatness and increased injury rates in high school football lineman. Clin J Sport Med. 1998;8:115–120. | ||
Kaplan TA, Digel SL, Scavo VA, Arellana SB. Effect of obesity on injury risk in high school football players. Clin J Sport Med. 1995;5:43–47. | ||
Knowles SB, Marshall SW, Guskiewicz KM. Issues in estimating risks and rates in sports injury research. J Athl Train. 2006;41:207–215. | ||
Huffman EA, Yard EE, Fields SK, Collins CL, Comstock RD. Epidemiology of rare injuries and conditions among United States High School Athletes during 2005–2006 and 2006–2007. J Athl Train. 2008;43(6):624–630. | ||
Rechel JA, Collins CL, Comstock RD. Epidemiology of injuries requiring surgery among high school athletes in the United States, 2005 to 2010. J Trauma. 2011;71(4):982–989. | ||
Marar M, McIlvain NM, Fields SK, Comstock RD. Epidemiology of concussions among United States high school athletes in 20 sports. Am J Sports Med. 2012;40(4):747–755. | ||
Tenforde AS, Sayres LC, McCurdy ML, Sainani KL, Fredericson M. Identifying sex-specific risk factors for stress fractures in adolescent runners. Med Sci Sports Exerc. 2013;45(10):1843–1851. | ||
Rauh MJ, Koepsell TD, Rivara FP, Margherita AJ, Rice SG. Epidemiology of musculoskeletal injuries among high school cross-country runners. Am J Epidem. 2006;163(2):151–159. | ||
Caine D, Caine C, Maffulli N. Incidence and distribution of pediatric sport-related injuries. Clin J Sport Med. 2006;16(6):500–513. | ||
Emery CA, Hagel B, Decloe M, Carly M. Risk factors for injury and severe injury in youth ice hockey: a systematic review of the literature. Inj Prev. 2010;16(2):113–118. | ||
Cusimano MD, Taback NA, McFaull SR, Hodgins R, Bekele TM, Elfeki N; Canadian Research Team in Traumatic Brain Injury and Violence. Effect of body checking on rate of injuries among minor hockey players. Open Med. 2011;5(1):e57–e64. | ||
Emery CA, Kang J, Shrier I, et al. Risk of injury associated with body checking among youth ice hockey players. JAMA. 2010;303(22):2265–2272. | ||
Dun S, Loftice J, Fleisig GS, Kingsley D, Andrews JR. A biomechanical comparison of youth baseball pitches: is the curveball potentially harmful? Am J Sports Med. 2005;36:686–692. | ||
Fleisig GS, Andrews JR, Cutter GR, et al. Risk of serious injury for young baseball pitchers: a 10-year prospective study. Am J Sports Med. 2011;39(2):253–257. | ||
Dennis RJ, Finch CF, Farhart JP. Is bowling workload a risk factor for injury to Australian junior cricket fast bowlers? Br J Sports Med. 2005;39(11):843–846. | ||
Hjelm N, Werner S, Renstrom P. Injury risk factors in junior tennis players: a prospective 2-year study. Scand J Med Sci Sports. 2012;22(1):40–48. | ||
DiFiori JP, Mandelbaum BR. Wrist pain in a young gymnast: unusual radiographic findings and MRI evidence of growth plate injury. Med Sci Sports Exerc. 1996;28(12):1453–1458. | ||
Loud KJ, Gordon CM, Micheli LJ, Field AE. Correlates of stress fractures among preadolescent and adolescent girls. Pediatrics. 2005;115(4):e399–e406. | ||
Luke A, Lazaro RM, Bergeron MF, et al. Sports-related injuries in youth athletes: is overscheduling a risk factor? Clin J Sport Med. 2011;21(4):307–314. | ||
Olsen SJ, Fleisig GS, Dun S, Loftice J, Andrews JR. Risk factors for shoulder and elbow injuries in adolescent baseball pitchers. Am J Sports Med. 2006;34(6):905–912. | ||
Lyman S, Fleisig GS, Waterbor JW, et al. Longitudinal study of elbow and shoulder pain in youth baseball pitchers. Med Sci Sports Exerc. 2001;33(11):1803–1810. | ||
Pinto M, Kuhn JE, Greenfield ML, Hawkins RJ. Prospective analysis of ice hockey injuries at the junior A level over the course of one season. Clin J Sport Med. 1999;9(2):70–74. | ||
Thein-Nissenbaum JM, Rauh MJ, Carr KE, Loud KJ, McGuine TA. Associations between disordered eating, menstrual dysfunction, and musculoskeletal injury among high school athletes. J Orthop Sports Phys Ther. 2011;41(2):60–69. | ||
Rauh MJ, Nichols JF, Barrack MT. Relationships among injury and disordered eating, menstrual dysfunction, and low bone mineral density in high school athletes: a prospective study. J Athl Train. 2010;45(3):243–252. | ||
Caine D, Goodwin B. Injury risk factors in pediatric and adolescent sports. In: Caine D, Purcell L, editors. Injury in Pediatric and Adolescent Sports: Epidemiology, Treatment and Prevention. New York, NY: Springer; 2016:191–204. | ||
Harmer P. Injury research in pediatric and adolescent sports. In: Caine D, Purcell L, editors. Injury in Pediatric and Adolescent Sports: Epidemiology, Treatment and Prevention. New York, NY: Springer; 2016:233–242. | ||
Furnham A, Badmin N, Sneade I. Body image dissatisfaction: gender differences in eating attitudes, self-esteem and reasons for exercise. J Psychol. 2002;136(6):581–596. | ||
National Association of Anorexia Nevrosa and Associated Disorders. 2013. Available at: http://www.anad.org/get-information/about-eating-disorders/eating-disorders-statistics/. Accessed April 25, 2016. | ||
Shriver LH, Betts NM, Wollenberg G. Dietary intakes and eating habits of college athletes: are female collegiate athletes following the current sports nutritional standards? J Am Coll Health. 2013;61(1):10–16. | ||
Nutter J. Seasonal changes in female athletes diets. Int J Sport Nutr. 1991;1(4):395–407. | ||
Schilling L, Nikita M. What coaches need to know about the nutrition of female high school athletes: a dietitian’s perspective. Strength Condit J. 2008;30(5):16–17. | ||
Buchholz A, Mack H, McVey G, Feder S, Barrowman N. BodySense: an evaluation of a positive body image intervention on sport climate for female athletes. Eat Disord. 2008;16:308–321. | ||
Abood DA, Black DR, Birnbaum RD. Nutrition education intervention for college female athletes. J Nutr Educ Behav. 2004;36(3);135–137. | ||
Prather H, Hunt D, McKeon K, et al. Are elite female soccer athletes at risk for disordered eating attitudes, menstrual dysfunction, and stress fractures? PM R. 2016;8(3):208–213. | ||
Giel KE, Hermann-Werner A, Mayer J, et al. Eating disorder pathology in elite adolescent athletes. Int J Eat Disorder. 2016;49(6):553–562 . | ||
Martinsen M, Sundgot-Borden J. Higher prevalence of eating disorders among adolescent elite athletes than controls. Med Sci Sports Exerc. 2013;45(6):1188–1197. | ||
Muia EN, Wright HH, Onywere VO, Kuria EN. Adolescent elite Kenyan runners are at risk for energy deficiency, menstrual dysfunction and disordered eating. J Sports Sci. 2016;34(7):598–606. | ||
Emery C, Roy TO, Hagel B, Macpherson A, Nettel-Aquirre A. Injury prevention in youth sport. In: Caine D, Purcell L, editors. Injury in Pediatric and Adolescent Sports: Epidemiology, Treatment and Prevention. New York, NY: Springer; 2016:205–229. | ||
Whittaker JL, Woodhouse LJ, Nettel-Aguirre A, Emery CA. Outcomes associated with early post-traumatic osteoarthritis and other negative health consequences 3–10 years following knee joint injury in youth sport. Osteoarthritis Cartilage. 2015;23(7):1122–1129. | ||
Golightly YM, Marshall SW, Caine DJ. Future shock: youth sports and osteoarthritis risk. Lower Extremity Rev. 2011;3(10):22–27. | ||
Allen KD, Golightly YM. Epidemiology of osteoarthritis: state of the evidence. Curr Opin Rheumatol. 2015;27(3):276–283. | ||
Ajuied A, Wong F, Smith C, et al. Anterior ligament injury and radiologic progression of knee osteoarthritis: a systematic review and meta-analysis. Am J Sports Med. 2014;42(9):2242–2252. | ||
Richmond SA, Fukuchi RK, Ezzat A, Schneider K, Schneider G, Emery CA. Are joint injury, sport activity, physical activity, obesity, or occupational activities predictors for osteoarthritis? A systematic review. J Orthop Sports Phys Ther. 2013;43(8):515–519. | ||
von Porat A, Roos EM, Roos H. High prevalence of osteoarthritis 14 years after an anterior cruciate ligament tear in male soccer players: a study of radiographic and patient relevant outcomes. Ann Rheum Dis. 2004;63(3):260–273. | ||
McNicholas MJ, Rowley DI, McGurty D, et al. Total meniscectomy in adolescence: a thirty-year follow-up. J Bone Joint Surg Br. 2000;82(2):217–221. | ||
Dai L, Zhang W, Xu Y. Meniscal injury in children: long-term results after meniscectomy. Knee Surg Sports Traumatol Arthrosc. 1997;5(2):77–79. | ||
Wroble RR, Henderson RC, Campion ER, et al. Meniscectomy in children and adolescents: a long-term follow-up study. Clin Orthop Relat Res. 1992;279:180–189. | ||
Manzione M, Pizzutillo PD, Peoples AB, Schweizer PA. Meniscectomy in children: a long-term follow-up study. Am J Sports Med. 1983;11(3):111–115. | ||
Zaman M, Leonard MA. Meniscectomy in children: results in 59 knees. Injury. 1981;12(5):425–428. | ||
Medlar RC, Mandiberg JJ, Lyne ED. Meniscectomies in children. Report of long-term results (mean, 8.3 years) of 26 children. Am J Sports Med. 1980;8(2):87–92. | ||
Anderson DD, Chubinskaya S, Guilak F, et al. Post-traumatic osteoarthritis: improved understanding and opportunities for early intervention. J Orthop Res. 2011;29(6):802–809. | ||
Fleming BC, Hulstyn MJ, Osksendahl HL, Fadale PD. Ligament injury, reconstruction, and osteoarthritis. Curr Opin Rheumatol. 2005;16(5):354–362 | ||
Maffulli N, Longo UG, Gougoulias N, Loppini M, Denaro V. Long-term health outcomes of youth sports injuries. Br J Sports Med. 2010;44(1):21–25. | ||
Caine DJ, Daly RM, Jolly D, Hagel BE, Cochrane B. Risk factors for injury in young competitive female gymnasts. Br J Sports Med. 2006;40:89–94. | ||
DiFiori JP, Benjamin HJ, Brenner J, et al. Overuse injuries and burnout in youth sports: a position statement from the American Medical Society for Sports Medicine. Clin J Sport Med. 2014;24(1):3–20. | ||
Roberts WO. Overuse injuries and burnout in youth sports. Clin J Sport Med. 2014;24(1);1–2. | ||
Winsley R, Matos N. Overtraining and elite youth athletes. Med Sport Sci. 2011;56:97–105. | ||
Hellstedt, JC. The coach/parent/athlete relationship. Sport Psychol. 1987;1:151–160. | ||
Williams JM, Andersen MB. Psychosocial antecedents of sport injury: review and critique of the stress and injury model. J Appl Sport Psychol. 1998;10(1):5–25. | ||
Kerr, G, Minden H. Psychological factors related to the occurrence of athletic injuries. J Sport Exerc Psychol. 1988;10:167–173. | ||
Petrie TA. Psychosocial antecedents of athletic injury: the effects of life stress and social support on female college gymnasts. Behav Med. 1992;18(3):127–138. | ||
Holmes TH. Psychological screening. In Football Injuries. Papers presented at a workshop. Sponsored by Subcommittee on Athletic Injuries, Committee on the Skeletal System, Division of Medical Sciences, National Research Council; February 1969; Washington, DC: National Academy of Sciences; 211–214. | ||
Steffen K, Pensgaard A, Bahr R. Self-reported psychological characteristics as risk factors for injuries in female youth football. Scand J Med Sci Sports. 2009;19(3):442–451. | ||
Puffer JC, McShane JM. Depression and chronic fatigue in athletes. Clin Sports Med. 1992;11(2):327–338. | ||
Cohn PJ. An exploratory study on sources of stress and athlete burnout in youth golf. Sport Psychol. 1990;4(2):95–106. | ||
Gould D, Jackson S, Finch L. Sources of stress in national champion figure skaters. J Sport Exerc Psychol. 1993;15(2):134–159. | ||
Puente-Diaz R, Anshel MH. Sources of acute stress, cognitive appraisal, and coping strategies among highly skilled Mexican and U.S. competitive tennis players. J Soc Psychol. 2005;145(4):429–446. | ||
Scanlan TK, Stein GL, Ravizza K. An in-depth study of former elite figure skaters: sources of stress. J Sport Exerc Psychol. 1991;13(2):103–120. | ||
American College of Sports Medicine, American Academy of Family Physicians; American Academy of Orthopaedic Surgeons, American Medical Society for Sports Medicine, American Orthopaedic Society for Sports Medicine, American Osteopathic Academy of Sports Medicine. Psychological issues related to injury in athletes and the team physician: a consensus statement. Med Sci Sports Exerc. 2006;38(11):2030–2040. | ||
Madison, R, Prapavessis H. A psychological approach to the prediction and prevention of athletic injury. J Sport Exerc Psychol. 2005;27:289–310. | ||
Rogers TJ, Landers DM. Mediating effects of peripheral vision in the life event stress/athletic injury relationship. J Sport Exerc Psychol. 2005;27:271–288. | ||
Anderson CB, Masse LC, Zhang H, Coleman KJ, Chang S. Contribution of athletic identity to child and adolescent physical activity. Am J Prev Med. 2009;37(3):220–226. | ||
Visek AJ, Hurst JR, Maxwell JP, Watson JC. A cross-cultural psychometric evaluation of the athletic identity measurement scale. J Appl Sport Psychol. 2008;20:473–480. | ||
Brewer BW, Van Raalte JL, Linder DE. Athletic identity: Hercules’ muscles or Achilles heel? Int J Sport Psychol. 1993;24(2):237–254. | ||
Horton RS, Mack DE. Athletic identity in marathon runners: functional focus or dysfunctional commitment? J Sport Behav. 2000;23(2):101–119. | ||
Miller PS, Kerr GA. The athletic, academic and social experience of intercollegiate student athletes. J Sport Behav. 2002;25(4);346–367. | ||
Ryba TV, Aunola K, Kalaja S, Selanne H, Ronkainen NJ, Nurmi JE. A new perspective on adolescent athletes’ transition into upper secondary school: a longitudinal mixed methods study protocol. Cogent Psychol. 2016;3(1):1–15. | ||
Verkooijen KT, van Hove P, Dik G. Athletic identity and well-being among young talented athletes who live in a Dutch elite sport center. J Appl Sport Psychol. 2012;24(1):106–113. | ||
Lemyre PN, Hall HK, Roberts GC. A social cognitive approach to burnout in elite athletes. Scand J Med Sci Sports. 2008;18:221–234. | ||
Frank R, Nixdorf I, Beckmann J. Depression among elite athletes: prevalence and psychological factors. Dtsch Z Sportmed. 2015. Available at: http://www.zeitschrift-sportmedizin.de/fileadmin/content/Englische_Artikel/Originalia_Frank_englisch.pdf. Accessed July 18, 2016 | ||
Hamer M, Stamatakis E, Steptoe A. Dose-response relationship between physical activity and mental health: the Scottish health survey. Br J Sports Med. 2009:43(14):1111–1114. | ||
Daley A. Exercise and depression: a review of reviews. J Clin Psychol Med Settings. 2008;15(2):140–147. | ||
Gulliver A, Griffiths KM, Christensen H, et al. Internet-based interventions to promote mental health help-seeking in elite athletes: an exploratory randomized controlled trial. J Med Internet Res. 2012;14(3):e69. | ||
Gulliver A, Griffiths KM, Christensen H. Barriers and facilitators to mental health help-seeking for young elite athletes: a qualitative study. BMC Psychiatry. 2012;12:157. | ||
Hammond T, Gialloreto C, Kubas H, Hap Davis H. The prevalence of failure-based depression among elite athletes. Clin J Sport Med. 2013;23(4):273–277. | ||
Leddy, MH, Lambert ML, Ogles BM. Psychological consequences of athletic injury among high-level competitors. Res Q Exerc Sport. 1994;65(4):347–354. | ||
Manuel JC, Shilt JS, Curl WW, et al. Coping with sports injuries: an examination of the adolescent athlete. J Adolesc Health. 2002;31(5):391–393. | ||
Jayanthi N, Pinkham C, Dugas L, Patrick B, Labella C. Sports specialization in young athletes: evidence-based recommendations. Sports Health. 2013;5(3):251–257. | ||
Bompa T. From Childhood to Champion Athlete. Toronto, Canada: Veritas Publishing, Inc. 1995. | ||
Barynina II, Vaitsekhovskii SM. The aftermath of early sports specialization for highly qualified swimmers. Fitness Sports Rev Int. 1992;27:132–133. | ||
Wall M, Cote J. Developmental activities that lead to dropout and investment in sport. Pediatr Exerc Sci. 2007;12(1):77–87. | ||
Butcher J, Lindner KJ, Johns DP. Withdrawal from competitive youth sport: a retrospective ten-year study. J Sport Behav. 2002;25(2):145–163. | ||
Law, M, Cote J, Ericsson KA. Characteristics of expert development in rhythmic gymnastics: a retrospective study. Int J Exerc Sport Psychol. 2007;5(1):82–103. | ||
Gould D, Udry E, Tuffey S, Loehr J. Burnout in competitive junior tennis players: a quantitative psychological assessment. Sport Psychol. 1996;10(4):322–340. | ||
Budgett R. Fatigue and underperformance in athletes: the overtraining syndrome. Br J Sports Med. 1998;32(2):107–110. | ||
Small E. Chronic musculoskeletal pain in young athletes. Pediatr Clin North Am. 2002;49(3):655–662. | ||
O’Conner PJ, Morgan WP, Raglin JS, Barksdale CM, Kalin NH. Mood state and salivary cortisol levels following overtraining in females swimmers. Psychoneuroendocrinology. 1989;14(4):303–310. | ||
Nixdorf I, Frank R, Hautzinger M, Beckmann J. Prevalence of depressive symptoms and correlating variables among German elite athletes. J Clin Sport Psychol. 2013;7(4):313–326. | ||
Steinacker JM, Brick M, Simsch C, et al. Thyroid hormones, cytokines, physical training and metabolic control. Horm Metab Res. 2005;37(9):538–544. | ||
Ariza-Vargas L, Dominguez-Escribano M, Lopez-Bedoya J, Vernetta-Santana M. The effect of anxiety on the ability to learn gymnastic skills: a study based on the schema theory. Sport Psychol. 2011;25(2):127–143. | ||
Maki BE, McIlroy WE. Influence of arousal and attention on the control of postural sway. J Vestib Res. 1996;6(1):53–59. | ||
Kolt GS, Kirkby RJ. Injury, anxiety, and mood in competitive gymnastics. Percept Mot Skills. 1994;78(3):955–962. | ||
Appleton PR, Hill AP. Perfectionism and athlete burnout in junior elite athletes: the mediating role of motivation regulations. J Clin Sport Psychol. 2012;6(2):129–145. | ||
Appleton PR, Hall HK, Hill AP. Relations between multidimensional perfectionism and burnout in junior-elite male athletes. Psychol Sport Exerc. 2009;10(4):457–465. | ||
Terry-Short LA, Owens RG, Slade PD, Dewey ME. Positive and negative perfectionism. Pers Indiv Differ. 1995;18(5):663–668. | ||
Flett GL, Hewitt PL. The perils of perfectionism in sports and exercise. Curr Dir Psychol. 2005;14(1):14–18. | ||
Frost RO, Henderson KJ. Perfectionism and reactions to athletic competition. J Sport Exerc Psychol. 1991;13(4):323–335. | ||
Dunn JGH, Dunn JC, Gotwals JK, Vallance JKH, Craft JM, Syrotuik DG. Establishing construct validity evidence for the Sport Multidimensional Perfectionism Scale. Psychol Sport Exerc. 2006;7:57–59. | ||
Gould D, Lauer L, Rolo C, Jannes C, Pennisi N. Understanding the role parents play in tennis success: a national survey of junior tennis coaches. Br J Sports Med. 2006;40(7):632–636. | ||
Shields DL, Bredemeir BL, LaVoi NM, Power FC. The sport behavior of youth, parents, and coaches: the good, the bad, and the ugly. J Res Character Educ. 2007;3(1):43–59. | ||
Kidman L, Mackenzie A, Mackenzie B. The nature and target of parental comments during youth sports competitions. J Sport Behav. 1999;22(1):54–68. | ||
Blom LC, Drane D. Parents’ sideline comments: exploring the reality of a growing issue. Athletic Insight. 2008;10(3). Available from: http://www.athleticinsight.com/. Accessed July 18, 2016. | ||
Vincent MA, McCabe MP. Gender differences among adolescents in family, and peer influences on body dissatisfaction, weight loss, and binge eating behaviors. J Youth Adolesc. 2000;29(2):205–221. | ||
Pike KM, Rodin J. Mothers, daughters, and disordered eating. J Abnorm Psychol. 1991;100(2):198–204. | ||
Blackmer V, Searight HR, Ratwik SH. The relationship between eating attitudes, body image, and perceived family-of-origin climate among college athletes. N Am J Psychol. 2011;13(3):435–446. | ||
Francisco R, Alarcao M, Narciso I. Aesthetic sports as high risk contexts for eating disorders: young elite dancers and gymnasts perspectives. Span J Psychol. 2012;15(1):265–274. | ||
Kerr G, Stirling A. Parents’ reflections on their child’s experiences of emotionally abusive coaching practices. J Appl Sport Psychol. 2012;24(2):191–206. | ||
Stirling EA. 2011. Initiating and sustaining emotional abuse in the coach-athlete relationship: athletes’, parents’, and coaches’ reflections. Available at: https://tspace.library.utoronto.ca/bitstream/1807/35742/3/Stirling_Ashley_E_201106_PhD_thesis.pdf. Accessed July 18, 2016. | ||
Glaser D. Emotional abuse and neglect (psychological maltreatment): a conceptual framework. Child Abuse Negl. 2002;26(6–7):697–714. | ||
Alexander K, Stafford A, Lewis R. The experiences of children participating in organized sport in the UK, Edinburgh: University of Edinburgh/NSPCC. 2011. Available at: http://www.nspcc.ork/uk/Inform/research/findings/experiences_children_sport_main_report_wdf85014.pdf. Accessed July 18, 2016. | ||
Huffington Post. Dominique Moceanu talks body image in gymnastics, says coaches can“scar for life.” Available at: http://www.huffingtonpost.com/2013/07/19/dominique-moceanu-body-im_n_3625224.html. Accessed July 18, 2016. | ||
Mountjoy M, Rhind DJ, Tilvas A, Leglise M. Safeguarding the child athlete in sport: a review, a framework and recommendations for the IOC youth athlete development model. Br J Sports Med. 2015;49(13):883–886. | ||
Emery CA, Roy TO, Whittaker JL, Nettel-Aquirre A, van Mechelen W. Neuromuscular training injury prevention strategies in youth sport: a systematic review and meta-analysis. Br J Sports Med. 2015;49:865–870. | ||
Schiff M, Caine D, O’Halloran R. Injury prevention in sports. Am J Lifestyle Med. 2010;4:42–64. | ||
Caine D, Maffulli N, Caine C. Epidemiology of pediatric and adolescent sports injuries “International Perspectives,” Micheli LJ (ed). Clin Sports Med. 2008;27(1):19–50. | ||
Emery CA, Meeuwisse WH, McAllister JR. A survey of sport participation, sport injury and sport safety practices in adolescents. Clin J Sport Med. 2006;16:20–26. | ||
Russell K, Christie J, Hagel, BE. The effect of helmets on the risk of head and neck injuries among skiers and snowboarders: a meta-analysis. CMAJ. 2010;182(4):333–340. | ||
Cusimano MD, Kwok J. The effectiveness of helmet wear in skiers and snowboarders: a systematic review. Br J Sport Med. 2010;44(11):781–786. | ||
Haider AH, Saleem T, Bilaniuk JW, Barraco RD; Eastern Association for the Surgery of Trauma Injury Control Violence Prevention Committee. An evidence based review: efficacy of safety helmets in reduction of head injuries in recreational skiers and snowboarders. J Trauma Acute Care Surg. 2012;73(5):1340–1347. | ||
Benson BW, Mohtadi NG, Rose MS, Meeuwisse WH. Head and neck injuries among ice hockey players wearing full face shields versus half face shields. JAMA. 1999;282(24):2328–2332. | ||
Benson BW, Rose MS, Meeuwisse WH. The impact of face shield use on concussion in ice hockey: a multivariate analysis. Br J Sport Med. 2002;36(1):27–32. | ||
Stuart MJ, Smothh AM, Malo-Oritguera SA, Fischner TL, Larson DR. A comparison of facial protection and the incidence of head, neck, and facial injuries in Junior A hockey players: a function of individual playing time. Am J Sports Med. 2002;30(1):39–44. | ||
Russell K, Hagel B, Francescutti LH. The effect of wrist guards on wrist and arm injuries among snowboarders: a systematic review. Clin J Sport Med. 2007;17(2):145–150. | ||
Emery CA. Injury prevention in paediatric sport-related injuries: a scientific approach. Br J Sports Med. 2010;44:64–99. | ||
Martinsen M, Bahr R, Borresen R, Holme I, Pensgaard AM, Sundgot-Borgen J. Preventing eating disorders among youth elite athletes: a randomized controlled trial. Med Sci Sports Exerc. 2014;46(3):435–447. | ||
Martinsen M, Sherman RT, Thompson RA, Sundgot-Borgen J. Coaches’ knowledge and management of eating disorders: a randomized controlled trial. Med Sci Sports Exerc. 2015;47(5):1070–1078. | ||
Main L, Grobe JR. A multi-component assessment model for monitoring training distress among athletes. Eur J Sport Sci. 2009;9(4):195–202. | ||
Nicolas M, Gaudreau P, Franche V. Perception of coaching behaviors, coping, and achievement in a sport competition. J Sport Exerc Psychol. 2011;33(3):460–468. | ||
Gustafsson H, Skoog T. The mediational role of perceived stress in the relation between optimism and burnout in competitive athletes. Anxiety Stress Coping. 2012;25(2):183–199. | ||
Gerber M, Kalak, N, Lmola S, et al. Are adolescents with high mental toughness levels more resilient against stress? Stress Health. 2013;29(2):164–171. | ||
Turner MJ, Jones MV, Sheffield D, Slater MJ, Barker JB, Bell JJ. Who thrives under pressure? Predicting the performance of elite academy cricketers using the cardiovascular indicators of challenge and threat states. J Sport Exerc Psychol. 2013;35(4):387–397. | ||
Tamminen KA, Holt NL, Crocker PRE. Adolescent athletes: psychosocial challenges and clinical concerns. Curr Opin Psychiatry. 2012;25(4):293–300. | ||
Knight CJ, Boden CM, Holt NL. Junior tennis players’ preferences for parental behaviors. J Appl Sport Psychol. 2010;22(4):377–391. | ||
Knight CJ, Neely KC, Holt NL. Parental behaviors in team sports: how do female athletes want parents to behave? J Appl Sport Psychol. 2011;23(1):76–92. | ||
Keegan RJ, Spray CM, Harwood CG, Lavallee D. The motivational atmosphere in youth sport: coach, parent, and peer influences on motivation in specializing sport participants. J Appl Sport Psychol. 2010;22(1):87–105. | ||
Cote J, Baker J, Abernethy, B. From play to practice: a developmental framework for the acquisition of expertise in team sports. In: Starkes J, Ericsson KA, editors. Expert Performance in Sports: Advances in Research on Sport Expertise. Champaign, IL: Human Kinetics; 2003:89–110. | ||
Arnold R, Fletcher D. A research synthesis and taxonomic classification of the organizational stressors encountered by sport performers. J Sport Exerc Psychol. 2012;34(3):397–429. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
