Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 10
The association of weight loss with patient experience and outcomes in a population of patients with type 2 diabetes mellitus prescribed canagliflozin
Authors Gerlanc NM, Cai J, Tkacz J, Bolge SC, Brady BL
Received 9 December 2016
Accepted for publication 17 January 2017
Published 20 March 2017 Volume 2017:10 Pages 89—99
DOI https://doi.org/10.2147/DMSO.S129824
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Ming-Hui Zou
Nicole M Gerlanc,1 Jennifer Cai,2 Joseph Tkacz,1 Susan C Bolge,2 Brenna L Brady1
1Health Analytics, LLC Columbia, MD, USA; 2Janssen Scientific Affairs, LLC Titusville, NJ, USA
Objective: Type 2 diabetes mellitus (T2DM) is a chronic condition complicated by being overweight or obese. This study used a patient survey to assess health, satisfaction, and diabetes self-management in relation to weight management.
Methods: A survey including the Current Health Satisfaction Questionnaire, Diabetes Distress Scale, and Diabetes Treatment Satisfaction Questionnaire was administered using an online platform to a sample of 205 patients with T2DM prescribed canagliflozin. Patients were placed into 5 groups based on their self-reported weight change since initiation of canagliflozin: Lost >10 lbs, Lost 5–10 lbs, Lost <5 lbs, No Change, and Gained Weight. One-way ANOVAs, Kruskall–Wallis tests, and multivariable regression were used to explore differences between weight loss groups.
Results: The majority of patients (66.8%) reported losing weight. Compared to other groups, patients who lost >10 lbs were more likely to be engaged in a weight loss program for at least 6 months. Patients in the Lost >10 lbs and Lost 5–10 lbs groups reported the greatest satisfaction with canagliflozin (p<0.05 for both). Multivariable analyses controlling for patient demographic and treatment characteristics revealed that losing >10 lbs was associated with reduced diabetes distress, improved A1c and blood glucose levels, and decreased perceived frequency of hyperglycemia (p<0.05).
Conclusion: Increased positive patient outcomes, engagement in diabetes self-management, and medication satisfaction were observed among patients who reported weight loss. These findings suggest that a T2DM regimen that includes canagliflozin as part of a weight loss regimen can help improve patient outcomes and experiences with T2DM.
Keywords: T2DM, patient outcomes, diabetes self-management, SGLT2 inhibitor, weight management
Introduction
Type 2 diabetes mellitus (T2DM) is a chronic metabolic disorder characterized by insulin resistance resulting in increased blood glucose levels (BGLs). Poorly managed BGLs can lead to numerous health complications including cardiovascular disease, nephropathy, retinopathy, and neuropathy.1–5 Diabetes affects approximately 6.7% of the US population, making it one of the most prevalent chronic diseases in the United States.6 Accordingly, diabetes also places a substantial burden on the US health care system, with estimated annual direct and indirect costs totaling US$245 billion.7 To optimize health care system performance, the Institute for Healthcare Improvement has developed the Triple Aim framework, calling for simultaneous pursuit of improving patient experience of care, improving health of population, and reducing per capita health care costs.8 Achievement of the Triple Aim in chronic diseases like diabetes can be particularly challenging as effective treatment and management of T2DM can require numerous medications, therapies, and appointments with various health care providers, all of which can lead to increased health care costs. Despite these challenges, patients who are actively engaged in managing their disease may be able to substantially improve their quality of care while still reducing health care costs.9 Therefore, achievement of the Triple Aim in diabetes may rely on effective patient-centered care to help empower patients to become self-managers of their disease. To achieve this goal, health care providers will need to understand the experience with T2DM from patients’ perspective in order to assist patients to become their own health care advocates. Use of validated questionnaires to gain patients perspective into the challenges associated with management of T2DM is one of the first steps in this process.
Treatment for T2DM focuses on controlling BGLs to maintain metabolic function and slow disease progression.1–5 Most patients require antihyperglycemic agents (AHA), in addition to self-care behaviors including healthy eating, being active, and diabetes monitoring, as part of their diabetes treatment regimen. 10,11 Treatment approaches to manage BGLs change over time or with increased disease progression. Treatment guidelines now stress a patient-centered approach to AHA therapy, basing treatment choices on factors including patient preferences, needs, and values.5,10 Although several older agents, including metformin, remain preferred agents for patients with T2DM, the abundance of newer pharmaceutical agents for diabetes hold promise for improving glycemic control with a reduced self-care burden and lower risk of hypoglycemia or weight gain. These agents may be effective for patients who require treatment intensification or experience difficultly with weight management.
Approximately 85% of patients with T2DM are overweight or obese.12 Aside from negatively impacting patient’s health and activity levels, being overweight or obese also contributes to insulin resistance making it more difficult to manage BGLs and increasing patients’ risk of diabetes complications.13,14 Moreover, some T2DM treatments can cause weight gain, which can negatively impact patient engagement in diabetes self-management practices, and exacerbate the weight issue already present.12,15 As a result, providers should consider patient weight, as well as their engagement in diet and exercise, when making choices on prescribing AHAs. Some of the newer AHAs, for example, the sodium glucose cotransporter-2 (SGLT2) inhibitors, can aid patients in weight management by assisting patients to lose 5–10 lbs, while still helping patients to manage their BGLs. Further, weight loss in diabetes is also associated with improved lipid profiles, improved blood pressure, regulation of BGL, and a reduction in cardiovascular risk factors.5,13,14,16,17
The physical toll and chronic nature of diabetes can also impact patient health-related quality of life (HRQoL), potentially worsening the health care experience of some individuals.18–20 Specifically, patients with diabetes report increased rates of anxiety and depression, presence of comorbidities, and an increased self-care burden.18,20,21 Additionally, intensive treatment regimens including use of multiple medications or insulin have also been shown to diminish patient HRQoL due to the burden these treatments place on patients’ daily lives. This interplay between HRQoL and treatment for T2DM highlights an interesting contradiction in diabetes, as treatment regimens, including pharmaceutical and lifestyle changes, aimed at improving HRQoL through improving patient’s health can themselves inhibit patient HRQoL.19,20,22 Although lifestyle changes are critical for T2DM management, the negative impact of diet and exercise plans on patient short-term HRQoL can overshadow the potential long-term positive effects of self-management, making these necessary lifestyle changes difficult for many patients to initiate and maintain.13,22,23 Therefore, incorporation of pharmaceutical or other treatment regimens that can assist in improving patient health may instill greater drive for positive diabetes self-management behaviors in the patient through improving their HRQoL.
Improvement in HRQoL stands to not only impact patient health but may also translate to cost savings in diabetes. Studies show that poor management of BGLs and the presence of diabetes-related complications dramatically increase health care costs of patients with T2DM.24,25 Therefore, comprehensive care regimens for patients with T2DM that can help to reduce the risk of developing diabetes-related complications stand to lead to substantial health care savings.26 Tailoring treatment regimens to individual patient preferences, comorbidity, or lifestyle may also lead to an improved patient experience and outcomes, which could further incentivize patients to initiate and maintain good health behaviors and diabetes self-management regimens.5,27 The objective of this study was to examine the relationship between weight loss and patients’ experience with T2DM; to address this objective, a panel of patients with T2DM prescribed canagliflozin, an SGLT2 inhibitor that has been shown to help patients with T2DM lose weight, were surveyed on various aspects of patient HRQoL known to be impacted by weight loss, including clinical factors, health satisfaction, diabetes self-management, and physical and emotional health.15,17,28,29
Methods
Survey development
The literature on T2DM was reviewed to identify appropriate scales and items for inclusion in the final survey; focus was placed on validated surveys that assessed the impact of T2DM on patient’s HRQoL, T2DM medication satisfaction, and diabetes self-management. Three established surveys, the Current Health Satisfaction Questionnaire (CHES-Q), Diabetes Treatment Satisfaction Questionnaire (DTSQ), and the Diabetes Distress Scale (DDS) were included in the final survey.30–32 The CHES-Q was included to capture patient’s level of satisfaction with their current physical and emotional health; with higher scores indicating greater health satisfaction. The DTSQ (DTSQ© Prof Clare Bradley)30 assessed patient satisfaction with diabetes treatment; a total treatment satisfaction scale is reported along with scores from two items that assess the perceived frequency of hyperglycemia and hypoglycemia. Higher total DTSQ treatment satisfaction scale scores indicate greater treatment satisfaction, while lower scores on the two items assessing hyperglycemia and hypoglycemia indicate a reduced perceived frequency. The DDS evaluated patient level of distress by assessing the degree to which diabetes-related problems impacted patients’ lives; a total score and four subscale scores are reported for the DDS, with lower scores indicating reduced distress. In the DDS a score of three or higher indicates a moderate level of distress. Additional items were generated for domains where validated survey items were not available. Engagement in lifestyle changes and satisfaction with medication were assessed through multiple response items that queried patients exercise, diet, and weight loss routines and their satisfaction with their current medication as compared to their previous oral or injectable AHA, respectively. For clinical factors patients were asked whether their diabetes health care provider told them that their A1c, blood glucose, or blood pressure improved, stayed the same, or got worse over the last 3 months.
An advisory panel, composed of an endocrinologist and patients with T2DM, reviewed the survey to ensure clarity of items and appropriateness of domains. All panel participants completed the survey along with a debriefing interview that focused on item definition and clarity, relevance of included domains, time to completion, and overall understanding of the survey. Participant comments approved by the survey development team were used to finalize the survey. The final questionnaire was composed of three validated scales and 21 new items that queried patient demographics, T2DM medication history, diabetes and weight management, and satisfaction with AHAs.
Participants
The results presented here are part of a larger study assessing the impact of treatment satisfaction and HRQoL in T2DM. Patients included in this analysis were required to be aged ≥18 years at the time of survey completion, have a diagnosis of T2DM (self-reported), have a current prescription for canagliflozin, and have been taking canagliflozin for a minimum of 3 months.
Recruitment and administration
Recruitment of participants took place from September 2015 through January 2016. Patients were recruited to complete the survey through emails and postings in physician offices, pharmacies, and T2DM community message boards.
This study was approved by the Chesapeake Institutional Review Board. All surveys were administered online using a point and click survey interface. All participants were required to complete an electronic informed consent that was presented prior to the online survey. The first portion of the survey served as an eligibility module, which excluded ineligible patients from the survey based on inclusion/exclusion criteria. All eligible patients who completed an informed consent form and the survey were remunerated US$50 for their time in survey completion; patients were only eligible to complete a single survey.
Statistical analyses
Bivariate analyses
Patient demographics and characteristics including gender, age, ethnicity, region of residence, insurance type, disease duration, medication use, and the presence of select comorbidities were reported as frequencies and percentages for the sample. As the focus of this study was to assess the impact of weight loss on patients’ experience with T2DM, the remaining analyses placed patients into one of five self-reported weight change groups: Lost >10 lbs, Lost 5–10 lbs, Lost <5 lbs, No Change, and Gained Weight. The weight loss categories were selected as the weight loss of 5–10 lbs has been shown to be associated with the improvement of many clinical indicators in T2DM.5,13,14 To test for significant differences among the five weight groups, one-way analysis of variance (ANOVA) was used for the normally distributed continuous variable body mass index (BMI). One-way median analysis was used to assess differences in CHES-Q scale scores, DTSQ, and DDS scores, which did not evidence a normal distribution. Kruskal–Wallis tests were used for ordinal categorical variables including age category, disease duration, and medication use, and chi-square tests of equality of proportions were used for the remaining binary categorical variables including patient demographics and characteristics, medication satisfaction and patient engagement items, and the clinical factors. For all bivariate analyses, significant omnibus tests were followed by the appropriate pairwise post hoc tests (t-test for ANOVA; median two-sample test for median analysis; Kruskal–Wallis and pairwise chi-square for chi-square tests) to identify specific group differences. As this study was exploratory in nature and not aimed at hypotheses testing, the critical value for significance was not adjusted for multiplicity.33 Pearson’s correlations were also calculated between the weight grouping variable and the summary scores from each of the validated surveys, allowing for a comparison of the relationship between each individual group’s validated survey scores to the balance of the sample.
Multivariate analyses
General linear multivariable regression models were constructed for scores from each of the established surveys, CHES-Q, DDS, and DTSQ, and the clinical factors. For each model, the dependent variable was regressed onto the same vector of covariates, which included weight change group, patient demographics of age, gender, insurance status, ethnicity, comorbid diagnoses, and current concomitant AHAs. Weight group served as the primary independent variable with the Gained Weight group serving as the reference category. The Wald test was used to determine significance in the general linear models.
For analyses in which normality was an assumption, distributions for dependent variables were tested for normality based on skewness and kurtosis statistics. For all statistical modeling, the critical alpha level was set at 0.05. All data management and analyses were conducted using SAS v9.4 (SAS, Cary, NC, USA).
Results
A total of 205 canagliflozin-treated patients qualified for the study and completed the survey; overall sample demographics were largely representative of the national T2DM population.6 There was a slightly greater representation of females than males in the sample (51.2% vs 48.8%; Table 1). Patients were primarily middle aged, with 74.1% of the sample between 35 and 64 years. The majority of patients were Caucasian (66.8%), followed by Black/African-American (16.6%), and Hispanic/Latino (9.8%); remaining patients reported being Asian/Pacific Islander (3.4%), multiracial (2.0%), or American Indian/Alaskan Native (1.5%). The south (44.4%) was the geographic region with the greatest representation, and approximately half of the sample received health insurance through their employer (48.8%). The mean BMI for canagliflozin patients was 32.5 kg/m2, indicating a moderately obese sample (Table 1). Overall, 90.2% of the sample reported having at least one comorbidity, with the most commonly reported comorbidities being hypertension (43.4%), hyperlipidemia (35.6%), and joint/chronic pain (30.2%). Approximately half (55.6%) of the sample had a diagnosis of T2DM for 1–5 years, 19.0% had T2DM for 6–10 years, and 22.0% of the sample had T2DM for >10 years. The majority of the patients (68.3%) had been taking canagliflozin for less than 1 year (Table 1).
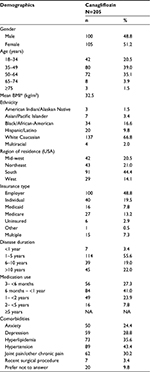  | Table 1 Patient demographics Notes: *Mean BMI based on n=199. Abbreviations: BMI, body mass index; NA, not applicable. |
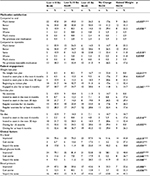
Few demographic differences emerged between weight groups (Table 2). Patients in the Lost >10 lbs group were older than the other weight groups, and patients who lost weight were significantly more likely to have insurance through their employer compared to patients whose weight did not change or who gained weight. Treatment and health satisfaction levels, as measured by the CHES-Q and DTSQ were generally similar across groups (Table 3), although the Lost >10 lbs group demonstrated a significantly lower perceived frequency of hyperglycemia compared to the remaining four weight groups on the DTSQ (Table 3). Differences in diabetes distress emerged between weight groups on the DDS with the Lost >10 lbs group exhibited a significantly lower scores for the total DDS as well as the emotional burden and physician-related distress subscale scores (Table 3). Further, the Lost >10 lbs group was the only group not to evidence a moderate level of distress, indicated by a score of ≥3 on the DDS total or subscale scores (Table 3).
Pearson’s correlations were also calculated between the weight grouping variable and the summary scores from each of the established surveys, allowing for a comparison of the relationship between each individual group’s established survey scores to the remaining groups in the sample (ie, Gained Weight vs other for groups). Reporting a loss >10 lbs was significantly correlated with a lower total DDS score (–0.166, p=0.017), indicating a decreased level of distress; decreased emotional (–0.174, p=0.013), physician-related (–0.154, p=0.028), and regimen-related DDS subscale scores (–0.167, p=0.017; Table 5), indicating a reduced level of distress in each of these three areas, were also significantly correlated with losing >10 lbs. A similar analysis of DTSQ scores that revealed a lower perceived frequency of hyperglycemia (–0.271, p<0.0001) and hypoglycemia (–0.153, p=0.028) was also significantly correlated with reporting having lost >10 lbs.
Regarding other health-related behaviors, patients who lost weight trended toward greater participation in weight management, exercise, and diet plans compared to patients who gained weight or whose weight remained the same (Table 4). The Lost >10 lbs group was significantly more likely to be engaged in a weight loss program for a period of at least 6 months compared to the other four groups (p<0.05; Table 4). In addition, patients who lost weight were generally more likely to report improvement in clinical variables of A1c, BGLs, and blood pressure. Patients in the Lost >10 lbs and Lost 5–10 lbs groups were significantly more likely to have improved A1c levels compared to patients who gained weight, while patients in the Lost >10 lbs group also showed significant improvement over patients with no weight change (Table 4). BGLs were also improved with weight loss, and patients in the groups that the Lost >5 lbs group showed a significant improvement compared to patients in the Lost <5 lbs or Gained Weight groups. Weight loss was also associated with improvement in blood pressure, especially in the Lost 5–10 lbs group. Patients who lost at least 5 lbs were also significantly more likely than other weight groups to report that canagliflozin was much better than their previous oral AHA. Additionally, there was a trend toward patients who lost at least 5 lbs to rate canagliflozin as better or much better than their previous injectable AHA; although, one quarter of the sample reported no previous use of injectable medications compared to <4% for oral medications.
Bivariate comparisons were also examined in regression models controlling for patient and treatment characteristics; for these analyses the weight gained group served as the reference group. Losing >10 lbs was a significantly associated with reduced distress on the DDS Total Score and the emotional burden and regimen-related distress subscales (p<0.05). Older age was also significantly associated with lower levels of diabetes distress, while concomitant use of DPP-4 or sulfonylureas was significantly associated with greater distress (p<0.05). In addition to decreased distress, losing >10 lbs was significantly associated with improved A1c and BGLs, whereas losing 5–10 lbs was significantly related to improved BGLs and blood pressure (p<0.05). Finally, losing >10 lbs and older age were both associated with decreases in the perceived frequency of hyperglycemia.
Discussion
Weight management is a major component of patient’s experience with diabetes care. The majority of patients with T2DM are overweight or obese, and this additional weight can lead to increased insulin resistance and increased risk for micro- and macrovascular complications.1–5,13,14 Although diet and exercise are suggested for all patients with T2DM, many patients continue to struggle with weight management in part due to undesirable metabolic effects of some AHAs.13,15 Canagliflozin is the first in the newest class of AHAs, SGLT2 inhibitors, that is proven to significantly lower A1C in adults with T2DM. SGLT2 inhibitors work by blocking glucose reabsorption in the kidney, which results in excretion of glucose and its associated calories in the urine. This mechanism of action lowers BGLs and may cause moderate weight loss.34,35 This study assessed the impact of moderate weight loss on two dimensions of the Triple Aim framework, patient experiences and self-reported outcomes, among patients with T2DM prescribed canagliflozin for at least 3 months. Specifically, patient health, treatment satisfaction, and engagement in lifestyle changes were assessed based on reported weight change since initiating canagliflozin.
Overall the sample was largely representative of the population of patients with T2DM. Patients were moderately obese with a mean BMI of 32.5 kg/m2, suggesting that weight management was an issue for most patients. The majority of patients had been diagnosed with T2DM for 1–5 years and had been taking canagliflozin for <1 year, which is consistent with its time on the market at the time of data collection for this study. The majority of patients (66.8%) in this study reported some weight loss since initiating canagliflozin, which is consistent with findings in clinical trials.34–36
Patients taking canagliflozin who reported losing weight exhibited better emotional and physical health compared to patients who did not report weight loss. In particular, patients who lost >10 lbs had significantly lower diabetes distress scores compared to the Lost <5 lbs, No Change, and Gained Weight groups. These patients also reported a lower perceived frequency of hyperglycemia compared to the other four weight groups, suggesting that patients who lost >10 lbs were more adept at managing BGLs. Additionally, any weight loss was generally associated with improvement in patient’s physical health, as quantified by self-reported improvements in BGLs, blood pressure, and A1c. In particular, BGLs were significantly improved in the sample of patients who lost >5 lbs in multivariate regression analyses, supportive of the trend toward reduced hyperglycemia observed in a portion of this group. Regression analyses also revealed significant improvement in A1c levels, within the Lost >10 lbs group. The finding of improved A1c levels only in the group of patients who lost the greatest amount of weight potentially points to an extended duration of positive self-management behavior in this group, as A1c levels do not change as rapidly as BGLs. The improvement in physical health with use of canagliflozin observed here, including weight loss and improvements in BGLs, blood pressure, and A1c, have been previously reported in clinical trials.34,36 The additional relationship demonstrated between weight loss and improved emotional health, as assessed by the reduction in distress, indicates that improvement in patient physical health stands to lead to improvement in multiple aspects of patient experience and outcomes with T2DM.
In addition to their gains in physical and emotional health, patients who lost weight also showed a trend toward increased engagement in lifestyle changes and increased satisfaction with canagliflozin. Patients who lost >5 lbs were significantly more likely than patients in the No Change or Gained Weight groups to have been engaged in a weight loss plan for at least 6 months. This trend toward increased participation in a weight loss plan was continued between the Lost >10 lbs group compared to patients in the Lost 5–10 lbs or Lost <5 lbs groups. Similarly, trends for increased participation in diet and exercise regimens were also observed for patients who reported weight loss compared to those who did not. These findings of increased engagement in lifestyle changes in the population of patients taking canagliflozin who lost weight may indicate that success in meeting lifestyle goals may initiate a positive feedback loop that promotes ongoing good health behaviors. Furthermore, the differences observed within the weight loss groups between patients who lost some weight (<10 lbs) compared to patients in the Lost >10 lbs group lends additional credence to the idea that a change in patient health can initiate long-term positive health behaviors as patients who lost the most weight were engaged in lifestyle changes for an increased duration. In addition to engaging in more positive health behaviors, patients who lost weight showed increased satisfaction with canagliflozin compared to previous oral and injectable AHAs. Other studies have also shown this relationship between weight loss and increased satisfaction, improved quality of life, or positive health outcomes.15,17,37 The results of this survey confirm many of these findings and demonstrate additional links between weight loss, medication satisfaction, engagement in self-management behaviors, and positive physical and emotional health outcomes within a sample of patients with T2DM prescribed canagliflozin. These findings mirror those of other studies of patients with T2DM prescribed canagliflozin that found improved HRQoL and greater physical and emotional health satisfaction with weight loss ≥5 lbs.15
There are several limitations of this study. The cross-sectional design makes it difficult to assess the direct impact of losing weight on patient’s motivation to maintain lifestyle changes over time. The trend toward greater weight loss, improved diabetes self-management behaviors, and improved blood glucose management observed in this study suggests that the two may be related and is consistent with other studies that link weight loss and self-management behavior,15 although it was not feasible to assess causality in this study. Further work is certainly needed to confirm the directionality between weight loss and the positive lifestyle changes and patient outcomes observed within the population with T2DM; a greater understanding of the impact of weight loss on patient’s long-term diabetes self-management behaviors is also of interest. Additionally, the impact of other concomitant medications, both for T2DM and other comorbidities, was not addressed in this study. Therefore, weight loss observed in this study cannot be attributed specifically to canagliflozin, but to a treatment regimen containing canagliflozin. Similarly, the potential impact of other medications on weight gain, despite inclusion of canagliflozin in a patient’s treatment regimen cannot be ascertained. Along a similar line, the relative impact of detailed patient factors, for example, education level or socioeconomic status, may also be confounding factors. Our finding that patients in the Lost >10 lbs group were more likely to have employer-sponsored insurance may point to an interaction between weight management and socioeconomic status within a population of patients with T2DM. Additional study into treatment and patient-related factors that influence weight management is certainly warranted within a T2DM population. Finally, this survey took all comers and results presented here only include patients who were prescribed canagliflozin; therefore, the findings reported may not generalize to all populations of patients with T2DM.
Although there are various medications to assist patients with T2DM in regulating their BGLs, lifestyle changes remain a critical factor in the management of T2DM, especially for overweight or obese patients. The American Diabetes Association and the European Association for the Study of Diabetes endorse an individualized treatment approach that accounts for each patient’s specific comorbidities, attitude and expected treatment efforts, and support system, among other factors.5 The variety of available AHAs have different risk/benefit profiles designating some agents more appropriate for subsets of the population of patients with T2DM. For example, weight gain is a side effect of multiple AHAs, making them a poor choice for patients having difficulty with weight management.12 In these cases, choices of agents that are weight neutral or help with weight reduction may assist patients in initiating and maintaining lifestyle changes. This assistance could be especially helpful in treating patients with T2DM who are having difficulty managing their weight with diet and exercise.12,38,39
This study demonstrates that weight loss is associated with positive diabetes self-management behaviors, improved patient outcomes, and reduced distress among patients with T2DM using canagliflozin. Taken together, these findings indicate that success within one area of diabetes management, for example, weight loss of 5–10 lbs, may be associated with patients’ overall experience and outcomes, which is critical in achieving two dimensions of the Triple Aim, improving patient experience of care and improving health of populations. Further studies are warranted to assess the impact of moderate weight loss, on the third dimension of the Triple Aim, reducing per capita health care costs.
Acknowledgment
Janssen Scientific Affairs, LLC,funded this study.
Disclosure
SCB and JC are the employees of Janssen Scientific Affairs, LLC, and are stockholders in Johnson and Johnson. Study sponsors contributed to study design, interpretation of results, and manuscript development. The other authors report no conflicts of interest in this work.
References
Bash LD, Selvin E, Steffes M, Coresh J, Astor BC. Poor glycemic control in diabetes and the risk of incident chronic kidney disease even in the absence of albuminuria and retinopathy: Atherosclerosis Risk in Communities (ARIC) Study. Arch Intern Med. 2008;168(22):2440–2447. | ||
Beckman JA, Creager MA, Libby P. Diabetes and atherosclerosis: epidemiology, pathophysiology, and management. JAMA. 2002;287(19):2570–2581. | ||
Kempen JH, O’Colmain BJ, Leske MC, et al. The prevalence of diabetic retinopathy among adults in the United States. Arch Ophthalmol. 2004;122(4):552–563. | ||
Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321(7258):405–412. | ||
Inzucchi SE, Bergenstal RM, Buse JB, et al. Management of hyperglycemia in type 2 diabetes: a patient-centered approach: position statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2012;35(6):1364–1379. | ||
Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014. Atlanta, GA: US Department of Health and Human Services; 2014. | ||
American Diabetes Association. Economic costs of diabetes in the US in 2012. Diabetes Care. 2013;36(4):1033–1046. | ||
Berwick DM, Nolan TW, Whittington J. The triple aim: care, health, and cost. Health Aff (Millwood). 2008;27(3):759–769. | ||
Hibbard JH, Greene J. What the evidence shows about patient activation: better health outcomes and care experiences; fewer data on costs. Health Aff (Millwood). 2013;32(2):207–214. | ||
American Diabetes A. Standards of Medical Care in Diabetes-2016 Abridged for Primary Care Providers. Clin Diabetes. 2016;34(1):3–21. | ||
American Association of Diabetes Educators. AADE7 self-care behaviors. Available from https://www.diabeteseducator.org/patient-resources/aade7-self-care-behaviors. Accessed June 23, 2016. | ||
Pi-Sunyer FX. The impact of weight gain on motivation, compliance, and metabolic control in patients with type 2 diabetes mellitus. Postgrad Med. 2009;121(5):94–107. | ||
Norris SL, Zhang X, Avenell A, et al. Efficacy of pharmacotherapy for weight loss in adults with type 2 diabetes mellitus: a meta-analysis. Arch Intern Med. 2004;164(13):1395–1404. | ||
Sullivan PW, Morrato EH, Ghushchyan V, Wyatt HR, Hill JO. Obesity, inactivity, and the prevalence of diabetes and diabetes-related cardiovascular comorbidities in the U.S., 2000–2002. Diabetes Care. 2005;28(7):1599–1603. | ||
Traina S, Guthrie R, Slee A. The impact of weight loss on weight-related quality of life and health satisfaction: results from a trial comparing canagliflozin with sitagliptin in triple therapy among people with type 2 diabetes. Postgrad Med. 2014;126(3):7–15. | ||
Lau DC, Teoh H. Benefits of modest weight loss on the management of type 2 diabetes mellitus. Can J Diabetes. 2013;37(2):128–134. | ||
Look ARG, Pi-Sunyer X, Blackburn G, et al. Reduction in weight and cardiovascular disease risk factors in individuals with type 2 diabetes: one-year results of the look AHEAD trial. Diabetes Care. 2007;30(6):1374–1383. | ||
Goldney RD, Phillips PJ, Fisher LJ, Wilson DH. Diabetes, depression, and quality of life: a population study. Diabetes Care. 2004;27(5):1066–1070. | ||
Huang ES, Brown SE, Ewigman BG, Foley EC, Meltzer DO. Patient perceptions of quality of life with diabetes-related complications and treatments. Diabetes Care. 2007;30(10):2478–2483. | ||
Redekop WK, Koopmanschap MA, Stolk RP, Rutten GE, Wolffenbuttel BH, Niessen LW. Health-related quality of life and treatment satisfaction in Dutch patients with type 2 diabetes. Diabetes Care. 2002;25(3):458–463. | ||
Wandell PE. Quality of life of patients with diabetes mellitus. An overview of research in primary health care in the Nordic countries. Scand J Prim Health Care. 2005;23(2):68–74. | ||
Watkins KW, Connell CM, Fitzgerald JT, Klem L, Hickey T, Ingersoll-Dayton B. Effect of adults’ self-regulation of diabetes on quality-of-life outcomes. Diabetes Care. 2000;23(10):1511–1515. | ||
Klein S, Sheard NF, Pi-Sunyer X, et al. Weight management through lifestyle modification for the prevention and management of type 2 diabetes: rationale and strategies: a statement of the American Diabetes Association, the North American Association for the Study of Obesity, and the American Society for Clinical Nutrition. Diabetes Care. 2004;27(8):2067–2073. | ||
Fu AZ, Qiu Y, Radican L, Wells BJ. Health care and productivity costs associated with diabetic patients with macrovascular comorbid conditions. Diabetes Care. 2009;32(12):2187–2192. | ||
Shetty S, Secnik K, Oglesby AK. Relationship of glycemic control to total diabetes-related costs for managed care health plan members with type 2 diabetes. J Manag Care Pharm. 2005;11(7):559–564. | ||
Zhuo X, Zhang P, Hoerger TJ. Lifetime direct medical costs of treating type 2 diabetes and diabetic complications. Am J Prev Med. 2013;45(3):253–261. | ||
Funnell MM, Anderson RM. Empowerment and Self-Management of Diabetes. Clinical Diabetes. 2004;22(3):123–127. | ||
Tchicaya A, Lorentz N, Demarest S, Beissel J, Wagner DR. Relationship between self-reported weight change, educational status, and health-related quality of life in patients with diabetes in Luxembourg. Health Qual Life Outcomes. 2015;13:149. | ||
Traina SB, Slee A, Woo S, Canovatchel W. The Importance of Weight Change Experiences for Performance of Diabetes Self-Care: A Patient-Centered Approach to Evaluating Clinical Outcomes in Type 2 Diabetes. Diabetes Ther. 2015;6(4):611–625. | ||
Bradley C. Handbook of psychology and diabetes : a guide to psychological measurement in diabetes research and management. Australia; Langhorne, Pa.: Harwood Academic Publishers; 1994. | ||
Polonsky WH, Fisher L, Earles J, et al. Assessing psychosocial distress in diabetes: development of the diabetes distress scale. Diabetes Care. 2005;28(3):626–631. | ||
Traina SB, Colwell HH, Crosby RD, Mathias SD. Pragmatic measurement of health satisfaction in people with type 2 diabetes mellitus using the Current Health Satisfaction Questionnaire. Patient Relat Outcome Meas. 2015;6:103–115. | ||
Rothman KJ. No adjustments are needed for multiple comparisons. Epidemiology. 1990;1(1):43–46. | ||
Stenlof K, Cefalu WT, Kim KA, et al. Efficacy and safety of canagliflozin monotherapy in subjects with type 2 diabetes mellitus inadequately controlled with diet and exercise. Diabetes Obes Metab. 2013;15(4):372–382. | ||
Stenlof K, Cefalu WT, Kim KA, et al. Long-term efficacy and safety of canagliflozin monotherapy in patients with type 2 diabetes inadequately controlled with diet and exercise: findings from the 52-week CANTATA-M study. Curr Med Res Opin. 2014;30(2):163–175. | ||
Schernthaner G, Gross JL, Rosenstock J, et al. Canagliflozin compared with sitagliptin for patients with type 2 diabetes who do not have adequate glycemic control with metformin plus sulfonylurea: a 52-week randomized trial. Diabetes Care. 2013;36(9):2508–2515. | ||
Alvarez Guisasola F, Tofe Povedano S, Krishnarajah G, Lyu R, Mavros P, Yin D. Hypoglycaemic symptoms, treatment satisfaction, adherence and their associations with glycaemic goal in patients with type 2 diabetes mellitus: findings from the Real-Life Effectiveness and Care Patterns of Diabetes Management (RECAP-DM) Study. Diabetes Obes Metab. 2008;10 Suppl 1:25–32. | ||
Idris I, Donnelly R. Sodium-glucose co-transporter-2 inhibitors: an emerging new class of oral antidiabetic drug. Diabetes Obes Metab. 2009;11(2):79–88. | ||
Krentz AJ, Bailey CJ. Oral antidiabetic agents: current role in type 2 diabetes mellitus. Drugs. 2005;65(3):385–411. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.