Back to Journals » Clinical Ophthalmology » Volume 14
Tear Film Characteristics During Wear of Daily Disposable Contact Lenses
Received 14 December 2019
Accepted for publication 23 April 2020
Published 4 June 2020 Volume 2020:14 Pages 1521—1531
DOI https://doi.org/10.2147/OPTH.S242422
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Giancarlo Montani, Maurizio Martino
Dipartimento di Matematica e Fisica “Ennio De Giorgi”, CERCA Università del Salento, Lecce, Italy
Correspondence: Giancarlo Montani
Dipartimento di Matematica e Fisica “Ennio De Giorgi”, CERCA Università del Salento, Via per Arnesano, Lecce 73100, Italy
Email [email protected]
Purpose: To evaluate changes induced over time by three daily disposable (DD) contact lenses on tear meniscus height (TMH), pre-lens non-invasive break-up time (pre-lens NIBUT), tear film osmolarity (TO) and objective quality of vision (OQV).
Patients and Methods: Forty-six subjects enrolled in this prospective open-label unmasked non-randomized simultaneous comparative cross-over study. For the first week of the study, subjects wore a nesofilcon A lens in the right eye and a delefilcon A lens in the left eye. After 3 days of washout, for the second week, subjects wore a nesofilcon A lens in the left eye and a stenfilcon A lens in the right eye. TMH, pre-lens NIBUT, TO and OQV were measured before contact lens fitting and for each contact lens combination on day 1 at 20 minutes and on day 7 after ≥ 8 hours of wear. OQV measurement included the changes of objective scatter index (OSI), the stability index (SI) and the fluctuation index (FI) calculated in a range of time of 20 s from a blink.
Results: TMH was unchanged at 20 minutes wear of all lenses but was significantly reduced after 8 or more hours wear (on day 7) of delefilcon A and stenfilcon A, respectively. Pre-lens NIBUT was significantly reduced with all lenses, while no significant change in TO was observed with any lens. SI and FI increased significantly for all lenses at both wear times.
Conclusion: While the presence of any contact lens on the eye challenges the tear film, nesofilcon A contact lenses, despite their high water content, compared to delefilcon A and stenfilcon A contact lenses, showed a lower overall effect. We speculate that superior tear film behavior while wearing nesofilcon A lenses may translate to improved subjective comfort, but this remains to be evaluated.
Keywords: nesofilcon A, delefilcon A, stenfilcon A, quality of vision, pre-lens tear film stability, tear osmolarity, tear meniscus height
Introduction
The anterior contact lens surface during wear is the first and most important refracting surface. Therefore, maintaining a consistent optical surface is important in order to reduce light scatter and prevent optical aberrations.1 For this reason, it is essential to have adequate tear function and maintain a clean, highly wettable lens surface.2 Contact lens wear has the potential to alter both integrity and stability of the tear film, which in turn will affect the quality of vision.3 Contact lens wear reduces the thickness of the lipid layer of tear film,4,5 induces a quicker tear thinning,6 and increases the evaporation rate,7 with the effect of a reduction of pre-lens tear film stability measured in both soft hydrogel and silicone hydrogel contact lens wearers.8–11 Furthermore, symptomatic soft contact lens wearers compared to asymptomatic ones have a reduced surface coverage by the tear film during the inter-blink period.12 During wear, a gradual accumulation of deposits on the anterior contact lens surface induces a further reduction in pre-lens tear film stability,13 with increased aberrations and light scattering.14 To date, only limited focus has been placed on the effect on retinal optical image quality induced by pre-lens tear film instability in contact lens wearers considering both aberration and light scattering.
Several studies have evaluated the tear meniscus height (TMH) during soft contact lens use;15–18 however, the effect of water content of the lens on TMH during wear is unknown. In other studies, it has been shown that during contact lens wear, tear osmolarity (TO) can increase.19–23 Increased tear film osmolarity has been attributed to an enhanced evaporation rate that results from an unstable pre-lens tear film, and some investigators have advocated that TO evaluation should be an essential part of tear film studies in contact lens wearers.20
Symptoms of dryness and discomfort are reported by up to one-half of contact lens wearers, especially towards the end of the day.24,25 As a result, many wearers will permanently cease contact lens wear.26 Moreover, additional issues such as microbial keratitis and inflammatory conditions induced by contact lens wear are still areas of concern.27–29 It is clear that both contact lens discomfort and inflammation are multifactorial.30,31 In this regard, a normal tear film and the health of the ocular surface both play a large role in the possibility of successfully wearing contact lenses.13
With the continual introduction of new contact lens materials, manufacturers are endeavoring to minimize complications to the ocular surface and maximize user comfort. DD contact lenses meet many of these expectations, and their use is increasing worldwide.32 Conventional hydrogel and silicone hydrogel DD contact lenses have gained in popularity over conventional lens types, although it is important to understand more about their behavior in terms of impact on ocular tear film and tear exchange, as well as on changes in TO during use. To date, there is only limited information in this regard.
Recent advances in technology have led to the production of novel, high-quality, soft lens materials that are believed to be more resistant to the accumulation of deposits and dehydration.33 For the purposes of evaluation, soft contact lenses are generally grouped into 5 categories according to the lens material.33 The first four groups are based on hydrogel materials and differ in water content and ionic properties, while the fifth group is based on silicone hydrogel materials. Silicone hydrogel lenses have a higher porosity to oxygen compared to standard hydrogel lenses, and they accounted for 74% of soft lenses prescribed in 2019, including extended wear lenses.32
The water content of contact lenses has a major impact on lens performance and vision, as well as comfort. Historically, dehydration of the lens has been shown to increase as a function of the lens water content.34,35 For example, silicone hydrogels generally have an inherently lower content of water and are less prone to dehydration than traditional hydrogels.36,37 In the last few years, several daily disposable (DD) contact lenses have been commercialized, some of which (nesofilcon A, delefilcon A, stenfilcon A) are made with innovative materials and designed to obtain the lowest interaction with the tear film. Nesofilcon A contains a high content of water (78%) and is a traditional hydrogel lens based on nonionic polymers that exploits the amphiphilic properties of Pluronic® F127 (BASF, Florham Park, NJ, USA), a polyethylene oxide (PEO)-polypropylene oxide (PPO)-PEO block copolymer surfactant, by incorporating it into a lens fabricated from 2-hydroxyethylmethacryate and an N-vinylpyrrolidone monomer.1 Delefilcon A is a lens with a silicone hydrogel core and bulk water content of 33%, and an approximately 5–6 μm thick layer of modified hydrogel-like “gel” with a water content of ≥80% on the lens surface.38 Stenfilcon A is also a silicone hydrogel lens, but with a low percentage of silicone (4.4%) and a water content of 54%.39
To shed more light on the impact of different materials on tear film during contact lens wear, we assessed the changes in TMH, pre-lens non-invasive break-up time (NIBUT), TO and objective quality of vision (OQV) of these three DD contact lenses in new and previous contact lens wearers.
Patients and Methods
Study Design
Forty-six subjects (12 new and 28 habitual contact lens wearers) with a spherical refractive error < ± 3.50 D and astigmatism <0.75 D were enrolled for this prospective, open-label, unmasked, non-randomized, simultaneous, comparative, cross-over study. The sample size was calculated for assuring validity, accuracy, reliability and integrity of the intended clinical study using the following parameters: effect size dz = 0.55, α error probability = 0.05, power (1-β error probability) = 0.95. This resulted in a total sample size of 38 (non-centrality parameter δ = 3.39, critical t = 1.68, Df = 37, actual power = 0.95). The non-randomized design was selected to prevent confusion during simultaneous wear of different lenses, ie, to ensure that subjects wore the proper lens in each eye over each weekly wear interval. Other outcomes, such as lens performance and wearer comfort were not evaluated as they are outside the scope of the study.
Tear characteristics inclusion criteria, measured before contact lens fitting in new wearers and after 3 days of washout from their contact lenses in habitual wearers, were as follows: pre-corneal NIBUT >10 s, TMH >180 µm and TO <316 mOsmol/L, with no statistically significant differences between eyes, based upon comparison of the means of three measurements of each parameter from each eye. Exclusion criteria included a history of ocular surgery, inflammation, or any contraindication to contact lens wear.
During the first week of the study, subjects were asked to wear always in the right eye (RE) a nesofilcon A lens (Biotrue ONEday, Bausch & Lomb, Rochester, New York, USA) and in the left eye (LE) a delefilcon A lens (Dailies Total1, Alcon, Fort Worth, Texas, USA). After 3 days of washout, the second week of the study was initiated using nesofilcon A lens in the LE and a stenfilcon A lens (MyDay, CooperVision, Fairport, New York, USA) in the RE. The characteristics of contact lenses used for the study are summarized in Table 1.
 |
Table 1 Characteristics of Contact Lenses Evaluated |
Exams were performed using the same sequence (TMH, NIBUT and TO) at controlled temperature (20–25°C) and humidity (30–50%). Baseline TMH was evaluated using a slit lamp-adapted frequency domain (FD) optical coherence tomography (OCT) unit (SL-SCAN-1, Topcon, Chapelle, The Netherlands) with an axial scan resolution of 8–9 µm in tissue, considering the vertical beam of light bisected the inferior meniscus below the center of the cornea, at the 6 o’clock position. NIBUT was measured with tearscope (Easytearsview+, Rovereto, Italy), which provides homogeneous specular reflections on a wide corneal area, mounted on a slit-lamp (SL-D7, Topcon, Chapelle, The Netherlands). NIBUT was considered as the time from the last blink to the first visible break in the tear film with the microscope focused on the anterior surface of the cornea. TO was evaluated with the TearLab Osmolarity System (TearLab Corp, San Diego, CA, USA). Each tear sample was taken by touching the tip of a test card to the surface of the lateral inferior tear meniscus. Before the measurements, reusable electronic check cards, which had been provided by the manufacturer as a means of procedural quality control, were used to verify the function and calibration of the device before testing the patients. Osmolarity control solution testing was also performed for each lot number of the test cards. The mean values obtained from three measurements for each eye were considered as baseline for every procedure used. To avoid the effects of reflex tearing, each set of measurements was separated by a five-minute interval.
The measurements of tear characteristics were repeated during contact lens use on the first day of wear at 20 minutes and on day 7 after a minimum of 8 hours of lens wear using the same test sequence used for baseline measurements (TMH, pre-lens NIBUT, and TO) at controlled temperature (22–25°C) and humidity (30–50%) and over the same range of hours of the day (4:00–6:00 PM) with contact lenses on-eye. Changes in OQV, at baseline and during all section of measurements, were evaluated for a pupillary diameter of 4mm, measuring the objective scatter index (OSI) every 0.5 s for a period of 20 s of interblink interval (subjects were asked not to blink during the time of acquisition and if this condition was not met the measurement was repeated) using a double pass instrument (HD Analyzer, Visiometrics, Terrassa, Spain), which has demonstrated good reproducibility.40,41 OSI quantifies the effect of both ocular light scatter and aberrations and is defined as the ratio between the light intensity in a peripheral annular area (from 12 to 20 minutes of arc) and the central peak (1 minute of arc); an increase of its value is associated with a reduction of optical quality of the retinal image.42 Since our aim was not to evaluate the optical quality of the retinal image immediately after blink but rather to evaluate the changes of OQV during a period of time of 20 s, the comparison was obtained by firstly normalizing all values between groups at the starting point of measurement after a blink by subtracting the respective initial OSI values measured at the beginning of each 20 s set of measures from the remaining values of the set. This approach was necessary to avoid the optical effect of aberrations induced by the different optical design of contact lenses used for the study.43 The changes of OSI over time were quantified also considering the fluctuation (FI) and stability (SI) indices. FI is defined as the average of the standard deviation of the OSI changes obtained over time and was devised to indicate the fluctuations in OSI changes;44 SI is defined as the slope of the linear regression line of the OSI changes obtained over time, to quantify the upward curve in the sawtooth pattern.43
This study followed the tenets of the Declaration of Helsinki and was reviewed and approved by the Institutional Review Board of the University of Salento; after the nature and possible consequences of the study had been explained, all participants signed an informed consent form.
Statistical Analysis
Data were analyzed using SPSS for Windows v.22.0 (SPSS Inc., Chicago, Illinois, USA) and the graphs realized using GraphPad Prism for Windows v.6 (GraphPad Software Inc., La Jolla, CA 92037 United States). The Shapiro–Wilk test was used to confirm normal distribution of all variables. A Student’s t-test for paired data was used to assess (1) differences between eyes at baseline, (2) differences between 20 minutes and 8 hours for the same lens material, and (3) differences between the two lens materials used during each week of study at each wear time. Values were not corrected for multiple comparisons as the variables measured in this study are not random but rather are correlated. Repeated-measures analysis of variance (ANOVA) was used to evaluate OSI changes during 20 s from the starting point. A p-value <0.05 was considered statistically significant for all comparisons.
Results
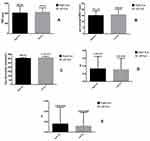
The subjects enrolled in the study presented a mean age of 24±4 years (range 20–26 years; and a mean refractive error of −1.65±1.16 D (range −3.50 to +1.50 D). At the beginning of the study, differences in baseline measurements for TMH, NIBUT, TO, FI and SI between eyes were not statistically significant (p>0.05) (TMH, Figure 1A; pre-corneal NIBUT, Figure 1B; TO, Figure 1C; FI, Figure 1D; SI, Figure 1E). Thus, it was assumed that, apart from the different types of lenses, any other factors affected both eyes equally. The significance of changes with respect to baseline for TMH, pre-lens NIBUT, TO, SI, and FI induced by all lenses tested at 20 minutes and after a mean wear time of 9.2±1.0 hours (range 8–11 hours) for the first week of the study and 9.0±1.2 hours (range 8–11 hours) for the second week of the study are summarized in Table 2.
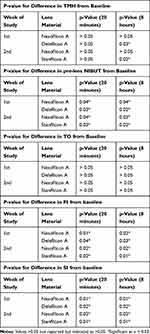 |
Table 2 Significance of Changes in Measured Parameters with Respect to Baseline at 20 Minutes and After 8 Hours of Wear |
The TMH comparison with baseline (Figure 2) showed a significant reduction in eyes wearing delefilcon A (p = 0.03) and stenfilcon A (p = 0.02) lenses after 8 hours wear, but not at 20 minutes wear (both p > 0.05, Table 2). Nesofilcon A lenses did not show a significant reduction of TMH relative to baseline, either at 20 minutes or after 8 hours of wear (both p > 0.05, Table 2). Comparing lenses at the same wear time, or the same lens between the two wear times, no change in THM reduction from baseline was observed between 20 minutes and after 8 hours wear of nesofilcon A lenses (p > 0.05), while TMH reduction was greater after 8 hours than at 20 minutes wear of both delefilcon A and stenfilcon A lenses (both p < 0.05; Figure 2). Further, there was no difference between nesofilcon A and delefilcon A lenses, nor between nesofilcon A and stenfilcon A lenses at 20 minutes of wear (both p > 0.05), but greater reduction with both delefilcon A and stenfilcon A lenses relative to nesofilcon A after 8 hours of wear (both p < 0.05).
For all lenses tested, pre-lens NIBUT compared to baseline was significantly reduced, both at 20 minutes and after 8 hours (all p < 0.05; Table 2), but did not change significantly between 20 minutes and 8 hours with any lens (all p > 0.05, Figure 3A and B). Comparing the reduction of pre-lens NIBUT from baseline, we found a significantly lower reduction with nesofilcon A relative to delefilcon A after both 20 minutes and 8 hours of wear (both p < 0.05) at the end of the first week of the study (Figure 3A). Similarly, we found a significantly lower reduction of pre-lens NIBUT with nesofilcon A relative to stenfilcon A after both 20 minutes and 8 hours of wear (both p < 0.05) at the end of the second week of the study (Figure 3B).
TO did not change significantly from baseline for all lenses tested at all visits (Table 2). Considering the results obtained with nesofilcon A and delefilcon A lenses, the differences from baseline between 20 minutes and after 8 hours wear were not significant with either lens nor were differences between the lenses at either time point (both p > 0.05, Figure 4A). Considering the results obtained with nesofilcon A and stenfilcon A lenses, differences from baseline between 20 minutes and after 8 hours wear were similarly not significant with either lens nor were differences between the lenses at either time point (both p > 0.05, Figure 4B).
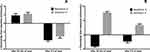
The changes over time of OSI relative to baseline were similar for all materials, although nesofilcon A presented a lower increase after 10 s for measurements done at 20 minutes and after 7 s for measurements done after 8 hours (p<0.05; Figure 5A and B). OSI changes between the measurements carried out at 20 minutes and after 8 hours of wear are also plotted in Figure 5C; in this case delefilcon A and stenficon A lenses presented significant increases after 8 hours of wear (p<0.05), while nesofilcon A lenses did not present significant changes.
 |
Figure 5 Normalized changes in OSI: (A) baseline versus 20 minutes, (B) baseline versus 8 hours, and (C) 20 minutes versus 8 hours for the three lenses tested. |
Considering the FI compared to baseline, its value was significantly increased for all lenses for both the measurements done at 20 minutes and after 8 hours of wear (all p<0.05; Table 2). Comparing the mean changes in FI from baseline induced by nesofilcon A lenses with respect to the other lenses tested, significant increases were found for both delefilcon A (Figure 6A) and stenfilcon A (Figure 6B) lenses both at 20 minutes and after 8 hours of wear (p<0.05). Further, while there was no difference in FI change between 20 minutes and after 8 hours of wear of nesofilcon A lenses (p > 0.05), greater change in FI from baseline was observed between 20 minutes and after 8 hours wear of both delefilcon A and stenfilcon A lenses (both p < 0.05).
Considering SI compared to baseline, its value was significantly increased for all lenses tested for both the measurements done at 20 minutes and after 8 hours of wear (all p<0.05; Table 2). The change in SI relative to baseline induced by nesofilcon A lenses was significantly different from that of stenfilcon A lenses but not delefilcon A lenses after 8 hours of wear, nor from either lens at 20 minutes of wear (Figure 7).
Discussion
Herein, we studied the effects of three DD contact lenses in different materials, namely, nesofilcon A, delefilcon A, and stenfilcon A, on TMH, NIBUT, TO, and OQV. The results broadly demonstrated that with respect to baseline, the contact lenses in nesofilcon A used in this study had a lesser impact on tear film characteristics, with fewer changes in TMH and pre-lens NIBUT relative to the other lenses tested. Compared to baseline, no differences in TO were observed at 20 minutes or after 8 hours of wear with all lenses tested. The results of OSI measurements compared to baseline showed an increase with increasing time from blink for all lenses with a reduction of OQV. Increases in OSI after 10 s from the last blink for measurements taken at 20 minutes and after 7 s for measurements taken after 8 hours were lower with nesofilcon A compared to the other lenses. These results indicate that nesofilcon A lenses may ensure a better optical quality of retinal image between blinks compared to the other lenses, and this effect was more pronounced with longer hours of wear. This behavior can be useful, for example, considering subjects using video display terminals, where the interblink intervals increase.45
While changes from baseline to 20 minutes of wear may reflect the presence of any contact lens more than the particular contact lens worn (nb, differences relative to baseline measured at 20 minutes were either significant for all lenses or not significant for all lenses for each parameter, Table 2), changes from 20 minutes to 8 hours of wear reflect the stability of the effects of respective lens materials on the tear film over wearing time (eg, relative differences between 20 minutes and 8 hours of wear were significant for delefilcon A and stenfilcon A but not nesofilcon A with TMH (Figure 2) and FI (Figure 6), while differences in NIBUT, osmolarity, and SI were not significant with any lens). It should be noted that while this study utilized a non-randomized design that could have affected the results, we do not believe this to be the case as all subjects wore all three test lenses, with no eye wearing the same lens for more than a one-week wearing interval.
All three DD lenses evaluated in the study have novel means of exploiting water characteristics to enhance their performance. Nesofilcon A has a high water content and is composed of a hydrophilic copolymer of 2-hydroxyethyl methacrylate and N-vinyl pyrrolidone. The rationale in designing this lens was to mimic the lipid layer of the tear film in order to inhibit lens surface dehydration and maintain consistent optics.46 Delefilcon A has a lower core water content and is a silicone hydrogel lens with a surface treatment that results in extremely high water content on the surface of the lens. The designers of this lens wanted to maintain the high oxygen permeability of a silicone hydrogel material with the wettability, lubricity, and resistance to the lipid repelling properties of traditional hydrogel lenses with a high water content.47 Stenfilcon A is a silicone hydrogel containing less raw silicone, enabling more space for the hydrophilic material. The differences among lens properties may explain the different results obtained with measurements more related to surface wettability. The pre-lens NIBUT was shorter with all lenses tested compared with baseline, confirming earlier studies on the effects of contact lenses on the tear film.8,48 This effect was found to be lower with nesofilcon A lenses, which had a pre-lens NIBUT that was approximately 3 s greater than those of the other materials. While one might speculate that this result is due to the traditional hydrogel character of the nesofilcon A lens, we do not believe that this alone explains this result since the delefilcon A silicone hydrogel lens behaves more like a traditional hydrogel lens at the surface, with much higher water content than that of the stenfilcon A silicone hydrogel lens. This result can be considered clinically relevant, especially for wearers with dry eye symptoms.25
The evaluation of the effect of contact lens wear on OQV through measurement of OSI showed a progressive increase over time with all materials, but a lower increase with lenses of nesofilcon A, the material with longest pre-lens NIBUT. It is interesting to note that both lenses made from silicone hydrogel materials showed an increase in ocular scattering after 8 hours of wear. This potentially could be explained by the presence of deposits on the anterior surface, higher with silicone hydrogel lens materials relative to conventional hydrogels,12,49,50 rather than by a reduction in wettability, since there were no significant changes in pre-lens NIBUT during wear.
A previous study comparing lenses made with nesofilcon A and delefilcon A found no difference in corneal thickness after 1 day of use.48 Moreover, Schafer et al evaluated the surface water characteristics of nesofilcon A and delefilcon A versus those of a conventional lens of etafilcon A.1 Compared with the other two lenses, nesofilcon A was seen to maintain its water content after 15 minutes of wear, and no significant differences were seen in tear film osmolarity, tear meniscus area, central corneal thickness, or corneal aberrations as a function of time of use. Our data largely confirm these results.
Of interest, some authors have suggested that a reduction in the amount of tear meniscus may be related to discomfort,51 and an increased tear film osmolarity has been associated with dry eye disease.52 It is well known that contact lens use has the potential to induce symptoms of dryness and discomfort, which may be related to alterations in TO.25 The study by Ruiz-Alcocer et al revealed no differences in TO after 8 hours wear of DD lenses, similar to that found herein, nor tear meniscus changes measured upon lens removal.48 Contrary to the present study, significant changes in TMH were seen with the silicone hydrogel lenses after 8 hours of wear; these differences between studies can be explained by the different procedures followed during the measurements (in our study done with lenses on). A possible explanation for our results could be related to an increase in water loss from silicone hydrogel lenses, even if there were no effects on TO. In this regard, it would seem relevant that compared to silicone hydrogel lenses, the hydrogel lenses have significantly higher thickness and higher water content. These hydrogel-based lenses appear to be more resistant to dehydration1 and do not significantly impact the tear film or corneal swelling after 1 day of normal wear.51 As a consequence, by minimizing dehydration, lenses made in nesofilcon A compared to a lens made in a silicone hydrogel material have the potential to reduce alterations in ocular physiology during contact lens wear, while providing greater stability of the tear film with a better retinal image optical quality after a blink. In contrast, it has been reported that other commercially available lenses with a high water content may be prone to dehydration leading to loss of comfort and alterations in visual acuity.35
Conclusion
Compared to silicone hydrogel contact lenses in delefilcon A and stenfilcon A materials, contact lenses in nesofilcon A hydrogel material, despite their high water content, showed a lower reduction of tear meniscus height after 8 hours of wear, even if there were no significant differences between lenses in TO. Nesofilcon A contact lenses were also associated with longer pre-lens NIBUT and numerically lower increases of OSI over time with respect to the other lenses, providing a higher quality of a retinal image. In conclusion, the results of this study highlight that nesofilcon A contact lenses reduce the effects of potential causes that can lead many wearers to permanently cease contact lens wear.
Acknowledgment
The abstract of this paper was presented at the NCC2018 the Dutch Contact Lens Congress as a poster presentation with interim findings. The poster’s abstract was published in “BCLA Conference Abstracts 2015 – 2018” in Contact Lens and Anterior Eye Vol. 41, Suppl. 1 June 2018, Pag. S94: https://doi.org/10.1016/j.clae.2018.04.045.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Schafer J, Steffen R, Reindel W, Chinn J. Evaluation of surface water characteristics of novel daily disposable contact lens materials, using refractive index shifts after wear. Clin Ophthalmol. 2015;9:1973–1979. doi:10.2147/OPTH.S90376
2. Cho P, Ng V. Clinical performances of two disposable soft contact lenses of different materials on Hong Kong-Chinese. Cont Lens Anterior Eye. 2000;23(2):53–60. doi:10.1016/S1367-0484(00)80026-0
3. Thai LC, Tomlinson A, Ridder WH. Contact lens drying and visual performance: the vision cycle with contact lenses. Optom Vis Sci. 2002;79(6):381–388. doi:10.1097/00006324-200206000-00012
4. Faber E, Golding TR, Lowe R, Brennan NA. Effect of hydrogel lens wear on tear film stability. Optom Vis Sci. 1991;68(5):380–384. doi:10.1097/00006324-199105000-00010
5. Young G, Efron N. Characteristics of the pre-lens tear film during hydrogel contact lens wear. Ophthalmic Physiol Opt. 1991;11(1):53–58. doi:10.1111/j.1475-1313.1991.tb00195.x
6. Nichols JJ, Mitchell GL, King-Smith PE. Thinning rate of the precorneal and prelens tear films. Invest Ophthalmol Vis Sci. 2005;46(7):2353–2361. doi:10.1167/iovs.05-0094
7. Guillon M, Maissa C. Contact lens wear affects tear film evaporation. Eye Contact Lens. 2008;34(6):326–330. doi:10.1097/ICL.0b013e31818c5d00
8. Llorens-Quintana C, Mousavi M, Szczesna-Iskander D, Iskander DR. Non-invasive pre-lens tear film assessment with high-speed videokeratoscopy. Cont Lens Anterior Eye. 2018;41(1):18–22. doi:10.1016/j.clae.2017.08.005
9. Alonso-Caneiro D, Iskander DR, Collins MJ. Tear film surface quality with soft contact lenses using dynamic area high-speed videokeratoscopy. Eye Contact Lens. 2009;35(5):227–231. doi:10.1097/ICL.0b013e3181b3350f
10. Szczesna-Iskander DH, Iskander DR, Read SA, Alonso-Caneiro D. Noninvasive in vivo assessment of soft contact lens type on tear film surface quality. Invest Ophthalmol Vis Sci. 2012;53(1):525–531. doi:10.1167/iovs.11-8257
11. Szczesna-Iskander DH. Comparison of tear film surface quality measured in vivo on water gradient silicone hydrogel and hydrogel contact lenses. Eye Contact Lens. 2014;40(1):23–27. doi:10.1097/ICL.0000000000000008
12. Guillon M, Dumbleton KA, Theodoratos P, et al. Association between contact lens discomfort and pre-lens tear film kinetics. Optom Vis Sci. 2016;93(8):881–891. doi:10.1097/OPX.0000000000000866
13. Downie LE, Craig JP. Tear film evaluation and management in soft contact lens wear: a systematic approach. Clin Exp Optom. 2017;100(5):438–458. doi:10.1111/cxo.12597
14. Koh S. Mechanisms of visual disturbance in dry eye. Cornea. 2016;35(Suppl 1):S83–S88. doi:10.1097/ICO.0000000000000998
15. Le Q, Jiang C, Jiang AC, Xu J. The analysis of tear meniscus in soft contact lens wearers by spectral optical coherence tomography. Cornea. 2009;28(8):851–855. doi:10.1097/ICO.0b013e318197ec24
16. Nagahara Y, Koh S, Maeda N, Nishida K, Watanabe H. Prominent decrease of tear meniscus height with contact lens wear and efficacy of eye drop instillation. Eye Contact Lens. 2015;41(5):318–322. doi:10.1097/ICL.0000000000000134
17. Wang J, Cox I, Reindel WT. Upper and lower tear menisci on contact lenses. Invest Ophthalmol Vis Sci. 2009;50(3):1106–1111. doi:10.1167/iovs.08-2458
18. Bitton E, Jones L, Simpson T, Woods C. Influence of the blink interval on tear meniscus height in soft contact lens and nonlens wearers. Eye Contact Lens. 2010;36(3):156–163. doi:10.1097/ICL.0b013e3181dae228
19. Iskeleli G, Karakoc Y, Ozkok A, Arici C, Ozcan O, Ipcioglu O. Comparison of the effects of first and second generation silicone hydrogel contact lens wear on tear film osmolarity. Int J Ophthalmol. 2013;6(5):666–670. doi:10.3980/j.issn.2222-3959.2013.05.22
20. Stahl U, Willcox MD, Naduvilath T, Stapleton F. Influence of tear film and contact lens osmolality on ocular comfort in contact lens wear. Optom Vis Sci. 2009;86(7):857–867. doi:10.1097/OPX.0b013e3181ae027b
21. Aslan Bayhan S, Bayhan HA, Muhafiz E, Bekdemir S, Gurdal C. Effects of osmoprotective eye drops on tear osmolarity in contact lens wearers. Can J Ophthalmol. 2015;50(4):283–289. doi:10.1016/j.jcjo.2015.03.008
22. Iskeleli G, Karakoc Y, Aydin O, Yetik H, Uslu H, Kizilkaya M. Comparison of tear-film osmolarity in different types of contact lenses. CLAO J. 2002;28(4):174–176. doi:10.1097/01.ICL.0000024117.46518.A4
23. Sarac O, Gurdal C, Bostanci-Ceran B, Can I. Comparison of tear osmolarity and ocular comfort between daily disposable contact lenses: hilafilcon B hydrogel versus narafilcon A silicone hydrogel. Int Ophthalmol. 2012;32(3):229–233. doi:10.1007/s10792-012-9556-y
24. Guillon M, Maissa C. Dry eye symptomatology of soft contact lens wearers and non wearers. Optom Vis Sci. 2005;82(9):829–834. doi:10.1097/01.opx.0000178060.45925.5d
25. Nichols JJ, Sinnott LT. Tear film, contact lens, and patient-related factors associated with contact lens-related dry eye. Invest Ophthalmol Vis Sci. 2006;47(4):1319–1328. doi:10.1167/iovs.05-1392
26. Dumbleton K, Woods CA, Jones LW, Fonn D. The impact of contemporary contact lenses on contact lens discontinuation. Eye Contact Lens. 2013;39(1):93–99. doi:10.1097/ICL.0b013e318271caf4
27. Chalmers RL, Keay L, Long B, Bergenske P, Giles T, Bullimore MA. Risk factors for contact lens complications in US clinical practices. Optom Vis Sci. 2010;87(10):725–735. doi:10.1097/OPX.0b013e3181f31f68
28. Chalmers RL, Wagner H, Mitchell GL, et al. Age and other risk factors for corneal infiltrative and inflammatory events in young soft contact lens wearers from the Contact Lens Assessment in Youth (CLAY) study. Invest Ophthalmol Vis Sci. 2011;52(9):6690–6696. doi:10.1167/iovs.10-7018
29. Stapleton F, Keay L, Edwards K, et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmology. 2008;115(10):1655–1662. doi:10.1016/j.ophtha.2008.04.002
30. Efron N, Jones L, Bron AJ, et al. The TFOS International Workshop on Contact Lens Discomfort: report of the contact lens interactions with the ocular surface and adnexa subcommittee. Invest Ophthalmol Vis Sci. 2013;54(11):TFOS98–TFOS122. doi:10.1167/iovs.13-13187
31. Fonn D. Targeting contact lens induced dryness and discomfort: what properties will make lenses more comfortable. Optom Vis Sci. 2007;84(4):279–285. doi:10.1097/OPX.0b013e31804636af
32. Morgan PB, Woods CA, Tranoudis IG, et al. International contact lens prescribing in 2019. Contact Lens Spectrum. 2020;35(1):26–32.
33. White P. Contact lenses & solutions summary; 2019. Available from: https://www.clspectrum.com/resources/class-pdfs/7_19-class_final.
34. Gonzalez-Meijome JM, Lopez-Alemany A, Almeida JB, Parafita MA, Refojo MF. Qualitative and quantitative characterization of the in vitro dehydration process of hydrogel contact lenses. J Biomed Mater Res B Appl Biomater. 2007;83(2):512–526. doi:10.1002/jbm.b.30824
35. Ramamoorthy P, Sinnott LT, Nichols JJ. Contact lens material characteristics associated with hydrogel lens dehydration. Ophthalmic Physiol Opt. 2010;30(2):160–166. doi:10.1111/j.1475-1313.2009.00705.x
36. Gonzalez-Meijome JM, da Silva AC, Neves H, Lopes-Ferreira D, Queiros A, Jorge J. Clinical performance and “ex vivo” dehydration of silicone hydrogel contact lenses with two new multipurpose solutions. Cont Lens Anterior Eye. 2013;36(2):86–92. doi:10.1016/j.clae.2012.10.071
37. Morgan PB, Efron N. In vivo dehydration of silicone hydrogel contact lenses. Eye Contact Lens. 2003;29(3):173–176. doi:10.1097/01.ICL.0000072825.23491.59
38. Stone RP. Introducing water gradient technology. Contact Lens Spectrum. 2013;28(6):34–38.
39. Pence N. New Entries into the SiHy Daily Disposable Category. Contact Lens Spectrum. 2015;30(12):17.
40. Hu A-L, Qiao L-Y, Zhang Y, Cai X-G, Li L, Wan X-H. Reproducibility of optical quality parameters measured at objective and subjective best focuses in a double-pass system. Int J Ophthalmol. 2015;8(5):1043–1050. doi:10.3980/j.issn.2222-3959.2015.05.34
41. Fernández J, Rodríguez-Vallejo M, Martínez J, et al. Agreement and repeatability of objective systems for assessment of the tear film. Graefes Arch Clin Exp Ophthalmol. 2018;256(8):1535–1541. doi:10.1007/s00417-018-3986-9
42. Artal P, Benito A, Pérez GM, et al. An objective scatter index based on double-pass retinal images of a point source to classify cataracts. PLoS One. 2011;6(2):e16823. doi:10.1371/journal.pone.0016823
43. Martinez-Roda JA, Vilaseca M, Ondategui JC, Aguirre M, Pujol J. Effects of aging on optical quality and visual function. Clin Exp Optom. 2016;99(6):518–525. doi:10.1111/cxo.12369
44. Koh S, Maeda N, Hirohara Y, et al. Serial measurements of higher-order aberrations after blinking in normal subjects. Invest Ophthalmol Vis Sci. 2006;47(8):3318–3324. doi:10.1167/iovs.06-0018
45. Coles-Brennan C, Sulley A, Young G. Management of digital eye strain. Clin Exp Optom. 2018;23(1):1–12.
46. FDA 510(k) Summary K113703. Bausch +Lomb Nesofilcon A contact lens; June 5, 2012. Available from: https://www.accessdata.fda.gov/cdrh_docs/pdf11/K113703.pdf.
47. Pruitt J, Bauman E. The development of Dailies Total1 water gradient contact lenses. Contact Lens Spectrum. 2013;28(6):40–44.
48. Ruiz-Alcocer J, Monsalvez-Romin D, Garcia-Lazaro S, Albarran-Diego C, Hernandez-Verdejo JL, Madrid-Costa D. Impact of contact lens material and design on the ocular surface. Clin Exp Optom. 2018;101(2):188–192. doi:10.1111/cxo.12622
49. Maissa C, Guillon M, Cockshott N, Garofalo RJ, Lemp JM, Boclair JW. Contact lens lipid spoliation of hydrogel and silicone hydrogel lenses. Optom Vis Sci. 2014;91(9):1071–1083. doi:10.1097/OPX.0000000000000341
50. Walther H, Subbaraman L, Jones LW. In vitro cholesterol deposition on daily disposable contact lens materials. Optom Vis Sci. 2016;93(1):36–41. doi:10.1097/OPX.0000000000000749
51. Del Aguila-Carrasco AJ, Ferrer-Blasco T, Garcia-Lazaro S, Esteve-Taboada JJ, Montes-Mico R. Assessment of corneal thickness and tear meniscus during contact-lens wear. Cont Lens Anterior Eye. 2015;38(3):185–193. doi:10.1016/j.clae.2015.01.010
52. Potvin R, Makari S, Rapuano CJ. Tear film osmolarity and dry eye disease: a review of the literature. Clin Ophthalmol. 2015;9:2039–2047. doi:10.2147/OPTH.S95242
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.